
Lumbar Facet RFA vs Repeat Facet Steroid Injections
If your back pain relief keeps expiring on a 90-day schedule, it’s not just your spine that’s tired—your calendar is, too.
Most people stuck deciding between these treatments aren’t chasing “perfect pain control.” They’re trying to stop the loop of procedure days, recovery days, and the weird hope that the next round will last longer. The catch is brutally unglamorous: if the facet joints aren’t the main pain generator—or if your last block wasn’t measured cleanly—both options can look like a failure.
Keep guessing and you lose months to “maybe,” plus money, time, and the confidence to plan anything.
This post gives you a decision path based on duration and function: how to interpret medial branch block (MBB) percent relief cutoffs, what relief “curves” mean, when RFA tends to buy a longer window (often tied to nerve regrowth), and how to set a stop-rule before repeating injections.
It’s built around real-world tracking: pain + three functions at 2, 6, 24, and 48 hours, then daily—so your next step isn’t vibes.
Here’s the part that changes everything:
- ✓ First, we make “lasts longer” measurable.
- ✓ Then we prove the generator.
- ✓ Then we compare the repeat-visit burden.
Table of Contents
Lasts Longer: what “3–6 vs 6–12+” really means
People say “lasts longer” and mean “keeps me out of the clinic.” Reasonable. But you’re comparing three clocks:
- Pain clock: how long your pain score drops.
- Function clock: how long life gets easier (sleep, sitting, stairs, driving).
- Calendar clock: how often you re-book, re-plan, and re-recover.
Open loop (we’ll close it): The question that decides the timeline for both options isn’t “How many months?” It’s: “Did we prove the facet joints are the main generator?”
Personal aside: I’ve watched smart, organized people get defeated by one thing: the moment they realize the “real cost” wasn’t pain. It was all the rescheduling around pain.
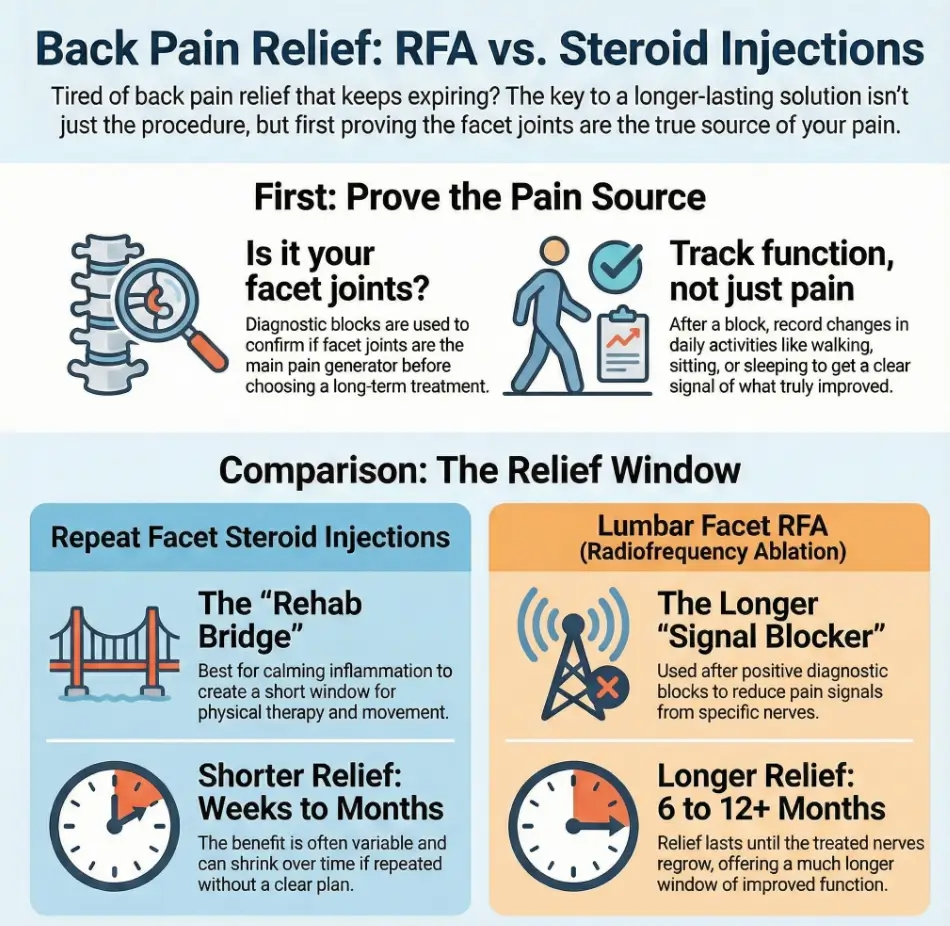
“Lasting” isn’t pain-only: the 3 metrics insurers don’t grade (but your life does)
Insurance wants documentation. Your body wants fewer “nope days.” Pick 2–3 outcomes you can feel: fewer procedure days, more walking days, better sleep, less rescue medication risk from back-pain NSAIDs. That becomes your scoreboard.
Open loop: the one question that changes the timeline for both options
Ask your clinician: “What would make you confident my pain is facet-dominant?” If the answer is vague, your timeline will be vague too.
The relief curve: steady, fading, or yo-yo (and why the shape matters)
Steady relief supports rehab. Fading relief signals you need a better plan, not “one more.” Yo-yo relief is the trap: a great week, then back to baseline, then you chase that first week forever.
Facet Pain First: prove you’re treating the right generator
Facet joints can cause deep, mechanical low back pain—often worse with extension (leaning back) and twisting. But “facet-ish” pain can also come from discs, the SI joint, hip issues, or nerve compression. That’s why the same procedure can look brilliant for one person and useless for another.
Let’s be honest… your MRI isn’t the diagnosis
Facet arthritis on imaging is common. Some people feel nothing. Others hurt badly with modest findings. Imaging is context; the diagnosis is the match between pain pattern, exam, and response to a targeted test.
Micro-story: One of the most heartbreaking clinic sentences is, “But my MRI looks terrible.” Your MRI can look dramatic and still not be the main source of today’s pain.
Facet clues vs “not facet” clues: the 2-minute pattern check
- More facet-ish: back-dominant ache, worse standing/extension, local tenderness, stiffness.
- Less facet-ish: sharp leg pain below the knee, progressive weakness, bowel/bladder changes, fever.
Diagnostic blocks: what a “good test” looks like in real life
Major pain centers describe medial branch blocks and facet joint injections as tools to confirm the pain source and create a rehab window. Your job is to track: What changed? For how long? Which activities improved? That data drives the next step.
- Yes/No: My worst pain is mainly in the back (not primarily down the leg).
- Yes/No: I had clear, time-linked relief from a targeted block.
- Yes/No: I can name 2 daily functions that improved during relief.
- Yes/No: I know which levels were treated (write them down).
Neutral next step: If 2+ answers are “No,” ask for clarity and the procedure note before repeating anything.
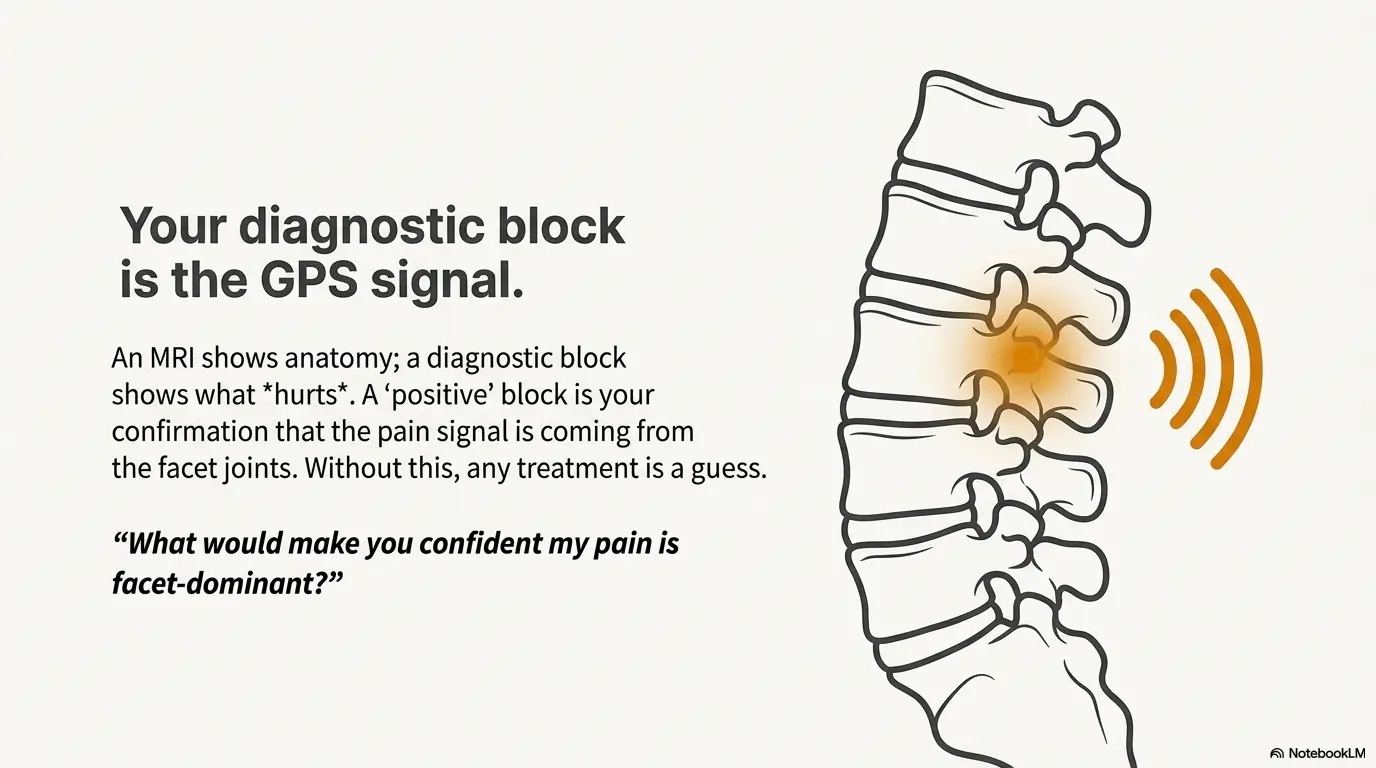
RFA Mechanics: why lumbar facet RFA can last 6–12+ months
Lumbar facet RFA targets the medial branch nerves that carry pain signals from facet joints. It’s not “fixing arthritis.” It’s reducing the signal so you can move and rebuild capacity.
What gets treated: medial branch nerves in plain English
Two small nerves feed each facet joint. RFA uses heat at the needle tip to create a tiny lesion that dampens pain signaling. Technique and targeting matter.
Nerve regrowth isn’t failure—it’s the mechanism
Patient-facing guidance from major institutions (including Cleveland Clinic) commonly notes that relief can last months and is often described in the 6–12 month range, with variability. Treated nerves can regrow, which is why repeat RFA is sometimes considered when the diagnosis still fits. If you want a deeper timeline discussion, see lumbar medial branch RFA duration (what “months” usually means in real life).
Micro-story: I’ve seen people panic at week 2 because they feel sore and think “it didn’t work.” Two weeks is too early to grade a months-long bet.
Open loop: the overlooked technique detail that quietly decides outcomes
Ask: Which levels? Which guidance (fluoroscopy or CT)? How will placement be confirmed? “Same procedure” isn’t always the same.
Show me the nerdy details
RFA outcomes vary with technique and patient selection. If diagnostic blocks are muddy (sedation effects, mixed pain generators, inconsistent function tracking), duration comparisons become unreliable. Strong selection makes head-to-head duration talk more meaningful.
Steroid Reality: what repeat facet steroid injections are actually “for”
Facet steroid injections can calm inflammation and buy a rehab window. They can be smart. But if your only plan is “repeat when it wears off,” the benefit can shrink—and your life becomes scheduled around procedures.
The 3 jobs injections do (and only one is “long relief”)
- Diagnostic clue: did a targeted shot change your pain pattern?
- Symptom calm-down: a shorter window can still be useful.
- Rehab bridge: the payout is what you do inside the window.
Here’s what no one tells you… early relief can be misleading
It’s common to feel a fast change because local anesthetic can “turn down the volume” before any steroid effect plays out. That first-day glow is information—but it’s not the whole story.
Micro-story: The worst accidental flex is using your “good day” to do everything you’ve avoided for three months. It feels heroic. It also scrambles the data.
Repeats over time: why benefit can shrink (and what to do before the next one)
Set a stop-rule: “If relief lasts less than X weeks twice, we reassess the generator and plan.” The stop-rule protects you from the treadmill.
Head-to-Head Table: duration, function, and repeat-visit burden
Evidence is messy because studies differ in technique, selection, and what they measure. Still, systematic reviews comparing radiofrequency and steroid injections across spine joint pain populations often show stronger short-term results for radiofrequency in pooled analyses, with less certainty as you push into longer follow-ups. Use that as a compass, not a promise.
| Decision factor | Lumbar facet RFA | Repeat facet steroid injections |
|---|---|---|
| Best use | Longer signal reduction after positive blocks | Bridge to rehab / flare control |
| Typical duration | Often months; commonly described as longer than steroid windows | Variable; can be shorter, sometimes weeks–months |
| Repeat-visit burden | Lower if it works; repeat when pain returns | Can become frequent if chasing short windows |
| Common disappointment | Wrong generator or missed levels; early soreness misread as failure | Shrinking benefit; no stop-rule; rehab not built |
Use it: schedule mobility/strength work while the window is open.
Use it: build tolerance so regrowth doesn’t equal relapse.
Risk Tradeoffs: what people regret after choosing
Regret usually sounds like: “I expected a cure,” “I didn’t track anything,” or “I kept repeating because uncertainty felt worse than pain.” Our brains hate uncertainty. Your spine hates rushed decisions.
Steroid repetition: the risk questions that matter to you
- If you have diabetes/prediabetes: “How might steroids affect my sugars for the next few days?”
- If bone health is a concern: “How do you think about cumulative exposure?”
- For everyone: “What’s the repeat plan before we re-evaluate?”
RFA tradeoffs: what it can feel like
Some people feel bruising or a “sunburn” sensation for days to a couple of weeks. Many return to usual activities quickly, but early soreness can still be real. Don’t grade the outcome on day 2.
Rare-but-serious: symptoms that should never be “wait and see”
Fever, severe increasing redness, drainage, or new progressive weakness deserve immediate attention.
Who It’s For / Not For: the scenario filter (US-focused)
Use these as quick self-sort cards—not self-diagnosis.
- Clear block response
- Back-dominant mechanical pain
- You want fewer repeats
Next step: confirm treated levels + guidance.
- Need a bridge to PT
- Flare pattern
- Diagnosis still forming
Next step: define the stop-rule now.
- Red flags
- Dominant nerve symptoms
- Generator unclear
Next step: get evaluated before procedures.
Who this is for / not for
For RFA: facet-dominant story + meaningful block response + function change you can describe.
For injections: a short window can be strategic—especially with a rehab plan and pacing.
Not for either (today): when red flags or dominant nerve symptoms need urgent evaluation.
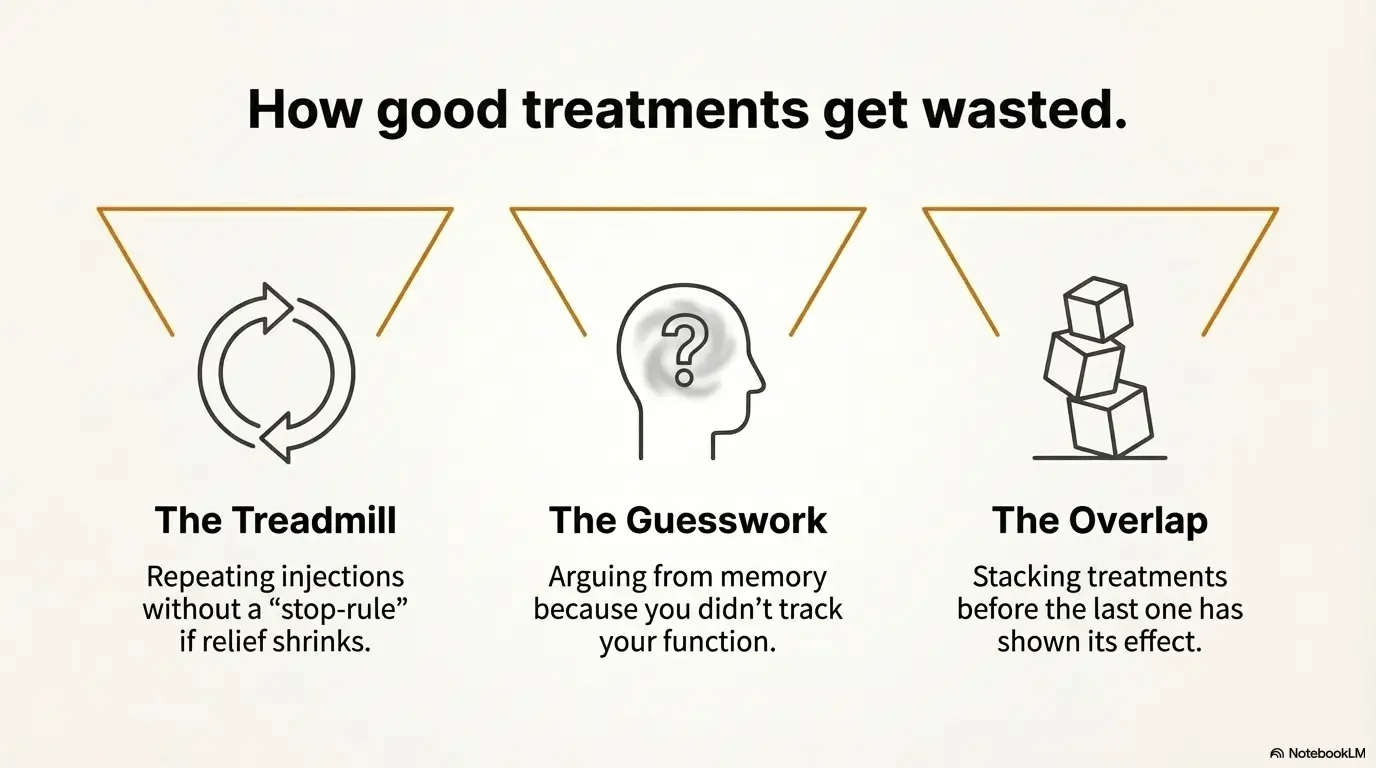
Mistakes That Shorten Relief: how good treatments get wasted
This is the loss-prevention section. Not because you’re careless—because chronic pain makes everyone fast.
Mistake #1: repeating steroids without a stop-rule
If the relief window is shrinking, the stop-rule protects you from becoming a frequent flyer.
Mistake #2: skipping a function diary (then arguing from memory)
Memory is unreliable under stress. Track pain plus three functions. That’s enough to guide the next decision.
Mistake #3: stacking treatments before the last one declares itself
Give each step time to show a trend. Otherwise you’ll never know what helped—and you’ll keep paying for uncertainty.
- Stop-rule prevents the treadmill
- Diary makes your block data usable
- Patience stops expensive stacking
Apply in 60 seconds: Put this in your phone notes: “If relief lasts under ____ weeks twice, we reassess.”

Cost & Coverage: the US pathway that quietly shapes your options
In the U.S., the path often looks like: conservative care → diagnostic blocks → RFA (if blocks are clearly positive). Many insurers, including Medicare and commercial plans, want evidence you’re targeting the right nerve before approving a longer intervention.
Micro-story: The most common “insurance surprise” is that you thought you were choosing a procedure, but you were really entering a workflow. Asking for the workflow early saves weeks.
3 inputs. 1 estimate. No storage.
Estimated yearly burden: —
Neutral next step: Decide if “fewer visits” is a top-3 priority before you choose.
What to request in writing
- Exact procedure name (facet injection vs medial branch block vs RFA)
- Levels treated
- Imaging guidance used
- Follow-up plan (including the stop-rule)
- Diagnosis and procedure codes (office can provide)
- Facility type (hospital outpatient vs ASC)
- Whether sedation is planned
- Deductible and out-of-pocket max status
Neutral next step: Gather these before you compare timelines or costs.
When to Seek Help: red flags before/after procedures
Keep this section. The riskiest move isn’t choosing the “wrong” option; it’s ignoring a red flag because you’re focused on the schedule.
Before: red flags that need urgent evaluation
- New or worsening weakness
- Bowel/bladder changes
- Fever or feeling systemically unwell with back pain
- Major trauma or cancer history with new severe pain
After: red flags after an injection or RFA
- Fever/chills, severe increasing redness, drainage
- New progressive numbness or weakness
- Severe worsening pain that doesn’t match your expected course
If you feel unsafe today: what to ask the clinic now
- “Is this expected post-procedure pain or a complication?”
- “What symptoms mean I should go to urgent care or the ER?”
- “Who do I call after hours?”
FAQ
What lasts longer—lumbar facet RFA or facet steroid injections?
For confirmed facet-mediated pain, RFA often provides a longer relief window than repeat steroid injections. The best choice depends on whether facets are truly the primary generator and whether function improved during diagnostic/therapeutic windows.
How long does lumbar facet RFA last on average?
Duration varies. Many clinicians describe relief in the months range, often around 6–12 months, but some shorter or longer. If pain returns as nerves regrow, repeat lumbar medial branch RFA timing and expectations may be discussed when the diagnosis still fits.
How long should a facet steroid injection last?
It varies from days to a few months. The most useful measure is what function you regained and how long that function stayed improved—not just the first 24 hours.
Do I need one or two medial branch blocks before RFA?
Protocols vary by clinician and insurer. Some pathways use one block; others use two to reduce false positives. Ask what your plan requires and what counts as a positive response—and if you want to be very specific, ask about what percent relief counts as a “positive” MBB for RFA.
What if the block helped only 50%?
A partial response can still be meaningful—especially if function improved clearly. It can also signal mixed generators. That’s when reassessing the source is more valuable than rushing.
Can lumbar facet RFA be repeated if pain returns?
It can be repeated in selected patients if it helped meaningfully and facets are still the likely generator. If the first round barely helped, repeating without re-evaluation is usually low value.
Is facet pain the same as sciatica?
No. Sciatica typically involves nerve root irritation with radiating leg symptoms. Facet pain is more often back-dominant and mechanical. People can have both—so it helps to understand what sciatica nerve pain feels like, and how clinicians sort out sciatica vs a herniated disc pain pattern (and, in some cases, sciatica vs piriformis syndrome).
Next Step: one concrete action for this week
Do a 7-day function-first diary. Not fancy. Not perfect. Just true.
- Daily pain (0–10)
- Three functions: choose 3 (sleep, sitting 30 minutes, stairs, walking, driving)
- One trigger note: extension, twisting, long standing, etc.
Bring three questions to your appointment:
- Is this facet-dominant or mixed?
- What’s our stop-rule if relief fades fast?
- If it doesn’t last, what’s Plan B?
This closes the open loop from the start: timelines get clearer when the generator is clearer. That’s how you stop buying hope in three-month installments—and start buying clarity. If you’re also trying to avoid missing something urgent in the noise, bookmark when low back pain is an emergency.
Last reviewed: 2025-12-18
