
Beyond the Fabric: A Strategic Guide to Compression Gloves
“You buy the gloves because your hands have started arguing with ordinary objects: jars, toothbrushes, coffee mugs, even the tiny zipper on a jacket that now behaves like a locked vault.”
The quiet truth about orthopedic pain management is simple: the glove only works if you give it the right job. Whether it’s morning stiffness, typing fatigue, or post-chore puffiness, guessing can lead to increased swelling or delayed care.
This guide helps you navigate when to choose compression, when to opt for a splint, and how to prioritize function over wishful thinking.
Table of Contents
Fast Answer
Compression gloves may help some people with arthritis manage hand pain, stiffness, warmth needs, and mild swelling, but they are not a cure and should not replace diagnosis, hand therapy, medication guidance, or splinting when joint support is needed. The safest approach is to treat gloves as one small tool inside a broader orthopedic pain plan: fit, timing, skin checks, activity changes, exercises, and clear stop signs.
- They may help with warmth, mild pressure, and routine.
- They do not replace diagnosis, splints, therapy, or medication advice.
- They should come off if they cause numbness, color change, or deep marks.
Apply in 60 seconds: Choose one painful hand task and ask, “Do I need comfort, support, less grip force, or medical help?”
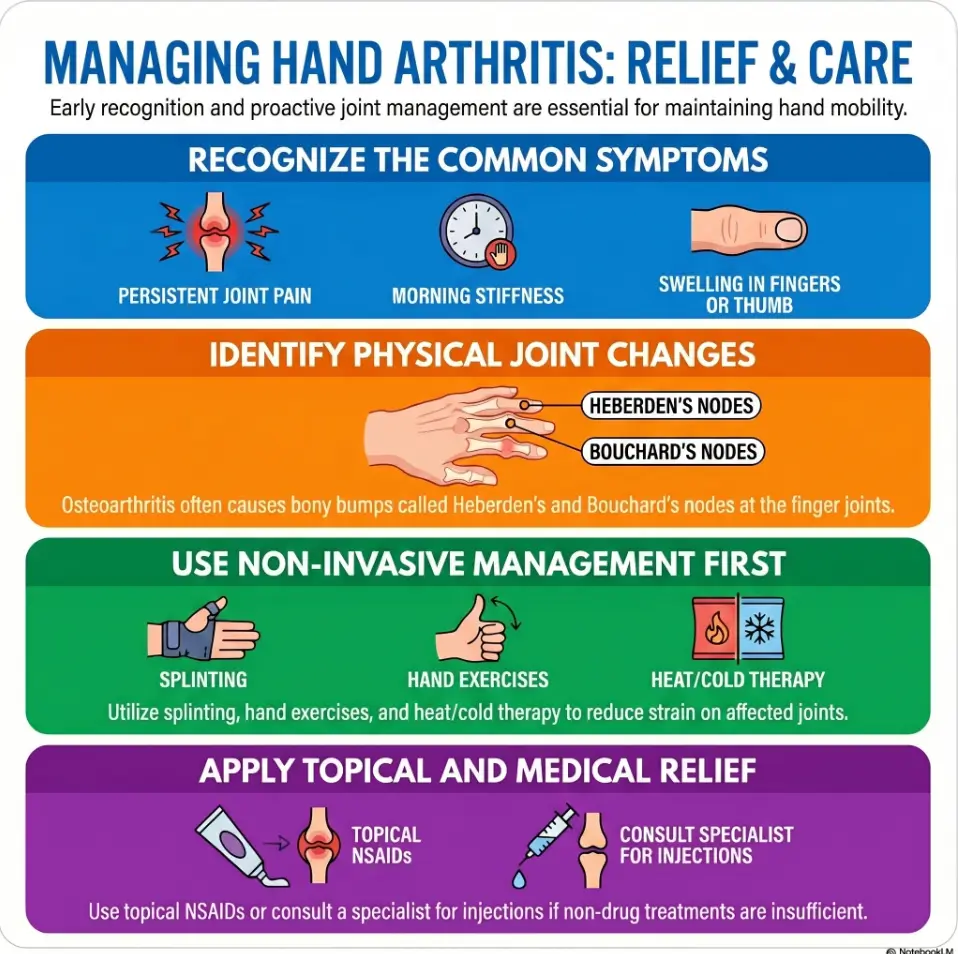
Safety / Disclaimer: Gloves Can Soothe, But They Cannot Diagnose
Compression gloves can feel reassuring. A little warmth, a little hug around the knuckles, a little less morning “tin robot hand.” That comfort matters. Pain is not improved by moral lectures or heroic suffering.
But gloves cannot tell you why your hand hurts. Hand arthritis can come from osteoarthritis, rheumatoid arthritis, post-traumatic joint damage, inflammatory disease, tendon problems, nerve compression, and other causes. The American Academy of Orthopaedic Surgeons explains that hand arthritis may affect everyday tasks such as gripping, tying, and opening objects, and treatment depends on the joints involved, disease progression, activity level, medical conditions, and personal goals.
What compression gloves may reasonably do
They may provide mild compression, warmth, sensory feedback, and a reminder to move more gently. Some people find that gloves make morning stiffness less dramatic or make typing and light chores feel more tolerable.
Think of them as a dimmer switch, not a breaker box. They may turn down discomfort. They do not rewire the whole house.
What compression gloves should never be asked to do
They should not be used to push through severe pain, hide swelling that is getting worse, replace prescribed medication, or support an unstable joint that needs a brace or splint. They also should not be worn over broken skin, infection, unexplained redness, or fingers that are cold, blue, numb, or tingling.
Why “arthritis hand pain” still needs the right diagnosis
Osteoarthritis and rheumatoid arthritis can both affect the hands, but they are not the same story in different shoes. Rheumatoid arthritis may need disease-directed medical care. Osteoarthritis often leans heavily on symptom management, joint protection, hand exercises, splints, and load reduction. If the diagnosis is fuzzy, the plan becomes fuzzy too.
- Sudden swelling or heat deserves medical attention.
- Numbness, tingling, or color change means the glove should come off.
- Persistent function loss deserves a clinician or hand therapist.
Apply in 60 seconds: Look at both hands side by side and note color, swelling, temperature, and finger motion before putting gloves on.
Start Here: Compression Is Comfort, Not a Full Pain Plan
The biggest mistake is asking a $15 to $40 glove to do a whole medical team’s job. It is tempting. A glove is simple. Arthritis is not. The glove arrives in the mail. Your hand still has history, mechanics, inflammation, habits, and a suspicious relationship with pickle jars.
The glove is not the hero
The hero is the plan. The glove is a supporting character with decent lighting. A good plan asks what hurts, when it hurts, what task triggers it, what joint is involved, and whether the hand needs pressure, warmth, support, reduced load, or medical treatment.
I once watched someone put on compression gloves before opening a stubborn pasta sauce jar. The gloves did their best. The jar did not care. A rubber jar opener and a larger grip would have helped more. That tiny scene is the whole article in miniature.
Why warmth, light pressure, and routine may feel helpful
Warmth can make stiff hands feel less hostile. Light pressure may feel calming when swelling is mild. A consistent routine can also reduce the mental tax of deciding what to do every morning. Pain loves chaos. Routine politely locks the side door.
The missing question: what task hurts most?
Do not start with “Which glove is best?” Start with the daily task that hurts most. Is it opening jars? Buttoning? Typing? Holding a steering wheel? Using a phone? Cutting vegetables?
That task tells you whether the better answer is a glove, a splint, a larger handle, pacing, heat, exercises, medication guidance, or a hand therapy visit. The same task-first thinking also matters when families compare orthopedic home care equipment, because the useful tool is the one that reduces the repeated painful moment, not the one with the most impressive product page.
Mini Infographic: The Hand Pain Sorting Map
Try warmth, gentle motion, possibly gloves.
Use caution. Check fit and ask if pressure helps or irritates.
Consider splint support, not just fabric compression.
Remove glove and seek medical guidance.
Who This Is For, and Who It Is Not For
Compression gloves make the most sense when symptoms are mild to moderate, predictable, and mostly related to stiffness, aching, warmth needs, or light swelling. They are less convincing when the problem is sharp instability, severe deformity, nerve symptoms, or pain that keeps rewriting the rules.
Good fit: stiff morning fingers, mild swelling, achy hands after use
If your hands need 15 to 30 minutes to wake up, gloves may become part of a gentle morning ritual. Put them on, sip coffee, do a few easy motions, and let your hands enter the day without being shouted at by a cold kitchen counter.
They may also help after light activity, especially when the hand feels tired and puffy rather than acutely injured.
Maybe not enough: unstable thumb, severe deformity, night-waking pain
Thumb-base arthritis often needs more than cozy fabric. If the thumb collapses during pinching, opening containers, or turning keys, a brace or splint may reduce stress better than a glove. Severe deformity or pain that wakes you repeatedly should not be filed under “normal aging” and left in a drawer with old batteries.
Not for this moment: numb, blue, cold, infected, or suddenly swollen fingers
Do not wear compression gloves over infected skin, open wounds, or unexplained sudden swelling. Remove them if fingers become numb, tingly, pale, blue, unusually cold, or more painful.
Let’s be honest: “I bought gloves” is not the same as “I have a plan”
A plan has timing, fit checks, task changes, and stop signs. A purchase has a tracking number. Both can be useful, but only one keeps you from blaming your hands when the setup is the problem. For older adults, that plan may need to fit inside a broader senior orthopedic pain management routine where hand comfort, fall risk, medication timing, and daily function all share the same kitchen table.
Eligibility Checklist: Are compression gloves worth a careful trial?
- Yes if your symptoms are mild, familiar, and mostly stiffness or aching. Next step: try a measured fit for short periods.
- Yes if mild swelling comes and goes without color change or numbness. Next step: inspect skin before and after use.
- No, not yet if symptoms are sudden, severe, hot, red, numb, or blue. Next step: seek medical guidance.
- Maybe if thumb-base pain is the main issue. Next step: compare glove comfort with splint support.
Neutral action: Write down your top 1 hand complaint before shopping.
Pain Pattern First: Match the Glove to the Moment
Arthritis hand pain is not one note. It is a small, badly rehearsed orchestra: morning stiffness in the violins, swelling in the brass, thumb pain banging a cymbal near the jar opener.
Morning stiffness: use gloves as a warm-up cue
If morning stiffness is the problem, gloves can become a cue for a low-force first hour. That means no heroic jar opening before breakfast. No cold steering wheel death grip. No “I will just quickly scrub this pan” while the kettle is still boiling.
Try wearing gloves for a short morning window while doing gentle finger bends, thumb circles, and light daily tasks. The goal is not to force range of motion. The goal is to invite it back into the room.
After-use aching: watch the delayed pain window
AAOS describes early hand arthritis pain as often appearing after heavy gripping or grasping, sometimes hours later or the next day, with morning pain and stiffness also common. That delayed window matters. If your hand hurts at 9 p.m., the cause may have been the 2 p.m. gardening session, not the innocent spoon currently in your hand.
Swelling days: check whether pressure helps or irritates
Mild compression may feel good on some swelling days. On other days, pressure can feel like a committee meeting in a tiny room. Try shorter sessions and check whether the hand feels calmer or more crowded after 20 to 30 minutes.
Night pain: don’t assume tighter means better
Night pain is tricky because sleep hides feedback. A glove that seems fine at 10 p.m. may leave deep marks by 3 a.m. If nighttime use is even on the table, it should be comfortable, mild, and preferably discussed with a clinician, especially if you have diabetes, nerve symptoms, circulation concerns, or fragile skin.
Show me the nerdy details
Compression, warmth, and sensory feedback may change how the hand feels during certain tasks, but the research picture is mixed. Some trials have found limited added benefit compared with looser gloves, especially for inflammatory arthritis. That does not mean nobody feels better. It means gloves should be tested against real function, not assumed to be a universal fix.
The Fit Trap: Why “Snug” Can Become a Small Disaster
Compression gloves should feel supportive, not like your fingers are being interviewed by airport security. Fit is where many people quietly lose the plot. Too loose, and the glove is just a hand sweater. Too tight, and it can irritate skin, worsen tingling, or leave pressure marks that look like tiny railroad tracks.
Correct fit should feel supportive, not strangling
A good fit allows comfortable finger motion, normal color, and no numbness. You should be able to type, hold a cup, and lightly bend your fingers. If you feel pulsing, prickling, coldness, or a strong urge to rip them off, listen to the hand. It has filed a complaint.
Finger seams, wrist cuffs, and pressure marks matter
Finger seams can rub bony joints. Wrist cuffs can dig into tender skin. A glove may fit the palm but squeeze the knuckles, or fit the fingers but bunch at the thumb web. The hand is not a rectangle. Product sizing sometimes forgets this and smiles anyway.
Remove the gloves and inspect the skin
For the first week, remove the gloves after short sessions and check skin. Look for deep grooves, red patches that do not fade, irritation between fingers, swelling beyond the glove edge, or color changes.
Don’t do this: sleeping in gloves that leave deep marks
Deep marks are not proof the glove is working harder. They are proof your skin and circulation may be annoyed. Especially for older adults or people with diabetes, neuropathy, fragile skin, or carpal tunnel symptoms, skin checks are not optional decoration.
Mini Calculator: Glove Fit Risk Check
Choose your answers, then check fit risk.
Neutral action: Use this before deciding a glove is “working.”
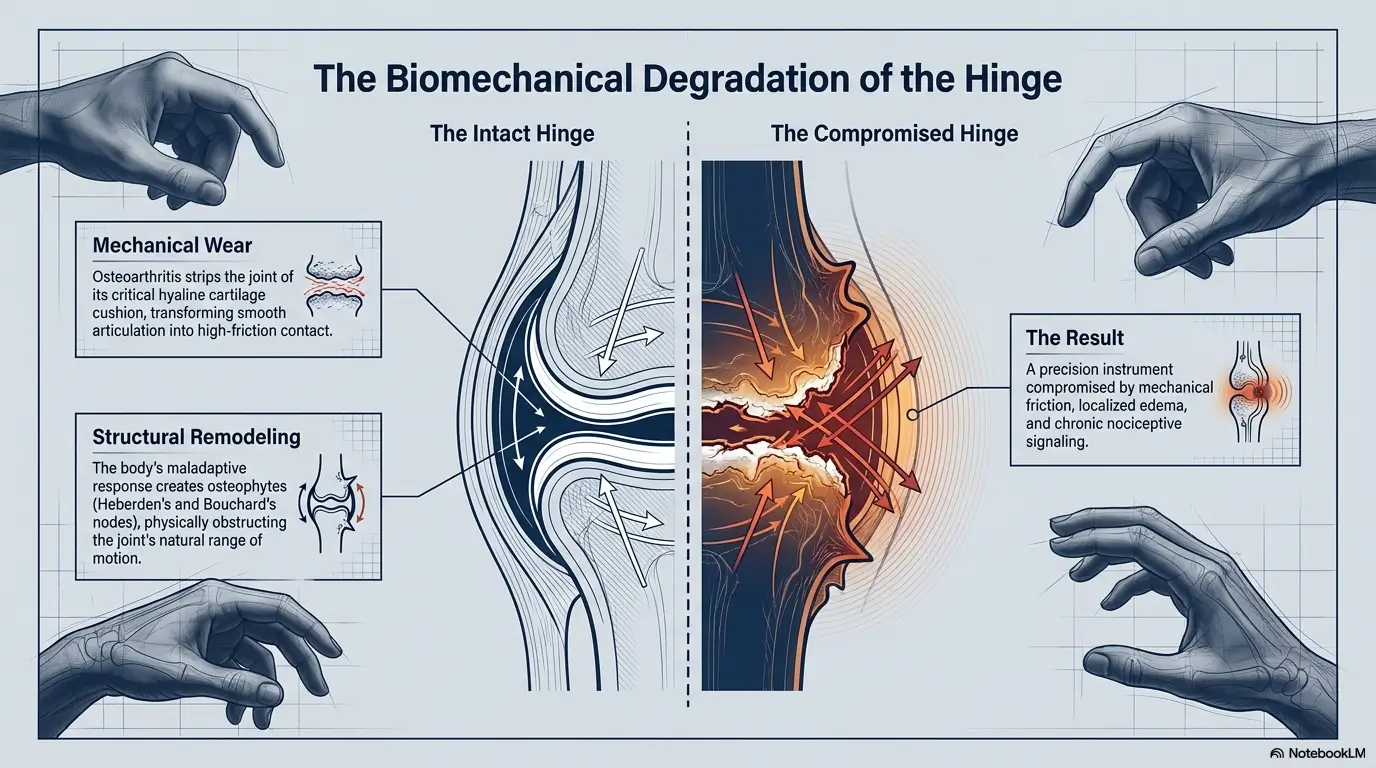
Compression Gloves vs Splints: They Are Not Interchangeable
A glove and a splint may live in the same drawer, but they do different jobs. Confusing them can lead to a familiar disappointment: the glove feels nice, the joint still gets bullied by the task, and the person concludes nothing helps. That is unfair to the hand and the drawer.
Gloves offer pressure and warmth
Compression gloves mainly offer mild pressure, warmth, and a sense of support. They may make the hand feel more awake or contained during light tasks. They do not strongly control joint alignment.
Splints limit motion and reduce stress on painful joints
AAOS lists splinting among nonsurgical treatment options for hand and wrist arthritis and explains that splints may limit motion and reduce pain by supporting the affected joint. The caution is that splints should be used thoughtfully, because overuse can contribute to stiffness or weakness. This is where a hand therapist earns their cape, even if it looks like a sensible cardigan.
Thumb-base pain may need support, not just fabric
Thumb-base arthritis is a classic example. If pain spikes during pinching, opening jars, writing, or turning keys, a thumb brace may reduce joint stress more directly than compression gloves. The glove can comfort the neighborhood. The splint may protect the address.
Here’s what no one tells you: soft comfort can hide poor mechanics
If the painful task still demands a high-force pinch, narrow grip, or awkward wrist angle, gloves may simply make the mistake feel nicer. That is not nothing, but it is not enough. If cost or reimbursement is part of the decision, it may also be worth reviewing how HSA-eligible braces and supports can fit into a practical orthopedic pain plan.
Decision Card: Compression Gloves vs Splints
- You want warmth or mild pressure.
- Symptoms are mild and familiar.
- You need finger mobility for light tasks.
- A joint feels unstable.
- Thumb-base pain dominates.
- Motion itself triggers sharp pain.
Neutral action: Match the tool to the job: comfort for gloves, alignment and motion control for splints.
Build the Orthopedic Pain Stack: Gloves + Hands + Habits
The most useful hand arthritis plan is usually not glamorous. It is a stack of small, boring, effective choices. Gloves may sit in the stack, but they should not be the whole tower.
Hand exercises keep motion in the room
A 2025 review in Rheumatology Advances in Practice emphasizes non-drug strategies for hand osteoarthritis, including education, hand exercises, splinting, joint protection, and offloading before relying mainly on medication. That phrasing matters. It puts daily mechanics back on the table.
Gentle range-of-motion work can help preserve movement, but painful forcing is not the assignment. Good hand exercise feels more like oiling a hinge than proving a point to a stubborn door.
Offload small grips before blaming inflammation
Small objects often demand more grip force. Larger or built-up handles can reduce strain because the hand does not need to clamp as hard. This applies to toothbrushes, pens, utensils, garden tools, steering wheel covers, and kitchen gadgets.
I have seen a $2 foam grip outperform a fancy glove for morning toothbrushing. The glove comforted the hand. The foam handle changed the workload.
Use heat or cold carefully, especially with sensation problems
Heat may help stiffness and comfort. Cold may help some swelling or post-activity soreness. But people with reduced sensation, diabetes, nerve compression, or fragile skin need extra caution. Burns and ice injuries do not announce themselves politely.
- Use larger handles where grip force is high.
- Break repeated tasks into shorter blocks.
- Use gloves for comfort, not as permission to overdo it.
Apply in 60 seconds: Wrap a towel around one hard-to-grip handle and test whether your hand relaxes.
Short Story: The Jar That Taught the Lesson
A woman I know kept a pair of compression gloves beside the fruit bowl. Every evening she put them on before making dinner, convinced she was “preparing” her hands. But the real villain was a squat glass jar with a lid that behaved like it had a personal grudge.
She would grip harder, twist harder, then spend the evening wondering why her thumb ached. The fix was almost embarrassingly plain: a rubber jar opener, a small electric opener for bad days, and moving heavy jars to a waist-height shelf. The gloves still stayed in the kitchen. But they were no longer asked to fight the jar dragon alone.
Common Mistakes: Tiny Choices That Make Hand Pain Louder
Hand pain often gets louder through ordinary choices that seem too small to matter. The problem is that hands do hundreds of small jobs a day. A tiny strain multiplied by 80 repetitions becomes less tiny. Mathematics, sadly, has no bedside manner.
Writing the pain story too late
Many people only notice the hand when it is furious. By then, the useful clue may be gone. Was it the phone? The pan? The laundry basket? The steering wheel? The 40-minute scrolling session with the thumb curled like a shrimp?
Common glove mistakes to avoid
- Wearing gloves all day without skin breaks: skin needs inspection and air.
- Buying by small, medium, large without measuring: hands vary more than product charts admit.
- Using gloves during messy, wet, or high-friction chores: damp fabric can rub and irritate.
- Treating copper, magnets, or special fibers as magic: comfort may help, but extraordinary claims need caution.
- Ignoring the jar, phone, toothbrush, and steering wheel problem: task design often matters more than fabric.
Waiting until the hand is furious before changing the task
Change the task earlier. Use two hands. Slide instead of lift. Choose a larger grip. Pause before the ache becomes a weather system. A 2-minute adjustment at noon may prevent a 2-hour complaint at night. If the same pain pattern keeps returning despite sensible changes, the issue may need a broader look at what to do when physical therapy is not helping orthopedic pain or when the current plan no longer matches the problem.
Quote-Prep List: What to gather before comparing gloves or braces
- Your hand measurements from the brand’s sizing guide.
- Your main painful task, such as typing, jars, driving, or gardening.
- Whether you need fingerless, full-finger, wrist coverage, or thumb support.
- Return policy details, especially if you are between sizes.
- Any medical cautions: diabetes, neuropathy, skin fragility, circulation issues, or carpal tunnel symptoms.
Neutral action: Gather these before comparing products so the purchase follows the problem.
Daily Routine: A Gentle Glove Schedule That Makes Sense
The best glove schedule is not heroic. It is boring in the way a good seatbelt is boring. It shows up, does a job, and does not require a dramatic soundtrack.
Morning: warmth, motion, and a low-force first hour
Start with short wear. Try 20 to 60 minutes while your hands warm up and you move through gentle tasks. Avoid high-force gripping early if morning stiffness is your main pattern.
A good morning rule: no jars, no pliers, no “quickly rearranging the garage” before breakfast. The hand has not even had coffee.
Midday: remove, inspect, reset
Take the gloves off and look at your skin. Check pressure marks, irritation, swelling at the glove edge, and finger color. Move the fingers gently. Ask whether the gloves made function easier or just made the discomfort feel less lonely.
Evening: use gloves after activity, not as punishment for activity
If hands ache after use, try gloves during a recovery window. Pair them with rest from high-force tasks. Do not use them as permission to keep chopping, scrubbing, pruning, knitting, or typing through worsening pain.
Night: only if comfortable, safe, and clinician-approved
Night use is not automatically wrong, but it deserves caution. If you have numbness, tingling, diabetes, neuropathy, circulation problems, fragile skin, or unexplained swelling, ask a clinician before sleeping in compression gloves. Your sleeping self is not an ideal safety inspector.
- Start with short sessions.
- Inspect skin after use.
- Stop if symptoms worsen.
Apply in 60 seconds: Set a 30-minute timer the first time you test a new pair.
When to Seek Help: Stop Guessing When the Hand Changes the Rules
Some hand changes should not be managed by online shopping and optimism. Compression gloves are not emergency equipment. They are not a diagnosis machine. They are definitely not a tiny knitted physician.
Sudden swelling, redness, heat, or severe pain
Sudden swelling, hot joints, redness, severe pain, or pain after injury deserves medical attention. These symptoms may point to inflammation, infection, fracture, gout, tendon problems, or other issues that need more than a glove. When symptoms feel urgent but not obviously life-threatening, comparing urgent care vs an orthopedic clinic can help you choose the safer next door to knock on.
Numbness, tingling, color change, or cold fingers
Remove the glove if your fingers become numb, tingly, pale, blue, or cold. These are not “break-in” symptoms. They are stop signs wearing tiny gloves of their own.
New weakness, dropping objects, or loss of function
If you are suddenly dropping objects, losing pinch strength, or avoiding ordinary tasks, get evaluated. Function tells the truth faster than pain scores. A hand that cannot button, grip, write, cook, or carry safely is asking for a better plan.
Pain that keeps waking you up
Night-waking pain deserves attention, especially if it is new, worsening, or paired with numbness, swelling, fever, or unexplained weight loss. Do not let “arthritis” become the junk drawer label for every new symptom.
A glove that makes symptoms worse
If gloves increase pain, swelling, tingling, stiffness, or skin irritation, stop using them. A product that worsens function is not failing because you are using it with insufficient enthusiasm. It may simply be the wrong tool.
Arthritis that is spreading, flaring often, or no longer predictable
AAOS advises seeking help early for hand arthritis so treatment can begin and function can be preserved. Nonsurgical options may include medication, splinting, activity modification, injections, ice or heat, and, when needed, surgery.
Buying Without Regret: What to Check Before You Click “Add to Cart”
Compression gloves look simple until you try to buy them. Fingerless or full-finger? Cotton blend or nylon? Copper? Wrist cuff? Thumb support? The shopping page becomes a small carnival with too many promises and not enough measuring tape.
Measure the hand, not your optimism
Use the brand’s sizing instructions. Measure around the knuckles or palm exactly where the company requests. If you are between sizes, check reviews for fit patterns and prioritize return policies. Arthritis hands often dislike wishful sizing.
Choose fingerless vs full-finger based on task
Fingerless gloves preserve touch for typing, phone use, cooking prep, and small objects. Full-finger gloves may feel warmer, but they can reduce tactile feedback. If you already drop items, reduced sensation may be a bad trade.
Look for breathable fabric and washable construction
Hands sweat. Creams transfer. Kitchen life happens. A glove that cannot be washed easily may become a tiny fabric swamp. Breathable, washable materials matter more than dramatic product language.
Prioritize return policy over miracle claims
“Copper,” “infrared,” “magnetic,” and similar claims may sound exciting, but comfort, fit, and function are the practical tests. A plain glove that fits safely beats a glamorous glove that squeezes your fingers into Morse code.
The quiet test: can you still button, type, and hold a cup?
After trying gloves, test three simple tasks: buttoning, typing or texting, and holding a cup. If function drops, the glove may be wrong for active use even if it feels cozy during rest. This same “function before gadget” logic also applies to larger orthopedic braces and supports, where the best purchase is usually the one that solves a specific movement problem safely.
Coverage Tier Map: What changes as support increases
| Tier | Tool | Best For | Trade-Off |
|---|---|---|---|
| 1 | Warm regular gloves | Cold sensitivity | Little compression |
| 2 | Compression gloves | Mild stiffness or swelling | Fit must be watched |
| 3 | Thumb or wrist brace | Joint stress or instability | Less motion |
| 4 | Hand therapy plan | Function loss or recurring pain | Requires appointments and practice |
| 5 | Medical procedures or surgery discussion | Severe cases not controlled conservatively | Needs individualized medical decision-making |
Neutral action: Start at the lowest tier that matches the problem, then escalate when function still suffers.
Next Step: Run a 7-Day Hand Pain Field Test
The cleanest way to judge compression gloves is not by vibes. Vibes are charming but unreliable. Use a simple 7-day field test. You are not running a laboratory. You are building a small map of your own hand.
Pick one painful task, not your whole life
Choose one task: morning typing, opening jars, holding a steering wheel, folding laundry, cooking prep, writing, gardening, or phone use. One task keeps the test honest. Testing your entire life creates fog.
Track pain, stiffness, swelling, and function
Use a 0 to 10 pain rating, but do not stop there. Track stiffness time, swelling, and function. Could you button a shirt? Hold a cup? Open a container? Type for 20 minutes? Function is where the truth puts on work boots.
Compare glove days with non-glove days
Try the glove during the same task on some days and skip it on others. Keep the task similar. Do not compare “gloves during gentle email” with “no gloves during six hours of yard work” unless you enjoy bad data wearing a garden hat.
Bring the notes to a clinician or hand therapist
If symptoms continue, your notes can make an appointment more useful. Instead of saying “my hand hurts,” you can say “typing is okay for 15 minutes, jars trigger thumb pain, swelling is worse by evening, and gloves help warmth but not pinching.” That is a much better starting point. Good notes can also support a more focused visit, whether you are preparing for telehealth vs in-person orthopedics or deciding whether the hand really needs a more detailed exam.
- Pick one task.
- Track symptoms before and after.
- Compare glove and non-glove days fairly.
Apply in 60 seconds: Write today’s task, pain score, stiffness time, and whether the glove helped or hurt.

FAQ
Do compression gloves actually help arthritis pain?
They may help some people, especially when pain is linked to mild swelling, warmth needs, or morning stiffness. Evidence is mixed, so the practical test is whether gloves improve your specific function without causing numbness, skin problems, or worse pain.
How tight should arthritis compression gloves be?
They should feel snug and supportive, not tight or restrictive. Your fingers should stay warm, normally colored, and comfortable. Remove the gloves if you notice tingling, numbness, cold fingers, blue or pale color, deep marks, or increasing pain.
Can I sleep with compression gloves on?
Some people do, but nighttime use needs caution because you may not notice pressure problems while asleep. Avoid sleeping in gloves if you have numbness, circulation problems, diabetes-related sensation changes, fragile skin, or unexplained swelling unless a clinician says it is appropriate.
Are compression gloves better than a hand splint?
No. They do different jobs. Compression gloves provide mild pressure and warmth. Splints or braces can limit motion and support painful joints. Thumb-base pain, instability, or sharp pain with motion may need splint support rather than fabric compression alone.
Should I wear compression gloves for rheumatoid arthritis or osteoarthritis?
People with either condition may try gloves for comfort, but rheumatoid arthritis and osteoarthritis require different medical strategies. If you have inflammatory flares, spreading swelling, or changing symptoms, do not rely on gloves alone. Get medical guidance.
Can compression gloves make numbness or tingling worse?
Yes, especially if they are too tight or if you already have nerve compression, carpal tunnel symptoms, neuropathy, or circulation issues. Numbness and tingling are reasons to remove the gloves and reassess.
Are copper compression gloves worth it?
Copper gloves may feel comfortable if the fit and fabric work for you, but copper itself should not be treated as a proven arthritis cure. Judge them by comfort, safe fit, washability, return policy, and whether your hand function improves.
How long should I try compression gloves before deciding?
A 7-day task-based trial is usually more useful than one random day. Track one task, wear time, pain, stiffness, swelling, and function. Stop sooner if symptoms worsen or your skin reacts.
Should I use heat, ice, or gloves for swollen arthritis hands?
It depends on the pattern. Warmth may help stiffness. Cold may help some post-activity soreness or swelling. Compression may or may not feel good on swelling days. Use caution with temperature if you have reduced sensation, diabetes, neuropathy, or fragile skin.
Conclusion
The little square of fabric on your hand is not the whole answer. That is the curiosity loop we opened at the beginning: why can a glove feel helpful and still fail at the task you bought it for?
Because arthritis pain is rarely just “pain.” It is stiffness at 7 a.m., thumb stress at the jar, swelling after overuse, a phone grip that quietly annoys the joints, a toothbrush handle too thin for the day’s hand, and sometimes a medical condition that needs more than comfort.
Compression gloves can belong in orthopedic pain management with compression gloves for arthritis, but they belong as one tool in a stack: diagnosis, fit, skin checks, hand exercises, offloading, splints when needed, medication guidance when appropriate, and clear stop signs. If the pattern becomes confusing, persistent, or more medical than mechanical, the next question may not be “which glove?” but whether to compare a pain clinic vs an orthopedist for the kind of help your hand is actually asking for.
Within the next 15 minutes, do this: pick one painful task, measure your hand if you are shopping, and write a 7-day trial note with pain, stiffness, swelling, and function. Your hands do not need a grand speech. They need a calmer workload, a safer fit, and a plan that does not ask fabric to perform miracles.
Last reviewed: 2026-04.
