
Beyond the Court: Managing Pickleball Hip Pain
Pickleball hip pain rarely begins with a cinematic injury. More often, it starts with one hurried pivot, one low reach, one “I’m fine” extra game, and then the next morning your hip feels like it has filed a formal complaint.
Orthopedic pain management for players has less to do with heroics and more to do with making smarter load decisions before a manageable flare turns into a stubborn cycle. The real frustration isn’t just the pain. It’s the uncertainty of whether you’re dealing with a strain, arthritis, a labral issue, or referred pain that is actually coming from the spine rather than the hip.
“Keep guessing too long, and you do not just lose court time. You risk turning a modifiable problem into a recurring one.”
This guide helps you read the pattern clearly, calm symptoms without the rebound trap, and return to play with more judgment and less trial-and-error. It is built around a function-first method: track location, trigger, timing, and next-day response.
Because a quieter hip is nice. A reliable hip is better.
Table of Contents
Safety / Disclaimer
This article is educational, not a diagnosis and not a substitute for medical care. Hip pain in pickleball players can come from overuse, tendon irritation, joint degeneration, bursitis, labral injury, referred back pain, or something less common that deserves prompt evaluation. MedlinePlus notes that hip pain can stem from strains, bursitis, fractures, arthritis, and labral tears, which is exactly why a one-size-fits-all “just stretch it” plan can go sideways fast. The safest posture is conservative: reduce aggravation, protect mobility, watch the pattern, and get medical help for severe, persistent, or worsening symptoms.
- Use calm, function-first decisions instead of pain bravado
- Do not treat catching, limping, or severe night pain like routine soreness
- Track the pattern before you try to fix the pattern
Apply in 60 seconds: Decide whether your pain is mild and modifiable, or whether it already has red-flag features that deserve evaluation.
Who this is for / not for
Who this is for
- Recreational pickleball players with mild to moderate hip pain during or after play
- Adults trying to stay active while reducing flare-ups
- Players wondering whether to rest, modify, or get evaluated
Who this is not for
- Players with sudden inability to bear weight
- Anyone with major trauma, suspected fracture, fever, numbness, or rapidly worsening pain
- Readers looking for a diagnosis without an exam
I have seen this pattern in active adults again and again: they are not asking for a miracle, just a sane next step. They do not want to be told to stop moving forever, and they definitely do not want a chirpy internet stranger promising that three band exercises and a foam roller will solve all earthly suffering by Thursday. Fair enough. This piece is for the player who wants to stay in the game without treating their hip like a rental car.
Eligibility checklist
- Yes: You can walk, even if you are annoyed about it
- Yes: Pain is mild to moderate and linked to activity
- Yes: You want practical, conservative guidance
- No: You have severe pain, fever, deformity, numbness, or major trauma
Neutral next step: If you checked any “No” item, skip self-management and arrange prompt medical care.
First question: what kind of hip pain is this, exactly?
Front, side, or deep joint pain changes the story
Location matters, even if it is not perfect. Front-of-hip or groin pain often raises a different set of questions than pain on the outer side of the hip. Deep joint pain can feel vague, almost rude in how unspecific it is, while outer-hip pain may point more toward soft tissue irritation around the side of the hip. Then there is the classic plot twist: the “hip pain” that is really coming from the low back or buttock and borrowing the hip’s identity badge.
Pain during play vs pain the next morning points to different problems
Pain that ramps up during lateral pushes, lunges, or pivots suggests one kind of load sensitivity. Pain that waits until the next morning can suggest another. Neither pattern is automatically serious, but timing is a clue. A player who feels fine on court and then wakes up stiff enough to descend stairs like a Victorian widow is telling you something important about recovery tolerance.
Stiffness, catching, burning, or weakness are not interchangeable
These words are not decoration. They are useful data. Stiffness after sitting may lean one direction. Catching or locking leans another. Burning or shooting symptoms may pull attention toward nerves or referred pain. Weakness during push-off changes the management conversation. When people say “it just hurts,” I understand the impulse. Pain is irritating and poetry often leaves the room. Still, the more specific your description, the fewer wrong turns you take.
Let’s be honest… most players say “hip pain” when they mean three different body regions
In ordinary conversation, the groin, outer hip, buttock, and low back all get dumped into one basket labeled “hip.” I once heard a player point to the back pocket area and say, with complete confidence, “Yep, definitely my hip flexor.” The human body is many things, but it is not always a careful cartographer. Spend 7 days getting more precise than that. It can change the entire quality of your next decision.
- Front or groin pain is not the same conversation as outer-hip soreness
- Catching, locking, or giving way deserves more caution than ordinary post-play stiffness
- Next-day flare patterns often reveal poor load tolerance
Apply in 60 seconds: Write down one sentence that names the exact spot, the exact trigger, and the exact time the pain appears.
Before you treat it: what pickleball is doing to your hip
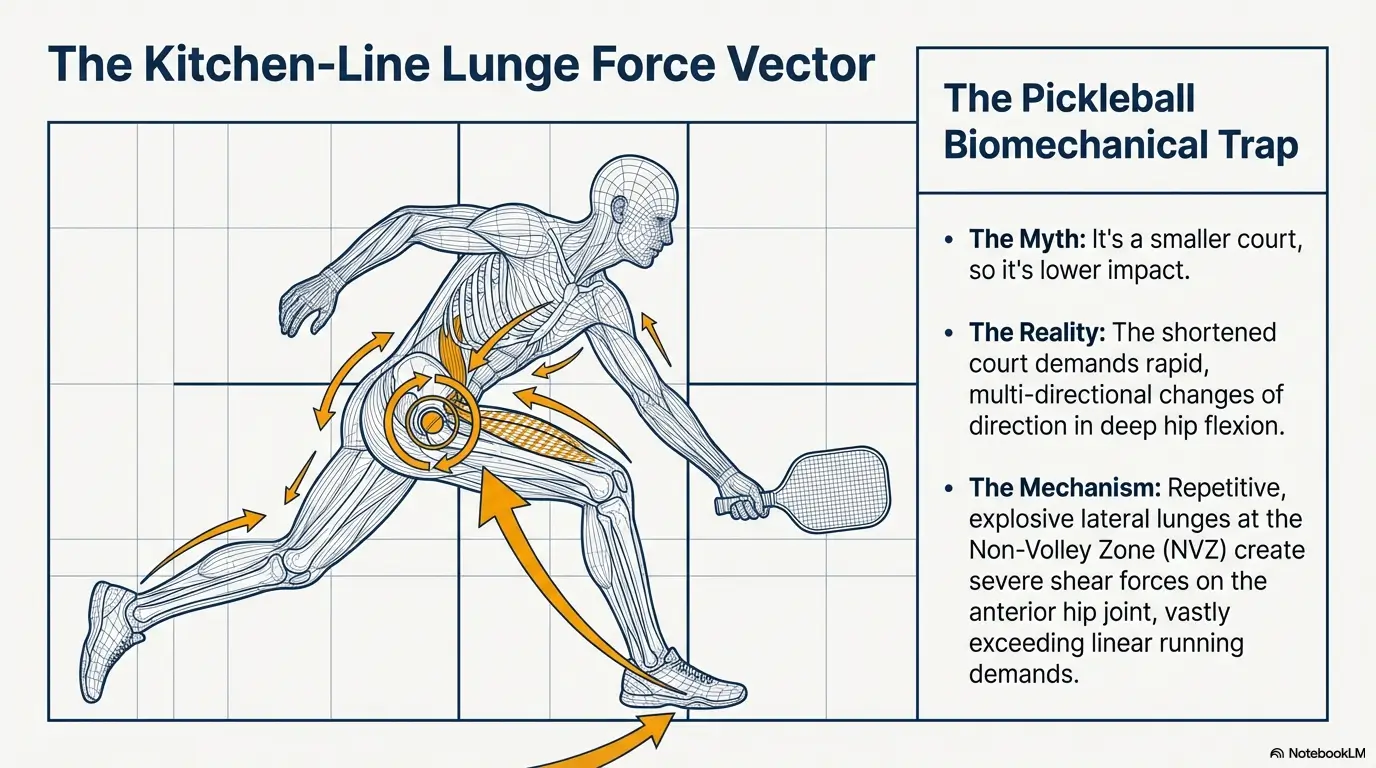
Quick starts, lunges, pivots, and low balls load the hip in sneaky ways
Pickleball looks friendly from the fence. Then you step onto the court and discover it is a festival of short accelerations, decelerations, rotation, low reaching, and awkward saves made while your brain is busy yelling “mine.” The hip does not merely move. It brakes, rotates, stabilizes, and absorbs force while the trunk and leg negotiate sudden changes of direction. That is a demanding job description for a sport people often underestimate.
Why pickleball pain is often a volume problem, not just an age problem
Blaming age is convenient and sometimes lazy. Volume matters. Four sessions in 6 days, a jump from doubles to long singles rallies, back-to-back tournament play, or returning after a quiet winter with the emotional confidence of 2019 can all change the load story. Many flares are not caused by one dramatic incident. They are caused by too much, too soon, too often. The hip usually sends warning emails before it sends a legal notice.
Court frequency, footwear, and surface all shape flare-up risk
Harder surfaces increase the cumulative demand on joints and soft tissues. Worn shoes change the feel of braking and push-off. Two extra days of play per week may matter more than the fancy massage gun you bought after midnight because the algorithm whispered sweet promises. Even session length matters. Sixty minutes with good pacing is not the same as 2.5 hours fueled by competitive delusion and a banana.
Singles vs doubles: same sport, very different load profile
Doubles usually lowers the amount of extreme court coverage and repeated wide chasing. Singles can expose poor deceleration tolerance fast. That does not make doubles “safe” and singles “bad.” It means they are different dose levels. Treat them that way.
Practical rule: Before you label your hip fragile, ask whether your weekly load changed in the last 2 to 3 weeks. Often the body is protesting arithmetic, not betrayal.
AAOS explains that hip osteoarthritis can cause pain and stiffness that interfere with ordinary tasks such as rising from a chair or taking a short walk. That matters here because pickleball asks the hip to do much more than ordinary walking. If day-to-day tasks are already getting stiffer, your return-to-play plan needs more humility than your group chat will likely recommend, especially for readers already navigating orthopedic pain management in older adults.
Red flags first: when hip pain is not a “play through it” situation
Pain that wakes you up, locks the joint, or makes weight-bearing hard
These are not the moments for stoicism. Severe pain with inability to bear weight, pain after a fall, joint locking, or rapidly escalating symptoms move you out of “manage and monitor” territory. MedlinePlus notes that hip fractures can cause sudden, acute pain and are especially serious in people with weaker bones. Even if you are not in that group, the principle still holds: sudden functional collapse deserves evaluation, not a brave face.
Limping after matches is a clue, not a badge of honor
A limp is the body changing movement strategy to protect itself. It is not a charming personality quirk. If you are limping after every match, the hip is not tolerating the current dose. Playing through a limp teaches bad mechanics, irritates tissue further, and muddies the picture of what is actually wrong.
Groin pain plus catching may need faster evaluation
Groin pain with catching, locking, or the feeling that the hip is not gliding smoothly is worth taking seriously. That combination does not diagnose a labral problem by itself, but it moves the conversation away from casual self-experimentation. A little caution here saves a lot of circular frustration later.
Back pain, numbness, or shooting symptoms may not be “just the hip”
If you have back pain paired with numbness, tingling, or shooting pain down the leg, the source may involve the spine or nerves rather than the hip alone. This is where home treatment often becomes a carnival of wrong assumptions. One stretch for the “hip” can aggravate a back-driven problem beautifully. The body, again, is a dramatic ensemble cast. If that overlap sounds familiar, it helps to read more closely about how hip pain and spine pain can imitate each other.
Decision card: play, modify, or stop?
| Pattern | Safer next move |
|---|---|
| Mild soreness, no limp, settles within 24 hours | Modify load and monitor |
| Pain during play with growing stiffness next day | Reduce duration and intensity, log pattern |
| Limp, catching, weight-bearing trouble, severe night pain, trauma, numbness | Stop self-management and seek medical evaluation |
Neutral next step: Use function, not pride, as the deciding variable.
Pain relief without the rebound problem
What “calm the pain” should mean for active adults
For a pickleball player, pain relief is not just about lowering a number on a scale. It is about improving the ability to walk, sit, sleep, climb stairs, and move with less guarding. That is a more useful target than “I want to feel nothing and play two hours tonight.” Numbness is not readiness. Temporary relief is not the same as restored load tolerance. This distinction is plain, unfancy, and extremely important.
Heat, ice, pacing, and relative rest: what each actually helps
Heat can feel good for stiffness. Ice may help some people after an irritating session. Relative rest means reducing aggravating load while keeping reasonable movement in the day. It does not mean becoming a decorative lamp for 5 days and then expecting greatness on Saturday. Gentle walking, position changes, and controlled movement often protect function better than total shutdown.
Medication decisions should protect function, not just lower pain scores
Medication belongs in a larger strategy, not on a throne. Some players chase enough relief to ignore symptoms and keep the same workload. That is how a manageable flare becomes a recurring script. The safer lens is this: does the pain strategy help you move better without tricking you into overdoing it? If not, it may be buying comfort at a lousy exchange rate.
Why “numb enough to play” is a dangerous standard
I understand the temptation. There is a round-robin tonight. Your doubles partner is already texting. The body is being uncooperative and your brain starts shopping for loopholes. But if your management plan ends with “good, now I can blast through warning signs,” it is not pain management. It is symptom camouflage. And camouflage works wonderfully until it does not.
Short Story: A player I once spoke with described a familiar cycle. He would feel tight after Thursday open play, spend Friday sitting more than usual, apply a mix of heat, determination, and wishful thinking, then show up Saturday feeling “surprisingly okay.” The first 20 minutes were always excellent. Then came the third wide forehand, the deep lunge, and the old pinch returned like a creditor who knows your schedule.
He kept treating the first pain-free minutes as proof that the problem had resolved. What finally changed things was embarrassingly simple: he stopped testing the hip with full-dose play every time it went quiet. He cut one session, switched to shorter doubles blocks, and tracked next-day stiffness for 2 weeks. That tiny shift did not feel cinematic, but it turned chaos into a pattern, and a pattern into a plan.
Show me the nerdy details
Pain relief methods and readiness to load tissue are separate questions. A modality can reduce symptoms temporarily without improving joint mechanics, tendon load tolerance, or change-of-direction capacity. For active adults, the clinically useful metric is usually function over 24 to 48 hours, not just symptom reduction in the next 20 minutes.
Don’t shut everything down: how to modify play without getting deconditioned
Reduce intensity before you reduce all movement
Many players move too late and then too hard. They either ignore symptoms until the hip is irritated enough to complain all day, or they stop everything and grow stiffer, weaker, and more hesitant. A better middle path is to reduce the aggravating dose first. Trim the session. Skip the extra game. Lower chase distance. Choose rallies over scrambles. Think dimmer switch, not breaker panel.
Smarter swaps: shorter sessions, doubles, fewer wide chases
Smart modification is gloriously unromantic. Thirty to 45 minutes may be better tolerated than 90. Doubles may be better than singles for a while. A warm-up rally may be useful while repeated max-effort reaches are not. This can feel psychologically annoying because it lacks cinematic heroism. It also tends to work better.
Warm-up changes that make more sense than heroic stretching
Some players attack pain with longer and more dramatic stretching, as if the hip will reward sincerity. Sometimes the issue is not lack of stretch. It is poor tolerance for force, rotation, or deceleration. A warm-up that includes easy walking, controlled hip movement, gentle trunk rotation, and a gradual ramp into play often makes more sense than wrenching on an irritated area.
Here’s what no one tells you… full rest can sometimes make the first game back feel worse
NIA guidance on osteoarthritis encourages safe, well-rounded activity including low-impact exercise and balance work because movement can help pain, stiffness, flexibility, strength, and endurance. Different problem, same useful principle: total inactivity can make return feel rusty and sharp. The goal is not to do more. It is to stay adapted enough that the first return does not feel like asking your hip to improvise on stage with no rehearsal.
- Shorter sessions often beat total shutdown
- Doubles can be a useful bridge back to play
- Warm up for control and rhythm, not for circus flexibility
Apply in 60 seconds: Pick one change for your next session: reduce duration, switch to doubles, or stop before symptoms climb.
Common mistakes pickleball players make with hip pain
Playing through a limp because the pain is “only a 4”
Pain scales are useful, but they are not the whole kingdom. A “4 out of 10” with a limp is often a bigger deal than a “6 out of 10” that settles and does not alter gait. Function matters. Walking pattern matters. Recovery pattern matters. Numbers without context are tidy and often misleading.
Stretching irritated tissue harder when the problem is load tolerance
This is common because stretching feels proactive. It gives the hands something to do and the mind something to believe. But when the issue is irritated tendon load, joint sensitivity, or poor deceleration tolerance, harder stretching may just be a more organized way to stay annoyed.
Copying rehab drills from social media without matching the diagnosis
The internet is full of excellent exercises and terrible timing. The same drill can be helpful for one person and foolish for another. A labral-style groin pain pattern, lateral hip tendon irritation, hip OA stiffness, and back-referred pain do not automatically want the same menu. Social media often sells choreography as certainty. Your body deserves something sturdier.
Returning after pain drops, even though capacity has not returned
Symptom reduction is not the finish line. Capacity means what the hip can tolerate repeatedly without the next-day penalty box. When players skip this distinction, they keep restarting the same flare. It is like repainting a wall without fixing the leak. Visually hopeful. Structurally unserious.
Quote-prep list: what to gather before comparing care options
- Exact pain location: groin, outer hip, buttock, low back, front crease
- Trigger pattern: start, stop, pivot, stairs, getting out of a chair, next morning
- Functional change: limp, shortened stride, trouble sleeping, trouble tying shoes
- Load data: sessions per week, minutes played, singles or doubles, court surface
- What helped or failed: heat, ice, rest, walking, medication, exercises
Neutral next step: Bring these notes to a clinician or use them to guide a more precise self-management plan.
The diagnosis trap: different causes need different decisions
Hip arthritis pain does not behave like gluteal tendinopathy
Hip osteoarthritis often brings stiffness, especially after sitting or first thing in the morning, and AAOS notes that it can make daily tasks like rising from a chair or walking more difficult. Gluteal tendon irritation around the outer hip often behaves differently and may become more obvious with side-lying pressure, single-leg loading, or repeated lateral work. Same body region. Different management tone. For readers who are further along that wear-and-tear spectrum, this can overlap with broader questions about pain management while waiting on a joint-related orthopedic plan.
Labral irritation and groin pain are not the same as outer-hip tenderness
Groin pain with catching or sharp pivot-related discomfort often leads the conversation in a different direction from soreness on the lateral side of the hip. That does not mean every groin pinch is a labral issue. It means the structure of your caution should change. You get less casual when symptoms sound mechanical.
Referred pain from the low back can imitate a hip problem
Back-generated symptoms can masquerade as hip pain with unsettling talent. Buttock pain, radiating discomfort, numbness, tingling, or a pain pattern that changes with spine position should widen the lens. A hip-only strategy may miss the driver entirely.
Why location alone can mislead even smart, athletic adults
Good athletes are still bad at being their own radiologist. That is not an insult. It is merely life. The sensible move is to treat pain location as a clue, not a verdict. Use it to narrow the field, not close the case.
Show me the nerdy details
Clinicians typically weigh a cluster of features rather than a single symptom: pain location, symptom behavior over time, gait changes, response to load, range-of-motion findings, strength, and whether pain reproduces with specific movements. The more “mechanical” the story sounds, the less useful generic advice becomes.
What an orthopedic evaluation may actually help you do
Rule out the problem that should not be self-managed
This is the boring, precious value of a good evaluation. It rules out the thing you should not be guessing about. That alone can save weeks of self-treatment roulette. When pain persists beyond 1 to 2 weeks despite modification, or when the symptom pattern includes catching, limping, or meaningful function loss, clarity becomes more valuable than optimism.
Build a return-to-play plan instead of a guess-and-check routine
A useful visit does not just name tissue. It helps build dose rules. How many minutes? Which movements irritate it? Which signs mean back off? What should improve over 2 weeks if the plan is working? That kind of structure feels less exciting than a magic phrase and far more useful on Tuesday night. If physical therapy enters the conversation, some readers also benefit from understanding the practical side of physical therapy copay versus coinsurance before starting treatment.
Know when imaging matters and when it changes very little
Imaging can matter. It can also become the world’s most expensive weather report if it does not change management. Sometimes the exam and history drive the plan more than a picture does. Sometimes the picture matters because it changes safety, expectations, or next steps. The best conversation is not “Do I need imaging?” in isolation. It is “Will imaging change what we do?” That question becomes even sharper when you have seen how often MRI findings and pain symptoms do not line up as neatly as people expect.
The best visit outcome is clarity, not just a prescription
People often imagine success as leaving with a medication or a dramatic label. But clarity is a better prize. Knowing what to avoid, what to train, how to dose return, and what counts as progress is usually more powerful than a bag of vague reassurance.
Coverage tier map: what changes from Tier 1 to 5 in decision complexity
- Tier 1: Mild soreness, no limp, easy to modify
- Tier 2: Recurring next-day stiffness, load pattern emerging
- Tier 3: Repeated flare-ups despite self-modification
- Tier 4: Catching, limping, reduced daily function, unclear driver
- Tier 5: Red flags such as inability to bear weight, trauma, fever, numbness, severe night pain
Neutral next step: The higher the tier, the less useful solo experimentation becomes.
Don’t do this: the “weekend warrior reset” that keeps restarting the injury
Rest all week, overplay on Saturday, repeat
This cycle is wonderfully common and wonderfully unhelpful. Symptoms settle just enough to create false confidence, then one long session reloads the exact tissues that never regained tolerance. It feels like random bad luck. It usually is not. It is a dosage problem wearing a fake mustache.
Using pain-free moments as proof that the issue is gone
Pain can dip before capacity returns. Quiet is not the same as healed. Plenty of players feel fine at the start of a session and only discover the truth after repeated decelerations, lunges, or the next morning’s first steps. Do not let 20 good minutes write the whole story.
Chasing harder massage, harder stretching, harder drills
When symptoms linger, people often turn up the volume on whatever they already tried. More pressure. More reps. More force. More “mobility.” Sometimes what the hip needs is not intensity. It is a cleaner decision tree and better pacing.
Confusing temporary relief with tissue readiness
This is the heart of the whole article. If you remember one sentence, make it this one. Relief can be real and still be temporary. Readiness means the hip handles the load and the recovery window. That is a different standard, and a better one.
Name the pain pattern: location, trigger, timing.
Reduce dose: shorter sessions, slower ramp, fewer wide chases.
Watch the 24 to 48 hour response, not just on-court feelings.
Escalate care if you limp, catch, cannot bear weight, or keep relapsing.
Strength, control, and movement: what long-term pain management usually needs
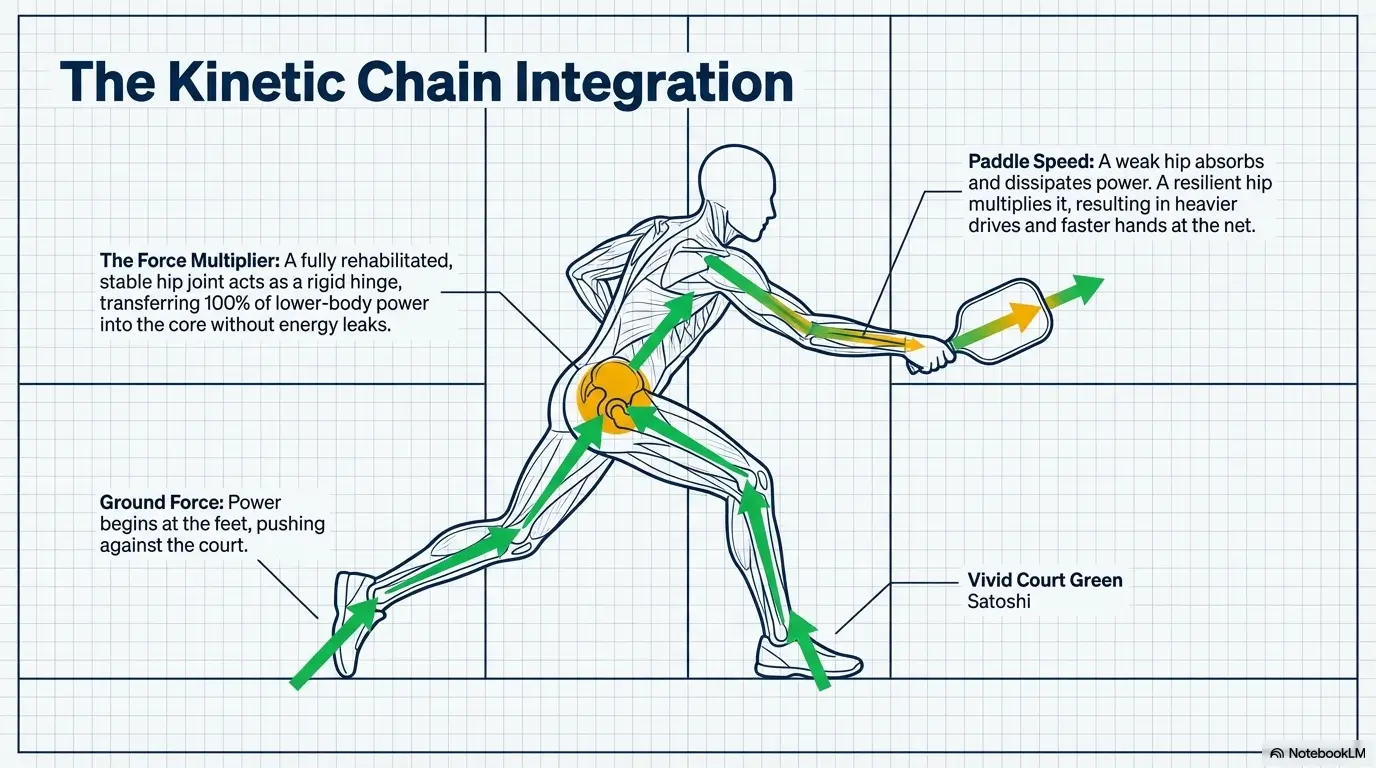
Hip abductors, glutes, trunk control, and balance all matter here
The hip does not work alone during pickleball. It collaborates with the trunk, pelvis, knee, foot, and your decision to chase a ball you had no business chasing. Long-term management usually needs strength, yes, but also control and timing. If the pelvis wobbles, the trunk drifts, and the leg has to improvise under speed, the hip often absorbs the confusion.
Why change-of-direction tolerance beats generic gym strength alone
Being strong in a calm gym does not automatically mean you are ready for a sport built on short reactions and rotational choices. Pickleball asks for braking, re-accelerating, recovering balance, and tolerating repeated low positions. That is why clinic-table success and court success are cousins, not twins.
Mobility is useful, but stability often decides whether pain returns
This is where many programs get lopsided. Mobility has appeal because it feels immediate. Stability and force control feel slower and less glamorous. Yet the hip that moves beautifully without controlling load is often the hip that keeps writing angry notes after league night. The same off-court logic shows up in unexpected places too, including orthopedic pain management for remote workers, where daily sitting and poor movement rhythms quietly shape recovery capacity.
Build capacity for pickleball, not just for the clinic table
The end goal is not to ace three exercises and declare victory. It is to tolerate a real match, a realistic warm-up, a few awkward reaches, and the next morning without drama. That means progression matters. Volume matters. Recovery matters. So does honesty. You cannot bluff biology with motivational quotes.
- Train strength, balance, and change-of-direction tolerance together
- Judge success by next-day function, not only by the session itself
- Progress the sport dose as carefully as the exercise dose
Apply in 60 seconds: Ask yourself whether your current plan trains the hip for a court, or only for a clinic mat.
When to seek help
Seek urgent care now if
- You cannot bear weight
- Pain followed a fall or collision
- You have fever, swelling, deformity, or severe night pain
- You notice numbness, weakness, or loss of bladder/bowel control
Book a medical evaluation soon if
- Pain lasts more than 1 to 2 weeks despite modifying activity
- You have groin pain with catching or locking
- You limp during or after play
- Symptoms keep returning every time you resume normal play
There is a quiet dignity in getting help before the situation gets theatrical. You do not win extra points for waiting until the body is shouting. You just make the eventual plan harder. MedlinePlus and AAOS both frame hip problems in a way that supports this common-sense threshold: persistent pain, meaningful function change, and mechanical symptoms deserve more than home improvisation.
Next step
Do this today: use a 7-day “pain and load” log
- Record when the pain appears
- Note exact pain location
- Track play duration, intensity, and next-day stiffness
- Bring that pattern to a clinician or use it to guide smarter activity modification
If you do only one thing after reading this, make it the log. Not because tracking is glamorous. It is not. Tracking is the plain oatmeal of self-management. But it reveals patterns your memory edits out. It separates the dramatic story from the useful one. Within 7 days, you may notice that symptoms are less about one magical stretch and more about session length, wide lunges, consecutive play days, or the first 12 hours after exertion. That is actionable. That is how uncertainty starts to shrink.
Mini calculator: is your weekly jump too big?
Compare last week’s total minutes on court to this week’s planned total.
Simple check: If your plan jumps by more than roughly 20 to 30 minutes across the week, and your hip is already irritated, treat that as a caution flag rather than a dare.
Neutral next step: Cut one session or shorten two sessions before you test a bigger week.
FAQ
Is it okay to play pickleball with hip pain?
Sometimes, yes, but only if the pain is mild, does not cause limping, settles with modification, and does not worsen over the next 24 to 48 hours. If pain changes your gait, produces catching, or keeps returning every time you resume normal play, step out of self-experiment mode and get assessed.
Is walking good or bad for hip pain from pickleball?
Walking is often useful because it keeps you moving without the sudden pivots and wide reaches of pickleball. It is not universally good in every situation, but gentle, tolerable walking often supports function better than total shutdown. Use your symptom response over the next day as the scorecard.
What is the difference between hip arthritis and a hip flexor strain?
A hip flexor strain usually has a clearer activity trigger and can feel sharper in the front of the hip, especially with lifting the knee or resisting hip flexion. Hip arthritis often behaves more like stiffness, reduced range of motion, and pain that affects ordinary tasks such as getting up from a chair or walking after sitting. Real life, of course, likes mixed signals, so evaluation matters when the story is unclear.
Can pickleball cause a labral tear?
Pickleball involves pivots, rotation, deceleration, and low reaching, so it can aggravate labral symptoms or reveal an existing issue. But not every groin pinch is a labral tear. Groin pain with catching, locking, or a sense of mechanical snagging should move you toward a clinical evaluation rather than broad internet guesswork.
Should I use heat or ice after playing?
Some people prefer heat for stiffness and ice for post-activity irritation. Neither is a moral virtue. Use the one that helps symptoms without encouraging you to overdo the next session. Relief is useful, but it should sit inside a larger load-management plan.
How long should I rest before returning to court?
There is no single number that fits everyone. What matters more is whether you can return with a lower dose, tolerate it during play, and avoid a meaningful next-day flare. For many players, partial modification works better than complete rest followed by a full-dose comeback.
When does hip pain need imaging?
Imaging is most useful when it changes management. Severe pain, trauma, inability to bear weight, or persistent symptoms with mechanical signs may make imaging more relevant. In milder cases, the history and physical exam often do a lot of the heavy lifting first. And if a clinician recommends imaging later, it can help to know what failed conservative care for MRI approval may mean in practical terms.
Why does my hip hurt more the day after I play?
That usually suggests your hip tolerated the session poorly even if it seemed manageable in the moment. Next-day stiffness or soreness can reflect volume, intensity, repeated pivots, or simply too much court time too soon. It is one of the clearest reasons to track both session dose and next-day response.
Can physical therapy help pickleball-related hip pain?
Often, yes. A good program can improve strength, movement control, balance, and return-to-play progression. More importantly, it can help match the plan to the actual problem instead of treating every hip complaint like the same generic inconvenience.
What shoes or court changes may reduce hip irritation?
Stable court shoes in decent condition and a more forgiving load plan often help more than people expect. Hard surfaces, worn shoes, and long sessions can all increase irritation. Sometimes changing from singles to doubles for a stretch is a smarter intervention than buying yet another gadget.
Final thought
The curiosity loop at the start of this article was simple: when does a friendly sport become a problem for the hip, and what do you do without turning into either a martyr or a hermit? The answer is less dramatic than most people want and more effective than most people expect. You get specific. You reduce the right dose. You respect red flags. You stop using temporary relief as proof of readiness. And you build back toward capacity instead of bargaining with symptoms one game at a time.
Within the next 15 minutes, make your first move concrete: write down your exact pain location, your last 3 sessions, and what happened the next morning. That tiny record is often the hinge between vague frustration and a real plan.
Last reviewed: 2026-03.
