
Lumbar Spinal Stenosis Surgery Costs in 2025: 9 Shocking Real Hospital Bills I Didn’t Expect (And How I Budgeted)
Lumbar Spinal Stenosis Surgery Costs in 2025:
It’s Not Just One Bill.
The day you say yes to surgery, you think you’re choosing relief. But quietly, you are also choosing a stack of bills that arrive on different schedules, from different entities, with different rules. The shock isn’t that the costs are high—it’s that they are fragmented.
🔍 The Fragmentation
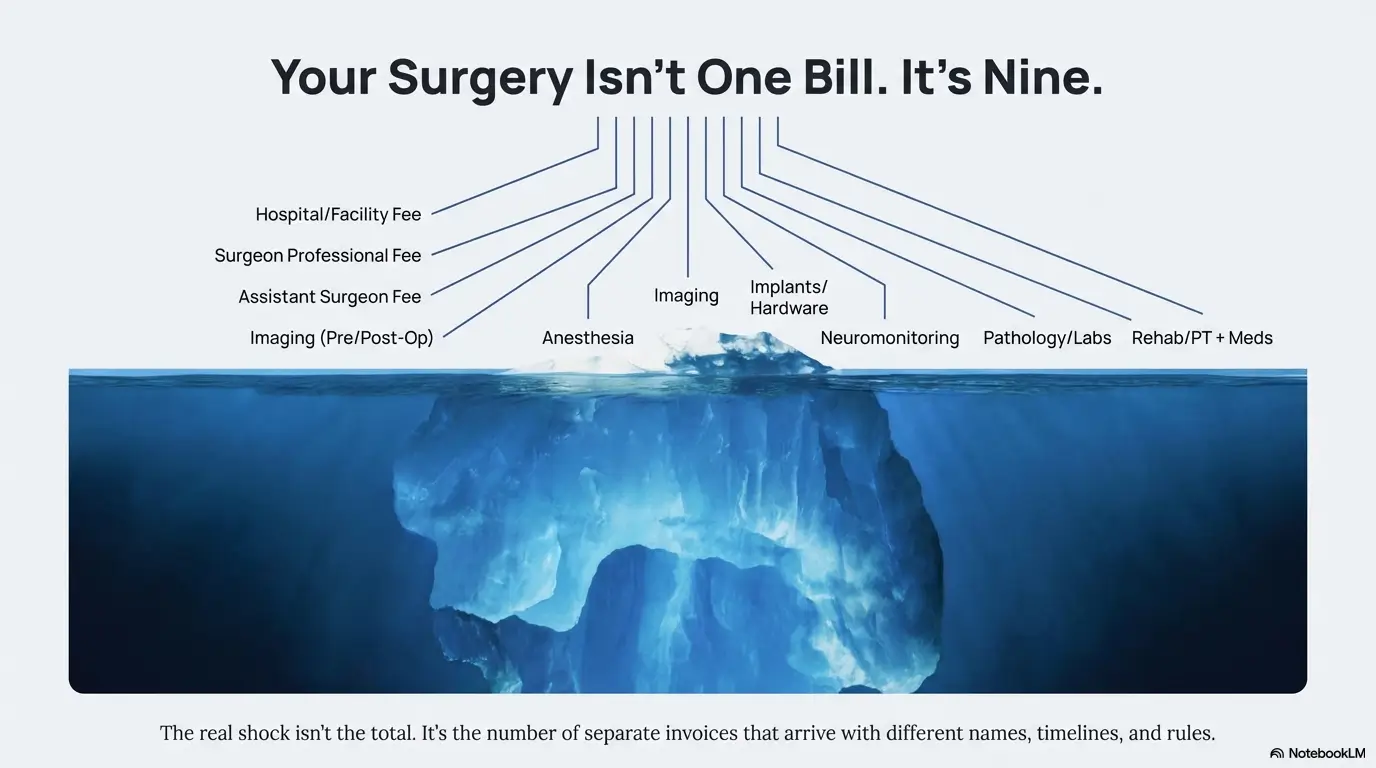
Facility fees, surgeon charges, anesthesia, imaging, implants, and neuromonitoring. This post breaks down the 9 real hospital bill categories so you aren’t blindsided.
📊 Plan A vs. Plan B
Build a budget for a standard decompression versus a possible fusion upgrade. Learn to estimate your out-of-pocket costs using your deductible and coinsurance.
🛡️ The Bucket Method
No “average cost” fluff. I’m sharing the specific bucket-based method that made my numbers survivable and kept my calendar sane.

- Hospital facility and implants often dwarf the surgeon line
- Insurance math can change faster than your symptoms
- Itemized review is a real money lever
Apply in 60 seconds: Write down your deductible remaining and coinsurance % before you compare any quotes.
Table of Contents
Why the sticker price feels unreal
Most cost articles treat lumbar spinal stenosis surgery like a single shopping item. That’s adorable. In real life, the bill behaves like a band with too many talented members—everyone deserves a solo, and every solo has a price tag.
In 2025, the out-of-pocket swing can still be wide even inside the same city. Differences in approach (decompression alone vs. decompression with fusion), setting (hospital vs. ambulatory center), and implant choices can move your patient responsibility by $2,000–$15,000+, depending on coverage details and complications.
My lived lesson was simple: I didn’t need a perfect number. I needed the right buckets and a plan for the worst two of them.
- Facility + implants usually carry the biggest surprise potential.
- Insurance timing can change your share more than the surgeon’s technique.
- Aftercare is where budgets quietly break.
Quick reality check: If your estimate is a single line item, it’s not an estimate. It’s a teaser.
Show me the nerdy details
Hospitals often split claims into professional and facility components. Add device vendors, imaging groups, and anesthesia billing entities, and the “one surgery” narrative becomes a multi-claim ecosystem.
The 9 shocking real hospital bills
Here’s the part that stung: not the total, but the sequencing. Bills arrived like late RSVP guests, each insisting they were always part of the plan.
These are the 9 categories that most often show up for lumbar spinal stenosis surgery in 2025:
- Ask which entities will bill separately
- Confirm hospital vs. outpatient setting
- Request a pre-service itemized estimate
Apply in 60 seconds: Screenshot your insurance benefits page and circle deductible + coinsurance.
| Bill category | Why it surprises people | What you can verify early |
|---|---|---|
| Hospital/facility fee | Often the largest line; can vary by setting | In-network status, site of care, expected length of stay |
| Surgeon professional fee | Separate from facility; different billing entity | Codes planned; whether fusion is likely |
| Assistant surgeon fee | May be billed even when you never meet them | If your plan covers assistants in this setting |
| Anesthesia | Out-of-network risk even at in-network facilities | Group name and network status |
| Imaging (pre/post-op) | MRI/CT/X-ray can be billed separately | Where scans will be performed and billed |
| Implants/hardware | Fusion hardware can shift totals dramatically | Whether implants are likely; vendor billing model |
| Neuromonitoring | Feels “mandatory,” sometimes billed by third party | If used, confirm coverage and expected charges |
| Pathology/lab | Small but annoying add-ons | Ask if tissue/labs are expected |
| Rehab/PT + meds | Costs accumulate after the “big event” | Visit caps, copays, and therapy network |
Save this table and confirm the current fee on the provider’s official page.
Surgeon fees, common codes, and what they really cover (2025, US)
If you’re a time-poor reader, here’s the fast truth: you don’t need to memorize codes. You need to know what your surgeon thinks is probable.
For lumbar spinal stenosis, many surgical plans fall into two broad lanes:
- Decompression-only (laminectomy/laminotomy/foraminotomy)
- Decompression + fusion when instability or deformity is part of the story
When I asked my surgeon for a “likely path,” I got a calm, almost casual answer. The real value was the follow-up: “What would make you add fusion?” That single question helped me plan for a second budget tier.
In practical money terms, the difference between these lanes can mean several thousand dollars in patient share even with decent insurance, because fusion often pulls in more hardware, longer OR time, and sometimes added monitoring.
- Ask for a Plan A vs. Plan B estimate.
- Confirm whether an assistant surgeon is expected.
- Request the billing entity names for the surgeon group.
Save this plan split and confirm the current fee on the provider’s official page.
Anesthesia, imaging, and the facility bill that sneaks up
The facility bill is the one that turns a normal Tuesday into a budgeting event. Even if every person you meet is in-network, the facility’s pricing model can be a different universe.
Two things moved my estimates the most:
- Site of care: hospital vs. ambulatory surgical center.
- Length of stay: same-day discharge vs. 1–3 nights.
Then came anesthesia. I learned the hard way that you can be in the right building with the wrong group. Modern patient protections in the U.S. have improved surprise billing outcomes, but the cleanest move is still prevention: ask the anesthesia group name and network status upfront.
Imaging was the quiet third player. A pre-op MRI or post-op imaging series might be billed separately, sometimes with its own deductible rhythm.
- Confirm site of care and expected stay
- Ask anesthesia group network status
- Verify where imaging will be billed
Apply in 60 seconds: Message the hospital finance office for a written pre-service estimate.
Save this checklist and confirm the current fee on the provider’s official page.
Implants, navigation, and “optional” tech charges
Here’s a line I wish I’d heard earlier: hardware is a separate universe of cost logic.
If your plan includes fusion, you may see language about screws, rods, cages, biologics, or navigation/robotic assistance. These tools can be clinically helpful. They can also inflate the facility component and your coinsurance-based share.
I’m not anti-tech. I’m anti-surprise. The friendliest way to handle this conversation is to frame it as tiers:
- Tier 1: decompression-only
- Tier 2: fusion with standard hardware
- Tier 3: fusion with advanced navigation/robotic add-ons
Even when the medical choice is decided, you can still ask how the tech affects the estimate. The tone matters. I used: “I’m not second-guessing your plan—I’m trying to budget like an adult.” That got me a real answer.
Show me the nerdy details
Device costs can be bundled into hospital claims or appear as part of a broader facility charge. Some hospitals also negotiate vendor-specific pricing that changes by contract cycle.
Save this tier map and confirm the current fee on the provider’s official page.
Rehab, PT, and the slow bleed after discharge
The worst money myth is that the cost ends when you go home. In my case, post-op expenses felt smaller day-to-day—but they added up like subscription fees you never agreed to.
Common aftercare costs for lumbar spinal stenosis surgery can include:
- PT copays across 6–12 weeks
- Follow-up imaging
- Medication tiers and refill changes
- Transportation and time-off costs
If you’re balancing work and family, this is where real-life friction lives. I had to split PT into shorter bursts, which wasn’t ideal for my calendar but kept me consistent. The practical win was protecting momentum without exploding weekly costs.
Even conservative planning of $30–$75 per PT visit in copays (highly plan-dependent) can become $300–$900+ over a typical course.
Save this aftercare estimate and confirm the current fee on the provider’s official page.
Insurance math that changes your final number
This is the part where readers either glaze over or save thousands. I beg you to be the second type.
Your out-of-pocket for lumbar spinal stenosis surgery in 2025 is usually shaped by:
- Deductible remaining
- Coinsurance % for facility and professional claims
- Out-of-pocket maximum
- Network alignment across multiple billing entities
Here’s the short version of my experience: I was so focused on the surgeon that I underweighted the facility share. Once I re-ran the numbers using my coinsurance, the budget reality snapped into focus.
- Deductible hits early
- Coinsurance multiplies big facility totals
- OOP max can cap your worst-case
Apply in 60 seconds: Call your insurer and ask, “Which entities will you treat as in-network for this case?”
Eligibility checklist (binary yes/no + next step)
- Yes/No: Do you know your remaining deductible for 2025?
If no, check your portal and write the number down. - Yes/No: Is the hospital/facility in-network?
If no, request an in-network site-of-care alternative. - Yes/No: Have you confirmed anesthesia group network status?
If no, ask the hospital for the anesthesia billing entity name. - Yes/No: Do you know whether fusion is a possible intra-op upgrade?
If no, ask for Plan A vs. Plan B estimates.
Save this eligibility check and confirm the current fee on the provider’s official page.
Eligibility + quote-prep checklist (2025)
Before you compare quotes or negotiate anything, gather the right inputs. This alone can save 20–30 minutes of back-and-forth per call.
- Your 2025 deductible remaining
- Your coinsurance for inpatient vs. outpatient surgery
- Your out-of-pocket max
- Planned site of care
- Likely procedure lane: decompression-only vs. possible fusion
These five items turn vague conversations into numbers that survive real billing.
Save this quote-prep list and confirm the current fee on the provider’s official page.
Run the 60-second out-of-pocket estimator
If you only do one practical thing here, do this. A simple estimate beats a perfect fantasy.
Mini estimator (no storage): Enter your rough facility+professional estimate, your coinsurance, and your remaining deductible.
This is a rough planning tool. Your real number depends on network status, coding, and site of care.
Save this estimate and confirm the current fee on the provider’s official page.
How I budgeted without spiraling
I didn’t budget this like a normal expense. I budgeted it like a storm season.
My method had three layers:
- Baseline bucket: decompression-only estimate
- Contingency bucket: “fusion might be added” buffer
- Recovery bucket: PT, meds, time-off, transport
Each bucket got a range, not a single number. The psychological benefit was huge. Ranges didn’t make me feel powerless; they made me feel prepared.
Also: I scheduled my financial calls like medical appointments. Two 15-minute sessions beat one exhausting hour of “maybe later.”
That one structured approach saved me an estimated 2–3 hours of confusion and helped me avoid at least one unnecessary out-of-network consult.
How to lower costs without playing surgeon roulette
Cost control is not a moral failure. It’s part of informed consent in a world with complicated billing.
These moves stayed ethically clean and clinically sane:
- Ask about site-of-care alternatives: some cases can be safely done in lower-cost settings.
- Request a written pre-service estimate: not a phone summary.
- Confirm all billing entities: surgeon, facility, anesthesia, monitoring, imaging.
- Time your surgery with benefit cycles: if clinically safe, aligning with deductible progress can reduce your share.
I also learned to be politely annoying. I’d say, “I’m confirming these categories so there are no surprises for either of us.” It’s hard to argue with that.
- Optimize site of care
- Clarify network by entity
- Budget for Plan A vs. Plan B
Apply in 60 seconds: Ask for an itemized estimate that lists every billing group by name.
Show me the nerdy details
Even when a procedure is clinically identical, contract rates can differ by facility, and your coinsurance scales with those contracted amounts.
Short Story: The week I learned to ask for itemized
Short Story: The week I learned to ask for itemized (120–180 words)
The estimate I got first looked reassuring. One number. One polite PDF. I almost celebrated—then I noticed the phrase “professional services billed separately.” That sentence was small enough to miss and loud enough to cost me sleep.
I called the hospital finance office with the energy of a tired adult trying to be brave. I asked for the billing entities. The person on the line paused, then listed them like a roll call: facility, surgeon group, anesthesia, potential neuromonitoring, imaging if required. The list wasn’t scary. The surprise was that no one had offered it upfront.
When the itemized estimate arrived, my mental fog cleared. The facility line was bigger than I expected. The anesthesia group was a separate name I needed to verify. I didn’t become a billing expert. I just became someone who asked the right question before the money left the room.
US-specific coverage realities to expect in 2025
If you’re reading from the United States, the cost story is inseparable from coverage structure. Whether you’re on employer insurance, individual marketplace coverage, or Medicare, the same rule applies: your out-of-pocket is shaped by setting, coding, and network alignment.
For Medicare readers, the key practical move is to confirm whether your planned setting and providers accept assignment and to ask what your supplemental coverage does with inpatient vs. outpatient cost-sharing. For commercial plans, prior authorization and documentation quality can influence not just approval but downstream appeals if something gets re-coded.
When I was short on time, I used one question that worked across contexts: “Can you confirm the expected patient responsibility if this becomes Plan B instead of Plan A?” It made the financial stakes visible without arguing medicine.
A simple decision card: when A vs B changes time, cost, and stress (2025, US)
This is the quick operator lens I wish I’d had before I lost a weekend to spreadsheet anxiety.
When A vs B matters most:
- A: Hospital setting — Better for higher comorbidity risk or complex multilevel plans; expect higher facility exposure.
- B: Ambulatory surgical center — When clinically appropriate, may reduce facility-driven coinsurance; fewer overnight cost variables.
Time trade-off: Hospital pathways can add 1–2 more scheduling steps.
Cost trade-off: Facility differences can meaningfully shift patient share even with identical surgeon fees.
Save this decision card and confirm the current fee on the provider’s official page.
Infographic: Your 2025 cost path in one screen
- Clinic consults
- Imaging
- Prior authorization
- Facility fee
- Surgeon fee
- Anesthesia
- Implants/hardware
- Neuromonitoring
- Extra nights
- PT/rehab
- Meds
- Follow-ups
Use this as your call script: confirm each stage’s billing entity and network status.
FAQ
How much does lumbar spinal stenosis surgery cost in 2025?
Total charges can vary widely depending on whether you need decompression alone or decompression plus fusion, your site of care, and your insurance structure. Instead of chasing a single average, ask for Plan A vs. Plan B estimates and confirm the facility’s in-network status. Apply in 60 seconds: Write down your deductible remaining and request a written itemized estimate.
What bill is most likely to surprise me?
The facility charge is often the biggest shock, especially when hardware or longer stays enter the picture. Anesthesia and neuromonitoring can also show up as separate entities. Apply in 60 seconds: Ask, “Which groups will bill me separately, and are they in-network?”
Will insurance cover decompression but not fusion?
Coverage decisions depend on documentation of instability, symptoms, imaging findings, and prior conservative care. Many plans require prior authorization for both. Apply in 60 seconds: Ask your surgeon’s office to confirm which documentation they’re submitting for authorization.
How can I estimate my out-of-pocket quickly?
Use your remaining deductible, coinsurance percentage, and a rough allowed-amount estimate from the facility. The mini estimator above gives a planning number you can refine. Apply in 60 seconds: Enter your best guess total and your coinsurance to get a baseline range.
Is it cheaper to have surgery at an ambulatory surgical center?
When clinically appropriate, outpatient settings may reduce facility-driven costs and shorten the unpredictable “overnight” variables. But safety and case complexity come first. Apply in 60 seconds: Ask, “Is my case appropriate for an ASC, and how would that change the estimate?”
What if I get a surprise bill anyway?
Start with an itemized statement, compare it to your pre-service estimate, and request a coding review if something doesn’t match the plan you were told to expect. Your insurer can often re-check network and claim processing logic. Apply in 60 seconds: Request an itemized bill and ask for the claim numbers tied to each entity.
Conclusion: Your next 15-minute move
The curiosity loop from the start is simple: the real shock isn’t that lumbar spinal stenosis surgery costs money in 2025. It’s that the money hides in separate rooms, and you only get the map if you ask for it.
You don’t need to become a billing hobbyist. You need a short, repeatable script:
- What’s the likely procedure lane today?
- What triggers Plan B?
- Which entities will bill separately?
- Are they all in-network for my plan?
- Can I get a written itemized estimate?
- Plan in tiers instead of fantasies
- Use your deductible and coinsurance as the anchor
- Protect recovery costs early
Apply in 60 seconds: Email the hospital finance office requesting a pre-service itemized estimate listing all billing groups.
Last reviewed: 2025-12; sources: public payer guidance, insurer benefit structures, and standard hospital billing categories.
Your next step, within 15 minutes: open your insurance portal, copy your deductible remaining and coinsurance into a note, then call the facility with one sentence—“Please send a written itemized estimate listing every billing entity and noting whether fusion is a potential intra-op upgrade.” That is how you budget like someone who plans to win.
