
Practicing Without the Payback: A Safer Path for Yoga & Sciatica
The flare often doesn’t happen in class—it shows up later, in the car seat, at dinner, or the next morning when putting on socks suddenly feels like a negotiation. That’s the trap with sciatica after yoga: the pose can feel fine in the moment, then quietly overdraw your nervous system by nightfall.
For busy adults, the real pain isn’t just leg symptoms—it’s losing trust in movement. You keep showing up, but forward folds, seated stretches, and “go deeper” cues leave you guessing about what’s helping versus what’s provoking nerve irritation. Keep guessing, and you risk the same cycle: one “good” class followed by 24–48 hours of setback.
This guide gives you a safer, usable path:
- • Forward fold substitutions you can use in normal classes.
- • Symptom triage that actually guides decisions.
- • A 7-day reset built around dose control—not fear.
“Think wall hip hinge, chair-supported half fold, and clear stop rules for tingling, numbness, or weakness.”
It’s a practical system grounded in movement quality and 24-hour response tracking, not flexibility bravado. Small cue edits, big symptom differences. And yes—you can keep yoga in your life without paying for it tomorrow.
Fast Answer
If forward folds trigger sciatic symptoms, pause deep spinal flexion and switch to supported hip-hinge patterns: wall hip hinge, chair-assisted half fold, and supine strap work. Keep your spine long, soften your knees, and stop at mild stretch with zero nerve zing. If pain shoots, tingles, numbs, weakens, or lingers past 24 hours, reduce range and seek a licensed clinician (PT, sports medicine, or spine specialist) for individualized guidance.
Table of Contents
1) Why Forward Folds Flare Sciatica (and Why It’s Not Just “Tight Hamstrings”)
Sciatica vs hamstring tension: how to tell the difference quickly
Hamstring stretch usually feels local and dull, like a firm pull behind the thigh. Nerve irritation often feels sharper, stranger, or farther away: zings, burn, pins-and-needles, or a pull that travels below the knee. A muscle says, “I’m short.” A nerve says, “I’m irritated.” Different signal, different strategy. If you want a deeper breakdown of this distinction, compare hamstring stretch vs nerve pain patterns.
One clue I see a lot: people say, “I felt okay in class, then worse in the car afterward.” That delayed rebound often means load tolerance was exceeded, not that you “did yoga wrong.” You simply crossed your current threshold.
The flexion + nerve sensitivity combo that sneaks up mid-class
Forward folds stack two variables at once: spinal flexion and posterior chain tension. On calm days, fine. On flare-prone days, that combo can be too spicy, especially if you add locked knees, long holds, and breath-holding. Think of symptoms like a volume knob. Your goal is not silence in one minute; your goal is keeping the knob from jumping from 2 to 7.
Let’s be honest… “go deeper” cues can be wrong for your body today
Group cues are broad by design. Bodies are not. If a cue pushes you toward numbness or electric pain, that cue is not “motivational,” it’s mismatched dosage. Your best class skill is not depth—it’s calibration.
- Local pull = often muscle
- Electric or traveling pain = likely nerve irritation
- Next-day flare = yesterday’s range/load was too high
Apply in 60 seconds: Before class, commit to “long spine + soft knees + stop at first nerve signal.”
Show me the nerdy details
Nerve tissue is mechanically sensitive and dislikes abrupt end-range loading when irritable. Reducing spinal flexion angle, lowering hold time, and avoiding breath bracing can reduce symptom provocation while preserving movement confidence.
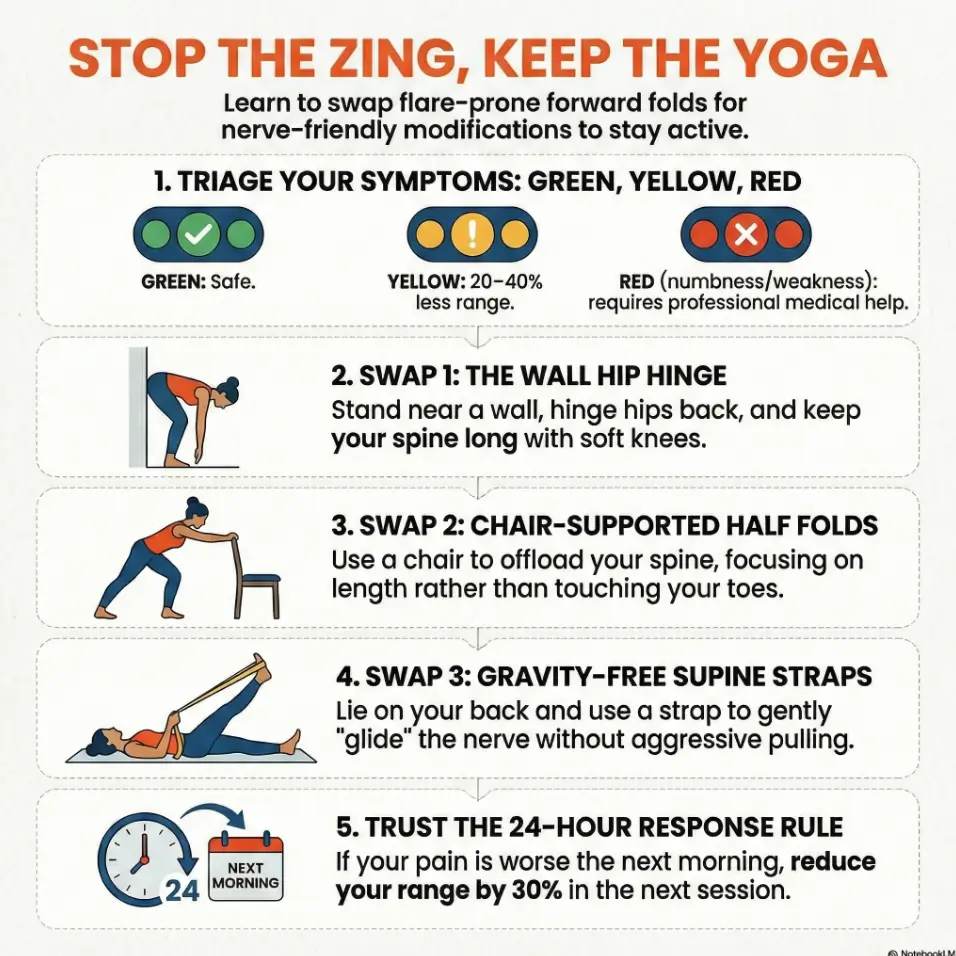
2) Symptom Check First: Green, Yellow, Red Before You Modify
Green-light signs: safe to experiment today
- Pain is mild (for example, 0–3/10) and not spreading.
- No progressive weakness, no numbness pattern changes.
- Symptoms settle within a few hours after activity.
- You can walk, sit, and sleep without significant worsening.
Yellow flags: proceed only with reduced range and props
- Pain rises during class but settles by next morning.
- Tingling appears only at deeper range.
- One position helps briefly, but rebound appears later.
Yellow means “modify, don’t quit.” Lower range by 20–40%, shorten holds to 10–20 seconds, and test one substitution at a time.
Red flags: stop class and switch to recovery mode
- New or progressive leg weakness
- Numbness that expands or persists
- Bowel/bladder changes, saddle-area numbness, severe trauma-related pain
- Pain that rapidly escalates and does not calm
Red flags are not a grit test. They are a referral signal. If any of these appear, use a clear low-back pain emergency checklist and seek urgent care as indicated.
Money Block: Eligibility Checklist (Can I self-modify today?)
Yes/No checklist:
- No red flags today? Yes/No
- Symptoms stay mild and non-progressive? Yes/No
- You can stop immediately when symptoms rise? Yes/No
If you answered “No” to any item, skip fold loading today and get professional guidance.
Neutral next step: Choose a conservative session and log your 24-hour response.

3) Swap #1: Wall Hip Hinge (Your New Forward Fold Baseline)
Setup in 30 seconds: feet, pelvis, ribs, breath
Stand about one foot from a wall facing away from it. Feet hip-width. Slight bend in knees. Gently send hips backward until they touch the wall while your torso tips forward. Keep ribs softly stacked over pelvis and neck long. Exhale slowly for 4–6 seconds on the way into the hinge.
My first week with this, I felt silly—like I was doing “beginner version forever.” Then I noticed something beautiful: no post-class ambush. That single outcome beats ego every time.
Range rule: stop before nerve symptoms, not after
Your stopping point is the first whisper of nerve tension, not the point where you “can handle it.” If symptoms appear, come up 10–15% and breathe. Stay there. Own that range for 2–3 sessions before progressing.
Progression ladder: fingertips → blocks → deeper hinge
- Step 1: Hands on thighs, small hinge.
- Step 2: Fingertips on a chair seat.
- Step 3: Fingertips to yoga blocks (high setting).
- Step 4: Slightly deeper hinge only if 24-hour rebound is calm.
In many U.S. clinics, PTs cue this as “hip load, spine calm.” It’s not glamorous; it’s reliable. You can pair this with a short dead bug core-control sequence for sciatica on non-class days.
- Soft knees are protective, not lazy
- Range is earned, not forced
- 24-hour response decides progression
Apply in 60 seconds: Do 5 slow wall hinges now, exhaling on each descent.
4) Swap #2: Chair-Supported Half Fold for Low-Irritation Length
How to offload the spine while still training posterior chain
Place both hands on a sturdy chair or countertop. Step back until arms are long and torso is angled, like an upside-down L. Knees softly bent. Hips back. This creates posterior chain loading with far less “collapse into spine” than a deep unsupported fold.
Knee bend, shin angle, and torso line that reduce flare risk
Use a small knee bend—think 10–20 degrees. Keep shins mostly vertical. Let torso lengthen forward while pelvis shifts back. If your lower back rounds or your breath stalls, you’re too deep. Come up one notch.
Here’s what no one tells you… support isn’t “cheating,” it’s dosage control
Support tools are not beginner badges; they’re precision instruments. A chair can save you two bad days of rebound pain. And yes, that matters more than touching your toes in public.
In class, translate “fold deeper” into “lengthen longer.” Different verb, safer outcome.
Show me the nerdy details
External support increases stability and lowers the demand for spinal end-range control. That frequently reduces protective muscle guarding and allows better breathing, which can reduce perceived threat and pain amplification.
Money Block: Decision Card (When A vs B)
When to use Wall Hinge: symptom-prone day, class is fast, you need simple guardrails.
When to use Chair Half Fold: you want longer holds, better balance, lower threat.
Time/cost trade-off: Wall hinge is faster (about 30 seconds setup); chair fold gives more control but needs equipment.
Neutral next step: Pick one substitution per class and stick with it for 7 days.
5) Swap #3: Supine Strap Series (No Gravity, More Control)
Supine hamstring glide vs aggressive stretch
Lie on your back. Loop a strap around one foot. Knee starts bent. Gently raise leg until mild stretch—no pulling contest. Hold 5–10 seconds, lower slightly, repeat 4–6 times. Think “glide,” not “grind.” If classic nerve glides have worsened your symptoms before, review why sciatic nerve flossing can backfire and keep the dosage gentler.
Bent-knee option when straight-leg raises provoke symptoms
If straightening the knee lights things up, keep 20–40 degrees bend and work within that range. A bent-knee version often gives better tolerance while preserving confidence and motion.
60-second protocol you can do post-class
- 20 seconds diaphragmatic breathing (hands on lower ribs)
- 20 seconds gentle strap-assisted raise (left)
- 20 seconds gentle strap-assisted raise (right)
Done. No drama. This is your “I still moved, and I didn’t flare” exit ramp.
- Bent knee is a valid progression step
- Short holds beat long battles
- Post-class calm-down helps tomorrow’s tolerance
Apply in 60 seconds: Do one round after your next class before leaving the mat.
6) Don’t Do This: Common Form Errors That Turn Stretch into Flare
Rounding to “find depth” instead of hinging from hips
Depth by spinal collapse is a short-term win with a long-term invoice. If your lower back domes and hamstrings scream, reduce range and rebuild hinge mechanics first.
Locking knees and yanking on range
Locked knees increase tension demand rapidly. Micro-bend buys control. A 5% bend can change the whole response curve.
Holding end range too long when nerve tissue is irritable
Long static holds at end range are often the hidden trigger. Try shorter exposures (10–20 seconds), more reps, less intensity.
Breath-holding (the hidden tension multiplier)
If you catch yourself bracing your face and jaw, you’re already over threshold. Exhale longer than inhale. Your nervous system listens.
I once tried to “win” a pose at minute 52 of class. I won the pose and lost the next 36 hours. That trade is overrated.
Money Block: Quote-Prep List (Before comparing clinicians/programs)
- Your trigger list (which poses, what depth, what timing)
- 24-hour rebound notes from 3 recent sessions
- What helped: wall hinge, chair fold, supine strap, walking, heat
- Your top goal: pain-free class, better sleep, longer walking tolerance
Neutral next step: Bring this list to a PT or sports medicine appointment for targeted advice.
7) Cue Translation Guide: What Yoga Cues to Ignore, Edit, or Keep
“Straight legs” → “soft knees + long spine”
You’re not breaking rules—you’re translating them for your body. Soft knees reduce threat and increase control. It’s a strategic edit.
“Head to shins” → “torso to thighs, then pause”
Proximity cues can create compression pressure. Replace with length cues. Your goal is cleaner patterning, not Instagram geometry.
“Feel the burn” → “no zing, no numbness, no aftershock”
For sciatica-prone practitioners, the best cue is symptom quality, not heroic sensation. If it zings, it’s a redirection cue.
Studio script you can use: “I’m modifying forward folds for nerve sensitivity today; I’ll keep neutral spine and supported range.” Short, calm, done.
Show me the nerdy details
Language shapes motor output. Threat-heavy cues can increase guarding; control-oriented cues improve tolerability. In practice, cue edits that prioritize breath, hinge mechanics, and symptom limits are often enough to maintain participation without flare escalation.
8) Who This Is For / Not For
Best for: mild-to-moderate flare-prone practitioners who want to stay active
This approach fits people who can move but flare after certain ranges, especially after deep folds, long holds, or fast transitions.
Not for: new severe pain, progressive weakness, bowel/bladder changes, trauma
If your pattern is rapidly worsening or neurologically concerning, this is not a self-experiment day. That’s a medical evaluation day.
If you’re postpartum/older athlete/desk worker: how to personalize substitutions
- Postpartum: prioritize breath and load management over maximal range.
- Older athlete: reduce hold duration first, then increase range gradually.
- Desk worker: add short walking breaks and avoid long post-class sitting spikes. A structured sit-stand schedule for desk-job sciatica can help prevent rebound irritation.
Real talk: you do not need a new identity as “injured person.” You need a better loading algorithm.
- Match the plan to your symptom pattern
- Use support to preserve consistency
- Escalate quickly when red flags appear
Apply in 60 seconds: Decide your category now: green, yellow, or red.
9) Mistakes Most People Make in Week 1 (and How to Avoid Setbacks)
Doing “good pain” math: more stretch ≠ better outcome
The most common myth is linear: if a little helps, a lot helps more. Nerves frequently disagree. Better rule: better tomorrow beats deeper today.
Testing too many substitutions in one session
If you change six variables at once, you learn nothing. Pick one primary substitution, one backup, and keep the rest stable for 3–4 sessions.
Ignoring the 24-hour symptom response window
Your body votes tomorrow. Rate symptoms right after class, before bed, and next morning. If morning is clearly worse, cut next session dose by 20–30%.
Mini log template: Range used, symptom peak (0–10), next-morning status, decision for next class. If mornings are consistently rough, compare with your routine on morning sciatica nerve glides and simplify.
Money Block: Mini Calculator (Dose Adjustment)
Inputs (3): Today’s peak symptom score, next-morning change, session duration.
Output rule:
- If next morning is worse by 2+ points → reduce next session range/time by 30%
- If stable or better → keep dose or progress by 10%
Neutral next step: Apply this rule for one week before making bigger changes.
10) When to Seek Help (PT, Sports Med, or Spine Specialist)
Pain pattern checklist worth bringing to your appointment
- Where symptoms start and where they travel
- What triggers onset (pose, depth, duration, transition)
- What settles symptoms and how long it takes
- Any weakness, numbness, night pain, or gait changes
What to ask in a US clinic visit for targeted movement advice
Ask for a movement-specific plan, not just a diagnosis label. Useful questions: “Which ranges should I limit for 2 weeks?” “What progression milestones should I track?” “What is my stop rule?” “How do I return to folds safely?” A good starting point is understanding how physical therapy for sciatica is usually structured.
Imaging myths: when scans help—and when they don’t change care
Imaging can be useful in select contexts, but many flare-management decisions are based on clinical signs and response to load. Ask whether scan results would change treatment decisions right now.
Trusted U.S. references many clinicians use in patient education include NINDS, AAOS, and major academic centers like Cleveland Clinic for plain-language guidance.
Short Story: The class I almost quit (120–180 words)
I remember one Thursday class where the room smelled faintly of mat spray and eucalyptus, and everyone around me was folding like pocketknives. I was two breaths from copying them out of pride. Instead, I used a chair, bent my knees, and stayed high. For five minutes I felt like the only person doing “less.” Then something unusual happened:
I finished class without that familiar electric aftertaste in my leg. I drove home without bargaining with the seat heater. The next morning, I could put on socks without the little grimace I had normalized for months. That day taught me a quiet lesson: modification is not retreat. It is intelligent participation. The pose stopped being a test of identity and became a test of signal quality. Once I made that switch, yoga felt like practice again, not roulette.
11) Next Step: Your 7-Day “No-Flare Fold Reset”
One concrete action
For the next 7 days, replace every forward fold with Wall Hinge + Chair Half Fold. If symptoms rise, finish with Supine Strap Series.
Track two metrics only
- Symptom intensity peak (0–10)
- 24-hour rebound (better / same / worse)
Keep, scale, or stop: day 8 decision rule
- Keep: symptoms stable or improving
- Scale up: increase depth or hold by ~10% only if 24-hour rebound is calm
- Stop + refer: progressive neurological signs or persistent worsening
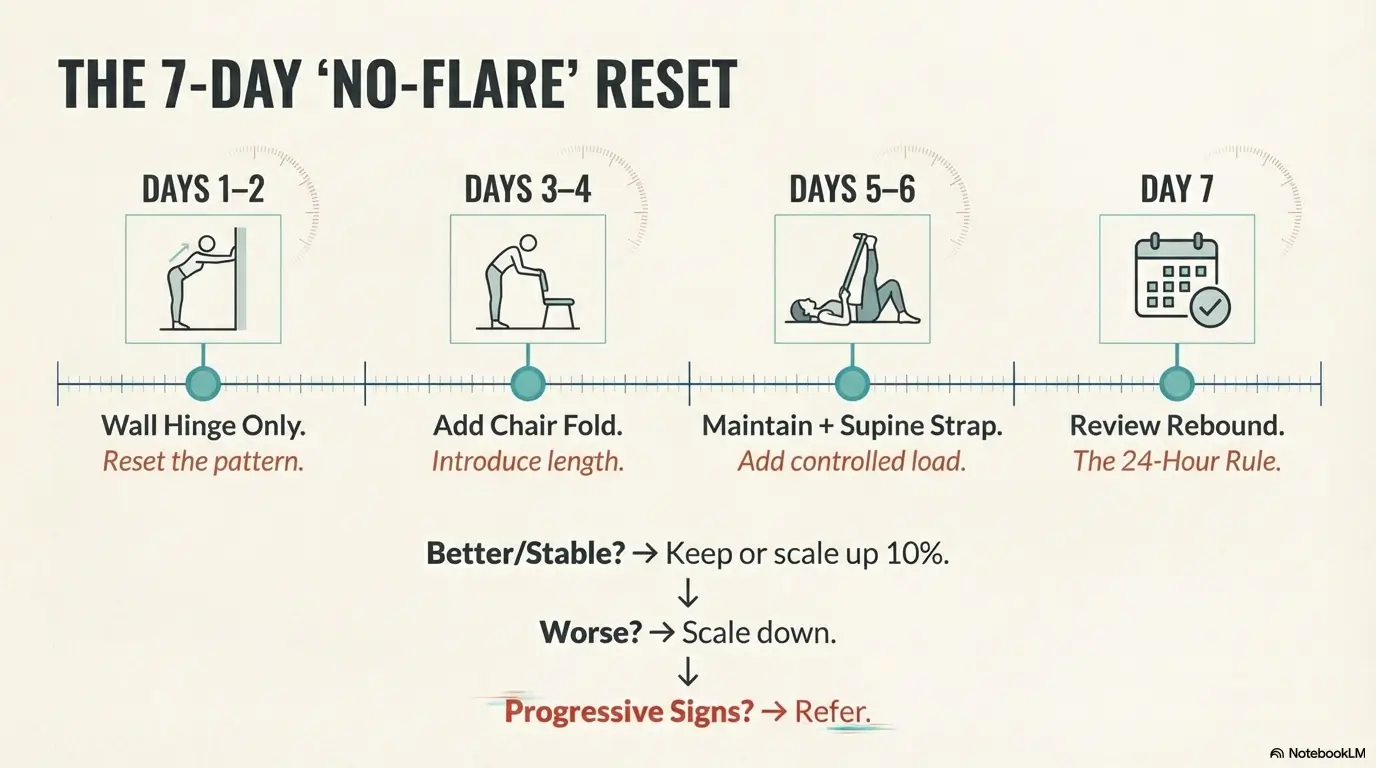
Infographic: 7-Day No-Flare Workflow
Day 1–2
Use Wall Hinge only.
Soft knees, short range.
Day 3–4
Add Chair Half Fold.
No end-range holds.
Day 5–6
Maintain if stable.
Add Supine Strap cooldown.
Day 7–8
Review 24-hour rebound.
Keep / scale 10% / refer.
FAQ
Can I still do yoga if forward folds trigger sciatica?
Yes, in many cases. You can stay active by swapping provocative folds for supported hinge patterns and keeping symptoms below your flare threshold. If symptoms escalate or neurological signs appear, pause and seek care.
Is it better to bend knees in Uttanasana with sciatic pain?
Usually yes. Soft knees often reduce posterior chain tension and make it easier to maintain a longer spine. Think control over depth.
Are seated forward folds worse than standing folds for sciatica?
Not always, but seated folds can still provoke symptoms if you collapse into spinal flexion or force end-range. Support, range, and timing matter more than pose category alone.
What’s the safest hamstring stretch when nerve pain is present?
Supine strap-assisted work is often better tolerated because it removes some gravity and lets you fine-tune range. Keep intensity low and stop at first nerve signal.
How long should I hold a modified fold without flaring?
Start with shorter holds (about 10–20 seconds), repeat 3–6 rounds, and watch the 24-hour response. Progress duration only if next-day symptoms stay calm.
Should I avoid all spinal flexion during a flare-up?
Not necessarily all flexion forever, but deep and prolonged flexion may be poorly tolerated during irritable phases. Use temporary range reduction and graded return.
Can props (blocks/chair/strap) really reduce sciatic irritation?
Yes, props can reduce load, improve control, and make breathing easier. They are not shortcuts; they are precision tools for symptom-guided practice.
Why does pain appear later, not during class?
Because tissues and the nervous system can react after cumulative load, not only in the moment. That’s why your next-morning check is essential. If late flares also show up during errands, compare your load with guides on sciatica while standing in line and safe grocery bag weight limits for sciatica.
When should I stop yoga and see a physical therapist?
If symptoms are progressive, recurrent despite good modifications, or accompanied by weakness/numbness changes, book a PT or sports medicine visit for individualized movement planning.
Are nerve glides safe to do at home?
Often, when done gently and within symptom limits. If they trigger lingering symptoms, reduce dose or stop and get clinician guidance on technique and timing.
Conclusion
Here’s the loop we opened at the start: the problem usually isn’t yoga itself—it’s the dose, timing, and cue translation. Once you stop treating forward folds as a depth contest, the whole practice gets kinder and more sustainable. In the next 15 minutes, do one thing: set your next class plan to Wall Hinge + Chair Half Fold, then track your 24-hour rebound. If tomorrow is calmer, you’re on the right path. If not, scale down or escalate care. Calm, specific, repeatable—that’s how you stay active without flare roulette.
If you want a complementary low-load conditioning option on non-yoga days, see recumbent bike setup for sciatica and decide between recumbent vs upright bike for sciatica based on your current tolerance.
Last reviewed: 2026-02.
Educational content only; not medical diagnosis or treatment. If symptoms are severe, worsening, or neurologically concerning, seek licensed medical care promptly.
