
Pain Relief Without the Trade-Off: Prioritizing Safety and Mobility
For many older adults, the worst part of pain treatment is not the pain. It is the strange trade that follows: a little less ache, a lot more wobble.
That is the quiet problem at the heart of orthopedic pain management. A plan that dulls pain but leaves someone groggy on the stairs, foggy at breakfast, or unsteady on the way to the bathroom is not really solving the problem. It is just moving the danger to a different room.
Keep guessing, and the cost can rise fast: more falls, less confidence, worse sleep, and a smaller daily life. This guide helps you think about pain relief the safer way, with function first.
- ✔ Spot the sedation trap before it starts.
- ✔ Discover non-drug relief that exceeds expectations.
- ✔ Master medication reviews where fall risk matters as much as comfort.
Because pain scores do not tell the whole story. Because “stronger” is not always better. Because staying alert is part of treatment, too.
Table of Contents
Safety / Disclaimer
This article is educational content, not individual medical advice. In older adults, medication choices can change fall risk, reaction time, bowel function, thinking, and breathing. That matters even more when pain treatment overlaps with sleep medication, anti-anxiety medication, antihistamines, alcohol, or other drugs that can cloud balance and attention.
The CDC advises added caution and closer monitoring when opioids are used in adults age 65 and older, and specifically notes fall-risk assessment and monitoring for cognitive impairment as part of safer care. The American Geriatrics Society’s public guidance also warns older adults to be cautious with medications that raise the odds of unwanted drug reactions or overmedication.
So the frame here is simple and serious: any plan that reduces pain but raises the risk of a fall, confusion, or frightening daytime grogginess deserves a second look. Medication changes, including stopping long-used drugs, should be reviewed with a licensed clinician or pharmacist.
- Ask whether a treatment protects alertness as well as comfort.
- Review all medications together, not one in isolation.
- Treat new dizziness, confusion, or morning “hangover” as a real safety issue.
Apply in 60 seconds: Circle every medication or over-the-counter product taken for pain, sleep, allergy, or anxiety before the next appointment.
When to Seek Help
Don’t wait this out if pain comes with red flags
Orthopedic pain can be ordinary and still exhausting. But some patterns should move you out of “maybe it will settle down” territory and into same-day or urgent evaluation. Pain with fever, new inability to bear weight, sudden major swelling, a hot red joint, or new weakness is not the time for heroic patience.
Seek urgent care for new weakness, fever, inability to bear weight, or sudden swelling
A few years ago, I watched an older neighbor call her knee “just angry” for three straight days. By the time she agreed to get checked, the real story was far less poetic and much more clinical. That is the trouble with orthopedic pain: the body sometimes whispers in the accent of something familiar. If the joint suddenly looks different, behaves differently, or comes with systemic symptoms, escalation is sensible, not dramatic.
Call promptly if a new medicine caused sleepiness, dizziness, confusion, or a fall
If a medication change is followed by wobbliness, “not feeling right,” slowed speech, unusual sleepiness, a near fall, or an actual fall, call promptly. Older adults often underreport sleepiness because it sounds minor, almost impolite. In real life, it can be the first domino.
- Yes / No: New weakness in the leg, foot, arm, or hand?
- Yes / No: Fever, chills, or a hot swollen joint?
- Yes / No: Suddenly unable to bear weight or walk as usual?
- Yes / No: New confusion, severe drowsiness, or a fall after a medication change?
Neutral next step: If any answer is yes, contact urgent care, the prescribing clinician, or emergency services based on severity.
Who This Is For / Not For
Who this is for
Older adults with joint, back, hip, knee, shoulder, or post-injury orthopedic pain
This article is for the reader whose pain is real, recurring, and annoyingly domestic. The stairs have become a negotiation. The car seat is now a puzzle box. Standing to cook feels longer than it used to, as though the floor has quietly raised its rent.
Caregivers trying to reduce “groggy but still hurting” treatment plans
It is also for spouses, adult children, and caregivers who have seen the unhappy math of a pain plan that dulls the person without solving the problem. Pain is still there, just wearing a bathrobe.
Readers who want pain relief without feeling foggy, unstable, or overmedicated
If the main goal is to stay mentally present, walk more safely, and protect independence while still treating pain with respect, you are in the right room.
Who this is not for
People with emergency symptoms, severe trauma, or rapidly worsening neurologic changes
Acute emergencies deserve urgent care, not a browser tab and optimism.
Readers looking for a medication-dosing guide
This is not a dosing guide or a substitute for individual medical advice. Older adults vary widely in kidney function, drug sensitivity, other diagnoses, and medication interactions.
Situations where cancer pain, palliative care, or end-of-life care changes the treatment frame
Those situations often call for a different balance of comfort, function, time horizon, and risk tolerance. The rules of the room change, and rightly so.
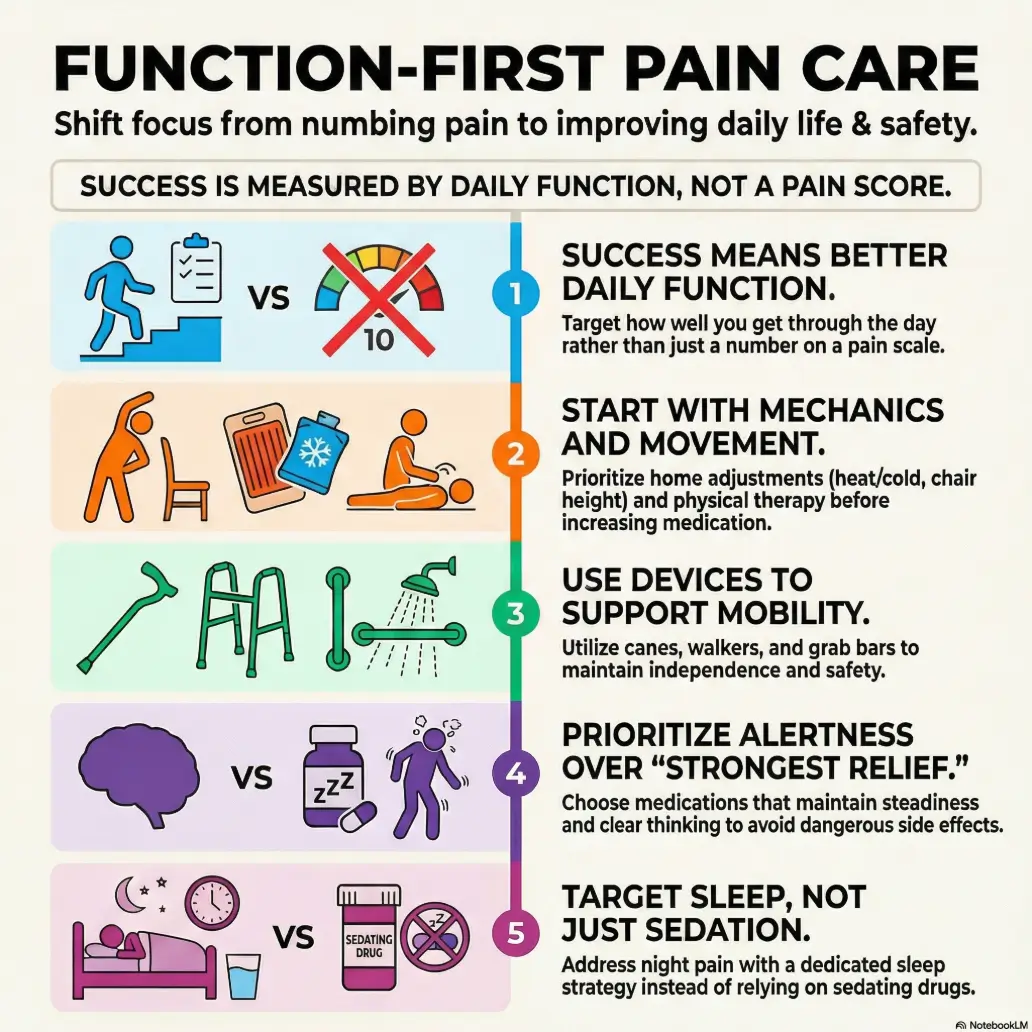
Start With Function, Not Just Pain Scores
The first question is not “How bad is it?”
We ask older adults to rate pain on a number scale because numbers are tidy and clinics run on clocks. But the better opening question is often: What has pain started stealing? Walking across the room? Getting up from a chair? Reaching a bra clasp? Carrying groceries? Turning over in bed without a small opera of groans?
Track what pain is stealing: walking, stairs, sleep, bathing, or confidence
Pain that blocks one essential daily task may matter more than pain that scores high but leaves life mostly workable. A knee that lets you sleep but not step down stairs is not “fine.” A shoulder that hurts only at night can still wreck the next day by wrecking the night before it. If nighttime shoulder pain is the main thief, practical sleep setup questions like whether a recliner or bed setup protects the shoulder better can become more useful than simply asking for stronger relief.
Relief that steals balance is not always relief
This is where the plot thickens. A treatment can improve a pain score and still worsen the day. If walking becomes uncertain, thinking becomes hazy, or the morning feels chemically overcast, the total burden may rise, not fall.
Let’s be honest: fewer pain points can still mean a worse day
I once used a chair cushion that genuinely reduced hip pain and somehow made every stand-up feel like exiting a beanbag trap. The body loves these little ironies. Medical treatment can behave the same way. Comfort is not the only metric that counts. The same logic shows up in spine pain too, where details like seat cushion versus lumbar roll support can change whether sitting feels restorative or treacherous.
The goal is steadier living, not just a smaller number
NIAMS describes treatment goals for osteoarthritis in terms that are beautifully practical: reduce pain, improve joint function, and maintain quality of life. That is the right compass for older adults, especially when sedation is part of the risk picture.
- Track one walking task, one sleep task, and one self-care task.
- Notice whether treatment helps the task, not just the feeling.
- Write down when relief comes with wobbliness or brain fog.
Apply in 60 seconds: Pick the one daily activity you most want back and bring that goal to the visit.
| Signal you see | Most likely priority | Neutral next move |
|---|---|---|
| Pain score improved, but walking is shakier | Safety and medication review | Report sedation, dizziness, and falls risk promptly |
| Pain unchanged, but stiffness eases after movement | Movement strategy and pacing | Ask for PT, home exercise, or a structured walking plan |
| Night pain mainly ruins sleep | Sleep mechanics and evening routine | Review pillows, timing, position, and bedtime triggers |
Neutral next step: Choose the row that sounds most like real life and use that language at the appointment.
The Sedation Trap: Why “Stronger” Can Backfire in Older Adults
Some medicines quiet pain by quieting the person
This is the sentence many families arrive at too late. The medication may technically help pain, but the way it helps can be crude. Instead of improving comfort while preserving function, it lowers the volume on the whole human instrument. That is a high price in later life, where a little extra dizziness can become a cracked wrist or a hospital stay.
Drowsiness, falls, and fog can become the real problem
CDC materials for clinicians advise added caution for patients 65 and older when opioids are prescribed and specifically call out the need for fall-risk assessment and monitoring for cognitive impairment. The CDC also warns clinicians to use special caution with opioid and benzodiazepine combinations, a pairing that can push risk in the wrong direction fast.
The American Geriatrics Society’s public fall-prevention guidance is equally plainspoken: medications that can increase fall risk include muscle relaxants, narcotic pain medications, sedatives and sleeping pills, and even some over-the-counter antihistamines. In other words, the danger is often not one dramatic prescription alone. It is the stack.
The hidden tradeoff: comfort at noon, instability by evening
Many readers know this pattern in their bones. A person takes something for pain, feels looser for a few hours, then fades by late afternoon into unsteadiness, constipation, or a kind of woolly thinking. The treatment story sounds better than the lived story. This is not moral failure or low pain tolerance. It is pharmacology meeting aging physiology at an awkward angle.
Here’s what no one tells you: “sleepy” is sometimes the side effect patients mention last
Because “sleepy” sounds harmless. It is not. In older adults, it can translate into slower reactions on stairs, worse transfers in and out of bed, clumsier bathroom trips at night, and less confidence walking outdoors. A medication can shrink the map of life without anyone quite naming it that way.
Pain control that shrinks independence is a costly bargain
The right question is not whether a medicine is “strong.” It is whether it lets the person remain usefully awake, stable, and able to participate in their own life. Strong is not always wise. Sometimes it is just louder.
Show me the nerdy details
Why older adults react differently to sedating medication has less to do with weakness and more to do with physiology. Aging can change drug metabolism, kidney clearance, body composition, sensitivity to centrally acting medicines, and reserve capacity after a poor night’s sleep or mild dehydration. That is why the same dose that felt tolerable at 52 can feel like walking through soup at 78.

Before Pills: The Low-Drama Strategies That Often Help More Than Expected
Start with movement that feels doable, not heroic
When pain is orthopedic and longish rather than explosive, a great deal of help comes from mechanical common sense. NIAMS notes that osteoarthritis treatment usually begins with exercise, including range-of-motion work, strengthening, balance, and low-impact activity like walking, swimming, cycling, tai chi, or water exercise. That is not because exercise is trendy. It is because joints tend to prefer motion with intelligence over stillness with dread.
The key is dose and dignity. Start smaller than your ego wants. Five minutes can be real exercise if pain has been running the household. The goal is to create a body that trusts movement again, not to audition for an inspirational montage. For readers sorting out structured rehab costs before they even begin, understanding how PT copay versus coinsurance changes the real price of physical therapy can remove a surprisingly large barrier to starting.
Bracing, shoe changes, walkers, canes, and supports are pain tools too
Supports are not consolation prizes. They are part of treatment. NIAMS specifically notes that braces or orthotics may help stabilize a joint, and that assistive devices such as a cane or walker can improve safety, stability, and pain. In plain English: the thing that makes movement less risky often makes it less painful too. Many families also wonder whether orthopedic braces and supports are HSA-eligible, especially when the support device becomes part of daily life rather than a short-lived experiment.
I have seen people resist a cane for six months and then, after one week of using it correctly, talk as if they had discovered indoor plumbing. Pride can be expensive. Stability is often a bargain.
Heat, cold, pacing, and joint-friendly home setup still matter
Heat can ease stiffness. Cold can calm a flared area. Chair height matters more than many medication discussions. So does the depth of the sofa that swallows a person whole and then demands a small engineering project to stand up again. If getting out of the living room chair costs a person their courage three times a day, the chair is now part of the pain problem.
Why tiny mechanical fixes can outperform another prescription
Because pain is not always just pain. It is leverage, pressure, timing, surface height, footwear, muscle fatigue, balance confidence, and sleep disruption dressed as one complaint. A small shoe change, a grab bar, a firmer seat cushion, or a better walker height can do what an extra pill only threatens to do. Even in desk-bound lives, seemingly small ergonomic changes such as choosing between an ergonomic chair and a standing desk can reshape how much pain accumulates across an ordinary day.
- A list of the top 3 activities pain interrupts most often
- The time of day pain is worst and the time of day grogginess is worst
- Current footwear, brace, cane, walker, or home setup issues
- Any recent falls, near falls, or “wall surfing” episodes
Neutral next step: Bring this list to a primary care, orthopedic, PT, or pharmacist visit.
Smarter Medication Conversations When Sedation Is the Concern
Ask which options protect alertness and balance
That sentence alone can improve a medical visit. Not “What is the strongest thing you can give me?” but “Which options are least likely to make me groggy or unsteady?” It changes the frame from rescue fantasy to risk-aware problem solving.
CDC guidance on nonopioid pain therapy notes that several nonopioid options exist, including topical and oral NSAIDs, acetaminophen, certain antidepressants used for pain, anticonvulsants, and topical capsaicin or lidocaine. But it also stresses that nonopioid medications carry real risks, particularly in older adults and those with kidney, cardiovascular, liver, or gastrointestinal concerns. So “nonopioid” is not a synonym for “harmless.” It is simply a category that still needs judgment. In back-pain-heavy households, that same caution shows up in questions about NSAID safety for chronic back pain, especially when older adults are already juggling other conditions.
Review every medicine, not just the pain medicine
This matters because the pain medicine may not be the whole story. The bedtime antihistamine, the anti-anxiety tablet, the leftover muscle relaxer from a previous injury, and the “just occasionally” sleep aid can all contribute to the daytime fog that gets blamed on age itself. Sometimes the real culprit is not pain severity. It is chemical crowding.
Watch for stacking: sleep meds, anxiety meds, muscle relaxers, and opioids
Stacking is where safety quietly unravels. The AGS fall-risk guidance lists multiple medication categories that can increase fall risk, including muscle relaxants, narcotic pain medications, sedatives, and sleeping pills. This is why a med review should include everything in the cabinet, including over-the-counter products and supplements.
Bring one simple question to the visit: “What is most likely to make me groggy or fall?”
That question cuts through performance. It invites the clinician to prioritize the outcome older adults often care about most: remaining present and upright. It also gives caregivers a clean way to participate without hijacking the encounter.
- Ask about alertness, balance, constipation, and next-day effects.
- Bring all meds, including OTC sleep and allergy products.
- Tell the clinician about near falls, not just pain.
Apply in 60 seconds: Write the sentence “Which option is least likely to make me groggy or fall?” at the top of your appointment note.
Common Mistakes
Mistake #1: Chasing nighttime relief with medicines that linger into the morning
Night pain is miserable, and sleep deprivation makes every body part more dramatic. But in older adults, a medicine that seems to help at 11 p.m. may still be rearranging balance and reaction time at 7 a.m. The morning bathroom trip becomes the real test, and it is not a forgiving one.
Mistake #2: Treating stiffness like a medication failure instead of a movement problem
Morning stiffness, post-sitting stiffness, and “first ten steps are the worst” patterns often respond better to mobility work, warm-up routines, heat, or timing changes than to simply escalating sedation. Not every uncomfortable sensation is a sign that medication intensity must increase.
Mistake #3: Adding “just one more” sedating medicine without a full med review
This is how accidental chemistry sets begin. A sleep aid here, a pain reliever there, an old prescription revisiting the scene like a poorly behaved ex. Older adults are especially vulnerable to the cumulative effect.
Mistake #4: Ignoring footwear, chair height, or stair pain while focusing only on pills
Orthopedic pain is mechanical more often than pride likes to admit. The wrong shoes, low chair, poor walker fit, or unsupported knee on stairs can keep the pain cycle alive while medication gets blamed for not being magical enough.
| Approach | Common upside | Common hidden cost |
|---|---|---|
| More sedating medication | Short-term comfort or sleepiness | Morning fog, falls risk, constipation, less confidence |
| Movement + support devices | Better function and stability over time | Requires patience, setup, and repetition |
| Targeted medication review | May reduce stacking and side effects | Takes coordination and honest reporting |
Neutral next step: Decide which hidden cost has been hurting daily life the most.
Don’t Do This: Four Habits That Quietly Worsen Orthopedic Pain
Don’t stay completely still for fear of “wearing out” the joint
This idea is stubborn because it sounds logical. If it hurts, freeze. But bodies often do not reward that strategy. Muscles weaken, confidence drops, transfers get harder, and the first movement after rest feels even more hostile. NIAMS explicitly includes range-of-motion work, strengthening, balance, and low-impact activity as part of common osteoarthritis care for exactly this reason.
Don’t mix old prescriptions, over-the-counter sleep aids, and pain meds casually
Medication archaeology is risky. A tablet from an old injury or an over-the-counter nighttime product can interact with current treatment in ways that do not announce themselves politely. The danger may show up as a stumble, not a dramatic allergic reaction.
Don’t judge a plan too fast if the missing piece is timing, pacing, or PT
Some plans fail not because they are weak, but because they are incomplete. The right medicine taken at the wrong time, or the right home exercise routine performed like a punishment ritual instead of a paced progression, can make a reasonable plan feel useless. Readers trying to avoid giving up on rehab too early may also benefit from a clearer sense of what structured physical therapy is actually supposed to do over time, because impatience loves to masquerade as realism.
Don’t let the treatment plan become more disabling than the pain
This is the central caution of the whole article. If the person is sleeping more, walking worse, thinking slower, fearing stairs more, or withdrawing from normal activity, the treatment burden may now rival the pain burden. That deserves recalibration, not stoicism.
Practical litmus test: if a person says “I’m more comfortable” but is walking less, doing less, and needing more supervision, the plan is not automatically succeeding.
If Sleep Is the Real Complaint, Treat Sleep as Its Own Problem
Night pain is not always a reason for a more sedating drug
Many people say “my pain is worse at night,” but the lived injury is often fragmented sleep, fear of turning over, poor mattress support, or the 3 a.m. ache that arrives after one position has overstayed its welcome. More sedation is not the only lever.
Bed setup, timing, pillows, and evening movement may change the whole night
A pillow between the knees, under the knees, behind the back, or supporting an arm can be a minor architectural miracle. So can moving a medication earlier, using heat before bed, or doing a brief mobility routine instead of dropping into bed like a felled tree and hoping the joint will negotiate. Readers navigating nerve-heavy nighttime pain often find that details like how to sleep with sciatica or whether a knee pillow or body pillow gives better support matter more than they first expected.
The midnight pattern matters: falling asleep, staying asleep, or waking stiff?
These are different problems. Trouble falling asleep may involve anticipation, pain spikes, or overstimulation. Waking repeatedly may suggest positioning or bladder trips or poor sleep continuity. Waking very stiff may respond better to heat and morning mobility than to more nighttime sedation.
Let’s be honest: many people say “pain” when the real heartbreak is exhaustion
That matters because it changes treatment. If the person mostly wants to stop waking four times a night, solving mechanics and routines may do more than turning up medication volume.
Fixing sleep mechanics can reduce the urge for risky shortcuts
I learned this the humiliating way with a shoulder flare that I kept blaming on “bad nights” until I realized the real villain was my pillow arrangement, which had all the ergonomic intelligence of a bag of turnips. Sometimes treatment begins with admitting the bedding is part of the cast.
- Track whether the problem is falling asleep, staying asleep, or waking stiff.
- Adjust pillows, bed position, and bedtime routine before assuming medication failure.
- Report next-day grogginess as part of the sleep problem.
Apply in 60 seconds: Write one sentence about the exact time and pattern of nighttime waking.
Use three numbers from the last 7 days:
- Nights with sleep interrupted by pain: ____
- Mornings with dizziness or grogginess: ____
- Days you could do your key activity safely: ____
If groggy mornings are rising faster than functional days, the plan may be relieving symptoms while worsening safety.
Neutral next step: Bring the three numbers to the next medication review.
The Caregiver Lens: How Adult Children Can Help Without Taking Over
Notice patterns the patient may normalize
Older adults are often brave in ways that are beautiful and occasionally inconvenient. They may describe a near fall as “a little silly moment” or daytime sedation as “just tired.” A caregiver can notice the pattern beneath the politeness.
Bring a medication list, a fall history, and three functional examples
This is where caregivers can be enormously useful. Not by speaking for the patient at every turn, but by bringing the missing ledger: what changed after each medication, whether there were near falls, which task became harder, which time of day is worst, and what the patient stopped doing without making an announcement about it.
Ask what changed after each new prescription
Not just “Did pain improve?” Ask whether walking changed, bathroom urgency at night changed, constipation worsened, thinking slowed, appetite changed, or confidence dipped. The side effect that matters most may be the one nobody thought counted as data.
Support independence, not surveillance
People do not want to feel studied in their own homes. A good caregiver helps restore agency. That might mean helping organize the med list, arranging PT transport, labeling a pill organizer more clearly, or making the home slightly less treacherous without turning it into a padded laboratory.
I once watched an adult daughter ask her father, not “Are you taking your meds?” but “When do you feel most steady?” It was such a better question. Less policing. More partnership.
What a Good Plan Usually Looks Like in Real Life
One primary pain target, not ten vague complaints
Good plans are specific. “Everything hurts” may be emotionally true and clinically unhelpful. A workable plan usually names the one place and one pattern causing the most damage right now: knee pain on stairs, shoulder pain when dressing, back pain after ten minutes standing, hip pain that wakes the person at 2 a.m.
A function goal tied to daily life
“Walk to the mailbox without stopping.” “Get in and out of the car with less fear.” “Sleep until 5 a.m. instead of 2 a.m.” “Shower without needing a recovery period.” These are real goals. They let the treatment plan answer to life rather than to abstraction. In some cases, ordinary tasks reveal the treatment target more clearly than any scan does, which is why comparisons like hip pain versus spine pain can matter when the body keeps telling a confusing story.
Fewer moving parts, clearer check-ins
The best plan is rarely the most baroque. It is usually one or two physical strategies, one or two medication decisions, and one clear follow-up question. Complexity flatters nobody at 3 p.m. when the pillbox, heating pad, and walker are all auditioning for attention.
A plan for what to stop if alertness gets worse
This is crucial. The family should know what symptoms count as “call us,” what should be held or reviewed, and what is considered unacceptable drift in alertness or balance. If a plan has no brakes, it is not finished.
Progress should feel steadier, not merely stronger
The right plan often feels slightly less dramatic than expected. Less rescue, more rhythm. Less “wow, I was knocked out,” more “I managed the day a little better.” For older adults, that quieter success is usually the better one.
Home mechanics
Heat/cold, chair height, footwear, safer transfers, pacing
Guided movement
Walking plan, mobility, strength, balance, PT referral
Device support
Brace, orthotic, cane, walker, grab bars, bed positioning
Medication review
Reduce stacking, prefer lower-risk options, monitor alertness
Re-evaluate diagnosis
New imaging, specialist input, injection discussion, red flag review
How to use it: Move upward only when the lower tier is clearly insufficient, unsafe, or not feasible.
Show me the nerdy details
Function-first plans are easier to troubleshoot because they separate mechanical pain drivers from medication burden. If the person improves after support devices and targeted exercise, the issue may be more load-distribution and movement-related than “under-treated pain.” If the person only improves when sedated and becomes less functional, the treatment may be masking symptoms while worsening global performance.
Short Story: The mailbox test
For one family I know, the breakthrough did not come from a dramatic new prescription. It came from a question the grandson asked while standing at the front door: “Grandma, what’s the one thing you miss doing without thinking about it?” She did not say “having less pain.” She said, “Walking to the mailbox without planning it like an expedition.” That changed everything.
Instead of chasing a perfect pain score, the next appointment focused on one route, one distance, one time of day, and one fear: feeling wobbly on the return walk. The plan became almost embarrassingly ordinary. Better shoes. A properly fitted cane instead of the decorative one she hated. Heat before the walk, not after.
A medication review that looked beyond the pain tablet to the nighttime sleep aid she had considered too innocent to mention. Two weeks later, the pain was not gone. But the mailbox was back. And with it came the thing the family had actually been mourning: her sense that the day still belonged to her. For patients caught in the long middle, that is not far from the logic behind pain management for seniors waiting on joint treatment, where the goal is not theatrical relief but arriving less depleted.
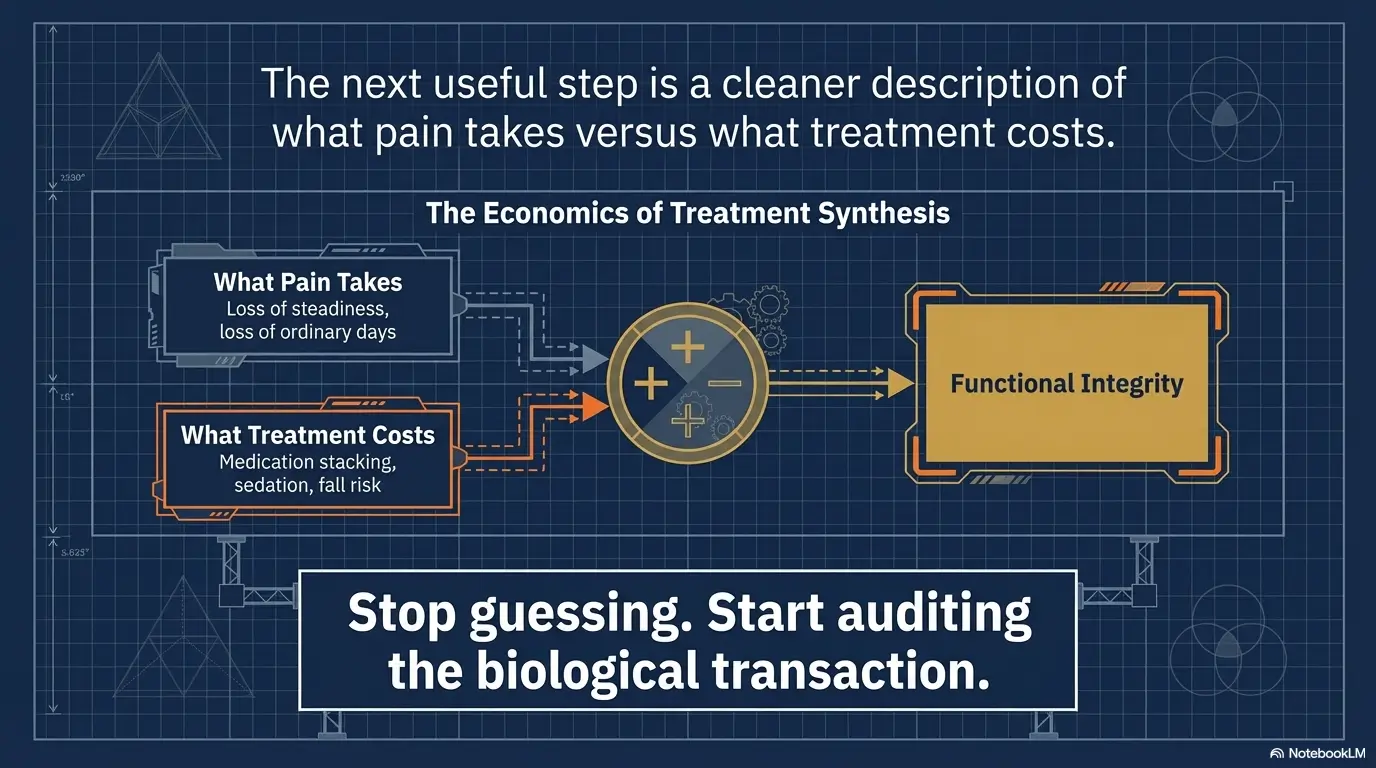
Next Step
Make a two-column note before the next appointment
Column one: “What pain stops me from doing”
Column two: “What makes me sleepy, dizzy, or unsteady”
This is the highest-yield move most readers can make in under 15 minutes. Write the note by hand if that helps. Keep it blunt. Not elegant. Not comprehensive. Just useful.
In the first column, list the real stolen things: climbing stairs, carrying laundry, sleeping through the night, getting off the toilet safely, cooking, dressing, walking the dog, driving comfortably, stepping into the shower. In the second column, list every effect that feels like the treatment taxing the body: morning grogginess, constipation, dry mouth, fuzzy thinking, a strange floaty feeling, needing furniture for balance, daytime napping that is new, or a fall that “probably wasn’t because of the medicine” but very much may have been.
Bring that note and ask for a safest function-first plan. Not the strongest. Not the most aggressive. The safest plan that still moves life forward.
- Write down one function goal.
- Write down one safety concern.
- Bring both to the next appointment.
Apply in 60 seconds: Start the note with the sentence “I want pain relief without feeling foggy or unsteady.”
The curiosity loop from the beginning closes here: the better question was never “How do I get stronger pain medicine?” It was “How do I get through an ordinary day with less pain and more of myself still intact?” For older adults, that distinction is not semantic. It is the whole architecture of safe pain care.
If you only do one thing today, make the two-column note and schedule the review. That small page can turn a vague visit into a practical one, and sometimes that is how steadier living begins: not with a miracle, but with a better question asked clearly.
FAQ
What is the safest orthopedic pain management approach for older adults who want to stay alert?
Usually a function-first plan works best: start with the specific activity pain is disrupting, add movement-based care, use supports such as braces or canes when appropriate, improve sleep mechanics, and review medications with alertness and fall risk in mind. The safest plan is the one that improves daily life without making walking, thinking, or mornings worse.
Which pain medicines are more likely to make seniors sleepy or unsteady?
Medication effects vary, but sedating or centrally acting drugs often deserve closer scrutiny in older adults. Public guidance from the American Geriatrics Society flags narcotic pain medications, muscle relaxants, sedatives, sleeping pills, and some antihistamines as medications that can raise fall risk. The issue is often cumulative when more than one is used.
Can older adults manage arthritis pain without opioids?
Many can reduce pain meaningfully through exercise, physical therapy, heat or cold, braces, assistive devices, pacing, and carefully chosen nonopioid options when appropriate. NIAMS describes exercise, weight management, braces or orthotics, support devices, and topical or oral treatments as common parts of osteoarthritis care. That does not mean every person can avoid opioids in every situation, but it does mean opioids are not the only serious option.
What should caregivers ask a doctor when an older parent seems groggy on pain medication?
Ask, “Which medication or combination is most likely causing the grogginess or raising fall risk?” Then ask what should be reviewed first, whether any bedtime or over-the-counter products may be contributing, and what symptoms should trigger a prompt call back. Bringing a full medication list and examples of real-life changes is often more useful than saying only, “They seem off.”
Are muscle relaxers a bad idea for seniors with back pain?
The answer depends on the person and the exact medication, but as a category they deserve caution in older adults because sedation, dizziness, and fall risk matter more in later life. They should not be treated as casual add-ons, especially when sleep medications, opioids, antihistamines, or alcohol are also in the picture.
How do you balance sleep, pain relief, and fall prevention in older adults?
By separating the problems instead of lumping them together. Figure out whether the main problem is pain intensity, stiffness, sleep positioning, repeated waking, or morning instability. Then build the plan around the dominant pattern. A “good night” that causes a dangerous morning is not truly a good night.
What non-drug treatments help orthopedic pain in seniors most often?
Common high-value options include targeted exercise, physical therapy, heat or cold, braces or orthotics, shoe changes, walkers or canes, safer furniture setup, grab bars, and pacing strategies. These may look unglamorous, but they often help because orthopedic pain is partly mechanical, not only chemical.
When should persistent joint pain be re-evaluated instead of just medicated?
If the pain is worsening, the joint is locking or giving out, swelling is new or significant, function is sliding despite treatment, or the treatment burden is becoming too high, re-evaluation is reasonable. NIAMS notes that imaging and further evaluation may be used when the clinical picture calls for it, especially if the joint is behaving differently rather than simply hurting in the same old way.
Last reviewed: 2026-03.
