
The Sciatica Imaging Strategy: Beyond the Reassurance Receipt
Most people with sciatica don’t need “more imaging.” They need the right picture at the exact moment it changes the plan, not a receipt for reassurance.
If you’re stuck choosing MRI vs. X-ray, here’s the quiet trap: an X-ray can look “fine” while your leg feels like a live wire, and an MRI can look “terrible” while the finding doesn’t match your nerve pattern. (If that disconnect sounds familiar, read why MRI findings and pain patterns can mismatch before you spiral.) Meanwhile, you’re losing sleep, dreading chairs, and collecting contradictory advice like unwanted souvenirs.
This guide helps you choose imaging based on decision points: red flags, neurologic changes, week-by-week trends, and whether you’re nearing injections or surgery. You’ll also get a short, calm script for your visit.
Sciatica is not a diagnosis. It’s nerve-pattern leg pain (often with numbness/tingling) that tracks from the low back or buttock down the leg, usually from irritation or compression of a nerve root.
Action Plan
- Read this part first.
- Then use the ladder.
- Walk into the appointment with a plan.
Key Objectives
- Clarify what an X-ray can rule out (bones, alignment, fracture).
- Know when MRI earns its cost (herniation, stenosis, surgery decisions).
- Avoid the two imaging mistakes that waste money or delay care.
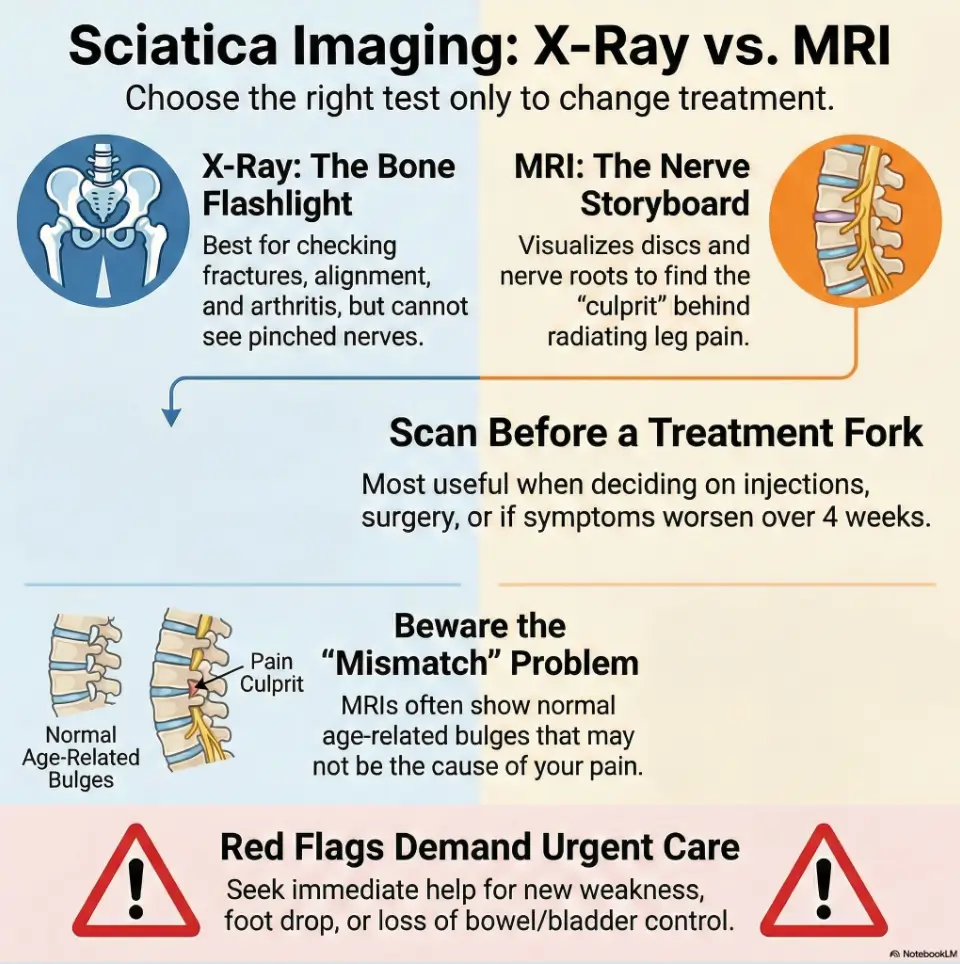
If you have sciatica (leg pain from suspected nerve irritation), an X-ray usually can’t “see” the nerve or a herniated disc. It’s mainly used to check bones, alignment, fractures, arthritis, or “something else”. An MRI is the test most likely to show a disc herniation or spinal stenosis that could match leg symptoms, but it’s most useful when results will change treatment (persistent symptoms, weakness, or before injections/surgery).
This guide is educational and not a diagnosis. Imaging choices depend on your exam, medical history, and red-flag symptoms. If you have severe or worsening weakness, new bowel/bladder problems, saddle numbness, fever, cancer history, major trauma, or unexplained weight loss, seek urgent medical care. (If you want a clean checklist you can screenshot, see cauda equina syndrome red flags and when low back pain becomes an emergency.)
Table of Contents
Leg pain first: what “sciatica” really means (and what it doesn’t)
The 30-second definition: nerve pattern pain vs “back pain that travels”
Sciatica is not a single diagnosis. It’s a pattern: pain (sometimes with numbness or tingling) that follows a nerve pathway from the low back or buttock down the leg. Often it’s one-sided. It can feel sharp, electric, burning, or like a deep ache that refuses to negotiate. The key idea is this: when people say “sciatica,” they usually mean suspected nerve irritation, not “my back hurts and sometimes my leg hurts too.” (If you want a clearer definition that separates the signal from the noise, bookmark what sciatica nerve pain actually is.)
Where symptoms map matters more than where your back aches
If your worst pain lives in the leg, that changes the imaging conversation. Clinicians listen for distribution (outer calf? top of foot? back of thigh?), triggers (sitting, coughing, bending), and neurologic clues (weakness, reflex change, numbness). Why? Because imaging isn’t the opening act. It’s the spotlight you point after you’ve decided what you’re hunting.
Pattern interrupt: Let’s be honest… “sciatica” is a label, not an answer
Here’s the unglamorous truth: “sciatica” is what we call it when your body says, “I have a nerve problem somewhere,” and your brain replies, “Cool, can we not?” It’s a useful label for starting care, but it’s not the end of the story. The end of the story is: what is irritating the nerve, and what do we do next. (If you’re stuck between “disc problem” vs “piriformis” vs “something else,” these two clarifiers help: sciatica vs herniated disc and sciatica vs piriformis syndrome.)
- Leg-dominant pain points toward nerve involvement more than back-dominant pain.
- Your symptom map often predicts usefulness of imaging better than your pain intensity.
- The right test depends on what you’re trying to rule out or confirm.
Apply in 60 seconds: Write the single most painful line on your leg (buttock → thigh → calf → foot) like drawing a route on a map.
- Yes if you have new or worsening weakness, foot drop, or you can’t heel/toe walk.
- Yes if you have new bowel/bladder control problems or saddle numbness.
- Yes if fever, significant trauma, cancer history, or infection risk is in the picture.
- Maybe later if pain is improving week to week and function is returning.
Neutral next step: Bring this list to your visit and ask which item (if any) applies to you.
What each test sees: bones on X-ray, nerves on MRI
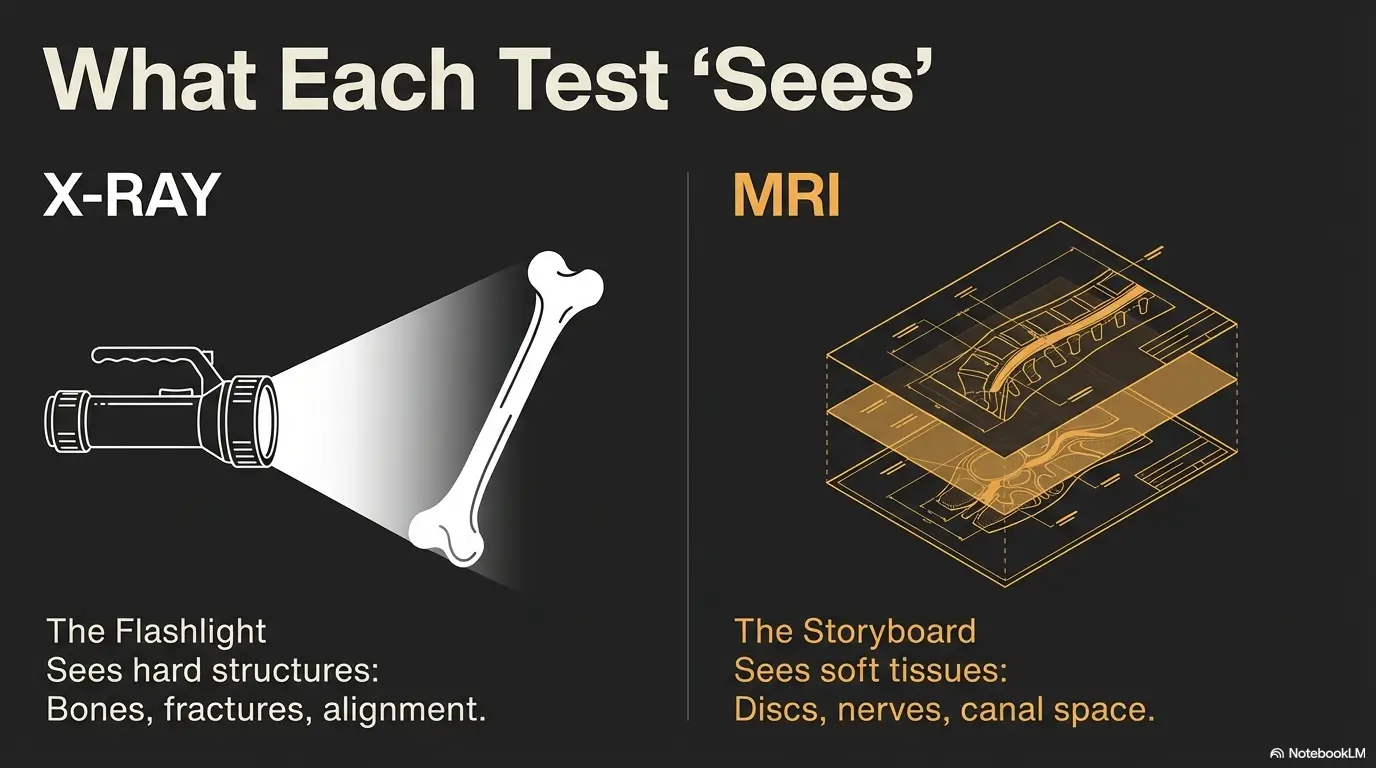
X-ray is a flashlight on skeleton structure (not soft tissue)
An X-ray is excellent at showing bony architecture. Think: fractures, alignment, visible arthritis changes, and certain structural clues. It can also hint at narrowing in spaces where nerves pass, but it does not directly show the nerve, the disc, or soft tissue detail the way an MRI does. In plain terms: an X-ray answers bone questions.
MRI is the soft-tissue “storyboard” (disc, nerve roots, canal space)
An MRI is built for soft tissue: discs, nerve roots, ligaments, and the canal where nerves travel. If your clinician is looking for a disc herniation, spinal stenosis, or inflammation affecting nerve roots, MRI is typically the imaging workhorse. It can also reveal “surprises” that need context, which we’ll talk about soon, because MRI is powerful and occasionally… too honest.
Why the right question is “What are we trying to rule out?”
Here is the mindset shift that saves time, money, and emotional energy: don’t ask “Which test is better?” Ask: What question are we trying to answer today? If the question is “Is there a fracture or major bony issue?” X-ray may be a reasonable first pass. If the question is “Is a nerve root compressed in a way that matches my symptoms?” MRI is usually the better tool.
Show me the nerdy details
MRI uses magnetic fields and radiofrequency signals to generate high-contrast images of soft tissues. X-rays use ionizing radiation and are best for high-density structures like bone. That difference is why an X-ray can “miss” disc and nerve-root problems while still being useful for bone-alignment and fracture questions.
- X-ray rarely explains classic nerve-pattern leg pain by itself.
- MRI is most valuable when it will change the next step (injection, surgery, escalation).
- The best imaging order depends on what needs ruling out first.
Apply in 60 seconds: Decide your main question: “rule out fracture/major bone issue” or “confirm nerve compression that matches symptoms.”
When X-ray helps: the “rule-out” list most people miss
Trauma, fracture risk, severe arthritis, spinal alignment issues
X-ray shines when there is a reason to suspect bone-related problems: significant trauma, osteoporosis-related fracture risk, notable deformity, or severe degenerative changes that could redirect the plan. Even then, an X-ray may not be the final answer. But it can be a fast gatekeeper: “Are there obvious bone-level reasons we need to change course immediately?”
Redirection moments: hip problems, SI joint, or something not-spine
Sometimes the most helpful outcome of an X-ray isn’t “diagnosis confirmed.” It’s diagnosis rerouted. Hip pathology, SI joint issues, and even non-spine causes can mimic “sciatica-ish” pain. A basic imaging step can occasionally reduce the chance that everyone runs down the wrong hallway for weeks, carrying a perfectly good flashlight but pointing it at the wrong wall.
Open loop: The surprising reason some clinicians start with X-ray anyway
In the US, a practical reason is workflow: an X-ray is fast, widely available, and often used as an initial screen before advanced imaging. Another reason is documentation: if you eventually need an MRI authorization, some pathways want proof that a basic evaluation has happened. Is it always ideal? No. Is it common? Very.
- Recent trauma or fracture risk
- Concern for major alignment/bony change
- Need to rule out “something else” quickly
Trade-off: Faster/cheaper, but often won’t explain nerve pain.
- Leg-dominant nerve-pattern symptoms
- Objective weakness/reflex changes
- Planning injection, surgery, specialist escalation
Trade-off: More detail, but can reveal incidental findings.
Neutral next step: Ask your clinician which “box” you’re in and why.
- American College of Physicians (ACP): High-value diagnostic imaging advice for low back pain
- NICE Quality Standard (QS155): Referrals for imaging for low back pain with or without sciatica
- American College of Radiology (ACR) Appropriateness Criteria: Low back pain imaging recommendations
When MRI earns its price: the situations where it changes decisions
Persistent leg-dominant pain after conservative care
Most acute sciatica improves with time and conservative management. But when leg pain remains stubborn, especially when it keeps you from working, walking, or sleeping for weeks, MRI becomes a more rational tool. The point isn’t “proving you’re not imagining it.” The point is: are we at a fork in the road? If yes, MRI can clarify the terrain. (If you’re currently in that limbo window, this timeline helps: how long herniated disc sciatica usually takes to improve.)
A tiny but real emotional note: persistent pain makes people feel like they have to “earn” care by suffering long enough. You don’t. You earn care by having a story and an exam that suggests imaging will change the plan.
Objective weakness, reflex loss, or progressive neurologic signs
Weakness is a different category than pain. Pain is loud. Weakness is a vote of no-confidence from your nervous system. If you are tripping, noticing foot slap, struggling to climb stairs, or cannot do heel/toe walking normally, that’s a “this might change urgency” conversation. MRI is often used in that context because it can identify compressive causes that may need faster escalation.
Planning an epidural injection, surgery, or specialist pathway
When an intervention is on the table, MRI often becomes the necessary blueprint. Injections and surgery aren’t chosen because an MRI looks scary. They’re chosen when symptoms, exam, and imaging line up and the next step requires anatomical precision. (If you’re near that point, it helps to understand treatment options in order: herniated disc sciatica treatment pathways and the injection comparison TFESI vs interlaminar epidural.)
Pattern interrupt: Here’s what no one tells you… MRI is most valuable right before a fork in the road
If your plan is still “watchful waiting and gentle rehab,” a very early MRI can add anxiety without adding actionable clarity. If your plan is “consider injection,” “refer to spine specialist,” or “rule out a serious cause,” MRI can become the right tool at the right moment. That is the whole trick: MRI should answer a decision, not just curiosity.
- It’s most useful when symptoms are persistent, disabling, or neurologically changing.
- Weakness and progressive deficits shift urgency more than pain intensity does.
- It’s especially useful before injections or surgery, when anatomy matters.
Apply in 60 seconds: Ask: “If MRI shows X, what would we do next within 30 days?”
You wake up on a Tuesday and your leg pain feels like it has opinions. Sitting is a betrayal. Standing is a negotiation. You open your calendar and realize you’ve been “waiting it out” for three weeks, but you’re not really waiting. You’re hovering. In your mind, there are two doors at the end of a hallway: “It gets better” and “It gets worse.” The trouble is you can’t see which door you’re walking toward.
That’s where imaging becomes emotionally tempting: it feels like a flashlight. But the best flashlight is the one you aim at the right thing. If your strength is stable and your function is slowly returning, the hallway might just be part of the healing tempo. If you’re losing strength or function, you’re not being impatient. You’re reading the signs on the wall. And that is a reasonable time to ask for a clearer map.
The mismatch problem: why MRI can “find” things that don’t explain your pain
Common incidental findings (bulges, degeneration) and why they’re common
MRI is so good at seeing anatomy that it often sees normal age-related changes too. Disc bulges, degenerative changes, and “wear-and-tear” language can show up even in people without symptoms. This is not because MRI is wrong. It’s because the spine is a living structure that changes over time, like the creases on a well-loved book. Not every crease explains the plot twist you’re currently living. (If you want a deeper, calmer explanation, revisit the MRI-pain mismatch guide here.)
“Clinical correlation” in plain English: matching image to symptoms + exam
When a report says “clinical correlation recommended,” it means: “This finding might matter, but only if it matches the patient’s symptom pattern and exam.” A disc herniation on the right side doesn’t explain left-sided symptoms. A mild bulge doesn’t necessarily explain severe weakness. The MRI is a clue, not a verdict.
Open loop: If MRI isn’t a truth machine, what is the anchor?
The anchor is the combination of (1) your symptom map, (2) your neurologic exam (strength, reflexes, sensation), and (3) whether your function is improving or declining. Imaging is the supporting actor. The exam and timeline are the main plot.
Timing matters: when imaging is too early (and when waiting is risky)
Early-phase sciatica often improves without imaging
Many cases of new sciatica improve over weeks with conservative care. That’s not a motivational poster, it’s a practical observation baked into many clinical pathways: early imaging often does not change management if you are improving and have no red flags. Early scans can also accidentally inflate fear, because the report reads like a list of everything your spine has ever experienced since college.
When waiting is reasonable vs when delay can cost function
Waiting can be reasonable when you are improving: better sleep, easier walking, less numbness, fewer “electric” zaps. Waiting is not a virtue when you are losing function: worsening weakness, new bowel/bladder symptoms, saddle numbness, escalating night pain with systemic illness signals, or a story that suggests infection, fracture, or malignancy risk. The core rule is simple: improvement buys time; deterioration demands attention.
The “week-by-week” decision trigger you can actually use
Use a week-by-week trigger instead of day-by-day panic. Day-by-day pain is moody and unreliable. Week-by-week function is a better narrator. If, over 2–4 weeks, you are trending better, imaging is often less urgent. If, over 2–4 weeks, you are flat or worse, or you’re unable to work or walk normally, you are closer to that fork-in-the-road moment where MRI becomes more useful.
Pick your answers:
- Weeks since onset: 0–2 / 3–6 / 7–12 / 12+
- Weakness: none / mild / worsening
- Trend: improving weekly / stuck / getting worse
Output: If weakness is worsening or trend is getting worse, imaging is more likely to change the plan now. If you’re improving weekly and have no red flags, imaging is less likely to change the plan this month.
Neutral next step: Bring these three answers to your clinician and ask how they affect imaging choice.
- Weekly functional trend is more useful than daily pain spikes.
- Improving symptoms often justify conservative care without imaging.
- Worsening weakness or red flags justify faster evaluation.
Apply in 60 seconds: Write one sentence: “Compared to last week, I can/can’t do ___.”
Who this is for / not for: a quick self-sort before you book anything
For: leg-dominant pain, recurrent episodes, planning injections, persistent symptoms
This guide is for you if your leg symptoms feel like the headline, not the footnote. Especially if you’ve had recurrent episodes, if sitting and coughing reliably light up the same nerve pathway, or if you’re nearing a decision about injections, specialist care, or work-limiting function. If you’ve ever found yourself thinking, “I don’t need a perfect diagnosis, I need a plan,” you are exactly the reader this was written for.
Not for: mild new symptoms improving daily, no red flags, no functional loss
If your symptoms are mild and you’re improving, you may not need imaging right now. It can be more useful to invest in movement, symptom tracking, and a focused exam than to chase pictures that don’t change management. Not because you don’t “deserve” an MRI, but because you deserve the kind of care that actually helps. (A practical next step many people skip: a structured plan for physical therapy for sciatica rather than random exercises.)
For urgent evaluation: severe/progressive weakness, bowel/bladder changes, saddle numbness, fever/trauma/cancer signals
If you recognize these symptoms, don’t treat this article as a substitute for urgent evaluation. Imaging urgency is not about proving bravery. It’s about preventing avoidable harm.
Common mistakes: the imaging traps that waste money (or delay care)
Mistake #1: Expecting an X-ray to “show the pinched nerve”
This is the most common mismatch between expectations and physics. An X-ray can’t directly show a compressed nerve root or a disc herniation. When people get an X-ray, hear “mild degenerative changes,” and feel dismissed, it’s often because they were promised (implicitly or explicitly) a different kind of answer than the test can provide.
Mistake #2: Treating MRI findings like a verdict instead of a clue
Reading an MRI report without context can feel like reading your fortune from a spreadsheet. “Bulge.” “Protrusion.” “Stenosis.” The words are real, but the meaning depends on whether those findings match your symptoms and exam. A scary report can coexist with a stable, improving clinical picture. A mild report can coexist with severe pain. The picture is part of the story, not the narrator.
Mistake #3: Skipping a real neuro exam because “we’ll just image it”
Strength testing, reflex checks, and sensory mapping are not optional theater. They are how clinicians decide whether imaging is urgent, and which type is likely to matter. If you don’t get a meaningful exam, you can end up with a scan that produces more questions than answers. (If you want a simple, safe self-check to discuss at your visit, try the straight leg raise test at home and note what reproduces your leg symptoms.)
Mistake #4: Not asking, “What will we do differently based on results?”
That sentence is your superpower. If the answer is “Nothing,” consider whether imaging is truly needed right now. If the answer is “If we see X, we’ll do Y,” you’ve just clarified the purpose of the test and reduced the odds of drifting into expensive uncertainty.
- X-ray doesn’t show nerves; MRI can show too much without context.
- A good neuro exam prevents “scan first, think later” spirals.
- The best question is always: “What changes if this is positive?”
Apply in 60 seconds: Write your “what changes” question on a note and bring it to the appointment.
Don’t do this: 2 decisions that backfire in US care pathways
Don’t rush to MRI “for reassurance” if symptoms are steadily improving
If you’re improving week to week, an early MRI can sometimes backfire by turning normal findings into fear. It can also pull you toward interventions you don’t actually need. This isn’t about toughness. It’s about avoiding the psychological tax of a report that reads like a diagnosis when it’s really a description.
Don’t ignore new weakness while waiting weeks for routine imaging
The opposite trap is stoicism. If weakness is new, worsening, or function is dropping, waiting quietly for a routine appointment can be the wrong move. You don’t need to panic. You do need to communicate clearly and be evaluated appropriately.
Open loop: The one sentence that gets your clinician to explain the plan
Try this: “What are we trying to rule out today, and what will we do differently depending on what the imaging shows?” It’s calm, respectful, and it forces the plan into daylight where it belongs.
What to ask at the visit: get the right test for the right reason
“What are we ruling out with X-ray vs confirming with MRI?”
This question resets the conversation from “test shopping” to “clinical reasoning.” It also helps you understand whether your clinician suspects bone-level issues, nerve compression, or something outside the spine that needs a different path.
“What exam findings make MRI necessary today?”
Ask what in your exam or history supports MRI now. Strength loss? Reflex change? Sensory loss that matches a nerve root? A story that suggests a serious cause? This makes the decision feel less arbitrary and more evidence-based, which is what you deserve when your body is already being difficult.
“If MRI shows X, what’s the next step and timeline?”
It’s not enough to know what the MRI might show. You want to know what happens next: conservative care extension, physical therapy focus, injection referral, surgical consult, or additional testing. Timelines reduce anxiety because they turn the unknown into steps you can take.
Bring this: symptom map, triggers, numbness zones, weakness examples, prior episodes
Bring a short, concrete summary. Not a novel. Think: two minutes of high-signal data. “Pain goes from right buttock to calf. Worse sitting. Numbness on top of foot. I trip on stairs sometimes. Started 4 weeks ago. Improving a bit except sitting.” That is gold.
- Your symptom map (where pain/numbness travels)
- Any weakness examples (heel/toe walking, stairs, foot drop)
- Duration and weekly trend (improving vs stuck vs worse)
- Prior imaging or surgeries (if any)
- Insurance requirement question: “What documentation do you need for MRI authorization?” (If you’re weighing cost in an HDHP, see lumbar MRI cost on an HDHP.)
Neutral next step: Bring this list and ask the clinic to explain the pathway in plain language.
FAQ
Is an MRI always better than an X-ray for sciatica?
Not always. MRI shows soft tissues and nerves better, so it’s often more relevant for true nerve-pattern leg pain. But “better” depends on the question. If the concern is fracture, major bony change, or quick structural screening, an X-ray can be useful. The best test is the one that changes your plan.
Can an X-ray show a herniated disc causing leg pain?
X-ray generally does not directly show a herniated disc or nerve compression. It can show bone alignment and degenerative changes that sometimes relate to narrowing, but disc and nerve detail usually requires MRI.
When should I get an MRI for sciatica?
MRI is most commonly considered when symptoms persist and remain disabling, when there is objective weakness or progressive neurologic change, when red flags are present, or when planning an intervention such as an epidural injection or surgical evaluation. Your exam and symptom trend matter as much as the calendar.
Why do doctors order an X-ray first in the US?
Often because it’s fast, widely available, and can rule out certain bone-level problems. It may also align with documentation or authorization pathways before advanced imaging. That said, if your story strongly suggests nerve root involvement, you can ask whether MRI is the more direct next step.
What if my MRI is “normal” but my leg pain is severe?
It can happen. Pain can be severe even when imaging doesn’t show a clear structural cause. It may mean the irritation is not easily visible, the timing/exam suggests a different pain generator, or the issue is outside what the scan captured. The next step is usually to revisit the exam, consider hip/SI or peripheral nerve causes, and refine treatment based on function and neurologic findings.
What does spinal stenosis look like on MRI vs X-ray?
X-ray can show bony changes that may contribute to narrowing, but MRI typically shows the canal and soft-tissue elements more clearly. When symptoms suggest stenosis, MRI often provides more actionable detail for planning care.
Will insurance require X-ray before MRI?
Sometimes. Requirements vary by plan and pathway, and they can depend on documented exam findings, duration, and attempted conservative care. Ask directly: “What do you need in my chart for MRI approval?”
Do I need contrast MRI for sciatica?
Many sciatica evaluations use MRI without contrast. Contrast is typically reserved for specific concerns (for example, certain infection, tumor, post-surgical evaluation, or other targeted questions). Your clinician can explain whether your situation suggests a contrast study.
Is CT better than MRI for sciatica?
CT can be useful in certain scenarios, especially for bony detail, but MRI is often preferred for soft tissue and nerve root assessment. The choice depends on what needs to be answered and what’s available or appropriate for your situation.
What symptoms mean I shouldn’t wait for imaging?
New or worsening weakness, bowel/bladder changes, saddle numbness, fever with back pain, major trauma, and concerning systemic signs (like significant unexplained weight loss with other risk factors) should prompt urgent evaluation.

Next step: one concrete action you can do today
Make a 60-second “symptom map” (location, numbness, weakness, worst triggers)
Do this today. Not because you need to become your own radiologist, but because you need to become a clearer narrator. Your symptom map is what helps a clinician decide whether imaging is likely to matter. Keep it simple: start point, end point, numbness areas, weakness examples, top two triggers, and what makes it better.
Use this decision question: “Will imaging change treatment this month?”
It’s blunt. It’s effective. If the answer is no, your energy might be better spent on a focused exam, functional rehab, and tracking progress. If the answer is yes, you now have a reason to push for the test that actually answers the clinical question.
If yes, ask for the test that answers the clinical question (not the one that feels thorough)
“Thorough” can be an emotional word. “Answering the right question” is a clinical word. Go with clinical. Your future self will thank you.
Conclusion: the calm, high-signal plan
Let’s close the open loop from the start: the test that “actually explains” leg pain is rarely the test that feels most comforting in the moment. It’s the test that answers the clinical question at the exact point where your care is about to change direction. An X-ray can be a quick gatekeeper for bone-level concerns. An MRI can be the best map for disc and nerve-root questions, especially when symptoms persist, weakness appears, or an intervention is being considered.
Here’s your next step within 15 minutes: open a note and write your symptom map plus this one sentence: “Will imaging change my treatment this month, and if so, how?” Bring it to your visit. You’re not asking for more testing. You’re asking for a plan. If the plan starts drifting toward “extra tests just because,” it can help to know when nerve testing becomes relevant, too: sciatica EMG timing.
When to seek help (urgent / same-day)
- New or worsening leg weakness (tripping, foot drop, can’t heel/toe walk)
- New bowel or bladder control problems
- Saddle numbness (groin/perineal numbness)
- Fever with back pain, recent infection risk, IV drug use
- Major trauma, cancer history, unexplained weight loss, night pain that’s escalating
Last reviewed: 2026-02-18
