
Transforaminal vs Interlaminar Epidural for Sciatica: Success Rates, Risks, and the 3 Questions I Wish I Asked
Transforaminal vs. Interlaminar Epidural for Sciatica
The decision felt like being asked to pick a route through an unfamiliar city—fast lane or wider road—without a map of my own nerve.
Both are epidural steroid injection approaches designed to calm irritated nerve roots. Transforaminal delivers medication closer to a specific exiting nerve through the foramen, while Interlaminar enters more centrally to allow broader epidural spread. The goal is the same; the targeting and risk conversation are not.
When your pain is relentless, it’s easy to accept the clinic’s default. And then wonder later if you picked the wrong kind of precision.
Keep guessing, and you lose time. You can lose money. You can lose the rehab window that actually changes your next month.
This post helps you match your symptom map and MRI to the right route, understand real-world success rates and risks, and talk through cost and coverage in 2025 without getting buried in jargon. I’m writing from the patient side of the table, with a simple method: anatomy first, expectations second, technique last.
Here’s the clean way to think about it:
- ✓ Get a one-sentence nerve-root explanation.
- ✓ Align approach with your pain pattern.
- ✓ Confirm a personalized safety plan.
- ✓ Define what “success” means for your next 2–6 weeks.
Good. Now you’re ready to choose like someone who won’t regret the follow-up visit.
Table of Contents
Why these two approaches confuse almost everyone
The first time I heard “transforaminal” and “interlaminar,” I nodded like I understood. I didn’t. Both are epidural steroid injections aimed at reducing nerve irritation, but the path the medication takes is different—and that path matters.
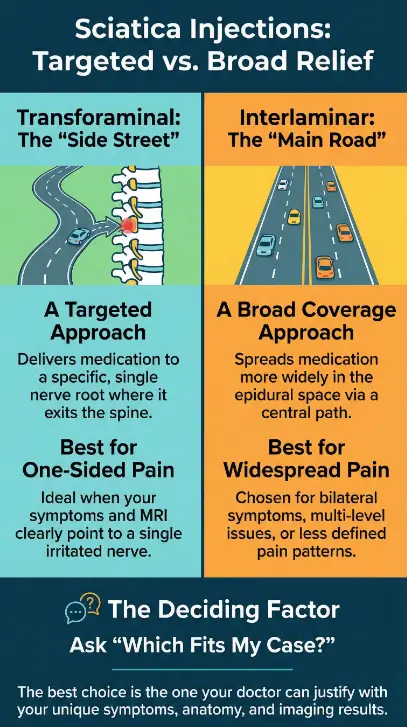
Think of it like two routes to the same neighborhood. One is a side street that drops you closer to a specific house. The other is a main road that serves the block. If your sciatica is clearly one-sided and tracks down a specific leg, the more targeted route often gets discussed. If symptoms are broader or anatomy is complex, the broader route may be chosen.
Clinics also differ in habit and training. Some physicians default to one style because it matches their workflow and imaging preferences. That’s not automatically bad—but it does mean you should ask why your anatomy and symptom pattern fits that choice.
- Transforaminal is usually framed as more targeted
- Interlaminar is often framed as broader coverage
- Your MRI + symptom map should drive the pick
Apply in 60 seconds: Write down which leg, which toes, and what movements trigger your pain.
Quick answer: who tends to do better (and when)
If you only read one section, read this one. The “success rate” conversation can get messy because studies measure different outcomes: short-term pain reduction, functional improvement, or avoidance of surgery. But clinicians often converge on a practical rule of thumb.
When pain is clearly radicular and one-sided—classic butt-to-calf or butt-to-foot pain—many specialists lean toward the transforaminal route because it can deposit medication closer to the affected nerve root. If you want a clean refresher on what counts as classic radicular pattern, skim sciatica nerve pain basics and symptom mapping before your next appointment.
When symptoms are more bilateral, diffuse, or when multi-level issues exist, interlaminar may be preferred for broader epidural spread. This situation shows up often when the diagnosis sits somewhere between disc-related sciatica and canal narrowing, so it can help to review lumbar spinal stenosis vs herniated disc patterns if your MRI report feels like alphabet soup.
My own “aha” was realizing that a lot of disappointment comes from expectation mismatch. Some people walk out hoping for a permanent fix. A more realistic target is improved function for weeks to months, often paired with physical therapy that consolidates the window of relief.
- Typical procedure time: about 10–20 minutes.
- Common onset: 24–72 hours for steroid effect.
- Best-case practical goal: a rehab-friendly pain drop.
Show me the nerdy details
The key distinction is the injection trajectory relative to the nerve root and the epidural space. “Targeting” isn’t a marketing word here—it’s anatomical geometry under fluoroscopy. However, real-world outcomes still depend on diagnosis accuracy, injectate volume, steroid choice, and whether the pain source is truly nerve inflammation versus mechanical compression.
Transforaminal epidural: how it works and where it shines
Transforaminal epidurals approach the epidural space through the neural foramen—near where the nerve exits the spine. In plain language: it’s the “close-to-the-nerve” approach.
The appeal is obvious when you’ve got a single angry nerve root. A clinician can aim for the exact level that matches your symptom pattern and imaging. That’s why you’ll often hear this described as a good option for unilateral sciatica tied to disc herniation. If you’re still unsure whether your symptoms are more disc-driven, this sciatica vs herniated disc breakdown can help you ask sharper questions.
But precision brings responsibility. The technique requires careful imaging guidance and an experienced hand. The safety conversation often includes steroid type and meticulous placement because the anatomy of blood vessels in this region can raise rare but serious risk considerations.
My small confession: I initially assumed “more targeted” automatically meant “better.” It doesn’t. It means more appropriate when the diagnosis is clean. If the pain generator is ambiguous, a laser pointer can still miss the right target.
- Best fit for one-sided nerve-root pain
- Relies heavily on accurate level selection
- Clinician experience matters a lot
Apply in 60 seconds: Ask your doctor which nerve root they believe is responsible and why.
Interlaminar epidural: what it is and why doctors still love it
Interlaminar epidurals enter between the laminae from a more central posterior route. This is often the “classic” epidural style many patients picture.
The strength here is coverage. The medication can spread more broadly within the epidural space, which can be helpful in multi-level degenerative changes or when symptoms are less cleanly mapped to one nerve root.
It’s also sometimes chosen when anatomy makes a transforaminal route technically challenging. A good clinician won’t frame this as a second-best option; they’ll frame it as the best match for your specific spinal landscape.
I once heard a physician explain it with refreshing honesty: “We’re not choosing the ‘cooler’ injection. We’re choosing the one that fits the story your body is telling.” That line stuck with me because it nudged me away from internet ranking fights and back toward data + symptoms + safety.
- Useful when pain patterns are broader or bilateral.
- May be favored when more epidural spread is desired.
- Still demands image guidance and careful technique.
Risks, side effects, and red flags you should know
Both approaches share common, usually short-lived side effects: temporary soreness, a brief pain flare, headache, or sleep/mood changes from steroids. Most of the time, these resolve within a few days.
The rarer risks are the reason you should insist on a clear explanation of technique and safety steps. These can include infection, bleeding, nerve injury, or severe headache from dural puncture. Transforaminal injections, because of their proximity to certain vascular structures, often prompt extra caution about steroid selection and imaging precision.
Here’s my very human moment: I didn’t ask about red flags because I assumed “if something bad happens, I’ll know.” That’s a terrible plan. You want a simple post-procedure instruction sheet and a clinic number you can actually reach. If your symptoms ever shift into true “don’t-wait” territory, keep this low back pain emergency guide bookmarked for a fast reality check.
- Ask about infection and bleeding precautions
- Confirm image guidance is used
- Understand expected vs abnormal symptoms
Apply in 60 seconds: Screenshot your post-op instructions and save the after-hours contact number.
Show me the nerdy details
Risk profiles are influenced by anticoagulant use, diabetes, immune status, prior spine surgery, and the choice of particulate vs non-particulate steroid. Many safety conversations today revolve around minimizing catastrophic vascular complications while preserving clinical benefit.
Cost, coverage, and eligibility in 2025 (US + Korea)
This is the part many articles dodge, but real people don’t. The price of relief matters—especially when you might need a series or when imaging and facility fees stack quietly.
In the US, out-of-pocket cost for an epidural steroid injection can vary widely by setting (hospital vs ambulatory center), insurance plan, deductible status, and whether imaging or additional evaluation is billed separately. I’ve seen patients quote anything from a few hundred dollars to well over a thousand when deductibles are in play.
In Korea, the National Health Insurance system often covers a significant portion of medically indicated spine injections, but copays may still vary by hospital grade, imaging needs, and whether your care is categorized under specific benefit rules. The smartest move is to ask for a written estimate before the procedure and confirm which components are covered (consultation, imaging, procedure fee, medication).
Eligibility checklist (fast yes/no)
- Yes/No: Does your pain follow a classic nerve-root pattern down the leg?
- Yes/No: Do imaging findings match your side and level of symptoms?
- Yes/No: Have conservative measures been tried for several weeks unless symptoms are severe?
- Yes/No: Are blood thinners managed appropriately per your clinician’s protocol?
- Yes/No: Do you have uncontrolled infection or unstable medical issues? (If yes, pause.)
Next step: If you answered “no” to the first two, ask whether your diagnosis should be re-checked before choosing a technique.
Save this checklist and confirm the current policy on the provider’s official page.
Typical cost ranges (context only)
| Region | Year | Common patient range | Notes |
|---|---|---|---|
| US | 2024–2025 | Varies widely; often hundreds to 4 figures | Facility + imaging + deductible status can dominate the bill |
| Korea | 2024–2025 | Often lower with NHI coverage; copays vary | Ask for an itemized estimate including imaging and medication |
Save this table and confirm the current fee on the provider’s official page.
60-second out-of-pocket estimator (simple)
Enter numbers above.
Save this estimate and confirm the current fee on the provider’s official page.
One more quiet truth: for many people, the real “value” of an epidural is the function it unlocks—sleeping better, walking longer, and doing rehab without white-knuckling every rep. If your bigger picture includes possible escalation, it may help to compare your long-range options alongside lumbar spinal stenosis surgery costs in 2025 so you’re not weighing injections in a financial vacuum.
Decision card: when I’d pick A vs B
This is the section I wish a calm, mildly skeptical friend had handed me.
Decision card
Pick transforaminal when:
- Your pain is clearly one-sided and follows a single nerve-root pattern.
- Imaging and symptoms align cleanly at one level.
- You want a targeted attempt before considering escalation.
Pick interlaminar when:
- Your symptoms are broader, bilateral, or multi-level.
- Your anatomy makes a foraminal route less ideal.
- Your clinician expects you’ll benefit from wider epidural spread.
Time/cost trade-off: The best value often comes from choosing the technique that reduces “trial-and-error visits,” not the one with the flashier reputation.
Save this card and confirm the current fee on the provider’s official page.
I once tried to “optimize” by insisting on the most targeted option without fully understanding my MRI. It added two weeks of frustration and one unnecessary spiral of doubt. That was my reminder that confidence without context is just expensive hope.

The 3 questions I wish I asked
This is where you protect your time, your wallet, and your future patience.
- “Which nerve root are we targeting, and what evidence supports that?”
If the answer is clear and ties your symptom map to imaging, your odds of a satisfying outcome generally improve. If the answer is fuzzy, ask what else could be contributing. This is also where differentials matter—especially if your symptoms overlap with other nerve conditions—so consider reviewing diabetic neuropathy vs sciatica if you have diabetes or atypical numbness patterns. - “What’s the specific safety plan for my risk profile?”
This includes blood thinner protocols, diabetes considerations, infection precautions, and the type of steroid used. - “What is the success definition for me in the next 2–6 weeks?”
A realistic goal might be sleeping longer, walking 10–20 extra minutes, or tolerating rehab sessions without flare-ups. If your daily triggers are sitting-heavy, you may also want your plan to address desk job sciatica flare-ups so the relief window doesn’t get wasted by the same old posture trap.
- Push for a nerve-root-level explanation
- طلب a personal safety plan
- Agree on a short-term success target
Apply in 60 seconds: Bring a one-sentence symptom summary to your appointment.
I walked into my appointment with the internet’s favorite debate line loaded: “Is transforaminal better than interlaminar?” The physician didn’t flinch. He just asked me to describe my pain in 15 seconds. I said “right leg, burning line, worse when I sit, sharp when I cough.” He nodded, pulled up my MRI, and traced one level with his pen. “Your question is fair,” he said, “but it’s too broad for your case. We’re not picking a champion technique. We’re picking a route that matches this nerve and this story.”
It was a tiny moment, but it changed how I behaved. I stopped trying to win a technique debate and started trying to understand my own anatomy. The appointment got shorter, clearer, and oddly calmer.
What to do the week after your injection
Even a well-placed injection can underperform if the aftercare is chaotic.
The first 24 hours are usually about calm: avoid heavy lifting, respect soreness, and monitor for unusual symptoms. A mild flare can happen. It doesn’t always mean failure.
The real opportunity is days 2–7. If your pain drops even modestly, treat that as a rehab window. Gentle walking, targeted mobility, and clinician-approved exercises can help convert short-term relief into longer-term function. When your walking routine comes back online, it’s worth revisiting sciatica-friendly walking shoes so your footwear doesn’t quietly sabotage your rebound.
- Track your baseline before the injection.
- Log sleep, walking tolerance, and sitting time.
- Use the improved window to rebuild confidence in movement.
My tiny mistake was going from “I feel better” to “I’m invincible” on day 3. The rebound was humbling. Now I treat improvement as a budget, not a lottery win.
Infographic: transforaminal vs interlaminar at a glance
Transforaminal
- Goal: Target a specific nerve root
- Best fit: One-sided, classic radicular pattern
- Why it’s chosen: Precision near the suspected pain generator
- Key caution: Requires meticulous technique and safety planning
- Patient mindset: “Match the level, then maximize rehab.”
Interlaminar
- Goal: Broader epidural spread
- Best fit: Multi-level, bilateral, or less clean symptom mapping
- Why it’s chosen: Coverage when the story is wider than one root
- Key caution: Still requires imaging and individualized risk review
- Patient mindset: “Use the coverage to regain function steadily.”
FAQ
Which epidural is better for a herniated disc sciatica?
If your symptoms and imaging point to a single irritated nerve root, transforaminal is often considered because it can be more targeted. The deciding factor is how cleanly your pain pattern matches a specific level. Apply in 60 seconds: Ask your doctor to name the suspected nerve root out loud and show you where it exits on your MRI.
How long does relief usually last?
Relief varies from person to person. Many clinicians frame it as a window of reduced pain over weeks to a few months rather than a permanent fix. The biggest win often comes when you pair that window with rehab. Apply in 60 seconds: Schedule your next PT session within the first week after the injection.
Is transforaminal riskier than interlaminar?
Both have rare serious complications, but transforaminal injections tend to trigger a more detailed safety discussion because of anatomical proximity to vessels near the foramen. The practical safety upgrade is choosing an experienced clinician who explains their risk-reduction steps clearly. Apply in 60 seconds: Ask what imaging guidance is used and which steroid type is planned.
How many injections can I get in a year?
This depends on clinical guidelines, your diagnosis, and payer/health system rules. Many practices limit the number to reduce steroid exposure and to ensure injections are part of a broader care plan. Apply in 60 seconds: Ask what the clinic’s annual limit is and what metrics they require before repeating.
What if the first injection doesn’t work?
It doesn’t automatically mean failure—sometimes the diagnosis needs refinement, the level may be wrong, or a different approach is more appropriate. A structured follow-up plan matters more than hope-based repetition. Apply in 60 seconds: Request a written “next-step if no relief” plan before you leave the clinic.
Will my insurance cover it?
Coverage depends on medical necessity documentation, prior authorization rules, and your plan’s deductible/coinsurance structure. In Korea, coverage and copays can vary by setting and classification. Apply in 60 seconds: Call your insurer or hospital desk and ask for an itemized estimate that includes imaging and facility fees.
Conclusion
If you came here looking for a simple winner, I get it. Pain makes us crave clean rankings. But the truth I wish I’d accepted earlier is calmer and more useful: transforaminal and interlaminar aren’t competing brands—they’re tools for different stories.
When your sciatica is sharply one-sided and traceable to a specific nerve root, the targeted route can make sense. When the story is broader or multi-level, the wider-coverage route may be the smarter, safer match. Either way, your real leverage is the conversation you have before the needle: diagnosis clarity, safety planning, and a shared definition of success over the next 2–6 weeks.
- Map symptoms to a specific level when possible
- Confirm personalized safety steps
- Plan rehab during the relief window
Apply in 60 seconds: Bring a one-page symptom + goal note to your next visit.
Last reviewed: 2025-12; sources: general clinical guidelines, large-review summaries, and standard patient-education materials.
Your next step doesn’t need to be dramatic. In the next 15 minutes, write your symptom map, list your medications, and copy the three questions from this article into your notes app. Then bring them to your clinician and ask for a technique choice you can explain back in one sentence. That’s how you turn a scary fork in the road into a decision you actually own.
