
The Durable Return: Navigating Sciatica & Running
Most runners don’t lose months to sciatica during a run—they lose them by restarting too early, then paying for it 24 hours later.
Sciatica and running can work together, but only when your return is gated by symptom behavior, not by calendar optimism. The real pain isn’t just leg discomfort; it’s the stop-start cycle: one “good” session, one bad flare, then another week of doubt. When nerve symptoms keep shifting, generic comeback plans become expensive guesswork.
Keep winging it, and you risk trading short-term momentum for longer layoffs, deeper fear, and a stride that never feels trustworthy.
This guide gives you a criteria-first return-to-run system: clear readiness gates, a conservative walk-run progression, and stop rules that protect nerve tissue while rebuilding confidence. You’ll know exactly when to progress, when to hold, and when to seek urgent care for red flags.
It’s built on load-response tracking—not hype—using what actually predicts safer outcomes: symptom location, 24-hour response, and whether signs are centralizing or peripheralizing.
The Practical Approach
- ✔️ No heroics.
- ✔️ No vague “listen to your body” fluff.
- ✔️ Just clean decisions you can repeat.
Let’s rebuild your running the durable way.
Returning to running with sciatica should be criteria-based, not calendar-based. Start only when leg symptoms are stable, walking is symptom-controlled, strength asymmetry is minimal, and next-day flare-ups stay within clear limits. Use a walk-run progression, 24-hour symptom checks, and strict stop rules for pain, numbness, weakness, or spreading symptoms. If red flags appear (progressive weakness, bowel/bladder changes, saddle numbness), seek urgent medical care.
Safety note: This is educational guidance, not diagnosis or treatment. Sciatica can come from disc irritation, stenosis, or other causes with different risk profiles. If symptoms are severe, persistent, or worsening, use this with a licensed clinician (sports PT, PM&R, sports medicine).
Table of Contents
Safety / Disclaimer
Let’s start with what matters most: nerves are not the place for bravado. A sore quad after hills is one thing. Progressive weakness, spreading numbness, or sudden bowel/bladder changes are a different universe. If those show up, the plan is not “tweak pace.” The plan is urgent medical evaluation.
In U.S. practice, sports PTs, PM&R physicians, sports medicine MD/DOs, and spine specialists often share care. That’s good news—you don’t need one perfect doorway; you need a competent team and clean symptom data. A tiny notebook can save weeks: symptom location, run dose, and next-morning response are often more useful than a dramatic pain number at 9 p.m. If you need a framework for tracking treatment episodes and documentation quality, this guide on an ERISA-style pain diary workflow can help you structure your notes.
I once watched a disciplined runner do everything “hardcore” and still stall because she tracked only pain intensity. Once she tracked where symptoms moved, progress finally became obvious and safe.

Who This Is For / Not For
Who this is for
- Runners with improving or stable sciatica symptoms who want a criteria-led return.
- People who can walk 30+ minutes with manageable symptoms.
- Athletes willing to track symptoms daily and progress conservatively.
Not for (pause and get evaluated first)
- Progressive leg weakness, foot drop, or worsening neurologic signs.
- New bowel/bladder dysfunction or saddle anesthesia.
- Severe unrelenting night pain, recent trauma, fever, unexplained weight loss, or serious medical history needing immediate rule-out.
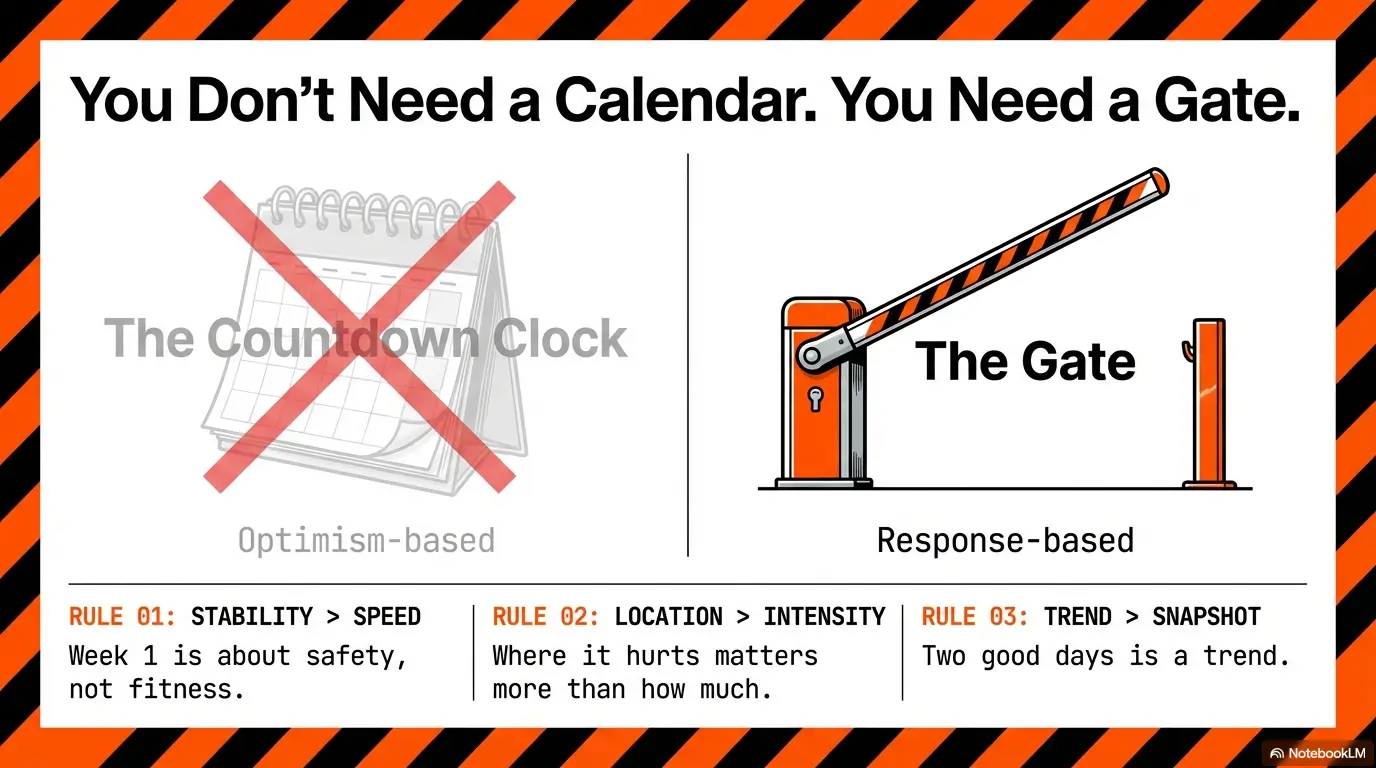
- Stability beats speed in week one.
- Location changes matter more than a single pain score.
- Urgent red flags override every training goal.
Apply in 60 seconds: Write your current symptoms in one line: location, intensity, and whether they spread below the knee.
Criteria First: The 5 Gates Before Your First Run
Most setbacks happen before the first run, not during it. Why? Because the decision to begin was made on hope, not criteria. Use these five gates for seven consecutive days.
Gate 1: Symptom stability over 7 consecutive days
- No upward trend in leg symptoms.
- No expanding numbness/tingling map.
- No new motor changes (trip-catching toes, ankle slapping, sudden weakness).
Gate 2: Baseline function threshold
- Brisk walking 30–45 minutes tolerated.
- Sit-to-stand and stairs without major symptom spike.
- You can finish daily life tasks without “paying for it” all evening.
Gate 3: Strength and control minimums
- Single-leg calf raises: controlled and similar side-to-side.
- Single-leg sit-to-stand from chair height: no obvious collapse.
- Hip control during step-down: knee tracks reasonably, trunk stays quiet.
Gate 4: Irritability score is “low enough”
- Symptoms return to baseline within 24 hours after loading.
- No “next-morning blow-up” after walking or drills.
Gate 5: Red-flag screen is negative
- No progressive neurologic deficits.
- No urgent warning signs.
Think of these gates like airport security for your training plan. Annoying? Maybe. Worth it? Absolutely. If you’re unsure what qualifies as an emergency threshold, review the low-back pain emergency red-flag checklist.
Show me the nerdy details
Nerve irritability is load-response behavior over time, not a single snapshot. A useful rule in early return phases is to allow mild symptom increase during loading only if symptoms settle to baseline by the next day and do not spread further down the leg. Peripheralization (distal spread) generally signals higher irritability than a stable proximal ache. This is why a 24-hour check is often more predictive than “pain during run.”
Not All Sciatica Is Equal: Why Your Cause Changes Your Run Plan
Two runners can both say “sciatica” and need opposite cues. One feels worse with prolonged sitting and repeated flexion; another hates standing and extension-heavy posture. If you copy a plan from a friend, you may copy their trigger too.
Disc-irritable pattern vs stenotic pattern (practical implications)
Disc-irritable runners often tolerate neutral-spine loading and graded reintroduction better than aggressive end-range flexion stretching. Stenotic patterns may prefer brief flexion relief and careful extension exposure. Neither camp gets a free pass; both need dose control. If you’re not sure which bucket you’re in, compare symptom patterns in sciatica vs. herniated disc signs and lumbar stenosis versus herniated-disc differences.
Symptom location matters more than pain intensity
A pain score of 4 that centralizes (moves out of calf toward buttock) can be safer than a pain score of 2 that migrates farther down the leg. That sounds counterintuitive until you’ve lived it. I’ve had athletes panic at “higher pain” while their symptom map was actually improving.
Here’s what no one tells you…
If you track only intensity, you miss the movie and stare at one frame. Track three things: location, latency (when symptoms appear), and next-day rebound.
- Centralization is usually a green trend.
- Peripheralization is a caution signal.
- Next-day response decides progression.
Apply in 60 seconds: Mark today’s farthest symptom point on your leg (hip, thigh, calf, foot).
Run-Readiness Tests You Can Do This Week (No Guesswork)
Before your first run interval, run these screens over 3–5 days. They are deliberately boring. Boring tests prevent exciting setbacks.
Brisk walk tolerance test
Walk 30–45 minutes at a purposeful pace. During and after, note whether symptoms spread lower in the leg. Recheck at 24 hours. If walking itself is your limiting factor, start with these practical adjustments for sciatica pain when walking.
Hop-and-control screen (low-volume)
Do 2–3 sets of 10 very gentle pogos or low hops in place. You’re not testing power; you’re testing nerve tolerance to spring-like loading.
Cadence-friendly form rehearsal
Practice 30–60 second drills with short stride and quick feet. A modest cadence increase often reduces overstride braking and lumbopelvic stress.
Let’s be honest…
If your body “passes” but your threat alarm is screaming, respect that too. Fear can alter gait and muscle guarding, which can mimic poor readiness. Graded exposure is not weakness; it is skill.
Money Block: Eligibility Checklist (Yes/No)
- Walk 30–45 minutes without distal spread? Yes/No
- Symptoms settle to baseline within 24 hours? Yes/No
- No progressive weakness or new neuro signs? Yes/No
- Single-leg control acceptable both sides? Yes/No
- Willing to progress by criteria, not ego? Yes/No
Neutral next step: If all five are “Yes,” begin day 1 walk-run intervals. If not, stay in bridge training and retest in 72 hours.
First 14 Days Back: Walk-Run Progression With Stop Rules
Here’s a conservative template. It is a starting frame, not a mandate. If your symptoms are irritable, stay longer at each phase.
Days 1–4: conservative intervals
- Example: 1 min run / 2–3 min walk × 8–10 rounds.
- RPE easy-conversational.
- Flat route, predictable surface, no hero finish.
Days 5–9: volume before speed
- Keep pace easy; increase total time gradually.
- Example: 90 sec run / 2 min walk × 8–10 rounds.
- One rest or cross-train day between harder load days.
Days 10–14: only one variable changes
- Increase duration or run ratio, not both.
- No hills or speedwork if any peripheralization appears.
- If next-day flare exceeds baseline, regress one step.
Stop rules (non-negotiable)
- Stop session if symptoms spread farther down leg.
- Stop if numbness increases, weakness appears, or gait compensation spikes.
- Abort progression if symptoms fail to settle by next day.
Mini anecdote: One runner insisted she “felt amazing” and doubled day-4 volume on day 5. She felt fine that evening, then woke with calf tingling and limp. We lost nine days undoing one emotional decision. Nerves invoice late.
Show me the nerdy details
Why walk-run first? Alternating load gives neural tissue and sensitized structures micro-recovery windows while preserving running-specific motor patterns. Continuous easy running can work later, but early in return phases, interval density controls risk better than distance goals. On non-run days, a recumbent vs. upright bike comparison for sciatica can help you choose lower-risk cardio.
Don’t Do This: 7 Mistakes That Trigger Re-Flare
Mistake #1: Passing pain to “earn” fitness back
Fitness debt is real. Nerve debt is expensive. If the price is distal spread, it’s not a win.
Mistake #2: Testing speed too early
Speed magnifies form errors and load peaks. Bank consistency first.
Mistake #3: Ignoring 24-hour response
Same-day “felt fine” is not clearance. Morning-after behavior is the judge.
Mistake #4: Long sitting after first run-back sessions
For many runners, hard run + long seated work block is a perfect irritability cocktail. A simple sit-stand schedule for desk-job sciatica can reduce post-run flare risk.
Mistake #5: Returning on old shoes + old stride habits
Worn shoes, overstride, and low cadence can quietly raise risk. If footwear is questionable, start with these principles for sciatica-friendly walking shoes before changing too many variables at once.
Mistake #6: Copying someone else’s protocol
Diagnosis labels match. Irritability profiles don’t.
Mistake #7: Progressing on a “good day” spike
Great day? Wonderful. Confirm it twice before upgrading.
- Do not stack speed + volume increases.
- Respect delayed symptom behavior.
- Protect your post-run recovery window.
Apply in 60 seconds: Pick your “one non-negotiable” stop rule and write it at the top of your training log.
Load Math That Works: Progression Rules for Irritable Nerves
“How much can I add?” is the right question. The useful answer is a range with conditions.
The 10–20% weekly load band (context, not dogma)
Use the lower end (around 10%) if symptoms are recently irritable; move toward 15–20% only when next-day responses stay calm for at least two exposures. If symptoms destabilize, the band is irrelevant—regress.
Two-green-days rule before progression
Need two symptom-stable sessions before adding load. One lucky day is weather; two is trend.
Regression ladder (what to cut first)
- Cut intensity (pace/hills).
- Then cut duration.
- Then reduce weekly frequency if needed.
Money Block: Mini Calculator (Simple)
Input 1: Last week total run minutes
Input 2: Current irritability (Low / Moderate / High)
Input 3: 24-hour response (Stable / Unstable)
Output rule: Stable + Low irritability: add 10–15%. Stable + Moderate: add 5–10%. Any Unstable response: add 0% and regress one rung.
Neutral next step: Set your next week minutes before your first session, not after a “good run” high.
Strength & Mobility Priorities That Actually Transfer to Running
You don’t need a circus rehab menu. You need a small set that actually carries over to stride mechanics and tissue tolerance.
Hip extension and calf capacity first
- Split squat or step-up patterns (pain-limited range).
- Calf raise progressions (straight knee and bent knee variants).
- Bridge or hip hinge variations that don’t provoke distal symptoms. If bridges are a main pillar in your plan, use this progression for glute bridge setup when sciatica is irritable.
Trunk stiffness + breath strategy
Think “quiet trunk, free legs.” Bracing isn’t breath-holding. Coordinate exhale with effort to keep spinal loading controlled without rigid guarding. Many runners do well with concise trunk routines like the McGill Big 3 in 10 minutes and dead-bug variants from this guide to the dead bug exercise for sciatica.
Mobility: dose for tolerance, not max range
Aggressive end-range stretching into nerve irritation is a common own-goal. Use gentle mobility that improves movement options without symptom spread. If you’re unsure whether your “hamstring tightness” is true muscle stiffness or neural sensitivity, compare patterns in hamstring stretch vs nerve pain.
One of my favorite reality checks: if a mobility drill gives instant “freedom” but your next morning is worse, it wasn’t freedom—it was a preview bill. This is also why some people flare after overdoing flosses; see why sciatic nerve flossing can feel worse before better.
Show me the nerdy details
Early return phases prioritize capacity in tissues that absorb running load (calf-soleus complex, hip extensors) plus lumbopelvic control. Neural sensitivity often improves with graded loading and reduced threat signaling, not maximal stretching. Favor repeatable, symptom-neutral exposures over dramatic single-session gains.
Common Mistakes (Quick Audit Checklist)
Programming mistakes
- Too many hard surfaces too soon.
- No deload week in first month back.
- Adding strides/hills while still uncertain on next-day response.
Monitoring mistakes
- Tracking only intensity, not symptom spread.
- No log for sleep/stress, even though both influence irritability.
- Ignoring pattern changes in numbness map.
Decision mistakes
- “No pain now = no problem later” assumption.
- Upgrading pace before consistency.
- Confusing motivation with readiness.
Money Block: Decision Card (When A vs B)
When A: Symptoms stable, no peripheralization, next-day calm → choose volume progression (small increase in total time).
When B: Symptoms variable, stress high, sleep poor → choose hold week (repeat prior load).
Time/cost trade-off: A hold week “costs” 7 days but often saves 14–28 days of relapse management.
Neutral next step: Decide your week type (Progress / Hold / Regress) before the first run.
When to Seek Help (Do Not Self-Manage Past This Point)
Urgent care now
- Bowel/bladder changes, saddle anesthesia, rapidly progressive weakness.
Prompt clinical follow-up
- Persistent neurologic symptoms beyond 2–4 weeks.
- Repeated flare cycles despite criteria-based progression.
- Night pain or function loss that keeps worsening.
Who to see in the US
- Sports physical therapist (return-to-run programming and symptom response).
- PM&R physician (function-focused medical management).
- Sports medicine MD/DO (load decisions, differential diagnosis, return timelines).
- Spine specialist when significant neurologic findings or persistent deficits exist.
Natural-language evidence cue: National Library of Medicine resources on sciatica describe symptoms and urgent warning patterns; major neurology and orthopedic groups similarly emphasize emergent red flags and early evaluation when neurologic deficits progress. For treatment-pathway orientation before specialist visits, see herniated disc sciatica treatment options and what to expect from physical therapy for sciatica.
Next Step (One Concrete Action)
Do this today
Run a 7-day readiness log. Track these four items daily:
- Symptom location (highest point and farthest distal point).
- Walk tolerance (minutes, pace feel).
- Morning-after response (better/same/worse).
- One strength marker (e.g., single-leg calf raises per side).
If all five gates are met by day 7, start day 1 of your conservative walk-run cycle.
Infographic: Sciatica Return-to-Run Flow
7 days symptom stability
Walk 30–45 min + 24h settle
Run-walk start (easy pace)
Peripheralization, weakness, new numbness
Progression rule: Two green sessions before any increase. Change one variable only.

FAQ
Can I run with sciatica, or should I stop completely?
Sometimes you can run, but only when symptoms are stable and criteria are met. If symptoms are worsening, spreading distally, or paired with neurologic changes, pause and get evaluated. “Active recovery” is not the same as “push through anything.”
What are the exact signs I’m ready to run again after sciatica?
Use the five gates: 7 days stable symptoms, 30–45 minute brisk walk tolerance, acceptable single-leg strength/control, symptoms settling within 24 hours after loading, and a negative red-flag screen.
Is walk-run better than continuous easy running for nerve pain recovery?
In early return phases, often yes. Walk-run intervals control dose and reduce continuous loading time. Many runners transition to continuous easy running after symptom stability proves itself across multiple sessions.
How do I know if symptoms are centralizing vs getting worse?
Centralizing means symptoms move out of the calf/foot toward thigh or buttock over time. Worsening often shows as distal spread, increasing numbness area, or slower next-day recovery.
Should I avoid hills, speedwork, or trails during return-to-run?
Early on, yes—usually avoid all three until you demonstrate stable next-day response on flat, easy sessions. Reintroduce one variable at a time, with at least two stable exposures before adding another challenge.
How long should symptoms last after a run before I worry?
A practical rule: mild symptoms may occur during loading but should settle to baseline by the next day. If symptoms remain elevated beyond 24 hours or spread distally, treat that as a warning and regress.
Can cadence changes reduce sciatica flare risk while running?
For some runners, a modest cadence increase can reduce overstride and braking forces, which may lower symptom provocation. Keep changes small and test response over 24 hours.
Do I need imaging (MRI) before returning to running?
Not always. Imaging decisions depend on neurologic findings, severity, duration, and red flags. Many runners return safely using clinical assessment and criteria-based progression. Seek imaging sooner when deficits are progressive or red flags are present.
What shoes are best when returning from sciatica?
There is no universal “sciatica shoe.” Prioritize comfort, stable fit, and predictable feel. Avoid major abrupt changes during early re-entry unless current shoes are clearly worn out or aggravating symptoms.
When is sciatica dangerous enough for urgent care?
Urgent evaluation is needed for bowel/bladder changes, saddle numbness, or rapidly progressive weakness. Those are not training adjustments—they are medical emergencies.
Conclusion
We opened with one promise: no countdown clocks, no motivational theater—just criteria that protect your nerve and rebuild trust in your stride. Here’s the loop-closing truth: confidence doesn’t return because you run farther; it returns because your data keeps matching your plan. That’s how your nervous system stops bracing for betrayal.
In the next 15 minutes, set up your 7-day readiness log, choose one stop rule, and schedule your first conservative run-walk only if all gates pass. If they don’t, that’s not failure; it’s intelligent timing. The finish line is not “fast again by Friday.” The finish line is durable running without panic.
Last reviewed: 2026-02.
