
TFESI vs Interlaminar ESI for Sciatica
Two people can both be told “get an epidural,” then walk into two completely different procedures—with two different risk conversations, two different spread patterns, and two different chances of hitting the real pain generator.
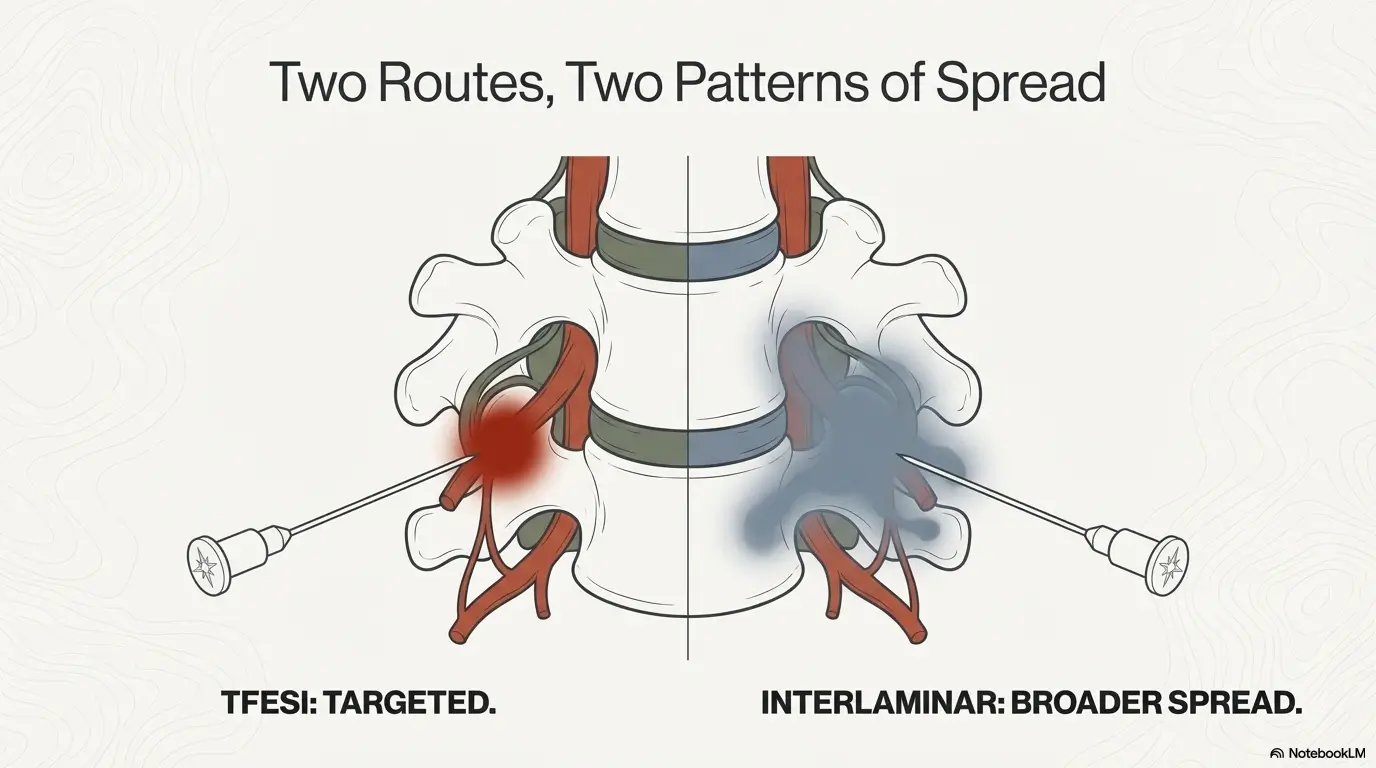
TFESI vs Interlaminar ESI for Sciatica is that fork in the road: TFESI (transforaminal) is typically a more targeted epidural route aimed near a specific irritated nerve root, while interlaminar ESI is often used for broader epidural spread—especially when symptoms or anatomy are less “one nerve, one level.” If you want the clean definition version in plain language, see transforaminal vs interlaminar epidural injections.
This post helps you walk into the appointment with a simple pain map, an MRI “zone” translation (foraminal vs lateral recess vs central canal), and the safety/process questions that matter (fluoroscopy, contrast confirmation, steroid choice). No bravado. Just a clean, data-informed decision framework.
- You’ll see the 7 differences that actually change outcomes.
- You’ll spot the common mismatch that makes any injection “fail.”
- You’ll steal a copy-paste script for your visit.
- You’ll leave with a 48-hour plan that protects your result.
Table of Contents
7 differences that actually change sciatica outcomes
Most comparisons online start with definitions. That’s fine—but it’s not what you actually need. You need the differences that change the result, because your goal isn’t to win trivia night. Your goal is to walk farther, sleep longer, sit without bargaining with your own spine, and get your life back in increments that feel real.
Think of TFESI (transforaminal) and interlaminar ESI as two ways of delivering medication into the epidural space. One tends to be more targeted toward a specific nerve root. The other often offers broader spread. “Better” is rarely universal—it’s match quality: the match between your pain pattern, your MRI, and the route your clinician uses safely.
- Route choice affects where medication goes.
- “Works better” depends on pain map + MRI zone.
- Success should be measured by function, not just pain.
Apply in 60 seconds: Write one sentence: “My worst symptom is ___ (leg pain, numbness, weakness) that travels to ___.” Bring it to your visit.

Difference #1: Targeting precision (one nerve root vs broader spread)
If your sciatica is driven by a specific irritated nerve root, the biggest practical advantage of a transforaminal approach is that it’s often designed to deliver medication closer to that nerve root’s exit zone. Interlaminar injections can still help—sometimes a lot—but their spread may be less “laser pointed.”
Decision clue: If your symptoms strongly follow one side and one nerve pattern (for example, classic L5 or S1 distribution), your clinician may discuss a targeted route. If your symptoms are mixed, multi-level, or less clearly mapped, broader spread may be part of the strategy.
Difference #2: Where medicine tends to go (ventral reach vs diffuse spread)
People talk about “getting the steroid to the front.” The practical translation: sciatica is often driven by irritation near the nerve root where it runs by discs and stenotic spaces. Some approaches are more likely to reach that area; others spread more generally. None of this is a guarantee—anatomy and technique matter—but spread patterns are part of why different routes exist.
Difference #3: Best-fit pain pattern (leg-dominant vs mixed back/leg pain)
Here’s a blunt, helpful filter: Is your problem mainly leg pain (nerve pain) or mainly back pain (mechanical pain)? Epidural steroid injections are generally discussed for radicular symptoms (leg-dominant nerve pain). If your pain is mostly axial back pain without a strong radicular picture, you may be comparing two routes that are both solving the wrong problem.
That doesn’t mean “nothing can help.” It means the best help may be a different tool—or a different target.
Difference #4: MRI match (foraminal vs lateral recess vs central)
Two people can both say “I have sciatica” and mean two different anatomy stories. If your MRI language points to foraminal narrowing (where the nerve exits), the transforaminal conversation often becomes more relevant. If your MRI points to central canal stenosis or multi-level changes, the “best route” becomes more nuanced. We’ll translate those words in the MRI zone map section—and if you’re still sorting the big labels, sciatica vs herniated disc can help you frame what’s actually being described.
Difference #5: Time window that matters (2 weeks vs 6+ weeks expectations)
When studies compare TFESI vs interlaminar ESI, differences—when they show up—often show up early. Later, things can blur: symptoms fluctuate, activity changes, and other treatments start or stop. The honest expectation for many people is a short-term “opening” (days to weeks) that you can use to rebuild function—rather than a permanent “fix” delivered through a needle.
Difference #6: Safety tradeoffs (why route + anatomy changes risk)
This is the part nobody wants to read, but everyone should understand: route choice is not only about effect—it’s also about risk profile. The FDA has warned about rare but serious neurologic adverse events reported after epidural corticosteroid injections, and notes that epidural use of corticosteroids is not FDA-approved. That doesn’t mean “never do it.” It means you deserve a clinician who treats safety as a first-class feature, not a footnote.
Show me the nerdy details
Comparative studies vary because “TFESI” and “interlaminar” are not single, identical procedures. Needle approach, level, contrast use, steroid type (particulate vs non-particulate), volume, and patient selection all change the result. That’s why two articles can both be “right” and still disagree.
Difference #7: Repeat strategy (what you do if it helps / doesn’t)
The best clinicians don’t just do an injection. They do a plan: what counts as success, when to reassess, and what the next move is if the benefit is partial or short-lived. If you’re offered “Come back anytime” with no success metric, you’re missing a key piece of the value.
Use this to avoid a “wrong-tool” appointment.
- Yes/No: Pain travels below the knee or follows a clear nerve path.
- Yes/No: MRI/clinical exam suggests a nerve root irritation level.
- Yes/No: You’ve tried time + activity modification + basic conservative care.
- Yes/No: You can list all meds (especially anticoagulants) accurately.
Neutral next step: If you answered “No” to the first two, ask your clinician to confirm the diagnosis before debating TF vs interlaminar.
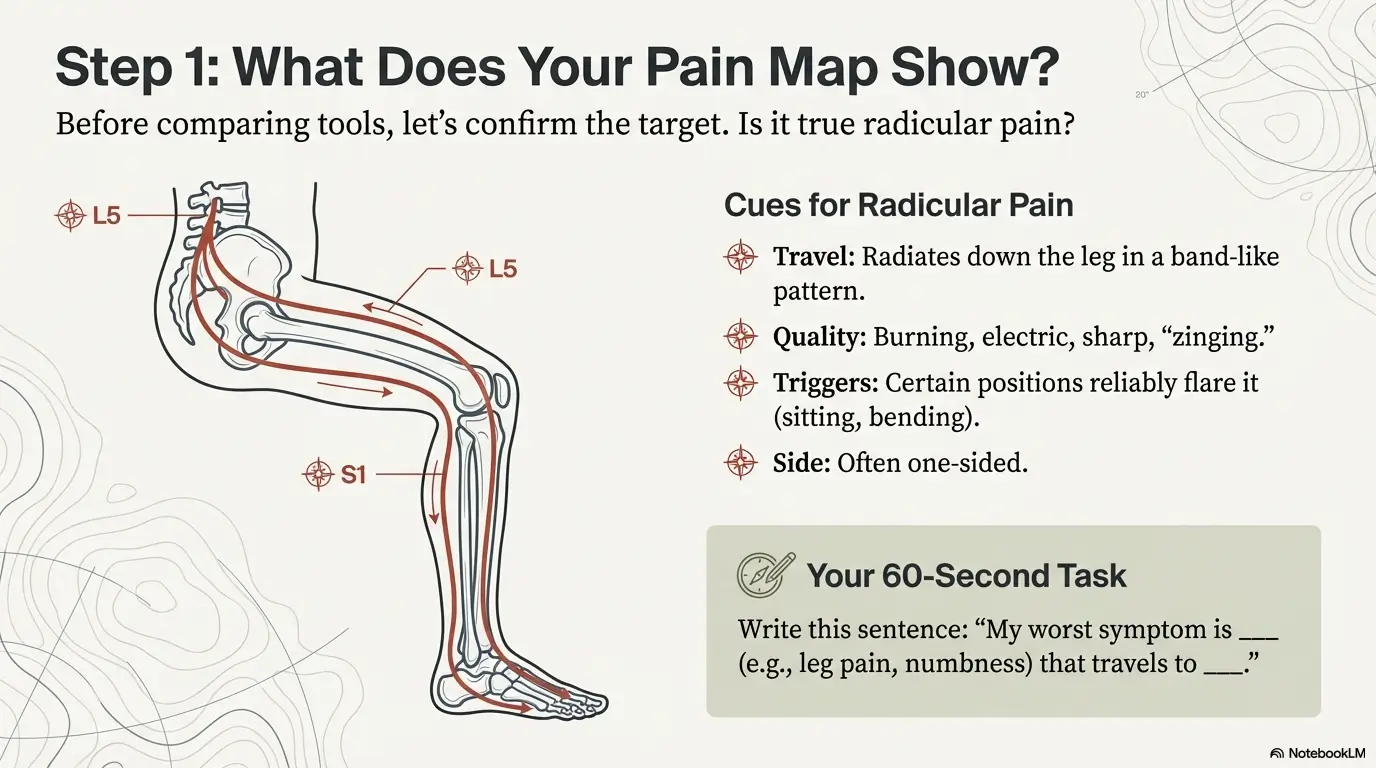
Quick self-check: is this true sciatica—or “back pain with referrals”?
Before you compare TFESI vs interlaminar ESI for sciatica, do one gentle thing: confirm that what you’re treating behaves like radicular pain. Because if it doesn’t, the “better” injection becomes the better way to be disappointed. If you need a calm baseline definition that separates “nerve pain” from everything else, start with what sciatica nerve pain typically feels like.
A common moment: you walk into the appointment thinking, “I just need the right injection,” and five minutes later you realize the real question is, “Are we sure this is the nerve root?” That moment is annoying. It’s also expensive to skip.
Pain-map cues that suggest radicular pain (without self-diagnosing)
- Travel: Pain radiates from back/buttock down the leg in a band-like pattern.
- Quality: Burning, electric, sharp, or “zinging” pain (often with numbness/tingling).
- Triggers: Certain positions reliably flare it (sitting, bending, coughing).
- Side: Often one-sided (though not always).
Bilateral/diffuse symptoms: when “which route” gets less obvious
If symptoms are widespread, bilateral, or feel more like heaviness/claudication when walking, you may be dealing with a different anatomy story (including stenosis patterns). In those cases, route selection is still relevant—but the “one nerve, one shot” framing is less reliable. And if symptoms include burning/tingling patterns that could be metabolic rather than spinal, it’s worth sanity-checking diabetic neuropathy vs sciatica before you over-commit to a spine-only explanation.
Let’s be honest… the wrong target makes any injection look “ineffective.”
If your pain generator is not the nerve root you’re treating, even a perfectly performed injection can “fail.” This isn’t your fault. It’s a diagnosis problem, a mapping problem, or an expectations problem—sometimes all three. (And yes: sometimes the “sciatica” label is covering something else, like sciatica vs piriformis syndrome confusion.)
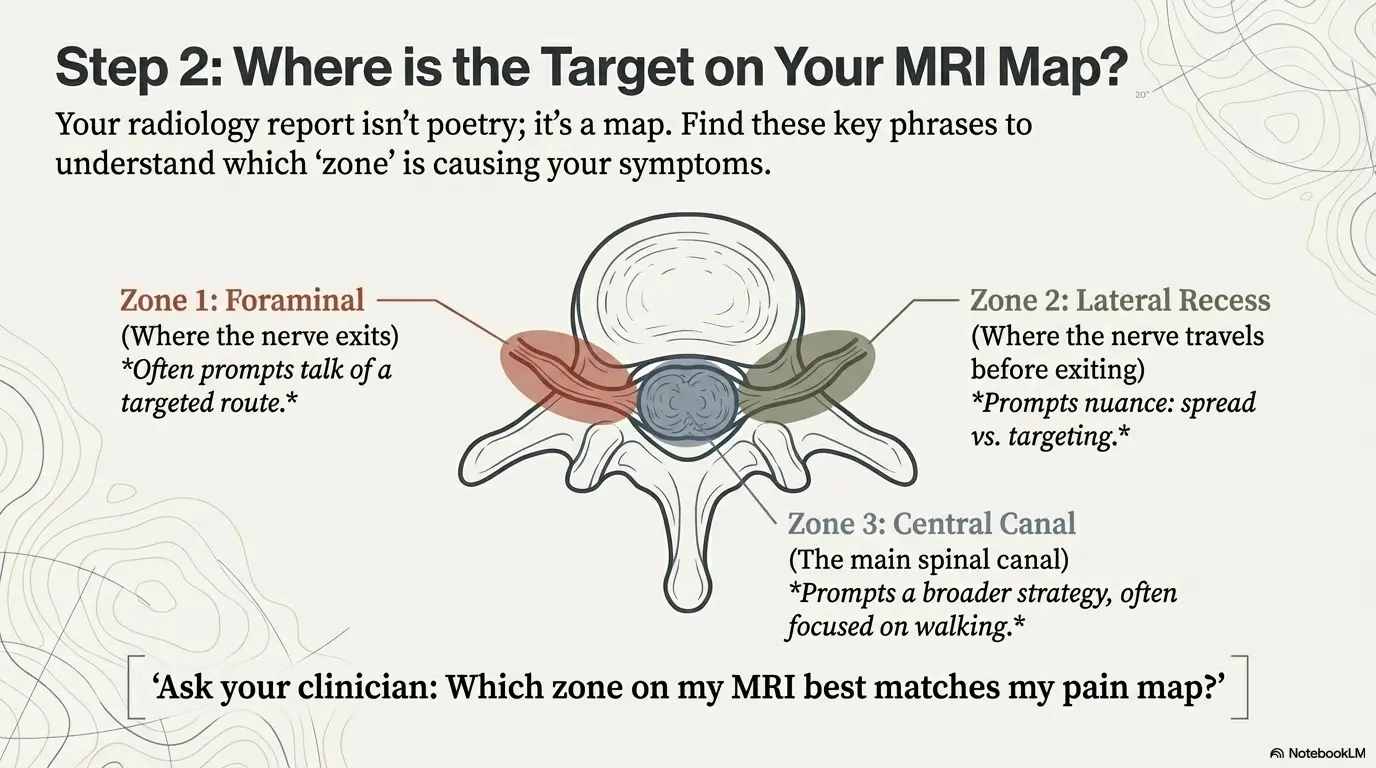
MRI “zone map”: the 3 compression zones that change route choice
Radiology reports can feel like a foreign language written by a cautious poet. You don’t need to become fluent. You just need to recognize three zones that often show up in sciatica discussions—and how each zone changes the TFESI vs interlaminar conversation.
Nerve exits the spine here.
Often prompts: “Targeted route” talk.
Nerve travels before exiting.
Often prompts: “Spread vs targeting” nuance.
Main canal narrowing.
Often prompts: broader strategy + walking tolerance focus.
How to use: Find the phrase in your MRI report (foraminal, lateral recess, central canal) and ask your clinician which zone fits your symptoms best.
Foraminal / exiting nerve root problems (often the TFESI conversation)
When the report emphasizes foraminal stenosis or exiting nerve root compression, clinicians often discuss transforaminal approaches because the target is near where the nerve exits. The clinical nuance: “foraminal” doesn’t automatically mean “TFESI wins,” but it often changes the logic of the conversation.
Lateral recess / traversing nerve root problems (route depends on level + spread)
Lateral recess narrowing can still produce classic sciatica. Here, the choice can hinge on level, anatomy, symptom dominance, and how your clinician expects medication to spread. This is a good place to ask, “How will you confirm epidural placement and spread?” and “What’s the plan if relief is partial?”
Central canal stenosis (why studies may not generalize to classic disc sciatica)
Central stenosis often behaves differently from a single-level disc herniation. People may describe heaviness, walking limits, or neurogenic claudication. Studies in central stenosis can’t always be applied cleanly to disc-driven sciatica, so route choice becomes more individualized—often focusing on function wins and walking tolerance. If you’re trying to separate these two “stories” quickly, lumbar spinal stenosis vs herniated disc is the comparison that keeps the logic straight.
What the best head-to-head data actually shows (and what it doesn’t)
“Data-backed” is not a magic spell. In this topic, it usually means: systematic reviews, randomized trials, registry data, and comparative studies that look at pain and function over set time points. Here’s the calm truth: different studies disagree because they’re studying different people, different techniques, and different outcome definitions.
One often-cited summary of comparative studies notes that short-term differences can favor transforaminal approaches for pain relief at around two weeks, while differences may disappear at one and six months. That doesn’t mean “TFESI is better” or “it’s the same.” It means the early window may be where route matters most—especially if you use that window to rebuild function.
- Short-term relief may differ by route in some analyses.
- Longer-term results often depend on diagnosis and rehab follow-through.
- Technique variability can be bigger than the route label.
Apply in 60 seconds: Ask: “What timepoint do you use to judge success—2 weeks, 6 weeks, or 3 months?”
Short-term: where some comparisons show a small edge (and why “small” matters)
A small percentage difference in pain relief can sound impressive or trivial depending on your week. If you’re sleeping 3 hours and limping, even a modest improvement is a win. But “small” also means: don’t bet your whole plan on the needle alone. Bet on the needle plus a function plan.
1–6 months: why differences often shrink or vary by study
Over months, a lot changes: activity levels, flares, work demands, physical therapy adherence, and natural healing patterns. Also, people who feel better move more—which can both help and aggravate. That’s why some longer-term comparisons don’t show a clear winner: the “treatment” becomes a bundle of everything that happens after the injection.
Here’s what no one tells you… technique + diagnosis mismatch can dwarf “TF vs IL.”
Two injections with the same label can be performed with different safety protocols, different medications, different levels, and different imaging confirmation. Meanwhile, two people with “sciatica” can have different underlying causes. If the cause isn’t matched, even the “best” approach can underperform.
Show me the nerdy details
Outcome studies may use different pain scales, different “success” thresholds (like 30% vs 50% improvement), and different patient populations (disc herniation vs stenosis vs mixed). Registry studies can capture real-world practice but may have confounding. Trials can be cleaner but may be smaller and less generalizable.
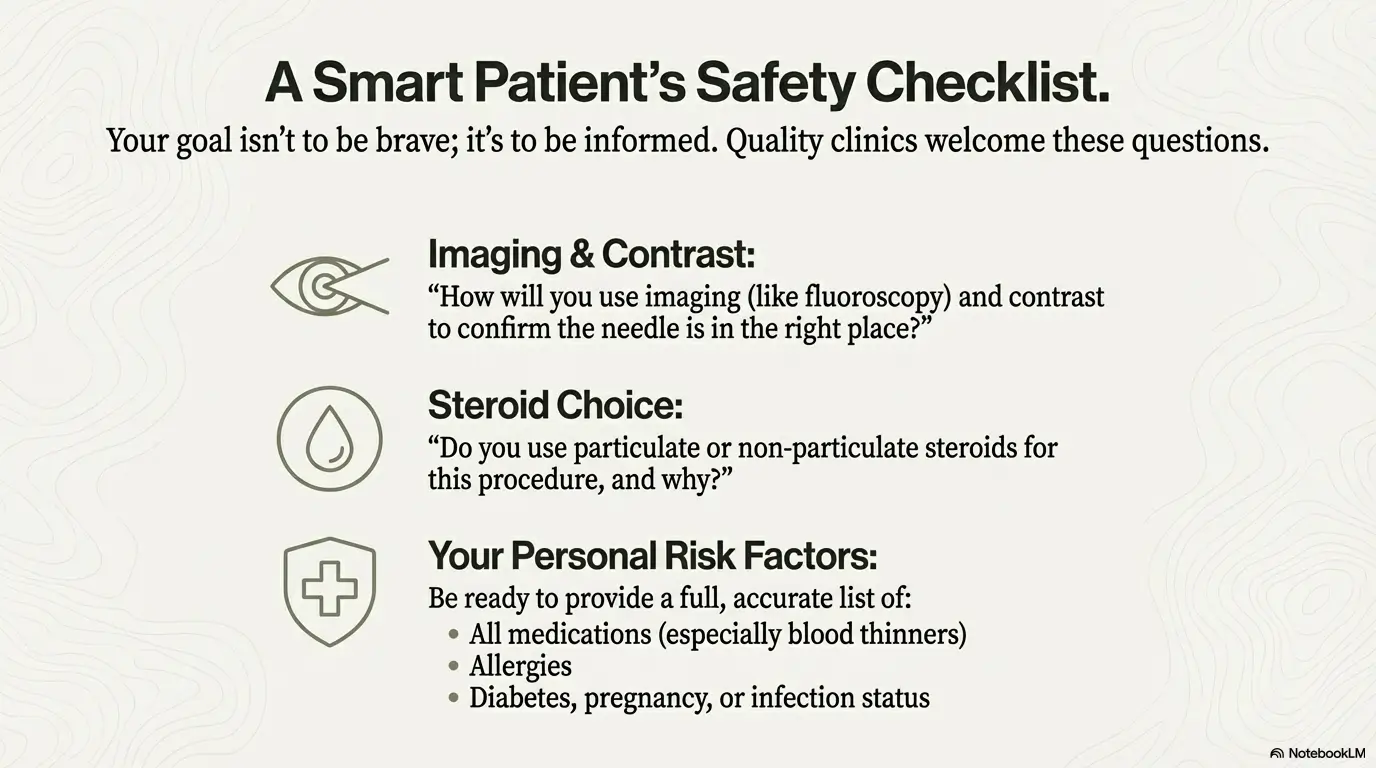
Safety-first comparison: the risks people underestimate (and how clinics reduce them)
Let’s treat safety like adults: rare events can still matter, and your goal is not to be “brave.” Your goal is to be smart. The FDA has communicated that rare but serious neurologic problems have been reported after epidural corticosteroid injections. The practical takeaway isn’t panic—it’s quality control: imaging guidance, contrast confirmation, careful medication choice, and clear post-procedure instructions.
Imaging guidance + contrast: what “good process” usually includes
Many coverage and clinical policies emphasize image guidance and contrast confirmation to verify epidural placement (with limited exceptions). You don’t need to argue about it—you just need to ask what your clinic does, and why. A clinician who welcomes that question is usually a good sign.
Steroid choice & particulate discussion (what to ask, not what to self-prescribe)
You’ll sometimes hear “particulate” vs “non-particulate” steroid discussions, especially in transforaminal injections. Specialty societies and safety-focused publications have discussed risk considerations around particulate steroids, and some clinicians prefer non-particulate options in certain contexts. This is not something to decide from a blog—but it is something you can ask about calmly.
Special risk factors: anticoagulants, diabetes, infection risk, allergies
- Blood thinners: You need specific guidance on holding/continuing meds—never guess.
- Diabetes: Steroids can raise blood sugar; plan monitoring.
- Infection risk: Fever, active infection, or immune suppression changes decisions.
- Allergies/pregnancy: Contrast and medication considerations matter.
Exact prices vary by region, facility, and insurance. Instead of guessing a dollar figure, use this table to compare what changes the bill.
| Cost driver | What to ask | Why it matters |
|---|---|---|
| Facility type | “Hospital outpatient vs ambulatory center?” | Site-of-service often shifts allowed amounts and patient responsibility. |
| Imaging guidance | “Fluoro/CT with contrast?” | Safety and coding/coverage criteria can depend on guidance. |
| Number of levels | “One level or multiple?” | Multi-level work can change time, meds, and billing. |
| Insurance rules | “Pre-auth required? PT trial required?” | Many plans use criteria; delays happen when paperwork is missing. |
Neutral next step: Call your insurer and ask for your estimated responsibility using the procedure description your clinic provides. If the broader picture is stenosis and you’re cost-planning beyond injections, bookmark lumbar spinal stenosis surgery costs (2025) so you’re not blindsided later.
TFESI: when it tends to be chosen—and when it’s a mismatch
Transforaminal ESI is often discussed when the clinician wants to deliver medication near a specific nerve root—especially when symptoms and imaging point to a particular level and side. That targeting can be the entire point of the procedure.
A common scene: someone comes in saying, “My MRI looks scary,” but their pain pattern doesn’t match the “scary” level. A careful clinician pauses, maps symptoms, and adjusts the plan. That pause is worth more than a confident speech.
Best-fit scenarios: single-root, foraminal-type irritation pattern
- Clear one-sided radicular pain pattern
- Imaging suggests an exit-zone problem that matches symptoms
- Prior injection helped briefly and you’re trying a more targeted match
Tradeoffs: why precision can come with stricter safety demands
Targeting is not “free.” In certain contexts, transforaminal injections carry specific safety considerations that drive technique choices (imaging confirmation, medication selection, careful approach). Ask your clinician how they reduce risk—and listen for specifics, not vibes.
Show me the nerdy details
“Targeted” does not mean “stronger.” It means the intended spread is more localized. Volume, level, anatomy, and prior surgery can alter spread. Clinicians may choose different steroid types based on risk considerations and location—and if you’re dealing with post-op anatomy, it helps to understand the bigger umbrella of failed back surgery syndrome conversations that can change expectations.
Interlaminar ESI: when broader spread is exactly what you want
Interlaminar ESI is sometimes framed as the “traditional” epidural injection. The more useful framing is: it can deliver medication in a way that may cover a broader epidural region. That can be helpful when the target is less clearly a single nerve root—or when symptoms suggest more diffuse irritation.
This is where people accidentally sabotage themselves: they hear “broader spread” and think “less effective.” Sometimes broader spread is the strategy. The point is to match the approach to your anatomy story.
Best-fit scenarios: multi-level irritation, less clear single-root target
- Symptoms are less clearly mapped to one nerve level
- Imaging shows multi-level changes that match a more diffuse story
- Clinician believes broader epidural distribution fits your case
What “success” can look like: function wins (walking, sleep, sitting)
If your pain goes from “can’t sit 10 minutes” to “can sit 35 minutes,” that’s not a minor win. That’s a life win. Aim to measure success by two or three function metrics you can repeat, not by the emotional roller coaster of hourly pain ratings—and if walking is your clearest metric, make it easier on your body with sciatica-friendly walking shoes that reduce flare triggers.
- TFESI can be chosen for a specific nerve-root target.
- Interlaminar can be chosen for broader epidural distribution.
- Success = pain + function + time window, not one number.
Apply in 60 seconds: Pick 2 metrics: “Walk __ minutes” and “Sit __ minutes.” Track before and after.
Common mistakes that sabotage results (don’t do this)
This section is pure loss prevention. Not because you’re careless—because pain makes the brain narrow its focus. When you’re exhausted, you want the fastest path to relief. That’s human. Here’s how to keep that human impulse from costing you time and money.
Mistake #1: Choosing based on someone else’s story (not your pain map + MRI)
Your cousin’s injection success doesn’t map onto your anatomy. The procedure name is not the diagnosis. The cure for this mistake is simple: bring a pain map and ask which MRI “zone” matches it best.
Mistake #2: Treating “back pain” like it’s always radicular sciatica
If the dominant symptom is axial back pain without a clear radicular pattern, you may be trying to solve a mechanical problem with a nerve-targeted tool. Ask the clinician to say out loud: “What exactly are we treating?”
Mistake #3: Skipping the meds list (bleeding risk conversations matter)
“I think I’m on a blood thinner” is not a safe sentence. Bring a printed list or a phone screenshot. Your clinic will thank you. More importantly, your body will.
Mistake #4: Measuring success only as “pain = zero” (instead: function metric)
Zero-pain expectations create two traps: you dismiss meaningful improvement, or you push too hard too soon. A better target is function: walk time, sit time, sleep hours, and “how many breaks to get through a workday.”
Mistake #5: Skipping a plan for rehab, sleep, and pacing
If the injection gives you a window, use it. If you don’t, you may spend the window “testing” your pain instead of rebuilding capacity. A simple, boring plan beats a dramatic, inconsistent one—and if you’re weighing options for guided care, physical therapy for chronic low back pain is often the “boring” lever that actually compounds.
- One-sided radicular pattern is clear
- MRI suggests exit-zone/foraminal match
- You want a targeted diagnostic/therapeutic approach
- Symptoms are broader or multi-level
- Coverage is the goal
- Clinician expects broader epidural spread to help
Neutral next step: Ask your clinician: “Which box am I in, and what evidence from my exam/MRI puts me there?”
Decision framework: pick the “next best step,” not the perfect answer
When you’re in pain, your brain wants certainty. But medicine often offers probabilities. The most rational move is not “pick the perfect injection.” It’s: pick the best next step with a clean reassessment plan.
A familiar pattern: people ask, “Which is better?” when what they mean is, “Which one prevents me from wasting the next month?” This framework is designed to protect the next month.
Step 1: Confirm radicular pattern + likely level
Ask the clinician to map your symptoms to a suspected level and side. If they can’t, pause. “No level” often means “no target.”
Step 2: Match route to goal (precision vs coverage)
Say it plainly: “Are we aiming for a specific nerve root target, or broader epidural coverage?” Route should follow goal.
Step 3: Define your success metric + time-box reassessment
Pick 2–3 metrics. Examples: sit time, walk time, sleep hours, number of breaks at work. Decide when you’ll reassess: commonly at 2 weeks and again at 6 weeks, depending on clinician guidance.
Copy/paste appointment script (questions that reveal quality & fit)
- “What diagnosis are we treating, specifically?”
- “Which MRI zone best matches my symptoms?”
- “What route matches that zone—and why?”
- “How will you confirm placement and spread (imaging/contrast)?”
- “What would count as success at 2 weeks?”
- “If it helps only a little, what’s the next step?”
Use 2 metrics you can measure without drama. No storage; do it on paper.
- Baseline walk time (minutes): ___
- Baseline sit time (minutes): ___
- After injection (same test): walk ___ / sit ___
Result rule: If either metric improves by ~20–30% and stays improved for several days, that’s meaningful—use the window to build consistency (gentle walking, pacing, PT guidance).
Neutral next step: Bring your numbers to follow-up instead of relying on memory.
After the injection: a 48-hour plan that protects your result
This is where many people accidentally ruin their own data. You feel a bit better and immediately “test” your back with the exact thing that flares it. Or you feel worse for a day and decide it “failed” before the medication timing has even had a chance to play out.
Two honest time truths: numbing medicine can create early relief (then fade), and steroids can take days to fully show effect. Your clinician’s instructions always come first, but here’s a practical way to avoid self-sabotage.
The “don’t evaluate too early” rule (local anesthetic vs steroid timing)
- First day: Treat early relief as information, not a verdict.
- First 48 hours: Avoid extreme movements and heavy “proving” activities.
- Days 3–14: Track trends and function, not hourly pain spikes.
Simple tracking: pain map + function (walk time, sit time, sleep)
Use the same two function tests every day for a week. Keep it boring. Boring is reliable. Pain is emotional; function is measurable. And if your flare-ups are tightly tied to sitting/commuting/desk posture, don’t ignore the pattern—desk-job sciatica flare-ups are one of the most common ways people accidentally erase their own progress.
When to seek help now (red flags + urgent symptoms)
This section is here to lower panic, not raise it. Most people don’t need urgent care after an injection. But certain symptoms are not “wait and see.” If you’re unsure, call your clinician’s office—or seek urgent evaluation. If you want a clearer checklist for when low back symptoms cross into “don’t wait,” use low back pain emergency warning signs as a second set of eyes.
Go urgently if you have
- New or worsening weakness (foot drop, cannot push off, frequent tripping)
- New bowel/bladder issues or saddle numbness
- Fever with severe back pain or signs of systemic illness
Call your clinician promptly if
- Severe headache, especially if positional
- Escalating pain that feels different than your usual pattern
- New neurologic symptoms (new numbness, new weakness)
- High blood sugar spikes if you have diabetes
FAQ
Does TFESI work better than interlaminar ESI for sciatica?
Sometimes, in some short-term comparisons, TFESI shows a small advantage—especially when symptoms and imaging point to a specific nerve root target. Over longer timeframes, differences can shrink or vary. The practical answer is: it depends on whether your symptoms and MRI point to a specific target (precision) or a broader strategy (coverage).
How long does relief usually last—and what if it wears off fast?
Relief can range from days to months, and some people feel only partial improvement. If relief is short-lived, don’t assume it was “useless.” It may still confirm the pain generator, or it may signal you need a different target, a different route, or a broader plan (rehab, meds review, imaging reassessment).
Which approach fits a herniated disc vs spinal stenosis?
Disc-related sciatica often maps cleanly to a specific nerve root distribution, which can make targeted discussions more common. Stenosis patterns can be more diffuse and may emphasize function (walking tolerance). The key is matching your symptoms to your MRI zone—not guessing based on the diagnosis label alone. If you’re time-boxing “how long do I wait before escalating,” herniated disc sciatica wait time can help you frame the decision without spiraling.
Is one approach safer than the other?
Both have risks, and route-specific anatomy can change risk considerations. Ask how your clinician reduces risk: imaging guidance, contrast confirmation (when appropriate), medication selection, and clear post-procedure monitoring instructions. The best safety signal is a clinician who can explain their process in plain language.
How many epidural steroid injections are considered “too many”?
Frequency limits vary by clinician judgment and insurance criteria. The smarter approach is to treat each injection as a time-boxed experiment with a success metric. If repeated injections don’t produce meaningful functional improvement, it’s reasonable to revisit the diagnosis and the overall plan.
Can an ESI make sciatica worse at first?
Some people feel temporary soreness, irritation, or a short flare. Numbing medicine can also create a brief “better then worse” swing. What matters is trend over days—not hour-by-hour emotion. If pain is severe, different, or accompanied by new neurologic symptoms, call your clinician promptly.
Do I need an MRI before choosing TFESI vs interlaminar?
Not everyone needs an MRI immediately, but route selection is often more rational when you can match symptoms to anatomy. If your symptoms are severe, persistent, or complicated by weakness, imaging may become part of the decision. Ask your clinician what information would change the plan.
What questions should I ask about fluoroscopy and contrast?
Ask what imaging guidance is used, how placement is confirmed, and what alternatives are used if contrast is contraindicated (for example, due to allergy or pregnancy). Your goal is not to micromanage—it’s to confirm that safety steps are routine.
Next step (10 minutes)
Do this before your appointment: write a 3-line pain map and bring your MRI report (if you have one) plus a full medication list.
- Start: Where does the pain start (back, buttock, hip)?
- Travel: Where does it travel (thigh, calf, foot, toes)?
- Triggers: What reliably worsens/relieves it (sitting, bending, walking, coughing)?
Then ask: “Given my pain map and MRI zone, which route best matches the target—and what safety steps will you use to confirm placement?”
- Medication list (especially anticoagulants/antiplatelets)
- Allergies (contrast, meds, latex)
- Imaging report (MRI/CT) + date
- Prior injection details (route, level, response timeline) — if you’re unsure what you previously had, compare it to an L5–S1 selective nerve root block so you can describe it accurately.
- 2 function metrics you care about (walk/sit/sleep)
Neutral next step: Send this list to the clinic portal before the visit if you can.
Conclusion
So—TFESI vs interlaminar ESI for sciatica: which works better? The honest answer is the one you suspected all along, but didn’t want to hear in the middle of a flare: the better one is the one that matches your target and your safety profile. For some people, that means a targeted route because the nerve root story is clear. For others, it means a broader strategy because the story is diffuse. And for many, the real win is using any relief window to rebuild function—walking, sitting, sleeping—like you’re buying back your week one measurable minute at a time.
Close the loop from the hook: vague answers fade when you bring a pain map, a success metric, and a clinician who can explain their method. You don’t need perfect certainty. You need a plan you can measure.
15-minute CTA: Put a timer on. Write your pain map (3 lines). Pick your 2 function metrics. Copy the appointment script from this article into your notes app. Show up calm—and specific.
Last reviewed: 2025-12.
