
At 2:17 a.m., Hip Pain Transforms Bedding into Hostile Architecture
For side sleepers, the problem is rarely just “bad sleep.” It is often a mix of pressure, alignment, and tissues that were already irritated long before the lights went out.
Orthopedic pain management for side sleepers needs to be less dramatic and more precise. Not every sore hip wants stretching, not every painful night means arthritis, and not every mattress problem is actually a mattress problem.
This guide helps you identify your nighttime hip pain pattern, discover which positions calm the nerves, and avoid popular fixes that quietly make things worse. We focus on conservative methods—symptom patterns and pressure behavior—instead of miracle claims.
Because a calmer night starts with a clearer pattern. And a clearer pattern beats desperation.
Table of Contents
Safety / Disclaimer
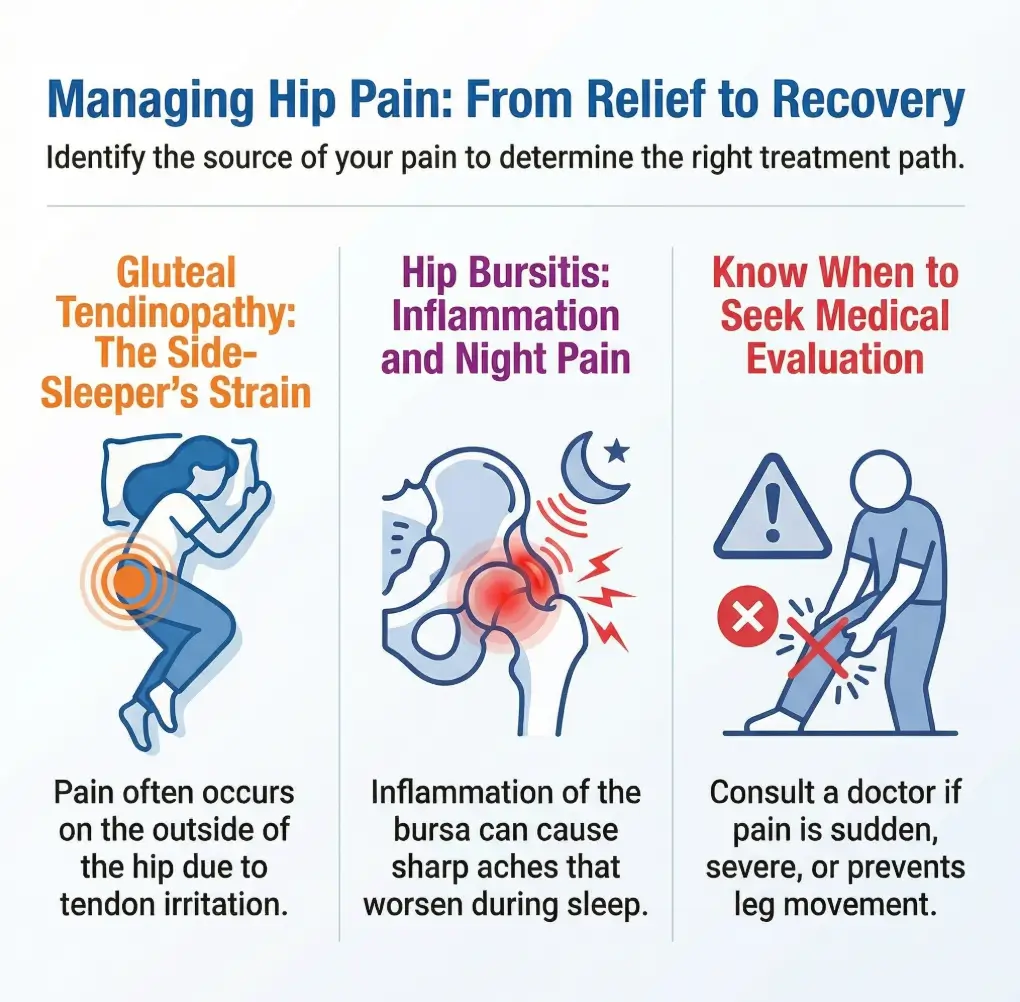
This article is educational and not a diagnosis or a substitute for medical care. Hip pain at night can come from greater trochanteric pain syndrome, bursitis, tendon irritation, osteoarthritis, labral pathology, referred lumbar pain, or other causes. Guidance here stays conservative on purpose. That is not timidity. That is respect for the fact that bodies are complicated, sleep loss makes judgment worse, and pain that keeps waking you deserves a calm, sensible plan.
Recent trauma, inability to bear weight, fever, major swelling, numbness, weakness, sudden severe pain, or unexplained pain that keeps escalating should not be handled like a do-it-yourself sleep puzzle. Those are evaluation problems, not pillow problems.
- Use position changes and load reduction first
- Watch for red-flag symptoms, not just pain intensity
- Do not turn a sleep tip into a diagnosis
Apply in 60 seconds: Decide now whether your pain fits a self-care trial or whether it already belongs in a clinician’s office.
Who this is for / not for
Who this is for
- Adults whose hip pain gets worse when lying on one side
- Side sleepers trying to reduce pressure pain and wake-ups
- Readers looking for practical positioning, mattress, pillow, and activity-modification ideas
- People who want a function-first plan before guessing at gadgets or aggressive stretches
Who this is not for
- People with recent trauma, inability to bear weight, fever, major swelling, numbness, weakness, or severe unrelenting pain
- Readers seeking a self-diagnosis instead of an evaluation
- Anyone looking for overnight cure claims or one-size-fits-all sleep hacks
I like side sleeping too. It feels familiar, cocooned, almost automatic. But once a hip is irritated, the same posture that used to feel like comfort can become a small compression machine operating for 6 to 8 hours. That is why this article is built around realism. Not “sleep perfectly.” Not “buy the deluxe orthopedic moon-pillow.” Just what can help tonight, what tends to backfire, and how to tell when this has drifted beyond self-management. For readers juggling multiple age-related aches at once, a broader guide to orthopedic pain management for older adults can also add useful context.
Eligibility Checklist: Is a 3-night self-care trial reasonable?
- Yes: Pain is positional, you can still walk, and symptoms are stable enough to observe.
- Yes: You can identify one or two movements or positions that clearly worsen it.
- No: Pain is severe, unexplained, rapidly worsening, or paired with weakness, fever, or recent injury.
- No: You cannot bear weight or the pain feels dramatically different from your usual aches.
Next step: If you checked a “No,” skip the experiment phase and seek evaluation.
Night Pain First: Why Side Sleeping Can Turn a Manageable Hip Into a 2 A.M. Problem
Compression changes everything when the sore side becomes the loaded side
During the day, your hip shares the job with movement. At night, especially in side-lying, the tissues around the outer hip can get pinned under your body weight for long stretches. That changes the conversation. The American Academy of Orthopaedic Surgeons notes that hip bursitis pain is often worse at night when lying on the affected hip. Even when bursitis is not the full story, the compression principle still matters. Tendons, bursae, and pressure-sensitive tissues are not famous for enjoying being squashed until dawn.
Why nighttime pain often feels sharper, meaner, and more personal than daytime pain
Night pain is psychologically rude. Daytime pain has competition: errands, email, work, stairs, groceries, life. Night pain gets the whole stage, a spotlight, and a microphone. The room is quiet. You are tired. Your body is less distracted. Sensation feels louder. That does not automatically mean something catastrophic is happening, but it does mean your perception of threat and irritation often grows in the dark.
The hidden cycle: pain, poor sleep, more sensitivity, worse pain the next night
This is the part many people miss. One rough night does not just make you grumpy. Poor sleep can lower your tolerance for discomfort the next day, which then makes the next night more fragile. I have watched this cycle in my own life with shoulder pain and once, memorably, with a mattress topper that felt “supportive” until 1:00 a.m. and “medieval” by 4:30. The point is simple: the longer the pattern continues, the less useful brute willpower becomes. In that sense, hip pain joins the same family of sleep-position puzzles people recognize in the recliner-versus-bed debate after shoulder surgery.
Pull-quote: Side sleeping is not the villain. Unmanaged pressure plus irritated tissue is.
Start With the Pattern: What Your Nighttime Hip Pain May Be Telling You
Outer hip pain that hates direct pressure
If the pain lives on the outside of the hip, feels tender to direct contact, and flares when you lie on that side, compression-sensitive structures move higher on the suspect list. People often call this “just bursitis,” but real life is usually less tidy. Greater trochanteric pain syndrome can involve irritated tendons, bursae, or both. The label matters less at home than the pattern: pressure hurts, side-lying hurts, and long days of walking or stairs may quietly set the stage.
Deep joint pain, stiffness, and the “I cannot get comfortable” pattern
Deep groin-side pain, catching, stiff transitions, or a sense that every position is wrong can suggest a different category of problem. Osteoarthritis, labral irritation, and other intra-articular issues tend to create a more internal, less “touch this exact spot and I hiss” kind of discomfort. Morning stiffness that takes time to unwind also matters here. Not because it gives you a home diagnosis, but because it helps you stop using outer-hip strategies for a deeper-joint problem.
Pain that travels from the back or buttock into the hip region
Some hip pain is not hip-first pain. Mayo Clinic notes that hip pain can sometimes be referred from the lower back. That matters because a pillow setup that reduces direct pressure may still fail if your lumbar position is the bigger irritant. If the discomfort tracks from the buttock, shifts with spinal posture, or changes with sitting more than with lying on the hip itself, broaden the frame. Not every “hip pain at night” story begins at the hip. Readers trying to untangle that overlap may also find it useful to compare hip pain versus spine pain patterns.
Morning clues that matter more than people think
The first 10 minutes after waking are excellent detectives. Are you stiff but better once you move? Do you limp for twenty steps? Is the outside of the hip angry to touch? Do stairs feel worse than walking? These clues are plain, unglamorous, and more useful than the internet’s favorite circus act of self-diagnosis-by-random-video.
Show me the nerdy details
Compression-sensitive lateral hip pain often reflects load intolerance in tissues around the greater trochanter. Deep joint pain patterns may behave differently, especially when stiffness, catching, or groin-dominant pain is present. Referred pain muddies the picture further. That is why position response, tenderness pattern, morning behavior, and daytime triggers are often more clinically useful than one dramatic symptom in isolation.
- Outer hip tenderness points differently than deep groin stiffness
- Back-linked pain can imitate “hip pain” at night
- Morning behavior gives clues your mattress never will
Apply in 60 seconds: Write down where the pain is worst: outer hip, groin/deep joint, or back-to-hip pathway.
Pillow Placement Matters More Than Most People Realize
Between-the-knees support: when it helps and why
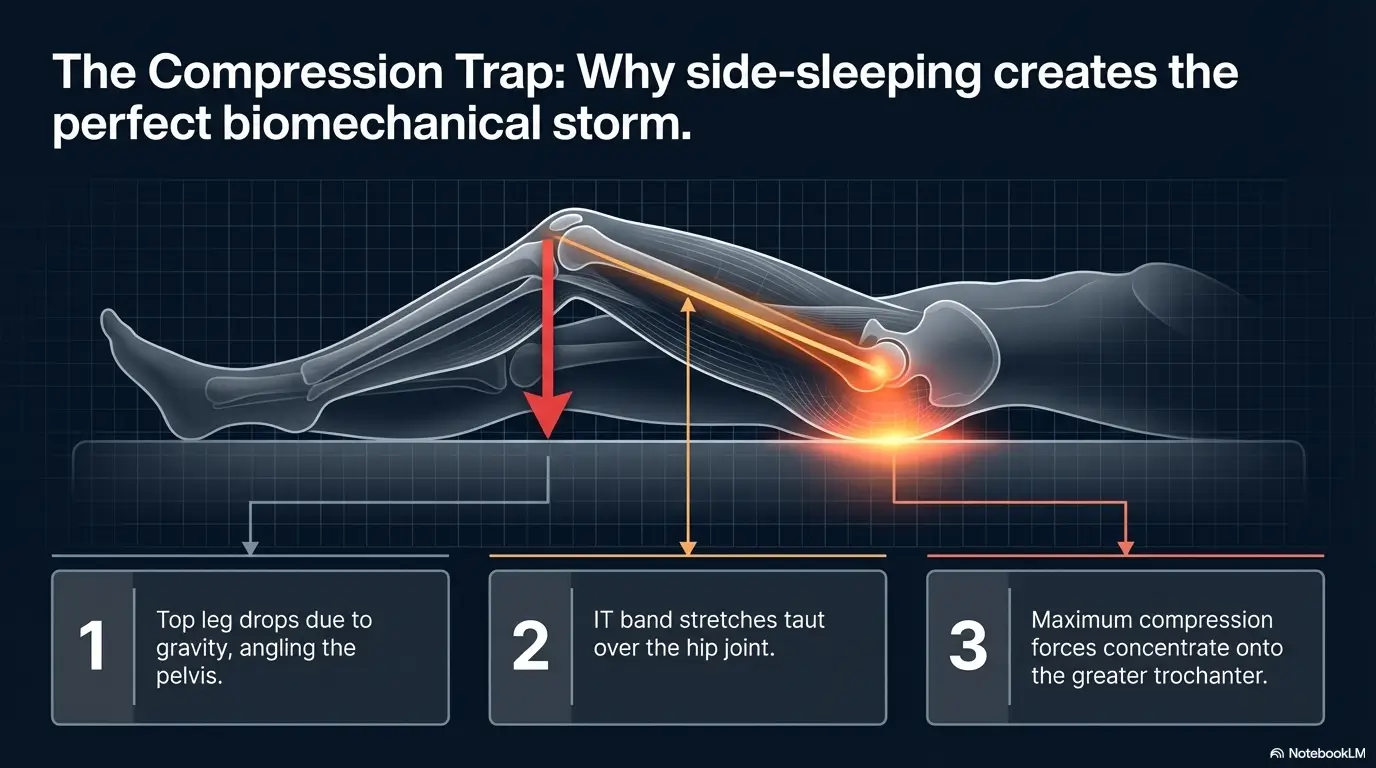
Cambridge University Hospitals advises side sleepers with gluteal tendinopathy to place a pillow between the knees to help keep the hips in a more neutral alignment. This is not mystical. It is mechanical. Without support, the top leg often drops forward and inward, adding adduction and rotational stress that can compress the outside of the lower hip. A pillow can reduce that twist and calm the tissues that have been filing complaints all week.
Ankle-to-knee alignment: the small detail that changes hip load
A common mistake is using a tiny pillow that supports only the knees while the ankles drift into a different zip code. That can still leave the hip twisted. Ideally, the support runs from knee toward ankle so the whole top leg rests in a quieter position. Think less “decorative cushion” and more “boring structural assistant.” Design rarely gets poetry, but structure wins arguments.
When a thin pillow fails and a thicker one overcorrects
Too thin, and the leg still collapses inward. Too thick, and you may feel pushed into awkward external rotation or back strain. The right size is the one that makes the hip feel less tugged, not more propped. This is where a folded bath towel can outperform a luxury pillow with branding that sounds like a Scandinavian startup. I once used a folded duvet corner in a hotel because the provided pillow was basically a resigned pancake. It worked better.
Let’s be honest… most people are not using the pillow in the way they think they are
If you start the night perfectly arranged and wake up twisted like a dropped charging cable, the setup is not truly working yet. Your nighttime system has to survive actual sleep, not just the optimistic 18 seconds before you close your eyes. Sometimes that means using a longer body pillow, adding a small pillow in front of the trunk, or experimenting with a semi-prone position so you are not fully stacked on the irritated side. That tradeoff is familiar to anyone who has wrestled with knee pillow versus body pillow choices for night pain.
Decision Card: Thin pillow vs thicker support
- Your lower back feels crowded or twisted
- You are already fairly aligned
- More height makes the top hip feel perched
- Your top leg still drops inward
- The outside hip feels stretched or compressed
- You wake with the knees touching and pain worse
Neutral action: Test one pillow height for 3 nights before changing anything else.
Don’t Sleep on the Angry Side? Not Always That Simple
When avoiding the painful side helps
Mayo Clinic’s general hip-pain guidance advises avoiding direct pressure and trying not to sleep on the affected side. That is a sensible starting point. If the problem is clearly pressure-sensitive, removing the pressure source is often the fastest way to reduce nighttime irritation. Sometimes the smartest intervention is not heroic. It is simply refusing to keep poking the bruise.
When switching sides just creates a different kind of irritation
But here comes the plot twist: moving to the non-painful side can still bother the painful hip if the top leg drops into a bad position, or it can light up the other side if that tissue is already grumpy. People sometimes interpret this as proof that “nothing helps,” when really the setup is incomplete. Side switching without support is not a strategy. It is a coin toss.
Back-sleeping as a temporary detour, not a moral victory
Back-sleeping can reduce direct lateral compression, but it is not morally superior. There is no prize. Some people sleep beautifully on their backs. Others lie there like a worried museum exhibit. If back-sleeping feels unnatural, use it as a temporary reduction strategy, not a spiritual conversion. A pillow under the knees can soften the position for some readers, especially when back or hip stiffness is part of the picture.
How to build a tolerable “best available position” instead of chasing perfection
This is the sentence I wish more people heard: you do not need the perfect position, only the least provocative one you can reliably maintain. Best available beats ideal imaginary. If pain is a 7 on one side and a 4 on another with support, that is useful. The body often improves through tolerable consistency, not through cinematic breakthroughs.
Practical rule: choose the position that gives you the fewest wake-ups and the least angry first 10 minutes in the morning. That is your current working winner.
Mattress, Topper, or Myth: What Surface Changes Are Actually Worth Trying
When a mattress is too firm for a pressure-sensitive hip
If your outer hip pain behaves like a pressure problem, an overly firm surface can be unhelpful. A firm bed can keep the body from sinking enough to distribute weight, leaving the greater trochanter region taking a very direct bargain it did not agree to. This does not mean soft is automatically better. It means pressure distribution matters.
When a softer surface quietly worsens alignment
Here is where people get tricked. A softer mattress can feel better for 20 minutes and worse over 6 hours if it allows the pelvis or trunk to sag into awkward alignment. Comfort on contact is not the same thing as comfort across the night. Mattresses are like first dates and office chairs. Initial charm can be a terrible predictor.
The case for a topper before replacing the whole mattress
For many readers, a topper is the more rational experiment before an expensive mattress replacement. It changes the pressure profile without forcing a full household financial summit. This is especially true if your current mattress is not ancient and your pain seems very position-specific. One measured change beats a dramatic purchase fueled by 3:00 a.m. resentment. If you are already weighing surface changes, the tradeoffs in a 2-inch versus 3-inch mattress topper comparison can help frame the decision more clearly.
Here’s what no one tells you… expensive sleep products often fail because the setup is wrong, not because the label is cheap
A premium mattress without knee support, trunk support, or attention to daytime load can still fail beautifully. Price cannot out-negotiate mechanics. I once tried a very expensive “supportive” mattress in a showroom and felt briefly like a prosperous cloud. At home, my shoulder hated it and my hip sent objections in writing. The lesson was humbling and extremely expensive for about eleven days.
Mini Calculator: How costly is your current night pattern?
Take your average nightly wake-ups from hip pain and multiply by the average minutes it takes to settle again.
Example: 3 wake-ups × 12 minutes = 36 minutes of disrupted sleep.
That number is not a diagnosis. It is a clarity tool. A “small” hip issue can quietly steal 180 minutes of sleep across 5 nights.
Neutral action: Track the number for 3 nights before you buy a new sleep surface.
Before Bed, Not in Bed: The Calming Routine That Makes Night Less Combative
Heat, pacing, and gentle movement before lying down
The worst time to ask an irritated hip to calm down is after you have already pinned it under body weight. A short wind-down can help lower the volume before bed. That might be 5 to 10 minutes of gentle walking around the house, light range-of-motion work, or a warm shower. Some people do well with heat before bed. Others prefer a brief cooling strategy earlier in the evening. This is a response test, not a religion.
Why aggressive late-night stretching can backfire
People love to stretch the sore thing because it feels tight. But “tight” and “needs more pulling” are not synonyms. Irritated lateral hip tissues, especially if compression-sensitive, often do not appreciate aggressive end-range stretching late at night. You are not buttering a croissant. You are dealing with a structure that may already be overloaded.
The role of daytime load management in nighttime pain
If you climbed six flights of stairs, did a hilly walk, sat crooked for three hours, then lunged into an enthusiastic workout, the hip may arrive at bedtime already annoyed. Night pain often reflects accumulated daytime load, not just poor sleep posture. That is why good nighttime relief sometimes starts with a quieter afternoon. Not glamorous, but mechanically sound. The same pattern shows up in other activity-triggered flares, including pickleball-related hip pain that builds after repeated loading.
What “calm the tissue down” actually means in real life
It means reducing the amount of compression, stretch, and repetitive load that the tissue cannot currently tolerate. It also means lowering the chaos of your experiments. Choose one or two changes and let them breathe. A calm plan is more persuasive than five desperate hacks fighting in the dark.
- Use a short calming routine, not a punishment circuit
- Avoid hard stretching when tissues already feel provoked
- Daytime overload can show up as nighttime pain
Apply in 60 seconds: Choose one pre-bed routine tonight: 5 minutes of easy walking or a warm shower, not both plus six other things.
Common Mistakes
Stretching the sore hip harder because it feels tight
This is the classic trap. The body sends a sensation of guarding or irritation, and the mind translates it as a flexibility problem. Sometimes it is. Often at night, especially with side-lying pain, it is a load-tolerance problem instead. Pulling harder may simply produce a more poetic version of the same pain.
Sleeping without knee support and blaming the mattress alone
The mattress gets accused for crimes committed by alignment. Surface matters, yes. But if the top leg is collapsing forward every night, the mattress is only part of the cast. Knee support is one of the cheapest high-leverage changes available, which makes it tragically easy to skip because it is not glamorous enough for the internet.
Trying five new fixes in one night and learning nothing from any of them
One new pillow, one stretch video, one topical cream, one new sleep position, one heating pad, one panic-purchase topper. By morning, you know only that you are tired and resentful. Change one main variable at a time. The body is not a casino machine. Pulling every lever at once does not create wisdom.
Ignoring daytime mechanics while obsessing over sleep posture
If limping, long sitting, stair-heavy days, or side-loaded exercise are feeding the problem, perfect pillow placement may not be enough. Night is where the symptoms become dramatic, but the script may have been written much earlier in the day. Desk-bound readers who notice a hip-and-back blend to their symptoms may also recognize pieces of orthopedic pain management for remote workers in that pattern.
Assuming all outer hip pain is “just bursitis”
Outer hip pain is common, but the blanket label can be misleading. Tendons, bursae, spinal referral, and gait mechanics can all participate. A casual label is not the end of the story. It is sometimes barely the preface.
Doctor Visit Prep List: What to gather before you compare treatment options
- Where the pain is worst: outer hip, groin, buttock, or back-to-hip
- How many nights per week it wakes you
- What positions help or worsen it
- Morning stiffness length: under 10 minutes, 10 to 30, or longer
- Daytime triggers: stairs, walking, sitting, exercise, or lying directly on the side
Neutral action: Bring 3 nights of notes instead of trying to remember everything in the exam room.
Don’t Do This: Popular Sleep Fixes That Can Keep the Hip Irritated
Forcing a painful side-lying position to “get used to it”
Exposure has its place in rehab. Randomly marinating an already irritated outer hip in hours of pressure is usually not it. Tissues that are compression-sensitive do not always learn bravery from being flattened into a mattress. They sometimes learn vengeance.
Buying ultra-firm support products without understanding pressure pain
There is a cultural myth that “more support” always means “harder.” For pressure pain, that can be exactly backward. What you need is enough support to maintain alignment and enough pressure distribution to avoid creating a nightly pressure point contest.
Using deep massage tools on a highly irritated lateral hip
This one tempts people because it feels active and decisive. But aggressive massage guns, hard balls, or deep tissue tools over a very irritated lateral hip can turn a touchy structure into a furious one. Sometimes the winning move is strategic gentleness. Your hip is not a rusted hinge.
Turning temporary pain relief into a full self-treatment plan without reassessment
If heat gives you 30 minutes of relief, good. That is useful. It does not mean heat is now the master key to the kingdom. Temporary relief is data, not a complete theory. Reassess the pattern. If you are still getting woken repeatedly after a sensible self-care trial, collect the clue and escalate appropriately.
- Helpful: Reduce direct pressure, support alignment, simplify experiments
- Risky: Force the painful side, use hard tools on angry tissue, confuse short relief with a full plan
The Daytime Link: Why Your Walking, Sitting, and Stairs May Be Ruining Your Night
Limping, pelvic drop, and irritated tendons after a long day
The body keeps score in remarkably petty ways. If your gait changes because you are protecting one side, the tendons and soft tissues around the hip can end the day more overloaded than you realize. Night pain may then look like a sleep issue when it is partly a movement-budget issue.
Long sitting and the stiff-then-painful transition
Some readers notice their worst nights after long desk days or long drives. Sitting can stiffen the hips, alter back posture, and make the transition to walking feel creaky or sharp. When the body spends hours in one position and then asks the hip to behave beautifully in bed, the result can be… diplomatically disappointing.
Exercise habits that load the hip in ways side sleepers overlook
Side-lying leg raises, steep hill walking, high-volume stairs, poorly tolerated squat variations, and sudden mileage increases can all feed lateral or deep hip irritation. Exercise is not the villain, but timing and dosage matter. The body usually tolerates what it is prepared for, not what your optimism ordered on sale.
Why nighttime relief often begins at 2:00 PM, not 2:00 AM
This is where the article’s hook closes its first loop. The night feels like the crisis, but the solution often begins long before the pillow. If you can reduce the hip’s daytime aggravation by even 15 to 20 percent, the night may become far less dramatic. Sometimes the most “sleep” intervention is actually a load-management intervention in daylight clothes.
My rule of thumb: when night pain is rising, do not judge your hip only by bedtime. Judge the whole day that delivered it to bedtime.
Long sitting, stairs, limping, side-loaded exercise
Outer hip gets pressure-sensitive or joint feels more reactive
Side-lying or poor alignment amplifies the complaint
Reduce load, support alignment, test one controlled change
When to Seek Help
Pain that wakes you repeatedly despite position changes
If you have given the hip a fair trial with alignment support, pressure reduction, and a few nights of calmer load, but it still wakes you again and again, that is useful information. Repeated wake-ups are not a character test. They are a sign that the current self-management tools may not be enough.
Pain with weakness, instability, or trouble bearing weight
Weakness, buckling, a sense that the leg does not trust itself, or major trouble bearing weight deserve medical attention sooner. Those features raise the stakes beyond ordinary positional discomfort.
Night pain with fever, unexplained weight loss, or recent injury
These are not “wait and see if the pillow helps” details. They change the frame entirely and should prompt evaluation.
Symptoms that linger beyond a reasonable self-care window
A reasonable window is not a fixed universal number, because severity varies, but if the pattern is not improving after a short, disciplined trial, or if it is gradually worsening, it is time to widen the plan. That may mean a primary care clinician, sports medicine physician, orthopedic clinician, or physical therapist depending on context and access. If cost questions are part of the hesitation, understanding physical therapy copay versus coinsurance can make the next step feel less foggy.
When an orthopedic clinician or physical therapist can help sort the pattern faster
A good clinician can separate pressure-sensitive lateral pain from deeper joint patterns, back referral, gait contributions, and load-management issues far more efficiently than an exhausted browser history. This is not a failure of independence. It is a better use of evidence.
- Repeated wake-ups despite smart changes matter
- Weakness, instability, fever, or recent trauma change the urgency
- Evaluation can shorten the guessing phase dramatically
Apply in 60 seconds: Decide now what your threshold is for booking an appointment: 3 nights, 2 weeks, or immediately for red flags.
Next Step
Try this tonight: set up one controlled sleep experiment
Do not end this article by buying four products and declaring war on your mattress. End it by running one clean experiment. That is how you get useful information instead of emotional clutter.
Choose one pillow strategy
Pick either a between-the-knees pillow that supports toward the ankles or a body-pillow setup that keeps the top leg from dropping forward.
Choose one position change
Either avoid the painful side entirely for a few nights or test a supported semi-prone setup on the non-painful side. One main position change. Not three.
Track wake-ups, pain side, and morning stiffness for three nights
Write down three simple numbers or notes: how many times you woke, which side you were on, and how stiff you felt on rising. That alone can make your next decision 10 times better.
Keep the routine simple enough to actually learn from it
This matters. If the experiment is too complicated, you will abandon it or misread it. Boring data beats dramatic confusion every time.
Short Story: A reader once told me she had tried “everything” for night hip pain. When we unpacked “everything,” it turned out to be nine things in four nights, including a new topper, a massage gun, two stretch videos, three pillows, and a heroic attempt to become a back sleeper despite hating every second of it. We simplified it.
One pillow between knees to ankles. No sleeping on the sore side. Short walk after dinner. Three nights of notes. By the third morning, the pain was not gone, but it was less chaotic. She could finally tell what was helping and what was theater. That is often the first real win. Not a miracle. A map. For readers in a longer holding pattern before formal treatment, the mindset overlaps with pain management while waiting on a joint procedure.
Within the next 15 minutes, set up tonight’s pillow configuration and start a 3-night note on your phone. That is the honest next step. Not a miracle purchase. Not stoic denial. Just a cleaner experiment, a calmer hip, and a better shot at sleep.
Last reviewed: 2026-03.
Differentiation Map
What competitors usually do
- Open with generic sleep-advice clichés
- Treat all hip pain as the same condition
- Recommend a pillow, a mattress, and a stretch, then call it a plan
- Use vague headings like “Causes,” “Treatment,” and “Conclusion”
- Promise relief without separating pressure pain from joint pain or referred pain
- Skip the mistake patterns that keep readers stuck
How this outline avoids it
- Starts with the real reader problem: pain that spikes at night in side-lying
- Organizes the article around pressure, positioning, pattern recognition, and conservative management
- Distinguishes outer hip compression pain from deeper joint or referred patterns
- Builds standalone sections that can rank individually and still read as one coherent journey
- Uses mistake-driven framing to reduce trial-and-error frustration
- Ends with one concrete, trackable action instead of a vague “sleep better” farewell
FAQ
Why does my hip hurt more when I sleep on my side?
Because side sleeping can place hours of direct compression on the outer hip and can also change alignment if the top leg drops forward. If tissues are already irritated, that sustained pressure can make the pain louder at night.
Is side sleeping bad for hip bursitis or outer hip pain?
It can be aggravating, especially if you sleep directly on the painful side or let the top leg collapse inward. Side sleeping itself is not banned forever, but it often needs better support and temporary modification during a flare.
Should I sleep on the painful hip or the non-painful hip?
In many cases, avoid direct pressure on the painful side first. If you sleep on the non-painful side, use support between the knees and ideally down toward the ankles so the sore hip is not left hanging in a provocative position.
Does putting a pillow between my knees really help hip pain?
Often, yes. It can reduce adduction and rotation stress and keep the top leg from pulling the hip into a more irritating position. The pillow works best when it supports enough of the leg, not just the knees.
Is a firm mattress better for hip pain at night?
Not always. A mattress that is too firm can increase pressure on a sensitive outer hip. A mattress that is too soft can allow poor alignment. The better choice depends on whether your pain is more pressure-sensitive, more alignment-sensitive, or both.
Why does my hip pain feel worse at night than during the day?
Night increases pressure time, reduces distraction, and often follows a full day of accumulated load. Poor sleep can also make pain feel louder the next day, which can feed the next night’s flare.
Can arthritis cause hip pain only when I lie down?
Arthritis can contribute to night pain, but it is not the only explanation. Deep joint stiffness, pain with walking, painful transitions, and morning stiffness may point in that direction, but positional outer hip pain can come from other structures too.
What is the best sleeping position for side sleepers with hip pain?
The best position is the one that creates the least irritation and the fewest wake-ups. For many people, that means not sleeping directly on the painful side, using support between the legs, and sometimes trying a supported semi-prone or temporary back-sleeping setup.
When should nighttime hip pain be checked by a doctor?
Seek evaluation sooner if you have recent injury, fever, weakness, inability to bear weight, unexplained worsening, or repeated wake-ups despite smart position changes and a short self-care trial.
