
The First Move is the Most Critical
A lot of orthopedic pain decisions go wrong before anyone touches the joint. Not because the injury is mysterious, but because the first move is. For people weighing orthopedic pain management at urgent care versus orthopedic clinic, the real problem is rarely anatomy first. It is choosing a care setting that matches the job.
A swollen knee after a minor twist, a shoulder that suddenly hates overhead reach, or a back flare that hijacks your workday, these problems all feel urgent in different ways. But fast access and the right access are not always the same thing. When you guess wrong, the cost is not just money; it is duplicated visits, delayed treatment, repeat imaging, and that draining sense of “medical pinball.”
This guide helps you sort the decision with more precision and less drama. You will see when urgent care makes sense for same-day triage, when an orthopedic clinic is the smarter first stop for musculoskeletal evaluation, and how to think about X-rays, function loss, follow-up, and insurance friction without overcomplicating the moment.
The method here is practical: match the visit to the purpose, not just the pain score. Because that changes everything. Start with the real question, then the right waiting room gets easier to find.
Safety note: This article is for general educational purposes and does not diagnose or treat medical conditions. Care decisions depend on symptoms, medical history, injury mechanism, and severity. For severe symptoms or possible emergencies, seek immediate medical care.
Table of Contents

Start With the Real Question: Fast Relief or a Better Diagnosis?
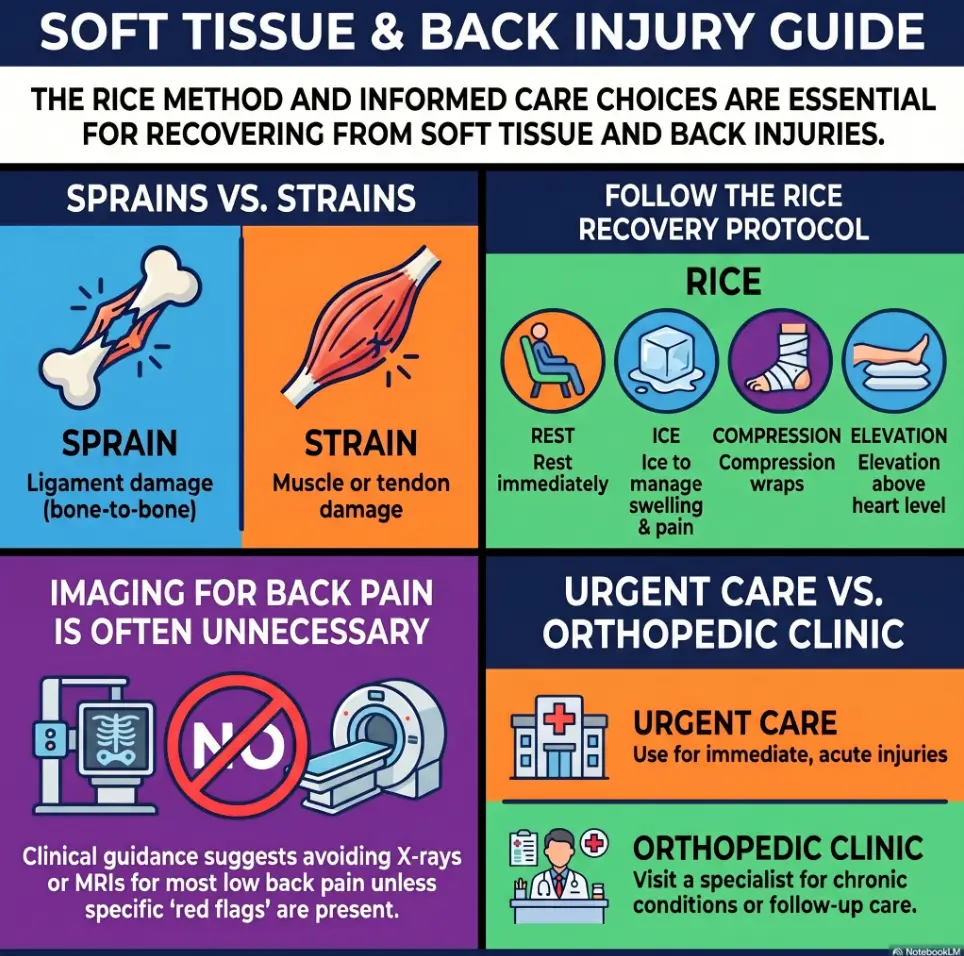
Urgent care is built for quick evaluation and short-term decisions
Urgent care is usually the better first stop when the problem is new, non-catastrophic, and time-sensitive. You twisted an ankle. Your back seized after lifting something that looked lighter than it was. Your wrist is swollen, painful, and making your coffee mug feel strangely ambitious. In moments like these, the job is often simple: rule out a bigger immediate problem, reduce pain, get basic imaging if needed, stabilize the area, and decide what comes next.
An orthopedic clinic is built for body-part-specific follow-through
An orthopedic clinic usually makes more sense when the story is already layered. The pain keeps returning. The joint catches, locks, buckles, or limits your function. You are no longer asking, “Can I get through today?” You are asking, “What is this, really, and what is the long-term plan?” That is a different question. It deserves a different room.
The fork in the road is not pain level alone, but care purpose
This is the part people often miss. Pain intensity alone does not decide the best setting. Plenty of sharp, sudden problems fit urgent care. Plenty of lower-drama, higher-friction problems fit orthopedics better. The real fork in the road is purpose. Do you need fast triage, or do you need deeper musculoskeletal evaluation? Once you name that honestly, the fog thins out.
- Urgent care is strong for same-day triage
- Orthopedics is stronger for diagnosis depth and follow-through
- Function loss matters as much as pain intensity
Apply in 60 seconds: Write one sentence that starts with “The main thing I need from this visit is…” and bring that with you.
Who This Is For, and Who It Is Not For
This is for adults deciding where to go for new or ongoing orthopedic pain
This guide is for adults navigating ordinary but stressful musculoskeletal decisions: sprains, strains, joint pain, new swelling, recurring shoulder trouble, knee pain after a minor sports injury, back pain without obvious catastrophe, and that deeply irritating category known as “I thought this would go away by now.”
This is for people trying to avoid unnecessary delay, duplicate visits, or extra cost
It is also for people who are trying to be practical. Not heroic. Not dramatic. Just practical. You want help, but you do not want to bounce between clinics like a lost suitcase. You want to avoid paying for the same story twice. You want the first visit to move the ball forward, especially if you are already weighing issues like high-deductible orthopedic pain costs or trying to make sense of a more general orthopedic pain management plan.
This is not for chest pain, stroke symptoms, major trauma, or other emergencies
This is not a guide for true emergencies. Severe trauma, chest pain, severe shortness of breath, stroke symptoms, uncontrolled bleeding, obvious deformity after major injury, or symptoms suggesting a neurologic emergency need higher-level immediate care. That is not the moment for elegant decision trees. That is the moment to move fast. The American College of Radiology also treats certain neurologic or red-flag back-pain situations differently from ordinary uncomplicated pain, which is another reminder that some symptoms change the care path completely.
- Yes: New sprain, strain, minor fall, swelling, or pain flare without obvious emergency signs
- Yes: Ongoing joint or back pain that is limiting function and needs a plan
- No: Major trauma, chest pain, stroke symptoms, or severe neurologic warning signs
Next step: If your symptoms sit in the “No” category, skip this comparison and seek higher-level urgent care immediately.
Urgent Care First: When Speed Matters More Than Specialty
Sudden sprains, minor falls, twists, and strain-type pain often start here
Urgent care earns its keep when the first priority is speed. A same-day exam, a quick assessment of swelling, tenderness, range of motion, and weight-bearing ability, maybe an X-ray, maybe a brace, maybe crutches, maybe a short medication plan, then a clear follow-up instruction. That is a perfectly respectable first move for many non-emergency injuries.
Same-day X-rays, bracing, and pain guidance can be enough for some cases
For many soft-tissue injuries, the first useful step is not a grand diagnosis worthy of a documentary narrator. It is simple stabilization. The AAOS notes that sprains and similar soft-tissue injuries often begin with supportive measures, and moderate cases may need bracing or temporary immobilization. That maps neatly onto what urgent care often does well. If that conversation turns practical fast, readers sometimes also care about which braces and supports may be HSA-eligible.
Urgent care shines when the first job is triage, not a full orthopedic roadmap
I have watched people use urgent care very well when they treated it as a launch point, not a final chapter. They went in because they needed same-day help, not because they expected a full specialty roadmap in 25 minutes under fluorescent lighting that makes everyone look vaguely overcooked. That expectation gap matters. When expectations are realistic, urgent care can be efficient, reassuring, and exactly enough for stage one.
What urgent care often does well:
- Assesses new pain or injury quickly
- Orders plain X-rays in many locations
- Provides basic bracing, splinting, or pain guidance
- Tells you whether you need a higher-level follow-up plan
Show me the nerdy details
Plain X-rays are good at showing bone-related issues such as fractures or alignment problems, but they do not fully explain many soft-tissue problems involving tendons, ligaments, or cartilage. That is one reason an urgent care visit can be useful without being the last word.
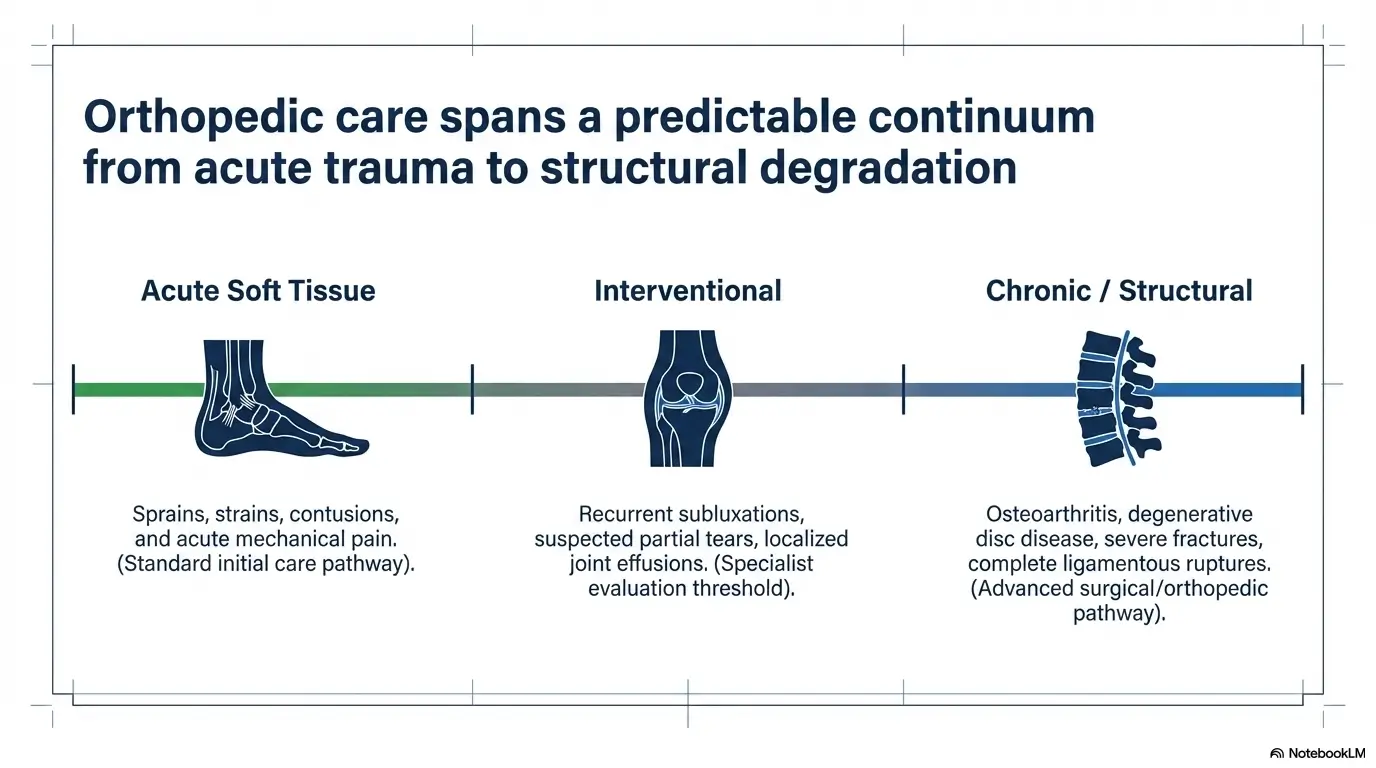
Orthopedic Clinic First: When the Pain Story Is Already Getting Complicated
Ongoing joint pain, repeat flare-ups, and function loss often need deeper follow-up
Orthopedic clinics are designed for the kind of pain story that no longer fits on a sticky note. Maybe your knee pain has lasted 6 weeks. Maybe your shoulder hurts every time you reach behind you. Maybe your back pain is not theatrical, but it keeps cutting off normal life in small, steady bites. You can still walk. You can still work. But everything costs more effort than it should. That is often the territory where orthopedic follow-through becomes more valuable than simple access.
Orthopedic clinics are better set up for exam nuance, treatment sequencing, and referrals
Orthopedics is about the musculoskeletal system, including bones, joints, ligaments, tendons, and muscles. That sounds obvious, but it matters. Specialty clinics are built around pattern recognition. They tend to think in sequences: history, focused exam, plain films when useful, rehab options, injections in some cases, additional imaging only when it answers a meaningful question, and surgical referral if truly needed. MedlinePlus describes orthopedic services as targeting the musculoskeletal system, which is exactly why this setting becomes more useful when the question is structural or persistent.
Chronic pain with a structural question usually fits better here
This is especially true when the pain is asking a structural question. Is something unstable? Torn? Arthritic? Recurrently inflamed? Mechanically irritated? Orthopedic clinics are better positioned to sort those questions without defaulting to “rest and see” forever. There is a big difference between giving your body time and accidentally entering a 3-month limbo sponsored by indecision. Sometimes that next layer of planning overlaps with choices like pain clinic versus orthopedist or whether you are heading toward an MRI referral for orthopedic pain.
| When this is your real need | Better first stop | Trade-off |
|---|---|---|
| Same-day check after a new, non-emergency injury | Urgent care | Fast access, less specialty depth |
| Recurring pain or reduced function over time | Orthopedic clinic | May take longer to book, but usually better sequencing |
| Need to know what the long-term plan should be | Orthopedic clinic | Less instant, more strategic |
Next step: Circle the row that sounds most like your situation before you choose where to go.
Here’s the Catch: The First Visit Is Not Always the Right Finish Line
A fast visit can stabilize the problem without fully explaining it
This is where many people feel let down, even when the visit was reasonable. The ankle was wrapped. The X-ray was negative. You were told to rest, ice, elevate, maybe follow up. Medically, that may have been appropriate. Emotionally, it can feel thin. People walk out thinking, “But do we actually know what this is?” Sometimes the honest answer is no, not yet. Early visits often answer the urgent question first: Is there anything dangerous, unstable, or clearly broken?
A specialty visit can be more useful when the pain keeps returning
If the symptoms linger, return, or interfere with daily function after that first phase, the next right step is often orthopedic follow-up. This is not failure. It is sequencing. The first visit did one job. The next visit does another. The mistake is expecting every setting to do every job equally well.
The wrong first stop is often the one that delays the next right step
In practice, the wrong first stop is not always the medically “wrong” place. It is often the place that lets the process stall. People sometimes leave urgent care without a real follow-up plan. Or they wait weeks hoping the issue will settle because the first visit did not sound alarmed. Or they book orthopedics first for a fresh, simple sprain that mainly needed an exam, an X-ray, and a brace that day. The trouble is rarely one dramatic mistake. It is usually a string of small delays wearing a polite face.
Short Story: A friend once tried to “be efficient” after a weekend pickleball mishap, which is a sentence that already contains trouble. She skipped same-day evaluation because the ankle was not grotesque, just swollen and stubborn. Three days later she went to urgent care, got the X-ray, got the boot, and felt relieved.
Then two weeks passed and she still could not push off normally. That is when orthopedics became useful, not because urgent care had failed, but because the question had changed. The first question was, “Did I break this?” The second was, “Why is function still off, and what do I do next?” Once she saw the visits as stages instead of rivals, the whole experience made more sense.
- Urgent care can rule out immediate issues
- Orthopedics can build a longer-term plan
- Needing both is common, not a sign that care “failed”
Apply in 60 seconds: Ask at checkout, “What symptom or timeline should trigger orthopedic follow-up?”
Cost Traps First: Where People Accidentally Spend Twice
Duplicate imaging and repeat intake can quietly raise the bill
Money leaks out of orthopedic care pathways in very ordinary ways. You tell the story once. Then again. Then again. You get imaging that answers a narrow question, then later more imaging that answers the real question. None of this feels dramatic in the moment. It just feels annoying. But stacked together, it becomes expensive friction.
Insurance networks, copays, and referrals change the math
Insurance logic can shape the “best” first stop as much as medical logic does. Some people have easier specialist access. Some plans nudge patients through primary care or require referrals. Some urgent care visits are modestly priced; others feel less modest once imaging or out-of-network surprises arrive. The practical point is simple: the medically reasonable first stop is not always the financially efficient one. That becomes especially clear in scenarios involving imaging cost estimates on an HDHP, physical therapy copay versus coinsurance, or broader self-pay cash price ranges.
Paying for convenience is one thing, paying twice for the same answer is another
Convenience can be worth money. What you want to avoid is paying twice for the same low-yield answer. If urgent care tells you clearly, “This needs orthopedic follow-up,” that can still be money well spent because it bought speed, stabilization, and direction. What hurts is vague duplication.
| Cost question | Why it matters | Ask before the visit |
|---|---|---|
| Copay or visit charge | Changes the true price of convenience | “Is this visit in-network?” |
| Imaging coverage | Plain films and advanced imaging may bill differently | “Is imaging billed separately?” |
| Referral rules | Affects access to orthopedics | “Do I need prior authorization or referral?” |
Next step: Spend 3 minutes checking network and referral rules before you choose based on convenience alone.
Don’t Do This: Mistaking Access for the Best Fit
The nearest clinic is not always the most efficient care path
There is a strange modern temptation to choose healthcare the way we choose a sandwich shop. Closest pin wins. Fastest appointment wins. Least parking drama wins. That instinct is understandable. Time is real. But the nearest clinic is not always the cheapest, most useful, or most resolving option.
Short wait times can tempt people into the wrong kind of visit
Short wait times are soothing because they promise action. Action feels better than uncertainty. But action without fit can waste momentum. A quick urgent care visit for months-long shoulder dysfunction may buy speed at the cost of depth. A delayed specialty visit for a clearly non-emergency, persistent problem may actually save you an extra round of guesswork.
Choosing by urgency alone can blur diagnosis and long-term management
Many people confuse urgency with importance. Some pain is important because it is persistent, function-limiting, and affecting sleep, work, exercise, or daily care. It may not be dramatic enough to win the urgency pageant, but it still deserves the right setting. Bodies are rude this way. They do not always perform their seriousness theatrically.
Don’t Do This Either: Waiting Too Long Because the Pain Feels “Manageable”
Lingering pain can train people to normalize a worsening problem
There is another trap on the opposite side: delay disguised as toughness. People normalize symptoms because they can still technically function. They can still walk. They can still type. They can still pick up groceries with the good arm doing most of the emotional labor. So they wait. Sometimes that is fine. Sometimes it quietly extends recovery or lets weakness, compensation, and stiffness settle in.
Function loss matters even when pain is not dramatic
This is why function is such a useful lens. Can you bear weight? Reach overhead? Sleep on that side? Climb stairs normally? Grip, twist, push, or stand from a chair without adjusting your entire personality around the pain? Function loss often tells a truer story than pain score theatrics.
Small symptoms sometimes become expensive delays
The delayed cost is not always structural damage. Sometimes the cost is weeks of poor sleep, reduced activity, lost exercise consistency, growing fear of movement, and extra visits because the original story got muddier over time. A 20-minute earlier decision can save a remarkable amount of life friction.
Ask yourself three yes/no questions.
- Has this lasted more than 2 weeks?
- Is normal function getting worse or not improving?
- Are you changing the way you walk, lift, sleep, or work because of it?
Output: If you answered “yes” to 2 or 3, the odds are good that you need more than simple watchful waiting.
Next step: Book an evaluation based on function loss, not stubborn optimism.
Let’s Be Honest: Most People Are Really Asking About Time, Money, and Reassurance
People want to know whether they need imaging, rest, rehab, or something more
Most readers are not trying to win a seminar on care pathways. They are trying to answer a smaller, more human question: What is the most sensible next move? Do I need imaging? Do I need rest? Is this rehab territory? Is this a problem to watch, a problem to brace, or a problem to escalate?
They also want to avoid being bounced from one clinic to another
Underneath the comparison is often a fear of medical pinball. Nobody wants to hear, “This isn’t really our lane,” after rearranging a workday and paying for a visit. That is why naming the purpose of the visit in advance matters so much. It keeps expectations tethered to reality.
Good care choice starts by naming the fear underneath the visit
Sometimes the fear is cost. Sometimes it is lost time. Sometimes it is the possibility of missing something serious. Sometimes it is just plain exhaustion. Once you name that, the comparison becomes easier. You stop chasing the illusion of the perfect clinic and start choosing the most useful first step.
- Start date of symptoms
- What movement or activity triggers the problem
- Whether you can bear weight or use the limb normally
- Prior imaging, braces, or treatment already tried
- Your actual goal for the visit: relief, diagnosis, or long-term plan
Next step: Put these notes in your phone so you do not walk into the appointment empty-handed.
What Each Setting Usually Does Best, and What It Usually Does Not
Urgent care is strong at short-term stabilization and rule-out decisions
Urgent care is often best at answering immediate, narrow questions. Is this likely broken? Is there a reason I should not wait? Do I need support, activity restriction, or quick symptom control? It is a strong setting for first-pass evaluation when time matters more than specialty nuance.
Orthopedic clinics are stronger at condition-specific evaluation and next-stage planning
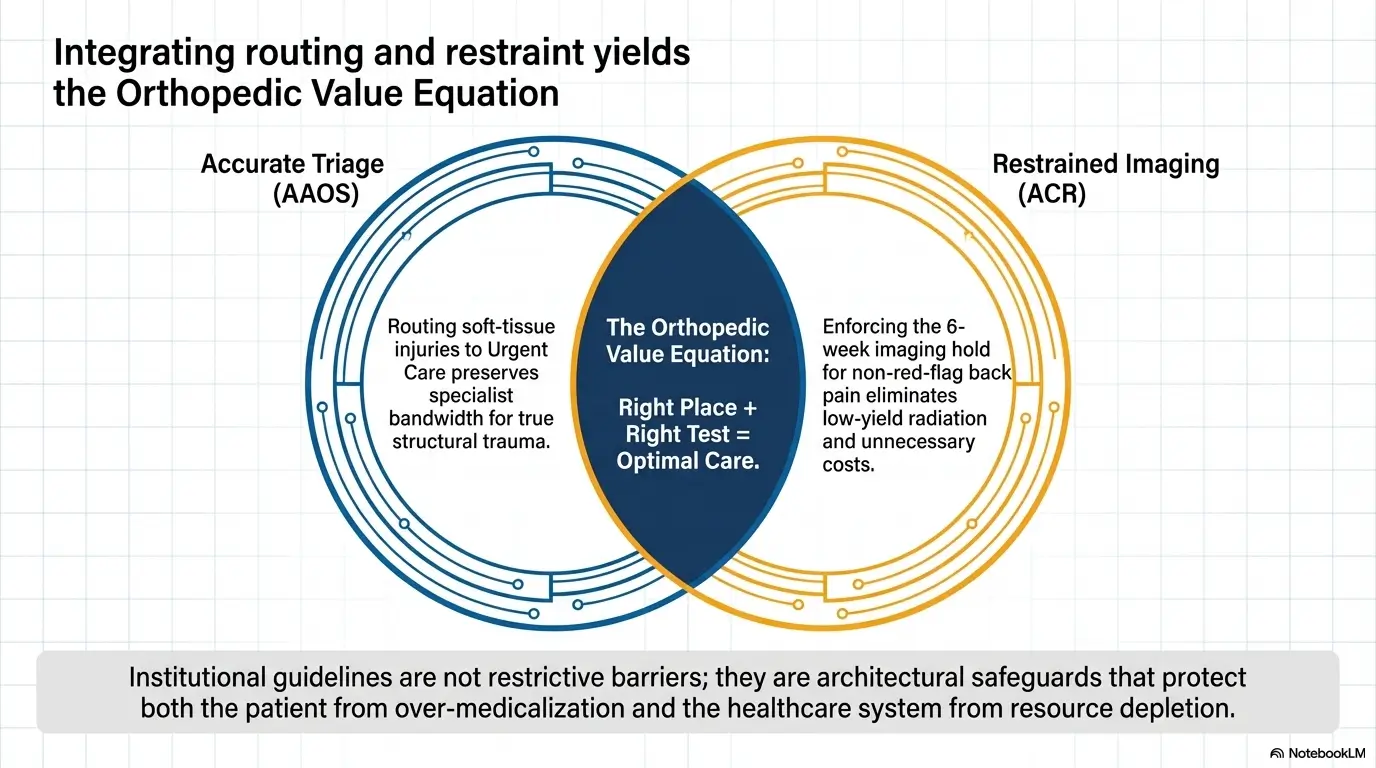
Orthopedic clinics are usually better when the question is more layered. Why does the knee keep swelling? Why is the shoulder weak despite rest? Does this back pain need imaging yet, or does it need targeted rehab first? The American College of Radiology generally advises against routine early imaging for acute uncomplicated low back pain without red flags, which is a useful example of why specialty planning matters. The better question is often not “Can I get an MRI?” but “Would imaging change what we do next?” That is also where articles on failed conservative care for MRI approval and what to do after an MRI denial appeal can become surprisingly relevant.
Neither setting is perfect when expectations are mismatched from the start
Neither setting is magical. Urgent care is not a full orthopedic pathway. Orthopedics is not always the fastest answer for fresh, straightforward minor injuries. When people feel disappointed, it is often because the setting and the expectation were slightly out of phase from the beginning.
Show me the nerdy details
Plain X-rays are commonly the first imaging step in many musculoskeletal evaluations because they help identify fractures, alignment issues, and some degenerative changes. They do not replace the physical exam, and they do not answer every soft-tissue question.
Here’s What No One Tells You: Better Notes Can Save a Whole Appointment
Pain location, timing, triggers, swelling, weakness, and injury mechanism matter
A good visit starts before you enter the building. If you can describe where the pain is, when it started, what triggered it, what movements worsen it, whether there is swelling, weakness, numbness, locking, catching, instability, or weight-bearing trouble, you make the visit better instantly. Not prettier. Better.
A short symptom timeline can make the visit more useful in either setting
I am always surprised by how often one clean timeline beats one emotional monologue. “Started 10 days ago after tennis, worse with stairs, swollen that night, improved a little, now catching when I pivot.” That is gold. It is calm, specific, and clinically useful. It gives the visit structure.
Clean information often gets you closer to the right next step than dramatic language
Dramatic language is human. When something hurts, everything feels louder. But vague intensity can obscure useful detail. Better notes help urgent care decide whether you need escalation. Better notes help orthopedics decide what question the exam and any imaging should answer. Either way, your notes are not homework. They are leverage. The same principle shows up in documentation-heavy situations too, like workers’ comp settlement documentation or appealing a denied second opinion for orthopedic pain.
- Track start date and mechanism
- Note function changes, not just pain score
- Bring prior imaging or visit summaries if you have them
Apply in 60 seconds: Write a 4-line symptom timeline before you book or leave for the visit.
When to Seek Help Sooner, Not Later
Inability to bear weight or use the limb normally
If you cannot bear weight, cannot use the limb normally, or your function drops sharply, that is usually a signal to seek same-day evaluation rather than simply “monitor it.” The question becomes less about convenience and more about safe next steps.
Visible deformity, severe swelling, numbness, or worsening weakness
Visible deformity, severe swelling, progressive numbness, or worsening weakness deserve faster attention. These features can shift the pathway away from routine wait-and-see decisions.
Fever, redness, rapidly increasing pain, or symptoms after a significant injury
Fever with joint pain, spreading redness, rapidly increasing pain, or symptoms after a more significant injury also raise the stakes. These are the sorts of features that make “I’ll just see how it feels tomorrow” a less charming strategy.
Pain with bowel or bladder changes, saddle numbness, or other neurologic red flags
Back pain paired with bowel or bladder changes, saddle numbness, or serious neurologic symptoms needs urgent escalation. The American College of Radiology separates uncomplicated pain from red-flag scenarios for good reason. Those symptoms can change the imaging and care pathway materially. If your worry is whether the situation has crossed from inconvenient to dangerous, the distinction is closer to low back pain emergency warning signs than to routine watchful waiting.
Common Mistakes People Make When Choosing Between Urgent Care and an Orthopedic Clinic
Assuming every orthopedic problem needs a specialist on day one
Not every sprain, strain, or mild new injury needs a same-day specialist. Sometimes fast triage and supportive care are the correct first moves.
Assuming urgent care can manage every musculoskeletal issue from start to finish
Urgent care can be excellent for the beginning of the story. That does not make it the best place for every middle and ending.
Chasing imaging before clarifying what question the imaging needs to answer
This is one of the most common and costly mistakes. People ask for imaging as though it is the plan. It is not. It is a tool. The plan is the plan. The ACR’s approach to uncomplicated low back pain is a good reminder that early imaging is not automatically the smartest opening move when red flags are absent.
Ignoring how insurance rules shape the care path
Medical logic matters. Insurance logic also matters. Pretending otherwise only makes the eventual bill more dramatic.
Focusing on pain intensity while overlooking function loss
The smartest readers track what the pain is doing to life, not just how loudly it complains. Function loss is often the clearest signal that it is time to stop improvising.
Show me the nerdy details
In many orthopedic decisions, the combination of history, physical exam, mechanism of injury, and whether symptoms are improving over time matters more than any single pain number. That is why two patients with the same “7 out of 10” score may belong in different care settings.
FAQ
Is urgent care or an orthopedic clinic better for a sprain?
For a new, non-emergency sprain, urgent care is often a sensible first stop because it can assess the injury quickly, check whether imaging is needed, and provide bracing or activity guidance. If recovery stalls or function stays limited, orthopedic follow-up may be the better next step.
Can urgent care treat knee, shoulder, or back pain?
Yes, urgent care can often evaluate many types of musculoskeletal pain, especially when the problem is new and needs same-day assessment. Its role is usually triage, basic evaluation, and short-term management rather than deep specialty planning.
Should I go straight to an orthopedic clinic after a minor sports injury?
Not always. If the injury is minor, new, and non-emergency, urgent care may be faster and sufficient as a first step. If the injury is recurring, mechanically limiting, or not improving, orthopedics becomes more useful.
Will urgent care do X-rays for orthopedic pain?
Many urgent care centers can perform plain X-rays on site, though capabilities vary by location. Plain films are often used to look for fractures or other bone-related issues, but they do not answer every soft-tissue question.
Do I need a referral to see an orthopedic specialist in the US?
Sometimes yes, sometimes no. It depends on your insurance plan and network rules. Some plans allow direct specialist access, while others require primary care referral or prior authorization.
Is an orthopedic clinic more expensive than urgent care?
It can be, but the cheaper first visit is not always the cheaper overall pathway. The real cost question is whether the first setting helps you avoid duplicate visits, repeat imaging, and unnecessary delay.
What if urgent care says I should follow up with orthopedics?
That is common and often appropriate. It usually means the urgent care visit handled the immediate job, while orthopedics is better suited for the next-stage question.
When is orthopedic pain serious enough to seek same-day care?
Seek faster care when there is inability to bear weight, visible deformity, severe swelling, worsening weakness, numbness, fever with joint symptoms, or serious neurologic warning signs such as bowel or bladder changes with back pain.
Next Step: Choose the Visit Based on the Job You Need Done
Go to urgent care if you need same-day triage for a new, non-emergency injury or flare
If this started suddenly, feels fresh, and you need help today, urgent care is often the practical first move. Think new sprain, strain, twist, minor fall, or sharp flare that needs exam, plain films, bracing, and immediate direction.
Book an orthopedic clinic if the pain is ongoing, recurring, or interfering with normal function
If this problem has already overstayed its welcome, keeps returning, or is steadily shrinking your normal function, orthopedic follow-up is often the more efficient path. Not because it feels fancier, but because it matches the real job: deeper evaluation and better sequencing.
Before you go, write down when it started, what worsens it, what limits you, and what answer you need most
That is the curiosity loop from the beginning, finally closed. The best first step is not the one that sounds most medical. It is the one that fits the actual question in front of you. In the next 15 minutes, write a four-line symptom timeline, check your insurance referral rules, and choose the visit based on whether you need fast triage or deeper orthopedic evaluation. That one small act can save time, money, and an astonishing amount of avoidable frustration.
Last reviewed: 2026-04.
