
Decoding the Shift: Managing Sciatica in the Workplace
Sciatica at a warehouse or standing job rarely becomes unbearable all at once. More often, it steals the shift in small installments: one long station block, one concrete floor, one pair of “still good” shoes, and one bad hour when your back and leg decide the bill is due.
That is why so many workers misread the problem. They blame standing in general, buy the softest shoes they can find, or wait until pain is loud enough to negotiate with. But standing jobs are not all the same, and sciatica-like pain at work is often less about total hours on your feet than static posture, poor task sequencing, hard surfaces, and footwear that stops helping halfway through the day.
Keep guessing, and you can lose more than comfort. You can lose pace, consistency, and the ability to finish the last third of the shift without compensating your way into a worse flare.
This guide helps you build a smarter rotation plan, choose work shoes for stability instead of shelf comfort, and spot the floor and station problems that quietly keep symptoms alive. It does that with a practical lens: flare timing, load patterns, shoe wear, micro-breaks, and ergonomic fixes that make sense in the real workplace.
- ✕ No miracle talk.
- ✕ No “just push through it.”
Just a calmer, more usable way to make the shift stop feeling like a dare. Because the useful question is not whether you are tough enough. It is whether your system is.
Fast Answer: For standing-job sciatica, the safest practical strategy is usually not “tough it out” or “buy softer shoes.” It is a rotation plan that changes load before pain spikes, combined with stable, task-appropriate footwear, firm footing, and workstation tweaks that reduce prolonged static standing. If pain is severe, worsening, or comes with weakness, numbness, or bladder or bowel changes, get medical help promptly.
Safety / Disclaimer: This article is informational only and is not medical, legal, or workplace safety advice. Sciatica-like pain can come from different causes, and the right plan depends on symptoms, job demands, footwear rules, and medical history. In the U.S., workplace changes may also intersect with employer policies, safety requirements, and formal ergonomic processes.
Table of Contents

Who this is for / not for
This is for workers whose pain flares during long standing, walking, picking, packing, or line work
If your shift has a rhythm of standing, scanning, reaching, pushing, pivoting, and pretending you are “basically fine” while your leg quietly writes a complaint letter, this guide is for you. Warehouse workers, retail-floor workers, manufacturing staff, stockroom crews, grocery back-room teams, and anyone on hard floors for hours at a time usually do not need a dramatic speech. They need a plan that still works at 3:40 p.m.
This is for supervisors and safety-minded leads trying to reduce flare-ups without vague “just rest more” advice
Good leads know that “take it easy” is not a system. It is a wish wearing a lanyard. The practical question is whether the shift can be arranged to change load before pain escalates, whether the station can be modified, and whether footwear and floor conditions are setting people up to fail. OSHA’s ergonomics guidance leans toward changing tools, tasks, and work practices because reducing physical demands is usually more reliable than asking a hurting worker to simply endure more.
This is not for sudden severe leg weakness, saddle numbness, or loss of bladder or bowel control
Those symptoms are not “monitor it and see.” If you need a clearer sense of what counts as urgent, review the warning signs in cauda equina syndrome red flags. MedlinePlus and other mainstream medical references consistently treat bowel or bladder changes, new weakness, and significant numbness as escalation signs that need prompt medical attention.
This is not for self-diagnosing every back or leg pain problem as sciatica
Sciatica describes a symptom pattern, not a personality type and not a one-size-fits-all explanation. Some people have nerve irritation. Some have back pain with referred leg pain. Some have a footwear-and-floor problem sitting on top of a low-back problem. Sometimes the first useful distinction is whether it feels more like hip vs spine pain. The label matters less, at first, than the pattern: what loads it, what eases it, and what red flags are present.
- Separate routine flare patterns from true red flags
- Think in tasks, surfaces, station time, and footwear
- Use work language, not just pain language
Apply in 60 seconds: Write down the first exact task and hour when symptoms reliably begin.
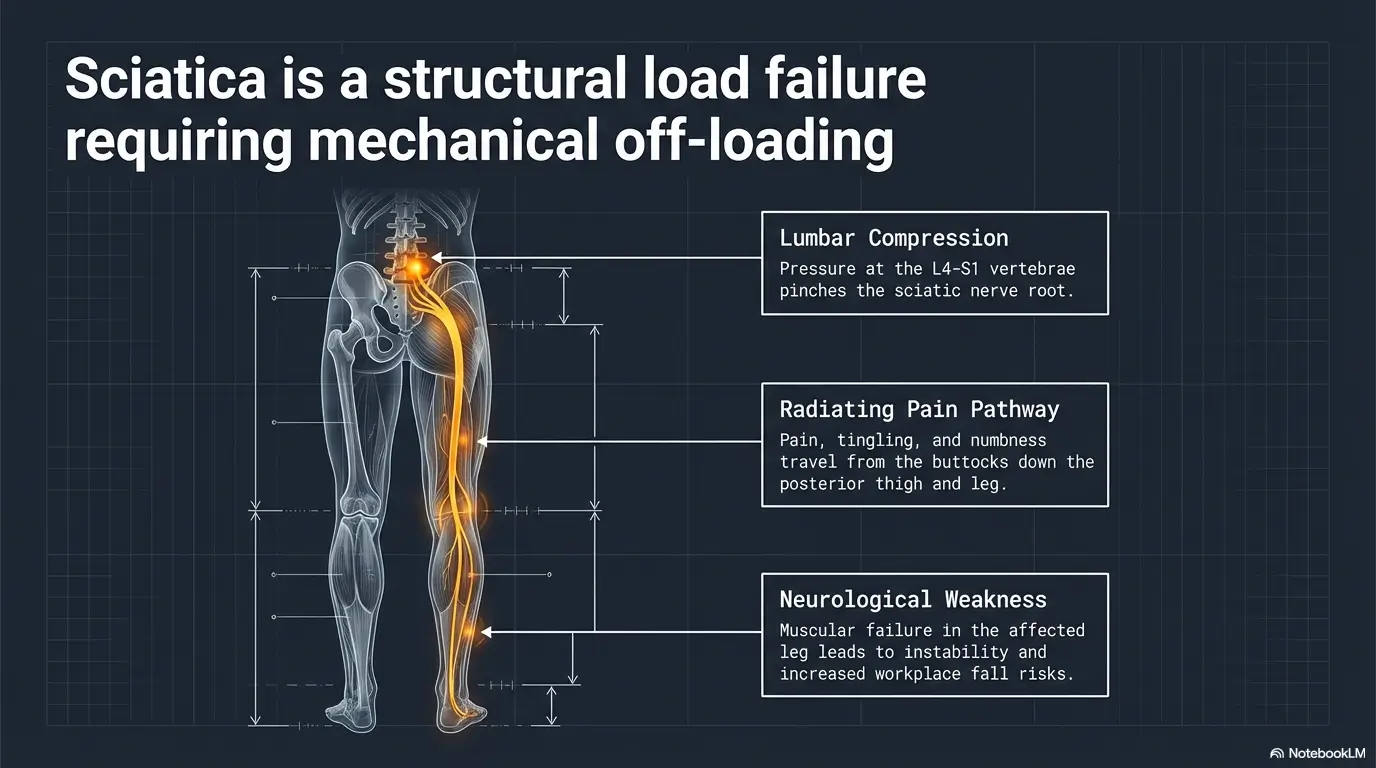
Start with the real problem: standing is not the same as moving
Prolonged standing loads the day differently than walking routes and mixed-motion tasks
This is the first misunderstanding that wastes good energy. Workers often say, “I’m on my feet all day,” as if all on-your-feet time is one bucket. It is not. A job with mixed walking, light carrying, and posture changes often feels very different from a fixed station where you stand nearly still, make short repetitive reaches, and twist in the same 12 inches of space for hours. Static standing has its own nasty little physics. The body does not love being a coat rack.
Static posture is often the hidden aggravator, not just total hours on your feet
CDC and NIOSH materials have long described static standing as a contributor to back and leg discomfort, especially when workers cannot change posture easily. That matters because many people chase the wrong villain. They blame steps when the real issue is stillness. They blame “bad feet” when the actual problem is that their station requires them to hover over one spot like a lighthouse with payroll deductions.
The pain spike after lunch may tell you more than the pain spike at clock-out
One of the most useful clues is timing. If pain rises sharply after a long block at one station, that points toward load concentration. If it builds late in the shift after lots of walking and lifting, accumulated fatigue may be the bigger story. If your symptoms tend to worsen during movement as much as during standing, it can help to compare that pattern with a broader guide to sciatica pain when walking. I once watched a worker swear the last hour was the problem, then track the shift and discover the real trigger lived in a 95-minute repacking station before lunch. The clock-out pain was just the bill arriving.
Useful frame: Ask not “How long was I on my feet?” Ask “How long was I in the same posture, on the same surface, in the same shoe, doing the same reach pattern?” That question usually tells the truth faster.
| Pattern | More likely problem | First move |
|---|---|---|
| Pain rises during fixed station time | Static load and posture concentration | Break station time into shorter blocks |
| Pain rises after long walking routes | Accumulated impact and fatigue | Audit footwear wear, pace, and route recovery windows |
| Pain rises with twisting and reaches | Station geometry and awkward posture | Change cart height, reach distance, or part placement |
Rotation first, not heroics: the shift plan that usually works better
Rotate before symptoms peak, not after the nerve is already angry
The most common scheduling mistake is waiting for pain to become obvious before changing tasks. By then, the body is already compensating. Hips hitch. Stride changes. Trunk position gets weird. The worker starts making tiny bargains with gravity. A smart rotation plan moves earlier. It treats the first 60 to 120 minutes as a prevention window, not a test of character.
Alternate standing, walking, light movement, and seated or lower-load tasks where possible
Task rotation works best when the tasks are genuinely different. Switching from one standing station to another standing station that uses the same reach pattern is not rotation. It is redecorated repetition. OSHA examples across several industries repeatedly emphasize rotating workers through tasks that use different body parts or motion patterns, and using sit/stand options or supportive changes where feasible. If your workplace also includes office time, a related comparison of standing desk sciatica can help clarify why posture variety matters more than slogans about standing being “better.”
Build a “high-load, medium-load, recovery-load” task rhythm instead of stacking the hardest stations back to back
A practical sequence often looks like this:
- High-load: lifting, sustained bending, fast-paced picking, frequent twisting
- Medium-load: walking routes, stocking, lighter pack-out, scanning with movement
- Recovery-load: seated admin, label work, quality checks with posture change, light bench work, or a station with anti-fatigue support and reduced reach
That rhythm matters because the body is not a forklift battery. You cannot drain it flat and expect a ten-minute break to perform wizardry.
Let’s be honest… most rotation plans fail because they are based on staffing convenience alone
That is the uncomfortable truth. Many schedules are built around coverage, not load balance. Coverage matters, of course. But if one worker spends 3.5 hours stacked in the most static or twist-heavy role because “they’re fastest there,” the plan is borrowing from tomorrow’s functioning. A better system identifies the highest-load stations first, then limits uninterrupted time there.
Eligibility checklist: Is your current shift plan ready for a real sciatica-aware rotation?
- Yes / No: Can at least one high-load task be capped before pain usually starts?
- Yes / No: Is there at least one true lower-load station in the sequence?
- Yes / No: Are workers changing posture and motion pattern, not just location?
- Yes / No: Does the team know the trigger hour instead of guessing?
Neutral next step: If you answered “No” twice or more, start with one shorter station block tomorrow instead of redesigning the whole shift at once.
Practical line for a manager: “I’m not asking for less work. I’m asking for a different sequence so symptoms don’t spike and productivity doesn’t fall off a cliff in the last third of the shift.”
The two-hour trap: why “I was fine until suddenly I wasn’t” keeps happening
Early fatigue changes posture long before workers notice it
The shift rarely announces the problem with trumpets. It sneaks in through mechanics. Your first hour might feel normal. Your second looks normal from across the room. But if someone filmed your posture, they would often see the drift before you feel the verdict. Slight lean. Reduced hip motion. More trunk sway. A protective limp that starts as a suggestion and ends as a habit.
Foot pressure, trunk position, and tiny compensations can snowball across a shift
This is why “I was okay until I wasn’t” is such a common report. The pain spike is late, but the setup began much earlier. A shoe losing stability. A station too low. A floor too hard. A pace too fixed. A twist repeated 200 times. None of these alone looks cinematic. Together, they form a little weather system, and by mid-shift the storm arrives.
The last third of the shift is often where bad footwear reveals itself
New shoes can be charming liars. At minute 30, many shoes feel decent. At minute 430, the truth comes out. If the heel is collapsing, the midsole is cooked, the outsole is uneven, or the upper lets the foot wander, your body spends the afternoon doing quality-control work it never applied for.
I learned this lesson the boring way, which is the expensive way. I once blamed a whole month of worsening standing pain on workload. Then I looked at the outsole of the shoes I kept calling “still good.” One side was worn like a bad confession. The body had been telling the truth. I had simply been listening to the calendar instead of the shoe.
Footwear strategy, not shoe roulette
Stability matters: soft is not always supportive
This is where many workers get trapped by shelf comfort. A very soft shoe can feel heavenly for 20 minutes and oddly punishing by late shift if it lets the foot wobble, sink, or fatigue. “Supportive” is not code for hard and joyless. It means the shoe helps you stay steady when the floor, pace, and repetitive motion begin asking more of you.
Match the shoe to the floor, the pace, and the load, not just the pain label on the box
A warehouse floor is not a treadmill. A retail floor is not a clinic hallway. A manufacturing station is not a weekend errand. Shoes need to match the actual environment:
- Hard concrete: often rewards stable cushioning and reliable outsole grip
- Frequent pivoting: needs secure heel hold and upper control
- Safety-toe or policy-mandated footwear: may require fit adjustments, sock changes, and more aggressive replacement timing
- Mixed walking plus static standing: usually demands balance, not the softest possible foam
Outsoles and traction matter because firm footing affects back-load risk
OSHA guidance for standing work and service roles often points to shoes designed for prolonged standing and walking on hard surfaces, and it also emphasizes floor conditions and traction. That matters because unstable footing does not stay a foot problem. When the shoe-floor relationship gets sketchy, the back and hips often pick up the tab. If you are comparing options, it can help to see how this overlaps with broader advice on sciatica-friendly walking shoes.
Replace worn shoes on wear-pattern evidence, not wishful thinking
A worker can tell a thousand noble stories about why a pair is “not that old.” None of those stories fixes heel collapse. Use evidence instead:
- Uneven outsole wear from left to right
- Visible tilt when the shoes sit on a flat surface
- Heel counter that folds too easily
- Midsole flattening with poor rebound
- Traction worn smooth in the high-contact zones
Show me the nerdy details
For long standing, the shoe is doing at least four jobs at once: distributing pressure, keeping the foot from excessive motion inside the upper, maintaining predictable contact with the floor, and controlling what happens when fatigue makes your gait sloppier. A shoe that is pleasant at rest but unstable under repetitive standing or pivoting can increase the amount of small corrections your body makes across a shift. Those tiny corrections are easy to ignore and hard to outrun.
- Audit stability, traction, and wear pattern together
- Match shoe choice to floor and task, not marketing copy
- Retire shoes when evidence says so
Apply in 60 seconds: Put both shoes on a table and compare heel wear from behind.
| Footwear pattern | What often feels good early | What may show up later |
|---|---|---|
| Ultra-soft max cushion | Immediate plushness | Possible fatigue if control feels mushy during long standing |
| Stable cushioned work shoe | Less flashy comfort, more grounded feel | Often better consistency over full-shift use |
| Old “broken-in” pair | Familiarity | Hidden instability, lost traction, uneven loading |
Don’t do this: the footwear mistakes that quietly prolong a flare
Swapping into ultra-soft shoes that feel good for one hour and worse by hour six
This is the classic rebound mistake. A flare starts, you panic, and you buy the softest shoe in a 20-mile radius. The first day feels promising. By late week, you realize the relief had a half-life. Softness can help some workers, but on hard floors and long shifts, too much softness without enough control can feel like standing on a persuasive marshmallow. Charming. Not always loyal.
Ignoring heel collapse, outsole wear, or uneven compression
The body notices these things even when the eye refuses. Uneven compression changes how load travels up the chain. That does not mean every ache is a shoe tragedy. It does mean worn shoes should be treated as evidence, not sentiment.
Treating insoles as a magic fix when the base shoe is unstable
Insoles can help with pressure distribution or fit, but they rarely rescue a collapsing structure. If the base shoe is unstable, an insole may just become a decorative witness.
Here’s what no one tells you… “comfort on the shelf” and “comfort at minute 430” are different tests
The store test is not useless. It is just incomplete. A better test asks four questions: Does the shoe hold you securely? Does the forefoot bend where your foot bends? Does the heel stay controlled? Does the outsole still feel reliable on your actual floor? Work comfort is a long-novel problem, not a first-date problem.
Quote-prep list: before spending money on another pair, gather these details:
- What hour symptoms rise
- Which stations worsen or ease them
- Whether symptoms are worse in fixed standing or walking
- How the outsole looks today
- What workplace footwear rules apply
Neutral next step: Bring the old pair and a photo of outsole wear when comparing replacements.
Floor, station, and surface: the part most articles leave in the shadows
Hard concrete changes the equation even when the shoe is decent
This deserves plain language: concrete is not neutral. It is an amplifier. A decent shoe on concrete can still produce a rough day if station time is long and posture change is limited. Many workers keep swapping shoes while never auditing the surface and station design, which is a little like changing umbrellas during a leaking-roof problem.
Anti-fatigue mats can help in fixed stations but can be awkward in fast-transfer zones
OSHA materials across multiple standing-work examples mention anti-fatigue mats, footrests, and sit/stand supports where feasible. That “where feasible” matters. A mat can be helpful at a fixed bench and annoying or unsafe in a fast movement lane. Use them where workers stand in one place, not where they need frictionless transitions, carts, or rapid pivots.
Reach distance, twist frequency, and cart height can matter as much as shoe choice
A station that forces repeated twisting or reaching away from the body can turn a tolerable shift into a punishing one. Raise a cart, change item placement, shorten reach distance, or re-stage frequently used materials and you may reduce symptoms more than a shoe swap alone ever could. I have seen workers spend weeks researching shoes when a cart handle 3 inches too low was the daily villain all along.
Infographic: What usually drives a flare on a standing job
1. Task Load
Lifting, twisting, repetitive reaches, fast pace, fixed stations
2. Surface
Concrete, slippery zones, no mat, poor footrest options
3. Footwear
Stability, traction, heel wear, fit, replacement timing
4. Timing
How long before posture drifts, pain rises, and productivity drops
Bottom line: flares usually come from a system, not one cursed object.
Common mistakes
Waiting until pain hits 8 out of 10 before changing tasks
By then, you are not preventing anything. You are negotiating with a flare already in progress. Preemptive rotation works better because it respects how pain builds in layers.
Building a rotation plan with no actual low-load station in the sequence
Some plans look impressive on paper and cruel in practice. If every station is standing-heavy, twist-heavy, or pace-heavy, then the worker is just touring the same problem in different lighting.
Assuming more cushioning always means less nerve irritation
Sometimes yes. Sometimes no. The real issue is whether the whole setup reduces the daily load pattern. Shoes are one vote in that election, not the entire government.
Keeping the same worn pair because “they’re already broken in”
Broken in is not always a compliment. Sometimes it means broken down.
Treating every morning as a reset when yesterday’s load still counts
This one is sneaky. A worker wakes up “not too bad” and assumes yesterday is gone. Then the same station, same surface, same shoe, same timing recreates the same flare. Patterns love repetition. They thrive on amnesia.
Mini calculator: estimate whether a station block is too long. Take the hour symptoms usually start, subtract 20 to 30 minutes, and use that earlier time as your first rotation target. If symptoms usually rise at 2 hours, your first experiment is a 90 to 100 minute cap. Neutral next step: test one earlier swap for three shifts before judging it.
Micro-breaks that do not look like slacking
Use brief unload windows to change posture, not just stand in a different kind of stillness
Not every job allows formal breaks on demand. But many jobs allow tiny transition windows. Use them well. The point is not to pause theatrically. It is to unload tissues that have been doing the same thing too long. Shift weight. Walk a short loop. Rest one foot briefly on a support if available. Lean at a sit/stand perch when permitted. Change the sentence your body has been forced to repeat.
Pair task transitions with tiny resets so recovery becomes automatic
The best micro-breaks are attached to something that already happens. End of a tote cycle. Pallet change. Scanner reset. New cart. Label batch completion. When recovery is built into the workflow, it stops looking like a personal favor and starts functioning like a process.
Supervisors get better results when relief timing is preplanned instead of negotiated mid-flare
This matters more than people think. A worker in the middle of a pain flare is not in a great position to make persuasive operational arguments. Preplanning small relief windows removes drama from the equation. Less pleading. More procedure. Everyone gets to keep their dignity, which is not a small thing.
I have seen the difference in tiny details. When a team expects one 60-second unload moment every cycle change, nobody side-eyes it. When the same worker suddenly needs relief at random, the room reads it as disruption. Same body. Different script.
- Use existing transitions instead of waiting for perfect conditions
- Change posture, not just location
- Preplanned relief usually gets less resistance
Apply in 60 seconds: Pick one repeatable task transition and attach a 30 to 60 second posture reset to it.
When a rotation plan needs manager buy-in, not just personal discipline
Symptoms that predict a productivity drop before the worker admits it
Managers do not need a medical seminar. They need early operational signs. Slower turns. Shorter stride. More pausing before lifts. More frequent hand-to-back moments. Less clean pivoting. More repositioning at the same station. Workers often hide pain until performance starts fraying at the edges.
How to describe the problem in work terms: load, station time, walking bursts, and flare points
This is the language that tends to travel well:
- “Symptoms rise after 90 minutes at Station B.”
- “Walking tasks are easier than fixed standing.”
- “The problem is worse on concrete with the older pair.”
- “Twisting to the right during repacking is the main flare trigger.”
Notice what is missing. No melodrama. No vague “everything hurts.” Just usable information. Managers can act on patterns more easily than on suffering, even when the suffering is very real. If a formal workplace request becomes necessary, it may help to see examples of ADA accommodations for sciatica doctor note wording or a broader ADA accommodation letter for back pain.
A useful plan sounds operational, not dramatic
Try something like this: “I can probably stay more consistent if we cap that station at 75 minutes, then move me to the walking route or bench check for one cycle before I go back.” That sentence has a pulse, but it also has a structure. It respects the shift while telling the truth.
Coverage tier map:
- Tier 1: Worker self-tracks timing and shoe wear only
- Tier 2: Team adjusts station order informally
- Tier 3: Lead caps time at high-load stations
- Tier 4: Supervisor adds equipment or station changes
- Tier 5: Formal ergonomic review or medical process enters the picture
Neutral next step: Figure out which tier you are actually in before asking for a tier-five solution to a tier-two problem.
Don’t do this either: the pacing errors that make “light duty” oddly painful
Trading lifting for endless static standing
This is one of the great workplace ironies. A worker gets moved off heavier tasks and lands in a station that involves less lifting but more standing still. On paper, that can look easier. In the body, it may feel worse. Lower force is not automatically lower strain if posture barely changes.
Moving from one repetitive reach pattern straight into another
Again, variety matters. Two “lighter” tasks can still pile load onto the same structures if both demand the same trunk angle, the same reach distance, or the same fixed stance. Light duty should not mean the exact same movement in softer language.
Believing no-lift automatically means low-strain
No-lift can still mean long standing, awkward wrist position, repetitive scanning, frequent turning, and a station too low or too far away. This is why the best plans are not built from job titles alone. They are built from posture, movement pattern, and timing.
Short Story: The station that looked merciful on paper
One worker I knew was relieved out of the “hard” picking role after a run of back-and-leg flares. Everyone felt virtuous. The replacement assignment was a quality-check station with almost no lifting. Beautiful, on paper. In real life, it pinned him in one place on concrete, with a slight forward lean, short repetitive reaches, and a twist to set items aside. For the first 40 minutes, he felt lucky.
By the second hour, his leg symptoms were louder than they had been on the walking route. The lesson was not that managers were uncaring. They were trying. The lesson was that lighter force did not equal lighter load. Once the team broke that station into shorter blocks and alternated it with a moving task, things improved. Not miraculously. Not perfectly. But enough that the shift stopped feeling like a dare.
When to seek help
Pain that is severe, worsening, or not settling with basic load changes
If symptoms are escalating despite sensible changes in station time, footwear, and recovery windows, it is time to stop treating the problem like a stubborn mood. Persistent or worsening symptoms deserve medical evaluation, especially if work is becoming harder to perform safely.
New numbness, weakness, foot drop, or trouble walking normally
MedlinePlus describes sciatica as potentially involving pain, weakness, numbness, or tingling in the leg. When weakness enters the story, the stakes change. New trouble lifting the foot, pushing off, or walking normally is not a “wait until next month” signal. For people trying to make sense of the nerve pattern itself, a quick comparison of L4 vs L5 vs S1 sciatica can sometimes make symptoms feel less mysterious.
Loss of bladder or bowel control, or saddle-area numbness, needs urgent evaluation
This is the clearest escalation line in the whole article. If bladder or bowel changes, new severe numbness in the saddle area, or serious neurologic changes appear, seek urgent medical care. That is not workplace grit territory. That is medical territory. If you are unsure whether a situation has crossed into emergency territory, review low back pain emergency signs alongside the more specific red flags for cauda equina syndrome.
Recurrent work flares may justify medical evaluation and a formal ergonomic review
If the same shift patterns keep recreating the same flare, especially over weeks, a formal process may be warranted. Depending on the workplace, that could mean occupational health, a primary care evaluation, physical therapy referral, a safety review, or an ergonomic assessment. If you are weighing next steps, it may help to compare when people use physical therapy for sciatica versus when imaging questions come up, such as sciatica MRI vs X-ray. OSHA’s ergonomics materials focus heavily on changing tools, work practices, and workstation setup because those structural changes often outlast heroic self-management.
FAQ
Is standing all day bad for sciatica?
It can be, especially when the job involves long blocks of static standing, hard floors, poor posture variation, and worn footwear. Mixed movement is often easier to tolerate than standing nearly still for long periods. In everyday life, many people notice the same pattern even outside work, like during sciatica while standing in line.
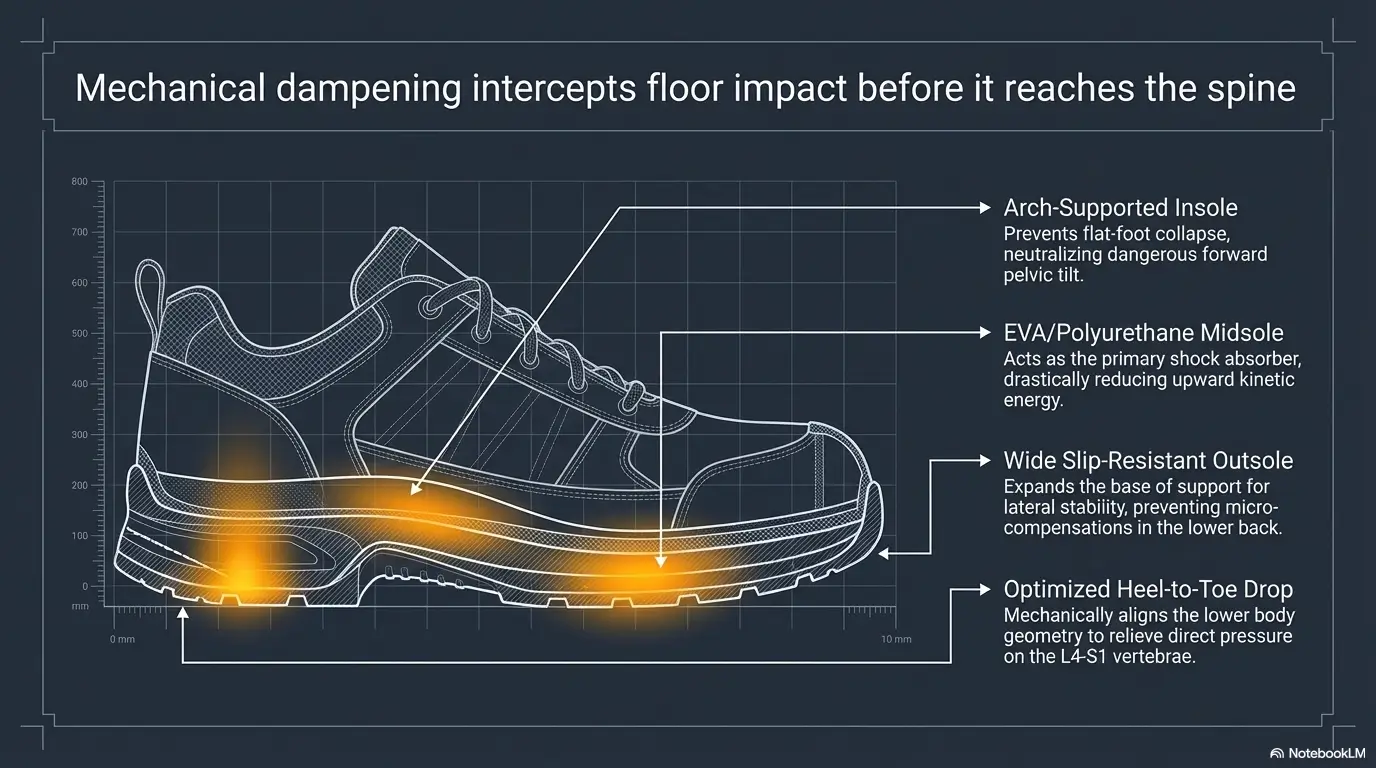
What kind of shoes are usually better for sciatica at work?
There is no universal winner, but for many workers the better choice is a stable, task-appropriate shoe with controlled cushioning, good heel hold, reliable traction, and a wear pattern that still looks honest. A shoe that feels amazing in the store but unstable late in the shift is not the right bargain.
Are anti-fatigue mats enough if my job is on concrete?
Sometimes they help a lot at fixed stations, but they are rarely the whole answer. They work best when combined with time limits on static standing, footwear that still provides control, and a station layout that reduces awkward reaching and twisting.
Is walking better than standing still during a flare?
For many workers, yes, because walking changes posture and load rather than locking the body into one position. But if walking is fast, prolonged, or combined with poor footwear and hard surfaces, it can also become aggravating. The best answer is often mixed motion rather than either extreme.
Can insoles fix the problem by themselves?
Usually not. They may help comfort, pressure distribution, or fit, but they do not usually rescue a fundamentally unstable or worn-out shoe. Think of insoles as helpers, not miracle workers.
How often should a warehouse worker rotate tasks?
There is no single perfect number. A good starting point is to rotate before symptoms usually rise, often 20 to 30 minutes before the typical flare point. Then test the plan across several shifts and adjust based on what the body and the workflow actually report.
Should I choose maximal cushioning or firmer support?
Choose the option that leaves you more controlled at the end of the shift, not just happier in the first half hour. Some workers do best with more cushioning, others with a firmer and more stable feel. The winning test is full-shift behavior.
When is leg pain serious enough to stop working and get checked?
Seek prompt medical help for new weakness, foot drop, worsening numbness, trouble walking normally, bladder or bowel changes, or saddle numbness. Those are not routine-work-flare symptoms to simply push through.
Next step
Now we can close the loop from the beginning. The shift was never a morality test. It was a systems problem wearing work boots. The most useful next move is not to buy three random shoe pairs or vow to endure better. It is to audit one full shift tomorrow with unusual honesty: note the exact hour symptoms rise, the station you were on, the shoe pair worn, the floor surface, and whether you were standing still, walking, twisting, or lifting when the change happened.
In 15 minutes, you can build the first version of a real plan:
- Cap one high-load station earlier than usual
- Insert one true lower-load task into the sequence
- Inspect shoe wear instead of trusting memory
- Choose one micro-break tied to an existing task transition
- Use operational language when you explain the problem
If you do only one thing, do the shift audit. It turns a vague bad day into a map. And maps, unlike pep talks, are good at getting people home.
Last reviewed: 2026-03.
