
Navigating the Limbo: Managing Orthopedic Pain During an MRI Appeal
When an MRI denial arrives in the middle of an orthopedic flare, the pain does not pause just because the paperwork did. What makes this stretch so draining is not only the discomfort, it is the strange limbo of trying to manage symptoms, protect an appeal, and explain your body in language an insurer will accept.
“Appeals usually get stronger when the chart tells a clean story.”
For many patients, the hardest part is the uncertainty. You are told to wait, but rarely told what to do with that waiting. Meanwhile, sleep gets thinner, work gets harder, and every missed follow-up risks making the medical record look calmer than reality. Keep guessing too long, and you can lose both symptom control and the documentation strength your MRI appeal needs.
- What actually helps
- Tracking functional loss
- What weakens the case
- Red flag monitoring
Learn what to say, track, and do while imaging approval is still in limbo.
Table of Contents
Who this is for, and who should skip it
This is for
- Adults in the US whose MRI was denied and is now under appeal
- Patients managing orthopedic pain during an insurance review delay
- Caregivers helping organize treatment notes, appointments, and symptom tracking
- Readers trying to understand what usually matters while waiting for imaging approval
This is not for
- Anyone with sudden neurologic symptoms, loss of bowel or bladder control, severe trauma, or rapidly worsening pain
- Readers looking for a diagnosis without clinical evaluation
- People who need emergency care rather than step-by-step planning during an insurance delay
I want to say this plainly because too many health articles get theatrical for clicks and foggy on boundaries. There is a world of difference between “my insurer is slow” and “my symptoms are unsafe to monitor at home.” This piece lives firmly in the first category. If you have new weakness, progressive numbness, saddle anesthesia, fever with severe spinal pain, or bowel or bladder changes, the delay story ends and the urgent-evaluation story begins.
For everyone else, the task is more modest and more useful. You are trying to manage pain, preserve function, and help your clinician document what is happening in a way that supports good care. That can feel frustratingly unglamorous. No one wants a masterclass in symptom logs while they are waking up at 3:12 a.m. because rolling over lights up the back, shoulder, knee, or hip like a bad fireworks finale. But this is the work that often sharpens the case.
A few years ago, I helped someone sort through a denial packet that looked as if it had been written by a committee of staplers. The turning point was not dramatic. We did not discover a secret phrase or win by sheer indignation. We built a cleaner timeline: when the pain started, what made it worse, what treatments had already been tried, what function had changed, and what the clinician found on follow-up. That boring little sequence did more than panic ever could.
- Know which symptoms are urgent
- Treat function as a core health measure
- Keep your story consistent across visits
Apply in 60 seconds: Write down the date of your denial, your next follow-up date, and the top three daily tasks pain is disrupting.
Start here first: what “pain management” really means during an appeal
It is not just about pain scores
Most people think they need a better number. “It is an 8 out of 10” feels precise, and sometimes it is useful, but insurers and clinicians often need more than a number floating in space. The fuller picture includes whether pain wakes you up, limits walking, changes lifting, reduces grip, prevents sitting through a workday, or makes stairs, driving, dressing, or caregiving harder. A chart that shows altered function often tells a more medically useful story than ten dramatic adjectives stacked on top of one another.
That is not because your suffering needs to audition for legitimacy. It is because orthopedic care is deeply tied to movement, load, range, endurance, and pattern. “It hurts when I exist” may be emotionally accurate on a bad day. But “I can only sit 20 minutes before sharp right hip pain makes me stand” gives a clinician and reviewer something they can actually use.
The hidden goal: build a cleaner evidence trail
During an appeal, your chart becomes a kind of map. It should show symptom location, duration, what has already been tried, whether you improved, stayed the same, or worsened, and what exam findings or function limits continue to matter. Consistency matters here. If one visit says pain radiates below the knee with numbness and the next says “mild soreness, improving” because you were trying to sound stoic, the story frays at the edges.
The American College of Radiology describes its Appropriateness Criteria as evidence-based guidance for selecting the most appropriate imaging, and its low back pain criteria note that MRI becomes more appropriate in certain patterns, including persistent or progressive symptoms after a period of optimal medical management or when serious red flags are present. That is a fancy way of saying timing, symptom pattern, and documented progression matter more than people realize.
I have watched more than one patient accidentally make themselves sound better out of politeness. It is a strangely common reflex. We do not want to be “difficult.” We do not want to sound dramatic. We shrink the facts until the record looks calmer than the body feels. In appeal territory, that instinct is expensive.
Show me the nerdy details
When clinicians talk about failed conservative care for MRI approval, they usually mean documented attempts over time, not vague self-treatment. The chart often becomes stronger when it shows treatment dates, response, side effects, functional limits, and exam findings in sequence.
Eligibility checklist: is your current record helping the appeal?
Yes / No questions:
- Do you have a follow-up appointment scheduled?
- Is there a written symptom timeline?
- Have prior treatments been documented by a clinician?
- Can you describe at least 3 function limits clearly?
- Have you reported any new weakness, numbness, or sleep disruption?
Neutral next step: Any “no” on that list is a practical place to tighten the record this week.
Appeal in progress: what doctors and insurers often look for next
Documentation that moves the case forward
At this stage, vague frustration is understandable but rarely productive. What usually moves the case forward is clean documentation of symptom duration, severity pattern, location, triggers, and functional loss. Insurers also tend to care whether conservative measures were attempted before advanced imaging. Clinicians care about that too, though often for different reasons. They are trying to decide whether the next step should be more time, a different treatment path, a referral, or faster reassessment.
- Symptom duration: “Started 7 weeks ago after lifting,” not “a while back”
- Location: “Pain in left shoulder radiating to upper arm,” not just “arm pain”
- Function: “Cannot sleep on that side or reach overhead,” not just “worse lately”
- Treatment history: physical therapy, home exercise, activity changes, medications, injections if applicable
- Response: better, unchanged, or worse, with specifics
Here’s what no one tells you…
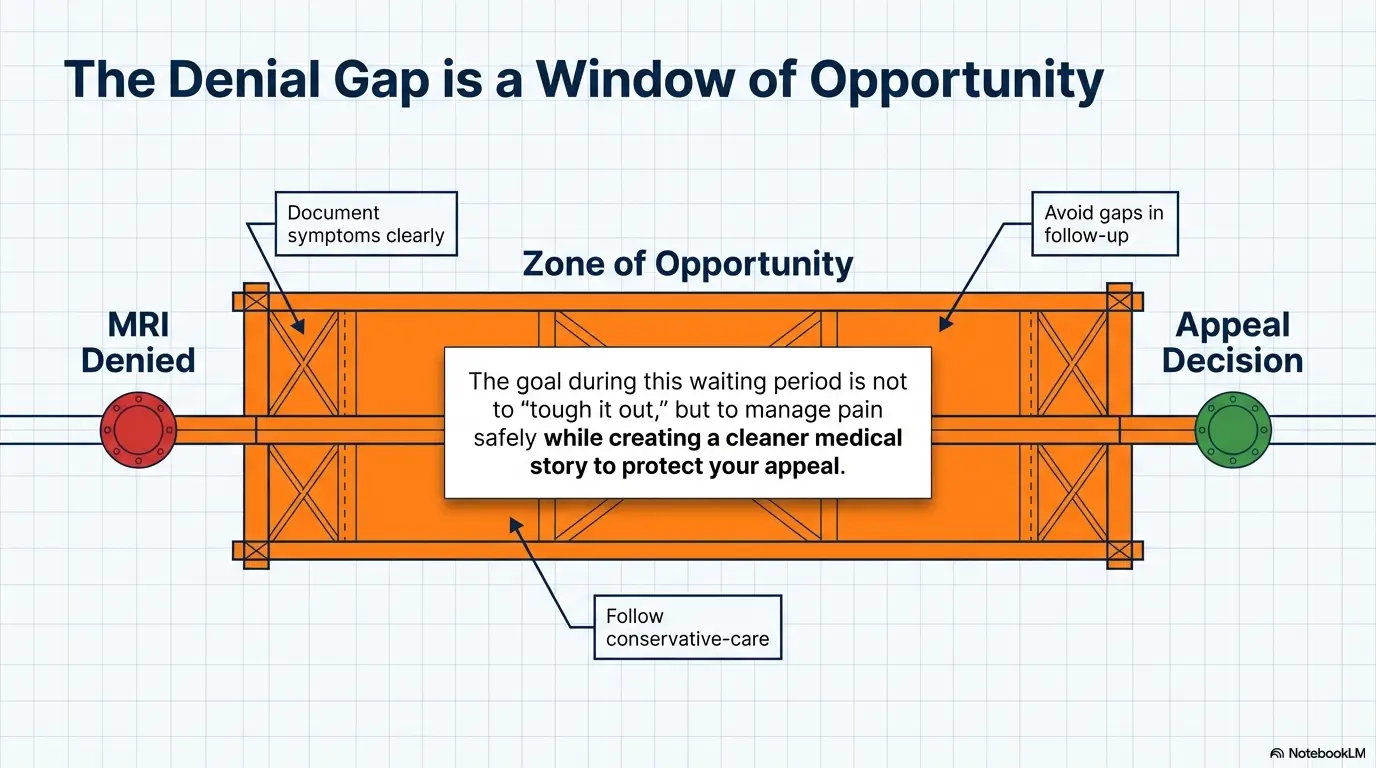
A denial does not always mean the insurer thinks you are making it up, and it does not necessarily mean “never.” Often it means the case, as submitted, did not yet satisfy the payer’s timing or documentation rules. That is maddening, yes. It is also why the weeks after a denial matter so much. This is the period where the chart either thickens into a coherent clinical story or dissolves into disconnected appointments.
MedlinePlus explains that diagnostic imaging includes MRI among several tools and that the type of imaging used depends on the symptoms and the part of the body being examined. That is a useful reminder that the real question is not “Do I want an MRI?” but “What does my symptom pattern and exam suggest, and what has already been tried?”
The honest emotional part is harder. Waiting does strange things to pain. It makes every twinge feel like evidence and every phone call feel like a verdict. One of the best ways to reduce that spiraling is to separate what you can control from what you cannot. You cannot personally approve the MRI. You can absolutely tighten the record that supports it.
Conservative care counts, but not all of it counts equally
What usually strengthens the record
Conservative care is a broad umbrella, and not every raindrop under it matters equally. What tends to strengthen an appeal record is clinician-documented treatment with clear response notes. That often includes follow-up with the ordering clinician, physical therapy attendance, home exercise plans that were actually discussed in a visit note, medication trials with benefits and side effects documented, and repeat visits showing what changed over time.
AAOS notes that orthopaedic patient education should help people understand symptoms, causes, and treatment options, and its patient materials on non-medication pain approaches describe tools like TENS, acupuncture, and brain-body methods as approaches a doctor may recommend in some musculoskeletal settings. The key phrase there is may recommend. The appeal record is strongest when treatments are not merely attempted in the privacy of your living room, but assessed and documented in clinical context.
What tends to weaken it
Three things quietly weaken a case. First, long gaps with no reassessment. Second, self-directed treatment that never appears in the chart. Third, inconsistent descriptions across visits. It is surprisingly easy to do all three while trying very hard to be “reasonable.” You skip a follow-up because life is busy, you try stretches from a video at midnight, you tell one clinician the pain is stabbing and another that it is mostly fine because today happens to be a lighter day. Individually, none of that feels sinister. In aggregate, it muddies the story.
I once knew someone who diligently used heat, reduced lifting, tried over-the-counter medication, and modified exercise for weeks. It was not laziness. It was textbook effort. But because almost none of it was relayed back to the clinician in a clear follow-up, the record looked oddly thin. The body had been doing overtime while the chart wore slippers.
- Attendance matters
- Response notes matter more
- Gaps can be misread as improvement
Apply in 60 seconds: Make a list of every treatment you have tried and bring it to your next appointment with dates and results.
Pain journal, but smarter: what to track so it actually helps
Record function, not just feelings
A useful symptom log is not a literary diary of suffering. It is a tool. The best logs are brief, concrete, and repetitive in the right way. Track what movement triggers pain, what you had to stop or reduce, whether pain woke you from sleep, and what happened after you tried the recommended treatment. This is the kind of note that makes a follow-up visit easier for both you and the clinician.
Let’s be honest…
“It hurts all the time” may be true at the level of mood, but it often flattens the picture. It is more helpful to show pattern: worse after stairs, worse after 25 minutes sitting, worse when reaching overhead, numbness after walking two blocks, sleep interrupted twice nightly. Pattern gives shape to the problem. Shape gives the next visit traction.
A better symptom log structure
- Date and flare trigger: what were you doing?
- Pain location and pattern: where, and does it radiate?
- What you tried: heat, ice, medication, stretching, PT exercise, rest, brace, position change
- What changed afterward: 20% better, no change, worse after 2 hours
- What you still could not do: sleep flat, lift laundry basket, drive 30 minutes, type, kneel, carry groceries
Here is a simple rule I like. Keep entries to 4 or 5 lines. That way the log stays usable instead of becoming a memoir with ibuprofen. You do not need a tragic monologue. You need a crisp pattern.
Mini calculator: function-loss snapshot
Pick 3 daily tasks that matter most right now. For each one, score how long you can do it before pain forces you to stop.
- Sitting: ___ minutes
- Walking: ___ minutes or blocks
- Sleeping uninterrupted: ___ hours
If those numbers are shrinking over 1 to 2 weeks despite treatment, that is useful information to bring to follow-up.
Neutral next step: Put these three numbers at the top of your symptom page and update them every few days.
Show me the nerdy details
Symptom logs become more persuasive when they track trend, not just intensity. A stable 6 out of 10 with worsening walking tolerance is a different clinical story than a fluctuating 6 out of 10 with improving function.
Don’t accidentally sabotage your own appeal
Common mistakes
- Waiting too long to follow up after the denial
- Assuming the clinic is handling every appeal detail automatically
- Using inconsistent language about symptoms from one visit to the next
- Stopping recommended care because the MRI was denied
- Underreporting numbness, weakness, or mobility decline because you do not want to “complain”
Don’t do this: the “I’ll just wait it out” trap
This is probably the most common unforced error. The denial creates a weird emotional pause. Patients assume the next move belongs to the insurer, so they become passive. Weeks pass. No reassessment happens. No updated exam is documented. No one records that stairs are worse, sleep is worse, or the numbness is spreading. Then, when the appeal is reviewed, the timeline has a hole right where the case needed shape.
The trap is especially sneaky because it can feel virtuous. You are being patient. You are trying not to overreact. You are not demanding. The chart, unfortunately, is not grading your character. It is recording events, or not recording them. Silence often looks like stability. Stability can look like improvement. Improvement is not the message you want accidentally sent if things are not improving.
One of the lightest but truest forms of self-advocacy is administrative follow-through. Call to confirm whether the appeal was submitted. Ask what clinical documentation was included. Ask whether your most recent visit note made it into the packet. This is not being difficult. It is being awake.
Decision card: wait quietly vs follow up now
| Choice | What you gain | What you risk |
|---|---|---|
| Wait quietly | Less hassle today | Chart gaps, stale exam, weaker timeline |
| Follow up now | Updated documentation, clearer plan | One phone call, one appointment, mild annoyance |
Neutral next step: Choose the option that improves the record, not just the afternoon mood.
Treatment while waiting: what usually happens before imaging is approved
Common next-step options clinicians may discuss
- Activity modification
- Short-term medication review
- Physical therapy or home exercise progression
- Recheck visits to document change over time
- Referral escalation if red flags appear
The real tension: relief now vs evidence later
This is where people get understandably tangled. You want relief today. You also need the chart to reflect what has and has not worked. Those are not enemies. They simply need to be handled carefully. A good treatment plan during the appeal window should do two things at once: reduce suffering where possible and create usable information for the next decision.
That may look like trying a medication adjustment with clear instructions on side effects, attending PT with attention to specific limitations, modifying activities without complete deconditioning, or using heat, ice, bracing, or positioning advice in a way that is actually discussed at follow-up. The point is not performative suffering. It is measured care.
MedlinePlus notes that MRI itself can take time and requires the patient to remain still, which sounds almost comic when you are already miserable, but it underscores something useful: imaging is a tool in a broader plan, not the whole plan. You still need symptom management, monitoring, and a clinician-guided path while the authorization piece is unresolved.
I once watched a person treat the denied MRI like the plot and the pain like a subplot. It should be the other way around. The real plot is care. The appeal is one chapter in it.
- Relief matters
- Documentation matters too
- Neither requires exaggeration
Apply in 60 seconds: Write down one treatment that helped, one that did not, and one side effect or limitation you need your clinician to know.
Red flags matter more than patience
When to seek help
- New weakness, foot drop, grip loss, or limb instability
- Numbness that spreads or worsens
- Fever, unexplained swelling, or signs of infection
- Severe pain after trauma
- Loss of bladder or bowel control
- Pain that becomes suddenly intolerable or rapidly progressive
Here’s where caution wins
One of the more dangerous myths in denial-land is that every problem must now wait its turn because insurance is “reviewing.” That is not how medicine works, and it is not how your body works either. New or rapidly worsening neurologic symptoms change the picture. Serious trauma changes the picture. Signs of infection change the picture. The review clock does not outrank those developments.
The ACR low back pain criteria specifically identify situations where MRI is usually appropriate earlier, including serious red-flag patterns such as suspected cauda equina syndrome and scenarios involving cancer, infection, or major neurologic concern. In plain language, some symptom changes deserve urgent reassessment even if the original denial is still sitting on someone’s desk. If you need a more focused explanation of those emergency patterns, see cauda equina syndrome red flags.
This section is where I would rather sound repetitive than clever. If something is worsening in a way that changes safety, seek care. You do not need to win a paperwork contest before reporting weakness or bladder changes. Sometimes the bravest health decision is also the least theatrical one: call now.
The insurance side nobody explains clearly enough
MRI denial does not always mean your case is weak
Many first-pass MRI denials are administrative rather than philosophical. That does not make them less frustrating. It just means the problem may be incomplete documentation, missing proof of step care, insufficient symptom duration in the submitted note, or a mismatch between the request wording and the payer’s criteria. In other words, the case may be underbuilt rather than unwinnable.
That is why the phrase “medically necessary” can be so misleading in ordinary conversation. People hear it as a moral judgment. But on the payer side, it often functions as a documentation threshold linked to symptom pattern, duration, prior treatment, and sometimes specialty-specific criteria. Annoying? Deeply. Final? Not always. For readers balancing this with cost questions, it may also help to understand a high-deductible health plan imaging cost estimate while the appeal is pending.
What makes appeals stronger over time
- Updated exam findings
- Clear documentation of failed treatment attempts
- Functional decline that is specific, recent, and consistent
- Clinician notes that connect symptoms to medical necessity
The strongest appeal material usually reads like a calm sequence, not a courtroom speech. Symptoms started here. Conservative steps were tried here. Function remained limited or worsened here. Exam findings now show this. Based on that progression, imaging is needed to guide the next treatment decision. It is almost disappointingly tidy. But tidy often wins.
Short Story: A friend of a friend, the kind of phrase that sounds suspiciously fictional and was very real in this case, had persistent back and leg pain after a lifting injury. The first MRI request was denied. She was furious and then, for two weeks, oddly silent. No follow-up. No updated note. No record of the fact that walking tolerance had dropped from 30 minutes to 8 and that sleep was breaking into splinters every night.
At the next visit, her clinician documented progressive symptoms, PT attendance without meaningful relief, and new radiating pain with numbness. The appeal looked different because the story had become visible. Not louder. Visible. That distinction matters. Pain had been unfolding the whole time. The chart just finally caught up.
Coverage tier map: what usually changes from Tier 1 to 5
| Tier | What the record usually contains |
|---|---|
| 1 | Pain complaint only |
| 2 | Pain plus location and duration |
| 3 | Pain plus function limits plus prior treatment |
| 4 | Updated exam plus failed conservative care |
| 5 | Clear progression and documented reason imaging changes management |
Neutral next step: Figure out which tier your current chart resembles, then ask what is missing to move it up one level.
Show me the nerdy details
Appeals become easier to support when the note explains how MRI results would affect management, such as referral planning, injection decisions, surgical evaluation, or investigation of red-flag pathology.
If pain is affecting work, sleep, or caregiving, say that plainly
Function is not a side note
Work, sleep, driving, childcare, bathing, dressing, lifting, standing, and sitting are not sentimental extras. They are often the real-life expression of orthopedic impairment. If pain is affecting them, that belongs in the medical story. Patients often hide this because they do not want to sound needy or because they think only “medical” facts count. But in musculoskeletal care, daily function is one of the most medical facts there is.
AAOS patient education frequently frames orthopedic conditions in terms of how they affect daily activities, including walking, stairs, and lost work time in common conditions such as knee arthritis. The broader lesson travels well: functional decline is clinically meaningful, not decorative.
Let’s keep it concrete
Useful language sounds like this:
- “I cannot sit more than 20 minutes without sharp hip pain.”
- “I wake up 2 to 3 times a night because rolling over triggers low back and leg pain.”
- “I can still work, but I have to stand every 15 minutes and I am slower with lifting.”
- “I can care for my child, but I cannot safely carry them upstairs right now.”
Less useful language sounds like this:
- “It is awful all the time.”
- “Everything hurts.”
- “I can’t do anything.”
The first set gives shape. The second set gives mood. Mood matters, of course. It is just not enough on its own. Think of it this way: your clinician is not trying to judge your poetry. They are trying to see the mechanics of your day.
- Use times, distances, and tasks
- Describe what changed
- Avoid vague drama and vague stoicism
Apply in 60 seconds: Write three sentences that start with “I can no longer…” or “I can only…” and bring them to your next visit.
What to ask at your next appointment so you leave with a plan
Questions that move the case forward
- What has already been submitted in the appeal?
- What conservative treatments still need to be documented?
- What symptom changes would justify faster reassessment?
- What should I track between now and the next visit?
- At what point would referral or escalation be appropriate?
The visit goal most people miss
Leave with one documented next step, not just reassurance. Reassurance has its place, but it is not a plan. A plan might be a PT course with a recheck date, a medication change with monitoring instructions, a specialty referral, an updated exam note for the appeal file, or clear criteria for when to call sooner. If you leave with “let’s see how it goes” and nothing else, the visit may feel emotionally fine and administratively weak.
Bring a one-page summary. Make it boring in the best possible way. Timeline. Treatments tried. Three functional limits. New symptoms. Questions. That single page can keep the appointment from drifting. In a rushed clinic day, drift is the enemy.
Quote-prep list: what to gather before the next visit
- Date of injury or symptom onset
- Date MRI was denied and appeal submitted
- Medication list and what each one actually did
- PT attendance or home exercise notes
- Top 3 function limits
- Any new weakness, numbness, falls, or sleep disruption
Neutral next step: Put this on one page so the clinician can see the whole story in under 30 seconds.
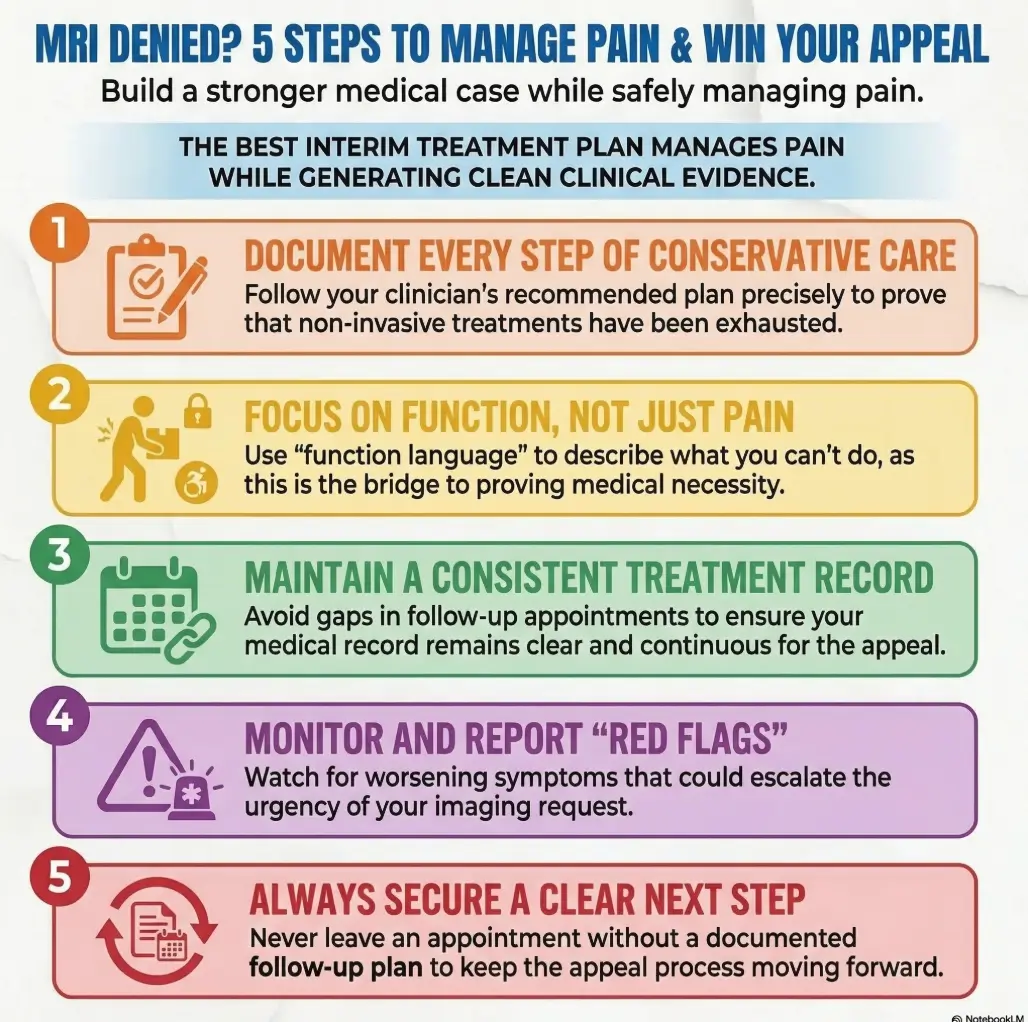
Infographic: the 5-step action map while you wait
Ask whether the appeal was filed and what records were included.
Follow the clinician-guided plan instead of freezing in place.
Log sitting, walking, sleep, lifting, and flare triggers.
Report new weakness, bladder changes, trauma, fever, or rapid progression.
Get a recheck date, updated note, and a clear threshold for escalation.

FAQ
Can I still get orthopedic pain treatment if my MRI was denied?
Yes. An MRI denial does not automatically stop orthopedic pain treatment. Clinicians can still recommend follow-up, physical therapy, medication review, activity modification, and reassessment. The important part is to keep care moving and keep the response documented.
Does physical therapy help an MRI appeal?
It often can, especially when attendance, exercise tolerance, and lack of improvement are documented clearly. PT is not a magic key, but it frequently helps show that conservative care was attempted and whether function improved, stayed limited, or worsened. Readers sorting out the money side may also want to compare physical therapy copay vs coinsurance before starting or continuing visits.
What if my pain is getting worse while I wait?
Tell your clinician. Worsening pain, especially with new weakness, spreading numbness, falls, fever, trauma, or bladder or bowel changes, may justify faster reassessment. Waiting quietly is not always the safe move.
How long do MRI appeals usually take in the US?
Timelines vary by insurer, plan, urgency level, and whether the appeal is standard or expedited. Because those timelines are plan-specific, it is smarter to ask your insurer and clinic exactly what stage the request is in rather than rely on generic averages.
Should I keep a symptom diary during an appeal?
Usually yes, but keep it short and practical. Focus on triggers, function limits, sleep disruption, treatment attempts, and what changed. A crisp pattern log helps more than an emotional narrative alone. If you are already documenting this for work or disability purposes, an ERISA LTD pain diary framework may give you ideas for keeping entries concrete.
What symptoms should I report immediately?
New weakness, loss of bladder or bowel control, rapidly worsening numbness, severe pain after trauma, fever with severe pain, or major functional collapse deserve prompt reassessment. These can change the urgency of care.
Can a second doctor help support the appeal?
Sometimes. A second opinion or specialist follow-up may add updated findings, a clearer diagnosis pathway, or documentation explaining why imaging would change management. Whether it helps depends on the case and the timing. If the issue involves network restrictions, a guide to an out-of-network spine surgeon gap exception may also be useful.
Does insurance care about daily function or only diagnosis?
Function often matters a great deal because it helps demonstrate severity, persistence, and how symptoms affect daily life. In musculoskeletal conditions, function is not fluff. It is part of the medical story.
What if conservative treatment is not helping at all?
That information matters. Make sure the lack of benefit is documented clearly, along with side effects, worsening function, or new findings on exam. “Not helping” becomes much more useful when it is specific and recorded over time.
Next step
Book one follow-up and bring one page
Schedule your next orthopedic or primary care follow-up, then bring a one-page summary of your symptom timeline, treatment attempts, and three specific ways the pain is limiting function. In appeal situations, clarity is often more powerful than volume.
This closes the loop from the beginning of the article. The bureaucratic magic trick stops feeling magical when you stop treating the denial as a verdict and start treating it as a documentation problem with a care plan attached. You may still be frustrated. Very normal. But you are no longer passive.
Within the next 15 minutes, do three things: confirm the appeal status, write down your top three function limits, and schedule or confirm follow-up. That small triangle of action will usually do more for your case than doom-scrolling denials at midnight with one eye open and an ice pack sliding toward the floor. If sitting at work is one of the main pain triggers you plan to document, resources on desk-job sciatica keyboard and mouse placement, a sit-stand schedule for desk-job sciatica, or seat cushion vs lumbar roll for sciatica may help you describe what worsens symptoms and what changes you have already tried.
Last reviewed: 2026-03.
Safety / Disclaimer
This article is for general educational purposes and does not diagnose, treat, or replace medical advice. Orthopedic pain can range from frustrating to urgent, and insurance delays do not rule out serious problems. Use a licensed clinician’s guidance for treatment decisions, especially if symptoms are worsening or new neurologic changes appear.
