
Beyond the Normal X-Ray
A normal X-ray can save time, money, and panic, but it can also send people down the wrong hallway. Orthopedic pain management when an X-ray is normal but pain continues is rarely about proving the pain is real. It is about figuring out what the first image could not show.
This is the frustrating middle ground many adults know too well: the scan looks fine, but the knee still catches on stairs, the shoulder still hurts at night, or the back pain still travels where it should not. Soft-tissue injury, nerve irritation, referred pain, inflammation, and load-related problems do not always announce themselves on plain films.
Keep guessing too long, and the price is not just discomfort. It is lost function, stalled recovery, and the common mistake of returning to activity before the body is ready.
Fast Answer: Orthopedic pain management when X-ray is normal but pain continues usually means the problem needs better sorting, not instant panic. A normal X-ray can miss soft-tissue injury, nerve irritation, inflammation, overuse problems, or pain referred from somewhere else. The next step is to match the pain pattern, function changes, duration, and red flags to a more targeted plan instead of assuming “nothing is wrong.”
Table of Contents
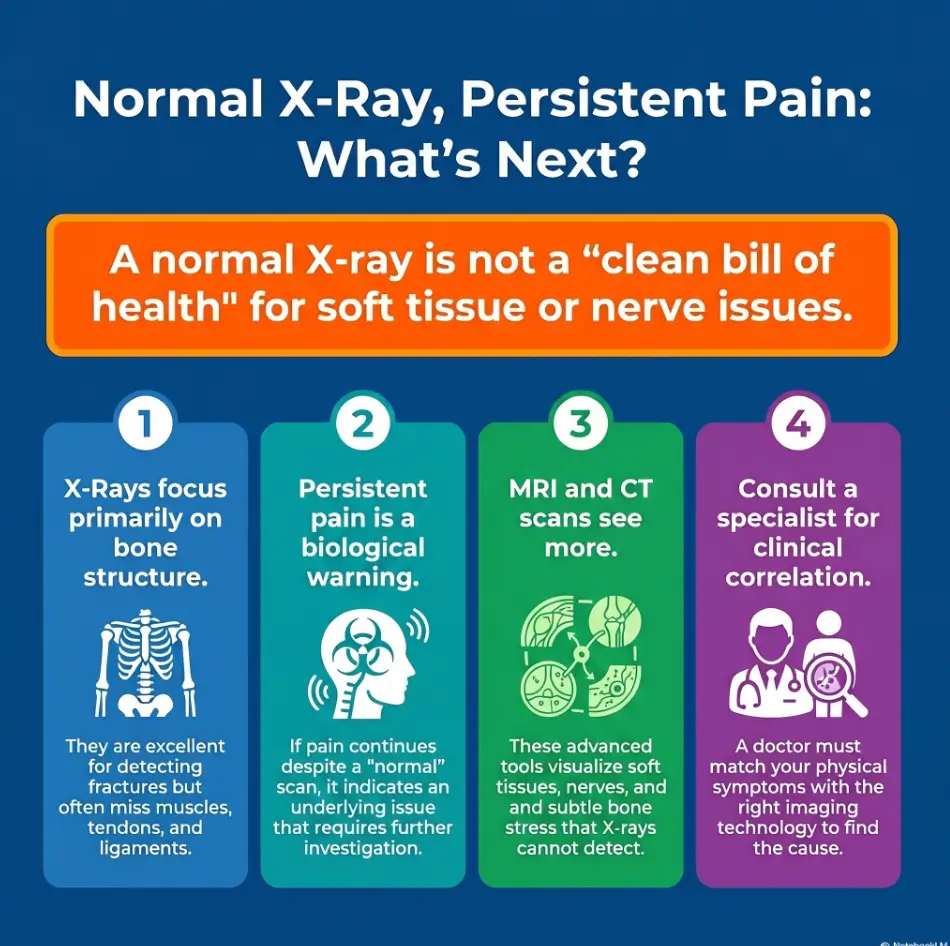
Start Here: What a Normal X-Ray Does and Does Not Rule Out
A normal image can exclude some bone problems without explaining the pain
X-rays are good at showing certain bone issues, alignment changes, some fractures, and some arthritis patterns. That matters. It is not nothing. But it is also not the whole orchestra. If your pain is coming from tendon, ligament, labrum, cartilage, disc, nerve irritation, or certain early stress injuries, the first image may look reassuring while your body keeps filing complaints.
This is where many people get emotionally stranded. They hear “normal” and translate it as “imagined.” Those are not the same sentence. A normal X-ray can mean, very usefully, that some urgent bony explanations are less likely. It does not automatically explain why your shoulder still catches, your knee still buckles on stairs, or your back pain still shoots down a leg when you bend to tie a shoe. In spine cases especially, the mismatch between symptoms and plain films often sounds a lot like the concerns people raise in sciatica MRI versus X-ray decisions.
Why soft tissue, nerve, and inflammatory issues often live outside the X-ray frame
AAOS patient guidance explains that MRI is designed to show soft tissues more clearly than plain X-ray, and that simple X-rays can be normal even when a rotator cuff problem or labral issue exists. The American College of Radiology also builds its imaging pathways around the idea that persistent symptoms after normal radiographs sometimes justify a different test, depending on the body part and the suspected problem.
That sounds technical, but the practical version is easy: the test has to match the question. An X-ray answers some questions beautifully. It answers others with the elegance of a toaster trying to perform violin.
The real question is not “Is it normal?” but “What was this test able to see?”
That one shift changes everything. Instead of asking whether the picture was normal in the abstract, ask what the test was actually built to show. Once you do that, the next step becomes less emotional and more strategic. You are not demanding “more tests because I’m worried.” You are asking whether the current symptoms fit what the first test can reasonably rule out. If that conversation is already moving toward advanced imaging, it can help to understand when an MRI referral for orthopedic pain starts making practical sense.
- It may lower concern for some bone problems
- It may miss soft-tissue or nerve-related causes
- The next step depends on the symptom pattern, not pride in the first image
Apply in 60 seconds: Write one sentence: “My X-ray was normal, but my main unresolved problem is ______.”
Who This Helps and Who Needs a Faster Medical Escalation
Best for adults with ongoing joint, back, neck, shoulder, knee, hip, wrist, or foot pain after initial imaging
This guide is for the common, messy middle. You had an injury, flare, overuse problem, or nagging pain. You got checked. You may even have been told to rest, ice, take something over the counter, and circle back if it lingers. Now it is lingering. Or stalling. Or acting polite until you try to live a normal life again.
If that is your situation, good. Not good that you hurt, obviously. Good that this is the part of the road where careful observation helps. This is where better symptom descriptions, smarter follow-up questions, and a less magical view of imaging can save weeks of wandering. If the delay itself is becoming part of the problem, readers often find it useful to understand what orthopedic referral wait times can realistically mean for care planning.
Not for chest pain, major trauma, fever with severe pain, sudden weakness, or loss of bladder or bowel control
Some situations move out of the “let’s think this through” category and into urgent re-evaluation. Severe trauma, a joint that looks deformed, rapidly worsening weakness, new numbness with loss of control, inability to bear weight after injury, fever with severe localized pain, or symptoms that suggest a neurologic emergency deserve prompt medical attention. MedlinePlus and emergency guidance from major health organizations consistently treat those patterns as escalation territory, not wait-and-see territory.
If the pain story is changing fast, this stops being a routine follow-up article
Many readers need permission to stop being stoic. If your body is changing faster than your calendar can explain, this is not the moment to win an award for quiet endurance. People often confuse patience with virtue. In medicine, timing matters. Waiting can be wise. Waiting can also be a traffic jam in nicer clothing. For low back symptoms with red flags, this kind of shift starts to resemble the concerns covered in low back pain emergency warning signs, not a routine follow-up question.
Eligibility Checklist: Is this a routine follow-up problem or a faster-escalation problem?
- Yes: Pain is persistent but stable, and you can still function somewhat.
Next step: prepare a targeted follow-up visit. - No: Pain is rapidly worsening, severe, or paired with major neurologic symptoms.
Next step: seek urgent medical evaluation. - No: The joint is visibly deformed, very swollen, or you cannot bear weight after injury.
Next step: do not rely on article advice alone.
Neutral action: Sort your symptoms into “stable” versus “changing fast” before you decide what kind of care to seek.
Pain That Lingers Has a Pattern: What the Timeline May Be Telling You
Pain that improves slowly is different from pain that stalls, spreads, or sharpens
Duration is not everything, but it is not wallpaper either. A problem that is slowly improving over 2 to 3 weeks may call for one conversation. A problem that plateaus, spreads, or becomes more mechanically dramatic may call for another. “Still hurts” is useful only up to a point. Clinicians need the shape of the story, not just the fact that the story exists.
If you have ever tried to explain pain from memory, you know the problem. Monday felt terrible. Wednesday was almost okay. Friday stairs became a personal enemy. By the time you sit in the exam room, the brain hands over one vague sentence and a shrug. That is not because you are careless. It is because pain is slippery, and memory edits for drama.
What two weeks, six weeks, and three months can signal in real-world care decisions
There is no sacred calendar page where pain becomes legitimate. Still, timelines matter. Around 2 weeks, many people are still learning whether a mild strain or flare is calming down. Around 6 weeks, persistent limitation may matter more, especially if home care or therapy is not moving the needle. By 3 months, “ongoing but unexplained” starts to deserve a cleaner strategy, especially if work, sleep, walking, lifting, or exercise tolerance remain impaired.
The point is not to turn yourself into a spreadsheet. The point is to show trajectory. A body that is healing usually changes in a recognizable direction, even if slowly. A body that is stuck, unstable, or misdiagnosed often tells a different story.
Here’s what no one tells you: duration changes the question your next visit should answer
Early on, the question may be: “Does this still fit a simple recovery pattern?” Later, the question becomes: “What important diagnosis has not yet been tested well?” That is a more sophisticated question, and it tends to produce more useful care.
Short Story: A reader once described her knee pain in a sentence I still like because it was so ordinary and so exact: “It’s not worse all the time, but it gets mean on stairs and weird when I pivot.” That line did more work than ten minutes of saying it was “kind of bad.” Her original X-ray had been normal.
What changed the visit was not drama. It was pattern. The knee was not simply sore. It was behaving mechanically. That difference pushed the conversation away from generic reassurance and toward a more useful next step. Medicine often opens when description sharpens. Not louder. Sharper.
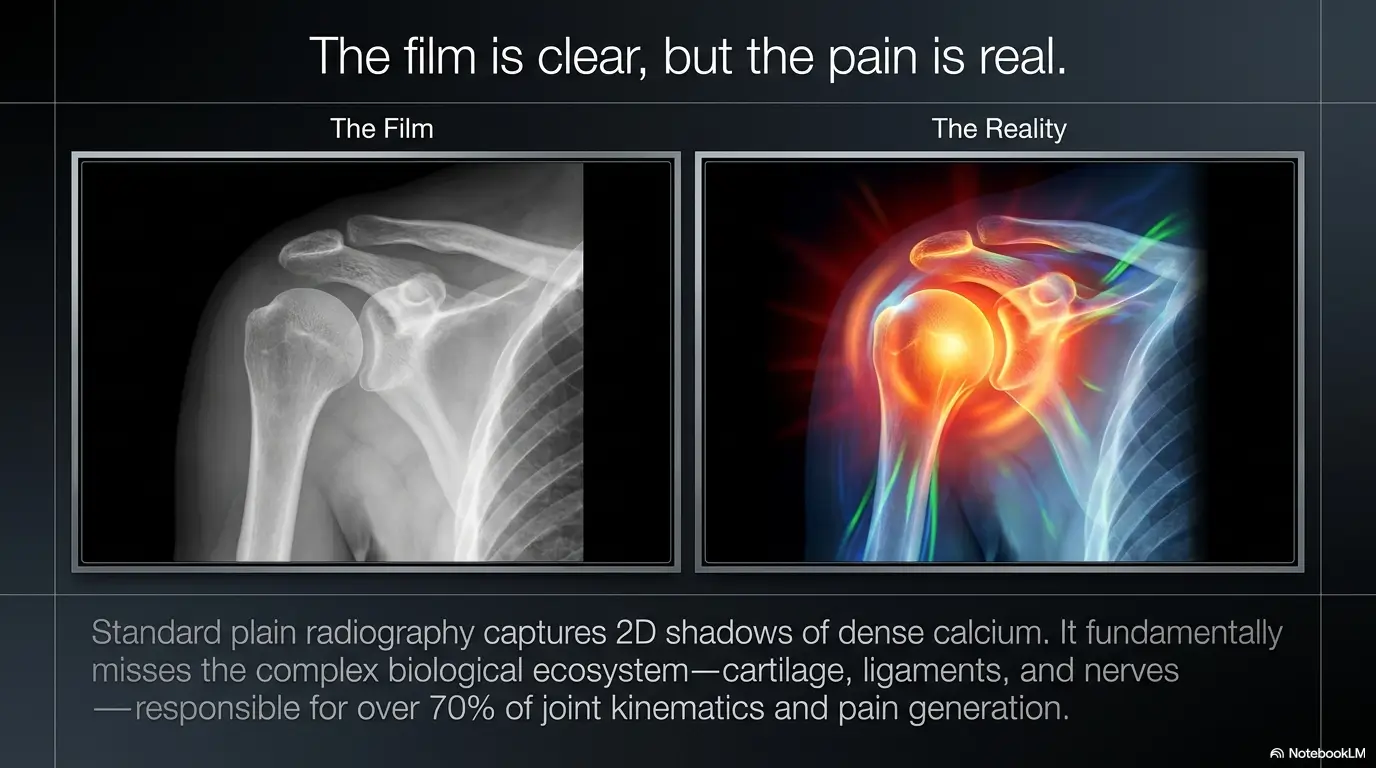
Look Past the Image: Clues Hiding in Function, Not Just Findings
Trouble sleeping, walking, lifting, reaching, sitting, or turning matters more than many people realize
Function is where pain stops being a number and starts becoming evidence. Can you sleep through the night? Reach into a cabinet? Sit through a meeting? Walk to the parking lot without rehearsing your limp? These details matter because they help separate soreness from disruption.
A lot of people underreport this. They say, “I can still do it.” But what they mean is: “I can still do it if I brace, bargain, avoid, shorten, compensate, and later pay for it.” That is not the same as preserved function. That is a truce with collateral damage.
Why “I can still do it, but it hurts” is not the same as normal recovery
Being technically capable of a movement does not tell you whether the movement is normal, sustainable, or safe. Someone with shoulder pain may still reach overhead while wincing, substituting posture, and avoiding the last part of the motion. Someone with back pain may still sit, but only by constantly shifting, standing early, and losing focus. Function is not binary. It has quality.
Functional loss often tells the story before a scan does
In the clinic, better function questions often lead to better next steps. The image is one chapter. The body in motion is the novel. If your pain is interrupting work tasks, caregiving, hobbies, walking speed, sleep, or the ability to return to exercise, that deserves to be described clearly, because it helps frame how aggressive or conservative the next plan should be. For desk-based readers, these details often overlap with the daily patterns described in orthopedic pain management for remote workers.
Decision Card: Pain score or function story?
| When this is happening | Focus on saying this |
|---|---|
| Pain varies day to day | “The number changes, but I still cannot walk more than 10 minutes comfortably.” |
| Movement is possible but altered | “I can reach overhead, but only by shrugging and then it aches for hours.” |
| Symptoms affect sleep or work | “The pain wakes me at night and I am changing how I work around it.” |
Neutral action: Bring one function sentence to your next appointment, not just a pain number.
Show me the nerdy details
Musculoskeletal imaging is a question-matching exercise. Plain radiographs are often first because they are fast, accessible, and useful for many bony questions. Persistent symptoms after normal radiographs can shift the clinical question toward soft tissue, inflammation, occult injury, or nerve-related causes. That is why body-part-specific imaging guidance exists. The mismatch between symptom pattern and first-line imaging is not rare. It is built into how different tests work.
Do Not Shrink the Story: Common Reasons Pain Gets Dismissed Too Early
Mistaking a normal X-ray for proof that nothing is wrong
This is the classic error, and it happens on both sides of the desk. Patients hear “normal” and minimize what they feel. Clinicians, pressed for time, may default to a less urgent explanation unless the symptom story clearly points elsewhere. Neither response is malicious. Both can be costly.
The cure is not panic. It is specificity. “The image was normal, but I still have weakness turning a doorknob,” is more useful than, “It still kind of hurts.” The first sentence opens diagnostic possibilities. The second drifts.
Underreporting weakness, numbness, instability, or activity limits during the visit
People edit themselves in medical visits for all kinds of reasons. They do not want to sound dramatic. They forget details. They think weakness is only true if a limb becomes useless. They say numbness only counts if the body part goes fully dead like a phone battery. Real life is more nuanced. Tingling, catching, locking, buckling, giving way, radiating pain, or trouble with fine motor tasks may all matter.
Let’s be honest: many patients say “it’s fine” when what they mean is “I’ve adapted around it”
I have seen this pattern everywhere outside medicine too. We call something manageable because we have rearranged our lives around it. We stop carrying heavy groceries with one arm. We stop sitting on the floor. We stop sleeping on one side. We stop running. Then we tell ourselves the problem is modest. It is not modest. It is expensive. It is charging rent in tiny behavioral changes.
- Report weakness, numbness, locking, or instability clearly
- Name what you stopped doing, not just what hurts
- A “normal” image does not erase an abnormal day
Apply in 60 seconds: List three things you now do differently because of the pain.
Body-Part Matters: Why the Next Step Depends on Where It Hurts
Shoulder and knee pain often raise different follow-up questions than low back or hip pain
The same frustration can live in very different anatomy. Shoulder pain with overhead weakness or night pain may raise soft-tissue questions. Knee pain with locking, catching, swelling, or pivot-related pain may raise mechanical questions. Hip pain can be joint, tendon, bursa, back-related, or even referred pain from elsewhere. Low back pain brings its own branching logic, especially if it radiates.
This is why “I want an MRI” is usually less helpful than “I want to understand what problem is now most suspected.” Imaging choice and urgency often change depending on where the pain lives and what the body does when provoked. For hip complaints in particular, it can help to think through whether the pain pattern sounds more like hip pain or spine pain, especially when the sore spot and the true source may not match.
Spine pain may involve nerve patterns that deserve a different workup than joint pain
Back or neck pain becomes a different conversation when it travels, causes numbness, changes reflexes, or produces weakness. The American College of Radiology treats radicular patterns differently than uncomplicated pain without red flags. That does not mean every twinge needs a scan. It means the symptom map matters. Radiating pain is not just pain with ambition. It may suggest nerve involvement. Some readers find it easier to describe that distinction after reading about what sciatica nerve pain tends to feel like.
One phrase to remember: same frustration, different anatomy, different next move
Keep this phrase because it prevents lazy thinking. Two people can both say, “The X-ray was normal and I still hurt,” while needing completely different care paths. Precision starts with respecting anatomy, not flattening it.
Coverage Tier Map for Your Own Thinking
- Tier 1: Where does it hurt?
- Tier 2: What movement or activity triggers it?
- Tier 3: Is there weakness, numbness, locking, or instability?
- Tier 4: Is function changing over days or weeks?
- Tier 5: What diagnosis is now most suspected, and what test or treatment would answer that best?
Neutral action: Move your thinking from “I need something done” to “I need the next question answered.”
Before More Testing: What a Good Conservative Plan Usually Tries First
Activity modification is not the same thing as total rest
One of the quietest mistakes in orthopedics is treating all motion as betrayal. Total rest often sounds noble. It can also make you stiffer, weaker, and more fearful of movement. For many routine musculoskeletal problems, the goal is not to stop existing. It is to reduce the specific load or movement pattern that keeps poking the bruise.
That may mean shorter walks instead of zero walks, lighter lifting instead of heroic lifting, or changing the range and speed of an exercise rather than deleting movement entirely. The body is often happier with calibrated motion than with panic-frozen stillness.
Physical therapy, home exercises, and load management can reveal as much as they treat
Conservative care is not just the appetizer before “real” medicine. It can be diagnostic. If pain improves with certain movement patterns, strengthening, or activity adjustments, that tells you something. If a good rehab effort fails, that also tells you something. In other words, treatment can generate information. Not glamorous information. Not movie-trailer information. But useful information. When the sticking point is whether therapy has been “enough” to justify the next step, that logic overlaps with what failed conservative care usually means before MRI approval.
Medication choices should support function, not just mute symptoms long enough to overdo it
Pain relief can be helpful. It can also trick people into overspending their recovery budget in one afternoon. The question is not just, “Did it help the pain?” The better question is, “Did it help me move and function in a way that supports recovery?” Relief is a tool, not proof of healing.
A small real-life scene here: someone feels better Saturday morning, cleans the whole garage, and spends Sunday meeting their consequences like an old enemy at a train station. We laugh because it is familiar. The tissue, sadly, does not care that we were in a productive mood.
Not Yet, Not Never: When More Imaging Starts Making Sense
Persistent pain plus weakness, locking, instability, numbness, or failed rehab changes the calculus
Needing more imaging is not a moral victory, and avoiding more imaging is not a virtue. What matters is whether the current symptom pattern justifies a better question. Persistent pain alone may or may not be enough. Persistent pain plus weakness, mechanical symptoms, neurologic features, or failed conservative care often makes the case more compelling.
This is especially true when the next result could change management. If a scan would not change what anyone does, the value may be limited. If it would affect treatment choice, referral urgency, or whether a procedure is considered, the conversation becomes more practical.
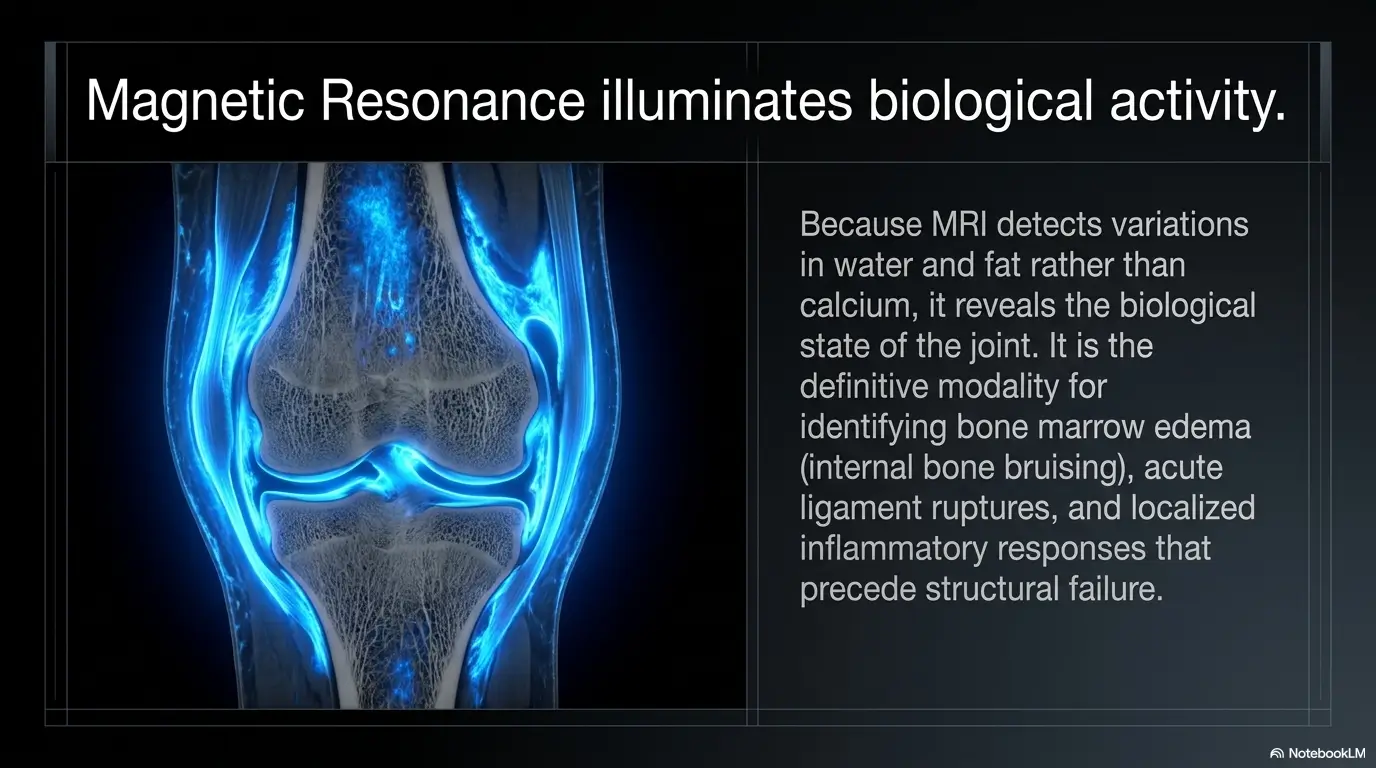
MRI, ultrasound, CT, or repeat imaging each answer different kinds of questions
MRI is often used when soft tissues, occult injury, marrow changes, or nerve-related structures are part of the suspicion. Ultrasound can be useful for some tendon or soft-tissue questions and has the bonus of real-time assessment in selected cases. CT may matter more for certain bone questions. Repeat X-rays can help in specific circumstances too, particularly when timing changes what becomes visible.
The important thing is not memorizing the menu. It is understanding that imaging is not one big bucket called “a scan.” Different tests are different flashlights. Use the wrong flashlight and you only learn that the room is still dark. That is also why patients often get frustrated after cost or authorization delays, especially in situations like orthopedic pain management after an MRI denial appeal.
The smarter goal is not “get a scan” but “get the right test for the right suspicion”
That sentence will make your follow-up visit better. It invites reasoning instead of a tug-of-war. Ask what problem is now most suspected, what imaging would best evaluate that suspicion, and whether the result would change treatment. That is the kind of question that often gets respect, because it sounds like someone trying to solve a problem rather than collect technology like keychains.
Mini Calculator: Is your next step descriptive enough?
Score yourself 0 or 1 for each item below:
- Can you name one trigger movement clearly?
- Can you name one function you lost or altered?
- Can you name whether symptoms are improving, stalling, or worsening?
2 to 3 points: You are ready for a focused follow-up conversation.
0 to 1 point: Spend 7 days tracking symptoms before your visit.
Neutral action: Better descriptions often improve decisions before any new imaging is ordered.
Mistakes That Make Orthopedic Pain Harder to Untangle
Chasing multiple opinions without tracking symptoms consistently
Second opinions can be wise. Five rushed opinions without a clear symptom record can turn your case into a blur. When every visit begins from scratch and every description changes shape, the story becomes hard to compare across time. That can create the illusion that medicine is failing when part of the problem is that the data are foggy. If insurance becomes part of that maze, some readers end up needing the kind of strategy discussed in what to do when a second opinion for orthopedic pain is denied.
Returning to aggravating activity too soon because the X-ray looked reassuring
This one is common because reassurance feels like permission. If the first image is normal, people often jump back into the very activity that lights the fuse. They assume the body is safe because the image was calm. But imaging and load tolerance are not the same thing. You can have a reassuring X-ray and still have tissue that hates what you are asking it to do on Tuesday afternoon.
Treating pain relief as proof of healing
Temporary improvement is not fake, but it is also not always structural recovery. Pain can ease before tissue capacity returns. That mismatch is where setbacks like to shop. The pain dipped, so the person resumed full speed, and the body replied with a memo written in capital letters.
The Follow-Up Visit That Works Better: What to Bring and What to Say
Bring a short symptom timeline with triggers, limits, and changes in pain quality
The best follow-up visits are rarely the ones with the most emotion. They are the ones with the clearest pattern. Bring 7 days of notes if you can. Not a novel. Not a tragic opera. Just the essentials: where it hurts, what triggers it, what improves it, what function is limited, and whether symptoms are spreading, sharpening, or calming down.
Use plain descriptions of function loss instead of vague pain adjectives alone
“Sharp” and “achy” are fine. But “I cannot carry groceries with my right arm” or “I have to stop after 15 minutes of walking” will usually do more work. Function tells a clinician where the body fails under load. That is often more informative than color commentary.
Ask what diagnosis is most likely, what has been ruled out, and what would change the plan
These three questions are gold:
- What is the leading diagnosis right now?
- What important possibilities have been reasonably ruled out?
- What would change the treatment plan from here?
That final question is especially helpful. It exposes whether more therapy, more time, a referral, or different imaging actually makes sense. It turns the visit into a decision tree instead of a vague wellness weather report. If the answer starts sounding procedural rather than orthopedic, it can also help to know the difference between a pain clinic and an orthopedist before the next referral lands in your portal.
What to Gather Before Comparing Next-Step Options
- Date symptoms started or changed noticeably
- Three trigger movements or activities
- One clear example of function loss at work or home
- What you already tried for at least 1 to 2 weeks
- Whether symptoms include numbness, weakness, locking, or swelling
Neutral action: Put this list in your phone notes before the appointment so the visit starts sharper.
- Bring a timeline
- Name a function loss
- Ask what would change the plan
Apply in 60 seconds: Draft your first line for the visit: “The X-ray was normal, but over the last ___ weeks I still cannot ___ without pain.”
When Lingering Pain May Be Coming From Somewhere Else
Referred pain can make the knee, hip, shoulder, or leg look guilty when the source is elsewhere
One of the trickier parts of musculoskeletal care is that the body does not always send pain from the scene of the crime. Hip issues can be felt in the groin or knee. Back problems can show up in the leg. Neck issues can disturb the shoulder or arm. That does not mean every ache is referred pain. It means location alone is not always the whole map.
If treatment keeps focusing on the sore spot without real progress, it is fair to ask whether the pain source and the pain location may be different. This is one reason a careful exam matters so much. Bodies are not always tidy narrators.
Nerve irritation, inflammatory conditions, and biomechanics can complicate the picture
Nerve-related symptoms may include tingling, burning, zinging, radiating pain, or weakness. Inflammatory problems may come with swelling, stiffness, warmth, or patterns that do not behave like a straightforward strain. Biomechanics can complicate things too. The knee may be the loudest complainer, while the hip, ankle, back, or movement pattern has been setting the stage. When hip symptoms keep masquerading as something else, readers often benefit from the comparison in hip pain at night and what those patterns can suggest.
If the treatment keeps missing, the location of pain may not be the full map
This is worth repeating because it rescues people from the exhausting loop of doing the wrong useful thing. You can follow instructions perfectly and still stall if the treatment is aimed at the wrong address. When progress stays flat, the question may need to widen.
When to Seek Help More Urgently
Severe swelling, deformity, fever, nighttime pain that feels alarming, or sudden neurologic symptoms
Urgent patterns deserve less storytelling and more action. A joint that is visibly deformed, intensely swollen, hot, or red with fever is not a casual follow-up problem. Sudden neurologic changes, rapidly worsening weakness, severe pain after significant injury, or new symptoms that feel systemically wrong should prompt prompt evaluation.
New inability to bear weight, rapidly worsening weakness, or uncontrolled pain after injury
These are the moments where normal-X-ray reassurance should not lull you into passivity. The timeline matters. The trend matters. And your sense that something is not right matters. Not every alarming symptom signals catastrophe, but the cost of underreacting can be higher than the cost of being checked.
Waiting is not always the brave option
Some readers need to hear this cleanly: endurance is not the same as judgment. There is a cultural script around “toughing it out.” It has its uses. It also leaves a lot of people limping through preventable delay. Bravery is not always staying quiet. Sometimes bravery is calling the clinic back because the story changed. If you are torn between settings, it may help to review urgent care versus orthopedic clinic for musculoskeletal problems before deciding where to go.
FAQ
Can you still have a serious orthopedic problem if the X-ray is normal?
Yes. A normal X-ray does not automatically rule out every meaningful problem. Soft-tissue injury, some occult injuries, nerve-related issues, and referred pain patterns may not be explained by the first plain radiograph alone. The seriousness depends on symptoms, function, and exam findings, not just the first image.
How long should pain last before I follow up again?
There is no single deadline for everyone, but follow-up becomes more important when symptoms stall, worsen, spread, or keep interfering with function. If you have already tried a reasonable conservative plan and remain limited after several weeks, or if red flags appear sooner, it is appropriate to re-evaluate.
What kinds of injuries or conditions do X-rays commonly miss?
X-rays can miss or under-explain some tendon, ligament, cartilage, labral, nerve-related, and certain stress or occult injuries, depending on timing and body part. They also may not fully explain inflammatory causes or referred pain patterns. The missing piece is often the mismatch between symptom pattern and what the first test can see well.
When is an MRI usually considered after a normal X-ray?
MRI may be considered when persistent symptoms, weakness, neurologic features, mechanical symptoms, or failed conservative care raise suspicion for a condition that plain radiographs do not evaluate well. It is most useful when the result would meaningfully change treatment or the next referral decision.
Should I keep exercising or rest completely while I wait?
For many musculoskeletal issues, complete rest is not automatically better. Activity modification is often more useful than total shutdown. The right answer depends on the body part, suspected problem, and how symptoms respond. The goal is usually to reduce aggravating load while preserving safe movement, not to turn yourself into furniture.
Can physical therapy help even if no clear diagnosis showed up on the X-ray?
Yes, in many cases it can. Physical therapy and well-designed home exercise programs can improve pain, restore function, and clarify whether symptoms respond to a mechanical or load-based approach. Lack of progress can also provide useful information for the next clinical decision. If coverage is part of the decision, some readers also need clarity on how Medicare Part B physical therapy coverage typically works.
What symptoms suggest nerve involvement rather than a simple strain?
Symptoms that travel, burn, tingle, feel electric, or come with numbness or weakness may suggest nerve involvement. Distribution matters too. Pain shooting from the neck into the arm or from the back into the leg often deserves different thinking than isolated local soreness.
Is worsening pain after a normal X-ray a reason to be re-evaluated?
Yes. Worsening pain, new weakness, inability to bear weight, spreading symptoms, escalating nighttime pain, or new neurologic changes are all reasons to seek re-evaluation. A reassuring first test should not overrule a worsening clinical picture.
Next Step: Make the Problem Easier to Solve Before Your Next Appointment
Track pain location, triggers, timing, and function limits for seven days
If this article has one practical purpose, it is this: make the next visit more useful than the last one. For the next 7 days, track where the pain is, what movement triggers it, whether symptoms travel, and what function is limited. Keep it short. You are building signal, not writing memoir, tempting though that may be.
Write down one clear question you need the visit to answer
Good options include:
- What diagnosis is now most likely?
- Do my symptoms suggest a soft-tissue, nerve, inflammatory, or referred-pain issue?
- Would a different test change treatment?
- What should improve over the next 2 to 6 weeks if the current plan is working?
Bring that record to your next clinician instead of relying on memory alone
This closes the loop from the beginning. The problem with a normal X-ray is not usually that it was useless. The problem is that people let it become the whole story. Do not do that. Bring the fuller story. The body has already been speaking. Your job, over the next 15 minutes, is to translate it into cleaner evidence. And if the next decision turns financial as much as clinical, it may help to compare your options through orthopedic pain management with a high deductible plan before you commit to the next round of care.
- Track symptoms for 7 days
- Name one lost function
- Ask one question that could change the plan
Apply in 60 seconds: Open your notes app and create four headings: Location, Trigger, Function, Change.
Last reviewed: 2026-04.
This article is informational and not a diagnosis. Seek urgent medical care for severe or rapidly changing symptoms, major trauma, loss of bladder or bowel control, sudden weakness, or other emergency warning signs.
