
Sciatica From Herniated Disc: How Long to Wait Before Surgery? 6-Week vs 12-Week Reality
I didn’t lose my patience to pain. I lost it to the calendar—because “reasonable waiting” can quietly turn into three more missed paychecks, sleepless nights, and a life that shrinks by inches.
Sciatica from herniated disc is leg-dominant nerve pain triggered when a damaged lumbar disc irritates a nerve root through pressure, inflammation, or both. The result can be burning calf pain, electric shocks, and walking limits that feel wildly out of proportion to the moment you’re in. If you want a clean baseline definition before we talk timelines, the difference between sciatica and a herniated disc is a helpful anchor for the rest of this guide.
Keep guessing and you don’t just lose weeks—you lose momentum, confidence, and the ability to trust your own body.
This post helps you use the 6-week vs 12-week window like a tool: what “good waiting” actually looks like, when imaging and injections make sense, and when a microdiscectomy conversation is the responsible next move.
It’s built around measurable checkpoints—walking minutes, sleep disruption, function wins, and red-flag awareness—not vague optimism.
No drama. | No doom. | Just a plan you can run between real-life obligations.
Here’s the timeline most people actually live.
Here’s how to stop paying for “hope-and-scroll.”
Here’s how to walk into your next appointment with numbers that change the plan.
Table of Contents
The two timelines most people actually live
In medical brochures, the timeline looks tidy. In real life, it looks like you trying to answer emails while your calf burns like it’s hosting a tiny, angry sun. The classic decision line for sciatica from herniated disc often lands somewhere between 6 and 12 weeks of structured conservative care—unless red flags appear.
I’ve watched friends (and yes, me too) do the “hope-and-scroll” plan: a couple of stretches, a random pill schedule, a brave face at work. That version of waiting is not neutral. It’s expensive in sleep, attention, and patience. If your symptoms are being amplified by long sitting and deadlines, the patterns in desk-job sciatica flare-ups may explain why your “reasonable waiting” feels harsher than it should.
- 6-week reality: you want proof you’re improving, not just surviving.
- 12-week reality: you want a plan that makes waiting worth it.
- The hidden truth: the clock only helps you if you’re measuring the right things.
Quick takeaway: Waiting can be wise, but only when it’s structured waiting with clear checkpoints every 7–14 days.
Show me the nerdy details
Most clinical pathways hinge on symptom trajectory, function, and neurologic findings—not pain intensity alone. A timeline without measurable function is just a calendar with anxiety attached.
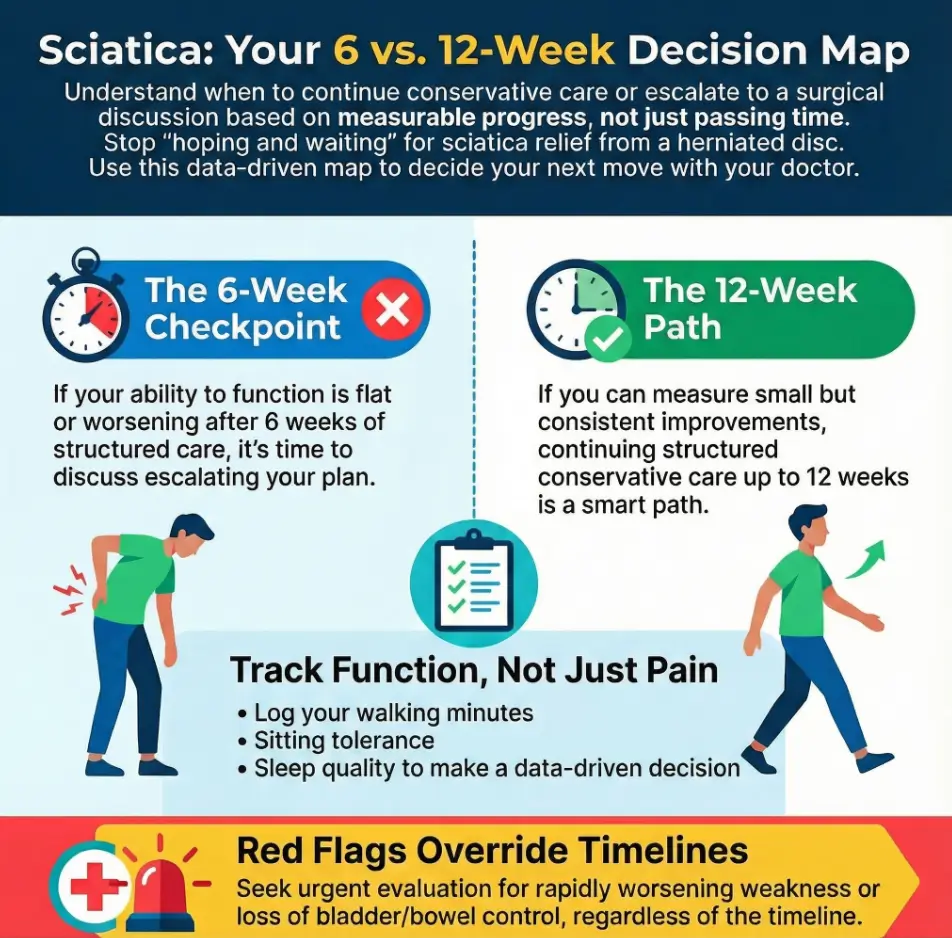
Red flags: when waiting is the wrong game
There’s a version of sciatica where patience is a virtue. There’s another version where patience is a gamble you didn’t agree to play. If you notice rapidly worsening weakness, loss of bowel or bladder control, or numbness in the saddle area, that’s an emergency pattern. This is not a “try a new pillow” moment. If you want a clearer, broader checklist for when to stop debating and seek urgent care, bookmark low back pain emergency warning signs.
I still remember the day I tested my toe strength against the floor like I was auditing my own nervous system. It felt dramatic until it didn’t. That tiny self-check gave me the confidence to call immediately instead of waiting three more “maybe it’ll pass” days.
- Sudden or progressive leg weakness is a high-priority signal.
- Bladder/bowel changes demand urgent evaluation.
- Severe numbness around the groin is not “normal sciatica.”
Apply in 60 seconds: Do a quick heel-walk and toe-walk test on a safe surface and note any clear asymmetry.
Neutral next step: Save these red flags in your phone notes and confirm your local urgent-care pathway today.
Why 6 weeks can be enough—and when it isn’t
If your pain is improving and your function is returning, 6 weeks can be a meaningful checkpoint. The goal isn’t to be pain-free by day 42. The goal is to see a consistent trend: better walking tolerance, less night pain, fewer “electric” episodes down the leg.
I once celebrated a 10-minute grocery trip like it was a marathon medal. That sounds silly until you’ve had to choose between toothpaste and the risk of another flare. If walking is your most reliable metric, practical tweaks—like pacing and even the right gear—matter; a quick scan of sciatica-friendly walking shoes can help you protect progress without turning every errand into a gamble.
- Look for a weekly function win, even small.
- Track sleep quality and morning stiffness.
- Notice whether pain is centralizing (moving up from the foot to the back).
When 6 weeks isn’t enough: persistent severe leg pain with little functional improvement, repeated inability to work, or meaningful weakness that doesn’t stabilize.
Show me the nerdy details
Disc-related radicular pain often improves as inflammation settles and the body adapts. Functional recovery and stable neurologic exams matter more than the most dramatic pain day you can remember.
The 12-week window: what good waiting looks like
The 12-week mark is where many clinicians and patients get honest. If you’re still functionally stuck, it may be time to discuss surgical options like microdiscectomy. But “waiting 12 weeks” doesn’t mean doing nothing for 12 weeks.
Good waiting is active:
- Focused physical therapy or guided home program.
- Medication strategy that protects sleep and movement.
- Clear plan for imaging and referral pathways where appropriate.
I once assumed time alone would fix me. It didn’t. What helped was a boring, consistent routine: short walks, symptom-guided exercises, and a boundary with my own hero complex. If you’re weighing your non-surgical team options, chiropractor vs physical therapy for back and leg pain can help you clarify what each approach is best suited to in this window.
- Schedule progress checks every 2 weeks.
- Prioritize sleep stabilization early.
- Use function goals, not pure pain scores.
Apply in 60 seconds: Write one measurable goal for next week (e.g., “walk 8 minutes twice a day”).
Neutral next step: Save your weekly goals and bring them to your next appointment to calibrate the plan.
The mechanics of pain: what a herniated disc is doing
A herniated disc can irritate a nerve root through mechanical pressure, chemical inflammation, or both. That’s why two people with similar MRI findings can live totally different pain stories. One walks around annoyed; the other can’t sit through a short meeting without bargaining with the universe.
I learned this the hard way when I saw a scary scan and assumed the worst. The radiology words felt like a verdict. My clinician reframed it as a map. That shift alone saved me a week of panic.
- Leg-dominant pain often reflects nerve irritation.
- Centralization can be a good sign of improvement.
- Strength changes matter more than pain drama.
Reality anchor: Imaging helps decision-making, but symptoms and function decide the urgency. And when your symptoms don’t perfectly match the herniated-disc script, quick differentials like diabetic neuropathy vs sciatica can help you ask sharper questions before you assume every leg signal is coming from the same source.
Your 60-second eligibility checklist for next steps
This isn’t a diagnosis tool. It’s a quick clarity filter for time-poor people who need to decide what to ask for next.
- Yes/No: Have you had persistent leg-dominant pain for ~6 weeks despite a structured plan?
- Yes/No: Is your walking/sitting tolerance still meaningfully limited?
- Yes/No: Are you missing work or daily roles more than 1–2 days per week?
- Yes/No: Do you notice stable or worsening weakness?
One-line next step: If you answered “Yes” to two or more, ask specifically about imaging, referral timing, and the 6- vs 12-week decision path.
Neutral next step: Screenshot this checklist and confirm your clinician’s criteria at your next visit.
Decision card: 6-week vs 12-week with time-cost tradeoffs
Think of this like choosing between two smart investments of your energy—both can be right, depending on your trend line.
Choose the 6-week escalation conversation if:
- Your function has barely moved despite consistent care.
- Sleep disruption is still severe most nights.
- You’re seeing early weakness or repeated “reset to zero” flares.
Choose the 12-week structured wait if:
- You can measure small weekly improvements.
- Leg pain episodes are less frequent or less intense.
- You’re rebuilding daily capacity without new red flags.
Time/cost trade-off: The 6-week path may shorten suffering but can accelerate testing and consult scheduling. The 12-week path may avoid surgery but demands disciplined tracking.
- Use function to decide, not fear.
- Escalate earlier if your life is shrinking fast.
- Stick with 12 weeks if the trend is clearly improving.
Apply in 60 seconds: Write down your three biggest functional limits and rate each from 0–10 today.
Neutral next step: Save this decision card and confirm your local referral timeline before you assume you can “wait and see.”
Mini calculator: how many weeks are you really losing?
This tiny estimator isn’t about medical certainty. It’s about personal clarity.
When I ran a version of this for myself, the number wasn’t a diagnosis—it was permission to stop minimizing the cost of “just waiting.”
Neutral next step: Save your estimate and confirm what improvement target would justify continuing conservative care.
Treatment options before surgery that actually move the needle
Before you jump to an operating-room calendar, many people deserve a fair shot at structured conservative options. The key word is structured. Random stretches and willpower rarely beat nerve inflammation.
- Targeted physical therapy: symptom-guided, not “push through everything.”
- Medication strategy: short-term anti-inflammatories or nerve-pain approaches when appropriate.
- Image-guided injections: sometimes used to reduce inflammation and buy functional time.
I once tried to out-stretch a nerve flare like it was a moral contest. My body responded with a polite but firm “nope.” The day I switched to pacing and clinician-guided progress, my improvement stopped being random. If you’re mapping this stage, it also helps to understand the broader category of sciatica nerve pain treatment pathways so your “conservative care” isn’t just a vague label.
- Define what “better” looks like in 14 days.
- Use walking tolerance as a primary metric.
- Escalate if your trend is flat.
Apply in 60 seconds: Ask for a written 6-week plan with a clear reassessment date.
Neutral next step: Save this options list and confirm which step is most appropriate for your specific level and symptoms.
If you and your clinician are discussing injections, you might hear different names depending on purpose and level. For very pattern-specific cases, an L5/S1 selective nerve root block can serve both diagnostic and therapeutic roles. And if you’re choosing between techniques, transforaminal vs interlaminar epidural approaches offers a practical comparison you can bring into the room without feeling like you’re guessing.
Medication strategy can be valuable for short, targeted windows—especially when sleep is falling apart. If NSAIDs or similar options are on the table, it’s worth reviewing back pain NSAID safety considerations so symptom control doesn’t quietly create a second problem.
How to talk to your clinician like a calm operator
The fastest way to get useful answers is to show your clinical team you’re tracking the right variables. You don’t need to sound like a textbook. You just need to sound like someone who respects time—yours and theirs.
- “My leg pain has lasted X weeks with a structured plan.”
- “My walking tolerance is Y minutes before symptoms spike.”
- “Sleep is disrupted Z nights per week.”
- “Here’s what improved and what didn’t.”
I used to say, “It hurts a lot.” That’s honest, but it’s not actionable. The moment I added numbers—minutes, nights, days missed—the conversation changed from sympathy to strategy. If your biggest struggle is nighttime positioning, the practical adjustments in side sleeping with sciatica can make your sleep data—and your week—less brutal.
Show me the nerdy details
Clinicians often triage based on function, neurologic exam, and response to conservative measures. A short, data-light tracker can speed decisions without over-medicalizing your life.
Neutral next step: Bring a one-page symptom and function log to your next appointment.
Short Story: The week I stopped pretending time was neutral (120–180 words)
Short Story: I kept telling myself I was being “strong” by waiting. Week six arrived like a quiet deadline I didn’t want to read. My leg pain wasn’t worse every day, but my life was smaller every day. I stopped walking to the corner café. I started scheduling my meetings around the least angry hours of my nerve. I told friends I was “fine” because explaining the truth felt like taking up too much oxygen.
One night, I watched the clock tick past 2 a.m. and realized I hadn’t measured anything that mattered. Not my walking time. Not my sleep losses. Not how often I canceled life. The next morning I wrote three numbers on a sticky note—minutes I could sit, minutes I could walk, nights I slept poorly—and carried it into my appointment. The plan changed in ten minutes. Not because I demanded surgery, but because I finally presented the story my body was actually living.
The 12-week reality checklist for a smart wait
If you’re going to wait toward the 12-week end of the spectrum, make the wait earn its place. This is how you protect hope from turning into drift.
- Week 1–2: confirm diagnosis impression, start symptom-guided movement.
- Week 3–4: evaluate trend; adjust PT/med strategy.
- Week 5–6: consider imaging plan if function is flat.
- Week 7–10: intensify functional rebuilding if improving.
- Week 11–12: set decision meeting: continue, inject, or discuss surgery.
I once treated weeks like wallpaper—always there, never informative. The moment I gave each two-week block a job, my anxiety dropped and my decision confidence climbed.
- Two-week reviews prevent silent stagnation.
- Function goals keep you honest and hopeful.
- Earlier escalation is reasonable when life impact is high.
Apply in 60 seconds: Put a reassessment date on your calendar for 14 days from today.
Neutral next step: Save this timeline and confirm your clinic’s recommended reassessment rhythm.
A simple coverage tier map for patients who need clarity
Insurance language can make a straightforward clinical decision feel like a bureaucratic maze. This simple map helps you ask better questions without pretending every plan works the same.
- Tier 1: Primary-care evaluation + basic meds + home program.
- Tier 2: Physical therapy with defined visit limits.
- Tier 3: Imaging pathways (often with prior authorization).
- Tier 4: Interventional options like injections.
- Tier 5: Surgical consult and procedure coverage rules.
What changes as you move up tiers: documentation requirements, referral rules, and timing expectations.
I learned to ask one sentence that saved me multiple phone calls: “What documentation do you need to approve Tier 4 or 5, and how long does it usually take?”
Neutral next step: Save this map and confirm your plan’s documentation checklist before you assume delays are unavoidable.

An infographic you can scan in 20 seconds
Stabilize sleep, reduce flare triggers, start gentle function tracking.
Look for function gains; if flat, discuss imaging and escalation.
Continue structured rehab if improving; book a decision consult if not.
Red flags or progressive weakness = urgent evaluation.
Use: Print or screenshot this and bring it to your next visit.
FAQ
Is surgery always needed for sciatica from a herniated disc?
No. Many people improve with structured conservative care. Surgery is usually considered when function remains significantly limited after a fair trial or when neurologic deficits escalate. Apply in 60 seconds: Write down your top 3 functional limits and how long they’ve persisted.
What’s the real difference between waiting 6 weeks and 12 weeks?
Six weeks is a practical early checkpoint for trend assessment. Twelve weeks is a more extended window for recovery when improvement is clearly happening. The decision hinges on your trajectory, not the calendar alone. Apply in 60 seconds: Rate your walking tolerance today and compare it to two weeks ago.
What if my MRI looks scary but I’m improving?
Imaging findings don’t always match symptom severity. If your function and neurologic exam are improving, that trend matters a lot. Apply in 60 seconds: Ask your clinician to explain how your symptoms align with the imaging level.
Do injections replace the need for surgery?
They can reduce inflammation and improve function for some people, buying time for recovery. They’re not a guaranteed substitute for surgery in persistent severe cases. Apply in 60 seconds: Ask about the expected goal of an injection: pain reduction, functional gain, or diagnostic clarity.
How do I know if weakness is “serious enough”?
Any new or worsening weakness deserves prompt evaluation. Progressive weakness is a higher-priority signal than pain alone. Apply in 60 seconds: Try a safe heel-walk/toe-walk test and note clear differences side to side.
How should I prepare for insurance or hospital approvals?
Bring a concise symptom timeline, prior treatments tried, and functional impact notes. Clear documentation can shorten delays. Apply in 60 seconds: Create a one-page log with dates, therapies, and outcomes.
Conclusion: the smartest next 15 minutes
The 6-week vs 12-week question isn’t really about patience. It’s about protecting your future function with the least wasted time. If you’re improving, the 12-week path can be a smart, calm investment. If you’re flat, shrinking your life to survive the day, or noticing weakness, the 6-week escalation talk is not “overreacting.” It’s responsible.
My own turning point was embarrassingly simple: I stopped arguing with the calendar and started tracking my life like it mattered. It did.
- Measure walking, sitting, and sleep weekly.
- Use 6 weeks as an honest checkpoint.
- Use 12 weeks only with a structured plan.
Apply in 60 seconds: Write a single sentence you’ll say at your next visit: “Here’s my 6-week trend, and here’s what I need help deciding.”
Last reviewed: 2025-12; sources: MedlinePlus, American Association of Neurological Surgeons, North American Spine Society.
Your next 15 minutes: Run the time-loss estimator, fill the eligibility checklist, then book a reassessment appointment date. You’re not choosing between bravery and surgery—you’re choosing between random waiting and strategic recovery.
