
The injection is rarely the hardest part. The hard part is the 48 hours after—when your brain rewrites everything into a verdict: miracle, failure, or “I’m out of moves.”
If you’re living with CRPS in the leg, that emotional whiplash can cost you the one thing you actually need: a clean, usable signal. And without that signal, you end up repeating procedures (or quitting them) based on vibes.
A lumbar sympathetic block for CRPS in the leg is an image-guided injection near the lumbar sympathetic chain, intended to reduce sympathetically maintained pain and shift vasomotor signs like temperature, color, or sweating. Relief can be brief or meaningful—and “no change” can still be actionable data when you measure it right.
Keep guessing, and you lose time, money, and rehab momentum that depends on a steady plan.
This post gives you a track-and-decide method: what to measure, what “counts,” and how to use any relief window with graded movement that supports recovery—without triggering a flare. You’ll also get a copy/paste results diary and a simple first-72-hours triage framework.
- No spiraling.
- No endless-injection loop.
- Just data you can bring to your next appointment.
- Track function (stairs, steps, sleep), not just pain.
- Use any relief window for safe, graded movement.
- Know your “call now” symptoms before you go home.
Apply in 60 seconds: Decide one functional test you’ll repeat daily (ex: “stairs once,” “10-minute walk,” or “shoe tolerance”).
Safety / Disclaimer
This article is general education, not medical advice. CRPS is complex and highly individual. A lumbar sympathetic block has risks and may not be appropriate for everyone. Discuss your meds, medical history, and specific risks with a licensed clinician. If you develop severe or worsening symptoms after an injection—such as fever, new weakness, chest pain, trouble breathing, fainting, or a severe headache—seek urgent medical care.
Table of Contents
Lumbar sympathetic block basics—what it actually does
If CRPS in the leg feels like your nervous system is running a fire alarm with the volume stuck at 9, an LSB is one attempt to turn that volume down—specifically on the sympathetic side of the wiring. The sympathetic nervous system helps regulate things like blood vessel tone (temperature, color), sweating, and “fight-or-flight” responses. In some CRPS cases, sympathetic activity is tangled up with pain signaling.
That’s why an LSB isn’t “a regular back shot.” It’s a targeted injection near the lumbar sympathetic chain with the goal of interrupting sympathetically mediated pain signals and/or changing blood flow patterns in the leg. Sometimes you see a temperature shift. Sometimes pain drops. Sometimes nothing changes—and that “nothing” is still information.
Show me the nerdy details
Clinical descriptions (including StatPearls-style summaries and major hospital patient pages) commonly frame lumbar sympathetic blocks as interventions near the lumbar sympathetic chain used for conditions where sympathetic activity may be contributing to pain. Imaging guidance and careful technique are emphasized due to nearby structures and the need for accurate placement.
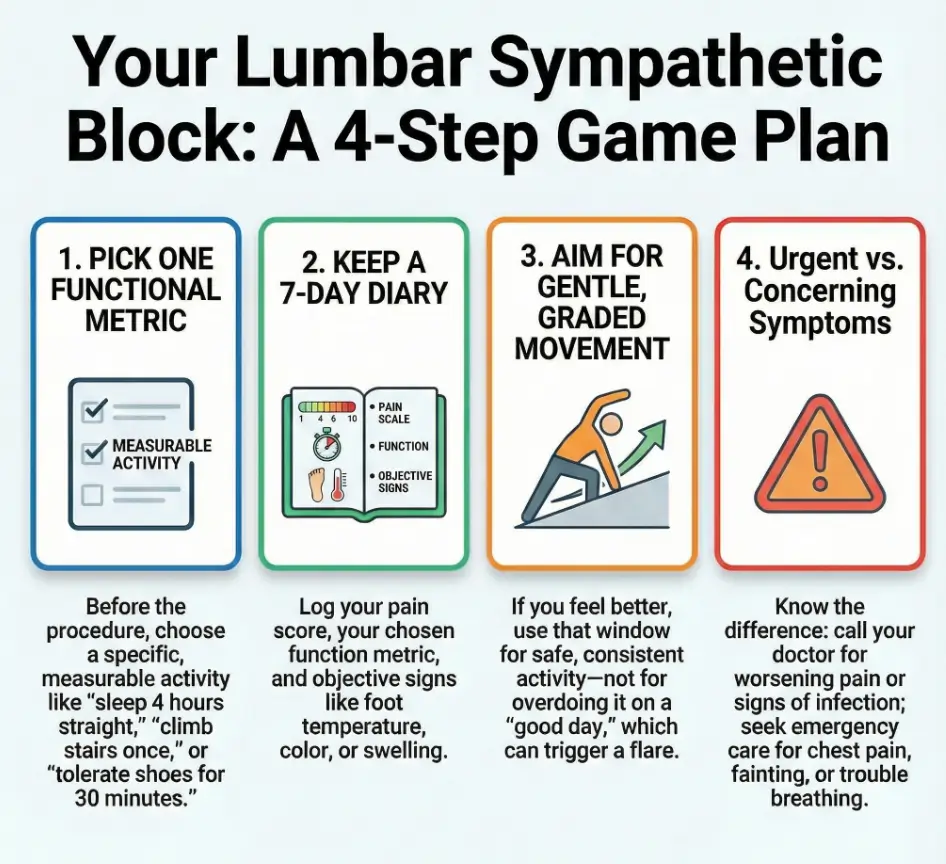
Quick skim: what people mean by “it worked”
- Signal win: you got a measurable change (temperature, color, sweating, function) even if pain didn’t vanish.
- Relief win: pain dropped enough to move, sleep, or tolerate rehab with less fear.
- Planning win: the response clarified the next step (repeat? change approach? reassess diagnosis?).
A common scene: you pull on a sock and notice the foot feels warmer. You want to celebrate—and you should—but you also want to measure. CRPS is sneaky like that. It will let you borrow hope for 12 hours, then ask for interest.
Here’s what no one tells you: blood flow can change without fixing pain (yet)
A warmer foot can mean sympathetic tone changed. It doesn’t automatically mean the full pain network quieted down. Think of it like opening one lane on a traffic jam: you may see movement, but you’re not done clearing the highway.
- Look for objective changes (warmth, color, sweating).
- Match them to function changes (walking, stairs, sleep).
- Write it down before memory edits it.
Apply in 60 seconds: Take a baseline foot temperature (same time daily) for 3 days before any procedure.
CRPS leg fit check—who it’s for / not for
This section is not a gatekeeping quiz. It’s a time-saver. Because time-poor readers don’t need 2,000 words of “maybe.” You need a fast way to decide if an LSB conversation is reasonable—or if you should slow down and address a different bottleneck first.
Who this is often for (in real clinic conversations)
- People with CRPS-like leg symptoms where sympathetic features may be present (temperature/color changes, sweating shifts).
- People whose care team is trying to clarify whether pain has a sympathetically maintained component.
- People who need a relief window to safely restart rehab or graded exposure.
Who this is often not for (or needs extra caution)
- Active infection or uncontrolled medical issues that raise procedural risk.
- Situations where medication risks (like anticoagulants/blood thinners) require careful planning.
- Anyone whose expectation is “one injection will fix my CRPS.” (That expectation is emotionally understandable—and strategically dangerous.)
Quick question: what outcome would make this “worth it” for you?
Not “pain 0/10.” Something you can actually observe: sleep 2 extra hours, stairs once without a flare, shoe tolerance for 30 minutes, PT session completed. This “worth it” metric becomes your anchor when emotions start bargaining.
- Yes/No: Can you name one functional goal you’ll measure daily for 7 days?
- Yes/No: Do you have a follow-up plan (PT/OT/graded movement) to use any relief window?
- Yes/No: Have you reviewed meds and bleeding/infection risk with your clinician?
- Yes/No: Do you know what symptoms require same-day calling vs urgent care?
Neutral action: If any answer is “No,” write it as your next appointment question—then fix that gap before deciding.

LSB purpose split—diagnostic test or therapy (or both)?
Competitor pages often imply a simple story: “We do the block; you get relief; we repeat if helpful.” The real story has a fork. Your clinician may use the block to test a hypothesis (diagnostic), to create a treatment window (therapeutic), or both.
Diagnostic: “Does the sympathetic system seem involved?”
A meaningful change in certain signs (like temperature differences or pain patterns) can support a clinical picture. It doesn’t “prove” anything with courtroom certainty, but it can guide next steps.
Therapeutic: “Can we buy a safer rehab window?”
Sometimes the best use of relief is not celebration—it’s movement. Not heroic movement. Measured movement. The goal is to gently re-train the nervous system while it’s less reactive.
Open loop (answered later): why a “meh” first result can still be useful
If you came here because the first block didn’t feel dramatic, keep reading. We’ll map what to track and what questions to ask so “meh” becomes information, not despair.
Micro-contrast: Relief is a feeling. A response is data. You want both—but data is what changes plans.
Before you book—10 questions that prevent regret
If you only do one thing before an LSB, do this: walk in with a question list that forces clarity. Not because your clinician is hiding anything—because clinics are busy, and “we’ll see” is the default language of rushed medicine.
10 questions to ask (copy/paste)
- What is the primary goal in my case: diagnostic clarity, symptom relief, or a rehab window?
- What changes would count as “responding” (pain, warmth, function)?
- What would make you recommend a second block—and what would make you stop?
- What should I do the same day (movement, rest, icing/heat) and what should I avoid?
- Will imaging guidance be used, and what type?
- What sedation (if any) is typical here—and can I drive afterward?
- Which meds/supplements should I disclose or adjust (especially blood thinners/diabetes meds)?
- What are the common side effects vs rare serious complications?
- What is my follow-up timeline (48–72 hours call? 2 weeks visit?)
- If it doesn’t help, what’s our next step—reassess diagnosis, different block type, different modality?
Let’s be honest: “wait and see” is not a plan
A plan is: measure → interpret → act. If you leave with only “call if problems,” you’re missing the most profitable part of the procedure: the learning.
- Diagnosis summary and symptom timeline (1 paragraph).
- Medication list + allergies + anticoagulants/supplements.
- Prior procedures and responses (even “no change”).
- Your baseline function metric (steps/stairs/sleep/shoe tolerance).
- Any objective signs (temperature/color/sweating changes).
Neutral action: Put this in your phone notes and bring it to your consult—clarity travels well.
Day-of walkthrough—what happens during the injection
You don’t need every technical detail. You do need a realistic mental script so your nervous system doesn’t treat the day like an ambush. Most patient-facing explanations describe a sequence: check-in, positioning, skin numbing, guided placement, medication injection, monitoring, discharge instructions.
What “guided” usually means
Imaging guidance is often used to help place the needle accurately. The aim is precision and safety—both matter when the target is near important structures.
What you might feel (and what’s normal)
- Pressure at the injection site.
- Brief discomfort during numbing.
- Temporary heaviness or odd sensations in the leg.
- Later: soreness, warmth, or a “different” temperature feel.
Show me the nerdy details
Hospital procedure pages commonly describe step-by-step flow and highlight monitoring after the injection. Clinical references emphasize anatomy, careful technique, and complication awareness. The patient experience varies, but the procedure is typically framed as outpatient with post-procedure observation.
Scene: you’re on the table, trying to breathe like a normal person. Your brain offers a highlight reel of worst-case outcomes. This is where a simple script helps: “I’m safe. I’m monitored. I’m collecting data. I can stop and ask questions.”
First 72 hours after LSB—normal, not-normal, and “call now”
The first 72 hours is where anxiety does its best work. You feel a sensation and your mind tries to interpret it as prophecy. Let’s replace prophecy with categories: expected, concerning, urgent.
| Category | What it can look like | What to do |
|---|---|---|
| Expected | Soreness, mild bruising, temporary warmth/coolness changes, “weird” sensations | Follow discharge instructions; track changes; keep activity gentle and measured |
| Concerning | Worsening pain that feels abnormal, new neurologic symptoms, signs of infection | Call your clinician or on-call service the same day |
| Urgent | Trouble breathing, chest pain, fainting, severe headache, major new weakness | Seek urgent/emergency care immediately |
If you’re scared right now—here’s the fastest way to create clarity
Set a 10-minute timer. Write down exactly what you feel (where, when it started, what makes it better/worse), then compare it to your discharge instructions. If it matches the “call” or “urgent” category, don’t negotiate with yourself—call.
Results diary—how to measure if it worked (beyond pain score)
This is the section most competitor pages don’t fully operationalize. And it’s the section that saves you money, time, and emotional energy. Because if you don’t track results, you’ll end up paying for repeats based on vibes.
The 7 relief lessons (quick skim)
- Lesson 1: Define “relief” before the needle (sleep, steps, stairs, shoe tolerance).
- Lesson 2: Warmth is data, not a trophy.
- Lesson 3: Function beats feelings—measure what you can do.
- Lesson 4: Timing matters—track hour-by-hour for the first day, then daily.
- Lesson 5: The rehab window is the real prize—use it gently.
- Lesson 6: You can’t out-inject a flare strategy—plan your pacing.
- Lesson 7: The plan after the block decides the outcome—don’t wing it.
Copy/paste: the 7-day CRPS LSB results diary
Daily (same time):
Pain (0–10): ____
Function test (pick 1): ______________________ Result: ____
Sleep (hours): ____
Foot temp (if you can): Left ____°F / Right ____°F
Color/swelling/sweating notes (1 line): _______________________
Triggers/exposures today (1 line): ____________________________
What helped (1 line): _______________________________________
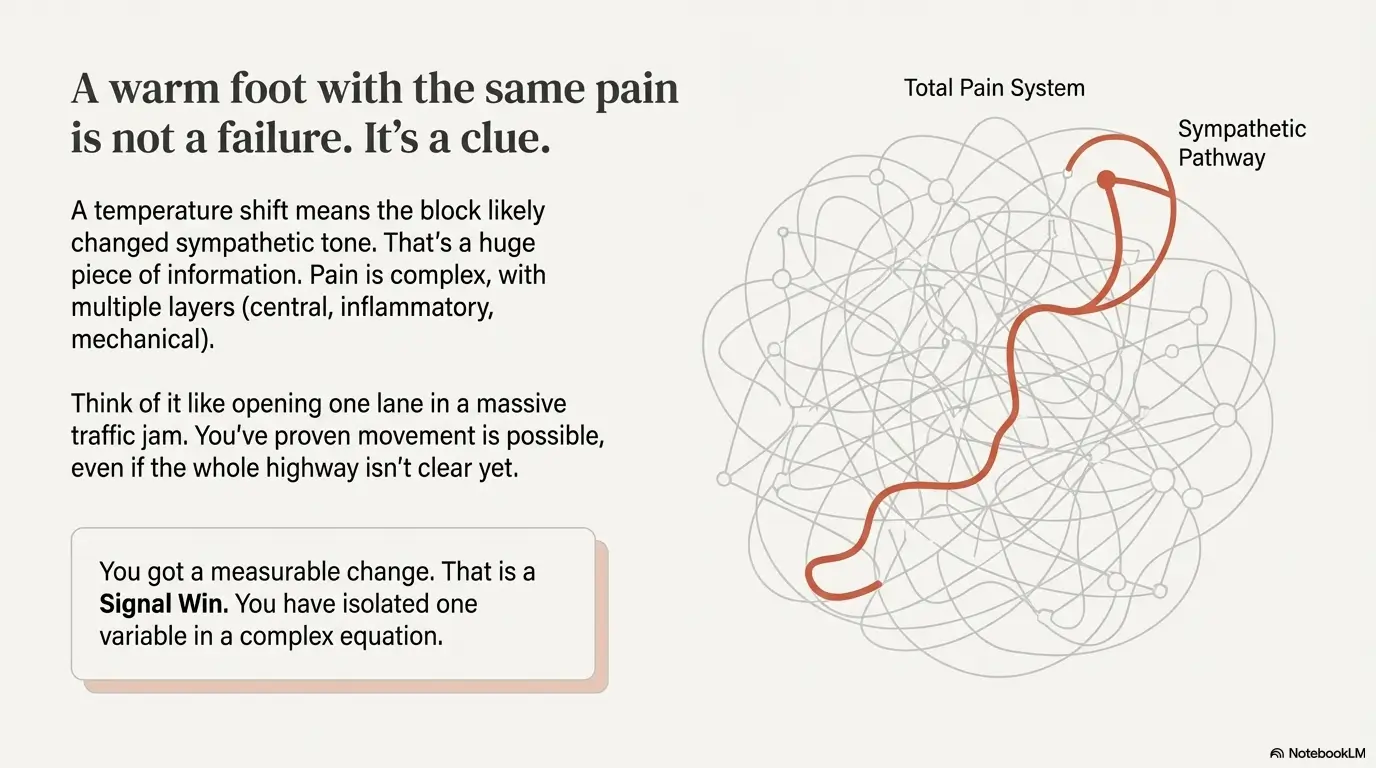
Warm foot, same pain—what that can mean (without panic)
A temperature shift can signal a change in sympathetic tone or blood flow. Pain can be driven by multiple layers—peripheral, central, inflammatory, mechanical, and emotional threat processing. Translation: one lane opened; the traffic jam isn’t fully cleared. That’s not failure. It’s a clue.
Show me the nerdy details
Many clinical explanations distinguish between objective physiologic changes (temperature, vasomotor signs) and subjective pain experience. CRPS symptoms can involve multiple systems, so single-mechanism changes may not map perfectly to pain intensity. Tracking multiple outcomes improves interpretation.
Use this to quantify your “worth it” threshold.
- Input 1: Baseline sleep hours: ____
- Input 2: Post-block sleep hours: ____
- Input 3: One function metric (ex: steps): Baseline ____ → Post ____
Output A: Sleep gain: ____ hours
Output B: Function change: ____ (units)
Neutral action: Bring these two numbers to your follow-up; ask, “Do these count as a response in my case?”
Common mistakes—how people waste the relief window
CRPS punishes extremes. Too much rest can stiffen fear pathways. Too much activity can spark a flare. The win is the middle: graded exposure and pacing.
Mistake #1: doing nothing with relief
If the block buys you even a small decrease in threat, that’s a chance to practice safe movement. Not as punishment. As retraining.
Mistake #2: overdoing a “good day” and paying for it
This one is heartbreakingly common. You feel 20% better and you try to live like it’s 80%. The nervous system doesn’t reward courage; it rewards consistency.
Mistake #3: changing five treatments at once
New meds, new supplements, new PT intensity, new brace, new everything—then the block happens. Result: you can’t interpret anything. Keep variables as stable as safely possible for 7 days.
Practical pacing rule: If you’re unsure, increase activity by 10–20%, not 200%.
Don’t do this—escaping the endless-injection loop
The “series of injections” idea can be reasonable. The trap is repeating without a decision framework. That’s how you end up in the loop: temporary relief → repeat → diminishing returns → frustration → sunk-cost thinking.
What to clarify if someone says “let’s do a series”
- What counts as a response (pain? warmth? function?)
- How long should relief last to justify repeating?
- What’s the stop point if benefits shrink?
- What’s the alternative plan if it doesn’t help?
Open loop: if relief fades fast, what should you ask next?
Ask for a re-check of the working diagnosis and mechanism. Ask whether the goal is diagnostic clarity or symptom relief. Ask what would change their plan. “Repeat it” is an action. “Why repeat it?” is strategy.
- Clear functional gain (sleep/steps/stairs)
- Objective change (temp/color) + meaningful relief
- Plan to use the window (PT/graded exposure)
- No measurable change in 7 days
- Side effects or complications concerns
- Relief too brief to act on safely
Neutral action: Pick one box you’re in and write one question for your clinician that matches it.
LSB vs other blocks—sympathetic vs peripheral (and why it matters)
Here’s the simple distinction: a peripheral nerve block targets a specific nerve path; a sympathetic block targets the sympathetic chain. That difference matters because it changes what “success” looks like and what you learn from the response.
Peripheral block: “nerve-specific targeting”
- Often used when symptoms map to a particular nerve distribution.
- May offer clearer “this nerve is involved” signals.
Sympathetic block: “system-level modulation”
- Targets sympathetic contribution to pain/vascular tone.
- May produce temperature/vasomotor shifts that need careful interpretation.
Pattern interrupt moment: If your clinic is using the same word “block” for everything, make them define which wiring they’re aiming at. The word is the same. The target is not.
If LSB doesn’t help—next smart paths (no spiraling)
If your LSB didn’t help, your brain might jump to “Nothing works.” That’s the CRPS anxiety narrative. Let’s give you a better narrative: “We collected a data point; now we refine the plan.”
Re-check the picture (without blaming yourself)
- Are CRPS features consistent and well-documented?
- Could there be mixed pain drivers (mechanical, neuropathic, central sensitization)?
- Did you track enough to interpret change (or lack of change)?
Alternatives your clinician may discuss (overview-only)
This is not a menu to self-prescribe. It’s a list to ask about. Depending on your case, clinicians may discuss different interventional approaches, medication strategies, and rehab-focused plans.
Operator move: Bring your diary and ask, “Given my data, what’s the next most informative step?”
Short Story: The most painful part of CRPS is how it shrinks your world. A reader described the moment as a tiny betrayal: the day they stopped going to the grocery store, not because it was impossible, but because it was unpredictable. After a procedure, they didn’t chase a perfect pain score. They chased one stable routine: a 6-minute walk to the mailbox and back, every day, same time, same shoes, same pacing. Some days it was ugly. Some days it was easier. But the diary proved something their mind kept forgetting: the trend line moved. Not fast. Not dramatic. But enough to rebuild trust in their own body.
Lumbar sympathectomy & other escalations—same family, different commitment
You may see “lumbar sympathectomy” mentioned in patient leaflets (especially UK/NHS materials). It’s related in concept—sympathetic pathway involvement—but it’s not the same as a block. A block is typically framed as temporary and diagnostic/therapeutic. A sympathectomy is a bigger commitment with its own risk profile and aftercare expectations.
What to ask if someone brings up sympathectomy
- What goal are we pursuing now that a block didn’t reach?
- What are the specific risks in my case?
- What does recovery and follow-up realistically look like?
Off-label steroid language (why you might hear it)
Some procedural leaflets mention that certain medications may be used in ways that are considered “off-label.” If you hear this, don’t panic—ask for the plain-English reason and the alternatives.

US logistics—coverage, documentation, and the paper trail
In the US, the procedure decision is only half the battle. The other half is documentation: what’s written, what’s coded, and what you can show as outcomes. This matters for coverage, for continuity of care, and for not repeating steps just because the record is thin.
What to request (politely, in writing)
- Procedure note (what was done, where, what meds were used).
- Discharge instructions (activity guidance and warning signs).
- Follow-up plan (timeline + what to track).
- Your clinician’s summary of the response (even if minimal).
Infographic: the CRPS LSB “decision flow”
Pick 1 function test + temp/color note. Track 3–7 days.
Know your “call now” symptoms. Keep variables stable.
Track hour-by-hour day 1, then daily. Note warmth + function.
If measurable gain: use rehab window. If not: reassess mechanism.
Accessibility note: This flow summarizes a track-and-decide approach: baseline → procedure → early tracking → next-step decision.
When to seek help—same-day call vs urgent vs 911
You don’t want to memorize every rare complication. You want a simple escalation ladder. If you’re not sure, err on the side of calling your clinic’s on-call line. That’s what it’s for.
Same-day call
- Signs of infection at the injection site (increasing redness, warmth, drainage).
- New or worsening neurologic symptoms in the leg.
- Pain that feels sharply different from your baseline pattern.
Urgent or emergency care
- Chest pain, trouble breathing, fainting.
- Severe headache, especially if accompanied by other concerning symptoms.
- Major new weakness or inability to walk safely.
Calm rule: You’re not “overreacting” when you call. You’re protecting your future self.
FAQ
How long does a lumbar sympathetic block last for CRPS in the leg?
Duration varies widely. Some people feel relief for hours, others for days or longer, and some feel no meaningful change. That variability is why tracking objective measures and function is so helpful—it tells you what actually happened in your body, not what you hoped would happen.
What does it mean if my foot gets warm but my pain doesn’t change?
Warmth can signal a change in sympathetic tone or blood flow, but pain can be driven by multiple mechanisms. A warmth-only response can still be a useful data point. Pair it with function tracking and discuss with your clinician what that pattern suggests for next steps.
How many lumbar sympathetic blocks are “normal”?
There isn’t a single universal number. Some clinicians recommend a short series when there’s measurable benefit, while others reassess quickly if the response is unclear. The key is to set repeat/stop criteria upfront using your function metrics and your risk tolerance.
Can an LSB make symptoms flare?
Some people report short-term flares or “weird” sensations after procedures. That’s one reason to pace activity, keep variables stable, and use the first 72 hours as a structured observation period rather than a test of bravery. If symptoms are severe or worsening, contact your clinician.
Do I need sedation—and can I drive afterward?
Policies vary by clinic. Some patients receive light sedation; others do not. Many clinics advise arranging a driver, especially if sedation is used. Confirm your clinic’s rules before the day of the procedure so you’re not negotiating logistics while stressed.
What should I do after the block to maximize the chance of benefit?
If your clinician approves, aim for gentle, graded movement—small, consistent activity that leverages any reduction in threat response. Use your diary to prevent overdoing it on a “good day,” and to keep your rehab window from becoming a flare trigger.
What if relief lasts only a few hours—does that “count”?
It can. Short relief may still provide diagnostic information or signal that a component of your pain is responsive. The practical question is whether that window is long enough to safely act on (movement, sleep, rehab) and whether the risk/benefit supports repeating.
Closing the loop—your next step in 15 minutes
Remember the open loop from the beginning—“Did it work?” Here’s the honest answer: it worked if it gave you a clean signal you can use to make a better decision than you could make yesterday. Sometimes that signal is relief. Sometimes it’s a temperature shift. Sometimes it’s “no change,” which pushes the team to reassess the mechanism.
Your 15-minute next step (do this today)
- Copy the diary template from this article into your notes app.
- Choose one function test you’ll repeat daily for 7 days.
- Write one sentence: “A successful outcome for me is ______.”
- Bring that to your next visit and ask for a repeat/stop rule upfront.
If you want to be ruthless (in the best way), here’s the final operator rule: don’t repeat a procedure you can’t measure. Your future self deserves better than guesswork.
Last reviewed: 2025-12
