
CBT-I for Insomnia with Chronic Pain
Clock-checking, negotiating, “trying harder,” and somehow feeling more awake with every attempt. If you’re living with pain, insomnia stops being a side symptom and becomes the engine that keeps everything loud. More time in bed, more “sleep hygiene,” more apps… and still the same brittle nights—especially if scrolling on your phone in bed quietly turns into a nightly habit.
Keep guessing long enough and you don’t just lose sleep—you lose mornings, momentum, and the small resilience your body needs to handle pain. This guide is built around CBT-I (Cognitive Behavioral Therapy for Insomnia): the fastest, most evidence-backed way to make sleep less fragile—without pretending pain isn’t real.
- Find legit behavioral sleep medicine help fast
- Use sleep efficiency to track progress without spiraling
- Adapt sleep restriction safely with pain-friendly “compression” rules
- Avoid the common traps that make CBT-I feel like it “failed”
CBT-I uses a sleep diary and tailored schedule changes to rebuild sleep drive, reduce time awake in bed, and lower sleep anxiety. The goal is steadier nights and better daytime function—even when pain still shows up.
Table of Contents
CBT-I is a structured, evidence-based program for chronic insomnia that retrains sleep drive and reduces “sleep effort.” In chronic pain and other chronic conditions, the mostanys; the most reliable win is better sleep first—with pain improvements often smaller and less consistent—so you’re aiming for steadier nights and better daytime function. Choose real CBT-I (sleep diary + tailored sleep window + follow-up) from a trained clinician or vetted digital program.
Start with the loop: pain-insomnia is a two-way amplifier
Here’s the unfair part: pain makes sleep harder, and poor sleep makes pain feel sharper the next day. That doesn’t mean “it’s all in your head.” It means your nervous system is doing what nervous systems do: learning, predicting, and overprotecting.
The loop usually looks like this:
- Night: pain flares → you watch the clock → you try harder to sleep → your brain stays on duty
- Morning: you feel wrecked → you cancel movement/social plans → your body gets less resilient
- Next night: you “make up” sleep by going to bed early → more time awake in bed → more frustration
Composite moment: a reader describes lying perfectly still so they “don’t provoke” their back—only to realize they’ve spent 2 hours in bed rehearsing tomorrow’s worst-case scenario. Not dramatic. Just… predictable.
Quick self-check: are you giving yourself a lot of “sleep opportunity” (time in bed) but your “sleep ability” (actual sleep) hasn’t improved? That gap matters, because CBT-I is built to shrink it safely.
- The goal is fewer awake minutes in bed
- Not perfect sleep—more reliable sleep
- Pain can stay present while insomnia gets smaller
Apply in 60 seconds: Tonight, pick one “bed is for sleep” rule you can keep even on a bad pain day.
Open loop (we’ll close it later): the single metric clinicians watch to decide when your sleep window should expand is not “how tired you feel.” It’s a number you can calculate from your diary.
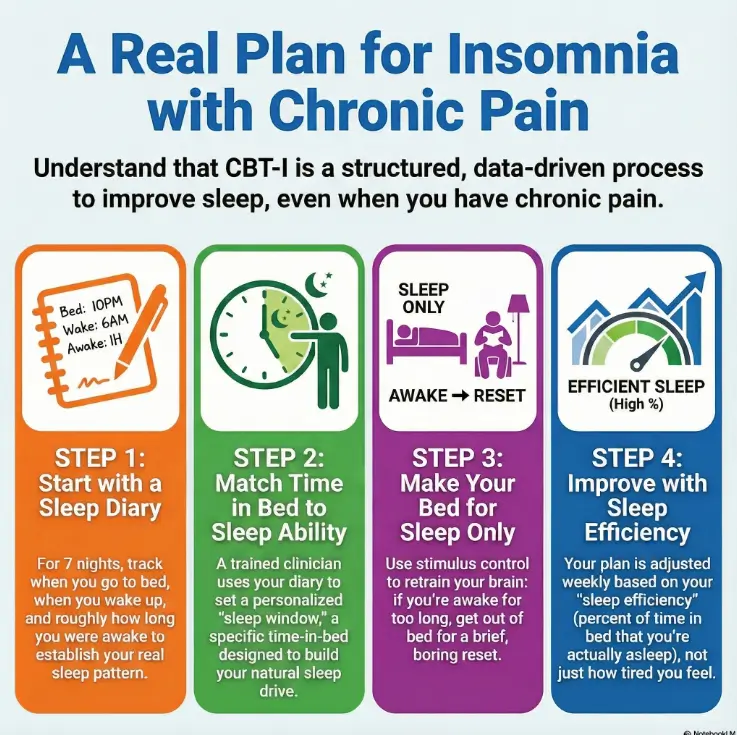
CBT-I defined: what you’re buying (and what you’re not)
CBT-I stands for Cognitive Behavioral Therapy for Insomnia. Think of it less like “therapy about your childhood” and more like a skills program that changes the behaviors and thoughts that keep insomnia alive.
Real CBT-I usually includes:
- Sleep diary tracking (your real pattern, not your worried guess)
- A tailored sleep window (time in bed set to build sleep drive)
- Stimulus control (bed = sleep, not scrolling, planning, or suffering)
- Cognitive work (reducing catastrophic sleep thoughts)
- Circadian anchors (wake time, light, timing cues)
What CBT-I is not: a generic “sleep hygiene” handout, a relaxation playlist, or a course that never adjusts to your data. Those can be supportive, but they’re not the main mechanism.
Pattern interrupt: Let’s be honest… if there’s no sleep diary, it’s not CBT-I
If a provider or program can’t tell you how they’ll use your diary to adjust your plan week to week, you’re probably buying a sleep-themed product—not CBT-I.
Composite moment: someone pays for a “CBT-I certified” course, then realizes every user gets the same bedtime recommendation. That’s like getting glasses without an eye exam. Cute, but not the point.
- YES if insomnia lasts 3+ months and affects daytime function
- YES if you spend 30+ minutes most nights trying to sleep or get back to sleep
- YES if you’re willing to track for 7 nights and follow a tailored schedule
Apply in 60 seconds: If you checked “yes” to two items, move to the provider-verification section and book an intake.
Neutral action: Screenshot the checklist and use it as your “should I pursue CBT-I?” filter.
Evidence reality: what improves first (and what’s less predictable)
People often come to CBT-I with one desperate hope: “If I sleep, my pain will disappear.” I wish that were the promise. The more honest promise is better—and it still matters: CBT-I reliably improves insomnia outcomes. In chronic pain contexts, pain improvements can happen, but they’re typically smaller and less consistent across studies. That’s not failure. That’s correct expectations.
Translation: you’re aiming for fewer long awake stretches, less dread at bedtime, and more predictable mornings. Pain may still be present, but your capacity to deal with it improves when you aren’t sleep-deprived.
Composite moment: someone notices their pain score hasn’t dropped much, but they stop canceling mornings. They can do a 12-minute walk and still function—sometimes helped by a simple, structured movement plan like physical therapy basics that make walking doable during nerve-pain flares. That’s not “nothing.” That’s your nervous system getting less brittle.
What helps you stick with it: expecting a slightly rough start. When sleep timing changes, the first 7–10 days can feel wobbly. If you quit right there, you miss the point where sleep starts consolidating.
Open loop: the point most people quit (right before it turns)
Many people drop out after the first week because they’re tired and annoyed. Reasonable! But the early phase is when you’re disrupting a long-standing pattern. Later in this article, I’ll show you what number to track so you don’t panic when it feels messy.
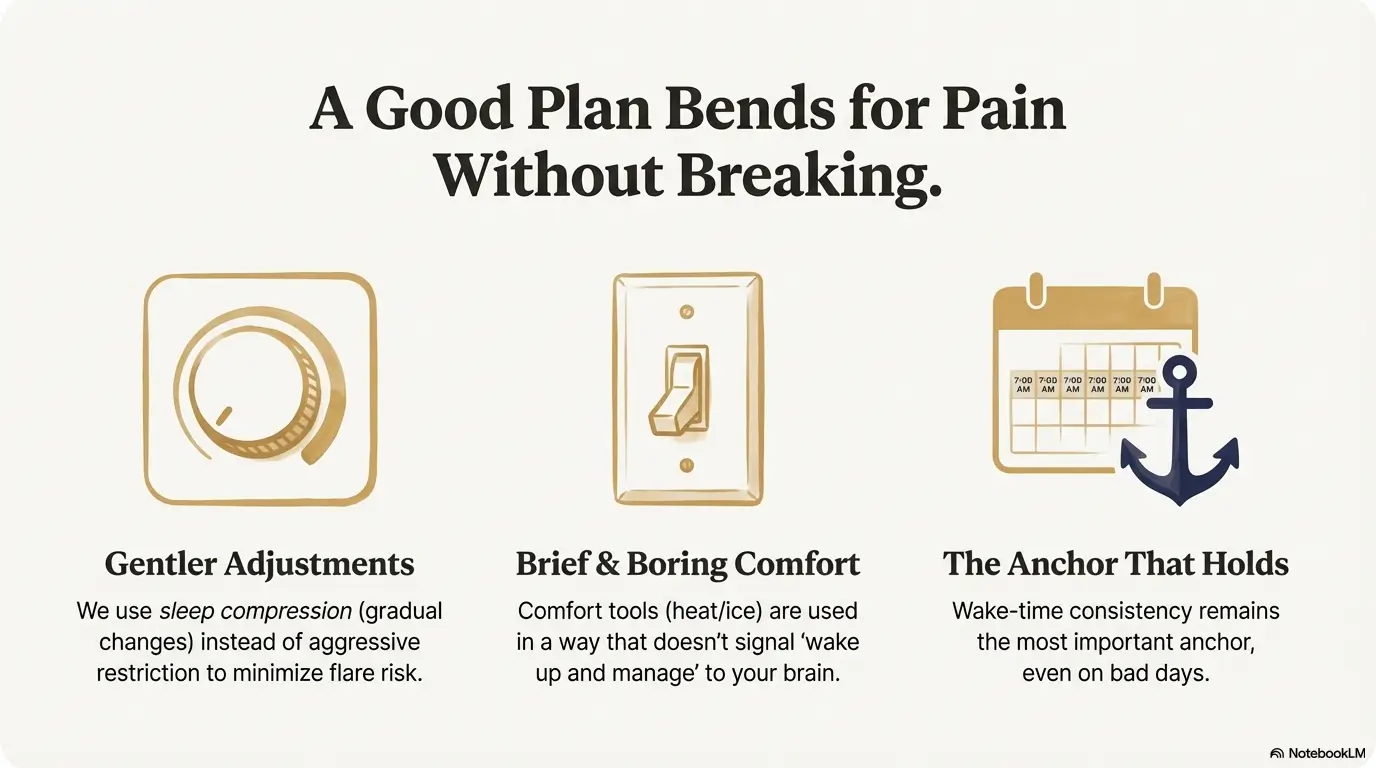
Pain-adapted CBT-I: the “rules” that must bend (without breaking)
Classic CBT-I can sound rigid on paper. Pain makes it feel even harsher—unless you adapt intelligently. A good CBT-I clinician won’t treat you like a robot. They’ll treat you like a human with a nervous system and a body that complains at 2:17 a.m.
Sleep restriction vs sleep compression (pain-friendly dial)
In pain populations, clinicians often use sleep compression rather than aggressive restriction—meaning you tighten time in bed more gently, based on your data and flare risk. The point isn’t suffering. It’s consolidating sleep.
Nighttime comfort without training wakefulness
You can use positioning, heat/ice, and medication timing in a way that doesn’t make your bed the command center of wakefulness. The line is simple: comfort tools should be brief and boring, not a whole performance that signals “wake up and manage.” (If positioning is a big part of your night, you may also find sleeping positions for neck/shoulder pain helpful as a comfort “menu” that doesn’t turn into a ceremony.)
Pattern interrupt: Here’s what no one tells you… comfort rituals can become insomnia fuel
If your routine grows to 45 minutes with special pillows, podcasts, scrolling, and negotiation with the universe, your brain learns: “Bedtime is an event.” CBT-I aims to make bedtime… unremarkable.
Composite moment: a person with fibromyalgia tells themselves they “need” three different supplements, two stretches, and an hour of reading to sleep. When they simplify to a 10-minute wind-down and a consistent wake time, their sleep becomes less fragile—even though their pain flares still happen.
- Adjust the sleep window gradually
- Keep wake-time consistent
- Use comfort tools briefly (not as a bedtime ceremony)
Apply in 60 seconds: Pick one comfort tool you’ll keep—and one you’ll remove—for the next 7 nights.
Dose and format: how many sessions/minutes actually matter?
Most CBT-I programs run about 4–8 sessions. But the real question is: do you get enough follow-up to adjust your plan based on data? If not, you’re buying information when you need iteration.
Formats you’ll see:
- 1:1 CBT-I (most tailored, often fastest to troubleshoot)
- Group CBT-I (can be efficient and effective, often lower cost)
- Telehealth CBT-I (same core mechanisms, more accessible)
- Digital CBT-I (varies widely—some robust, some basically “sleep content”)
Show me the nerdy details
Many studies describe CBT-I in terms of “dose” (sessions, minutes, weeks) and outcomes (insomnia severity, sleep efficiency, wake after sleep onset). The practical takeaway is that results depend less on fancy features and more on whether the program includes (1) structured tracking, (2) a sleep window that changes over time, and (3) accountability for adjustments. If those three are missing, it’s usually not delivering the core CBT-I mechanism.
- Sleep efficiency = (Total Sleep Time ÷ Time in Bed) × 100
- Higher usually means sleep is consolidating
- Lower often means time in bed is too wide for your current sleep ability
Apply in 60 seconds: Use the calculator below with last night’s best estimate—then discuss patterns with your clinician.
Sleep efficiency: —
This is educational only. Don’t change medications or treatment plans based on a single night.
Neutral action: Track this number for 7 nights to spot trends, then bring it to your intake.
Open loop: the one deliverable you should get every week
If the program is legitimate, you should receive (or agree on) a specific sleep window and a clear rule for how it changes based on your diary. Keep that thought—we’ll use it in the verification checklist.
Who this is for / not for (so you don’t self-blame)
CBT-I works best when the target is truly insomnia—not just “my pain was bad last night.” You can have both. But it helps to know what you’re treating.
Who CBT-I is for
- Insomnia 3+ months (trouble falling asleep, staying asleep, or waking too early)
- Daytime impact (fatigue, mood shifts, cognitive fog, irritability)
- Willingness to track and follow a tailored schedule for a few weeks
Who may need evaluation first (or parallel care)
- Loud snoring, choking/gasping, or witnessed breathing pauses (possible sleep apnea)
- Severe depression, suicidal thoughts, or mania-like symptoms
- Complex medication situations (opioids, benzodiazepines, multiple sedatives) that require clinician coordination
Composite moment: someone is “doing CBT-I perfectly” but still wakes up with headaches and daytime sleepiness. Turns out sleep apnea was part of the puzzle. CBT-I can still help insomnia—but it shouldn’t be asked to fix breathing.
Short Story: The Tuesday Night Experiment (120–180 words) …
She called it “the Tuesday Night Experiment” because naming it made it feel less personal. Tuesdays were her worst: long meetings, stiff hips, and that particular fatigue that feels like wet sand—sometimes the same pattern people describe in desk-job flare-ups that spike leg/back pain after sitting. For months, she’d gone to bed early, hoping to “bank” sleep before the next day. It never worked.
She’d lie there—still, polite, obedient—while her brain ran a highlight reel of pain. At intake, the CBT-I clinician didn’t argue with her pain. They argued with the clock. They tightened her sleep window by a small amount, anchored her wake time, and gave her one rule: if she’s awake too long, she gets out of bed for a boring reset. The first week felt rude. The second week felt steadier. By week four, Tuesday wasn’t magical—but it wasn’t a catastrophe, either. She stopped “going to bed” to fight pain, and started going to bed to sleep.
Find legit CBT-I: credentials, directories, and quick verification
This is where you protect your time and money. The internet is full of well-meaning sleep advice and lightly branded coaching. You’re looking for behavioral sleep medicine competence: someone who can implement CBT-I with tracking and adjustments.
Credentials that actually matter (and why)
- Licensed clinician (psychologist, therapist, clinical social worker, etc.) with insomnia specialization
- Behavioral Sleep Medicine training (often listed as BSM)
- ABSM certification (a strong signal, not the only path)
The 3 questions to ask on the first call (copy/paste friendly)
- “Do you provide CBT-I specifically (not just sleep hygiene)?”
- “Will we use a sleep diary and adjust a sleep window week to week?”
- “How do you adapt CBT-I when pain flares or mobility is limited?”
What good answers sound like: specific and process-driven. They mention diaries, sleep windows, stimulus control, and gradual adjustments. They don’t promise pain cures. They do promise a plan.
Red-flag phrases that often mean “not really CBT-I”
- “We don’t do sleep diaries—it stresses people out.” (that’s… the method)
- “Our program is one-size-fits-all so it’s simple.” (simple isn’t tailored)
- “Guaranteed pain elimination.” (that’s not a responsible claim)
- No diary = high chance it’s not CBT-I
- No tailored sleep window = low chance it’s effective CBT-I
- No follow-up adjustment = you’re buying information, not treatment
Apply in 60 seconds: Email the 3 questions above to two providers and compare the specificity of their answers.
Telehealth or in-person? a reality-check that protects your wallet
Telehealth CBT-I can be excellent. In-person CBT-I can be excellent. The difference is usually not “quality vs quality.” It’s logistics: availability, fit, and how your pain behaves.
When telehealth is a strong choice
- You have limited local options or long waitlists
- Travel increases pain or fatigue
- You want consistency without the extra friction of commuting
When in-person can be worth it
- You need coordinated care through a sleep clinic (screening, referrals)
- You prefer a clinic structure for accountability
- You have complex comorbidities and want a local team
Mistake to avoid: paying for a fixed “course” that never adjusts your plan
Legit CBT-I changes over time. If an app or program never changes your sleep window based on your diary, it may still be helpful—but it’s not delivering the central CBT-I mechanism.
- Telehealth if travel worsens pain or you need faster access
- In-person if you want integrated clinic evaluation and referrals
- Digital CBT-I if you need a bridge while waiting (but verify it’s structured)
Apply in 60 seconds: Decide your “must-have”: speed, tailoring, or integrated evaluation—then choose the format that delivers it.
Neutral action: Circle one must-have and use it to filter your search results.
Common mistakes: the fastest ways to make CBT-I feel like it “failed”
CBT-I doesn’t usually fail because your body is “broken.” It fails because the plan gets unintentionally sabotaged by very human decisions—especially when you’re exhausted and hurting.
Mistake #1: extending time in bed to “recover”
It feels logical. It often backfires. More time in bed can mean more time awake in bed—teaching your brain that bed equals wakefulness.
Mistake #2: turning the bed into a pain-management command center
If you do work calls, scrolling, intense stretching, arguments with your insurance portal, and a full-body symptom scan in bed… your bed becomes a high-stimulation environment. (If your nights blur into laptop-and-phone time, it may help to separate “bed” from the posture load that quietly fuels neck and shoulder pain during late-night work.)
Mistake #3: chasing perfect sleep hygiene instead of the core levers
Sleep hygiene is supportive. CBT-I is the engine. If you treat “no caffeine after noon” like the main treatment, you’re often aiming at the wrong target.
Mistake #4: quitting during a flare week
Flares happen. The skill is learning how to “hold the line” with gentle adaptations (compression, boring resets) without blowing up your schedule.
Composite moment: someone does five nights of progress, then has a flare and decides “it’s not working.” The truth is more boring and more hopeful: you hit the first real test. The next step is not quitting—it’s adjusting.
Safety + when to seek help first
Safety note: This article is educational, not medical advice. Don’t start, stop, or change prescription medications (including opioids, benzodiazepines, or sleep medications) without your clinician’s guidance.
When to seek medical help promptly
- Breathing pauses, choking/gasping at night, or severe daytime sleepiness (possible sleep apnea)
- Chest pain, severe shortness of breath, or neurological red flags
- Severe depression, suicidal thoughts, or mania-like symptoms
If your “red flags” involve severe back symptoms (new weakness, bowel/bladder changes, or rapidly escalating pain), treat it as urgent—this quick guide on when low back pain is an emergency can help you sort “today” from “watchful waiting” while you seek care.
Sleep apnea question: CBT-I can help insomnia, but it can’t fix breathing
If you suspect apnea, ask your primary care clinician or a sleep specialist about evaluation. CBT-I can still be part of your plan—but it shouldn’t be your only plan.
Cost and coverage (US): the least painful way to pay for CBT-I
Let’s talk about the part no one wants to talk about: money. CBT-I is a high-ROI intervention when it’s real and tailored—but access can be uneven. A 2025 assessment of US CBT-I providers (using a behavioral sleep medicine registry) reported that many providers were accepting new patients, but a smaller share accepted insurance, and wait times could stretch weeks. Translation: it helps to go in prepared—especially if chronic pain is already pressurizing your budget the way long-running back pain costs can quietly accumulate.
What you’re actually purchasing
- Clinical CBT-I (therapy-style billing): tailored sessions with tracking and adjustments
- Sleep clinic CBT-I: may bundle with evaluation pathways
- Digital CBT-I: varies; some require clinician involvement; some are self-guided
Fee/Rate table (real-world, US; ranges vary by location)
| Year | What people commonly run into | Range / notes |
|---|---|---|
| 2025 | Initial CBT-I session cost (out-of-pocket) varies widely | Reported average around $261; reported range $100–$530 in a registry-based assessment |
| 2025 | Follow-up session cost | Reported average around $228; reported range $75–$500 |
| 2025 | Wait times | Can be days to months; reported averages around 7 weeks in the same assessment |
How to use this table: not to panic—just to plan. If you need care sooner, consider telehealth options or a vetted digital bridge while you wait.
Insurance, superbills, HSA/FSA (practical path)
- Ask the office: “Are you in-network? Do you accept my plan? What’s the CPT/diagnosis coding typically used?”
- If out-of-network: request a superbill and ask your insurer about reimbursement
- If time-poor: use HSA/FSA if eligible and the provider supports itemized receipts
One cost “gotcha” to ask about up front is whether your visit is billed in a setting that adds extra fees—especially if it’s a hospital outpatient facility fee situation. If you’re comparing options, this breakdown of hospital outpatient vs ASC facility fees can help you know what questions to ask before you commit.
If you can’t access a CBT-I clinician (safe fallback ladder)
- Start a sleep diary for 7 nights
- Use a structured CBT-I tool designed to support clinician care (not replace it)
- Schedule the soonest legit intake you can find, even if it’s telehealth
Composite moment: someone spends $300 on supplements because it’s “faster than therapy.” Then they realize one CBT-I intake would have given them a plan instead of a shopping bag. No shame—just a painful lesson.
Next step: one concrete action you can take today
If you do nothing else, do this: spend 15 minutes turning “research mode” into a booked intake. You don’t need motivation. You need a script.
Do this in 15 minutes (script included)
Subject: Request for CBT-I intake (chronic insomnia + chronic pain)
Hi [Name/Clinic],
I’m looking for CBT-I for chronic insomnia alongside chronic pain. Do you provide CBT-I with a sleep diary and weekly sleep-window adjustments?
If yes, what’s your earliest appointment (telehealth OK), estimated cost/insurance options, and what should I track before intake?
Thank you, [Your Name]
Bring this to session: 7 nights of a simple sleep + pain diary
- Bedtime, estimated time asleep, final wake time
- Longest awake stretch (roughly)
- Pain level at bedtime and on waking (simple 0–10 is fine)
- Med timing (only if you’re comfortable sharing)
If you want a pain-tracking template that clinicians and insurers tend to take seriously, borrow the structure of an ERISA long-term disability pain diary format and adapt it for sleep (same idea: concrete patterns, not vague suffering).
Quote-prep list: what to gather before comparing providers
- Your insurance card (or plan details)
- Preferred format (tele vs in-person)
- Scheduling constraints (work, caregiving, flare patterns)
- Any prior sleep studies or diagnoses (if applicable)
Neutral action: Put these four items in a note on your phone before you start calling.

FAQ
Can CBT-I work if pain wakes me up multiple times a night?
Yes—because CBT-I targets the insomnia mechanics (long awake stretches in bed, sleep anxiety, irregular timing) even when pain is a trigger. The win is usually fewer and shorter awakenings, less clock-watching, and a more stable sleep pattern. Pain may still wake you sometimes; CBT-I helps you stop turning awakenings into a full night of wakefulness.
Will sleep restriction make my pain worse?
It can feel tougher briefly, especially early on. That’s why pain-adapted CBT-I often uses gentler sleep compression and flare-day decision rules. The aim is not “less sleep forever.” It’s consolidated sleep now, then gradual expansion when your pattern stabilizes. If your pain condition is complex, do this with a trained clinician.
How long does CBT-I take to work?
Many programs run 4–8 sessions over several weeks. Some people notice changes within 2–3 weeks; others need longer, especially with irregular schedules or multiple comorbidities. What matters most is weekly adjustment based on your diary.
How do I know a provider is actually delivering CBT-I?
Ask whether they use a sleep diary, set a tailored sleep window, and adjust it over time. If the plan is generic, never changes, or avoids tracking entirely, you may be getting sleep coaching or sleep hygiene—not CBT-I.
Is telehealth CBT-I legitimate?
It can be, as long as it includes the core pieces: structured tracking, a tailored sleep window, stimulus control rules, and follow-up adjustments. Telehealth can also reduce flare triggers from travel and make scheduling more realistic.
Can I do CBT-I while taking opioids, benzodiazepines, gabapentin, or sleep meds?
Often yes, but you should coordinate with your prescriber. Don’t change medications on your own because sleep and sedation can interact with breathing, mood, and safety. A good CBT-I clinician will work alongside your medical team.
What if my insomnia is tied to anxiety, PTSD, or depression?
That’s common. CBT-I can still help insomnia directly, and many clinicians integrate or coordinate care for mood/anxiety conditions. If symptoms are severe (suicidal thoughts, mania-like symptoms), seek prompt professional help and prioritize safety.
When should I be evaluated for sleep apnea before starting CBT-I?
If you snore loudly, gasp/choke at night, have witnessed breathing pauses, or have severe daytime sleepiness, ask about evaluation. CBT-I can help insomnia, but it won’t treat breathing-related sleep disruption.
Wrap-up: close the loop (and keep it doable)
Remember the open loop from the beginning—the number clinicians watch to decide when to expand your sleep window? It’s usually sleep efficiency: how much of your time in bed you’re actually asleep. That’s why diaries matter. Not because we love paperwork. Because data prevents panic.
If you’re time-poor, here’s the simplest version of the plan:
- Track 7 nights (rough estimates are fine)
- Book one legit CBT-I intake (telehealth counts)
- Verify the process: diary + tailored sleep window + weekly adjustments
One last gentle truth: chronic pain may not let you have “perfect” nights. CBT-I can still give you less fragile nights—nights that don’t collapse after one flare, one stressful email, one slightly-too-late dinner. That stability is not glamorous, but it’s life-changing.
15-minute CTA: Copy the booking script, email two providers, and start your 7-night diary tonight. You’re not trying to win sleep. You’re building it.
Last reviewed: 2025-12.
