
Beyond the Stall: Navigating Orthopedic Pain When PT Isn’t Enough
When physical therapy is not helping orthopedic pain, people often waste the most money in the most ordinary way: by repeating a plan that has already stopped earning its keep. They do more sessions, more stretches, and more hopeful guessing, while the pain keeps interrupting sleep, stairs, work, or the simple act of trusting their own body.
That stall can feel strangely personal, as if better outcomes belonged to people who were more disciplined, less busy, or somehow built from more obedient cartilage. But persistent orthopedic pain after PT usually points to a decision problem, not a character flaw. Keep guessing too long, and the bill grows while function quietly shrinks.
This guide helps you sort what stalled progress may actually mean, when a rehab plan needs adjustment, when MRI referral for orthopedic pain or a second opinion might make sense, and how to prepare for a smarter follow-up without drifting into expensive medical theater.
• Protect function, reduce waste, and make your next step more precise.
• Based on symptom patterns, function changes, and the questions that actually change treatment.
• Because “PT failed” is usually too crude to be useful.
Start here. The pattern tells you more than the frustration does.
Fast Answer: When physical therapy is not helping orthopedic pain, the next move is not always “more PT” or “stop everything.” Often, the smarter step is to figure out why progress stalled: wrong diagnosis, wrong intensity, poor fit between exercises and symptoms, or a condition that needs a different workup. The goal is to reassess, protect function, and choose the next decision carefully rather than spending blindly.
This article is for general education, not diagnosis or medical advice. New weakness, numbness, fever, loss of bowel or bladder control, severe swelling, major injury, chest pain, or rapidly worsening pain needs prompt medical evaluation.
Table of Contents

When PT Stops Helping, What That Usually Means
“Not helping” can mean no change, partial change, or delayed flare-ups
“Physical therapy is not helping” sounds like one sentence, but it usually hides at least three different stories. In one, pain never changed at all. In another, pain improved 20% to 30%, then plateaued. In a third, each session helped for a day or two, then symptoms flared like a smoke alarm with bad timing. Those are not the same clinical picture, and they should not lead to the same next step.
I have watched more than one patient describe all three patterns with the same frustrated shrug. From the outside, it looked like failure. From the inside, it was data. Not glamorous data, not movie-trailer data, but the useful kind. The kind that can save two more months of circling the block.
Lack of progress does not automatically mean the pain is “in your head”
A stalled response does not mean the pain is imaginary, exaggerated, or somehow morally disappointing. Orthopedic pain can persist because the original diagnosis was incomplete, because the painful tissue is not the whole story, because the exercise dosage was too aggressive, or because the body needed a different sequence of care. Pain is not a courtroom verdict. It is a signal, and sometimes a messy one.
Why stalled recovery is often a signal to reassess, not panic
The best next step is often boring in the best way: reassess the problem carefully. That means asking what the working diagnosis was, what changed, what did not, which movements helped, which worsened symptoms, and whether the plan still matches the current pattern. The American Academy of Orthopaedic Surgeons and the American College of Radiology both lean toward decision-based evaluation rather than reflexive testing for every ache. That is helpful news. It means a careful reassessment can be more valuable than a dramatic next move.
- No change, partial change, and flare-based change are different patterns
- Stalled progress does not prove the pain is minor or imaginary
- Reassessment often creates more value than panic
Apply in 60 seconds: Write one sentence describing your pattern: no change, some change, or flare after sessions.
Who This Is For, and Who It Is Not For
This is for people with orthopedic pain who tried physical therapy and still feel stuck
This guide is for adults who have already tried physical therapy for orthopedic pain and still do not feel meaningfully better. Maybe your shoulder still wakes you at 3 a.m. Maybe your knee tolerates grocery shopping but mutinies during stairs. Maybe your low back is less dramatic than before, but still not functional enough to trust. That stuck-in-between place is exactly where many expensive decisions happen.
This is for patients trying to choose the next step before spending more time or money
It is also for people trying to think clearly before booking another round of visits, chasing imaging, switching providers three times, or assuming surgery is now around the corner wearing a black cape. The goal here is not to replace a clinician. It is to make the next appointment sharper, faster, and less wasteful, especially if you are trying to manage orthopedic pain with a high deductible or decide between insurance and self-pay cash price ranges.
This is not for emergencies or severe new symptoms that need urgent care
This is not the right framework for emergencies. Sudden severe weakness, loss of bowel or bladder control, marked swelling, suspected fracture, fever with worsening pain, hot red joints, major trauma, chest pain, or rapidly progressive neurologic symptoms deserve prompt medical attention. When red flags show up, strategy articles should step aside and let medicine do its louder work.
Eligibility checklist
- Yes: You completed some PT, but pain or function is still not where it needs to be.
- Yes: You want a calmer, more cost-aware next step.
- No: You have severe new neurologic symptoms, major trauma, fever, or other urgent warning signs.
Next step: If this sounds like you, prepare for reassessment rather than assuming the only options are “keep going” or “give up.”
Pain After PT: The First Question Is Not “What Treatment?” but “What Changed?”
Did pain stay the same, move, intensify, or become more predictable?
The first useful question is not “What treatment should I try next?” It is “What changed?” Pain that moved from sharp and random to dull and predictable may still be unpleasant, but it tells a different story than pain that expanded into new areas, became more constant, or started arriving with weakness or numbness. Pattern matters. Location matters. Timing matters.
I once saw someone insist nothing had improved, then describe that they could now sit for 40 minutes instead of 10. That is not nothing. That is function quietly entering the room while the pain score hogged the microphone.
Did function improve even if pain did not fully leave?
Function may improve before pain fully settles. You may walk farther, lift more safely, sleep better, or recover faster after activity even while pain still nags. That does not mean you should ignore ongoing symptoms. It means pain alone may be a sloppy reporter. Good follow-up visits look at both pain and function because management decisions often hinge on both.
Here’s what no one tells you: pain score alone can hide real progress
A single 0-to-10 pain score is useful, but incomplete. Two people can both say “6 out of 10” while one is missing work and the other is back to gardening for 30 minutes. That is why a simple symptom timeline beats memory. Write what you could do four weeks ago, what you can do now, and what reliably triggers symptoms. You are building a map, not a diary entry written in a parking lot.
Bold truth: Pain that is still present is not the same thing as pain that is unchanged.
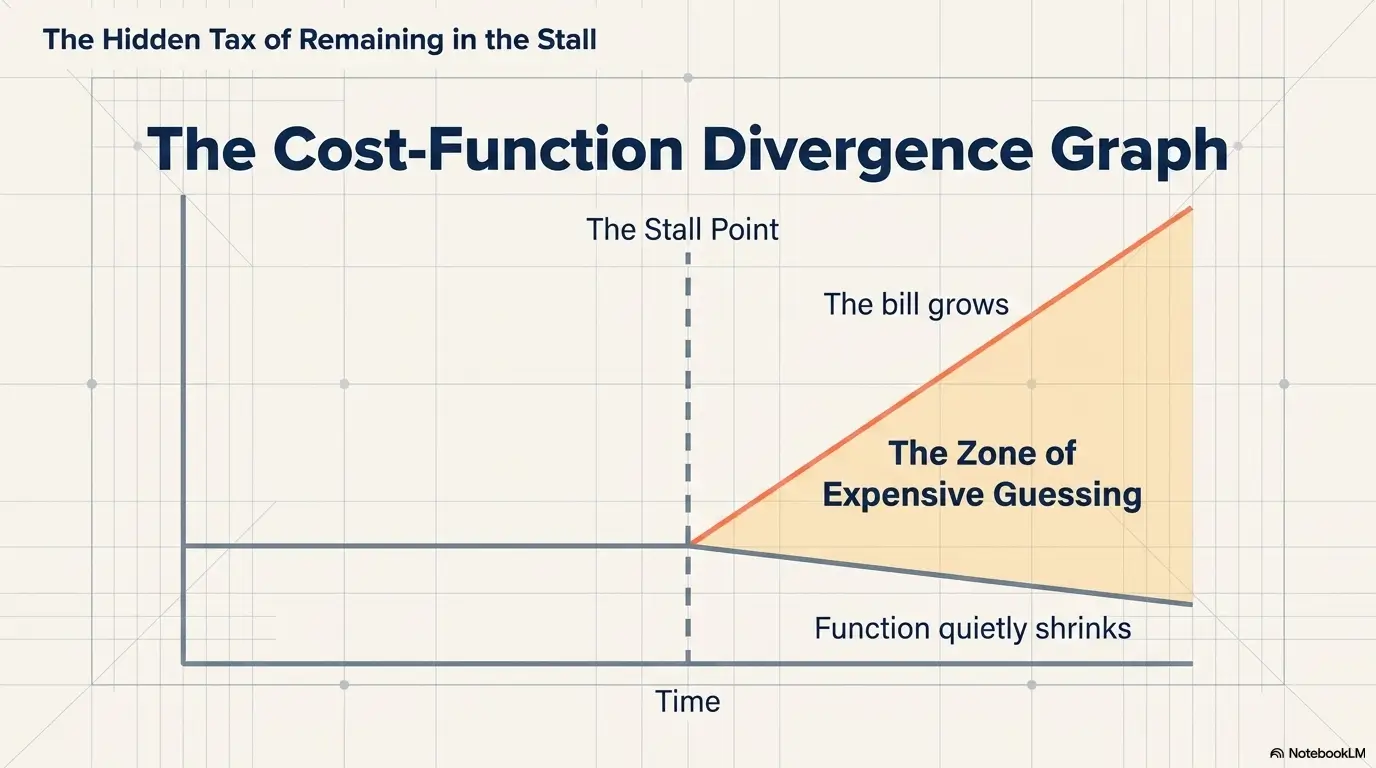
Wrong Target, Wrong Tempo: Why Good Effort Still Fails
Sometimes the exercise plan is sound, but the dosage is off
Good exercises can still be wrong at the wrong dose. Too much too soon can keep irritated tissues stirred up. Too little can fail to build capacity. Some programs are technically correct and practically unbearable, which is a fancy way of saying the sheet looked smart but your body filed a complaint. Dosage, frequency, range, speed, and recovery all matter. A plan that works beautifully for one knee can annoy another like a shoe that fits on paper but blisters in real life.
Sometimes the painful structure is not the only driver
Orthopedic pain is not always driven by one neat structure. Strength deficits, mobility limits, sleep disruption, fear of movement, nerve irritation, gait changes, repetitive work demands, and plain old schedule chaos can all change outcomes. If treatment aimed at one structure only, progress may stall because the larger pattern was never addressed.
Sometimes the body is irritated by repetition, not rescued by it
There is also the possibility that repetition itself is the irritant. Not every painful shoulder wants more overhead volume. Not every sore hip enjoys a thousand heroic clamshells. Not every back responds well to being “challenged” five days a week because the internet loves hustle. Bodies are not productivity apps. Recovery has rhythm. When tempo is wrong, effort turns into noise.
Show me the nerdy details
In musculoskeletal rehab, dosage often includes total volume, frequency per week, intensity, and recovery tolerance. A program can fail because the exercise choice is wrong, but also because the load progression outpaced tissue tolerance or because symptom response was not monitored closely enough.
Decision card: When A vs B
A: Symptoms are mildly irritated for less than 24 hours after exercise, but function is improving. That often suggests adjustment, not abandonment.
B: Symptoms are escalating, spreading, or repeatedly knocking out daily function. That often suggests reassessment before pushing forward.
Time/cost trade-off: A smart reassessment visit can cost less than weeks of repeating the wrong plan.
Neutral action: Track symptom response for 3 to 7 days before your next appointment.
Before You Quit PT Completely, Check These Three Friction Points
Was the diagnosis ever clearly explained in plain language?
If you cannot explain the diagnosis in one or two plain sentences, the plan may never have had a fair chance. “We are treating irritation around the rotator cuff and trying to improve shoulder mechanics” is usable. “There are multiple contributing factors with compensatory dysfunction” may be technically true, but it does not help much while standing in your kitchen with a resistance band that already feels like a symbol of betrayal.
Did the home program feel realistic enough to follow consistently?
Many home programs fail not because patients are lazy, but because the plan does not fit real life. Ten exercises, twice a day, in perfect sequence, with equipment scattered between the bedroom and the laundry room, is not a home program. It is an obstacle course with branding. A sustainable plan often beats an ideal one. Three well-chosen exercises done consistently can matter more than ten abandoned ones.
Let’s be honest… a plan you cannot sustain is not really a plan
Consistency is clinical information. If you kept skipping the same exercise because it always caused a flare, that matters. If a movement helped but you forgot which one because no one asked you to track it, that matters too. Before quitting PT completely, ask whether the problem was the entire concept of rehab or a poor fit in explanation, dosage, or logistics.
- Diagnosis should be understandable in plain language
- Home programs must be realistic to count
- Repeated flares are feedback, not personal failure
Apply in 60 seconds: Circle the one exercise that consistently worsened symptoms and bring that note to your follow-up.
Common Mistakes That Can Keep Orthopedic Pain Going
Pushing harder just because the last session “should have worked”
Frustration often makes people negotiate badly with pain. They double down, add more reps, restart old workouts, or test themselves every other day. It feels productive. Sometimes it is just expensive stubbornness in gym clothes. When a plan is not working, intensity is not automatically the missing ingredient.
Resting completely for too long and losing strength, mobility, or confidence
The opposite mistake is total retreat. A few days of relative rest may help during a flare, but long stretches of doing almost nothing can reduce strength, stiffen joints, and increase fear around movement. The goal is not bedrest with better branding. It is the right amount of movement for the current problem.
Changing providers too fast without carrying forward useful information
Provider changes can be necessary, but constant resetting wastes time. Every new clinician needs the same story, the same symptom pattern, the same failed attempts, and the same hopes translated into new paperwork. If you do switch, carry forward what happened. Keep your timeline, medication list, imaging reports if you have them, and a brief summary of which exercises worsened or helped symptoms. Do not make memory do all the lifting.
Treating all pain flare-ups as proof that movement is dangerous
Some flare-ups mean the dosage was off. Some mean the movement choice was wrong. Some are temporary and manageable. The trick is not to romanticize pain, but not to catastrophize every response either. Many orthopedic problems live in the gray zone where careful adjustment matters more than dramatic interpretation.
Three quiet mistakes that cost people weeks:
- Testing painful movements repeatedly “to see if it’s still there”
- Adding multiple new treatments at once, then not knowing what caused what
- Ignoring function gains because pain has not dropped as fast as hoped
Do Not Do This: The Expensive Detours That Often Happen Next
Chasing back-to-back imaging before the clinical picture is clear
Imaging can be useful, but it is not always the best first move after PT stalls. Many scans show age-related changes, old wear, or dramatic-sounding findings that do not fully explain symptoms. A report can sound like a thunderstorm while your actual decision still depends on the exam, the symptom pattern, and whether results would change management. The American College of Radiology generally frames imaging around clinical appropriateness, not reassurance on demand. That is a good discipline to borrow.
Stacking treatments without a clear question each one is supposed to answer
Another common detour is stacking everything at once: more PT, massage, injections, braces, supplements, new shoes, new pillows, and a device with a suspiciously futuristic name. The problem is not that every one of these is useless. The problem is that none of them is being asked to answer a clear question. If you try five things at once, you may spend more and learn less. For some people, it also helps to compare pain management options before a cortisone injection rather than letting the next step happen by momentum alone.
Assuming surgery is the “serious” option and rehab is the “small” one
People sometimes assume surgery is the grown-up move when conservative care stalls. Sometimes surgery is appropriate. Sometimes it is not. Sometimes the better next step is a clearer diagnosis, a different rehab strategy, medication adjustment, or targeted imaging only if it would change treatment. “Serious care” is not a category defined by drama. It is care matched to the actual problem.
| Next step | What it can clarify | Common waste risk |
|---|---|---|
| Reassessment visit | Pattern, diagnosis fit, red flags, next question | Low, if you bring a useful timeline |
| Another PT block | May help if plan and dosage were the issue | Moderate, if repeated without adjustment |
| MRI or other imaging | Can clarify some diagnoses or surgical planning | Higher, if it will not change management |
| Injection consult | May reduce pain or help localize a pain source | Moderate, if used as a shortcut to avoid diagnosis questions |
Neutral action: Before booking anything, ask what question that step is supposed to answer.
What to Ask the Orthopedic Specialist When PT Is Not Working
What diagnosis are we actually treating, and what else could mimic it?
This may be the most important question in the entire article. Ask what diagnosis the team is treating right now, and what other conditions could look similar. Tendon pain, joint irritation, referred pain, nerve involvement, instability, inflammatory conditions, and overload patterns can overlap. If you do not know the working diagnosis, you cannot judge whether the plan still makes sense.
What findings would change treatment, and what findings would not?
This question is quietly excellent because it sharpens everything. If imaging, exam findings, or symptom changes would not alter treatment, that matters. If a specific finding would change the plan, that matters too. You are trying to separate curiosity from decision value.
What is the goal now: pain reduction, function, diagnosis, or surgical triage?
Not every visit has the same mission. Some visits aim to lower pain. Some aim to restore function. Some aim to sort diagnosis. Some are about determining whether surgery should even be discussed. Clarifying the goal prevents that strange clinical moment where everyone is nodding politely while secretly having four different conversations.
What to gather before comparing next-step options
- Your symptom timeline, including what changed over 2 to 6 weeks
- A list of PT exercises or approaches that worsened, helped, or did nothing
- Medication list, prior imaging reports, and daily function limits
- One or two clear goals, such as walking, sleeping, stairs, work tasks, or lifting a child
Neutral action: Put these notes on one page so the visit starts with facts instead of guesswork.
When Imaging Helps, and When It Mostly Adds Noise
Imaging is most useful when it will change management
Imaging is most useful when it answers a question that affects treatment. That may include persistent symptoms with neurologic findings, concern for a structural issue that changes management, pre-procedure planning, or situations where the diagnosis is uncertain after appropriate evaluation. In plain English, a scan earns its keep when it helps choose a better road, not just when it decorates the chart.
Many scans show age-related changes that may not explain symptoms
This is one of the quiet traps of modern care. Imaging can reveal degeneration, bulges, tearing, and wear that sound dramatic, especially in report language. But not every finding is the reason for your pain. Age-related changes can appear in people with very different symptom levels. That does not mean imaging is useless. It means interpretation matters, and context matters even more, especially in the familiar puzzle of MRI findings that do not match the pain.
Here’s the quiet trap: a dramatic report can distract from the real problem
I have seen people walk out of a scan discussion convinced they were “falling apart” because of one alarming phrase. Then a month later, the real issue turned out to be a different pain driver, a rehab mismatch, or a problem the report did not fully explain. A report is not a prophecy. It is one piece of the puzzle. Useful, sometimes essential, but still one piece.
Show me the nerdy details
The ACR Appropriateness Criteria often frame imaging around symptom pattern, neurologic findings, red flags, and whether results will change management. That logic is especially useful for persistent orthopedic pain because it reduces low-value testing while still making room for targeted evaluation when needed.
- Imaging can be valuable for diagnosis and planning
- Incidental findings are common
- Report language should be interpreted with the full clinical picture
Apply in 60 seconds: Write down one sentence to ask: “How would imaging change treatment in my case?”
If It Is Not Getting Better, What Other Paths Might Be Discussed?
Medication adjustments, activity modification, or a different rehab strategy
If the current path is not working, other reasonable options may include medication changes, activity modification, temporary workload reduction, bracing in selected cases, or a different rehab strategy with altered dosage, pacing, or focus. Sometimes the right next move is not brand-new care. It is better-aligned care. In some cases, a practical support choice such as HSA-eligible braces and supports can be part of that broader discussion.
Injection conversations: when they are used and what question they are trying to answer
Injections may come up. They can be used for pain relief, to reduce inflammation in certain situations, or occasionally to help clarify the pain source. But they should still answer a question. Are they meant to calm symptoms enough to resume rehab? Help localize where pain is coming from? Delay surgery? Support function during a work-critical period? Vague injections are like vague meetings. Something happens, but no one is quite sure why. If cost is part of the hesitation, it can help to look at a joint injection consultation cost framework before the visit.
Specialist referral, second opinion, or broader workup when symptoms do not fit cleanly
Sometimes symptoms simply do not fit neatly. When pain patterns are odd, when progress is absent, when neurologic signs appear, or when the diagnosis feels fuzzy despite treatment, a second opinion or a broader workup can be appropriate. That might involve orthopedics, sports medicine, physiatry, pain medicine, rheumatology, or another relevant specialist depending on the pattern. If your insurer pushes back, it may help to understand what to do after a denied second opinion for orthopedic pain.
Coverage tier map for next-step conversations
Tier 1: Reassessment and plan adjustment
Tier 2: Targeted rehab revision or home program redesign
Tier 3: Medication or injection discussion when clinically appropriate
Tier 4: Imaging when results would change management
Tier 5: Procedure or surgical evaluation if the clinical picture points there
Neutral action: Ask which tier your clinician believes you are in today, and why.
Infographic: The sane next-step ladder when PT is not helping
1. Pattern
No change? Partial change? Flare after sessions?
2. Function
Walking, stairs, sleep, work, lifting, sitting
3. Friction
Diagnosis clear? Dosage right? Home plan realistic?
4. Decision
Adjust rehab, seek reassessment, or order targeted imaging
Short Story: A reader once described six weeks of shoulder PT as “professionally disappointing,” which was funny only because it was so accurate. She had done almost everything right: showed up, tried the home program, avoided lifting, and even bought the extra band pack that always seems to arrive with the optimism of a small fitness cult. But her pain kept flaring after overhead work, and the exercises felt harder, not smarter. At follow-up, the most helpful moment was not a new treatment.
It was a better question. Her clinician asked what had actually changed. The answer was revealing: pain was no longer random, night pain was slightly better, and the biggest spike was tied to a specific reach pattern at work. That redirected the plan from generic strengthening to activity-specific modification and a different rehab tempo. Nothing magical happened overnight. But the next four weeks made more sense than the previous six, and that alone felt like oxygen.
When to Seek Help Sooner, Not Later
New numbness, weakness, instability, or rapidly worsening symptoms
Some symptoms should move the timeline forward. New weakness, progressing numbness, increasing instability, repeated giving-way, or rapidly worsening symptoms deserve timely medical review. Waiting longer is not always stoic. Sometimes it is just delay wearing a brave hat.
Fever, redness, marked swelling, or concern for infection or clot
Fever with worsening joint pain, redness, significant swelling, warmth, or concern for infection should not be brushed aside. The same goes for calf swelling, chest symptoms, or other signs that suggest a clot or a more urgent medical issue. Orthopedic pain can overlap with conditions that are not simple overuse problems.
Night pain, unexplained weight loss, or pain after significant trauma
Persistent night pain, unexplained weight loss, severe pain after significant trauma, and other concerning patterns warrant medical evaluation. These symptoms do not automatically mean something catastrophic is happening, but they are important enough to justify quicker attention. If back-related symptoms are part of the picture, readers sometimes benefit from a plain-language guide to when low back pain may be an emergency.
- Progressive neurologic symptoms deserve faster evaluation
- Infection or clot concerns are not “wait and see” territory
- Major trauma and severe escalation need prompt review
Apply in 60 seconds: If any red flag fits, stop optimizing and contact appropriate medical care now.
Next Step: Build a Smarter Follow-Up Visit
Bring a one-page symptom timeline with triggers, limits, and failed attempts
The best follow-up visits are not longer because of luck. They are clearer because the patient brings usable information. A one-page timeline is enough. Include when symptoms began or worsened, what PT involved, what changed, what did not, your main triggers, your biggest functional limits, and anything that briefly helped. This does not need to win an award for prose. It just needs to be legible and honest.
List what PT included, what worsened symptoms, and what briefly helped
Write the exercises or treatment types you remember, especially the ones that reliably flared symptoms or seemed to help. Add practical context. “Pain worse after stairs and after step-down drills” is useful. “Still hurts” is emotionally true and clinically underfed. The more concrete you are, the less likely the next visit will drift into generic advice.
One concrete action: book a reassessment visit and bring written notes, not memory alone
Here is the part that closes the loop from the beginning: when PT is not helping, the smartest next move is often not more willpower. It is a cleaner reassessment. Book the follow-up. Bring the notes. Ask what diagnosis is being treated, what would change the plan, and what the real goal of the next step is. That can happen in under 15 minutes of preparation, and it often saves far more time than it takes. If getting seen quickly is part of the problem, it can also help to understand typical orthopedic referral wait times or compare telehealth vs in-person orthopedics for your next follow-up.
Mini calculator: Is your next step worth it?
Count these three numbers:
- How many weeks since symptoms clearly improved?
- How many daily functions are still limited? Use 0 to 5.
- How many red flags are present? Use 0 or more.
If improvement has stalled for several weeks, daily limits remain high, or any red flags are present, reassessment usually makes more sense than repeating the same plan unchanged.
Neutral action: Use your numbers to explain urgency at scheduling.
FAQ
How long should physical therapy take before orthopedic pain starts improving?
It depends on the condition, severity, duration of symptoms, and how clearly the plan matches the diagnosis. Some people notice early improvement within a few weeks. Others improve more gradually. A lack of any meaningful change after several weeks, especially if the plan has been followed reasonably well, often justifies reassessment rather than passive waiting.
Is it normal for pain to get worse before it gets better in PT?
Mild temporary soreness can happen, especially when activity changes. But repeated major flares, increasing pain, spreading symptoms, or worsening function are different. Those patterns deserve discussion and often plan adjustment. “A little sore” and “I cannot trust my leg after each session” are not the same sentence.
Should I stop physical therapy if every session causes a flare?
Do not assume you must either push through or quit forever. Contact the treating clinician and describe the flare pattern clearly. Sometimes the answer is changing the dosage, exercise selection, frequency, or home program. Sometimes the answer is reassessment before continuing. The key is not to keep repeating a pattern that is clearly going badly.
When should I ask for an MRI or other imaging?
Ask when imaging would change management. That might include concerning neurologic findings, unclear diagnosis after evaluation, persistent symptoms that affect next-step decisions, or pre-procedure planning. Imaging is most useful when it answers a question that matters, not when it is used only to reduce uncertainty emotionally.
Can the diagnosis be wrong if PT is not helping?
Yes, that is possible. It does not mean someone was careless. Orthopedic pain patterns can overlap, and the first working diagnosis may need revision as symptoms evolve. That is why asking what diagnosis is currently being treated is so important.
What if physical therapy helped a little, then progress stopped?
That is a common pattern. Partial improvement followed by a plateau may mean you need a change in progression, activity modification, different exercise selection, or a closer look at what still limits function. A plateau is not the same thing as total failure.
Is surgery more likely if PT fails?
Not automatically. Some conditions do move toward surgical discussion when conservative care fails, but many do not. The right next step depends on the diagnosis, exam findings, function limits, symptom pattern, and whether other reasonable nonoperative options remain.
Should I get a second opinion from another orthopedic doctor?
A second opinion can be reasonable when the diagnosis is unclear, treatment recommendations conflict, symptoms do not fit neatly, or you want confirmation before more invasive care. It is most helpful when you bring organized records and a concise timeline so the second opinion starts from useful ground.
Can I keep exercising while I wait for my follow-up appointment?
Often some level of movement remains appropriate, but it should be matched to your symptoms and diagnosis. Avoid assuming total rest or total intensity is the answer. If a specific movement clearly worsens symptoms, stop treating that as a personality challenge and ask how to modify it safely.
What notes should I bring to make the next visit more useful?
Bring a one-page timeline, current medications, prior imaging if available, PT details, the main activities you still cannot do, and a short list of what worsened or helped symptoms. Also bring one or two goals that matter in daily life. “Walk 20 minutes without limping” is far more useful than “feel normal.”
The hook at the beginning was simple: stalled progress does not always mean you need more grit. Usually, it means you need better sorting. That is the real closing note here. The body is not a vending machine where you insert six weeks of effort and expect a tidy product drop. Sometimes the plan was right and the dosage was wrong. Sometimes the diagnosis needs another look. Sometimes imaging matters. Sometimes it mostly adds theater.
Your next useful step can happen today. Spend 10 to 15 minutes making a one-page symptom timeline, list what PT included, note what worsened symptoms, and book a reassessment visit with those notes in hand. That small act is often the moment the fog starts to lift.
Last reviewed: 2026-04.
