L5/S1 Selective Nerve Root Block for Sciatica: What Happens on Procedure Day, Risks, and Real-World Costs
I thought my first sciatica injection would be a simple shot. What surprised me was the hidden complexity: the drive-home rules, the sedation fork, the insurance wording, and the way one targeted decision can change the entire treatment map.
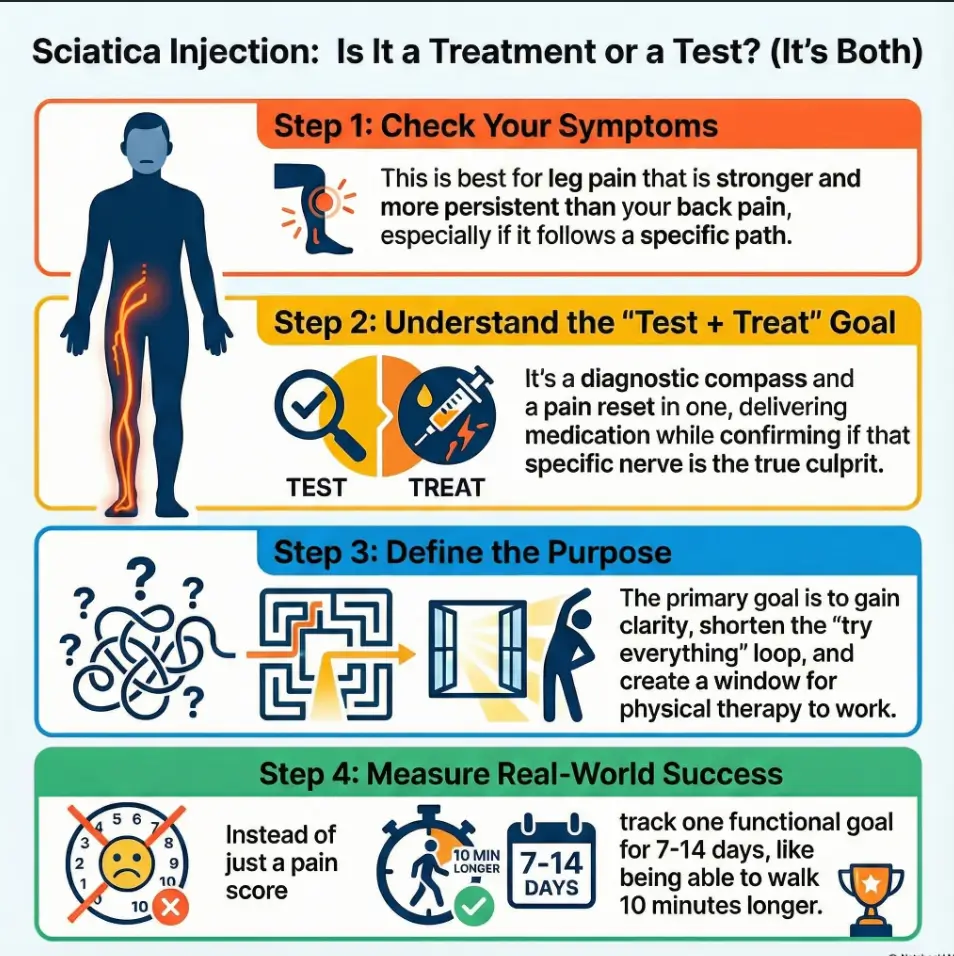
An L5/S1 selective nerve root block for sciatica is a guided injection placed near a specific nerve root to reduce inflammation and, just as importantly, confirm whether that root is truly driving your leg pain. That “test + treat” dual purpose is why it’s often recommended when symptoms are pattern-specific but your next step still feels uncertain.
Keep guessing and you can lose weeks to the wrong rehab plan, the wrong injection type, or the wrong level of focus.
This guide is designed to help you walk into procedure day with a clean plan, understand the real risks without doom-scrolling, and estimate out-of-pocket costs before you’re surprised by a facility bill.
I’m approaching this the way a time-poor patient has to: as one integrated decision—experience, safety, and money.
No fluff.
No panic.
Just a smarter next move.
- Know if your symptoms fit L5 vs S1
- Understand what the injection is likely to feel like
- Get a practical insurance and cost checklist
Table of Contents
Why L5/S1 matters when sciatica gets specific
Sciatica is often described like a single highway of pain, but it’s more like a multi-exit interchange. The L5 and S1 nerve roots supply slightly different territories of sensation and strength. When your symptoms are precise—pain down the side of the leg into the top of the foot, or down the back of the calf into the sole—your clinician may want a targeted test-treatment combo rather than a broad “spray and hope” approach.
That’s the logic of a selective nerve root block: deliver medication close to a specific nerve root to reduce inflammation and, just as importantly, confirm whether that root is truly the villain in your story.
- Diagnostic value: helps pinpoint a pain generator when imaging and symptoms don’t fully line up.
- Therapeutic value: may reduce pain enough to let rehab finally work.
- Time value: can shorten the “try everything for months” loop by weeks.
My own small wake-up moment was realizing this wasn’t just an injection—it was a decision about information. I wasn’t only paying for relief. I was paying for clarity.
- It can confirm L5 vs S1 involvement
- It may buy time for rehab to stick
- It’s most useful when symptoms are pattern-specific
Apply in 60 seconds: Write your pain map from hip to toes before your consult.
Who this injection is for—and who should pause
This procedure is usually considered when conservative care hasn’t fully broken the cycle. That might mean a few weeks of persistent leg-dominant pain despite activity modification, physical therapy, or medication. It’s especially common when your MRI shows a plausible culprit at L4-L5 or L5-S1, but the clinical picture still needs confirmation—particularly if you’re weighing whether this looks more like sciatica vs a herniated disc in real-world function.
Time-poor reality:
Quick fit signals
- Your leg pain is stronger than your back pain.
- Your symptoms follow an L5 or S1 distribution that a clinician can test.
- You need clearer diagnostic direction before considering surgery.
Reasons to slow down
- Uncontrolled diabetes or active infection.
- New bowel/bladder changes or rapidly worsening weakness.
- Blood thinner questions that haven’t been reconciled with your prescribing clinician.
I once wanted the injection simply because I was exhausted. That’s a human reason—but not always the best medical one. The better reason is that the block can help you choose your next step with fewer guesses, including ruling in or out overlaps like diabetic neuropathy vs sciatica.
- Leg-dominant pain lasting roughly 3–6+ weeks despite guided care
- Neurologic exam suggests L5 or S1 involvement
- Imaging shows a plausible correlate at the matching level
- No red-flag infection signs or unstable medical conditions
- Anticoagulant plan reviewed with your care team
Next step: If you checked 3+ items, ask your clinic whether the goal is diagnostic clarity, pain relief, or both.
Neutral action: Save this list and confirm your clinic’s criteria before scheduling.
Procedure day timeline for an L5/S1 selective nerve root block, 2025 (US)
Procedure day isn’t hard, but it’s oddly easy to get wrong in ways that waste time and money. The main friction points are fasting rules (if sedation is involved), medication instructions, and the “who’s driving you home?” puzzle.
What a typical timeline looks like
- Arrival:
- Vitals + brief exam:
- Positioning:
- Local anesthetic:
- Needle placement + contrast:
- Medication delivery:
- Observation:
My most practical lesson was small: wear easy shoes and bring a written pain baseline. When a nurse asks, “What’s your pain right now from 0–10?”, your answer matters for both clinical assessment and insurance documentation. If you’re rebuilding your day-to-day mobility, you might also want to glance at walking shoes that are sciatica-friendly so your post-procedure “test walks” don’t become a confounding variable.
In many U.S. clinics, these procedures are done under local anesthetic with optional light sedation depending on policy and patient anxiety. If sedation is used, expect stricter fasting rules and a longer recovery window.
Show me the nerdy details
Clinicians typically use real-time imaging to reduce the risk of incorrect placement and to confirm medication spread. The diagnostic signal often comes from short-term changes in radicular pain—especially when the anesthetic phase produces meaningful relief consistent with the suspected root.
What it feels like (and what I wish I’d known)
I’m not going to pretend this is spa-adjacent. But it also isn’t the horror story many of us rehearse in our heads at 2 a.m. The sensation is usually more pressure and lightning than deep pain.
For me, the oddest moment was the brief reproduction of my familiar leg pain. It was unsettling, but it also felt like confirmation: “Okay, that nerve really is involved.”
What you might feel
- A short sting from local numbing
- Deep pressure
- A brief flare of your classic leg symptoms during positioning or medication delivery
- A split-second “electric” sensation that resolves quickly
Two realistic numbers:
- Expect pressure more than sustained pain
- A brief symptom “echo” is common
- Your before/after notes matter
Apply in 60 seconds: Set a phone timer to record pain levels at 30, 60, and 120 minutes post-procedure.
Risks, side effects, and rare red flags
Most people want a simple answer: “Is it safe?” The honest answer is that selective nerve root blocks are commonly performed and generally considered low-risk when done by experienced clinicians with proper imaging, but no injection is risk-free.
More common, usually short-lived effects
- Soreness at the injection site for 24–48 hours
- Temporary numbness or heaviness in the leg
- A short pain flare that settles within a couple of days
Less common but important to know
- Infection
- Bleeding or hematoma risk (higher with certain medications)
- Allergic reactions to contrast or medication
- Unexpected neurologic changes
My rule of thumb was blunt: if something feels “new and escalating” rather than “expected and fading,” I call. It’s not dramatic. It’s efficient. If you’re ever uncertain about the boundary between “normal post-injection weirdness” and danger, keep a simple reference point for when low back pain becomes an emergency.
Red flags that deserve immediate contact with your clinic or urgent care:
Real-world costs, insurance, and out-of-pocket, 2025 (US)
This is where most posts get fuzzy. Clinics may quote a single number, but your real out-of-pocket depends on where the procedure is done (hospital outpatient vs ambulatory center), your plan’s deductible, and how your insurer classifies the injection.
In everyday U.S. reality, you’re usually juggling three cost concepts:
- Facility charge (often the bigger variable)
- Professional fee for the clinician
- Imaging/contrast components
If you’re on a high-deductible plan, the first injection of the year can feel like a financial cliff. If you’re late in the calendar year and near your out-of-pocket max, it can feel oddly “discounted.” Both experiences are real, and both deserve planning rather than surprise.
| Setting | Self-pay ballpark | Notes |
|---|---|---|
| Ambulatory surgery center | Mid hundreds to low thousands | Often lower facility fees vs hospitals |
| Hospital outpatient | High hundreds to several thousand | Facility component can swing widely |
| In-network with deductible met | Copay/coinsurance range | Ask for a written estimate with CPT/diagnosis context |
Neutral action: Save this table and confirm the current fee on the provider’s official estimate.
For readers outside the U.S., the coverage mechanics may be simpler if your system bundles facility and professional fees more predictably. But even then, you’ll still want clarity on whether this is framed as a diagnostic block, a therapeutic injection, or part of a larger pain-management pathway.
My personal cost-saving mistake:
Decision card: SNRB vs epidural vs PT
If you’re trying to choose between a selective nerve root block, a broader epidural approach, and doubling down on rehabilitation, you’re not indecisive. You’re navigating three different “why” frameworks—very similar to the trade-offs you’ll see in transforaminal vs interlaminar epidural decisions.
- Choose an L5/S1 selective nerve root block when diagnosis is murky, symptoms are root-specific, and you need a cleaner next-step signal.
- Choose a broader epidural approach when pain is multi-level or your clinician suspects wider epidural inflammation.
- Prioritize PT-first escalation when symptoms are improving, strength is stable, and your daily function is trending up.
Time/cost trade-off: A selective block may save weeks of trial-and-error, but can cost more upfront depending on facility setting.
Neutral action: Screenshot this card and confirm which goal your clinician is targeting before you sign consent.
My own turning point was admitting that “waiting it out” was also a decision with a cost. The cost wasn’t just money. It was weeks of compromised sleep, shorter walks, and that subtle shrinkage of confidence. When I finally recommitted to structured rehab, I also revisited the old debate of chiropractor vs physical therapy so my next step wasn’t just hopeful—it was coherent.
How to prep for prior authorization and a clean quote
Prior authorization has a way of turning pain into paperwork. The fastest way through is to be unromantic and organized. Insurers often want evidence of conservative management and a clear rationale for targeted injection. If meds have been part of your bridge, it’s worth having a quick safety frame for NSAID use for back pain documented alongside your timeline.
Quote-prep list
- Your symptom timeline (start date + changes)
- PT dates and short outcome notes
- Imaging report summary
- Current meds and any adverse reactions
- Your plan details: deductible, coinsurance, out-of-pocket max
Two numbers that can change your decision:
Also, if your insurer offers a cost-estimator portal, treat it as a starting point, not a promise. The final check is always a written estimate from the facility.
Aftercare, results window, and when to escalate
Aftercare is usually simple, but the interpretation is not. A selective nerve root block can produce two distinct time windows:
- Short anesthetic window:
- Anti-inflammatory window:
The most useful thing you can do is track function, not just pain. Can you walk 10 minutes longer? Sit without the leg burning? Sleep without the 3 a.m. negotiation? If night is where your symptoms get cruel, pairing your notes with a quick reset on side sleeping and sciatica strategies can help you separate “position pain” from true post-injection response.
My “operator” habit here was small and oddly powerful: I wrote down one functional metric I cared about most—walking to the corner store without that calf clamp—and I measured only that for a week.
- Track a single daily activity
- Note short-term anesthetic response
- Use the data to shape your next step
Apply in 60 seconds: Pick one “win metric” and write it in your phone notes before the procedure.
What to do if relief is short—or zero
This is the section nobody wants to read, which is exactly why you should. A disappointing response does not always mean the injection was “a failure.” It might mean:
- The wrong root was targeted.
- The pain source is multi-factor (disc + facet + muscle guarding).
- The primary driver is not inflammatory.
- The timeline of your condition demands a different approach.
I remember the quiet sting of thinking I’d wasted money when relief didn’t last. The more accurate framing was that we’d narrowed the map. Sometimes that map-narrowing also means revisiting differential questions like sciatica vs piriformis syndrome when the symptom story and the imaging story refuse to shake hands.
If the diagnostic signal suggests L5/S1 isn’t the main culprit, your clinician may discuss different imaging correlation, alternative injection strategies, or a deeper rehab reset.
Short Story: The day I stopped pretending I was fine
Short Story: I told myself I could “just work through it.” I was still taking meetings, still pretending the limp was a quirky personality trait. But my calendar didn’t show the truth: three micro-breaks per hour to stand, an ice pack wedged behind my laptop, and the way my leg pain stole every quiet moment between tasks. On the morning of the block, I felt oddly embarrassed—like I was admitting defeat.
Then the nurse asked me to point to the exact path of pain. I traced it down my calf with the precision of someone who has memorized a storm. When the anesthetic phase softened that familiar burn, I didn’t feel triumphant. I felt relieved in a different way: the story finally matched the anatomy. That clarity gave me permission to rehabilitate seriously instead of improvising in denial—especially after reading more about why desk jobs trigger sciatica flare-ups and adjusting my workday before the next relapse.
Mini calculator: your back-pocket out-of-pocket estimator
This is not a perfect billing tool. It is a fast sanity check for busy humans.
Estimated out-of-pocket: Enter numbers to estimate.
Neutral action: Use this estimate to request a written quote that confirms the allowed amount and setting.
How many injections is “too many” and why the interval matters
Patients often ask this because they’re trying to avoid two things at once: long-term reliance and short-term suffering. The best answer depends on your diagnosis, your response pattern, and your clinician’s protocol. The honest baseline you can use in conversation is that injections are usually spaced to balance symptom control with careful medical judgment about cumulative exposure and diminishing returns.
Practically, your decision hinges on whether the block is functioning as:
- A one-time diagnostic clarifier
- A bridge to rehab
- A repeated symptom-management tool
I once thought needing a second injection meant the first “failed.” In reality, the first helped me reclaim just enough movement to make the second unnecessary—because rehab finally became tolerable.
Questions to ask your clinic in one minute
- Is the goal primarily diagnostic, therapeutic, or both?
- Which setting will be used, and can I get a written estimate?
- What should I pause or continue on my medication list?
- How will we define success in the first 7–14 days?
- If this doesn’t help, what is Plan B?
That last question is the quiet power move. It keeps your next steps structured instead of emotional.
Infographic: the L5/S1 SNRB decision map
Leg-dominant, root-specific pain? → move to step 2.
Tried guided PT/meds/activity changes for weeks? → step 3.
MRI suggests a plausible L5/S1 culprit? → step 4.
Need diagnostic certainty or a rehab bridge? → consider SNRB.
Compare facility settings + request written estimate.
Track pain + one function metric for 7–14 days.
Use case: Best when you want a targeted answer about which nerve is driving your sciatica.
FAQ
1) Is an L5/S1 selective nerve root block the same as an epidural steroid injection?
They overlap in technique and medication options, but the intent is often more targeted with a selective block. The emphasis is on isolating one nerve root for clearer diagnostic and therapeutic signal. Apply in 60 seconds: Ask your clinician to state the primary goal in one sentence before scheduling.
2) How quickly should I expect relief?
Some people notice short-term change within hours from the anesthetic phase, while the anti-inflammatory effect can take a few days. Your functional improvement over the first week is often the most meaningful metric. Apply in 60 seconds: Choose one daily task to track for 7 days.
3) What if my MRI shows a disc issue but my pain pattern is messy?
That’s a common reason for selective blocks. When imaging and symptoms don’t fully agree, a targeted block can help confirm which root is truly contributing. Apply in 60 seconds: Bring a simple pain map drawing to your appointment.
4) Will insurance cover it?
Many plans cover medically indicated nerve root blocks, but prior authorization rules vary. Your out-of-pocket depends on deductible status and the facility setting. Apply in 60 seconds: Request a written estimate that includes the setting and your plan’s cost-share context.
5) How many times can I get this done?
Protocols vary and depend on your response, diagnosis, and risk profile. The practical question is whether the block is functioning as a diagnostic tool, a rehab bridge, or ongoing symptom management. Apply in 60 seconds: Ask, “What outcome would make a repeat unnecessary?”
6) When should I consider surgery instead?
If you have progressive weakness, severe function collapse, or persistent disabling symptoms despite well-structured conservative care and targeted interventions, a surgical consult may be appropriate. Apply in 60 seconds: Write down your top three function losses to discuss in a focused consult.
Three trustworthy places to double-check the medical basics
You don’t need a dozen tabs. You need three calm, credible references for the underlying mechanics and safety framing.
Last checked and your next 15 minutes
Last reviewed: 2025-12. This article reflects common clinical workflows, typical U.S. billing realities, and patient-experience patterns. Policies and pricing vary by region, facility, and insurer, so treat any cost range as a planning tool—not a final bill.
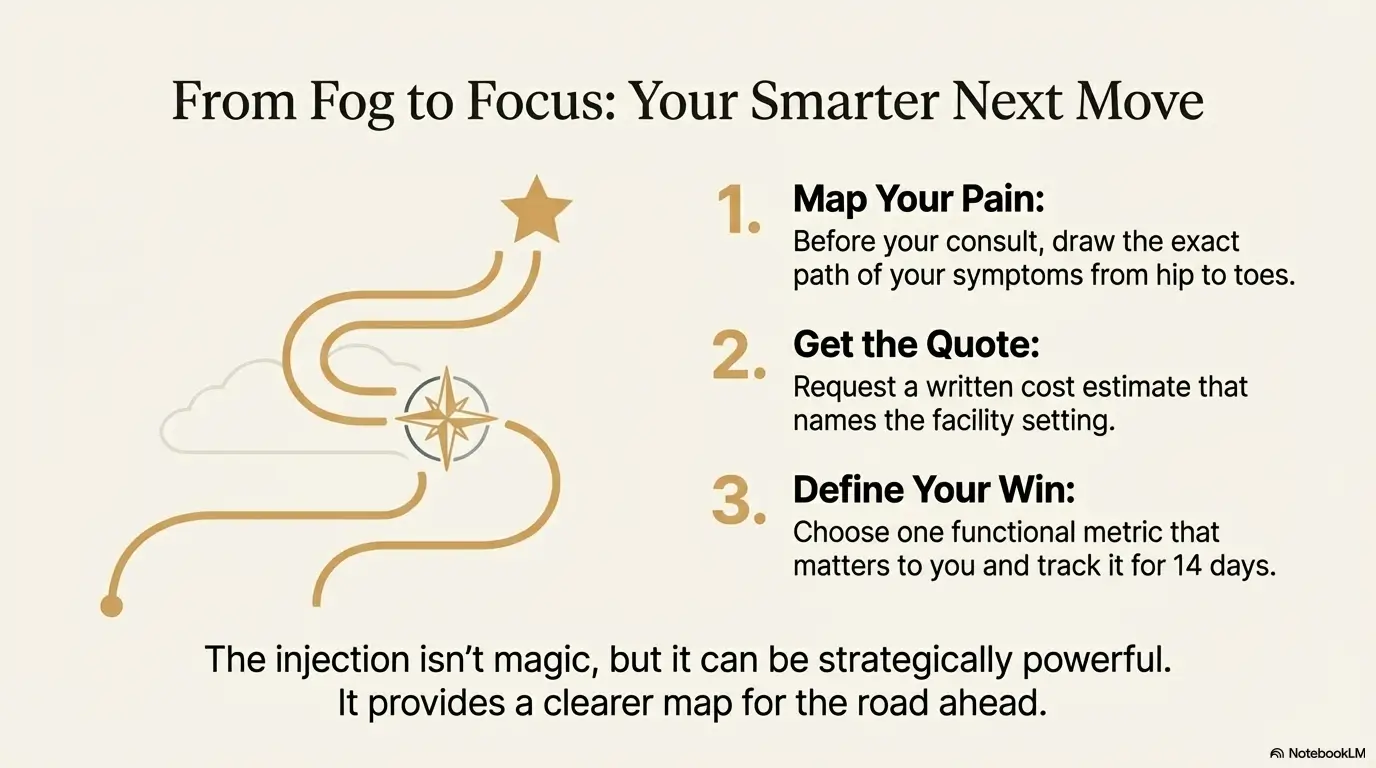
If you only do three things after reading:
- Write your pain map and bring it to your consult.
- Request a written estimate that names the setting and your plan’s cost-share context.
- Define one success metric you care about over 7–14 days.
The curiosity loop from the start deserves an honest ending: the injection may not be magical, but it can be strategically powerful. When it works, it buys you motion, sleep, and a clearer diagnosis. When it doesn’t, it still narrows the map and prevents months of vague guessing. If your broader pathway starts touching stenosis conversations, it can help to compare the long-arc options alongside lumbar spinal stenosis surgery costs in 2025 so you’re not blindsided by the next tier of decisions.
Your 15-minute next step:
