
Physical Therapy for Chronic Low Back Pain: 10 Brutally Honest Recovery Secrets
Why Your Back Still Feels Like a Rusty Hinge (Even After Doing Everything “Right”)
Let’s be real for a second: if you’ve followed the rules, done the stretches, gone to physical therapy, bought the fancy pillow, foam rolled yourself half to death—and your back still feels stiff every morning like you’re 97 years old… you are not crazy. The truth? The whole system is just wildly confusing.
Chronic low back pain is one of those weirdly frustrating things where you can throw time, money, and good intentions at it for months and still end up limping to brush your teeth. And while your physical therapist might be kind and encouraging, there’s often a quieter conversation that happens behind closed doors (or whispered over the foam roller): here’s what PT can really do for chronic back pain… and what it just can’t.
This is the brutally honest guide to making sense of the madness—no fluff, no miracle cures, just straight-up clarity. We’ll walk you through 10 recovery “secrets” that combine science-backed guidelines, what actually happens in clinics, and the reality of needing your back to cooperate now, not six months from now.
You’ll learn:
- Why exercise is still the #1 recommendation (even when it feels like it’s doing nothing),
- Why “small” improvements can be a huge deal in your day-to-day life,
- How to do a quick, 60-second check later in this article to see if your plan is worth the time and cost—or if you’re just spinning your wheels.
Give us 30 minutes, and you’ll leave with a clearer plan for the next 6–12 weeks. No more endless Googling at 2 a.m., no more trying five apps and six stretches only to end up feeling worse. Just some practical hope and a better way forward.
Important reality check before we begin:
This article is meant to inform, not diagnose. If your pain is new, suddenly worse, or comes with scary stuff like numbness, fever, loss of bladder or bowel control, or a history of major trauma or cancer—please see a doctor or go to urgent care before starting any exercises. Your spine deserves expert eyes in those cases.
Table of Contents

Why physical therapy for chronic low back pain feels so hard
Chronic low back pain—pain lasting longer than three months—is one of the most studied and still-most-frustrating conditions on earth. This is especially common in the life stage many readers recognize as chronic low back pain after 40. Global and national guidelines now agree on a core message: education, exercise, and staying active are first-line treatments, with medication and procedures as backup, not the opening move. That’s good science… but not always comforting when you’re exhausted, scared, and staring at another intake form.
Here’s the uncomfortable truth: for many people, physical therapy helps “enough,” not “perfectly.” Research on exercise for chronic low back pain shows small-to-moderate improvements in pain and function compared with doing nothing, usual care, or placebo. Those are not miracle numbers, but in real life they can mean “I can sit through dinner” or “I can walk my dog again,” which is the level that actually matters to you.
Another frustration: the timeline. Guidelines and trials often use programs lasting at least 8–16 weeks, with exercise done several times per week. That’s very different from the silent expectation many of us carry in: “Three visits and I’m fixed.”
Think of physical therapy less like taking an antibiotic and more like learning an instrument. You don’t “fail piano” if you still sound shaky after four lessons—you’re exactly where the process says you’ll be.
To get honest about whether PT fits your current life and health, start with a quick eligibility scan.
Money Block #1 — 60-second eligibility checklist
Yes/No questions to answer before you double down on PT:
- Has your back pain lasted > 3 months and is it mostly in the low back (not spreading below the knee with severe weakness)?
- Has a doctor or qualified clinician ruled out red flags like recent major trauma, cancer, infection, or progressive nerve loss?
- Can you safely walk around your home and do light daily tasks, even if it hurts?
- Do you have at least 15 minutes, three times per week, that you could realistically reserve for exercises?
- Is there a clinic, telehealth service, or home-visit option you can actually get to without wrecking your schedule?
If you answered “no” to the first two: you need medical clearance before starting or continuing PT—think doctor, urgent care, or emergency care depending on how severe things are.
If you answered “no” to the time or access questions: PT can still help, but your main job is to debug your logistics first—transport, work hours, childcare, or telehealth options.
Neutral next step: Save this checklist and review it with your doctor or physical therapist at your next appointment.
- Guidelines prioritize education, exercise, and staying active.
- Improvements are often modest on paper but meaningful in real life.
- Eligibility is about safety and logistics, not willpower.
Apply in 60 seconds: Answer the five checklist questions above and write down one barrier you need to fix before you commit to a new plan.
Recovery Secret #1: Pain relief is not the same as recovery
Most people start PT hoping for one thing: “Make it stop hurting.” The twist is that pain often improves before your back is truly resilient—and sometimes, function improves before pain fully quiets down. If you only track the pain, you’ll call PT a failure just as it’s starting to work.
Recent reviews suggest that for adults with chronic low back pain, exercise programs done 15–30 minutes, three times per week, for at least 16 weeks are among the more effective options, especially when they combine strength, flexibility, and control. That sounds simple, but it’s a big mindset shift: your “treatment” is not just the 30 minutes on the table; it’s the hundreds of minutes you accumulate outside the clinic.
Here’s a more honest way to score your recovery:
- Pain score: “How bad is it from 0–10 today?” (useful, but jumpy)
- Function score: “How long can I sit, stand, walk, or concentrate before my back dominates the room?”
- Confidence score: “How scared am I to move, from 0–10?”
One office worker I’ll call Jae started PT barely able to sit for 20 minutes. Eight weeks later, his pain score had improved only a little—but he could sit 90 minutes, walk 30 minutes, and go a whole morning without obsessing over his back. On spreadsheets, that’s “small effect.” In real life, that’s a job saved.
Track at least one functional metric (like “minutes I can walk” or “minutes I can sit”) every week. When pain plays tricks, those numbers will tell you whether you’re quietly getting your life back.
- Recovery is a three-part score: pain, function, and confidence.
- Exercise programs need weeks, not days, to shift those scores.
- A small change in function can mean a big change in your actual life.
Apply in 60 seconds: Write down one activity that matters to you (for example, “sit through a 45-minute meeting”) and note how long you can handle it today—this becomes your new weekly scoreboard.
Recovery Secret #2: Your therapist is a coach, not a mechanic
A lot of us secretly hope a physical therapist will “realign” something and send us home fixed. That’s understandable—manual therapy can feel amazing. But the most up-to-date guidelines consistently nudge us toward a different picture: hands-on treatment is a valuable support act; active exercise and education are the headliners.
Think of your therapist as your back coach. Their job is to:
- Help you understand what’s happening (and what’s not happening, like “your spine is not crumbling”).
- Find movements your body tolerates now and gradually expand them.
- Teach you what to do on flare-up days vs. good days.
- Coordinate with your doctor about medication, imaging, or referrals when needed.
My favorite kind of clinic conversation sounds like this:
“I sit eight hours a day, commute an hour, and have kids’ homework at night. I can realistically do 10 minutes in the morning and 10 at night. What should those 20 minutes look like?”
That’s partnership. What doesn’t work is silently hoping for miracles while saying “everything’s fine” during the session and then doing zero exercises at home because they weren’t practical in the first place.
Spend one visit being brutally honest about your schedule, stress, and fears. It’s not complaining; it’s giving your therapist the actual puzzle they need to solve.
- Manual techniques can help, but they can’t replace your own movement.
- Honesty about time and stress lets your therapist design a realistic plan.
- Good PT feels collaborative, not mysterious.
Apply in 60 seconds: Before your next session, jot down your real weekly schedule and bring it; ask, “What’s the minimum effective home plan that fits this?”
Recovery Secret #3: Consistency beats intensity (and saves money)
In back pain rehab, small, repeatable effort nearly always beats heroic, occasional effort. Many exercise-based programs that show benefit use roughly two to three sessions per week plus home practice, stretched over several months.
The problem is that real life works on budgets: time budget, energy budget, money budget. If you go all-in for three weeks and then disappear because you’re burnt out or broke, you lose most of the momentum you paid for.
Out-of-pocket cost to complete an 8-week physical therapy plan for chronic low back pain, 2025 (US)
Let’s look at a simplified scenario, assuming you’ve already cleared PT with your doctor.
Money Block #2 — Decision card: 1x/week vs 2x/week
Scenario: Your copay is about $40 per PT visit, and your schedule is tight.
Option A — 1x/week for 8 weeks
- Visits: 8
- Estimated out-of-pocket: $320
- Time in clinic: about 6–7 hours total
- Requires strong home-exercise follow-through
Best for: Busy schedules, strong self-discipline, or if you already know your exercises.
Option B — 2x/week for 8 weeks
- Visits: 16
- Estimated out-of-pocket: $640
- Time in clinic: about 13–14 hours total
- More coaching, faster feedback on flare-ups and form.
Best for: New to exercise, high fear of movement, or complex pain patterns.
Neutral next step: Screenshot this card and ask your PT, “Given my history and budget, which option gives me the best chance of progress?”
Typical physical therapy price ranges for chronic low back pain, 2024–2025 (US)
Money Block #3 — Fee / rate table
| Setting | Typical session price (no insurance) | Typical copay / coinsurance (with insurance) | Notes (2024–2025) |
|---|---|---|---|
| Outpatient PT clinic | $75–$350 per visit | $20–$50 average copay | Ranges widen with region and clinic type. |
| Specialized spine clinic | $130–$150+ per visit | Often standard copay, higher if out-of-network. | More complex cases, more advanced equipment. |
| Home or in-home PT | $100–$150+ per visit | May require higher coinsurance. | Travel time and convenience drive cost. |
| Digital / telehealth PT program | Flat monthly or per-visit fees | Copay similar to in-clinic; some programs cash-pay only. | Often cheaper over a full episode of care, especially for remote patients. |
These ranges come from recent PT and rehab clinic reports in 2024–2025 and large clinic networks in the US; your exact fee depends on region, insurance, and clinic type.
Neutral next step: Save this table and confirm the current fee and visit limit on your clinic’s price sheet or your insurer’s official site.
- Decide how many sessions you can afford in time and money before you start.
- Match your visit frequency to your confidence and complexity.
- Use rough cost estimates to avoid mid-plan financial surprises.
Apply in 60 seconds: Multiply your expected copay by 8–16 visits and ask yourself, “Can I sustain this?” If not, discuss a lower-frequency plan with your PT.
Recovery Secret #4: The “boring” exercises rewire your back
Most chronic low back pain programs don’t look dramatic. There’s no cinematic barbell, no wild stretches—just tiny movements: drawing your belly in, gently tilting your pelvis, sliding your heel on the mat. It’s easy to think, “This is too basic to matter.”
Yet clinical guidelines for physical therapists specifically recommend trunk muscle activation and movement-control exercises for many people with chronic low back pain. These movements retrain how your spine, hips, and core coordinate, which affects how load travels through your body when you stand, bend, or lift.
A typical “boring but powerful” sequence might include:
- Gentle knee-to-chest and hamstring stretches.
- Pelvic tilts and bridges on the floor.
- Bird-dog (opposite arm and leg lift) on hands and knees.
- Side-lying leg lifts or clamshells for hip strength.
One parent I’ll call Dani did these while watching dramas at night. For the first month, she felt like nothing was happening. In month two, she realized she could unload groceries from the car without that familiar lightning bolt of fear. The exercises didn’t look heroic, but they changed her automatic movements, which is where the real win lives.
Show me the nerdy details
Movement-control exercises aim to dial down unnecessary muscle guarding and improve timing between your deep stabilizers (like the multifidus and transverse abdominis) and your larger movers (like the glutes). Over time, this can reduce the constant “bracing” pattern that many chronic pain sufferers develop, which may lower perceived stiffness and improve efficiency when walking, sitting, or lifting.
- Movement-control drills are a core part of modern chronic back rehab.
- They feel subtle—until you notice daily tasks getting smoother.
- Entertainment (podcasts, dramas, music) can make the repetition bearable.
Apply in 60 seconds: Pick one “boring” exercise you’ve already been given and commit to doing it during the first 5 minutes of your favorite show tonight.
Recovery Secret #5: Walking is medicine when you dose it right
If exercise therapy is the backbone of chronic low back pain care, walking is often the first and most underrated prescription. A 2025 study following more than 11,000 adults found that people who walked between about 101 and 124 minutes per day had a roughly 23% lower risk of developing chronic low back pain compared with those who walked less.
That doesn’t mean you need to hit 100 minutes tomorrow. For many people with established pain, even 5–10 minutes is a win. The trick is to treat walking like medication: adjust the dose, frequency, and progression instead of swinging between “marathon” and “couch.”
- Start where you are: If 7 minutes triggers pain, start at 4 or 5.
- Use intervals: For example, 5 minutes walk, 2 minutes rest, repeat.
- Increase slowly: Add 1–2 minutes every week or every other week if it feels manageable.
Short Story: Mina, a 42-year-old designer, lived between her office chair and ride-share seats. Her PT asked her to aim for three 7-minute walks spread through the day. Week 1 was a mess of calendar reminders and forgotten loops around the block. By week 4, those walks became her unofficial “reset buttons” between meetings. She noticed that on days she got all three, her evening pain stayed at a 3–4 out of 10 instead of spiking to 7. Nothing else changed—same deadlines, same chair—but her back no longer felt like a ticking time bomb at 5 p.m.
Walking also plays nicely with your wallet: it’s free, scales to your fitness, and works even when you’re on a PT waitlist.
- You don’t have to hit 10,000 steps; you just need a consistent minimum.
- Intervals and tiny weekly increases prevent flare-triggering leaps.
- Walking also boosts mood and sleep, which indirectly calms pain.
Apply in 60 seconds: Decide on a “bare-minimum walk” time for today—maybe 5–10 minutes—and schedule it right after a routine event like lunch or your last meeting.
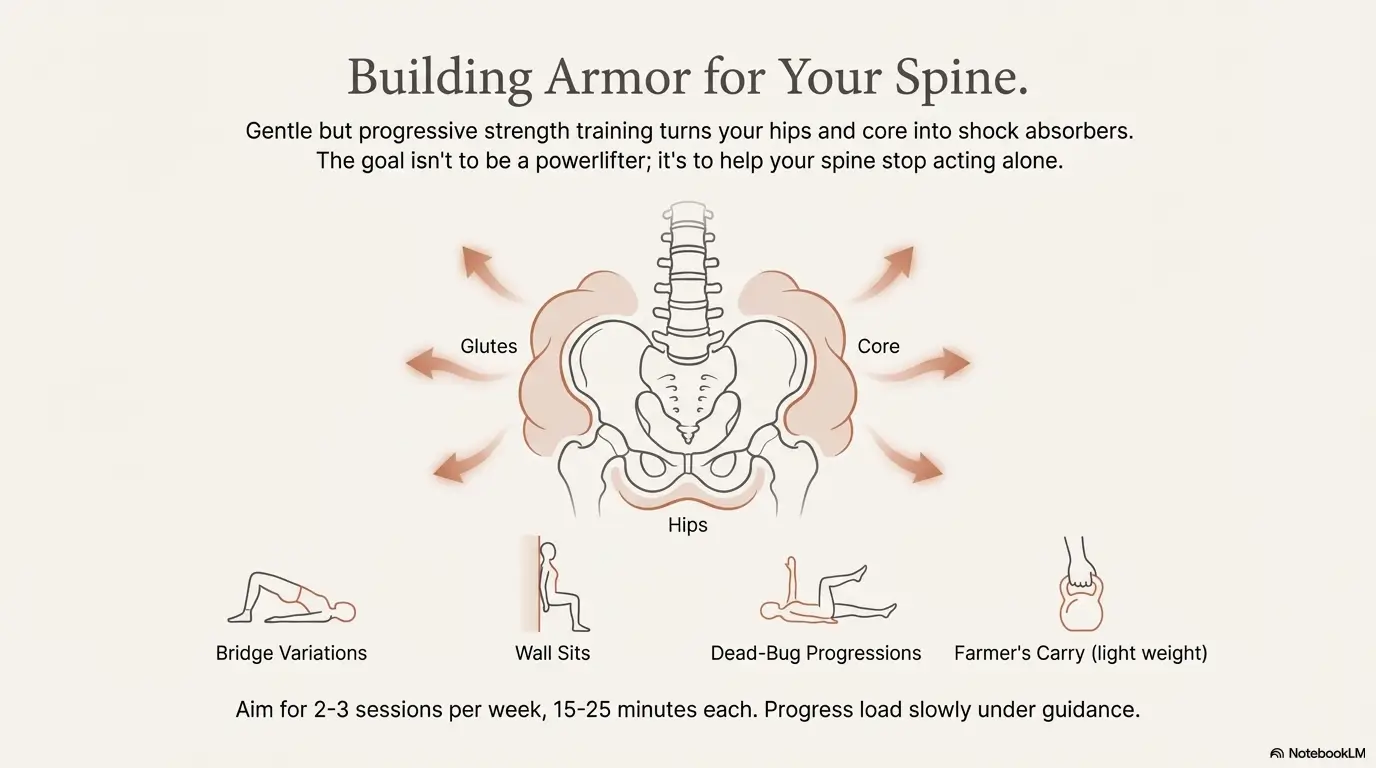
Recovery Secret #6: Strong hips and core protect your spine
Once basic tolerance and walking are in place, strength and load become your long-term armor. Updated low back pain guidelines emphasize resistance training, Pilates-style work, and targeted hip and core strengthening as part of chronic care, not just elite athlete rehab.
The goal isn’t to turn you into a powerlifter; it’s to help your spine stop acting alone. When the glutes, hips, and core do their share of the work, each lift, twist, and stair climb becomes less of a threat.
Examples of gentle starter strength moves your PT might use include:
- Bridge variations (double-leg, then single-leg) for glutes.
- Wall sits or supported mini-squats for legs and hips.
- Dead-bug and bird-dog progressions for core control.
- Farmer’s carry with light weights for whole-body endurance.
In practice, that might look like 2–3 strength sessions per week, 15–25 minutes each, rotating exercises so no single area gets overwhelmed. You’ll likely stay at low loads at first—think resistance bands or light dumbbells—before cautiously building up under professional guidance.
Show me the nerdy details
Strength work for chronic low back pain often uses a “graded exposure” model. Instead of avoiding all painful movements, your PT helps you perform versions of them at lower load or smaller range—like a partial hip hinge instead of a full forward bend. Over time, your nervous system learns that the pattern is safe, pain sensitivity can decrease, and your muscles become better at absorbing force before it hits passive structures like discs and ligaments.
- Strength work is recommended in modern chronic back guidelines.
- Progress slowly under guidance instead of chasing big weights fast.
- The goal is durability in daily life, not gym bragging rights.
Apply in 60 seconds: Ask your PT, “What is one strengthening move I can safely do twice a week that will help my back over the next month?”
Recovery Secret #7: Your nervous system needs therapy too
Chronic low back pain is rarely just a “hardware” issue. By the time pain has persisted for months, your nervous system often becomes extra sensitive, like a smoke alarm that goes off when you make toast. That doesn’t mean your pain is imaginary; it means the pain system is doing its job a little too enthusiastically.
Several lines of research support pairing movement with pain neuroscience education and cognitive-behavioral strategies—essentially, learning how pain works and how thoughts, stress, and fear interact with it. Programs that combine these elements with motor-control training have shown meaningful improvements in pain and disability for chronic spinal pain.
In real life, this might include:
- Learning why “hurt” doesn’t always mean “harm” once serious causes are ruled out.
- Practicing graded exposure to feared movements—like bending to pick up a laundry basket.
- Using breath work, sleep hygiene, and basic stress management to turn down background nervous-system noise.
- In some cases, working with a psychologist who understands chronic pain.
People often notice that when life stress spikes—deadlines, conflict, poor sleep—their back “mysteriously” flares too. That isn’t weakness; it’s a reminder that your spine is attached to a whole human.
- Pain education plus exercise can outperform either one alone.
- Fear of movement is a modifiable piece of the puzzle, not a life sentence.
- Better sleep and stress patterns make your back rehab easier.
Apply in 60 seconds: Write down one movement you avoid because of fear (for example, “bending to tie my shoes”) and show it to your PT; ask for a safe, smaller-range version you can start practicing.
Recovery Secret #8: Plan for time, insurance, and out-of-pocket costs
You’re not shallow for caring about money. Physical therapy lives in a world of copays, coverage tiers, deductibles, and visit limits. If you ignore those, you risk bailing midway through a promising plan because your bank account taps out first.
In many US plans, outpatient PT sessions might have a $20–$60 copay, often with annual visit caps or prior-authorization rules. Medicare Part B typically covers a percentage of the approved amount after the deductible is met, leaving you with a smaller per-visit cost but still a real out-of-pocket total.
How to check your physical therapy coverage and deductible before your first visit, 2025 (US)
Before you book a full block of appointments, call your insurer or check your online portal and ask three questions:
- “What is my copay or coinsurance for outpatient physical therapy?”
- “How many visits are covered per year, and do I need prior authorization?”
- “How close am I to meeting my deductible and out-of-pocket maximum?”
Money Block #4 — 60-second physical therapy cost estimator
Rough out-of-pocket estimate (US example):
Neutral next step: Use this as a rough sketch, then compare it with the actual numbers from your clinic and insurance plan.
What to gather before you request insurance quotes or prior authorization
Money Block #5 — Quote-prep list
- Your diagnosis (or working diagnosis) from the doctor, if you have one.
- The PT clinic’s full name, address, and phone number.
- Any referral or prescription your doctor wrote for PT.
- Your insurance ID, group number, and plan name.
- A rough idea of how many visits your PT expects for the first 6–8 weeks.
Neutral next step: Keep this list next to your phone or laptop and use it the next time you contact your insurer so you can get accurate coverage information on the first call.
If you live in a country with national health insurance—like South Korea or parts of Europe—the details will look different, but the logic is similar. There may be strict rules about referrals, approved clinics, and how many PT sessions are covered per condition. Many hospital-based clinics will help you translate your doctor’s recommendation into the exact paperwork or online steps you need; don’t hesitate to ask the front desk to spell it all out.
- Know your copay, coverage tier, and visit limits before you commit.
- Use a quick calculator to see the total cost of a full 6–12 week block.
- Prepare key details so insurance calls are short and productive.
Apply in 60 seconds: Grab your insurance card and write down your plan name and member ID so they’re ready for your next coverage call.
Recovery Secret #9: Setbacks are normal data, not personal failure
Almost everyone with chronic low back pain has relapses and flare-ups. You have a good week, then you reach for a suitcase the wrong way, or sleep badly, or sit through a long flight, and suddenly you’re back at square one—or it feels that way.
From a rehab perspective, flare-ups are not a verdict on your worth or effort; they are information. They often highlight one of three gaps:
- A load gap (for example, you suddenly asked your back to handle more weight, time, or repetition than it was prepared for).
- A recovery gap (poor sleep, more stress, less walking or exercise than usual).
- A strategy gap (no clear “flare plan,” so you panic and either do nothing or too much).
One practical approach is to create a personal “flare script” in advance. It might include three parts: your safe movement pattern (like a gentler walking plan), your medication or heat/ice approach as agreed with your doctor, and your rules for when to call your PT or doctor again.
- Most long-term back pain stories include flare-ups.
- A pre-written plan keeps fear from driving your decisions.
- Red-flag changes still deserve urgent medical attention.
Apply in 60 seconds: Write one sentence that starts with “When my back flares, I will…” and fill in a calm, safe plan you can follow.

Recovery Secret #10: Build a back-care plan you can live with for years
The real win with physical therapy for chronic low back pain isn’t just a good six-week block—it’s a sustainable life pattern that keeps your back as calm as reasonably possible while you keep living your actual life.
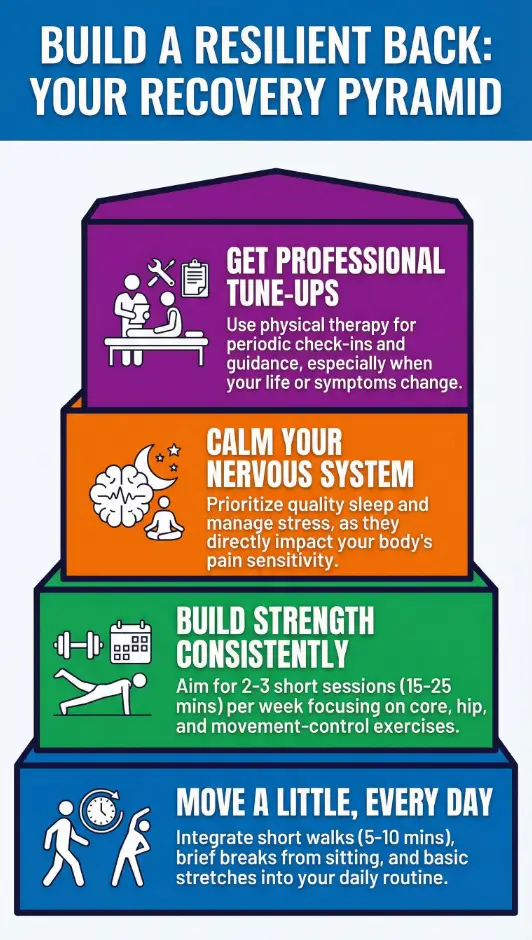
A sustainable plan usually has four layers:
- Daily micro-habits: short walks, posture changes, mini breaks from sitting.
- Weekly strength and control: 2–3 short sessions of targeted exercises.
- Periodic tune-ups: occasional PT check-ins when life or workload changes.
- Emergency rules: what to do when pain suddenly spikes or red flags appear.
Infographic — The Back Recovery Pyramid
Read the pyramid from bottom to top: the lowest level is your daily non-negotiable; the upper levels kick in when life gets heavier or symptoms change.
If you’re in a season of life where work, caregiving, or finances are tight, your long-term plan might be modest: a few key exercises, a walking minimum, and occasional telehealth check-ins. If you’re able to invest more, you might layer in gym work, yoga or Pilates, and structured programs aligned with the latest guidelines on exercise prescriptions for chronic low back pain.
- Think in layers: daily, weekly, periodic, and emergency.
- Let your routine flex with seasons of stress, travel, and workload.
- Check in with a professional when your life or symptoms change.
Apply in 60 seconds: Circle one habit for each layer of the pyramid that you’re willing to try for the next four weeks.
FAQ
1. How long does it usually take for physical therapy to help chronic low back pain?
Most studies and clinical programs that show benefit for chronic low back pain run for at least 8–12 weeks, often with 2–3 sessions per week and home exercises on top. Some people feel small improvements within 2–4 weeks—more ease walking, slightly better sleep—but meaningful changes in function and confidence usually take longer. If you’ve done a solid 8–12 week block with good adherence and absolutely nothing has changed, it’s worth revisiting the diagnosis with your healthcare team.
60-second action: Look at your calendar and count how many weeks of reasonably consistent PT and home practice you’ve actually completed—it’s often less than it feels.
2. When is low back pain a medical emergency instead of a PT problem?
Go to emergency or seek urgent medical care—not just PT—if you notice any of the following: sudden difficulty controlling your bladder or bowels, new or rapidly worsening weakness in your legs, numbness in the groin or genital area, back pain with fever or unexplained weight loss, or severe pain after major trauma like a fall or car crash. These “red-flag” signs can point to conditions that need immediate medical evaluation, not just exercise and manual therapy. If you want a clear checklist you can share with family, see when low back pain is a medical emergency.
60-second action: If any of those symptoms apply to you right now, stop reading and contact emergency services or urgent medical care before scheduling more PT.
3. What should I do if physical therapy seems to make my pain worse?
Mild soreness or stiffness after new exercises can be normal, especially in the first 1–2 weeks. But sharp, lasting increases in pain, new nerve symptoms, or a big drop in your ability to function are reasons to slow down and reassess. Bring specific details to your PT: which exercises, how many reps, how long the pain lasted, and what it felt like. Often the answer is to adjust the “dose”—fewer reps, smaller range of motion, or more rest days—rather than abandoning PT entirely.
60-second action: Write down the top three exercises that triggered more pain, with sets and reps, and bring that list to your next PT visit so you can problem-solve together.
4. How can I keep the cost of physical therapy manageable?
Start by understanding your copay, coinsurance, and visit limits, then design a plan that fits within those constraints. You might choose a higher-intensity block of sessions early on, then taper to less frequent “tune-ups” while relying more on a home program, community exercise classes, or digital PT options. Telehealth-based PT and group exercise programs can sometimes reduce overall costs compared with long-term one-on-one care, especially if travel is expensive or time-consuming.
60-second action: Use the cost estimator in this article to sketch a rough total for your next 6–12 weeks and then compare that number with what you’re realistically willing and able to spend.
5. What if I’ve tried physical therapy before and it “didn’t work”?
There are many flavors of PT. If your previous experience focused mostly on passive treatments (like heat, ultrasound, or massage) with little emphasis on exercise, education, or progressive strength, your body might not have received the kind of input that current guidelines emphasize. Even with a solid program, life factors—stress, sleep, mental health, work demands—can sabotage progress. It’s reasonable to try again with a clearer focus: ask for a plan built around exercise, functional goals, and a written home program, with realistic expectations set from day one. If you’re wrestling with the bigger question of whether chronic low back pain can be cured, that framing can also help you set gentler, more realistic goals while you rebuild momentum.
60-second action: List what your last PT block actually included (how often, what kind of work) and bring that list when you meet a new provider so you can design something deliberately different.
6. How do I know if I should switch therapists or clinics?
Good PT should feel collaborative, with clear explanations and a plan that adapts to your feedback. If you consistently feel rushed, unheard, or stuck on the same exercises for weeks without any adjustment or progress review, it may be worth seeking a second opinion—especially from someone with specific experience in chronic low back pain. Switching doesn’t mean your previous therapist was bad; it simply means you’re looking for a better match for your needs and learning style.
60-second action: Ask your current PT, “What is the specific goal for the next 4 weeks, and how will we know if we’re on track?” Their answer will tell you a lot.
Your next 15-minute step
Chronic low back pain is stubborn, but it is not chaos. Modern guidelines, years of physical therapy experience, and thousands of patient stories converge on the same, unglamorous reality: education, exercise, gradual load, and nervous-system support—done consistently and realistically—beat quick fixes almost every time.
The “brutally honest” part is that this takes time, attention, and some money. The hopeful part is that you don’t have to rebuild your entire life to move the needle. A few carefully chosen habits—backed by physical therapy that respects your schedule, budget, and fears—can change how your days feel this year, not just on a research chart.
Pick one secret from this article to focus on for the next four weeks: maybe it’s walking a little more, finally doing the “boring” exercises, or getting your coverage numbers so you can commit to a full PT block without financial surprise. Then, if possible, bring this plan to a physical therapist and say, “Here’s what I’m willing and able to do. Help me make it count.” If your symptoms ever shift toward persistent leg heaviness, walking intolerance, or sharper radiating patterns, it can help to understand lumbar spinal stenosis vs herniated disc as a conversation starter for your next clinical visit—without self-diagnosing.
Last reviewed: 2025-12; sources include global and national chronic low back pain guidelines and recent exercise and rehabilitation research.
physical therapy for chronic low back pain, chronic low back pain recovery, physical therapy cost calculator, walking for chronic low back pain, long-term back-care plan
