
The same injection can cost 2–4× more for one boring reason: you didn’t upgrade the medicine—you upgraded the building.
When a pain clinic visit is billed as hospital outpatient (often a hospital outpatient department / HOPD), a second charge can appear: the facility fee. That’s the moment people feel “surprised,” even when nothing went clinically wrong.
Facility fee (definition): A facility fee is a separate charge for the site’s overhead—staffing, equipment, compliance, and monitoring—billed in addition to the clinician’s professional fee. It’s most common in hospital outpatient settings, and it changes the “allowed amount” and your deductible/coinsurance math.
Keep guessing and you risk locking in the priciest place of service by accident—often signaled by one paperwork word: “department.”
This post helps you spot HOPD billing early, get a two-part, CPT-based estimate (professional + facility), and avoid the “two networks” trap (in-network doctor, out-of-network facility)—without spending your week on hold.
“I’ve been the person who thought I booked an office… until the portal posted a second bill.”
Here’s the shortcut.
The language to listen for.
The script that gets numbers, not vibes.
And the calm steps if the bill already landed.
Table of Contents
Facility fee first: why the “same injection” bills differently
Here’s the uncomfortable truth: your injection didn’t suddenly become “premium.” The building did. In most surprise-bill stories I hear (and yes, I’ve been the person refreshing the portal like it owes me money), the cost jump is driven by a facility fee or a higher “technical” charge that comes with a hospital outpatient setting—often layered on top of the baseline chronic back pain costs that already wear people down.
- Professional fee = the clinician’s work (the “hands and brain” part).
- Facility/technical fee = the site’s resources (staff, equipment, compliance, room, monitoring).
- Same needle can still produce a totally different bill depending on the site-of-care.
Curiosity gap (answered soon): the single word that often predicts the facility fee is hiding in plain sight—usually in scheduling language or your portal’s “location type.” We’ll name it in Spot it early, and show you how to confirm it in writing.
One more grounding note: the “2–4×” swing isn’t a promise or a universal ratio. It’s a pattern people report when the second bill appears. The mechanism is what matters: two separate charges plus a different “allowed amount” structure depending on the setting.
Quick mental model: If your bill feels like it multiplied, ask yourself: “Did I accidentally pay for the building?”
Show me the nerdy details
In billing terms, the same procedure code can be priced differently based on the site-of-service. A hospital outpatient department often bills a facility component (and may follow a different contracted schedule) while an office-based setting typically bills primarily the professional component (plus supplies). Your insurer’s “allowed amount” and your cost-sharing (deductible/coinsurance) can change as a result.

Who this is for / not for (and when cost-shopping is the wrong move)
This article is for time-poor readers who want a clean answer: “How do I avoid a surprise facility fee without risking my safety?” You’re not trying to become a billing expert. You’re trying to not get ambushed—especially when you’re already juggling diagnosis questions like sciatica vs herniated disc and the practical reality that different injections (and approaches) can come with different billing patterns.
Best fit (you’ll get high value here)
- You’re scheduled for an injection and haven’t seen an itemized estimate.
- You’re choosing between an office-based pain clinic, a hospital outpatient department, or an ASC.
- You have a deductible or coinsurance and want a realistic out-of-pocket picture.
Not the moment to bargain (safety > savings)
If you have medical complexity that requires higher-level monitoring, sedation, or immediate backup resources, the costier setting may be appropriate. This can include severe cardiopulmonary issues, complicated medication situations (like certain blood thinners), or conditions where your clinician recommends a higher-acuity environment.
Let’s be honest… sometimes the safest building is the expensive one. The goal isn’t “cheapest.” It’s “cheapest that’s still appropriate.”
- Ask: “Is the hospital outpatient setting medically necessary for me?”
- Ask: “Could the same injection be done safely in-office or at an ASC?”
- Ask: “Can we document the reason for this site in the chart?”
Apply in 60 seconds: Write one question on a sticky note and read it verbatim on the next call.
- Yes/No: Do I require sedation or advanced monitoring per my clinician?
- Yes/No: Do I have major medical conditions that raise procedural risk?
- Yes/No: Can the clinician confirm the injection can be done safely in an office or ASC?
Neutral next action: If you answered “No” to the first two, request a two-site price comparison.
Office vs HOPD vs ASC: the site-of-care decoder (US billing version)
Three settings. One big difference: how the site gets paid. If you remember nothing else, remember this: the setting is the pricing engine. (And yes, even if you’re comparing the same doctor doing the same thing—like a TFESI vs interlaminar ESI for sciatica—the bill can still follow the building.)
Office (often POS 11): usually fewer “building charges”
Office-based care is commonly billed with the professional component as the main event. That doesn’t mean “cheap,” but it often means fewer separate facility charges.
Hospital outpatient department (HOPD): facility fees are common
Hospital outpatient settings often generate a facility component. It can be clinically appropriate—and financially loud. The trick is catching it before you show up.
ASC: can be a middle path (but watch networks)
Ambulatory surgery centers can be a cost middle-ground for certain procedures, but they can also be out-of-network even when the doctor isn’t. The site and the clinician can be separate contracting entities.
Open loop (answered now): “POS can change after you arrive” happens when your appointment is scheduled under one location type and later billed under another due to how the facility is classified, how the service is documented, or how the claim is submitted. That’s why you want the place-of-service confirmed in writing.
- Choose Office when the procedure is routine, no sedation, and your goal is the lowest cost-sharing.
- Choose ASC when office isn’t available or isn’t equipped, but you still want to avoid hospital outpatient pricing.
- Choose HOPD when your clinician gives a clear safety reason (monitoring, complexity, backup resources).
Neutral next action: Ask for the same CPT-based estimate at two sites before you finalize the date.
Spot it early: how to tell you’re being billed as hospital outpatient
This is the section that saves people money because it prevents the “I didn’t know” moment. A facility fee is rarely advertised with a trumpet. It’s hinted at in small, bureaucratic words.
The “hospital-owned clinic” tell (the waiting room can lie)
If the clinic is owned by a hospital system, the visit/procedure may be billed as hospital outpatient even if it looks like a normal office. The furniture can be identical. The billing category isn’t.
Portal wording that often predicts a facility charge
- “Outpatient department”
- “Hospital outpatient”
- “Provider-based clinic”
- “Department” instead of “office” in the location type
The one word on your paperwork that predicts the fee: “Department” (especially “outpatient department”). If you see that, treat it like a weather warning: it doesn’t guarantee a storm, but you grab an umbrella.
The fastest question to ask scheduling (and the answer you want)
Ask: “Will this be billed as a hospital outpatient department with a facility fee, or as an office visit/procedure without a facility fee?”
Good answers sound like: “It’s office-based (no facility fee)” or “Yes, it’s HOPD (there may be a facility fee).”
Soft answers sound like: “It depends” without offering to check. If they won’t check, you can.
Micro-humor truth: If the answer is delivered like a bedtime story—warm, vague, soothing—ask again, slower.
Ask for numbers, not vibes: the two-part estimate script that works
If you’ve ever asked for a price and received poetry (“It varies… depends on insurance…”), you already know: you need a more specific ask. The goal is a written estimate that separates the charges you’ll actually see—especially if you’re comparing a billed claim against the self-pay TFESI cost some clinics can quote upfront.
The exact ask (copy/paste)
Message: “Hi—before scheduling, I’m requesting a written, itemized estimate for my injection that includes (1) the professional fee (physician) and (2) the facility/technical fee (site). Please include the place of service (office vs hospital outpatient vs ASC), the procedure code (CPT), and whether both the physician and facility are in-network for my plan.”
Neutral next action: Send this through the portal so it’s timestamped.
What to collect (so your insurer can answer)
- Procedure code(s) (CPT) and whether imaging guidance is included
- Diagnosis code (the “why”)
- Levels/laterality if relevant (e.g., left/right, single vs multiple levels)
- Place of service (office vs HOPD vs ASC)
- Physician identifier and facility identifier (billing entity)
Pattern interrupt: Here’s the awkward question that saves the most money: “What is the facility’s billing name and tax ID?” You’re not being difficult. You’re being accurate. Networks are built on entities, not vibes.
- Get the estimate in writing (portal message > phone memory).
- Confirm the site type (office vs HOPD vs ASC) explicitly.
- Ask for the billing entity name for both clinician and facility.
Apply in 60 seconds: Paste the script into a note so you can send it fast.

The “two networks” trap: in-network doctor, out-of-network facility
This is where people get burned. You call your insurer, you confirm the doctor is in-network, you feel responsible and adult… and then the facility shows up like a second villain in Act Two.
How to check network status for the facility entity
- Ask the facility: “What is your billing entity name and are you in-network for my plan name?”
- Ask your insurer: “Is this facility entity in-network at this address for this procedure type?”
- Ask both: “Is this billed as hospital outpatient (HOPD)?”
What to ask your insurer so you get a real answer
Use concrete identifiers. Insurers can’t confirm what you don’t name.
- “Is the facility in-network?” (not just the provider)
- “What is my coinsurance for outpatient hospital vs office?”
- “Does this fall under my deductible?”
If the clinic says “we’re in-network”—the follow-up that verifies it
Ask: “Are you in-network as the facility billing entity for my plan, and will this be billed as HOPD?”
That second clause matters. “In-network” can still be expensive if your plan uses higher coinsurance for outpatient hospital services.
- Confirm both entities, not just the clinician.
- Ask how the claim will be categorized (office vs outpatient hospital).
- Write down the name of the plan tier you’re referencing.
Apply in 60 seconds: Ask for the facility’s billing name and save it in your phone notes.
Insurance math that predicts your out-of-pocket (without a finance degree)
Insurance feels like it was designed by someone who hates joy. But for your out-of-pocket, you only need a few moving parts:
- Deductible remaining (how much you still pay before cost-sharing improves)
- Coinsurance (your percentage after deductible)
- Out-of-pocket max (the ceiling, for covered in-network care)
- Allowed amount (the negotiated number your plan uses)
Charged vs allowed: which number matters
The “charge” can be eye-watering. The “allowed amount” is what typically drives your cost-sharing in-network. When you compare office vs HOPD, you’re often comparing different allowed amounts and sometimes different coinsurance categories—and this is the same logic that shows up when people try to forecast other line items, like a lumbar MRI cost on an HDHP.
Deductible timing: why January appointments feel “more expensive”
If your deductible resets at the start of the year, early-year procedures can feel like a punch. Late-year procedures can feel “cheaper” because you’ve already paid into your deductible and out-of-pocket max. This isn’t medical advice—just calendar reality.
Copays vs coinsurance: why procedures rarely behave like simple office visits
Many plans treat procedures (especially in hospital outpatient settings) as coinsurance-based. Translation: your out-of-pocket can scale with the allowed amount.
- Input 1: Deductible remaining (in dollars)
- Input 2: Allowed amount estimate (in dollars)
- Input 3: Coinsurance % (example: 20%)
Quick output idea: You’ll typically pay up to your deductible remaining first; after that, you pay your coinsurance on the remaining allowed amount—until your out-of-pocket max is reached.
Neutral next action: Ask your insurer for the allowed amount estimate tied to the place of service.
When hospital outpatient is worth it (clinical reasons, not billing reasons)
I’m pro-saving-money. I’m also pro-not-being-brave-in-the-wrong-direction. Sometimes hospital outpatient is the right call—especially when your situation is more complex than a straightforward sciatica nerve pain flare and your clinician is worried about monitoring or rescue resources.
When higher-acuity resources may matter
- Need for closer monitoring
- Higher medical complexity that increases procedural risk
- Potential need for rapid escalation of care
What hospitals have that offices may not
Hospitals can offer broader staffing, equipment, and immediate backup resources. Offices can be excellent—especially when they’re specialized and experienced—but they’re not identical environments.
How to ask for a one-sentence justification
Ask: “What is the safety or clinical reason you recommend hospital outpatient for me specifically?”
If there’s a clear reason, your next job is not arguing—it’s budgeting. If there isn’t, your next job is options.
Common mistakes that accidentally lock you into the priciest site
Surprise bills usually start with a small decision made while you were busy being a human with a calendar.
Mistake #1: Scheduling the earliest slot without confirming place of service
I’ve done this. You’re in pain, you’re tired, you grab the soonest appointment like it’s a life raft. But “soonest” can quietly mean “hospital outpatient department.”
Mistake #2: Assuming “same doctor” means “same bill”
Doctors often practice at multiple sites. Your bill follows the site, not the name on the door.
Mistake #3: Skipping the estimate because “insurance will cover it”
Insurance often covers it—after you meet deductible and pay coinsurance. “Covered” is not a number.
Let’s be honest… most surprise bills start with a rushed yes. If you slow down by 90 seconds, you can save hours later.
Already got the bill? A calm, step-by-step repair plan
If you’re reading this with a bill open in another tab, I get it. The nervous system does a little sprint. The good news is you still have moves.
Step 1: Ask for an itemized statement + claim details
- Request an itemized bill.
- Ask which parts are professional vs facility.
- Ask how it was categorized (office vs outpatient hospital).
Step 2: Compare with a self-pay quote (when appropriate)
Sometimes self-pay pricing can be lower than the patient portion after a complicated claim path—sometimes not. You won’t know until you ask. Keep the tone neutral: you’re comparing options, not accusing anyone of villainy.
Step 3: Payment plans, financial assistance, and timing leverage
If the balance is real and you can’t magic it away, ask about payment plans or financial assistance policies. Also ask whether the facility offers any prompt-pay discount (some do, some don’t). The key is to get terms in writing.
- Itemize first (what am I paying for?).
- Verify category (office vs outpatient hospital).
- Then negotiate terms (plan, assistance, timing).
Apply in 60 seconds: Write down the date of service and the facility billing name before you call.
Safety / Disclaimer + When to seek help
Important: This article is educational and general. It is not medical advice, legal advice, or insurance advice. Your clinician and your insurer are the best sources for decisions specific to you.
When to seek urgent care
- New or rapidly worsening weakness
- New bowel or bladder control problems
- Fever with severe pain or signs of infection
- Severe, escalating symptoms that feel different from your baseline
If symptoms rapidly worsen
Pause the cost-optimization mission and seek medical evaluation. If you’re worried, it’s okay to choose safety first—and do the billing cleanup after. (If you’re unsure what counts as “don’t wait,” this guide on low back pain emergency red flags can help you sanity-check the moment.)
Short Story: The day I learned “department” is a money word (120–180 words) …
I once walked into a clinic that felt like every other clinic: beige walls, sleepy magazines, the quiet hum of someone’s bad daytime TV. The nurse was kind. The doctor was sharp. I left thinking, “Okay. That wasn’t so bad.” Two weeks later, my portal posted a second bill I didn’t recognize—one that looked like it belonged to the building itself.
I reread the appointment details and noticed a phrase I’d skimmed past: “outpatient department.” Not “office.” Not “suite.” A department. It was such a small word, so normal, so administrative—yet it carried a price tag. I didn’t feel tricked. I felt untrained. Now, when I schedule anything involving an injection, I treat location labels like ingredients on a food package. If I can’t pronounce it, I ask what it means.
FAQ
Why does my injection cost more at a hospital outpatient pain clinic?
Often because a hospital outpatient department can bill a facility/technical component in addition to the clinician’s professional fee, and the allowed amounts and coinsurance categories may differ by site-of-care.
What is a facility fee and why am I being charged it?
A facility fee is a charge for the site’s resources—staffing, equipment, compliance, and operational overhead. It’s separate from the clinician’s professional fee and is more common in hospital outpatient settings.
How do I know if a clinic is billed as a hospital outpatient department (HOPD)?
Look for portal/location language such as “outpatient department,” “hospital outpatient,” or “provider-based clinic,” and ask scheduling directly whether the visit/procedure will include a facility fee.
Can the doctor be in-network but the facility out-of-network?
Yes. The physician and the facility can be separate billing entities with different network contracts. Always verify both.
Is an ASC cheaper than a hospital outpatient department for injections?
It can be, depending on your plan’s allowed amounts and coinsurance rules. The key is to request estimates tied to the same procedure code and confirm network status for the ASC entity.
Does the No Surprises Act protect me from facility fees?
The No Surprises Act focuses on certain surprise out-of-network bills and balance billing protections in specific situations. It may help in some out-of-network scenarios, but it does not automatically remove all facility fees. When in doubt, ask your insurer how your scenario is covered.
What should a written estimate include?
Ask for a two-part breakdown (professional + facility/technical), the procedure code(s), place of service (office vs HOPD vs ASC), and confirmation of network status for both the clinician and facility.
Next step: one concrete action you can do today
If you do one thing in the next 15 minutes, do this: send the two-part estimate request through the portal and ask for place-of-service confirmation in writing. If you’re already scheduled, do it anyway—“before arrival” still counts. And if your plan is steering you toward conservative care first, having a clean roadmap for physical therapy for sciatica can keep the next steps from feeling like guesswork.
- Your plan name (exact tier)
- Deductible remaining + coinsurance
- Procedure code(s) (CPT) from the clinic
- Place of service (office vs HOPD vs ASC)
- Facility billing name (and tax ID if available)
Neutral next action: Put these into one note titled “Injection Cost Snapshot.”
Conclusion
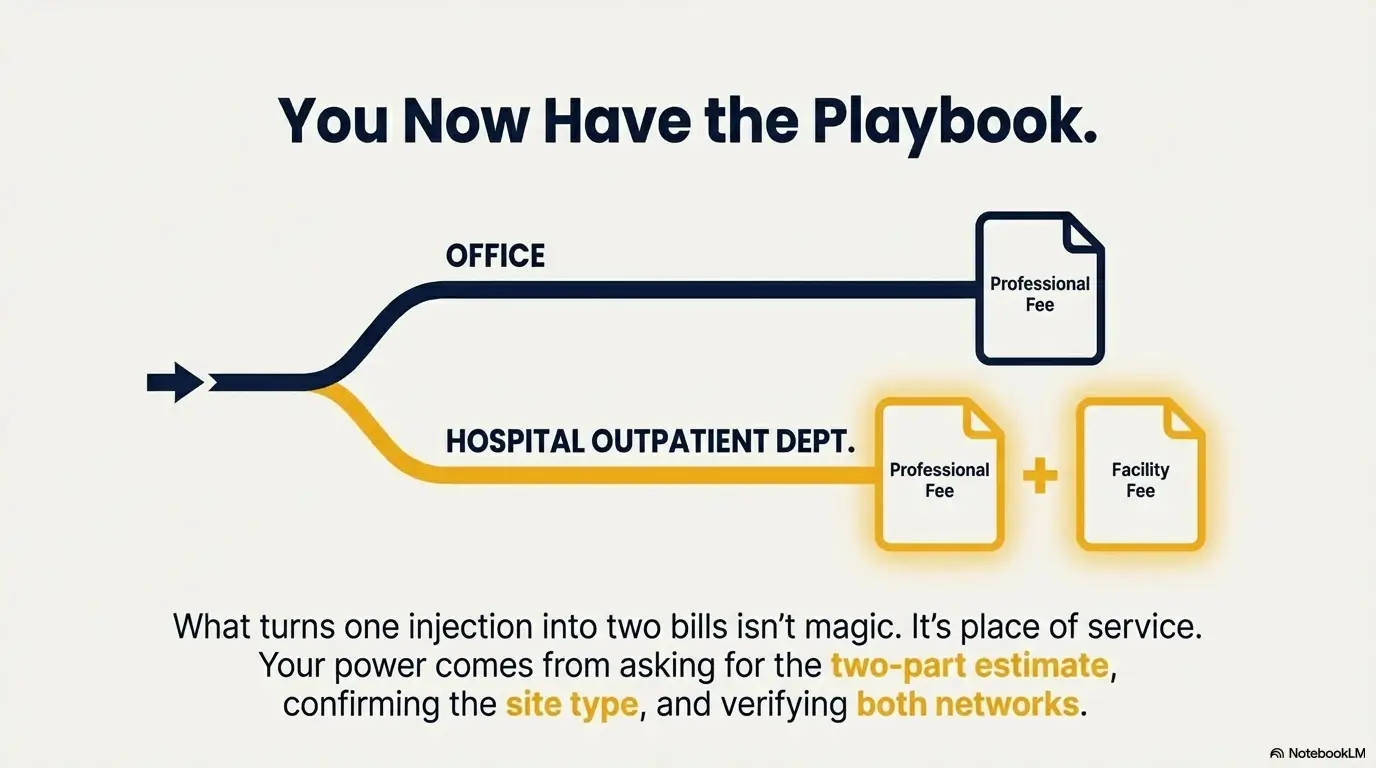
We opened with a small mystery: What turns one injection into two bills? Now you know the answer isn’t magic or better medicine—it’s often place of service, and the tiny paperwork word “department” that signals hospital outpatient billing and potential facility fees.
If you want the cleanest win: don’t ask “How much is it?” Ask for the two-part estimate, confirm the site type in writing, and verify both networks (doctor + facility). That’s the whole playbook.
Note: Bar lengths are illustrative to show “split,” not a universal pricing ratio.
Your 15-minute next step: send the portal message requesting the itemized two-part estimate, then screenshot the reply for your records. Your future self (and your wallet) will feel the difference.
Last reviewed: 2025-12.
