
Mastering the Glute Bridge: Beyond the Flare
A glute bridge can go from “safe staple” to nerve flare trigger in a single week—and it usually isn’t because you suddenly got weak. It’s because the dose, range, or setup drifted just far enough to irritate a sensitive system.
When sciatica from glute bridges shows up, most people make the same costly move: they either push through electric leg symptoms or quit lower-body training entirely. Neither works for long. You need a calmer way to read signals, adjust mechanics, and keep momentum.
Keep guessing, and you risk turning a manageable flare into a repeating cycle that steals sleep, confidence, and training consistency.
This guide gives you a practical, conservative playbook: how to spot form errors, use a same-day self-screen, choose safer bridge variations, and progress without re-flaring. You’ll also get clear stop rules, next-day checks, and swaps that preserve glute strength while symptoms settle.
Everything here is built around real-world load management—small adjustments, observable responses, and decisions you can trust tomorrow morning. Here’s the key:
- ✕ Not hero reps.
- ✕ Not perfect rehab theater.
- ✓ Just repeatable progress with fewer bad days.
Table of Contents

Why Bridges Flare Sciatica: The 3 Mechanisms Most People Miss
Nerve sensitivity vs muscle soreness: how to tell in real time
Muscle fatigue feels local and predictable: your glutes burn, recover, and settle. Nerve irritation is moodier. It can travel, tingle, zap, or feel “electric,” especially down one leg. A lot of people mistake one for the other, then push through and wonder why tomorrow feels worse than today.
Pelvic tilt + lumbar extension: when “higher hips” becomes irritation
Higher isn’t always better. When the bridge turns into a low-back arch contest, the load drifts away from glutes and into irritated tissues. I’ve done this myself on autopilot—trying to “finish strong” and waking up with that stubborn posterior chain tension that makes socks feel like a negotiation.
Load tolerance mismatch: the hidden gap between ability and ambition
Your current tolerance matters more than your old PR mindset. Even a technically clean bridge can flare symptoms if volume, range, and frequency jump too fast. The mismatch is usually subtle: one extra set, one harder variation, one “I’m fine” day too soon.
- Local burn is not the same as radiating nerve pain.
- Over-arching the lower back often magnifies irritation.
- Progressions fail when tolerance is guessed, not tested.
Apply in 60 seconds: On your next rep, stop 10% short of your usual top position and compare symptoms immediately and next morning.
Eligibility Checklist: “Should I bridge today?”
- Symptoms are stable or better than baseline: Yes/No
- No spread further down the leg today: Yes/No
- No new weakness, numbness, or odd gait changes: Yes/No
- You can stop at first warning signs: Yes/No
Neutral next step: If any answer is “No,” run a regression session instead of forcing full bridges.
Quick Self-Screen First: Is This Even the Right Exercise Today?
Pain-location map: back-only, buttock-only, or below-knee symptoms
Location changes decisions. Back-only and buttock-only discomfort can still be workable with strict form and light dosing. Symptoms moving below the knee deserve more caution, slower progression, and tighter stop rules.
24-hour response test: what your body says tomorrow matters most
Think like a coach, not a gambler. In-session discomfort can be manageable, but next-day escalation is the loud signal. If symptoms are worse the next morning, yesterday’s dose was too much—period.
Let’s be honest… if symptoms spread down the leg, that’s your red flag
Many of us keep bargaining: “Maybe one more set.” I’ve done the same thing while staring at a mat, pretending effort can overrule physiology. It can’t. Symptom spread is your stop sign, not your challenge coin.
Show me the nerdy details
Practical triage uses behavior over labels: symptom location, intensity trend, and 24-hour recovery curve. A movement that causes temporary local discomfort but returns to baseline by next day can be acceptable in a graded program. A movement that increases radiating symptoms or lingers beyond baseline usually needs regression, reduced range, or substitution.
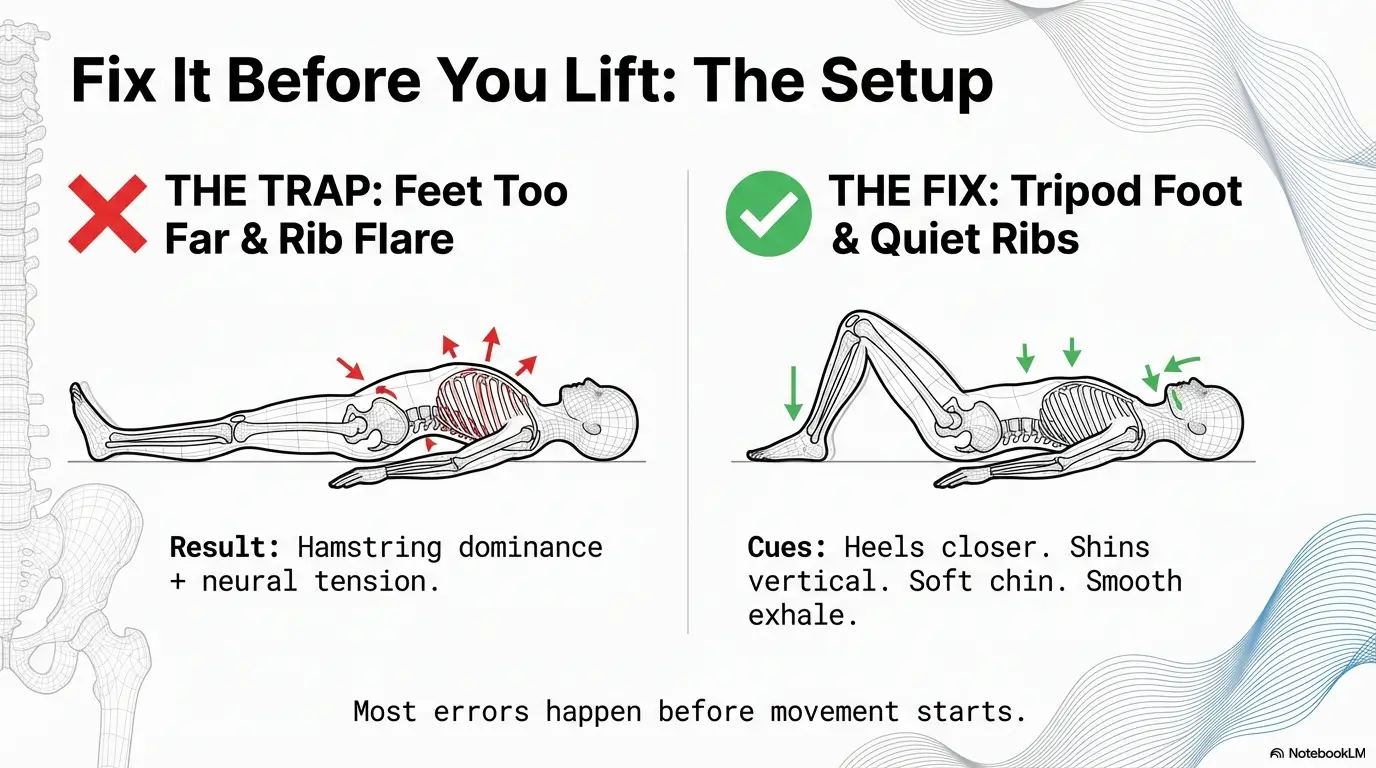
Setup Errors That Trigger Symptoms Before the First Rep
Foot distance trap: too far = hamstring dominance + neural tension
Feet too far from hips often pulls the move toward hamstrings and away from clean glute drive. If your hamstrings cramp before your glutes feel involved, shorten the lever: heels closer, shins more vertical at the top. If hamstrings stay cranky, compare your response to this breakdown on hamstring stretch vs nerve pain patterns.
Rib flare + neck tension: the “brace” mistake that backfires
Over-bracing can become stiff-necked, rib-flared, and breath-held. You don’t need stone abs. You need quiet ribs, easy neck, and a smooth exhale through effort.
Bench/step height mistakes in elevated bridges
Elevated variations are not “more advanced by default.” Too much height can exaggerate range and irritability. If you’re reactive, floor first. Earn elevation later.
- Fast setup cue: “Tripod foot, quiet ribs, chin soft, lift from hips.”
- Tempo cue: 2 seconds up, 2-second hold, 3 seconds down.
- Exit rule: Stop before symptoms sharpen, spread, or feel unstable.
One quick personal note: I once fixed a week-long flare by changing only two things—foot distance and exhale timing. Same exercise, different response.
Common Mistakes: Don’t Do These If Symptoms Are Reactive
Chasing range over control (high bridge, low tolerance)
If the top range requires compensation, it’s not your range today. A lower, controlled bridge beats a high, irritated one every time.
Holding breath to “stabilize” and accidentally spiking tension
Breath-holding can increase global tension and symptom reactivity. A deliberate exhale during lift gives you stability without the pressure spike.
Ignoring asymmetry: one-leg bias during bilateral reps
Watch your knees and pelvis. If one side takes over, bilateral doesn’t mean balanced. Use a mirror or film one set from the front. Two minutes of feedback can save two weeks of irritation.
Decision Card: When A vs B
- A: Keep bridges — symptoms stay local, no next-day spike, form remains crisp.
- B: Swap bridges — symptoms travel, intensity rises next day, or technique degrades by rep 4–6.
Neutral next step: Choose A or B before the session starts, not after you’re fatigued.
Rep-by-Rep Form Cues: A Sciatica-Safer Bridge Checklist
Start position: tripod foot, neutral neck, quiet ribs
Set your feet hip-width, press big toe–little toe–heel evenly, and keep neck long. Think “heavy shoulders, light jaw.”
Up phase: posterior pelvic tilt, then lift—no lumbar “snap”
Initiate by gently tucking the pelvis, then lift as one unit. If you feel a sharp “hinge” in low back, reduce range immediately.
Down phase: slow eccentric, stop before symptom edge
The lowering phase is where control lives. Three seconds down. If symptoms increase while descending, shorten depth and tempo again.
Infographic: Bridge Reps in a Traffic-Light System
🟢 Green (Proceed)
- Local effort only
- No spread below knee
- Next day at baseline
🟡 Yellow (Modify)
- Mild increase during set
- Form starts to drift
- Shorten range or reps
🔴 Red (Stop & Regress)
- Symptoms spread down leg
- Sharp/zapping pain
- New weakness or numbness
Safer Variations Ladder: Regressions to Progressions That Earn Trust
Level 1: Supine isometric glute squeeze (no lift)
Lie on your back, knees bent, feet planted. Gently squeeze glutes 8–12 seconds, 5–8 reps. No lifting, just recruitment.
Level 2: Short-range bridge holds with strict tempo
Lift only a little, hold 5 seconds, lower slowly. Start with 2 sets of 5 reps. If next-day response is calm, keep going for 2–3 sessions.
Level 3: Band-assisted bridge with reduced range
Light band above knees can improve hip alignment for some people. Keep range modest. If band increases discomfort, remove it. Tools are optional, not moral victories.
Level 4: March bridge (only after zero next-day flare)
At top of a controlled bridge, tiny alternating heel lift without pelvic wobble. If the pelvis rotates or symptoms rise, step back immediately.
Level 5: Single-leg bridge criteria (and why most people rush it)
Only progress when bilateral reps are symptom-stable for at least 2–3 weeks, with clean tempo and no next-day payback. Single-leg work is a privilege, not a right.
- Earn each level with symptom stability, not confidence alone.
- One bad progression can erase two good weeks.
- Regressing is strategy, not failure.
Apply in 60 seconds: Pick your current level and write the exact criteria required to move up.
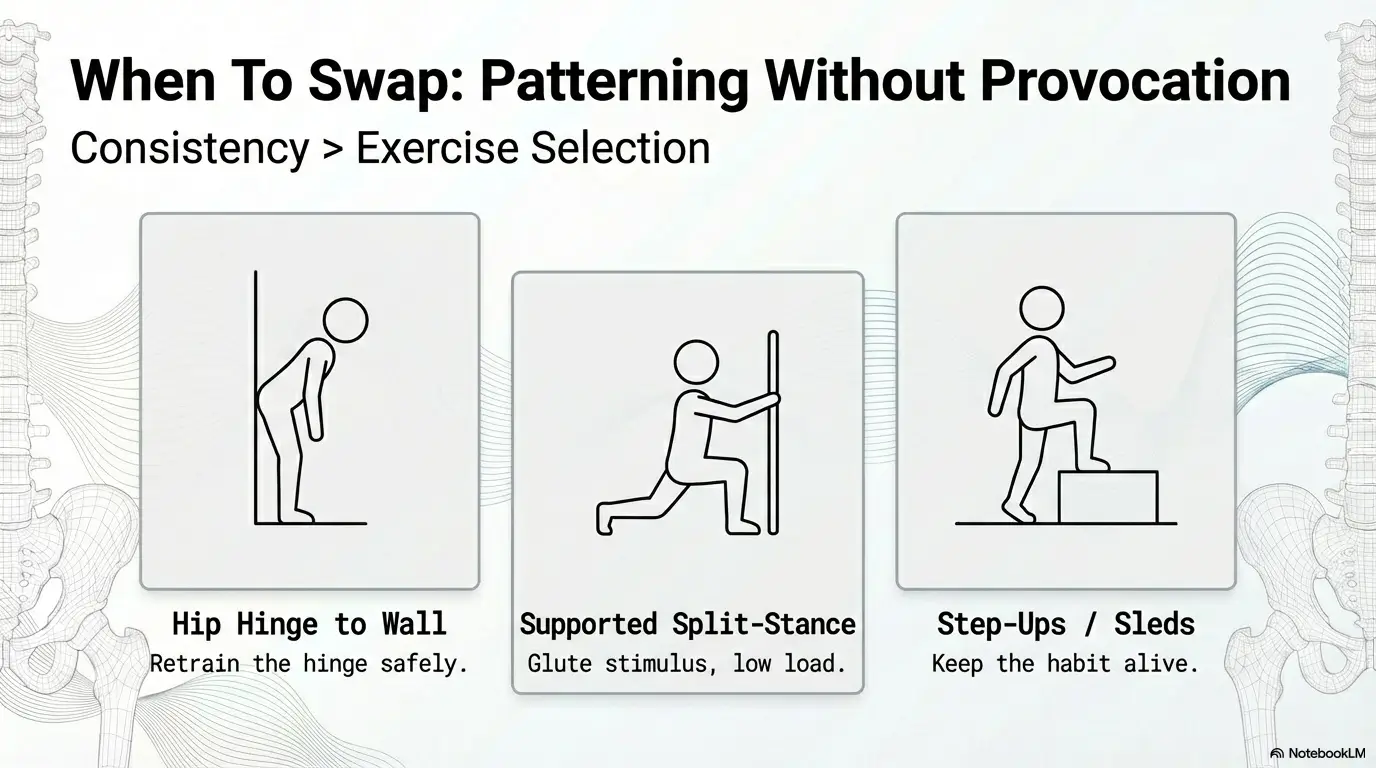
If Bridges Still Irritate You: Swap Patterns, Keep Progress
Hip hinge to wall (glute loading with less provocation)
Stand about 15–25 cm from a wall and push hips back to tap it. Minimal spinal motion, big hip signal. Great for retraining hinge without provoking symptoms.
Split-stance RDL patterning with support
Use a dowel or rack for light support, small range, deliberate tempo. This gives glute stimulus while reducing instability load. If you’re rebuilding core control first, pair this with a dead bug progression for sciatica-sensitive days.
Step-up and sled alternatives for glute strength continuity
Low step-ups with controlled descent, or light sled drags/pushes, often let people train lower body while bridges calm down. These are “keep the habit alive” options.
Here’s what no one tells you… consistency beats “perfect” exercise selection
Some weeks, your best training move is the one that doesn’t flare you tomorrow. I’ve had phases where a humble step-up delivered better month-long progress than any flashy bridge variation. On rough weeks, even a simple walking plan for sciatica flare management can preserve momentum.
Coverage Tier Map: What changes from Tier 1 → 5
| Tier | Movement Demand | Risk of Flare |
|---|---|---|
| 1 | Isometric activation | Lowest |
| 2 | Short-range bridge | Low |
| 3 | Band + controlled range | Moderate-low |
| 4 | March bridge | Moderate |
| 5 | Single-leg bridge | Highest |
Neutral next step: Train one tier below your ego and one tier above your fear.
Programming Rules: How to Progress Without Re-Flare
The 2/10 symptom rule during sets
If symptoms rise above mild (roughly over 2/10), or shift in quality toward sharp/radiating, stop and regress.
The next-day rule: progress only when symptoms return to baseline
Progress is earned after stable next-day recovery, not after one good session. This one rule saves more setbacks than any “perfect cue.”
Weekly variables: adjust one lever at a time (range, load, or volume)
Only one lever per week. If you increased reps, keep range and load fixed. If you increased range, keep reps fixed. This keeps causality clear when symptoms change.
Mini calculator (quick):
Current tolerable reps × sets × pain-response factor.
Example: 6 reps × 2 sets × 1.0 (stable next day) = 12 “green-load units.”
Next week target: 12 × 1.1 ≈ 13 units (small bump only).
Neutral next step: Write your weekly target before training day, not in the middle of fatigue.
Show me the nerdy details
Graded exposure works best when progression is small and recoverable. A 5–15% weekly change is often easier to tolerate than abrupt jumps. The key metric is not pain-free perfection; it is symptom behavior over 24 hours and trend over 2–3 weeks. If training volume management feels slippery, this McGill Big 3 in 10 minutes framework can help anchor your baseline days.
Who This Is For / Not For
For: exercisers with mild, stable, movement-related radiating symptoms
If symptoms are predictable, not escalating, and respond to modifications, this framework can help you keep momentum without gambling.
Not for: severe/progressive neuro signs, trauma-related pain, systemic red flags
If you have rapidly worsening weakness, major numbness patterns, trauma history, fever, unexplained weight loss, or other systemic concerns, this is not a DIY lane.
Borderline cases: when “wait and see” is the wrong strategy
If you’re stuck in a repeat-flare cycle for more than 1–2 weeks despite conservative changes, professional assessment can save time, money, and morale. A structured start with physical therapy for sciatica is often the fastest way to stop guessing.
Quote-Prep List: Bring this to PT/MD consult
- Symptom map (where pain travels, where it stops)
- 24-hour response notes from 7 days
- Top 3 aggravating movements + 2 tolerated alternatives
- Current training frequency, volume, and sleep trend
Neutral next step: Bring objective notes; they improve decision quality fast.
When to Seek Help: Don’t Train Through These Signs
Urgent: bowel/bladder changes, saddle anesthesia, rapid leg weakness
These are urgent neurologic red flags. Stop training and seek immediate medical evaluation.
Prompt medical review: pain worsening beyond a week despite modification
If symptoms keep escalating even after reducing load and range, it’s time for clinician-guided next steps.
PT/MD consult triggers for stubborn, recurring flare patterns
Recurrent flares with routine movements often mean your current plan is underpowered, over-aggressive, or missing a key driver (mechanics, dosage, or adjacent tissue irritability).
One grounded reminder: major institutions like Mayo Clinic and national health services consistently emphasize urgent evaluation for red-flag neurologic symptoms and prompt review when symptoms worsen rather than settle. That guidance exists for a reason.
FAQ
Can glute bridges actually cause sciatica, or just reveal it?
Usually they reveal or aggravate a sensitive system rather than “create” a brand-new condition overnight. Dose, setup, and progression speed are the big levers.
Why do I feel symptoms more the next morning than during the workout?
Because irritability can accumulate after training stress. That’s why next-day response is a better programming signal than in-session bravado.
Are floor bridges safer than hip thrusts on a bench for nerve irritation?
Often yes, because floor range is naturally capped. But safety depends on your mechanics and symptom behavior, not equipment prestige.
Should I stop all glute work if symptoms travel below the knee?
Not always all glute work—often just the provocative pattern. Substitute with lower-irritation options and seek assessment if spread persists or worsens.
Is hamstring cramping during bridges a form problem or a strength issue?
Could be both, but form is the first fix: foot distance, pelvic setup, and tempo. If cramping persists despite clean setup, reduce range and rebuild tolerance gradually.
How many pain-stable sessions before progressing to single-leg work?
A practical baseline is 6–10 stable sessions over 2–3 weeks, with no next-day flare and consistent form.
Do bands help or make sciatic symptoms worse?
They can help alignment for some people and irritate others. Treat bands as optional tools; keep only what improves symptom behavior.
Can walking replace bridges while symptoms calm down?
For many people, yes—short, frequent walks can maintain activity and reduce deconditioning while you temporarily regress bridge work.
Is stretching the hamstrings always helpful for sciatic pain?
Not always. Aggressive stretching can irritate sensitive neural tissue in some cases. Start gentle, monitor 24-hour response, and avoid forcing end range.
When should I ask for imaging vs starting PT first?
If there are urgent neurologic red flags, seek immediate medical care. Otherwise, many cases begin with conservative care and structured rehab before imaging decisions.
Next Step: One Concrete Action You Can Take Today
Run a 7-day “bridge reset”: Level 1–2 only, symptom log, next-day check, then decide progression
Here’s the simple plan:
- Days 1–3: Level 1 only (isometric squeeze), 5–8 rounds.
- Days 4–5: Add Level 2 short-range holds if days 1–3 were stable.
- Days 6–7: Keep volume steady; evaluate next-day trends, not ego.
Short Story: The week I stopped “winning” workouts and started winning recovery
I once had a stubborn flare after what looked like a perfectly normal glute session. Nothing dramatic—just a gradual leg ache that turned electric by bedtime. My old pattern was obvious: push, bargain, regret. So I ran a strict 7-day reset.
Level 1 squeezes, tiny bridge holds, a boring log on my phone. Day 2 felt too easy. Day 3 felt almost insulting. Day 4, I noticed something better than motivation: predictability. By day 7, symptoms were quieter, sleep was better, and I could finally trust a progression plan again. No cinematic breakthrough. Just fewer spikes, better mornings, and training that didn’t steal tomorrow. That’s when it clicked: consistency is the advanced move.
- Use symptom behavior as your coach.
- Progress slowly enough to recover fully.
- Escalate care quickly for neurologic red flags.
Apply in 60 seconds: Start your 7-day reset note now with “baseline today” and one concrete training choice.
Safety / Disclaimer: This article is educational and not a diagnosis or individualized treatment plan. Seek urgent care for new bowel/bladder dysfunction, saddle numbness, or rapidly worsening leg weakness. If symptoms are severe, worsening, or not improving with conservative changes, get medical evaluation promptly.
Last reviewed: 2026-02-07.
