
Stop the “Co-pay Cycle”: Finding the Right Path to Relief
Choosing between a pain clinic and an orthopedist sounds simple until pain turns scheduling into a money leak. One wrong first appointment can cost a co-pay, a week of delay, and the special fatigue of repeating your story to yet another office that cannot answer the question you actually came to solve.
The real problem isn’t just the pain—it’s the drain of uncertainty. Is this a structural issue needing orthopedic imaging and rehab, or chronic pain requiring steady symptom control and a smarter long-term plan?
This guide helps you sort the decision faster and with less waste. You will learn when musculoskeletal pain points toward an orthopedist, when pain management makes more sense, and when red-flag symptoms change the whole script.
Because the best first visit isn’t the one with the most impressive title—it’s the one that answers the right question.
Fast Answer: If your main question is “What is causing this pain, and do I need imaging, rehab, or surgery?” start with an orthopedist. If your main question is “How do I function better while living with pain that is already diagnosed or ongoing?” a pain clinic may fit better. The smartest first visit usually depends on whether you need structural evaluation or symptom control.
Table of Contents

Start Here First: What Problem Are You Actually Trying to Solve?
Choose an orthopedist when the question is structural
An orthopedist usually makes the most sense when your pain seems tied to something physical and specific. A twist. A fall. A knee that catches. A shoulder that suddenly refuses overhead motion. A back that started barking after lifting a suitcase like it personally insulted you. In these cases, the core question is often structural: what is hurt, inflamed, torn, compressed, unstable, or degenerating?
Choose a pain clinic when the question is ongoing pain control
A pain clinic can be a better first stop when the pain has already been evaluated, has dragged on for months, or keeps flaring even after the obvious first-line steps. Here the question is less “what is it?” and more “how do I live, move, sleep, and work better while this is going on?” That is a different job. Not smaller. Not second-rate. Just different.
The hidden fork in the road is diagnosis vs. management
This is the fork patients miss. They book by title, not by task. It is understandable. When you hurt, every specialist name starts to shimmer like a lighthouse. But the cleanest way to choose is to ask what the first appointment needs to decide. If it needs to decide whether you have a structural musculoskeletal problem that changes imaging, bracing, therapy, or surgery, the orthopedist is usually the sharper tool. If it needs to reduce pain burden, improve function, and build a longer plan around already-known or chronic pain, pain management may be the better fit.
- Diagnosis-heavy question: think orthopedist
- Function-heavy question: think pain clinic
- Unclear goal: write the question down before booking
Apply in 60 seconds: Finish this sentence before you schedule: “By the end of this appointment, I need to know whether…”
Pain Clinic vs Orthopedist: Same Pain, Different Job Description
What an orthopedist is usually looking for
The American Academy of Orthopaedic Surgeons describes orthopaedists as physicians focused on the prevention, diagnosis, and treatment of disorders of bones, joints, ligaments, tendons, and muscles. In plain English, they are trained to sort out whether your pain maps to a musculoskeletal problem and what path fits that problem best. Sometimes that means imaging. Sometimes a brace. Sometimes physical therapy. Sometimes watchful waiting. Sometimes surgery, though not nearly as often as worried patients imagine in the parking lot.
What a pain clinic is usually trying to improve
Pain clinics, by contrast, are generally built around pain reduction, function, and quality of life. That may include medication strategy, non-drug treatments, procedural options, flare management, and a plan for living more capably with persistent pain. MedlinePlus notes that pain treatment may involve medicines, physical therapy, exercise, and other non-drug approaches, which is exactly why pain management often feels broader and less anatomy-obsessed than an orthopedic visit.
Why these visits can feel similar at first, but lead in different directions
At the first appointment, both may ask where it hurts, how long it has hurt, what makes it worse, and what you have already tried. That overlap fools people. The difference shows up in what happens next. The orthopedist is usually trying to identify or rule out a structural driver. The pain clinic is usually trying to build a workable management ladder. Same opening scene. Different script by act two.
I once watched a friend schedule three visits in two weeks because every office sounded right on paper. She did not need three opinions. She needed one cleaner question. That tiny shift would have saved her two co-pays and one spectacularly useless waiting room afternoon.
Show me the nerdy details
In clinical reality, there is overlap. Some orthopedists emphasize conservative care before surgery. Some pain specialists evaluate diagnosis history carefully before offering management options. But their center of gravity is usually different: anatomy and structural decision-making on one side, symptom control and function on the other.
Decision Card: When A vs B
| If your priority is… | Usually start here | Time/cost logic |
|---|---|---|
| Finding the structure causing the pain | Orthopedist | May reduce repeat referrals |
| Managing persistent pain day to day | Pain clinic | May reduce trial-and-error drift |
| Pain after failed first-line treatment but unclear diagnosis | Usually orthopedist first | Clarify structure before procedures |
Neutral next step: Match the booking to the decision you need made first.
Red Flags First: When You Should Not “Wait and See”
Sudden weakness, numbness, or loss of function
Some symptoms move you out of the blog-and-calendar zone and into urgent evaluation territory. Sudden weakness, foot drop, new loss of grip strength, numbness that is spreading, or loss of bladder or bowel control need prompt medical attention. This is not the season for leisurely comparison shopping.
Fever, trauma, swelling, or symptoms that are escalating fast
Fever with joint pain, major swelling, inability to bear weight, major trauma, or rapidly escalating pain can point to problems that should not marinate in your notes app for five days. Infection, fracture, dislocation, or acute neurologic issues deserve faster escalation than a routine specialist visit.
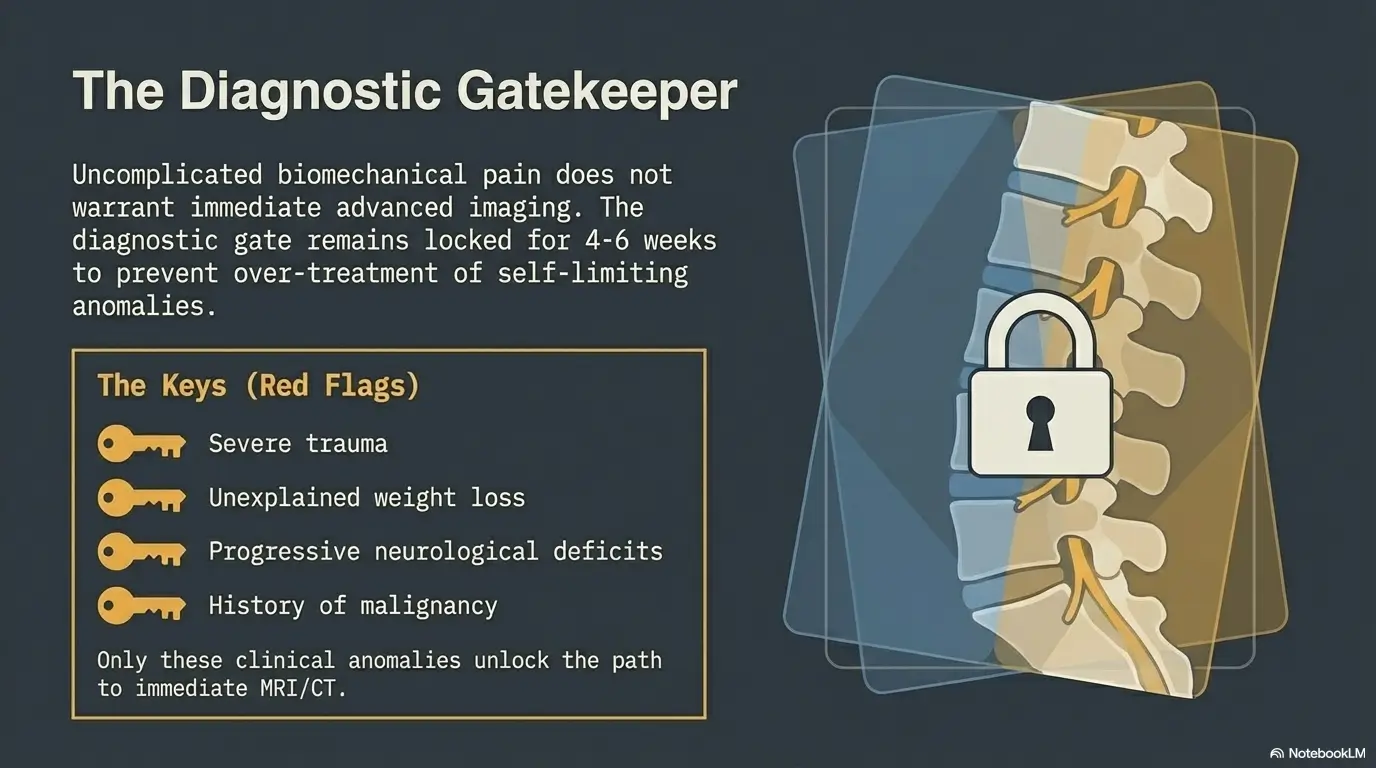
Pain that feels mechanical is not always harmless
People love to self-soothe with labels like “just a strain.” Sometimes they are right. Sometimes that sentence ages badly by Thursday. The American College of Radiology’s appropriateness guidance for low back pain makes a similar distinction between uncomplicated cases and cases with red flags or specific risk patterns. Translation: not every painful back or joint needs imaging first, but some symptom patterns absolutely change the script. If your symptoms are moving into true warning-sign territory, it helps to review what counts as a low back pain emergency rather than treating every flare like routine inconvenience.
- Rapid worsening changes urgency
- Fever, trauma, or major weakness raise the stakes
- Loss of function is a louder signal than pain score alone
Apply in 60 seconds: If symptoms are severe, new, or escalating fast, stop comparing specialists and seek urgent medical evaluation.
Pick the Right Door: When an Orthopedist Makes More Sense
Joint injuries, sports injuries, and pain after a clear movement or accident
If the pain began after a specific event, an orthopedist often makes sense first. Knees that twist and swell. Shoulders that pop after reaching or lifting. Ankles that balloon after a misstep. Hips that suddenly hurt with rotation. Orthopedists live in this neighborhood. They are used to deciding whether the problem sounds like tendon, ligament, cartilage, bone, joint irritation, or something referred from nearby structures.
Pain that may need imaging, bracing, physical therapy, or surgical evaluation
Importantly, choosing an orthopedist does not mean you are volunteering for surgery like it is an awkward raffle prize. It often means you are choosing a clinician whose daily work includes deciding when imaging matters, when it does not, and which nonoperative next steps fit best. Good orthopedic care is frequently conservative first, especially for common musculoskeletal complaints. If you are stuck specifically on whether the next step should be imaging, it may help to read more about when an MRI referral for orthopedic pain actually makes sense.
When you need someone to rule in or rule out a structural problem
This matters more than patients realize. A clean “we do not think this is a major structural issue” can save money. So can a clean “this pattern does need more focused evaluation.” The value of the visit is not only in what gets found. It is often in what gets ruled out before you spend six weeks bouncing between vague plans.
A few years ago I ignored a stubborn shoulder issue because I could still type, which is the sort of logic people invent when they want denial to wear a lab coat. What finally helped was not heroism. It was getting clear on whether the problem was mechanical enough to need structural assessment. That question changed everything.
Eligibility Checklist: Orthopedist first?
- Yes if pain followed an injury, twist, fall, lift, or sport movement
- Yes if the joint feels unstable, catches, locks, or swells
- Yes if you need to know whether imaging or rehab is the next step
- No if the problem is already diagnosed and the main issue is chronic pain control
Neutral next step: If you checked 2 or more “yes” items, an orthopedic evaluation is usually worth considering first.
Manage the Fire: When a Pain Clinic May Be the Better Fit
Long-lasting pain that keeps returning despite basic treatment
Pain clinics often become more useful when pain has overstayed its welcome. You tried time. You tried rest. Maybe physical therapy. Maybe simple medication. Maybe activity modification. Yet the pain keeps boomeranging back like it pays rent. At that point, management becomes a legitimate primary goal, not a consolation prize.
Nerve pain, spine pain, or pain already tied to a known diagnosis
For some people, the diagnosis is not the missing piece anymore. The missing piece is what to do next with it. A person may already know they have chronic spine pain, post-surgical pain, degenerative joint disease, or nerve-related pain. They may need a clinic that thinks in layers: symptom patterns, flares, function, sleep, side effects, exercise tolerance, and realistic goals. When the issue sounds more nerve-driven than purely mechanical, reading about how sciatica-style nerve pain behaves can also help you describe symptoms more clearly before that first visit.
When the goal is function, flare control, and day-to-day livability
This is where pain management can shine. The work is not always glamorous. It often looks like steady, uncinematic improvement: better walking tolerance, fewer bad nights, less panic during flares, fewer missed workdays, or enough symptom control to return to rehab more consistently. Not dramatic. Very valuable.
There is a dignity to this kind of care that people sometimes underrate. They imagine diagnosis as noble and management as boring. But when pain has colonized your schedule, boring becomes beautiful. Boring means you cooked dinner. Boring means you sat through a meeting. Boring means your life stopped shrinking.
Show me the nerdy details
“Pain clinic” is not one uniform model. Some clinics emphasize multidisciplinary care. Some emphasize procedural care. Some are medication-light. Some are procedure-forward. The useful question is not just “Do they treat pain?” but “How do they structure treatment and what problem are they best set up to solve?”
Do Not Start Backward: The Costly Mistake of Choosing by Procedure Alone
Injections are not a diagnosis
People in pain understandably get seduced by nouns. MRI. Injection. Ablation. Surgery consult. These words feel concrete. They promise movement. But choosing your first specialist based on the procedure you think you want can send the visit sideways. A procedure may be useful. It is just not a diagnosis wearing better shoes. If you are already leaning toward an injection because it sounds decisive, it may be worth pausing with a guide on what pain management should look like before a cortisone injection.
Surgery consults are not always the first smart step
A surgical consult can be appropriate when a structural problem is reasonably suspected. It can also be premature when the actual need is a careful exam, a conservative plan, or a different type of diagnosis entirely. The same is true in reverse. Jumping straight to pain procedures without a clean structural workup can create a strange kind of progress theater: lots happening, not enough being clarified.
Chasing the fastest appointment can create a slower recovery
I understand the temptation to take whichever office can see you first. Pain scrambles patience. But the fastest appointment is only efficient if it answers the right question. Otherwise you collect a receipt, a portal login, and a polite referral to somewhere else. That is not momentum. That is administrative cardio.
- Injections can help, but they do not replace diagnosis
- Imaging can clarify, but it should answer a real clinical question
- The fastest booking is not always the fastest path
Apply in 60 seconds: Replace “I need an MRI” with “What decision would imaging change?”
Mini Calculator: Is the wrong first visit costing you more than you think?
Estimate: first co-pay + time off work cost + travel/parking. Then multiply by the number of likely repeat referrals if the visit cannot answer your main question.
Neutral next step: Even a rough estimate can make “book the right specialty first” feel less abstract.
Who This Is For, and Who It Is Not For
This is for adults deciding where to book first for bone, joint, spine, or nerve-related pain
This guide is for adults trying to choose an efficient first stop for musculoskeletal or pain-related symptoms. It is especially useful when the pain is annoying enough to deserve action but not so explosive that you already know you need emergency care.
This is for people trying to avoid unnecessary visits, imaging, and repeat referrals
It is also for the practical reader who does not want healthcare as a hobby. Some people have generous insurance and still hate wasted time. Others are staring at high deductibles, referral rules, or specialist scarcity. Either way, cleaner sequencing matters. If cost pressure is quietly shaping your choices, the math can look very different under orthopedic pain management with a high-deductible plan.
This is not for emergencies or severe new symptoms that need urgent medical care
It is not for emergencies, rapidly worsening neurologic symptoms, serious trauma, suspected infection, or inability to bear weight after an acute event. Those situations deserve prompt medical evaluation rather than leisurely optimization.
There is a special irritation that comes from being sick enough to need help and well enough to have options. This guide lives in that middle zone. Not the ambulance zone. Not the shrug-it-off zone. The gray hallway in between.
Let’s Be Honest: What Patients Often Want Is Certainty, Not Just Treatment
Why “I just need an MRI” can send the visit sideways
What patients often want is not imaging itself. It is certainty. They want the machine to name the villain. That is human. Pain is unnerving partly because it turns your own body into a vague narrator. But the desire for certainty can lead people to overvalue tests that do not necessarily change treatment.
Why a label can feel comforting, even when it does not change treatment
A label can reduce anxiety. It can also create false closure. Some findings are meaningful. Some are incidental. Some explain symptoms beautifully. Some merely decorate the chart. The relief of “finally knowing” is real, but the more practical question is whether the information will change what happens next. This is especially true when people discover that MRI findings and pain symptoms do not always match neatly.
The better question is what the next appointment should actually help decide
Try this instead: what does the next appointment need to decide for me? Do I need to know whether this is structural? Do I need a management plan that improves function? Do I need urgent evaluation because symptoms have changed sharply? That question strips away a surprising amount of medical fog.
Short Story: A reader once described her knee pain to me with perfect emotional precision and almost no useful timeline. She knew it was “getting worse,” knew stairs were now dreadful, knew she was tired of feeling old in a young body. What she had not tracked was when the swelling began, whether the pain followed a twist, whether it locked, whether rest changed it, or what had already failed.
Once she wrote those details down, the path got simpler. The first visit did not need to promise miracles. It only needed to answer the right question. In her case, the useful question was structural, so orthopedics came first. Had the joint already been worked up and the issue shifted to persistent pain despite a known diagnosis, pain management might have been the smarter front door. The body had not changed overnight. The clarity had.
Don’t Do This: Common Mistakes That Delay Real Relief
Booking by title instead of by pain pattern
This is the biggest mistake. “Pain doctor” sounds right because pain is the problem. “Orthopedic specialist” sounds right because the body part hurts. But titles are blunt instruments. Pain pattern, duration, mechanism, and goal are better guides.
Forgetting to track what makes pain better, worse, or radiate
Patients often arrive with intensity but not texture. “It hurts a lot” matters, but it is only one slice. Does it travel? Does it burn, ache, stab, catch, throb, or tingle? Does sitting worsen it? Walking? Stairs? Sleep? Rotation? Lifting? Those clues help specialists decide whether the problem sounds structural, neurologic, inflammatory, or less specific.
Bringing intensity without bringing a timeline
Timeline matters more than many people think. New pain after injury is one universe. Chronic pain after months of failed treatment is another. Post-operative pain, recurrent flares, and unexplained persistent symptoms each carry different logic. Without a timeline, the visit starts with fog.
Quote-Prep List: What to gather before comparing clinics
- Pain location and whether it travels
- Date or timeframe symptoms began
- What movement or activity triggers it
- What you have already tried and for how long
- Whether sleep, work, mobility, or daily function is worsening
Neutral next step: Put these five items in your phone notes before you call any office.
Before You Book: The 5 Clues That Help You Choose Better
Where the pain is and whether it travels
Localized joint pain after a clear movement or injury often pushes the needle toward orthopedics. Pain that radiates, burns, or behaves like nerve irritation can make the picture more complex and may still require structural evaluation before management becomes the main focus. For example, many people get stuck trying to sort out whether the pain is really coming from the hip or the spine.
What movement triggers it and what rest changes
If certain motions reproducibly trigger the pain, that can suggest a mechanical component. If the pattern is less movement-specific and more persistent or flare-based, management considerations may loom larger.
Whether the pain is new, chronic, post-injury, or post-treatment
New and post-injury complaints often deserve a structural lens first. Chronic pain after known workup may deserve a management lens. Post-treatment pain sits in the middle and often depends on what has already been ruled in or out.
What has already been tried, and for how long
If nothing meaningful has been tried, the first visit may need to set a basic plan rather than escalate. If several reasonable steps have already failed, the value of a more targeted specialty choice increases. In real insurance terms, documented failed conservative care before an MRI request can also change what gets approved next.
Whether function, sleep, work, or mobility is getting worse
Pain score alone can be theatrical. Function is often the quieter and more useful metric. If the pain is shrinking your life, that deserves weight in the decision.
Infographic: Which door fits the question?
Orthopedist
Best when the question is:
- What structure is injured?
- Do I need imaging, bracing, rehab, or surgical evaluation?
- Did this start after injury or a specific movement?
Pain Clinic
Best when the question is:
- How do I function better with ongoing pain?
- How do I manage flares and daily limitations?
- What plan fits a known or chronic pain problem?
Red flags override both: major weakness, fever with joint pain, inability to bear weight, major trauma, loss of bladder or bowel control, or rapidly worsening symptoms.
Here’s What No One Tells You: Insurance and Referral Logic May Quietly Shape Your Path
Specialist access may depend on referral rules
In the United States, the “best” first specialist is not always the one you can directly access. Some insurance plans require primary care referrals. Some health systems have their own routing habits. Some offices require imaging or prior records before scheduling with certain providers. It is not romantic, but logistics shape medicine all the time.
Prior treatment history can affect what gets approved next
Insurance logic also affects what is approved. A plan may want to see conservative treatment first before covering advanced imaging or certain procedures. That does not mean you should tolerate nonsense forever. It does mean that documenting what has already been tried can save friction later. For patients who run into a wall, that often becomes the story of what to do after an MRI denial and appeal.
The “best” specialist on paper may not be the best first stop in your plan
Think of the first appointment as part clinical fit, part systems navigation. A perfect theoretical choice can become a terrible practical choice if it requires months of waiting while a more appropriate intermediate step sits ignored. The right path is sometimes less like a straight line and more like a sensible relay race.
- Referral rules can shape access
- Prior treatment history often shapes approvals
- Records and timelines are currency in specialist care
Apply in 60 seconds: Before booking, ask the office and your insurer whether referral, prior records, or documented prior treatment are required.
If the First Visit Fails: What to Do When the Appointment Answers the Wrong Question
When to switch from orthopedist to pain clinic
If the structural workup is mostly complete, surgery is not indicated, and the central problem is ongoing pain with impaired function, pain management may become the more useful next step. This is especially true when symptoms are now chronic, flaring, or affecting sleep and daily life more than the original diagnostic uncertainty.
When to move from pain clinic back to orthopedic evaluation
If symptoms change sharply, weakness appears, a joint becomes unstable, swelling increases, or the original diagnosis feels shaky, you may need to circle back to structural evaluation. Management without clarity can only carry you so far.
Why second-step care is often more useful than perfect first-step care
There is good news here. You do not need to choose perfectly to make progress. You need to choose intelligently enough that the first visit produces information, not just activity. Plenty of good care paths involve one handoff. Trouble begins when nobody is clear what the handoff is for.
Healthcare is rarely a violin solo. It is more often chamber music, useful when the players know whose part comes next. Your job is not to perform expertise. It is to make sure the next clinician is holding the right page.
FAQ
Should I see a pain clinic or orthopedist for back pain?
It depends on the question. If your back pain is new, tied to a structural concern, or may need focused evaluation for imaging or rehab, an orthopedist may be the better start. If it is already evaluated, chronic, and the main issue is function or flare control, a pain clinic may fit better. Red flags such as weakness, loss of bladder or bowel control, or rapidly worsening symptoms need urgent evaluation.
Is an orthopedist better than a pain doctor for knee pain?
For new knee pain after injury, swelling, locking, instability, or pain with mechanical features, an orthopedist often makes more sense first. For chronic, already-evaluated knee pain where the main issue is ongoing symptom control, a pain specialist may become more relevant later.
Can a pain clinic diagnose the cause of my pain?
Sometimes they can help refine the picture, especially in complex chronic pain. But if the main unresolved issue is whether there is a structural musculoskeletal problem, orthopedics is often the cleaner starting point.
Will an orthopedist prescribe pain medication?
Orthopedists may prescribe medication in some situations, but their main role is not long-term pain management. Their work is typically centered on diagnosis, structural assessment, treatment planning, and rehabilitation pathways.
Do I need imaging before seeing either specialist?
Usually not. In many cases, the specialist decides whether imaging is useful after history and exam. For some uncomplicated pain patterns, early imaging is not the most useful first step. For other patterns, it may matter a great deal.
Can I go to a pain clinic without a referral?
Sometimes yes, sometimes no. It depends on your insurance plan, local health system, and the clinic’s own rules. Always check referral requirements, records requirements, and whether prior imaging or treatment history is needed.
What if my pain is chronic but still undiagnosed?
If the diagnosis is still meaningfully unclear, an orthopedic or other appropriate structural evaluation may still need to come first. Chronic pain does not automatically mean the first job is management. Sometimes it means the first job was never cleanly finished.
Should I see both a pain clinic and an orthopedist?
Sometimes yes. The question is sequence. It is often more efficient to start with the specialty best positioned to answer the most important unresolved question, then add the other if needed.
Which specialist is better for nerve pain?
It depends on whether the nerve pain seems tied to a structural cause that needs diagnosis, such as spine or joint-related compression, or whether the structural picture is already known and the main issue is symptom management. New weakness, significant numbness, or worsening neurologic symptoms need prompt medical attention.
What should I bring to my first appointment?
Bring a short timeline, prior imaging reports if you have them, a medication list, what treatments you have already tried, and notes on what worsens or relieves the pain. A one-page summary often helps more than a heroic verbal monologue.
Next Step: Book the Visit That Matches the Question, Not Just the Pain
Write down your pain location, timeline, triggers, and failed treatments before scheduling
Do this before you click anything. A clean symptom summary saves time with schedulers, primary care, and specialists. It also keeps you from narrating your pain like a weather system with no map.
Choose the specialist based on whether you need diagnosis or management first
This is the central thread of the whole article, and the hook closes here. People often think they are choosing between two kinds of doctors. In practice, they are choosing between two kinds of problems. Diagnosis first, or management first. Once you name the problem accurately, the specialist choice gets less theatrical and more useful.
If red flags are present, seek urgent medical evaluation instead of routine scheduling
That final rule matters because it protects the whole framework from misuse. Not every painful condition belongs in a routine specialty lane. Some belong in urgent care, emergency care, or same-day evaluation. When the pattern is severe or rapidly changing, speed matters more than optimization.
Safety / Disclaimer
This article is informational only and does not diagnose or treat medical conditions. In health topics, the safest path is usually the one that matches the type of problem you are having, not the most dramatic-sounding intervention. Severe symptoms, rapid worsening, loss of function, or signs of infection deserve prompt medical attention.
When to Seek Help
Seek urgent care for severe weakness, loss of bladder or bowel control, major trauma, or rapidly worsening symptoms
If any of these are happening, do not rely on routine scheduling logic. Seek urgent medical evaluation. If bowel or bladder symptoms are part of the picture, familiarize yourself with cauda equina syndrome red flags and treat them with appropriate urgency.
Seek prompt evaluation for fever with joint pain, marked swelling, inability to bear weight, or unexplained severe pain
These patterns deserve timely medical attention because they may reflect a problem more serious than a routine pain flare.
Do not rely on blog content alone when symptoms are intense, unusual, or changing quickly
Blogs can clarify decisions. They cannot examine a joint, test strength, or see what is changing in real time. When symptoms move fast, real-world care should move faster.
Practical Pathway Table
| Situation | Usually the smarter first stop | Notes |
|---|---|---|
| New knee, shoulder, ankle, or hip pain after injury | Orthopedist | Structural questions come first |
| Known chronic pain with flare control and function issues | Pain clinic | Management questions come first |
| Major weakness, fever, trauma, inability to bear weight | Urgent evaluation | Routine specialist comparison is not the priority |
Neutral next step: Use the table to narrow the front door, then confirm referral and insurance details.
Last reviewed: 2026-04.
The goal was never to become an amateur scheduler with a pain problem. The goal was relief, or at least a cleaner road toward it. In the next 15 minutes, write down your timeline, your triggers, your function changes, and the one question your first appointment needs to answer. Then book the visit that matches that question. Not the scariest title. Not the fastest office. The right question. That is usually where wasted time and money begin to loosen their grip.
