
Moving Beyond the Scan: Evidence-Based Pain Management
MRI often takes center stage too early. The more useful question is simpler: what is your body failing to do, and what would actually change the next decision?
“Pain alone is noisy. Function tells a cleaner story. A normal scan and a useful plan are not the same thing.”
Orthopedic care is less about chasing a machine and more about sorting symptoms, function loss, and red flags before the bill gets bigger than the answer. When pain lingers and X-rays are normal, every week of uncertainty feels like a tax on your life.
This guide helps you walk into your appointment with a sharper case: identifying pain patterns, documenting conservative care outcomes, and understanding when imaging truly adds value.
Start there. Then keep reading.
Table of Contents
- Describe what you cannot do, not just what hurts
- Sort urgency before chasing imaging
- Use treatment response as decision-making data
Apply in 60 seconds: Write one sentence that begins, “Because of this pain, I can no longer…”

Start With the Real Question, Not the Scan
An MRI is a tool, not a treatment plan
An MRI is powerful because it can show soft tissues, nerves, discs, cartilage, tendons, ligaments, and other structures that ordinary X-rays may not show well. But a picture is not a plan. A clear-looking image can still leave the real treatment question fuzzy. An alarming-looking image can also send people sprinting toward the wrong conclusion.
I have watched this happen in ordinary life more times than I care to count. Someone says, “I just need the scan.” What they usually mean is, “I need this uncertainty to stop chewing on me.” Fair. Pain is bad enough. Uncertainty is pain’s overly talkative cousin.
The American Academy of Orthopaedic Surgeons explains that MRI is useful for evaluating soft tissues, while X-rays remain better for many bone questions. That does not make MRI the automatic first move. It makes it the right move when the clinical question matches the tool. (orthoinfo.aaos.org)
The better first question is what your clinician is trying to confirm or rule out
A better opening question is usually this: what are we trying to confirm, exclude, or change with imaging? Are you trying to distinguish tendon injury from bursitis? Disc irritation from muscular back pain? Instability after shoulder trauma? Labral damage in the hip? A scan has value when it helps separate those branches.
If the answer would not change treatment, timing, or referral, MRI may simply arrive early to the party and eat the budget. That is not a scandal. It is just common. In US care, imaging decisions often live inside a triangle made of symptoms, physical exam, and what treatment would happen next. If you are already stuck at the “scan or no scan” stage, a more focused guide on when an MRI referral for orthopedic pain actually makes sense can help narrow the logic.
Pain alone does not always tell you which test comes first
Pain severity matters, but it is not the whole map. Two people can rate pain as 8 out of 10 and need very different next steps. One may have severe muscle spasm with no dangerous signs. Another may have weakness, numbness, or loss of reflexes that changes urgency. The difference often lives in pattern, not volume.
Useful framing: pain tells you something is wrong; pattern tells you where to look; function tells you how much it matters right now.
Show me the nerdy details
In musculoskeletal care, imaging is most useful when pretest probability is sharpened first. The more specific the symptom pattern and exam findings, the more likely an MRI result will be clinically actionable rather than merely descriptive.
Why “Get an MRI” Feels Logical but Often Starts Too Early
When pain drags on, imaging can feel like control
Persistent pain makes people hungry for certainty. That is not weakness. It is a rational response to feeling stuck. You rest. You stretch. You ice. You try to sleep like a folded lawn chair. Three weeks later, you are still bargaining with your shoulder while putting on a sweater. Of course imaging starts to look like control.
But control and progress are not always the same thing. Sometimes the most controlling move is not ordering a scan. It is sharpening the question so the next visit is more efficient.
Early scans can reveal findings that look alarming but do not explain symptoms
This is where people get ambushed. MRI can find real structural changes that are not the true cause of the current pain. Bodies are living biographies, not showroom floors. By adulthood, many knees, backs, and shoulders have a few plot twists. If those findings do not line up with symptoms and exam findings, they can distract more than they help. If that mismatch is exactly what is haunting you, read more about when MRI findings and pain do not line up cleanly.
That is one reason evidence-based imaging frameworks exist. The American College of Radiology publishes appropriateness criteria to help clinicians match imaging to clinical scenarios rather than reflexively scanning every painful region. (acr.org)
The hidden cost is not just money. It is what the wrong starting point can set in motion.
The obvious cost is the bill. The less obvious costs are harder: delayed treatment, insurance denials that waste weeks, follow-up testing on incidental findings, and a visit that turns into a debate about pictures instead of function. Sometimes patients leave with more data and less clarity. That is a rotten trade.
Decision card: When symptoms are stable, non-traumatic, and not accompanied by serious neurologic or systemic signs, a structured exam and early conservative care often beat a rushed MRI for decision quality.
When A: stable pain, still functional, no red flags. When B: major trauma, progressive weakness, bowel or bladder change, infection concern, cancer concern. Trade-off: A may save cost and improve diagnostic focus; B may justify faster escalation.
Neutral next step: Match your current symptoms to one of those two paths before the appointment.
Who This Is For and Not For
Best for adults with ongoing joint, back, neck, shoulder, knee, hip, or soft-tissue pain who are still functioning but unsure about next steps
This guide is for the person who can still get through the day, technically, but everything feels narrowed. You can work, but sitting is a negotiation. You can climb stairs, but your knee sends a little legal threat with each step. You can reach overhead, but your shoulder behaves like it has opinions.
It is especially useful if you are trying to understand whether primary care, sports medicine, orthopedics, or physical therapy makes sense first, and whether MRI belongs now, later, or only if the picture changes. If that choice itself feels muddy, a comparison of urgent care versus an orthopedic clinic can make the first stop clearer.
Especially useful if you already had basic evaluation, rest, medication, or an X-ray and still feel stuck
If you already tried the first layer of care and nothing is moving, that does not automatically mean “MRI next,” but it does mean the conversation should become more specific. What was tried? For how long? Did it help a little, not at all, or only until you resumed activity? That history matters.
Not for severe trauma, rapidly worsening weakness, loss of bowel or bladder control, fever with severe pain, or other urgent red-flag scenarios
This guide is not a substitute for urgent evaluation when serious red flags are present. In low back pain guidance, the American College of Radiology identifies scenarios such as suspected cauda equina syndrome, infection, or cancer concern as situations where MRI may be appropriate much earlier. (acsearch.acr.org)
Eligibility checklist:
- Yes: pain has lasted days to weeks and you are unsure what the next sensible step is
- Yes: you can describe what movements fail or flare symptoms
- Yes: you want a cost-aware plan, not just more testing
- No: severe trauma, sudden major weakness, bowel or bladder changes, fever with severe pain, or rapidly worsening symptoms
Neutral next step: If you checked “No,” use urgent medical evaluation rather than an article-driven self-triage loop.
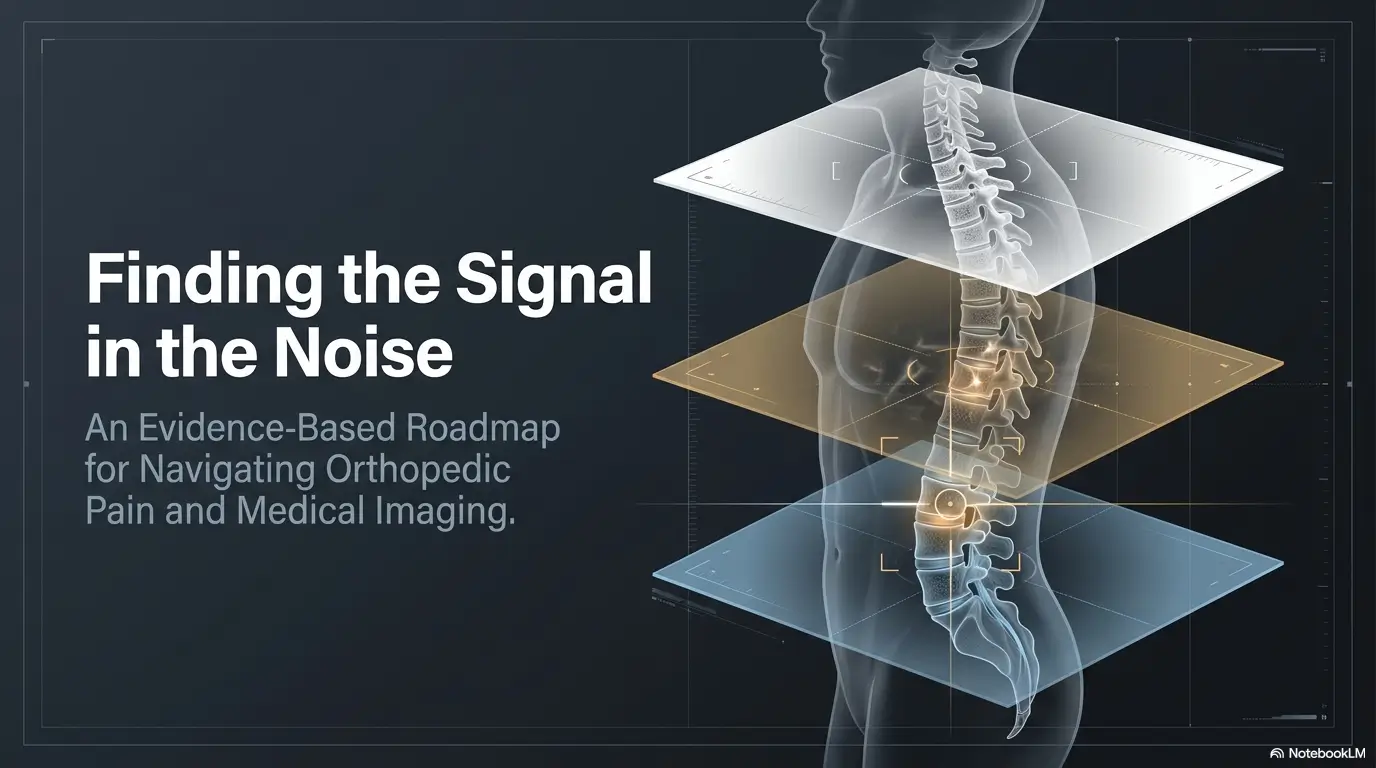
First Sort the Pain Pattern Before You Sort the Imaging
Mechanical pain, nerve-type pain, inflammatory pain, and post-injury pain do not point to the same next move
Before imaging, sort the pain pattern. Mechanical pain often changes with movement, load, posture, or repeated activity. Nerve-type pain may shoot, burn, tingle, or travel along a path. Inflammatory pain may come with morning stiffness, swelling, heat, or pain that seems strangely disconnected from simple mechanics. Post-injury pain adds timing and mechanism to the puzzle. Twist? Fall? Sudden pull? Collision?
When people skip this step, every ache becomes “maybe I tore something.” Sometimes they did. Sometimes they are dealing with referred pain, overload, irritation, or a nerve issue that needs a different lane entirely.
Function loss matters as much as pain intensity
Clinicians often learn more from “I cannot lift a pan onto the stove” than “it really hurts.” Function loss sharpens the case. It helps distinguish discomfort from impairment. It also helps decide which specialist, which exam maneuvers, and which imaging, if any, would answer something useful.
I once had a nagging shoulder episode where pain ratings were vague and dramatic in alternating shifts, but the real clue was boring: I could not smoothly reach the back seat of the car. That one movement said more than my entire theatrical monologue.
Duration changes the decision tree more than many patients realize
How long symptoms have lasted matters because short-lived flare-ups often behave differently from persistent or progressive problems. A pain story at day 3 is not the same story at week 6. In some back-pain scenarios, the ACR criteria indicate MRI becomes more appropriate after persistent symptoms and failed conservative management, especially if intervention or surgery is being considered. (acsearch.acr.org)
- Mechanical pain behaves differently from nerve pain
- Function loss gives the visit diagnostic traction
- Persistence changes the imaging conversation
Apply in 60 seconds: Write three labels beside your symptoms: pattern, function loss, and duration.
Red Flags First: When an MRI Conversation Becomes More Urgent
Sudden neurologic changes, major trauma, suspected infection, or suspected fracture need faster escalation
There is a world of difference between stubborn pain and dangerous pain. If you develop major weakness, foot drop, saddle numbness, loss of bowel or bladder control, or severe symptoms after major trauma, the clock starts ticking differently. The same goes for suspected fracture, serious infection, or rapidly worsening neurologic changes.
In those settings, imaging is no longer a casual consumer choice. It becomes part of urgent decision-making.
Night pain, unexplained weight loss, fever, or cancer history can change the imaging timeline
These are the kinds of details people sometimes leave out because they seem unrelated or overly dramatic. Do not leave them out. Fever, unexplained weight loss, immune suppression, steroid exposure, cancer history, or persistent night pain can move the clinical reasoning away from “let’s watch and wait” and toward earlier imaging or broader workup. Again, not because every case is a disaster, but because missing the wrong case is costly. For spine-related panic points, a separate review of cauda equina red flags that require urgent action is worth having in your back pocket.
This is the line in the sand: persistent pain is one thing, dangerous pain is another
This distinction is worth memorizing. Persistent pain says, “Investigate me thoughtfully.” Dangerous pain says, “Escalate me now.” When people blur those categories, they either panic unnecessarily or delay care they should not delay. Neither option is charming.
Red flag snapshot:
- Major trauma or suspected fracture
- Rapidly worsening weakness or major numbness
- Bowel or bladder changes with spinal symptoms
- Fever, infection concern, or unexplained systemic symptoms
- Cancer history with new concerning pain pattern
Before the Referral: What a Good Orthopedic Workup Should Clarify
Where the pain starts, where it travels, and what movement changes it
A strong orthopedic workup starts with geography. Point with one finger where the pain begins. Then describe where it travels. Then explain which motion, load, position, or time of day changes it. That sounds almost embarrassingly simple. It is also where the visit gains precision.
“My leg hurts” is a shrug. “Pain starts in the right buttock, shoots to the calf after ten minutes of standing, eases when I sit, and my foot feels tingly by evening” is diagnostic gold by comparison.
What makes symptoms better, worse, sharper, weaker, or unstable
Clinicians are not being nosy when they ask what helps or worsens symptoms. They are sorting mechanisms. Better with rest but worse with overhead reaching? Different clue. Worse with coughing or sneezing? Different clue. Feels unstable when pivoting? Different clue again.
What the physical exam may answer before imaging does
A good physical exam can often narrow the field before any scan enters the room. Strength testing, reflexes, range of motion, provocative maneuvers, gait, instability tests, and palpation are not decorative. They shape what the next step should be. Sometimes they even tell you which MRI protocol would matter, or whether a different study is more useful.
Quote-prep list: Bring these before comparing doctors or clinics.
- Exact pain location and where it travels
- Three movements that worsen symptoms
- Two activities you can no longer do normally
- Past treatments and whether each helped, failed, or partially helped
- Any red flags, even if they seem awkward to mention
Neutral next step: Put that list in your phone notes so you do not improvise under fluorescent lighting.
Midway through this process, it helps to read a patient-facing overview from an orthopedic source that explains how X-rays, CT scans, and MRI differ in what they show.
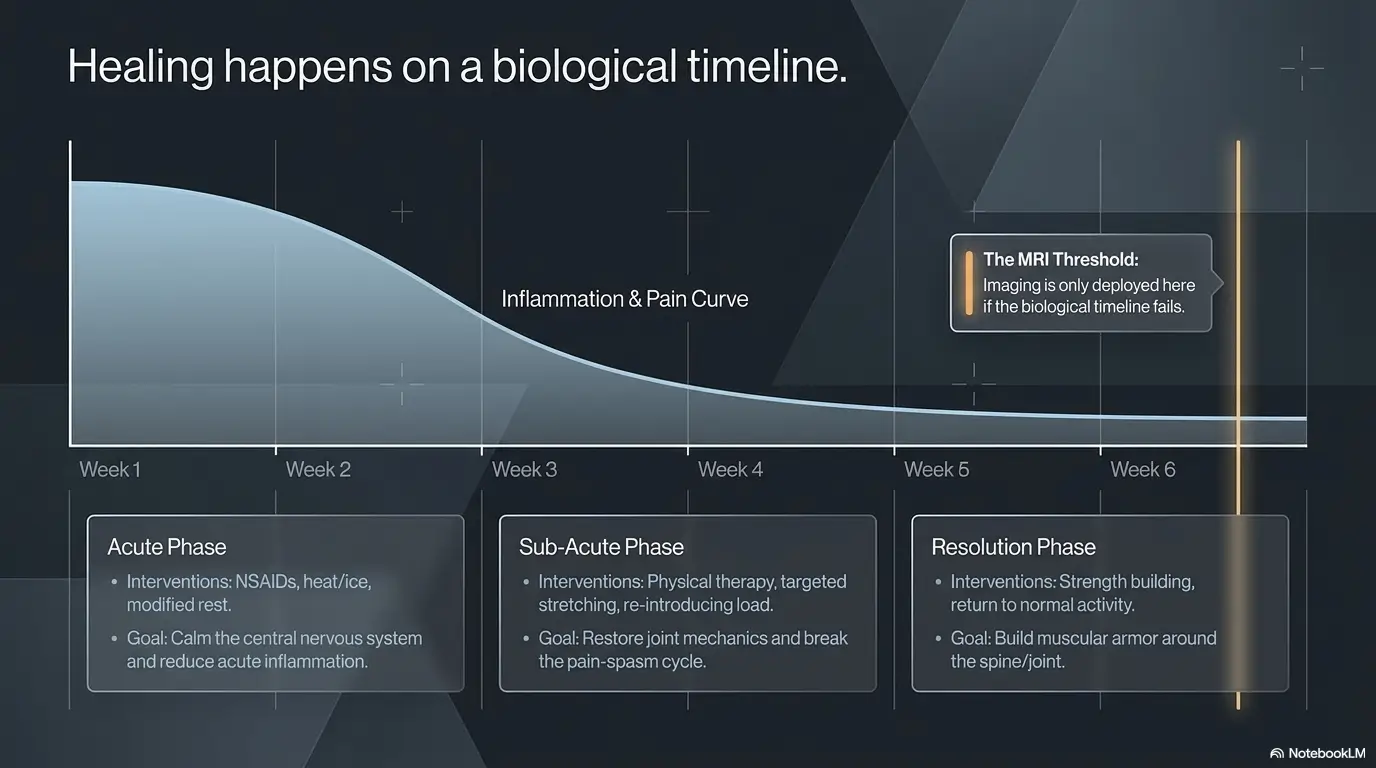
Don’t Skip This: Conservative Care Still Counts as Data
Relative rest, targeted physical therapy, medication trials, and activity changes can help reveal the source
Conservative care is often misheard as “do nothing.” It is not nothing. It is a diagnostic experiment with a therapeutic goal. Relative rest, guided exercise, targeted physical therapy, a brief medication trial, load modification, and sleep-position changes can reveal what kind of problem you are dealing with. If symptoms improve with a targeted rehab plan, that information matters. If they do not, that also matters.
In real life, this is the part many people resent because it feels less dramatic than a machine. Yet it is often the part that saves the specialist visit from becoming vague and expensive. If you need language for that stage, this companion piece on what counts as failed conservative care before MRI can help you document it more clearly.
A failed conservative step is still useful information when it is specific and documented
“Tried PT, didn’t work” is less helpful than “Completed four weeks focused on scapular stability and range of motion, pain at rest improved, overhead weakness unchanged.” Specificity helps clinicians decide whether the treatment was mismatched, too short, helpful but incomplete, or a clue that imaging now has more value.
Here’s what no one tells you: a thoughtful trial can make the later MRI more meaningful
This is the strange mercy of conservative care. It can turn a later MRI from a general fishing trip into a much more targeted answer. For back pain, evidence-based guidance often reserves MRI for persistent symptoms, suspected nerve involvement, or treatment decisions like injections or surgery. (acsearch.acr.org)
Examples of conservative care as data:
- Symptoms improve with unloading or posture change
- Night pain persists despite rest
- Strength improves but instability remains
- Medication blunts pain but numbness progresses
Show me the nerdy details
Response to conservative care helps refine differential diagnosis and influences imaging yield. If pain improves with a specific rehab pattern, the pretest probability for certain structural lesions may fall. If neurologic deficits persist or progress, the threshold for imaging rises.
Common Mistakes People Make Before Asking for MRI Referral
Mistaking longer pain for automatic imaging necessity
Longer pain matters, but time alone does not decide imaging. A quiet six-week overuse pattern without red flags is different from a two-day crisis with neurologic changes. Duration matters inside context. It is not a magic spell.
Asking for the scan before describing the function problem clearly
This is one of the most common own-goals in the exam room. People lead with “I think I need an MRI” before explaining what changed in their body and life. That puts the conversation on rails too early. A clinician cannot judge the value of imaging until they understand the functional problem.
Treating a normal X-ray or a painful flare as the whole story
A normal X-ray does not erase soft-tissue, nerve, cartilage, or certain inflammatory issues. The AAOS notes that MRI provides better soft-tissue images than X-ray, which is exactly why a normal X-ray does not end the story, but also why the next question still matters. (orthoinfo.aaos.org)
Let’s be honest: many people can describe the pain, but not what they can no longer do
This sounds almost rude, but it is clinically useful. Many patients can narrate pain beautifully and function vaguely. Reverse that ratio. The sharper you are about lost function, the smarter the MRI decision becomes.
- Time alone does not justify a scan
- Normal X-ray does not equal no problem
- Function loss often speaks louder than pain adjectives
Apply in 60 seconds: Replace “I need an MRI” with “I need help because I can no longer…”
The Referral Trap: When “I Need an MRI” Becomes the Wrong Conversation
Why clinicians respond better to a change in function than a request for a specific test
Clinicians generally respond better to a problem statement than a test request because problems can be reasoned through, while test requests can be too narrow or too early. “My left leg becomes weak after walking one block, and I now avoid stairs” gives them something to evaluate. “Can you order an MRI?” gives them a utilization question before a clinical one.
That does not mean you must tiptoe or be passive. It means your strongest case is usually functional, not technological. When the visit stalls anyway, some patients find it useful to review what to do after a denied second opinion for orthopedic pain so they can move forward without losing momentum.
How to explain your symptoms in a way that sharpens decision-making
Use a simple four-part structure:
- Where the pain is and whether it travels
- What movements or situations trigger it
- What function you lost
- What you already tried and what changed
That structure keeps the visit from turning into a fog machine.
Better questions to ask than “Can you order an MRI?”
Try questions like these instead:
- What are you trying to rule out here?
- Would imaging change treatment right now?
- What findings on exam make MRI more or less useful?
- What should happen first if we are not imaging yet?
- What would make you reconsider imaging sooner?
Short Story: A friend of mine once went into a sports medicine visit absolutely convinced she needed an MRI for knee pain. She had rehearsed the speech on the drive over, the way people rehearse imaginary courtroom scenes in the shower. But once the visit started, the doctor asked one irritatingly good question: “What can’t you do now that you could do a month ago?” That changed everything.
She stopped talking about “pain” in the abstract and started talking about stairs, pivoting, and that weird half-second buckle when turning quickly. The exam suddenly made more sense. An X-ray ruled out one issue, rehab was adjusted, and the MRI moved from emotional wish to conditional next step. She did end up getting imaging later, but by then it answered a real question. Same machine. Better timing. Better visit. Less panic tax.
Cost-Aware Care: How to Avoid Paying for a Scan That Does Not Change the Plan
Insurance approval, prior authorization, and step-therapy rules often shape timing
In the US, MRI timing is not just a medical question. It is also an administrative one. Many plans want documented symptoms, exam findings, prior treatment attempts, or a specific duration before approval. This can be maddening, but pretending it does not exist does not help. Cost-aware care means understanding the system you are actually in, not the one you wish existed. For readers staring down deductibles and sticker shock, it also helps to compare how to estimate imaging costs under an HDHP before the order is ever placed.
The most useful MRI is the one that answers a live treatment question
A “live treatment question” means the result would change something now: referral type, injection planning, surgical decision-making, rehab direction, or urgency. If the answer would be “do the same thing regardless,” the scan may be early or low-yield.
A cheaper earlier step can sometimes improve the specialist visit more than imaging alone
Sometimes the better spend is a focused evaluation, a high-quality PT assessment, or the right specialist rather than the first available scan. A good visit can narrow what needs imaging. A random scan cannot always rescue a vague visit. That is especially true when you are balancing symptoms against out-of-pocket spending under a high-deductible orthopedic pain management plan.
Mini calculator: Estimate whether your MRI request is answering a live question.
- Input 1: Do you have a new or worsening function loss? yes or no
- Input 2: Have you tried a documented first-line step? yes or no
- Input 3: Would the result change treatment now? yes or no
If you answered “yes” to two or three, the MRI discussion may be more mature and more likely to be useful. If you answered “yes” to zero or one, the visit may need better sorting first.
Neutral next step: Bring those three answers into the appointment.
| Care step | Typical role | Cost logic | Notes |
|---|---|---|---|
| Focused clinical exam | Clarifies pattern, function, urgency | Often the highest-value first spend | Improves imaging decisions |
| X-ray | Bone alignment, fracture, arthritis clues | Often cheaper and faster | Can be normal even when pain is real |
| MRI | Soft tissue, nerve, disc, cartilage detail | Higher cost and authorization friction | Best when result changes treatment |
Body-Part Reality Check: Why Knees, Shoulders, Backs, and Hips Do Not Follow One Script
Back pain decisions often turn on nerve symptoms and red flags
Back pain has its own logic. If there are no red flags and no concerning neurologic findings, early imaging may not help much. If there is persistent radiculopathy, progressive weakness, or concern for serious causes, the threshold changes. The ACR low back pain criteria reflect this kind of scenario-based decision-making rather than a blanket “scan if it hurts.” (acsearch.acr.org)
Shoulder pain may depend on weakness, trauma, instability, or failed rehab
Shoulders are theatrical. They click, catch, ache at night, and make shirts feel like engineering problems. But not all shoulder pain means the same thing. Weakness after trauma, instability, persistent night pain, or failure to improve with directed rehab may point the conversation toward imaging differently than simple overuse pain. AAOS patient education notes that MRI can show soft-tissue problems in the shoulder, and in some labral situations an MRI arthrogram may be considered. (orthoinfo.aaos.org)
Knee and hip pain may need a different mix of exam findings, X-ray results, and treatment response
Knees and hips often need a mix of history, exam, and plain films before MRI earns its keep. Locking, instability, traumatic twisting, failure to bear weight, or persistent mechanical symptoms can change the picture. Hip pain may involve joint, labral, tendon, or referred pain pathways that are not obvious at first glance. AAOS explains that MRI can better show cartilage and labral damage in certain hip conditions, but again, only after the question is clear. (orthoinfo.aaos.org)
- Back pain often turns on nerve signs and red flags
- Shoulders care about weakness, instability, and trauma context
- Knees and hips often need pattern plus mechanics, not just a picture
Apply in 60 seconds: Write the one body-part-specific problem that bothers you most, such as instability, numbness, or locking.
What to Bring to the Visit So the MRI Decision Gets Smarter
Timeline of symptoms, prior injuries, treatment attempts, and what changed
Bring a timeline. It does not need to be elegant. A phone note is enough. Include when symptoms began, whether there was an injury, what you tried, what improved, and what worsened. Add dates if you can. Not because dates are romantic. Because memory gets weird in exam rooms.
Specific movement losses such as walking, lifting, reaching, sleeping, bending, or climbing stairs
List the concrete tasks that changed. Think walking distance, overhead reaching, turning in bed, sitting tolerance, lifting, typing, carrying groceries, stairs, or sports. That list is often more valuable than a polished speech about pain intensity.
A short symptom log can outperform a vague memory in the exam room
A symptom log is quietly powerful. It captures flares, triggers, time of day, radiation, numbness, weakness, and treatment response. It also keeps you from leaving the visit and realizing you forgot the one detail that mattered. When delays are part of the stress, it may also help to plan around typical orthopedic referral wait times so your notes stay useful by the time the appointment arrives.
Coverage tier map:
- Tier 1: symptoms, exam, no major red flags, first-line care still in play
- Tier 2: persistent symptoms, documented treatment attempts, function loss becoming clearer
- Tier 3: progressive deficits, intervention planning, or strong concern for structural pathology
- Tier 4: urgent scenarios such as major neurologic change, fracture, infection, or cancer concern
Not every insurance plan uses these exact words, but this is the practical logic many patients encounter.
Neutral next step: Figure out which tier your situation most closely resembles.
Infographic: A practical MRI decision path
1. Start
Where is the pain? What function changed? How long has it lasted?
2. Sort urgency
Any red flags such as major weakness, trauma, fever, or bowel or bladder change?
3. Match first step
Exam, X-ray, PT, medication trial, sports medicine, or orthopedics.
4. Reassess
If symptoms persist, progress, or treatment decisions depend on it, MRI becomes more meaningful.
FAQ
Do I need an MRI if the pain has lasted more than a few weeks?
Not automatically. Duration matters, but the next step depends on pain pattern, function loss, red flags, prior treatment attempts, and whether imaging would change management now. Persistent symptoms can make MRI more reasonable in some scenarios, but “a few weeks” alone is not a universal trigger.
Can an orthopedic doctor refuse to order an MRI?
Yes. More accurately, they may decide it is not the best next step yet. That is not necessarily dismissal. It may reflect clinical reasoning, insurance requirements, or the belief that exam findings and first-line treatment should come first. Ask what question they are trying to answer and what would make MRI more useful later.
Is physical therapy supposed to happen before MRI?
Often, yes, depending on the body part and the symptoms. Physical therapy is not just treatment. It can also function as diagnostic information. A meaningful response or failure to respond can sharpen later imaging decisions. If coverage is the practical snag, a quick review of how Medicare Part B handles physical therapy may save you from guessing.
What if my X-ray was normal but the pain is still strong?
A normal X-ray does not rule out many soft-tissue, nerve, cartilage, or certain inflammatory problems. MRI may become relevant if the symptom pattern and exam findings suggest an issue X-ray cannot show well. The key is matching the scan to a real clinical question rather than treating normal X-ray as the last word.
Will insurance deny an MRI if I have not tried conservative treatment?
It can happen. Many plans require symptom duration, exam findings, and prior treatment attempts before approving advanced imaging, especially when there are no urgent red flags. This is one reason documentation matters so much. If denial has already happened, you may want the next layer of strategy in what to do after an MRI denial appeal in orthopedic pain management.
What symptoms make MRI more urgent?
Major or progressive weakness, bowel or bladder changes with spine symptoms, severe trauma, suspected infection, suspected fracture, cancer-related concern, or rapidly worsening neurologic findings can raise urgency. Those situations belong in urgent medical evaluation, not slow self-navigation.
Is it better to see primary care, orthopedics, or sports medicine first?
It depends on the symptom pattern and access. Primary care can be excellent for first sorting, initial treatment, and referral coordination. Sports medicine often shines with activity-related injuries and nonoperative management. Orthopedics may be especially useful when structural questions, instability, trauma, or potential procedures enter the picture.
Can MRI findings be unrelated to the pain?
Yes. Imaging can show structural findings that are real but not the main reason for current symptoms. That is why MRI works best when read in the context of a focused history and physical exam rather than as a stand-alone oracle.
Next Step: Use a One-Page “Why I Need Further Evaluation” Summary
Write down where the pain is, what function you lost, what you tried, and what changed
If you do nothing else after reading this, make this one-page summary. It can be messy. It can be blunt. It just needs to be usable. Include:
- Exact pain location and whether it radiates
- Main functional loss
- Triggering and relieving factors
- Red flags or absent red flags
- Treatments tried and response
- What has worsened, improved, or stayed stubbornly identical
Bring the summary to your appointment so the conversation starts with evidence, not frustration
That summary does something beautiful to a medical visit: it shortens the distance between your lived experience and the clinician’s reasoning. It reduces rambling. It reduces forgotten details. It reduces the temptation to lead with “Please just order the MRI” because you finally have a cleaner way to show why more evaluation may be needed.
The goal is not to demand a scan. It is to make the next decision harder to get wrong
That is the whole game. Better decisions, not louder requests. Once the summary is in hand, the MRI question becomes less emotional and more operational. That is where patients usually do better.
- It organizes symptoms into decision-ready language
- It highlights what has actually changed
- It makes MRI a question of fit, not desperation
Apply in 60 seconds: Start a note titled “Why I Need Further Evaluation” and add four bullet points.
If you want a plain-language government overview of what MRI is, how it works, and what to mention before a scan, MedlinePlus is a useful final-read resource.
If your main concern is back pain and whether imaging is actually appropriate in different scenarios, the American College of Radiology criteria are one of the clearest evidence-based references available.
Conclusion
The hook at the beginning was simple: the MRI feels like the door with the answer behind it. Sometimes it is. Often it is only a room in the house, and not even the first room you should enter. Orthopedic pain management before asking for MRI referral works best when you slow the instinct to chase the machine and instead sharpen the clinical question. That is not less proactive. It is more strategic. If you want a broader framework beyond this one article, you can also continue with a fuller guide to orthopedic pain management decisions.
Within the next 15 minutes, make your one-page summary. Write where the pain is, what you cannot do, what you tried, and what changed. Then bring that to the appointment. The aim is not to win an argument for imaging. The aim is to make the next medical decision cleaner, faster, and less likely to waste your time.
Last reviewed: 2026-04
