Diabetic Neuropathy vs Vitamin B12 Deficiency in Long-Term Metformin Users: Lab Tests, Nerve Damage, and Treatment Costs
Diabetic Neuropathy vs. Metformin-Induced B12 Deficiency
By the time your feet start burning at night, metformin has usually been sitting quietly in your pillbox for years.
Labs look “fine,” A1c looks “better,” yet nobody has clearly sorted out the one question that actually keeps you awake: is it diabetic neuropathy or vitamin B12 deficiency from long-term metformin? What’s really driving your nerves crazy, and what’s still fixable?
Right now you’re stuck guessing between overlapping neuropathy symptoms, expensive EMGs, and a drug you’re told is “standard of care.” Guess wrong, and you don’t just live with avoidable nerve damage—you also slide into years of repeat copays, nerve studies, and trial-and-error pain meds that may never touch a B12 problem.
This guide shows you how to use specific lab tests, symptom patterns, and 2025 treatment costs to tell if low B12, diabetes, or both are behind your nerve pain—so you can act early, protect function, and stop overpaying for the wrong plan. If some of your symptoms sound more like pain shooting from your back down one leg, our separate guide on diabetic neuropathy vs sciatica walks through that overlap.
It’s built from current diabetes guidelines, metformin safety updates, and real-world US pricing for B12 tests, EMG, and neuropathy meds.
- First, you’ll see how typical B12-related symptoms differ from classic diabetic neuropathy.
- Then we’ll map which blood tests and nerve studies actually change decisions.
- Finally, you’ll get simple money blocks and scripts you can take straight into your next visit.
Table of Contents
Why this question matters now for long-term metformin users
Picture someone like Daniel, 63, who has taken metformin for a decade. His A1c finally sits in the safe zone, but his toes feel like they’re plugged into a weak power socket every night. One specialist shrugs, “diabetic neuropathy, part of the deal.” Another quietly orders a vitamin B12 test and talks about metformin.
Over the last few years, large studies have shown that long-term metformin use increases the risk of vitamin B12 deficiency and neuropathy, especially after four or more years on the drug. Safety regulators in multiple countries now label B12 deficiency as a “common” adverse effect of metformin and advise testing levels when neuropathy or anemia appears. Diabetes guidelines also explicitly recommend periodic B12 checks for people taking metformin chronically.
On the money side, the gap is just as important. A vitamin B12 blood test in the US typically runs somewhere between about $11 and $100 cash, depending on the lab, with common online panels listing prices in the $35–$90 range. A combined nerve conduction study and EMG, often used to document neuropathy, can cost $150–$500 or more per limb without insurance. With insurance, you may still face meaningful coinsurance if your deductible isn’t met. If some of your symptoms are driven by low B12, that’s a very different cost curve than years of escalating nerve pain and prescription copays.
In other words, getting the cause roughly right changes both your body and your budget. You’re not being dramatic for wanting to know whether your metformin and vitamin B12 status have ever been checked together.
- Metformin is effective, but long-term use can quietly drain vitamin B12.
- Low B12 can mimic or worsen diabetic neuropathy.
- Blood tests for B12 are relatively cheap compared with nerve studies and chronic pain meds.
Apply in 60 seconds: Write down: “Years on metformin, current dose, first day I noticed tingling.” Take that note to your next appointment.
Money Block #1 – 60-second eligibility checklist for B12 testing (metformin users, 2025, US)
- Have you taken metformin for ≥4 years or at doses ≥1,000–1,500 mg/day? (Yes/No)
- Do you have numbness, tingling, burning, or “stocking-glove” sensations in your feet or hands? (Yes/No)
- Any balance issues, clumsiness, or “walking on foam” feeling? (Yes/No)
- Any unexplained fatigue, pale skin, or shortness of breath? (Yes/No)
- Are you vegetarian/vegan, over 60, or on acid-suppressing drugs like PPIs? (Yes/No)
If you answered “Yes” to metformin use plus any nerve symptom or risk factor, you’re a strong candidate for a B12 check. This doesn’t mean you have deficiency; it just means the test is reasonable and defensible when you ask for it.
Save this checklist and confirm with your own clinician whether you meet their local criteria for vitamin B12 testing.
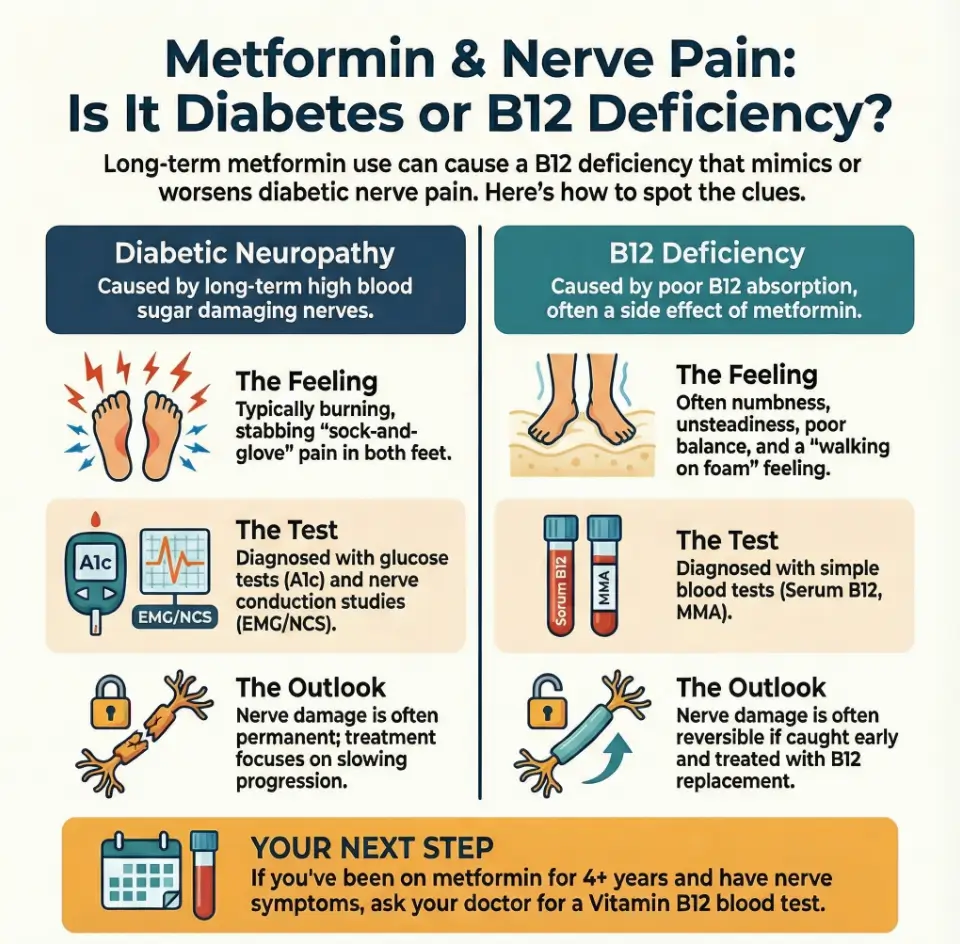
Symptom patterns: diabetic neuropathy vs vitamin B12 deficiency
Think of your nerves as a complex wiring system. Diabetes tends to fry the wiring from the ends inward; B12 deficiency tends to damage both the wiring and the insulation, sometimes higher up near the spine as well as in the feet. By contrast, when pain follows a single nerve from the lower back down one leg, that pattern fits more with classic sciatica nerve pain than with symmetric diabetic neuropathy.
Classic diabetic peripheral neuropathy pattern:
- Slow onset over years of elevated blood sugar.
- Starts in both feet, then creeps upward like socks.
- Burning, stabbing, or electric pains, especially at night.
- Reduced vibration sense in toes; harder to feel a tuning fork or phone vibration.
- Loss of protective sensation: painless blisters or ulcers on the feet.
Classic vitamin B12 deficiency pattern (which can overlap with diabetes):
- Numbness, tingling, or “pins and needles” in feet and hands.
- Unsteady gait, trouble with balance, or feeling like you’re walking on cotton.
- Weakness, fatigue, or breathlessness from anemia in more advanced cases.
- Mood changes, memory issues, or “brain fog,” especially in older adults.
- Sore or smooth tongue, sometimes with loss of taste.
One reader described it like this: “My feet felt weird for years, but when I started dropping my keys and wobbling on stairs, that’s when my doctor finally checked B12.” Their level was low, they started treatment, and over six months their coordination improved, though the burning at night didn’t vanish completely.
Here’s the uncomfortable truth: symptoms alone almost never tell the full story. A person with well-controlled A1c can still have B12 deficiency from metformin; someone with chronically high glucose can have pure diabetic neuropathy; many people have a blend.
Show me the nerdy details
Diabetic neuropathy often shows length-dependent axonal loss on nerve conduction studies: slowed conduction velocity and reduced amplitudes in distal sensory nerves. Vitamin B12 deficiency, by contrast, frequently affects the dorsal columns of the spinal cord and peripheral nerves, leading to impaired vibration and joint position sense and sometimes positive Romberg testing. In practice, electrodiagnostics alone can’t reliably separate the two; correlation with lab measures (serum B12, methylmalonic acid, homocysteine) and clinical context is essential.
- Diagonal balance issues and clumsiness lean more B12-ish.
- Pure stocking-glove pain with long diabetes history leans more diabetic neuropathy.
- Metformin users often sit somewhere in the messy middle.
Apply in 60 seconds: Write three columns: “Feet,” “Hands,” “Balance.” Jot any symptoms and how long they’ve been present. This will help your clinician see patterns quickly.
How long-term metformin changes vitamin B12 levels
Metformin is still the first-line workhorse for type 2 diabetes: cheap, effective, and proven to reduce complications when used properly. But like any long relationship, there are side effects you only notice after a few years together.
Multiple observational studies and reviews have shown that:
- Metformin interferes with vitamin B12 absorption in the small intestine over time.
- People on metformin for ≥4 years, especially at higher doses, have a significantly higher rate of B12 deficiency than those not on metformin.
- The risk of B12 deficiency and neuropathy appears to rise a few percentage points for every year of ongoing metformin therapy in some cohorts.
In 2022, the UK medicines regulator officially labeled reduced vitamin B12 levels as a common side effect of metformin and advised testing for patients with symptoms or at high risk; similar alerts have appeared in other countries since. Updated diabetes care standards in 2024–2025 now call for periodic B12 monitoring in long-term metformin users, particularly when anemia or neuropathy is present.
The frustrating part for patients: you can feel perfectly fine while your B12 quietly drifts down, then one day you realise your feet feel dull and your memory isn’t what it used to be. In some people, neurological symptoms show up before obvious anemia or wildly abnormal routine blood tests.
I’ve seen more than one person assume their “age-related” clumsiness was inevitable, only to discover a low B12 level, treat it, and find that stairs no longer feel like a tightrope walk. The earlier the problem is caught, the more nerve function you tend to preserve.
Money Block #2 – Decision card: B12 supplementation vs changing metformin dose (2025, US)
| When to focus on | Keep metformin, add B12 plan | Revisit metformin dose/alternatives |
|---|---|---|
| Glucose control | A1c improves or stays stable on metformin alone. | A1c remains high even with maxed-out dose and lifestyle changes. |
| B12 status | Mild deficiency, responsive to oral or injectable B12. | Severe deficiency that recurs despite supplementation and good adherence. |
| Side effects | GI side effects manageable; lactic acidosis risk low. | Multiple intolerable side effects or other contraindications to metformin. |
| Cost/coverage | Metformin is inexpensive on your plan; B12 lab/tests covered after deductible. | You face repeated high-cost hospital visits or complex polypharmacy for side effects. |
Use this decision card as a conversation starter with your clinician; they can adjust it to your lab results, glucose targets, and insurance coverage.
Lab tests that separate the two in 2025 (US): what to order and why
When you strip away the jargon, you’re really asking two questions:
- Is my vitamin B12 level low or borderline?
- Are my nerves damaged from diabetes, B12 deficiency, or something else entirely?
The core blood tests most clinicians consider:
- Serum vitamin B12 – the basic starting point. Very low levels usually confirm deficiency; borderline results may need further testing.
- Methylmalonic acid (MMA) – often rises early in B12 deficiency, sometimes before serum B12 looks terrible.
- Homocysteine – can also be elevated in B12 (and folate) deficiency, though it’s less specific.
- Complete blood count (CBC) – to look for macrocytic (large-cell) anemia, which often accompanies more advanced B12 deficiency.
In many US cash-price lab menus, a standalone vitamin B12 test can cost as little as about $11–$40 in discounted online panels, up to around $80–$100 at some national chains, depending on location. MMA and homocysteine can add to that bill; older and newer cash menus often place them roughly in the $20–$80 range per test.
To document neuropathy itself, clinicians may order:
- Nerve conduction studies and EMG – measure how well electrical signals travel along nerves and into muscles.
- Quantitative sensory testing – looks at vibration and temperature thresholds.
- Occasional MRI – if spinal cord disease is suspected.
Without insurance, a combined EMG and conduction study for one limb in the US commonly lands in the $150–$500 range, sometimes higher at large hospital systems. With insurance, you may see a $10–$50 copay or 10–50% coinsurance if you haven’t met your deductible yet. When tests point more toward a compressed nerve in the spine than a metabolic neuropathy, the conversation sometimes shifts to targeted injections or surgery; you can see examples in our explanations of L5–S1 selective nerve root blocks and transforaminal vs interlaminar epidural injections.
Money Block #3 – Fee table: B12 vs nerve tests after new neuropathy symptoms, high deductible, 2025 (US)
| Test (2025, US) | Typical cash range | Notes |
|---|---|---|
| Serum vitamin B12 | $11–$100 | Often closer to $35–$90 via online pay-upfront labs. |
| MMA / homocysteine | $20–$80 each | Ordered when B12 is borderline or symptoms are severe. |
| EMG + nerve conduction (one limb) | $150–$500 | Price can stack if multiple limbs are tested. |
Save this table and confirm the current fee on your lab’s or clinic’s official price list before scheduling tests, especially if you haven’t met your deductible.
If you’re outside the US, the structure is similar but numbers move. For example, in parts of Europe and the UK, B12 testing is often covered under national systems when clinically indicated, while EMG pricing can vary widely between public hospitals and private centers. In some countries, regional formularies now explicitly reference metformin–B12 safety updates when deciding who deserves funded testing.
Nerve damage: what’s reversible, what isn’t, and how fast to act
Here’s the scary part first, then the hopeful part.
With long-standing diabetes, some nerve damage is genuinely structural: axons have degenerated, the blood supply to tiny nerve fibers has been impaired for years, and fully reversing that is unlikely. The realistic goal is slowing progression, reducing pain, and protecting balance as much as possible.
With vitamin B12 deficiency, nerves and spinal cord tissue can sometimes recover impressively if treatment starts early. Evidence from case series and reviews suggests that:
- Symptoms present for months often show meaningful improvement after B12 replacement.
- Symptoms present for years may improve partially but rarely go back to “never happened.”
- Severe spinal cord damage may leave residual gait problems even after B12 normalises.
Short Story: you’d be surprised how often the body forgives you when you give it what it was missing. One woman in her late 60s had been chalking up her “drunken hallway walk” to getting older. She finally had labs done: her B12 level was low, and she started injections. Three months later, her description changed: “I still feel wobbly if I close my eyes in the shower, but I no longer bounce off the doorframe.” The diabetes didn’t vanish, but one ingredient of the nerve misery turned out to be fixable. That’s the quiet power of catching B12 deficiency before every symptom has calcified into permanent damage.
In mixed cases (diabetes plus B12 deficiency), the realistic goal is:
- Correct B12 deficiency quickly to stop that part of the damage from getting worse.
- Intensify glucose management to slow additional diabetic nerve injury.
- Use pain management strategies (medications, physical therapy, footwear) to keep life livable.
Show me the nerdy details
Pathologically, B12 deficiency causes demyelination in the posterior and lateral columns of the spinal cord and peripheral nerves, while diabetic neuropathy is primarily a distal symmetric axonal neuropathy with microvascular ischemia. Early B12 replacement can remyelinate affected areas and reduce abnormal nerve firing. However, once axons have degenerated and Wallerian degeneration is complete, both conditions share the same limitation: regeneration is slow and often incomplete, especially in older adults or in the presence of continued hyperglycemia.
- Think in months, not years, for the best chance at reversal.
- Even partial improvement can mean better balance and less pain.
- “Too late to bother” is rarely true; it’s just sometimes less dramatic.
Apply in 60 seconds: If you’ve had neuropathy symptoms for under a year, circle that fact on your symptom list and highlight it for your clinician—it’s a strong argument for urgent B12 testing and aggressive diabetes control.
Treatment costs, coverage tiers, and out-of-pocket risk in 2025 (US)
Once you know what’s going on, the money questions hit: How much will fixing this cost me? and What lands under deductible, copay, or Medicare Part D?
For B12 deficiency in the US:
- Oral B12 supplements – generic cyanocobalamin tablets can cost under $10 per month at retail; with coupons, a month’s supply may be as low as around $5.
- B12 injections – clinic prices for a shot may be anywhere from $20–$80 per injection, sometimes more at medspas. The underlying drug itself, cyanocobalamin, can be as little as roughly $4–$15 per vial when purchased with pharmacy discount programs.
- Monitoring labs – follow-up B12 tests usually follow the fee pattern mentioned earlier.
For diabetic neuropathy pain medications:
- Gabapentin – generic, often covered by most plans. A monthly supply of common doses may cost about $10–$30 with discounts, though some pharmacies list higher retail prices before coupons.
- Pregabalin (Lyrica) or brand-name options – can run $100–$500+ per month, depending on tier placement and plan rules.
- Duloxetine and other antidepressants used for neuropathy – typically mid-range, but Part D copays vary heavily by plan and tier.
For those on Medicare:
- Medicare Part B usually covers medically necessary lab tests and nerve studies with 20% coinsurance after deductible, assuming the provider accepts assignment.
- Neuropathy medications are mostly under Medicare Part D or Medicare Advantage plans with drug coverage, not Parts A or B.
- B12 injections for documented deficiency may be covered, but coinsurance and administration fees vary.
A quick, region-specific note: in many national health systems (for example parts of the UK or EU), once deficiency is documented, B12 treatment is covered with modest prescription charges or no direct patient fee, but waiting lists for nerve studies may be long. That makes it even more valuable to push for B12 testing early, before you need more complex investigations.
Money Block #4 – 2-minute mini calculator: B12-first vs meds-first path (hypothetical, 2025, US)
Scenario A – “B12-first” workup
- 1× initial B12 panel (B12 ± MMA) – say $120 total billed, $80 allowed.
- 3 months of oral B12 ($10/month) – $30.
- 2 follow-up labs over a year – $160 allowed.
Rough 1-year out-of-pocket if under deductible: about $270.
Scenario B – “Meds-first, no B12 check” path
- 1× EMG/NCS (two limbs) – say $800 billed, $500 allowed.
- 12 months of brand-name neuropathy meds at $150/month copay – $1,800.
- Extra visits for side effects and medication adjustments – say $200 allowed.
Rough 1-year out-of-pocket if under deductible and with mid-tier copays: >$2,500.
These are illustrative numbers, not a quote, but they demonstrate why checking reversible causes like B12 deficiency early can dramatically change your cost trajectory.
Save this mini-calculator and rerun it with your own deductible, copays, and pharmacy prices using your insurer’s online tools before choosing a path with your clinician.
Self-checks you can do today before your next visit
You can’t diagnose yourself at home, but you can walk into your next appointment with sharper data than “my feet feel weird.”
Try this tonight:
- Timeline check: Note the month and year you started metformin, any dose changes, and when nerve symptoms began.
- Pattern check: Are both feet involved? Is one side worse? Do hands tingle too? Is balance affected?
- Daily impact: How many minutes of sleep do you lose each night because of nerve discomfort or side-sleeping sciatica flares?
- Red flags: Any difficulty controlling bladder/bowel, sudden severe weakness, or rapidly worsening gait? Those need urgent evaluation, especially if paired with new severe low back pain that can signal a low back pain emergency.
One man who did this “homework” told me his doctor actually paused, looked at the notes, and said, “This is better than half the consult letters I get.” It also made it much easier to justify B12 testing and an EMG order to his insurer.
Show me the nerdy details
When clinicians risk-stratify neuropathy, they pay attention to tempo (acute vs chronic), distribution (length-dependent vs focal), and associated systemic signs (anemia, weight loss, autonomic symptoms). A well-documented symptom timeline can differentiate subacute B12-related changes from slowly progressive diabetic neuropathy and more urgent etiologies like Guillain–Barré syndrome or spinal cord compression, which mandate different investigations and timelines.
- Log timing, distribution, and daily impact of nerve symptoms.
- Bring medication list, including metformin dose and duration.
- Mention any falls, near-falls, or stair trouble explicitly.
Apply in 60 seconds: Create a note on your phone titled “Neuropathy + Metformin” and add three bullet points—start date, current dose, first symptom date.
How to talk to your doctor about B12, metformin, and neuropathy
Many readers tell me the hardest part isn’t the lab draw; it’s the 10-minute visit where they need to advocate without sounding like they’re second-guessing everything.
Here’s a simple script you can adapt:
“I’ve been on metformin for about X years at Y mg per day. Over the last Z months I’ve developed numbness and tingling in my feet and some balance issues. I’ve read that long-term metformin use can lower vitamin B12 and increase neuropathy risk. Could we check my B12 level and related labs, and then decide whether this is diabetic neuropathy, B12 deficiency, or both?”
If your clinician seems hesitant, you can gently add:
- “My understanding is that several diabetes guidelines now recommend periodic B12 monitoring in people on long-term metformin, especially with neuropathy or anemia. I’m worried about missing something treatable.”
- “I’m not asking to change medications today. I just want to make sure we’re not overlooking a reversible piece of this.”
For those worried about coverage tiers, premiums, and deductibles, it can also help to say:
“Since my deductible is high, could we start with the most cost-effective tests that would change the treatment plan, like B12 and a basic neuropathy workup, before we add more expensive imaging or brand-name medications?”
That signals that you’re thinking like a partner, not a challenger—someone who cares about both medical outcomes and the out-of-pocket line on the bill.
Infographic: diabetic neuropathy vs B12 deficiency at a glance
Diabetic Neuropathy vs Vitamin B12 Deficiency – Quick Comparison
Diabetic Neuropathy
- Main driver: Long-term high blood sugar.
- Typical pattern: Burning, tingling in both feet, slowly ascending.
- Key tests: A1c, fasting glucose, EMG/NCS.
- Reversibility: Often partial; focus on slowing damage.
- Core levers: Glucose control, nerve pain meds, foot care.
Vitamin B12 Deficiency
- Main driver: Poor absorption (including metformin), low intake.
- Typical pattern: Numbness, balance trouble, cognitive changes.
- Key tests: Serum B12, MMA, homocysteine, CBC.
- Reversibility: Often substantial if treated early.
- Core levers: B12 replacement, treating root cause.
In long-term metformin users, both can coexist. The job is to find out how much of your nerve story belongs to each column.
Long-term strategy for metformin users: monitoring, supplements, and dose decisions
Once you’ve answered the immediate “what’s happening to my nerves?” question, it’s time to design a calmer long-term plan—one that respects both your blood sugar and your B12.
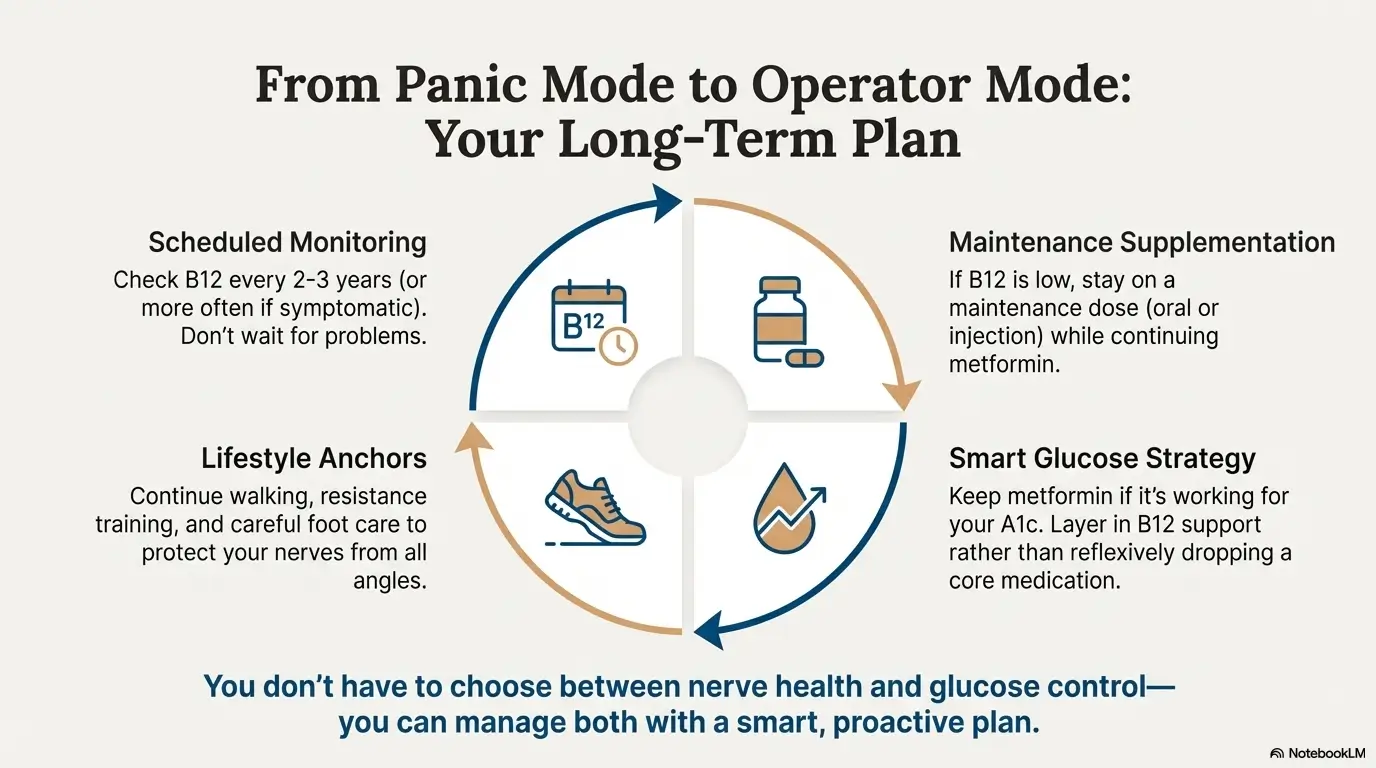
A practical, sustainable approach often includes:
- Scheduled B12 monitoring: Many experts now suggest checking B12 every 2–3 years in stable metformin users, earlier and more often if symptoms or risk factors appear.
- Maintenance supplementation: After correcting deficiency, some people stay on a lower-dose oral B12 regimen or intermittent injections while continuing metformin.
- Glucose strategy: Continue to use metformin as foundational therapy if tolerated, adding or adjusting other agents as needed rather than dropping it reflexively.
- Lifestyle anchors: Walking, resistance training, and careful foot care reduce ulcer risk and may modestly improve neuropathy symptoms over time.
I like to think of it as moving from panic mode (“My feet are on fire; something is wrong with my meds!”) to operator mode (“Every 24 months we check B12, A1c, kidney function, and feet; if something drifts, we adjust the plan.”).
- Keep metformin on the table if it’s working.
- Layer in B12 monitoring and supplementation as needed.
- Use structured follow-up to avoid “silent drift” in either direction.
Apply in 60 seconds: Add a recurring reminder to your calendar for a “metformin + B12 + foot check” review every 2 years, then discuss the timing with your clinician.
FAQ
1. If my B12 is “normal,” can I still have neuropathy from metformin?
Yes. “Normal” reference ranges are wide, labs differ, and some people have symptoms at low–normal values, especially if B12 has dropped quickly from a higher baseline. Borderline results sometimes prompt additional tests like MMA and homocysteine or a trial of B12 replacement. A single lab number should be interpreted in the context of your symptoms, exam, and metformin history.
60-second action: Ask your clinician what your actual B12 number is, what range the lab uses, and whether additional testing is worthwhile.
2. How long does it take for B12 treatment to improve nerve symptoms?
For many people, energy and mood improve first, often within weeks. Nerve symptoms are slower: tingling may ease over several months, while balance and gait changes can take six to twelve months to plateau. If neuropathy has been present for years, full reversal is less likely, but stabilisation or partial improvement is still a win.
60-second action: When you start treatment, jot down a “baseline” description of your symptoms; revisit it at 3 and 6 months to track real changes rather than relying on memory.
3. Will checking B12 and getting EMG covered be hard with my insurance?
Most insurers and Medicare plans cover B12 testing and EMG when there’s a clear clinical indication: documented neuropathy symptoms, anemia, long-term metformin use, or neurologic findings on exam. Prior authorization sometimes enters the picture for more expensive imaging or brand-name neuropathy medications, not usually for basic labs.
60-second action: Call the member services number on your insurance card and ask, “What is my deductible and typical coinsurance for lab tests and EMG?” Note the CPT codes if your clinic provides them.
4. Is it safe to take over-the-counter B12 while I wait for testing?
For most people without severe kidney disease, over-the-counter B12 is considered low-risk because excess is usually excreted in urine. However, self-treating without testing can blur the picture—if you start high-dose B12 before labs, it may normalise levels and make it harder to know how deficient you were. It’s usually better to discuss this explicitly with your clinician, especially if you have complex health conditions.
60-second action: If you’re already taking B12, tell your clinician the exact dose and when you started; don’t hide it to “keep the labs clean.”
5. What if my doctor dismisses my concerns about metformin and B12?
Clinicians are busy and not all of them have internalised the latest safety updates yet. You can calmly reference long-term metformin’s documented link with B12 deficiency and neuropathy, mention current guideline recommendations for periodic B12 monitoring, and—if needed—request a second opinion. It’s your body and your nerve function, and you’re allowed to care about both outcomes and costs.
60-second action: Bring a short written summary (one page) with your symptom timeline and metformin history; hand it over at the start of the visit so the conversation begins with clear facts.
Conclusion and 15-minute next steps
Let’s close the loop on the question you started with: Is this diabetic neuropathy or vitamin B12 deficiency from long-term metformin—and what can I do about it without wrecking my finances?
In reality, many long-term metformin users with neuropathy sit in the overlap: some damage from years of high glucose, some from slowly falling B12, some from other contributors like age, diet, or co-medications. The win is not in proving that only one cause exists; it’s in finding and fixing the pieces that are still fixable, especially B12 deficiency and uncontrolled blood sugar.
In the next 15 minutes, you can:
- Make a one-page summary of your metformin history, nerve symptoms, and daily impact.
- Check your insurance portal or call member services to learn your current deductible and likely coinsurance for lab tests and EMG.
- Book an appointment (or send a portal message) asking specifically to discuss neuropathy, B12 testing, and metformin together.
If you do those three things, you’ve already shifted from passive passenger to thoughtful operator in your own care—someone who understands that lab tests are not abstract numbers but tools to protect your nerves, your independence, and, yes, your bank account.
Last reviewed: 2025-12; information reflects recent diabetes care standards, medicines safety updates on metformin and vitamin B12, and contemporary studies on neuropathy and long-term metformin use.
