
Anti-Inflammatory Medications for Back Pain: 7 Safety Rules I Learned the Hard Way
You know that kind of 3:00 AM panic, right? The one where you shift in bed just a little and suddenly your lower back lets out a primal scream that could wake the neighbors—or at least your dog. Yeah, I’ve been there. Flat on my back, eyes glued to the ceiling like it’s going to offer answers, mentally negotiating with the universe (“If you just make this stop, I swear I’ll stretch every day”), and reaching for that battered bottle of ibuprofen on the nightstand like it’s some kind of divine relic.
Back pain has a special way of turning otherwise rational adults into amateur pharmacists. You start googling half-remembered drug names and wondering if it’s okay to mix naproxen with that half-dose of Tylenol you took three hours ago… or was it four? All in the desperate pursuit of just one blessed hour of uninterrupted sleep.
But here’s the cold, hard truth I had to learn the painful way—like, actual-ER-visit kind of painful: treating inflammation isn’t a free-for-all. It’s not a “take what you want, when you want” situation. NSAIDs (non-steroidal anti-inflammatory drugs) are no joke. They’re incredibly effective—when used properly. But most of us never read the fine print. (Let’s be honest, who has read the back of an Advil bottle without a magnifying glass and a minor in pharmacology?)
So if you’re out here juggling insurance co-pays, wondering why that generic naproxen seems about as useful as a Tic Tac, or nervously side-eyeing the kidney warning on the label, you’re in good company. I’ve been through it—and lived to tell the tale (and rebuild my stomach lining).
Stick with me for the next five minutes. I’m going to walk you through the 7 safety rules that quite literally saved my back—and kept me out of the ER. Because managing pain shouldn’t come with a side order of gastrointestinal regret.
Table of Contents
The Mechanism: Why Back Pain Fights Dirty
Before we dive into the rules, we need to understand the enemy. When your back “goes out,” it’s rarely just a muscle spasm. It’s a chemical cascade. Your body releases enzymes called cyclooxygenase (COX), which produce prostaglandins. These prostaglandins are essentially little messengers that tell your brain, “Hey, we are injured down here! Swell up and throb!”
NSAIDs (Non-Steroidal Anti-Inflammatory Drugs) work by blocking those COX enzymes. Think of them as jamming the communication lines so the “swell and throb” message never fully arrives. But here is the catch: those same prostaglandins protect your stomach lining and keep blood flowing to your kidneys. When you block the pain, you are also blocking your body’s natural armor.
I learned this the hard way when I assumed that because I could buy Aleve at a gas station, it was as safe as drinking water. It isn’t. It’s a serious pharmaceutical intervention that requires respect.
- Prostaglandins cause pain but protect the gut.
- COX-1 enzymes maintain stomach lining.
- COX-2 enzymes drive inflammation.
Apply in 60 seconds: Check your current bottle. If it says “NSAID” (Ibuprofen, Naproxen, Aspirin), treat it with the same caution as a prescription drug.

Rule 1: The Full Stomach Mandate (No Exceptions)
If you take nothing else away from this article, let it be this: Never take an oral NSAID on an empty stomach.
I used to wake up in pain, swallow two ibuprofen with a gulp of black coffee, and head to work. By 10:00 AM, my back felt better, but my stomach felt like it was digesting itself. I ignored it for weeks until “heartburn” turned into a gnawing, erosive pain that necessitated a very expensive camera down my throat.
The “Full Stomach” rule isn’t about eating a cracker. It’s about buffering. You need a lipid or protein barrier. When the pill dissolves, it sits against the stomach wall. Without food, the drug comes into direct contact with the mucosa while simultaneously shutting down the repair mechanisms we discussed earlier. It’s a double tap to your gut health.
What Constitutes a Protective Meal?
You don’t need a Thanksgiving dinner. In fact, overeating can slow absorption too much. Aim for:
- 6-8 ounces of water: Dilution is the solution to pollution.
- Fat or Protein: A spoonful of peanut butter, a slice of cheese, or half an avocado. Fats coat the lining effectively.
- Avoid Acid: Taking NSAIDs with orange juice or coffee is like pouring gasoline on a spark.
Show me the nerdy details
Traditional NSAIDs are non-selective COX inhibitors. They block both COX-1 (stomach protection) and COX-2 (inflammation). Newer generation drugs like Celecoxib (Celebrex) are COX-2 selective, meaning they target the pain more than the stomach. However, even selective inhibitors carry risks and often require higher insurance copays or prior authorization. A 2021 review in Gastroenterology highlighted that up to 25% of chronic NSAID users develop some form of ulcer disease, often asymptomatic until a bleed occurs.
Rule 2: The Kidney Filtration Check
Your kidneys are the silent heroes of back pain management. They filter out the metabolites of the drugs you take. NSAIDs restrict blood flow to the kidneys. If you are young and hydrated, your body compensates. If you are dehydrated, older, or have underlying issues, this constriction can cause acute kidney injury.
I see this happen in amateur sports leagues all the time. Guys play hard, get dehydrated, drink a beer (which dehydrates further), and then pop 800mg of ibuprofen. That is a perfect storm for renal stress. The “kidney check” is a mental pause you must take before opening the bottle.
💧 Dehydration & NSAID Risk Calculator
Are you safe to take that dose right now? Run this quick mental check.
- Thirsty or dry mouth
- Dark yellow urine
- Just finished intense cardio
- Consumed alcohol in last 2 hours
- Well hydrated (clear urine)
- Ate food recently
- Resting heart rate
- No alcohol in system
Action: If you are in the Red column, drink 16oz of water and wait 30 minutes before dosing.
Chronic use is where the real danger lies. If you are taking these daily for more than 10 days, you need blood work. Specifically, you want to ask your doctor about your eGFR (estimated Glomerular Filtration Rate). It’s a number on your standard metabolic panel that tells you how well your kidneys are filtering. I monitor mine yearly now, and it gives me peace of mind when I need a week of Naproxen for a flare-up.
Rule 3: The “Ceiling Effect” Myth
There is a dangerous misconception that if 2 pills reduce pain by 50%, then 4 pills will reduce it by 100%. This is the “Ceiling Effect,” and ignoring it is physically dangerous.
Most NSAIDs have a therapeutic ceiling. Once you hit the maximum effective dose (for ibuprofen, this is often around 400mg-600mg per dose for analgesia, though anti-inflammatory effects might require higher doses under doctor supervision), taking more does not block more pain. It only increases toxicity. The pain relief plateaus, but the risk line shoots straight up like a hockey stick graph.
Short Story: The “Super Bowl” Mistake (140 words) During the Super Bowl two years ago, I threw my back out moving a cooler. I wanted to enjoy the game, so I took 800mg of ibuprofen. Two hours later, still in pain, I took another 800mg. I assumed I was just “built different” and needed a horse dose. By halftime, I wasn’t watching the game.
I was in the bathroom, dizzy, with a ringing in my ears (tinnitus—a classic sign of overdose) and violent nausea. I didn’t get less back pain; I just added a poisoning symptoms list to my misery. My doctor later explained that I had blown past the ceiling dose. I had saturated the enzymes. The extra 800mg was just floating around attacking my organs for no benefit. Lesson learned: The label isn’t a suggestion; it’s a biochemical law.
Rule 4: Interaction Roulette: Blood Thinners & SSRIs
This is the section where you need to pay attention if you take any other daily medication. We often think of OTC drugs as chemically inert regarding interactions. We are wrong.
The most common silent interaction is with SSRIs (antidepressants like Prozac, Zoloft, Lexapro). Both NSAIDs and SSRIs affect how your platelets work. Taking them together significantly increases the risk of upper gastrointestinal bleeding. It’s not a guarantee you’ll get hurt, but the risk multiplier is real.
Then there are the blood thinners (Warfarin, Eliquis, Xarelto). Mixing these with aspirin or ibuprofen is essentially removing your body’s ability to stop bleeding. A minor bruise becomes a hematoma. A gum bleed doesn’t stop.
The Hypertension Trap
Do you take blood pressure medication? ACE inhibitors (like Lisinopril) or diuretics? NSAIDs can actually cancel out their effects, causing your blood pressure to spike silently. You think you’re managing your back pain, but you’re actually putting yourself into a hypertensive crisis zone. I now check my blood pressure at home (those cuff machines are $30 online) whenever I’m on a multi-day course of anti-inflammatories.
Mayo Clinic’s overview of NSAIDsRule 5: Topical vs. Oral: The Absorption Game
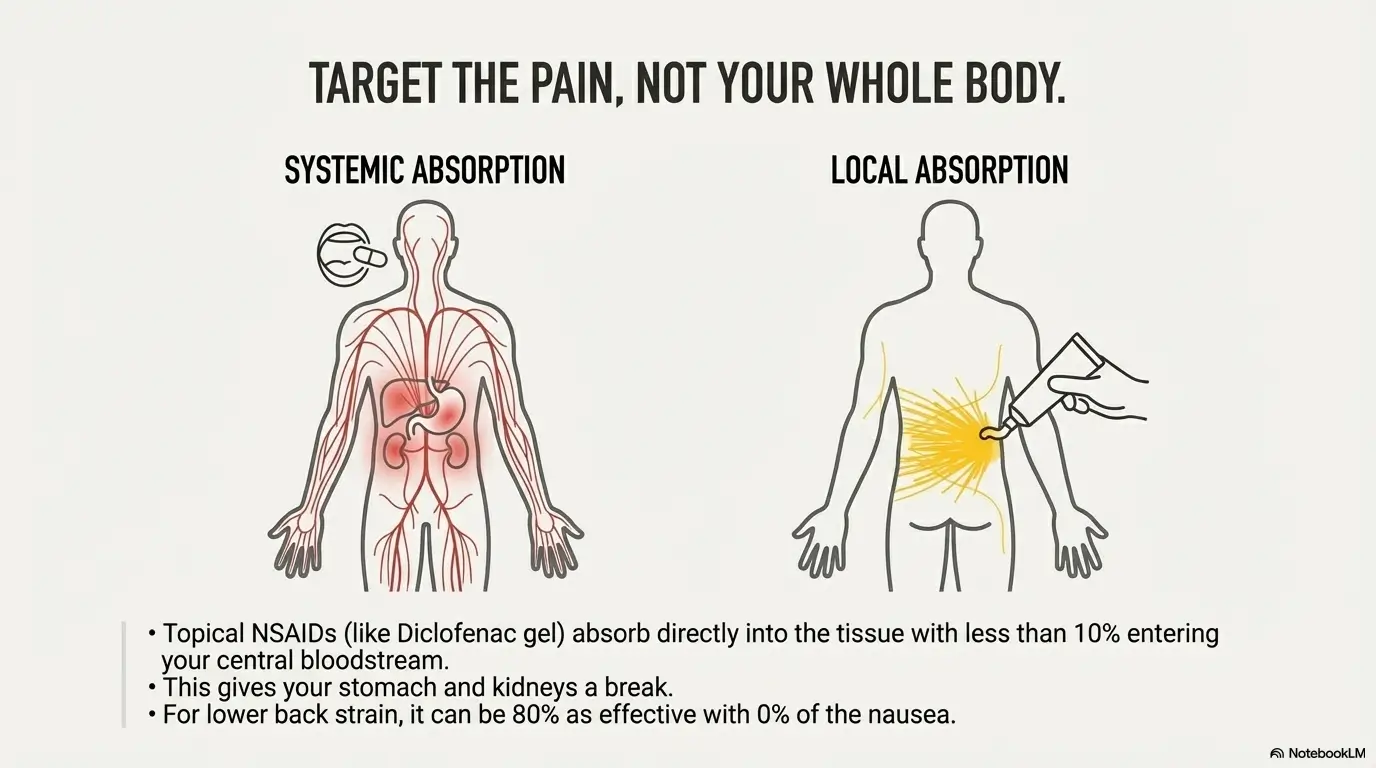
For years, I thought creams and gels were placebos. I thought, “If I can’t swallow it, it’s not strong enough.” That was ignorance talking. Enter Diclofenac Sodium Gel (Voltaren).
Topical NSAIDs are a game-changer for localized back pain. The medication absorbs through the skin directly into the inflamed tissue, but—and this is the key—very little of it enters your central bloodstream compared to a pill. Studies suggest systemic absorption is significantly lower (often less than 10%) compared to oral dosing.
This means your stomach and kidneys get a break. For lower lumbar strain, where the tissue is relatively close to the surface, I found the gel to be about 80% as effective as the pill, but with 0% of the stomach nausea. If you have “GI sensitivity” or are on that “Red Light” list for kidney issues, topicals should be your first line of defense.
- Significantly lower risk of ulcers and kidney stress.
- Best for “shallow” pain (joints, lower back fascia).
- Do not combine with oral NSAIDs unless directed by a doctor (you can still overdose).
Apply in 60 seconds: Next time you are at the pharmacy, compare the price of generic Diclofenac gel vs. the brand name. The active ingredient is identical.
Rule 6: Duration Limits & Cycling Strategies
My doctor gave me a rule that I live by: The 7-Day Hard Stop.
If you are taking OTC anti-inflammatories for 7 days straight and the pain hasn’t subsided significantly, the drug isn’t the solution anymore; it’s a crutch for a problem that needs a different diagnosis. Maybe it’s nerve impingement (sciatica), maybe it’s a disc issue. Inflammation is usually the initial response; chronic pain involves different pathways.
When I hit day 7, I taper off. I don’t just stop cold turkey if the pain is high, but I switch modalities. I move to heat/ice, stretching, or physical therapy exercises. Continuing NSAIDs past 10-14 days without a doctor’s oversight is drifting into the danger zone of cardiovascular risk. Yes, long-term NSAID use is linked to higher risks of heart attack and stroke. It’s a slight increase, but why risk it for a pill that stopped working three days ago?
Rule 7: The Tylenol Stagger Method
This is the advanced operator move. Acetaminophen (Tylenol) is not an NSAID. It works on pain receptors in the brain, not inflammation at the site. Because they are processed by different organs (NSAIDs = Kidneys/Gut, Tylenol = Liver), you can technically use them in the same timeframe—if you are careful.
When my pain was at a 9/10, my pharmacist recommended “The Stagger.”
- 12:00 PM: Dose of Naproxen (Aleve) – Lasts 12 hours.
- 6:00 PM: Dose of Acetaminophen (Tylenol) – Bridging the gap.
- 12:00 AM: Dose of Naproxen.
This keeps a steady level of analgesia without doubling up on the toxic load for any single organ system. However, you must be rigorous about tracking total daily milligrams. Acetaminophen is the leading cause of acute liver failure in the US/UK because it hides in other drugs (cold meds, sleep aids). If you do the Stagger, you take NOTHING else with Tylenol in it.
Smart Economics: Insurance, Generics, and Costs
Let’s talk money, because back pain is expensive. You might be paying for brand names, or worse, paying out-of-pocket for prescriptions your insurance would cover if coded correctly.
If you require daily, high-dose NSAIDs (like Celebrex/Celecoxib for arthritis-related back pain), the costs add up. Generic Celecoxib is available, but coverage varies by “Tier” on your insurance formulary.
💰 Monthly Cost Comparison (Estimated, 2024)
Treating chronic back pain? Here is what you are looking at paying out-of-pocket vs. insured.
| Medication Type | OTC Cost (Mo) | Rx Copay (Avg Tier 1) | Notes |
|---|---|---|---|
| Ibuprofen (Generic) | $10 – $15 | $0 – $5 | Often cheaper to buy bulk OTC than use insurance. |
| Naproxen (Generic) | $12 – $18 | $0 – $8 | Higher duration means fewer pills/bottles. |
| Celecoxib (Generic) | N/A (Rx Only) | $10 – $45 | Requires “Prior Authorization” on some plans. |
| Voltaren Gel (Generic) | $30 – $50 | $5 – $15 | Huge savings if prescribed vs OTC tubes. |
Tip: If you use the gel daily, ask your doctor for a prescription. Insurance often covers the large tubes for a small copay, whereas buying small tubes OTC costs a fortune.
Always check your insurance “Formulary” (drug list) for the current year. Sometimes they move a drug from Tier 1 (cheap) to Tier 2 or 3. If you have a Health Savings Account (HSA) or FSA, remember that OTC anti-inflammatories are now generally eligible expenses without a prescription, thanks to recent law changes in the US. Save your receipts.

FAQ
Can I take Ibuprofen and Naproxen together?
No. Taking two different NSAIDs together (like Advil and Aleve) does not increase pain relief; it exponentially increases the risk of side effects like stomach bleeding and kidney damage. They compete for the same enzymes. Choose one and stick to the dosing schedule.
How long does it take for anti-inflammatories to work for back pain?
Short-acting NSAIDs (Ibuprofen) typically kick in within 20-30 minutes. Long-acting ones (Naproxen) may take up to an hour but last longer. However, for the full anti-inflammatory effect (reducing the swelling, not just the pain), you often need to take them consistently for 2-3 days as directed by a doctor, rather than just “as needed.”
Is it safe to drink alcohol while taking NSAIDs?
It is highly risky. Alcohol irritates the stomach lining, and NSAIDs remove the stomach’s protection. Combining them significantly raises the chance of gastric bleeding (gastritis). If you are on a course of back pain meds, skip the wine/beer until you are done.
What is the safest anti-inflammatory for someone with high blood pressure?
This is a strict “ask your doctor” question, but generally, NSAIDs can raise blood pressure and interfere with BP meds. Often, doctors may recommend Acetaminophen (Tylenol) as a safer alternative for cardiac patients, or prescribe a specific NSAID at the lowest dose for the shortest time, monitored closely.
Does heating the back help NSAIDs work better?
Heat increases blood flow to the area, which can help relax muscles, while the NSAID reduces chemical inflammation. They work well as a team. Apply heat for 20 minutes on, 20 minutes off. Just don’t apply heat directly over a patch or gel unless the package says it’s safe (most say don’t, as it speeds absorption too much).
Conclusion: Respect the Chemistry
Back pain makes us desperate. I remember lying on that floor, willing to trade a kidney for relief. But the “hard way” taught me that your body keeps score. You can’t cheat the chemistry.
Treat these medications with the same respect you’d give a power tool. They are effective if you follow the safety protocols: full stomach, hydration check, proper dosing, and listening to your body when it says “enough.”
Don’t just guess. Take 60 seconds right now to look at the bottle you have. Check the expiration, check the dosage, and calculate when you last ate. If you are in chronic pain that isn’t shifting after a week of safe usage, put the bottle down and pick up the phone to see a specialist. Your stomach—and your back—will thank you.
The 4 Pillars of Safe Relief
Never on an empty stomach. Buffer the acid.
Protect the kidneys. Clear urine is the goal.
Respect the dosing intervals. No overlapping.
If pain persists, stop and see a doctor.
Disclaimer: I am a writer sharing personal experiences, not a doctor. This article is for informational purposes and does not constitute medical advice. Always consult your physician before starting or changing any medication regimen. Last reviewed: 2024-11
Anti-Inflammatory Medications for Back Pain, NSAID safety rules, back pain relief medication, kidney safety with ibuprofen, prescription back pain costs
