
Navigating the Orthopedic Referral Gap
Orthopedic pain management when referral wait times are long is less about heroic pain tolerance and more about not letting a scheduling delay quietly wreck your sleep, mobility, and daily function. The cruel little trick of referral limbo is that nothing looks dramatic on paper while real life keeps getting smaller: stairs become negotiations, desk work turns brittle, and lifting a grocery bag starts to feel oddly strategic.
For many adults, the hardest part is not the pain alone. It is the blur. Symptoms change, notes get sloppy, and by the time the orthopedic visit finally arrives, you are left trying to summarize weeks of stiffness, weakness, swelling, nerve symptoms, and missed sleep from memory.
Keep guessing too long, and the wait becomes more expensive than the appointment.
This post helps you use the gap well: spot red flags, protect function, make conservative care more useful, and arrive with a cleaner clinical story instead of a foggy one. It is built around the details that actually move care forward, like function loss, movement limits, sleep disruption, and whether physical therapy, primary care, or imaging would change the next decision.
Just a steadier plan while the calendar crawls. Because a long wait should be a working interval, not a slow unraveling.
Table of Contents
Fast Answer: Orthopedic pain management when referral wait times are long works best when you do three things at once: screen for red flags, protect function, and document the problem clearly. A wait should not become a fog. Conservative care, smarter tracking, and better use of primary care or physical therapy can make the eventual specialist visit more useful and less repetitive.

Start Here: A Long Referral Wait Should Not Mean a Frozen Plan
The real risk is not only pain, but losing function while waiting
When people say, “I’m waiting for ortho,” they often mean, “I have paused my whole strategy until someone with a specialist badge tells me what this is.” That sounds sensible. It is also where drift begins. Pain itself matters, of course. But function is often the louder signal. Can you climb stairs? Carry groceries? Sit through work? Sleep past 3 a.m. without waking up like a crooked umbrella?
I have watched plenty of people describe a seven-out-of-ten pain score with perfect fluency, then casually mention they have stopped lifting their toddler, quit walking the dog, or started using the good arm for everything. That is not background noise. That is the plot.
Why “just wait for ortho” often leads to drift, repeat visits, and frustration
The waiting period can turn into a medical version of airport carpeting. You are technically moving through a system, but nothing feels like progress. Notes get fuzzy. Symptoms blur together. The first visit becomes a rewind of three months of half-remembered frustration instead of a focused decision-making appointment.
The American Academy of Orthopaedic Surgeons notes that symptoms affecting daily function, difficulty moving around, and limited range of motion are meaningful reasons to seek orthopedic evaluation. That is useful because it reframes the question. The issue is not only “How bad does it hurt?” but also “What is this stopping me from doing?”
Here’s what matters first: safety, function, and the next decision
Think of the wait in three lanes:
- Safety: Are there red flags that mean the timeline should change?
- Function: What movements or tasks are breaking down?
- Decision: What is the next clinician actually being asked to clarify?
If you keep those three lanes visible, the waiting period becomes a working interval instead of dead time.
- Pain score alone is too thin
- Function decline often reveals urgency
- A better next appointment starts before the appointment exists
Apply in 60 seconds: Write down the top three tasks your pain is interfering with this week.
Who This Helps: Who This Is For and Not For
This is for adults with non-emergency joint, back, neck, shoulder, knee, hand, or foot pain waiting on specialist input
This guide is for the ordinary but exhausting middle ground: pain that feels real, limiting, and persistent, but not obviously catastrophic. Maybe you are waiting on orthopedics, sports medicine, physiatry, spine, or hand. Maybe the referral is “processing.” Maybe it has been rescheduled twice, which is the medical equivalent of being ghosted by a calendar.
This is for people trying to manage pain without overspending, overtesting, or spiraling
Many readers are not just hurting. They are also budget-conscious, short on time, or tired of being bounced between clinics. You may want help that is concrete and restrained. Not every ache needs an MRI. Not every flare needs panic. And not every week of waiting should be filled with buying braces, gadgets, supplements, and hope in shiny packaging. If cost is part of the stress, a guide to orthopedic pain management with a high deductible can help you think more clearly before money starts dictating the whole mood.
This is not for symptoms that suggest urgent neurologic, infectious, traumatic, or circulatory problems
This is not a substitute for urgent or emergency care. If you have severe trauma, sudden inability to bear weight, major swelling after injury, loss of bladder or bowel control, rapidly worsening weakness, fever with significant back pain, signs of infection, or a limb that looks pale, cold, blue, or badly deformed, the queue is no longer the main story. The story has changed.
Eligibility checklist
- Yes: Pain is limiting but stable enough to monitor day to day
- Yes: You need a clearer plan while waiting on a specialist
- Yes: You want conservative steps that respect cost and time
- No: You have major red flags, new trauma, or rapidly worsening neurologic symptoms
Next step: If you land in the “No” category, seek faster medical evaluation rather than waiting out the referral.
First Filter: What Needs Faster Care Before the Referral Arrives
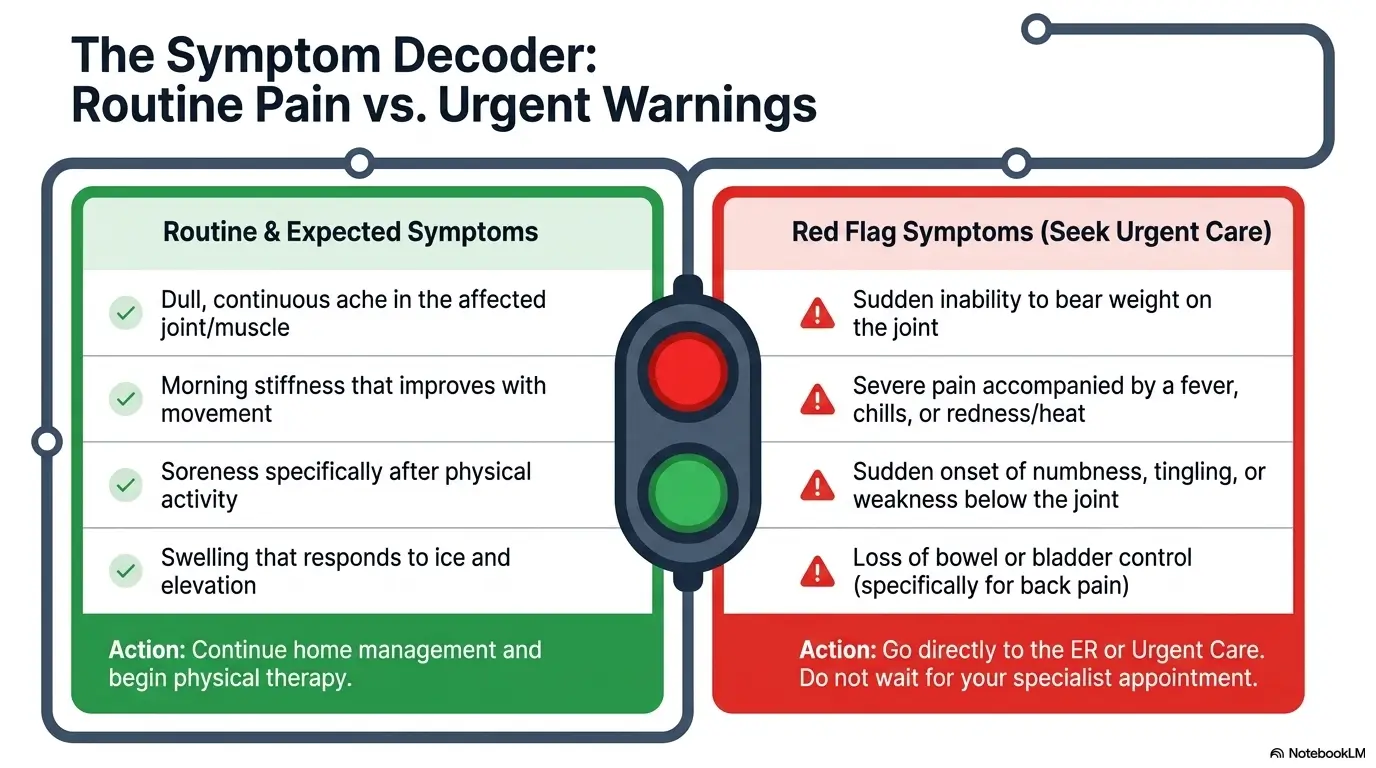
Red flags that can change the timeline from “wait” to “seek urgent evaluation”
Not every musculoskeletal problem is a sit-tight situation. MedlinePlus lists several warning signs for acute low back pain that should prompt faster evaluation, including loss of urine or stool control, unexplained fever with back pain, worsening weakness, numbness, severe pain after trauma, and difficulty walking or maintaining balance. Even if your problem is not in the back, the logic travels well: some symptoms announce themselves as structural or neurologic trouble rather than routine soreness.
When worsening weakness, numbness, fever, swelling, or loss of bladder or bowel control changes the equation
These symptoms matter because they suggest the body may be doing more than protesting. It may be struggling. Worsening weakness is different from pain-limited effort. Fever plus localized pain or swelling raises different concerns than ordinary overuse. A joint that becomes red, hot, and rapidly swollen deserves more respect than a stubborn ache after gardening, tennis, or hauling laundry like it was a CrossFit event.
Do not normalize severe changes just because the referral queue is long
One quiet danger of a crowded system is that patients start adapting to it emotionally. They tell themselves, “If it were serious, someone would have called me back faster.” Systems do not think that way. Your symptoms still need their own judgment. A slow scheduling pipeline is not a clinical opinion.
Use this simple rule: if symptoms are rapidly worsening, neurologic, infectious-looking, traumatic, or functionally dramatic, escalate. The goal is not to be stoic. It is to be accurate. For spine-related warning signs in particular, readers dealing with back and leg symptoms may want a more focused review of cauda equina syndrome red flags.
Show me the nerdy details
Clinicians often sort urgency by mechanism and pattern, not by volume alone. Constant pain with fever, progressing neurologic loss, inability to bear weight after injury, and bowel or bladder changes all suggest a different risk category than a stable overuse flare with preserved strength and mobility.
While You Wait: What Problem Are You Actually Trying to Solve?
Pain intensity is only one clue, not the whole story
Most people lead with pain because it feels obvious. But pain is only one axis. A “5” can be more disabling than an “8” if it wrecks sleep, makes stairs unreliable, or turns every reach, bend, or turn of the steering wheel into negotiation.
Separate pain, stiffness, instability, weakness, and sleep disruption before you choose the next step
Try sorting symptoms into plain buckets:
- Pain: sharp, dull, burning, throbbing, electric
- Stiffness: hard to start moving, worse after sitting, loosens later
- Instability: giving way, catching, locking, buckling
- Weakness: cannot do what you normally can, even when trying
- Sleep disruption: wakes you, keeps you from settling, forces position changes
This kind of sorting helps because each pattern points the conversation differently. A locking knee is not the same as a sore knee. Night pain is not the same as end-of-day soreness. A hand that goes numb and weak at work tells a different story than a stiff hand on waking.
Let’s be honest: many people say “it hurts” when the bigger issue is “I can’t function normally”
A friend once described shoulder pain for six weeks. After ten minutes of talking, the real problem emerged: she could no longer fasten her bra without staging a small one-woman tragedy in front of the mirror. That detail was more useful than the number she kept repeating. Function tells the truth with less poetry.
- Sort by pattern, not just intensity
- Function loss often sharpens the diagnosis story
- Sleep disruption deserves to be documented
Apply in 60 seconds: Finish this sentence in writing: “The main thing this pain is stopping me from doing is…”
Use the Gap Well: Build a Conservative Plan That Matches the Body Part
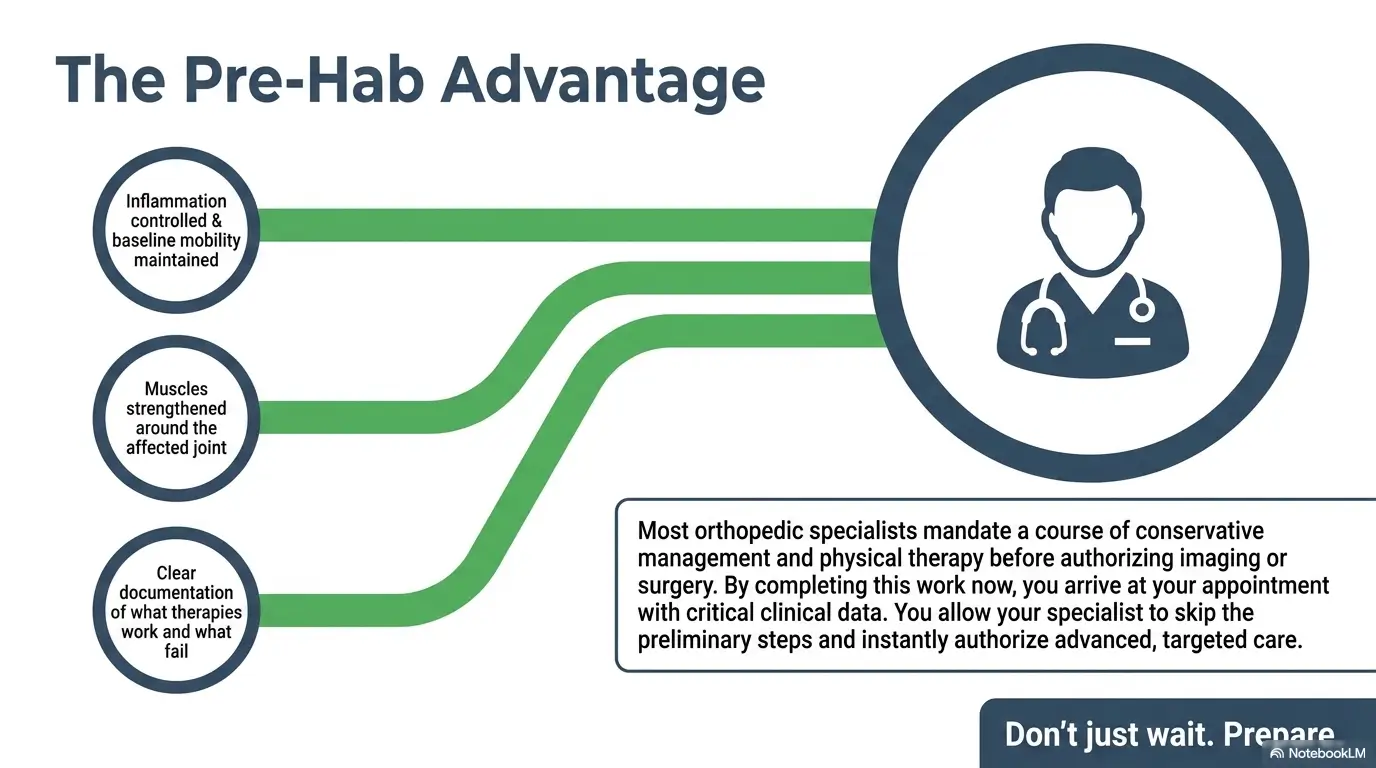
What self-care can realistically do during the waiting period
Conservative care is not glamorous, which is probably why it does not get enough respect. But done well, it can reduce pain spikes, preserve movement, and prevent the specialist visit from starting at a worse baseline. This is not about home heroics. It is about lowering friction.
How activity modification differs from complete shutdown
Activity modification means changing load, duration, range, or repetition. It does not mean turning yourself into a decorative statue. MedlinePlus notes that, for acute low back pain without red flags, prolonged bed rest is not recommended and gentle return to activity is usually preferred. The same principle often helps elsewhere: avoid the specific aggravator, not all movement forever.
When heat, ice, gentle movement, bracing, or pacing may help depending on the pattern
A few examples:
- Heat: often feels better for stiffness and muscle guarding
- Ice: may help after activity flares or recent irritation
- Gentle movement: can reduce the “rusty hinge” feeling after sitting
- Bracing or support: sometimes useful for short periods, not as a permanent identity
- Pacing: especially helpful when boom-and-bust cycles keep restarting the problem
One small personal lesson here: people love the good-day trap. They feel 20% better, then reorganize the garage, deep-clean the kitchen, and carry three mystery bins labeled “winter stuff.” The body then submits a formal complaint. Pacing is boring, but it often saves the week. If support devices are part of the interim strategy, it also helps to know which HSA-eligible braces and supports may be worth considering before you buy something bulky and regret-shaped.
Why the goal is not heroics, but fewer bad days and less backtracking
A good waiting strategy should make daily life slightly less dramatic. Not perfect. Just steadier.
Decision card
| When this fits | Try this | Trade-off |
|---|---|---|
| Stiff, sore, guarded | Heat + brief gentle movement | May soothe, but can tempt overdoing it |
| Flared after activity | Relative rest + ice + load reduction | Helpful short term, not a forever plan |
| Repeated boom-bust cycle | Pacing and smaller activity blocks | Feels slow, usually saves setbacks |
Neutral action: Pick the pattern that sounds most like your week, not your best day.
Do Not Do This: The Common Mistake of Resting Too Hard or Testing Too Early
Why total inactivity can quietly worsen stiffness, fear, and deconditioning
Rest has a role. Over-rest has a reputation it did not earn. Too much shutdown can make muscles less tolerant, joints stiffer, confidence shakier, and the return to normal activity more dramatic than it needed to be. The body likes reasonable input. Not punishment. Not hibernation.
Why chasing imaging before the clinical question is clear can waste money and momentum
Imaging has its place. But images answer specific questions; they do not replace them. MedlinePlus explains that many cases of acute low back pain are not imaged right away unless certain concerning symptoms are present. That is not neglect. It reflects a simple truth: pictures are most useful when matched to a clinical reason.
People often imagine imaging as a finish line. In reality, it is closer to a flashlight. Very useful in the dark. Less useful if you are shining it into the wrong room.
Here’s what no one tells you: an MRI is not a plan by itself
A scan can show age-related changes, old findings, incidental oddities, and dramatic-sounding words that may or may not explain your symptoms. If the clinical question is vague, the result may increase confusion rather than reduce it. The better path is usually: clarify pattern, document functional limits, try sensible conservative steps, and then decide whether imaging is needed to answer a real next-step question. Readers trying to sort out when an MRI referral for orthopedic pain actually changes the next move often do better than those collecting scans like anxious souvenirs.
- Movement usually beats total shutdown
- Imaging works best when the clinical question is specific
- The goal is decision clarity, not image collection
Apply in 60 seconds: Write one sentence beginning with “I think imaging would help only if it answers whether…”
Primary Care Matters: How to Use Non-Specialist Visits More Strategically
What primary care, urgent care, physical therapy, or a musculoskeletal clinician can still clarify before orthopedics
One of the most expensive myths in musculoskeletal care is that nothing useful can happen until the specialist appears. In reality, primary care can often screen for red flags, review medication safety, guide interim symptom management, start physical therapy, examine range of motion and strength, and update the referral based on worsening function. Urgent care can sometimes help with acute changes, though it is not always ideal for long-story problems. Physical therapy can be especially useful when movement, load tolerance, and function are the actual battlefields. If you are unsure where to go when symptoms suddenly change, it may help to compare urgent care versus an orthopedic clinic before defaulting to whichever building answers the phone first.
How to ask for symptom-based help instead of only saying “I need a referral faster”
Try this language instead:
- “My knee is buckling twice a day and stairs are getting less safe.”
- “My shoulder pain now wakes me most nights and I cannot reach overhead.”
- “My back pain is no longer the only issue. I am getting new weakness and balance trouble.”
That is stronger than “Can you speed this up?” because it gives the clinician something clinical to work with.
Which details make a primary care visit more useful than a generic pain complaint
Bring timing, triggers, what you have already tried, what helps, what clearly worsens it, and what daily tasks are failing. The American Physical Therapy Association also notes that many patients can self-refer to physical therapy in many situations, though coverage rules and state access details vary. Translation: there may be more movement available than the queue makes you think. For readers on Medicare, understanding how Medicare Part B handles physical therapy can turn a vague maybe into a more usable plan.
Entities worth recognizing: AAOS, MedlinePlus, APTA, and your insurer all shape this landscape differently. The clinic, the referral system, and your coverage are not one machine, even though they often behave like a committee trapped in a trench coat.
Show me the nerdy details
Interim visits matter because they can update triage quality. New weakness, swelling, loss of motion, inability to bear weight, or severe sleep disruption can change how a referral is prioritized or what conservative treatment starts before the specialist sees you.
Track Smarter: The Notes That Make Specialist Visits Shorter and Better
Record triggers, time of day, movement limits, swelling, sleep effects, and failed treatments
A two-week symptom log can do more good than three months of vague memory. Keep it simple. You are not writing a novel. You are building a cleaner handoff.
- What movement triggers it?
- What time of day is worst?
- Is there swelling, numbness, catching, locking, or instability?
- What have you already tried?
- What happened after you tried it?
Document what improves function, not just what briefly reduces pain
This matters more than it sounds. A treatment that lowers pain for an hour but does not let you walk farther, sleep better, or work more comfortably may not be your best interim tool. Function is a tougher, better metric.
Why a two-week symptom log can be more valuable than a vague three-month memory
I once saw someone bring four months of fuzzy recollection and one sticky note that said, “Worse at night.” Not useless, but not exactly surgical-grade clarity. Compare that with a page showing: “Pain worse after sitting longer than 30 minutes, stiffness in first ten steps, swelling after stairs, relief after brief walk, wakes me around 2 a.m.” That second version saves time and sharpens decisions. People facing insurance friction may also find that the same disciplined note-taking helps if they later need to show what counts as failed conservative care for an MRI request.
Mini calculator
If your pain wakes you 3 nights a week and each wake-up costs 45 minutes of sleep, that is 135 minutes lost weekly. Over 4 weeks, that becomes 9 hours of sleep disruption.
Neutral action: Add sleep loss to your symptom notes. It often changes how serious the problem looks.
Avoid This Trap: Mistaking All Orthopedic Pain for the Same Kind of Wait
Back pain, knee pain, shoulder pain, and hand pain often need different interim strategies
There is no universal “orthopedic pain plan.” A stiff lower back, a locking knee, a weak shoulder, and a numb hand do not ask for the same waiting strategy. The body is not one giant offended hinge. Different regions fail in different ways.
Mechanical pain versus inflammatory or nerve-related symptoms changes what to watch
Mechanical patterns often change with movement or load. Inflammatory patterns may involve prolonged morning stiffness, heat, swelling, or a more systemic feel. Nerve-related symptoms can include burning, tingling, numbness, shooting pain, or weakness that does not feel purely pain-limited. You do not need to self-diagnose these categories perfectly. But noticing the pattern helps you describe the problem more usefully.
The quiet mistake: copying someone else’s recovery routine from social media
This one deserves a small sigh. Social media loves tidy recovery rituals because they look cinematic. The matching bands, the dramatic massage gun, the caption about “fixing” pain in seven days. Unfortunately, your shoulder is not obliged to follow an influencer’s lower-back routine, and your numb hand may not care about a stranger’s ice bath content.
Use body-part logic instead: ask what this region needs to preserve safe movement, reduce flare triggers, and avoid worsening function before the specialist visit.
- Body part matters
- Symptom pattern matters
- Borrowed routines are often a poor fit
Apply in 60 seconds: Label your symptoms as mostly mechanical, inflammatory-looking, nerve-like, or mixed.
Referral Delays and Daily Life: How to Protect Work, Sleep, and Basic Tasks
What to do when pain is affecting driving, lifting, childcare, or desk work
Daily life is where long waits become expensive. Not only in money. In energy, patience, and quiet dignity. If driving hurts, change route length, seat setup, or break timing. If childcare lifts are the trigger, change how you lift, when you lift, or where you place the child before lifting. If desk work lights up your neck or back, shorten static postures and build in movement resets. Readers whose pain sharpens at the laptop may benefit from a more specific guide to neck pain from laptop work while they wait for specialty input.
How to think in function targets instead of vague hopes
Vague hope sounds like this: “I just want it to stop.” Function targets sound like this:
- Walk 15 minutes without a major flare
- Drive 20 minutes with tolerable symptoms
- Sleep 5 nights without waking from pain
- Type for 30 minutes before needing a reset
These are more useful because they can improve before the pain is gone. And improvement that shows up in life usually matters more than an abstract score.
Small adaptations that reduce strain without turning your life into a waiting room
You do not need a total life renovation. Often, the winning moves are embarrassingly modest: a towel roll behind the low back, alternating tasks, shorter bursts of overhead work, using both hands instead of one heroic one, setting down the laundry basket before resentment enters the chat.
Short Story: A reader once told me she spent six weeks waiting on a shoulder referral while trying to “be normal.” That phrase turned out to mean yanking the car trunk shut, carrying one heavy tote because two felt inefficient, and sleeping with the sore arm under her pillow like it owed her rent. Nothing changed until she chose three tiny rules:
no single heavy carry, no repeated overhead reaches, and a nightly note about what actually aggravated the shoulder. Two weeks later, the pain was not gone, but the chaos was. By the time she saw the specialist, she could say exactly what failed, what helped, and which movements still felt unstable. The visit moved faster because her story had stopped being fog and started being evidence.
Common Mistakes: What Makes a Long Wait Feel Even Longer
Waiting passively with no symptom tracking or care plan
The first mistake is passivity dressed up as patience. Patience is calm attention. Passivity is letting the situation become blurrier every week.
Using pain scales without describing what movements actually fail
A specialist can do more with “I cannot squat to the toilet without grabbing the sink” than with “It is about a seven.” Numbers help. Function translates.
Repeating treatments that are not helping because they feel “safe”
People repeat heat, ice, braces, stretches, and over-the-counter routines far beyond their usefulness because they feel like doing something. But if an intervention has no clear effect after a reasonable trial, keep the honesty and lose the ritual.
Underreporting worsening symptoms because you do not want to seem dramatic
This is common in thoughtful people. They do not want to bother anyone. Unfortunately, medical systems do not award medals for under-describing decline.
Overreporting panic while underreporting function loss
Emotion deserves space. But if fear gets all the airtime, the concrete changes may stay hidden. “I’m worried” is true. “I now limp by the end of the day and cannot carry groceries” is actionable. For some people, this spiral also becomes internet-fueled symptom doomscrolling, which is why a piece on cyberchondria and chronic pain can be strangely clarifying.
Quote-prep list
- When did this start or change?
- What 3 tasks are most affected?
- What have you already tried, and what happened?
- Any weakness, numbness, swelling, locking, fever, falls, or sleep loss?
- What is the one question you want answered next?
Neutral action: Put these in your phone notes before your next call or visit.
The Appointment Before the Appointment: How to Prepare for the Orthopedic Visit
Bring a one-page summary so the specialist sees the shape of the problem quickly
Specialist appointments often move fast. Your job is not to impress. It is to compress. One page is ideal. Think of it as a map, not a memoir.
- Body part and main symptom pattern
- How long it has been going on
- Top functional limitations
- Red flags absent or present
- What you tried and what happened
- What question you need answered
List what has already been tried, what made things worse, and what question you need answered
Useful questions sound like this:
- “Does this pattern suggest a tendon, joint, nerve, or spine issue?”
- “What should I avoid while trying to preserve function?”
- “Would imaging change treatment right now?”
- “What is the best next conservative step?”
Turn “my pain is bad” into “I need help understanding why this movement fails and what the next step should be”
That sentence alone can upgrade the visit. It tells the clinician you are not just seeking sympathy. You are seeking a decision pathway. And if the next branch in that pathway involves injections rather than immediate surgery, some readers like to compare pain management options before a cortisone injection so the appointment starts with sharper questions.
Infographic: The 4-step waiting-period workflow
1. Screen
Check for red flags, worsening neurologic changes, fever, major trauma, or sudden function loss.
2. Protect
Use conservative care, load modification, pacing, and simple daily adaptations.
3. Track
Log triggers, movement limits, sleep disruption, swelling, numbness, and what actually helps.
4. Prepare
Bring a one-page summary and one clear next-step question to the referral visit.
When to Seek Help: Signs the Waiting Strategy Is No Longer Enough
When pain, weakness, swelling, falls, fever, or rapidly changing symptoms need reevaluation
There is a point where “monitor and manage” stops being disciplined and starts becoming stale. If symptoms are changing meaningfully, the plan should change too. New weakness, escalating swelling, falls, fever, a dramatic pain jump, inability to bear weight, or new numbness are all reasons to re-contact a clinician sooner.
When sleep loss and function decline become their own medical issue
Sleep loss is not decorative suffering. If pain is repeatedly wrecking sleep, work, mobility, or caregiving, that matters clinically. It changes stress load, recovery, mood, and safety. It can also make every symptom feel louder, which is rude but very human.
When the safest next move is escalation, not endurance
Endurance is not always wisdom. Sometimes the courageous move is escalation: calling primary care again, asking whether worsening symptoms change triage, seeking urgent evaluation, or clarifying whether physical therapy or a musculoskeletal clinician can start earlier. The system may be slow. Your reassessment should not be.
- New symptoms matter more than calendar age alone
- Sleep loss and function decline count
- A slow system is not permission to ignore change
Apply in 60 seconds: Decide now what change would trigger a same-day call back to a clinician.
FAQ
What can I do for orthopedic pain while waiting for a referral?
Start with red-flag screening, then build a simple interim plan around load reduction, pacing, gentle movement, symptom tracking, and protecting key tasks like sleep, work, and stairs. The goal is not to fix everything alone. It is to keep the problem from getting fuzzier or more disabling while you wait.
Should I get imaging before I see the orthopedic specialist?
Sometimes, but not automatically. Imaging is most useful when it answers a specific clinical question or when red flags or severe structural concerns are present. Ordering it too early can raise costs and confusion without changing what happens next.
Can primary care or physical therapy help before orthopedics?
Yes, often. Primary care can screen for urgent issues, start conservative treatment, review medications, and update the referral if symptoms worsen. Physical therapy may help preserve motion, reduce flares, and improve function, depending on the problem and your local access and insurance rules.
How do I know whether my pain is getting dangerous instead of just annoying?
Danger is more about pattern than annoyance. New weakness, numbness, fever, major swelling, inability to bear weight, falls, bowel or bladder changes, severe night pain with other concerning features, or symptoms after serious trauma deserve faster medical attention.
Is it better to rest completely or keep moving?
Usually neither extreme works well. Relative rest and activity modification are generally more useful than total shutdown. The sweet spot is enough movement to preserve function without repeatedly triggering major flares.
What should I track so the specialist visit is more useful?
Track triggers, time of day, sleep disruption, range-of-motion limits, swelling, numbness, weakness, instability, and what treatments you tried. Also record what improves function, not just what briefly changes pain.
What if my referral wait time keeps getting pushed back?
Re-contact the referring office and describe any meaningful symptom change or function decline. Ask whether updated symptoms affect prioritization, whether another specialty is appropriate, and whether conservative support such as physical therapy can begin sooner. If insurance barriers enter the picture, readers sometimes need a separate plan for a denied second opinion for orthopedic pain rather than assuming the original referral path is the only path.
Can urgent care help with musculoskeletal pain, or will they just refer me again?
Urgent care can be useful for sudden worsening, new swelling, new inability to bear weight, suspected fracture, or other acute changes. For stable long-story problems, they may still refer you onward, but that visit can still document a clinically important change.
Next Step: Do One Concrete Thing Today
Start a simple symptom-and-function log for the next seven days
Nothing elaborate. One minute in the morning. One minute at night. Note the trigger, the task it affects, sleep impact, and whether function is trending up, flat, or down.
Write down three movements or tasks your pain is interfering with most
This is the shortest path from helplessness to clarity. Not because it makes the pain disappear, but because it turns an abstract complaint into a real clinical story.
Prepare one sentence that explains what you need the next clinician to help decide
Try this template: “I need help understanding why this movement or task is failing, what I should watch for, and what the best next step is while protecting function.”
The curiosity loop from the beginning closes here: the wait does not have to be empty. It can be a planning window. In the next 15 minutes, make your one-page summary, start your seven-day log, and decide what symptom change would mean you should escalate sooner. That alone can turn a stalled referral into a more useful, safer path.
Safety / Disclaimer: This article is general health-navigation education, not diagnosis or individualized medical advice. Musculoskeletal pain ranges from routine strain to urgent neurologic, infectious, traumatic, or circulatory problems. Seek prompt medical care for red-flag symptoms, rapidly worsening weakness or numbness, major swelling, severe trauma, fever with concerning pain, loss of bladder or bowel control, or sudden major loss of function.
Last reviewed: 2026-04.
