Heat vs. Ice: The Strategy of Relief
A heating pad can feel like mercy. An ice wrap can feel like discipline. The trouble is that orthopedic pain does not care which one you prefer, and the wrong choice can turn a small flare into a longer, louder problem.
Orthopedic pain management comes down to signals: swelling, warmth, stiffness, timing, and skin safety. Most people reach for whatever is nearby, only to wonder why the shoulder complains again by dinner.
Fresh, swollen, warm, or activity-triggered flares.
Stiff, tight, chronic, or muscle-guarded patterns.
The method is simple: Read the pain pattern, use short sessions, protect your skin, and judge the result by function, not just “vibes.” Let your next walk, stair, or night of sleep tell the truth.
Table of Contents
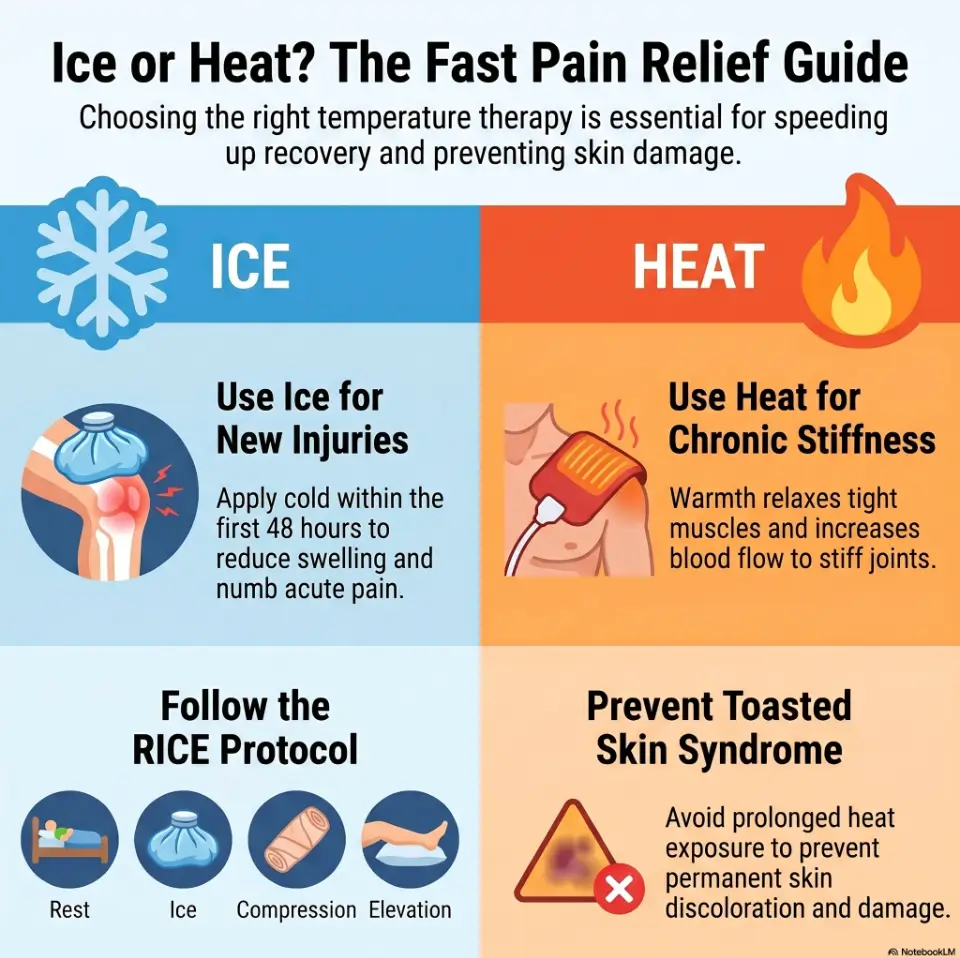
Safety / Disclaimer: Home Relief Is Not a Diagnosis
Heat and ice can calm symptoms. They do not explain the cause. That difference matters, especially with orthopedic pain, where a mild ache, tendon irritation, arthritis flare, nerve symptom, or fracture can all arrive wearing the same gloomy coat.
Johns Hopkins Medicine describes cold therapy as useful for numbing pain and reducing swelling or inflammation, while warmth is often used for sore, tight muscles. That is a helpful starting line, not a full map.
Heat and ice can help symptoms, not explain the cause
A heating pad may loosen a guarded back. An ice wrap may quiet a swollen knee. But if pain follows a fall, a pop, a visible deformity, fever, spreading redness, numbness, weakness, or inability to bear weight, the next tool should not be another pack. It should be medical guidance.
Why “it helped last time” can be a risky rule
I learned this the unglamorous way after treating every cranky joint like the same old villain. One week, warmth helped a stiff shoulder. Another week, the same warmth made a hot, irritated knee feel as if a tiny committee of bees had moved in.
Same person. Same drawer of supplies. Different pain pattern.
Use short sessions, skin barriers, and symptom tracking
For most simple at-home use, think in short sessions: often around 15 to 20 minutes for ice, and limited awake use for heat. Place a cloth barrier between your skin and the pack. Check your skin before, during, and after.
Avoid heat or ice if sensation, circulation, or skin integrity is impaired unless a clinician says it is safe
People with reduced sensation, poor circulation, fragile skin, open wounds, diabetes-related nerve changes, or certain vascular conditions need extra caution. If the skin cannot properly feel heat or cold, it cannot warn you early. The body’s alarm system gets muffled, which is rude but important.
- Use cold for many new, swollen, warm, or injury-linked patterns.
- Use heat more cautiously for stiffness, tightness, and guarded muscles.
- Stop if skin changes, pain worsens, or function drops.
Apply in 60 seconds: Before using either tool, write one sentence: “My pain is mostly swollen, stiff, hot, sharp, achy, or tight.”
Start Here: The Pain Pattern Decides More Than the Product
The product label is not the boss. The pain pattern is. A plush heating pad with seven settings can still be the wrong choice for a knee that is warm and puffy after a misjudged staircase moment. An expensive ice wrap can also be overkill for a back that feels stiff until you walk for 8 minutes.
New, swollen, or hot pain usually points toward cold
Cold tends to make more sense when the area feels newly irritated: swelling, warmth, sudden soreness after activity, or pain after a twist, bump, or strain. The goal is not to punish the tissue into silence. The goal is to reduce the “angry signal” enough to move safely and reassess.
Stiff, tight, or chronic muscle discomfort may respond better to heat
Heat often makes sense when the body feels locked rather than inflamed: morning stiffness, muscle guarding, chronic tightness, or aches that improve with gentle movement. Warmth can make the first few steps, reaches, or bends feel less like negotiating with a rusty gate.
The hidden question: “Is this irritation or restriction?”
Ask this before choosing:
- Irritation: new pain, swelling, warmth, tenderness after activity, throbbing, or sharp flare.
- Restriction: stiffness, tightness, slow warm-up, guarded movement, or chronic muscle ache.
It is not perfect, but it is better than choosing based on which pack is closest to the couch.
Let’s be honest: most people choose based on habit, not signals
We are creatures of drawers. If the heating pad lives on the nightstand, heat becomes the family doctor. If the gel pack lives beside frozen peas, ice becomes the household philosopher. Signal-based choice is less dramatic, but it works better.
Mini Infographic: The 3-Door Choice
🧊
Door 1: Ice Wrap
Choose when pain is new, swollen, warm, or flared after activity.
♨️
Door 2: Heating Pad
Choose when pain is stiff, tight, chronic, or better after gentle motion.
🚩
Door 3: Get Help
Choose care when pain is severe, worsening, traumatic, numb, weak, red, feverish, or function-limiting.
Ice Wrap First? When Cold Therapy Makes the Most Sense
An ice wrap earns its place when pain feels fresh, hot, swollen, or activity-provoked. Cold is the quiet friend who turns down the volume when the room gets too loud. It is especially useful after minor sprains, bumps, flare-ups, and sudden overuse, assuming there are no red flags.
After a twist, bump, flare, or sudden overuse
If your ankle rolls during a walk, your knee swells after yard work, or your shoulder protests after moving boxes, cold is often the safer opening move. Think of the first 24 to 48 hours as a period of observation. The body is sending weather reports. Do not ignore the thunder.
When swelling is the loudest symptom in the room
Swelling is not automatically evil. It can be part of healing. But too much swelling can increase pain, limit motion, and make normal tasks harder. Cold may help reduce the intensity of that response long enough for you to move carefully, elevate, or avoid the activity that stirred the pot.
Why compression-style ice wraps can feel more controlled than loose packs
A wrap can stay in place better than a bag of ice cubes sliding around like a fish with opinions. For knees, ankles, elbows, and shoulders, that steadiness matters. A wrap also makes it easier to combine cold with light compression when appropriate.
Still, compression should feel supportive, not strangling. If toes or fingers tingle, turn pale, turn blue, or feel numb, loosen it and reassess.
The 15–20 minute guardrail: relief without skin trouble
More is not always more. Ice left too long can irritate skin and, in rare cases, damage tissue. A common practical guardrail is roughly 15 to 20 minutes, with a cloth barrier and skin checks. If the area becomes painfully cold, numb in a concerning way, or oddly colored, stop.
- Use a towel barrier.
- Keep sessions short.
- Watch skin color and sensation.
Apply in 60 seconds: After icing, check whether walking, bending, gripping, or stairs feel easier 30 minutes later.
Heating Pad First? When Warmth Is the Better Opening Move
A heating pad is not just a device. It is a small domestic sun. That is why people love it. Warmth can relax muscles, soften stiffness, and make the first movement of the day feel less like opening an old library door.
Morning stiffness, chronic tightness, and guarded muscles
Heat often fits pain that feels stiff rather than swollen. Think chronic low back tightness, a guarded shoulder, an achy hip that loosens after walking, or arthritis stiffness that feels worse after sitting. The goal is to make gentle motion easier, not to roast the joint into submission.
Before gentle movement, stretching, or daily tasks
Heat is often most useful before activity. Ten to 20 minutes of mild warmth before a short walk, gentle stretching, or a shower routine can make movement feel more available. That matters because function is the real scoreboard.
One caregiver trick I like: use warmth before the task that keeps getting avoided. If getting dressed is the daily mountain, do not use the heating pad randomly at 10 p.m. Use it before the mountain.
Why heat can feel emotionally comforting but still needs limits
Warmth calms more than tissue. It calms the nervous system, the mood, the small household panic that arrives when pain interrupts ordinary life. That comfort is real. But comfort can also make us sloppy.
Use a low or moderate setting, keep a fabric layer between skin and pad when needed, and stay awake. A heating pad is not a teddy bear with a plug.
Here’s what no one tells you: warmth can hide a worsening flare
Heat can feel good while swelling increases. That is the trap. If warmth makes the area redder, puffier, hotter, more painful, or less functional afterward, it was probably the wrong tool for that moment.
Show me the nerdy details
Heat tends to increase local blood flow and tissue extensibility, which may help muscles relax and make gentle movement easier. Cold tends to reduce nerve signal speed and local metabolic activity, which can reduce pain sensation and calm irritated tissue. In plain English: heat can help stiffness move; cold can help angry swelling quiet down. Neither tool fixes the underlying cause by itself.

Don’t Do This: The “Heat on Fresh Swelling” Mistake
This is the classic household error: something hurts after a twist, bump, or sudden overuse, and the heating pad appears like a well-meaning aunt with soup. Kind, but possibly not useful.
Why warmth can be the wrong guest at a fresh injury party
Fresh swelling often means the area is already irritated and full of activity. Adding heat may increase blood flow and make the area feel more congested. That can mean more throbbing, more puffiness, and a louder pain signal later.
Not every fresh injury needs panic. But it does need respect. If a joint is newly swollen, hot, or sharp after a specific event, cold usually gets first consideration.
Red flags that heat is making things angrier
Stop heat and reassess if you notice:
- More swelling within 30 to 60 minutes.
- Increasing redness or warmth.
- Throbbing that gets louder after heat.
- Less ability to walk, grip, climb stairs, or sleep.
- Burning, blistering, or unusual skin color.
Safer swap: cold, elevation, rest from aggravating activity, and reassessment
If heat makes fresh swelling worse, switch the strategy. Use cold with a barrier, elevate when practical, pause the activity that triggered symptoms, and monitor function. If the pain is severe, traumatic, or not improving, get medical advice.
- New warmth plus puffiness usually favors cold first.
- Comfort during use does not prove the tool helped.
- Function after use matters more than the momentary “mmm.”
Apply in 60 seconds: Take a quick “before” note: swelling, warmth, pain score, and one function such as stairs or standing.
- Johns Hopkins Medicine: Ice Packs vs. Warm Compresses for Pain
A highly credible medical source explaining when to use heat versus ice. It fits naturally with sections discussing cold therapy for swelling and inflammation, and heat therapy for stiffness and muscle tension.
- Mayo Clinic: Sprain First Aid
A trusted reference for early sprain care, including ice use, skin protection, and first-aid steps after minor injuries. It works well with sections about fresh swelling, acute injury, and the first 48 hours.
- Cleveland Clinic: Toasted Skin Syndrome
A useful safety resource on skin damage from repeated low-level heat exposure, including heating pads and other heat sources. It fits well with sections warning against falling asleep with a heating pad and emphasizing skin safety.
Don’t Do This Either: Falling Asleep With a Heating Pad
Falling asleep on a heating pad sounds harmless until you remember that skin is not cookware. Burns can happen slowly, especially with prolonged exposure, high settings, thin skin, reduced sensation, or fatigue.
Burns can happen slowly, especially when you are tired
A sleepy person is a terrible safety monitor. The body stops giving useful feedback, and the heating pad keeps doing its little electric opera. Even low heat, used too long and too often, may irritate or damage skin.
Why older adults and people with reduced sensation need extra caution
Older adults may have thinner skin, slower reaction time, or reduced sensation. People with neuropathy or circulation problems may not feel temperature accurately. That makes “it doesn’t feel too hot” a weak safety test.
Caregivers should check the skin, the setting, the session length, and whether the person can remove the pad independently. This is not fussing. This is engineering the room so pain relief does not become a new problem.
Safer setup: timer, low setting, towel layer, awake use only
Use heat while awake. Choose a lower setting. Set a timer. Avoid lying directly on top of the pad unless the product instructions clearly allow that position. Do not use a damaged cord, a pad with strange hot spots, or a device that looks as if it survived a basement flood in 1998.
Eligibility checklist: Is a heating pad a reasonable home option today?
- Yes / No: The area is stiff or tight, not newly swollen or hot.
- Yes / No: Skin sensation is normal.
- Yes / No: Skin is intact, not irritated, open, or fragile.
- Yes / No: You can stay awake and remove the pad easily.
- Yes / No: You can use a timer and a safe setting.
Neutral next step: If any answer is “No,” skip heat for now and ask a clinician or pharmacist what is safe for your situation.
Heating Pad Versus Ice Wrap by Body Area
Body area matters, but not as much as the pattern. “Knee pain” is not one thing. Neither is shoulder pain, back pain, hip pain, ankle pain, or foot pain. The joint is the address. The symptoms are the message inside the envelope.
Knee pain: swelling clues matter more than “joint pain” labels
If the knee is swollen, warm, or irritated after activity, cold usually makes more sense first. If it is stiff in the morning and eases after gentle movement, heat before motion may be useful. For older adults, also watch stairs, toilet transfers, and walking distance. Knees love to report through daily logistics, especially when knee osteoarthritis pain management becomes less about one perfect remedy and more about safer daily patterns.
Shoulder pain: cold after irritation, heat for guarded tightness
Cold can help after a shoulder flare from lifting, reaching, or yard work. Heat may help when the shoulder feels guarded, tight, or stiff before gentle range-of-motion work. But severe weakness, sudden loss of motion, or pain after a fall deserves evaluation. If support is part of the conversation, it may also help to understand the practical difference between a shoulder immobilizer and a sling before improvising with whatever is in the closet.
Low back pain: heat may help muscle tension, but sharp radiating pain changes the story
Heat often helps low back muscle tightness. Many people use it before walking or gentle mobility. But pain that shoots down the leg, comes with numbness or weakness, or follows major trauma is not a simple heating-pad moment. That is a different animal, with sharper teeth.
Hip pain: stiffness, bursitis-like irritation, and walking tolerance clues
Hip stiffness that warms up with movement may respond to gentle heat. Lateral hip tenderness after overuse may prefer cold, especially if it feels irritated after walking. Track walking tolerance: can you get across the room, to the mailbox, or through the grocery aisle without paying for it later? If nights are the main battlefield, a separate guide to side sleeper hip pain relief can help connect temperature therapy with sleep position and pressure management.
Ankle or foot pain: swelling usually deserves respect first
For ankle twists, foot flare-ups, or post-activity swelling, cold is often the first home tool. Do not bury a swollen ankle under heat because it “feels cozy.” Cozy is lovely. Cozy is not a clinical strategy.
| Body area | More likely ice wrap | More likely heating pad |
|---|---|---|
| Knee | Swollen, warm, post-activity flare | Morning stiffness, achy tightness |
| Shoulder | After lifting or irritation | Guarded muscles, stiffness |
| Low back | Recent strain with irritation | Muscle tension before movement |
| Ankle or foot | Twist, swelling, tenderness | Chronic stiffness without swelling |
Timing Matters: First 48 Hours, Chronic Pain, and After Activity
The calendar is not everything, but it helps. A pain that started 2 hours ago behaves differently from a pain that has been visiting every morning for 2 years, paying no rent and leaving crumbs.
First day or two after a minor injury: cold usually gets priority
For many minor sprains, strains, bumps, or overuse flares, cold is commonly used early, especially when swelling or warmth is present. Pair it with rest from the aggravating activity and gentle reassessment. If symptoms are severe or function is limited, do not wait it out heroically.
Chronic orthopedic pain: heat before movement, cold after flare-ups
For chronic stiffness, heat before gentle activity can help. For chronic joints that swell after activity, cold afterward may be better. Many people with arthritis-like patterns find the day has two chapters: warmth for the stiff opening scene, cold for the irritated closing credits.
After exercise or chores: match the response, not the calendar
After activity, ask what the body did. If the area feels swollen and hot, cold makes sense. If the area feels tight and guarded without swelling, gentle heat may help later. If activity repeatedly causes flares, the bigger issue may be pacing, footwear, technique, strength, or load.
Tiny test: what changes 30 minutes later?
The best home test is not “Did it feel good while I used it?” It is “What changed afterward?” Track pain, swelling, warmth, range of motion, and one function. For example: “I iced the knee for 15 minutes. Thirty minutes later, stairs were easier.” That is useful data.
Mini calculator: Did the tool actually help?
Neutral next step: If pain drops but walking, sleep, or stairs worsen, treat that as a warning sign.
The Decision Card: Heating Pad or Ice Wrap?
This is the refrigerator-door version. Not fancy. Useful. Slightly bossy in the way good checklists are bossy.
Choose ice wrap when pain is swollen, warm, sharp after injury, or activity-triggered
Cold is often the safer first choice when the area feels irritated. Choose an ice wrap when swelling is visible, the area feels warm, pain began after a twist or bump, or an old joint flares after too much activity.
Choose heating pad when pain is stiff, tight, achy, or improves with movement
Heat often fits when the body feels restricted: stiff back, tight shoulder, achy hip, or morning joint stiffness. Use it before gentle movement rather than as an all-night background appliance.
Consider alternating only when symptoms are mixed and your clinician allows it
Alternating heat and cold can be helpful for some people, but it can also confuse the signal. If you are recovering from surgery, managing a complex condition, or dealing with nerve or circulation issues, ask your clinician before experimenting.
Stop if numbness, burning, skin color change, or worsening pain appears
Skin is not a passive bystander. It gets a vote. Stop if you notice burning, blistering, unusual redness, pale or blue skin, increasing numbness, or pain that worsens after treatment.
Decision card: Ice wrap
- Best for new swelling or warmth
- Often useful after activity flares
- Usually short sessions around 15–20 minutes
- Requires skin barrier and skin checks
Trade-off: Can feel uncomfortable and may stiffen the area temporarily.
Decision card: Heating pad
- Best for stiffness or muscle guarding
- Often useful before gentle movement
- Use awake, with timer and safe setting
- Avoid on fresh swelling unless advised
Trade-off: Can worsen swelling or burn skin if misused.
Neutral action line: Choose the tool based on today’s symptoms, then retest function 30 minutes later.
Who This Is For / Not For
This guide is for ordinary home decision-making, the kind that happens near a freezer drawer, a medicine cabinet, or a couch with one suspiciously permanent body-shaped dent.
For adults managing mild orthopedic aches at home
This is for mild strains, post-activity soreness, arthritis-like stiffness, tight muscles, and small flares that do not involve major trauma or alarming symptoms. It is practical comfort guidance, not a substitute for diagnosis.
For caregivers helping someone compare simple comfort tools
Caregivers often notice patterns the person in pain misses. Maybe Mom says her knee is “fine,” but she stopped using the stairs. Maybe Dad says the heating pad helps, but the skin looks red afterward. Function tells the truth when pride starts wearing cologne. For families comparing supports, seating, wraps, and safer room setups, orthopedic home care equipment should be chosen around the repeated task that hurts most, not around fear-shopping.
Not for unexplained severe pain, major trauma, suspected fracture, or post-surgical uncertainty
Do not use this guide as the main plan for severe pain, inability to bear weight, deformity, sudden weakness, spreading redness, fever, or pain after significant injury. If surgery is involved, follow the surgical team’s instructions rather than improvising with household gear.
Not for replacing a physical therapy or orthopedic care plan
If a physical therapist, orthopedist, primary care clinician, or surgeon gave you specific instructions, those win. Home heat and ice should support the plan, not stage a tiny rebellion in the living room. If your plan feels stalled or confusing, a guide on what to do when physical therapy is not helping orthopedic pain can help you organize symptoms before the next appointment.
- Care plans beat generic advice.
- Post-surgical changes deserve special caution.
- Reduced sensation or circulation changes raise the stakes.
Apply in 60 seconds: If you are helping someone else, ask, “What daily task got easier or harder after using it?”
Common Mistakes That Turn Simple Relief Into a Setback
Most heat-and-ice mistakes are not dramatic. They are small, repeated, and wrapped in good intentions. The villain is rarely laziness. It is usually habit wearing comfortable socks.
Using heat because it feels better while swelling increases
Heat can feel wonderful while making an irritated area more reactive. Watch the after-effect. If swelling, warmth, or throbbing increases later, your body just left a review. It was not five stars.
Icing too long because “numb” feels productive
Numbness can feel like victory, but excessive cold exposure can irritate skin and tissue. Use a timer. Take breaks. Do not keep icing simply because the pain signal has gone quiet.
Putting packs directly on skin
Direct ice can injure skin. Direct heat can burn. A thin towel or cloth barrier is a boring little hero. Invite it.
Treating every joint the same way
A swollen ankle, a stiff back, and a guarded shoulder do not need the same answer. The tool follows the symptom pattern, not the body part alone.
Ignoring function: walking, stairs, sleep, and transfers matter too
Pain scores are useful, but function is the better witness. Can you walk more safely? Sleep better? Climb stairs? Stand from a chair? Shower without bracing like a pirate in a storm? For older adults, broader orthopedic pain management for older adults often starts with exactly those daily-life questions.
Quote-prep list: What to gather before buying a heating pad or ice wrap
- The main body area and whether swelling is present.
- Whether pain is new, chronic, or post-activity.
- Any clinician restrictions, surgery instructions, or skin concerns.
- Needed size: knee, shoulder, back, ankle, or multipurpose.
- Safety features: timer, washable cover, adjustable compression, clear instructions.
Neutral next step: Compare products by safety fit and body-area fit before comparing price.
When to Seek Help Instead of Reaching for Another Pack
There is a moment when another ice session becomes procrastination with a gel filling. There is also a moment when another heat session becomes denial with a power cord. Know the line.
Pain after a fall, pop, deformity, or inability to bear weight
If pain follows a fall, you heard a pop, the limb looks deformed, or you cannot bear weight, get medical care. Do not ask a heating pad to solve what may need imaging, bracing, or a clinician’s hands.
Swelling that rapidly increases or does not improve
Rapid swelling, swelling with severe pain, or swelling that does not improve deserves attention. This is especially true for knees, ankles, and post-surgical areas.
Numbness, weakness, fever, redness, or spreading warmth
Numbness and weakness can suggest nerve involvement. Fever, redness, and spreading warmth can point toward infection or inflammation that needs evaluation. Home packs are not designed for that kind of plot twist.
Pain that disrupts sleep, walking, or normal daily function
If pain repeatedly interrupts sleep, walking, stairs, bathing, dressing, or transfers, it is no longer “just a little ache.” Function loss is a serious signal, especially for older adults living alone. When mobility aids are part of the day, walker pain management for seniors can help families connect relief choices with safer standing, turning, and bathroom routines.
Post-surgery pain that changes suddenly or feels out of pattern
After surgery, follow the surgeon’s instructions on cold, heat, compression, and activity. Sudden changes in pain, swelling, drainage, redness, fever, or calf pain should be handled through the surgical team or urgent medical care. If pain happens during a longer recovery window, especially after knee surgery, a dedicated guide to knee replacement pain management may help you separate expected discomfort from symptoms worth reporting.

FAQ
Is heat or ice better for knee pain?
For knee pain with swelling, warmth, or a recent activity flare, an ice wrap is usually the safer first choice. For knee stiffness that improves after gentle movement, a heating pad before activity may help. If the knee locks, gives way, swells suddenly, or you cannot bear weight, seek medical advice.
Should I use a heating pad or ice wrap for arthritis pain?
Many people with arthritis-like stiffness use heat before movement and cold after swelling or flare-ups. The key is matching the tool to the symptom. Stiff and tight often points toward heat. Swollen and warm often points toward cold.
Can I alternate heat and ice for orthopedic pain?
Sometimes, but do not treat alternating as automatically safer. If symptoms are mixed, alternating may help some people. If you recently had surgery, have reduced sensation, circulation problems, or worsening symptoms, ask a clinician before experimenting.
How long should I use an ice wrap?
A common home range is about 15 to 20 minutes with a cloth barrier, followed by a break and skin check. Stop sooner if your skin hurts, changes color, becomes unusually numb, or the cold feels intolerable.
How long should I use a heating pad?
Use heat in limited awake sessions, often around 15 to 20 minutes for simple stiffness or tightness. Use a timer, safe setting, and skin checks. Do not sleep on a heating pad.
Is heat bad for swelling?
Heat can worsen fresh swelling or irritation in some cases. If the area is newly swollen, warm, throbbing, or painful after injury, cold is often the better first home option.
Can ice make pain worse?
Yes. Ice can feel too intense, increase stiffness temporarily, or irritate skin if used too long or directly on skin. Use a barrier, limit time, and stop if symptoms worsen.
What should older adults be careful about with heat and ice?
Older adults should be especially careful with skin checks, sensation changes, circulation issues, timers, and safe setup. Caregivers should watch function after use: walking, bathroom transfers, sleep, stairs, and steadiness. For broader safety planning, senior orthopedic pain management should treat comfort tools as one part of a safer daily routine, not the whole orchestra.
Next Step: Run the 3-Signal Pain Check Before You Choose
Here is the loop we opened at the beginning: the safer choice is not the tool that feels nicer in the first 2 minutes. It is the tool that matches the pain signal and leaves function better afterward.
Signal 1: Is the area swollen, warm, or newly injured?
If yes, cold usually gets first consideration. Use a barrier, keep the session short, and reassess. If symptoms are severe, traumatic, or worsening, skip the home experiment and get help.
Signal 2: Is the pain stiff, tight, or better after gentle movement?
If yes, heat may be reasonable before movement, especially for chronic tightness or morning stiffness. Stay awake, set a timer, and check the skin.
Signal 3: Did function improve or worsen after the last session?
This is the signal people forget. Pain relief that does not improve function is incomplete data. Track one practical task: stairs, walking, standing from a chair, reaching overhead, sleeping, or showering.
One concrete action: write down “tool used, minutes, symptom before, symptom after, function after”
Use this tiny log for 3 sessions:
- Tool used: heating pad or ice wrap
- Minutes: how long you used it
- Symptom before: swollen, stiff, warm, tight, sharp, achy
- Symptom after: better, worse, same, or different
- Function after: what daily task changed
If the pattern is clear, you have a safer home routine. If the pattern is confusing, worsening, or tied to function loss, bring the log to a clinician. That little note can save a lot of fog.
- Cold usually fits swelling and fresh irritation.
- Heat usually fits stiffness and guarded muscles.
- Function decides whether the tool truly helped.
Apply in 60 seconds: Choose one function to track today: stairs, walking, sleep, reaching, or standing from a chair.
Conclusion: Heating pads and ice wraps are not rivals. They are different keys for different locks. Use ice when pain is newly angry, swollen, warm, or activity-triggered. Use heat when pain is stiff, tight, chronic, or easier after gentle movement. Protect your skin, keep sessions short, and let function be the judge.
Your next step within 15 minutes: run the 3-signal pain check, choose one tool, set a timer, and write one honest line afterward. Not a diary. Not a novel. Just enough evidence to keep tomorrow’s you from guessing in the freezer light.
Last reviewed: 2026-05.
