
The First Shower: Strategy Over Soap
The first shower after hip surgery is rarely about soap. It is about timing, balance, incision rules, and a wet floor that suddenly feels far less innocent than it used to. Orthopedic pain management for showering is not about pushing through discomfort heroically; it is about making the routine safer, steadier, and far less exhausting.
The real frustration is how ordinary this task looks from the outside. You are technically “just showering,” yet the process can trigger pain, wobbliness, fatigue, and a quiet fear of one bad step or one careless twist. Without a plan, a basic hygiene task can become a setback that delays confidence and complicates recovery.
This guide helps you turn that vulnerable moment into a repeatable system. You will learn how to:
- • Time pain relief intelligently and reduce hip strain during transfers.
- • Protect the incision according to surgeon guidance.
- • Utilize shower chairs and grab bars that actually earn their footprint.
No drama. No recovery cosplay. Just a cleaner, calmer way through one of the trickiest ordinary tasks after surgery. Because the safest shower is usually the one that feels almost boring.
Table of Contents
Safety / Disclaimer
This article stays conservative. After hip surgery, showering instructions can differ based on incision closure, dressing type, surgeon protocol, posterior vs anterior precautions, weight-bearing status, and whether complications are present. Do not override your surgical team’s instructions on when to shower, whether the incision can get wet, or which movements to avoid.
Falls, wound problems, fever, new drainage, sudden swelling, calf pain, chest pain, or shortness of breath deserve prompt medical attention. The bathroom is not where pride should be auditioning for a lead role. It is a high-risk room with water on the floor, strange angles, and a body that is still negotiating trust with itself.
I have seen people make the same emotional mistake in recovery again and again: they treat the first shower like a test of character. It is not. It is a task. Tasks go better when they are broken into sequence, supported by equipment, and stripped of unnecessary drama.
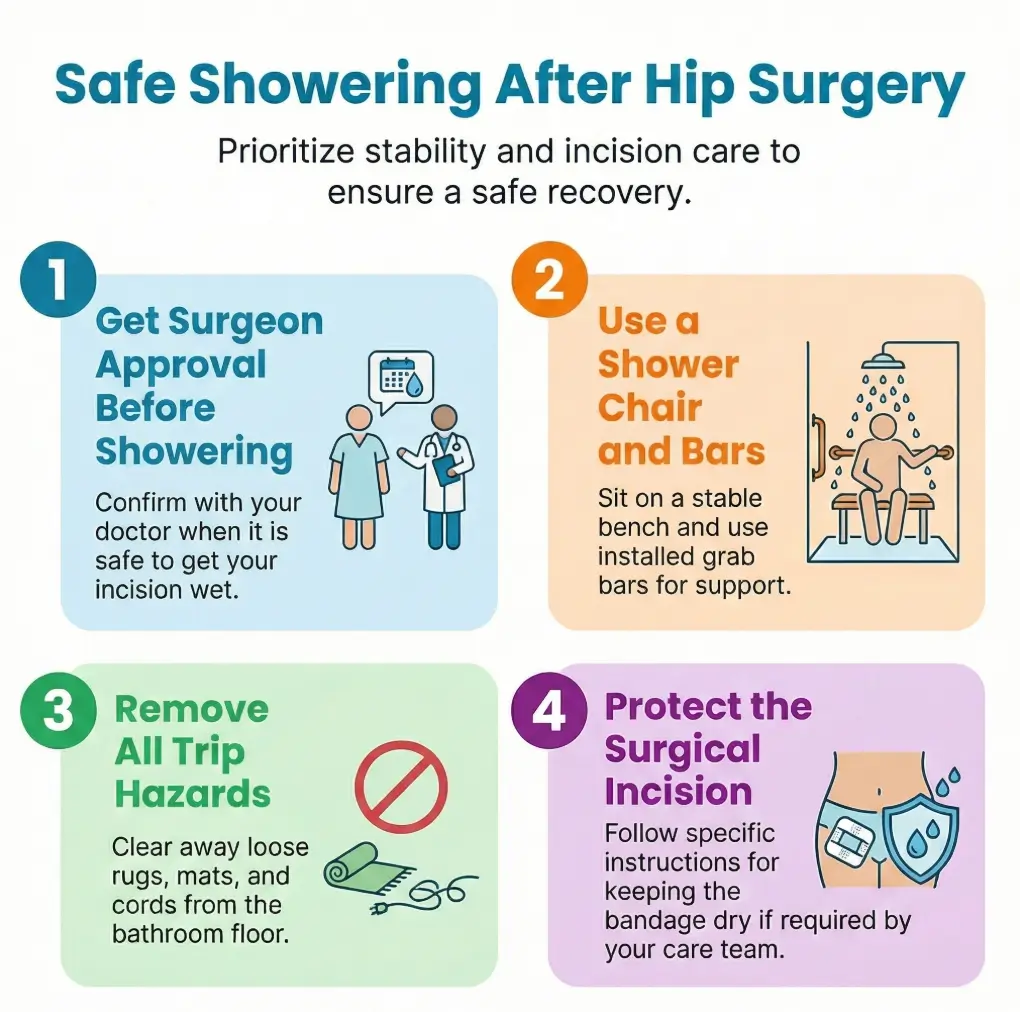
- Confirm when showering is allowed
- Protect the incision exactly as instructed
- Treat fall risk as seriously as pain
Apply in 60 seconds: Put your surgeon’s bathing instructions on your phone notes or bathroom counter before the next shower.
Who This Is For / Not For
Who this is for
- Adults recovering from hip replacement or other major hip surgery
- Patients trying to reduce pain, fear, and instability during showering
- Caregivers setting up a safer bathroom routine at home
Who this is not for
- Anyone with new wound drainage, fever, severe dizziness, fainting, or uncontrolled pain
- Patients who were specifically told not to shower yet
- People needing individualized clearance because of complications, revision surgery, or significant medical instability
There is also a middle group worth naming. Some readers are technically “allowed” to shower, but they are not ready to do it the way they used to. That is often where the real confusion lives. You may be cleared to get the incision wet, but not cleared to twist freely, bend casually, stand for long, or improvise on a slick tub floor like you are in a soap commercial from 1998.
One patient once described this stage as “being medically permitted but mechanically suspicious.” That is exactly it. Your care team may say yes to showering while your body says, “I would prefer a committee meeting first.” This guide is for that gap.
Eligibility checklist
Use this before a real shower.
- Yes/No: Did your surgeon or discharge instructions say showering is allowed?
- Yes/No: Can you stand or transfer safely with your current walker or support plan?
- Yes/No: Is the bathroom set up with a stable seat or bench if needed?
- Yes/No: Do you know exactly how to handle the dressing and incision?
- Yes/No: Can someone be nearby if you are still unsteady?
Neutral next step: If you answered “no” to any item, solve that one barrier before trying to “power through.”
Showering After Hip Surgery Starts Before the Water Turns On
Why pain management is really a timing problem, not just a medication problem
Many people think shower pain means they chose the wrong medication. Often, it means they chose the wrong timing. A shower asks your hip to tolerate standing, stepping, weight shifts, reaching, and mild fatigue in one compact sequence. If pain medicine has not had time to work, or if you waited until you were already exhausted, the whole routine becomes sharper and shakier.
That is why “I’ll shower now and take something after” is often a poor bargain. Comfort planning is not weakness. It is logistics. The pain does not care whether you are being stoic. It simply arrives on schedule. For some patients, this same collision between fatigue, stiffness, and bad timing also shows up later in the day as hip pain at night that feels worse than expected, which is another reminder that timing shapes pain more than pride does.
The pre-shower setup that prevents mid-routine panic
Lay out the towel, clean clothes, toiletries, walker, and any dressing supplies before the water starts. Put frequently used items between waist and chest level if possible. The point is to remove the tiny bad ideas that appear when you are wet and tired, such as reaching for shampoo on the floor or hopping one-handed while trying to catch a slipping towel. Recovery has a dark sense of humor. It loves to turn small laziness into large paperwork.
Here’s what no one tells you: the hardest part is often the transition, not the washing
The actual washing may only take 5 to 8 minutes. The stressful part is often everything around it: approaching the shower, stepping over a threshold, turning to sit, standing back up, drying off, and getting dressed without bending too much. I once watched a friend’s parent handle the warm water just fine, then nearly lose confidence completely at the point of stepping out. The lesson was simple. Practice the transitions, not just the shower.
Decision card: morning shower vs later shower
| Option | Best when | Trade-off |
|---|---|---|
| Earlier in the day | You have more energy and a helper nearby | May be too soon if stiffness is high right after waking |
| After meds have kicked in | Pain is better controlled and you are less guarded | Too late in the day may collide with fatigue |
Neutral next step: Pick one time window and keep it consistent for the next 2 or 3 showers so you can actually compare how it goes.
Incision Rules First, Comfort Second
When “getting clean” can quietly interfere with healing
There is a temptation, once the fog of surgery lifts a little, to think cleanliness is automatically healing. But wound care has rules, and those rules outrank the lovely human urge to feel normal again. MedlinePlus explains that after hip replacement, many patients are told not to shower until 3 to 4 days after surgery or until the surgeon says it is okay, and when showering is allowed, water may run over the incision but the incision should not be scrubbed or blasted directly. That sounds simple until you are standing there with soap in one hand and optimism in the other.
Dressing, waterproofing, and surgeon instructions: what must outrank convenience
The AAOS notes that many modern dressings are waterproof and are often left in place for 7 to 10 days, but this is exactly why individual instructions matter. “Waterproof” does not mean “freestyle.” It does not automatically answer whether you should remove anything, cover anything, or let water hit the site for long. Convenience has a very persuasive voice in the bathroom. Ignore it.
Why guessing about incision care is a terrible recovery bargain
If you are unclear about whether the dressing stays on, how long showering should last, or whether soap can go near the incision, stop and ask your surgical team. A five-minute phone call is cheaper than a week of anxiety and wound surveillance. Infection prevention is not glamorous content, but neither is an avoidable setback.
One of the quiet victories of a good post-op shower is this: you come out cleaner without creating a new problem for tomorrow. That is the standard.
Show me the nerdy details
Different surgeons use different closure methods, dressings, and bathing protocols. That is why general internet advice can only go so far. Mechanically, the wound question is separate from the hip movement question. A patient may be cleared to let water run over a dressing yet still need strict caution with twisting, deep bending, or unstable transfers. Keeping those two categories separate prevents a lot of confusion.
Pain Peaks in the Bathroom for Predictable Reasons
Warmth, standing, twisting, and fatigue can stack up fast
Bathrooms compress effort. Even a short shower can involve 10 or more little balance decisions in a small, slick space. Warm water may feel wonderful at first, but standing in one spot, turning slightly, or shifting weight while washing can make the hip bark louder by the minute. Pain in this setting is often not mysterious at all. It is a stack of predictable loads arriving too close together.
Why shower pain is often part orthopedic stress, part energy crash
Post-op bodies tire quickly. A shower can be a sneaky endurance event because it asks for upright tolerance, coordination, and focus all at once. That is why some people feel fine during minute 1 and surprisingly weak by minute 6. The problem is not always that the surgery “went wrong.” Sometimes the shower simply cost more energy than expected. For readers trying to zoom out and make recovery more manageable overall, a broader guide to pain management for seniors waiting on joint replacement can also help frame the difference between daily function and heroic overreaching.
Let’s be honest: feeling weak in the shower can be more frightening than painful
Fear changes movement. The moment you feel a wobble, you may stiffen, rush, twist, or grab awkwardly. Ironically, those protective reactions can increase pain and fall risk. I remember helping reorganize a bathroom for someone after hip surgery and realizing the fear was not really the water. It was the possibility of being trapped mid-task with shampoo in the eyes and no graceful exit. Once we added a seat, a handheld showerhead, and a better entry plan, the panic dropped more than the pain did. Often, that is the first win.
- Standing tolerance matters
- Fatigue can arrive before you notice it
- Fear can trigger rushed, painful movement
Apply in 60 seconds: Cut your next shower goal in half. Aim for a “good enough” clean, not a deluxe spa performance.
Equipment That Earns Its Place in a Post-Op Bathroom
Shower chair vs tub bench: which problem each one actually solves
A shower chair helps if the main issue is standing tolerance inside a walk-in shower. A tub transfer bench solves a different problem: the dangerous choreography of getting over a tub wall. These are not interchangeable in spirit, even if both look like humble pieces of medical furniture. One saves endurance. The other saves transitions.
AAOS guidance for hip replacement recovery mentions a stable shower bench or chair, a shower hose, and securely fastened safety bars or handrails. Notice the theme. The useful tools are boring. Boring is good. Boring does not skid, wobble, or tempt you into dumb improvisation. The same logic shows up in other rehab-friendly bathroom setups, including this guide to how a shower chair setup reduces strain in a painful bathroom routine.
Handheld showerheads, grab bars, and non-slip surfaces without the gadget circus
A handheld showerhead reduces twisting and allows seated bathing. Properly installed grab bars help with transfers. Non-slip mats or strips reduce slipping. The CDC’s fall-prevention materials repeatedly stress basics like grab bars, better lighting, and non-slip surfaces. That advice may feel almost insultingly plain, but plain is what prevents the operatic sequel nobody wants.
The best bathroom aids reduce decisions, not just effort
The true value of equipment is not merely muscular help. It reduces decision-making under fatigue. A bench says where to sit. A grab bar says where to place the hand. A caddy at waist height says where the soap lives. Post-op safety improves when the room stops asking existential questions.
Quote-prep list: what to gather before buying bathroom aids
- Type of shower: walk-in or tub/shower combo
- Threshold height or tub-wall height
- Your current weight-bearing and transfer ability
- Whether you live alone or have standby help
- Available wall support for professionally installed grab bars
Neutral next step: Write down these 5 details before comparing equipment so you buy for your bathroom, not for a stock photo.
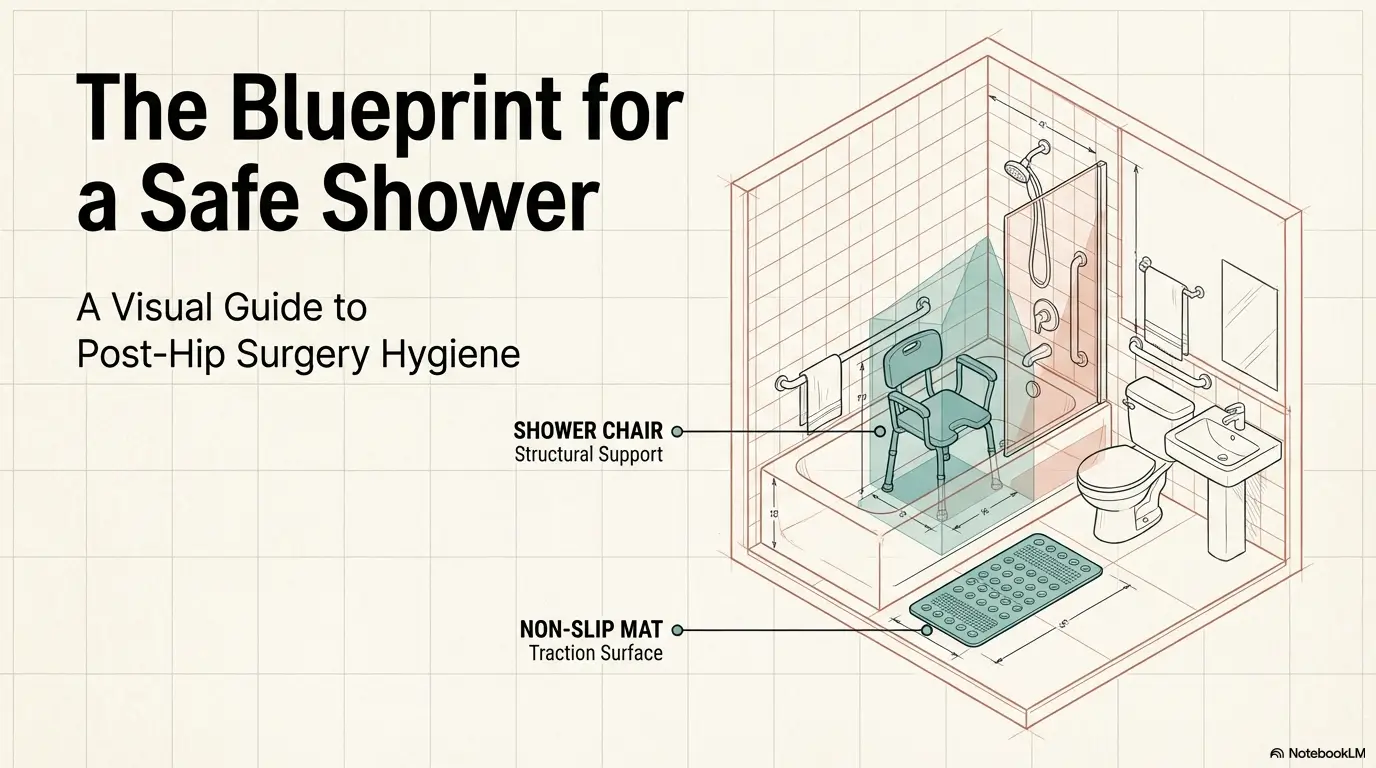
Infographic: the low-drama post-op shower zone
Walker parked safely, towel ready, clean clothes within reach, floor dry.
Grab bar or stable support, slow step or bench transfer, no twisting rush.
Chair or bench centered, handheld showerhead, soap and shampoo at easy height.
Pause before standing, dry stable surface, towel first, then clothing seated if possible.
Entry and Exit Are the Real Risk Zone
How getting in and out of the shower becomes the make-or-break moment
Many people assume danger lives in the middle of the shower. Often it lives at the edges. Entering and exiting combine balance, stepping, turning, and confidence when the floor is dry on one side and wet on the other. This is where one rushed motion can spoil an otherwise careful routine.
Safer sequencing for stepping, turning, and sitting without sudden hip strain
Use the same sequence every time. Stop at the threshold. Make sure the assistive device is positioned where it will be useful after the shower, not abandoned three feet away like a forgotten side character. If using a tub transfer bench, sit first and move across in a controlled way rather than performing a heroic sideways swing. If using a shower chair, enter, turn carefully as instructed by your therapy team, and sit before fatigue starts bargaining with your judgment.
The tiny rushed move that can undo an otherwise careful routine
It is often the reach. Reaching for the towel, reaching for shampoo, reaching for the faucet, reaching for a dropped washcloth. The body leans before the brain fully objects. Recovery hates the phrase “I’ll just.” I’ll just lean. I’ll just twist. I’ll just grab that. No. That phrase has sequel energy.
Short Story: A few years ago, a relative recovering from joint surgery told me her first shower “went fine,” which sounded reassuring until the next sentence. She had nearly slipped reaching for a towel that was hanging too far away, then caught herself with a painful jolt and said nothing because she did not want to alarm anyone. What stayed with me was not the near-fall itself. It was how small the original mistake was.
The shower chair was in place. The water temperature was fine. She had even timed her medication well. The problem was a towel hook placed six inches too far into the kingdom of bad ideas. After that, we staged the room like a tiny theater set. Towel here. Soap here. Walker here. Dry mat here. The next shower was not heroic. It was uneventful. Which, in recovery, is practically poetry.
- Practice the order before the water is on
- Place the towel and walker where they will be needed next
- Never reach for dropped items on autopilot
Apply in 60 seconds: Stand in the bathroom right now and move the towel to the exact place you can reach safely after the shower.
Don’t Do This: Common Shower Habits That Increase Pain and Fall Risk
Reaching, twisting, and balancing on one leg when you are already fatigued
Pre-surgery habits have muscle memory. That is why people keep trying to shave a leg standing up, step around clutter, or pivot casually with wet feet even when their current body has filed an official complaint. Recovery is not offended by your old habits. It just declines to support them.
Showering too soon after waking, too late in the day, or before pain medicine has kicked in
Right after waking, stiffness may be worst. Too late in the day, fatigue may be worst. And if medication timing is poor, both pain and guarding may climb at once. A little planning here can save a lot of swearing later. Quiet swearing counts. The hip still hears it.
Why “I’ll just do it quickly” is one of the most expensive thoughts in recovery
Rushing causes sloppy transfers, poor footing, skipped equipment, and bad incision decisions. A fast shower is not automatically a safe shower. A well-sequenced 7-minute shower often beats a chaotic 3-minute one. Speed should be the result of confidence and system design, not the substitute for them.
Mini calculator: shower stress score
Add 1 point for each “yes.”
- Did you sleep poorly last night?
- Are you more sore than usual today?
- Are you planning to shower without a seat even though standing still is tiring?
0 to 1 points: Your usual plan may be fine if surgeon-approved.
2 to 3 points: Scale down the shower, use more support, or wait for a better window.
Neutral next step: Use the score to reduce demand, not to prove toughness.
Common Mistakes
Mistaking independence for readiness
Being able to do something once is not the same as being ready to do it reliably. The first successful shower proves only that one shower succeeded under one set of conditions. It does not mean all future showers are cleared for improvisation.
Using unstable furniture instead of proper bath equipment
A dining chair near a wet bathroom is not a shower chair. A towel rack is not a grab bar. A plastic stool of mysterious internet origin is not a tub bench. The room may look calm, but poor equipment turns calm into comedy with a very bad ending.
Letting the bathroom become slippery, cluttered, or improvisational
Extra rugs, trailing cords, damp floors, narrow pathways, and toiletries scattered at floor level create problems before the first drop of water hits the tile. CDC fall-prevention guidance for older adults emphasizes reducing tripping hazards, improving lighting, adding grab bars, and using non-slip surfaces. Those are plain interventions because plain interventions work. The same principle carries into other painful home chores too, like setting up bathroom cleaning in a more back-friendly, low-risk way, where the room itself can quietly become the problem.
Treating the first successful shower like proof that every shower will go the same way
Recovery fluctuates. Sleep, swelling, bowel issues, appetite, medication timing, and physical therapy all influence how the body behaves on a given day. Some mornings your hip will cooperate like a professional. Some mornings it will act like it did not read the memo. Build for variability.
Support tier map: what changes from Tier 1 to Tier 5
| Tier | What it looks like | Why it matters |
|---|---|---|
| 1 | Dry run only | Build sequence without water risk |
| 2 | Helper nearby, no hands-on help | Confidence plus quick backup |
| 3 | Standby assist with cueing | Useful during early transfers |
| 4 | Hands-on transfer help | Needed when balance is still limited |
| 5 | Pause shower plan, call team | For dizziness, wound issues, severe pain, or unsafe transfers |
Neutral next step: Choose the lowest tier that is actually safe, not the tier that flatters your ego.
Pain Control During the Shower: What Actually Helps
Medication timing, water temperature, pacing, and seated strategies
Pain control during a post-op shower is rarely one magic trick. It is a bundle of small advantages. Take medication only as directed by your care team and allow time for it to work if that has been part of your routine. Keep the water warm, not punishingly hot. Sit when standing adds needless strain. Pause between tasks. Wash what matters most first. The hip does not award medals for shampoo commercial stamina.
Why shorter showers are often smarter than braver showers
A shorter shower lowers time spent standing, turning, and concentrating in a wet environment. This is especially useful in the first days or weeks after surgery. Think efficient, not sloppy. Clean the important zones, protect the incision according to instructions, and get out before fatigue turns your thinking grainy.
Comfort measures that reduce strain without pretending pain should be ignored
Use a long-handled sponge if bending is limited. Sit for drying and dressing if allowed. Keep a robe or towel within easy reach. Some people also find it easier to split the full task into phases: shower now, rest, then dress. That may sound almost comically modest compared with your former adult life, but temporary modesty is cheaper than a fall.
In a practical sense, pain management here is not about eliminating every ache. It is about keeping discomfort inside a manageable range so that movement quality stays decent and decisions stay sane. If readers are looking for a wider framework beyond this one task, a broader overview of orthopedic pain management for older adults can help connect bathroom safety with the rest of daily function.
Caregiver Help Without Taking Over the Whole Scene
What kind of help preserves dignity and still improves safety
Good help reduces risk without turning the patient into luggage. The best caregivers often do the invisible work first: laying out supplies, drying the floor, steadying the bench, staying nearby, and helping only where the risk actually rises. Dignity survives much better when assistance is specific instead of theatrical.
Cueing, guarding, and standby assistance: where support is useful
Sometimes the most useful help is verbal. “Pause first.” “Reach left, not down.” “Sit before washing your legs.” That sort of cueing can interrupt bad habits without making the patient feel helpless. Standby assistance can also be enough for early showers, especially when the person is cleared to shower but still wobbly or anxious.
Let’s be honest… too much help can create a different problem
When caregivers do everything, patients may stop practicing safe independence. Then the first solo attempt happens later, when everyone is overconfident. That is not ideal. The aim is graduated help. Enough support to stay safe. Enough space to learn the routine. It is a dance, though a rather unglamorous one involving towels, plastic benches, and earnest discussions about where the shampoo should live.
- Set up the room before the shower
- Give cues before giving hands-on help
- Scale help down as safety improves
Apply in 60 seconds: Decide in advance which part of the shower your helper will assist with so nobody improvises in the riskiest moment.
Red Flags That Change the Plan
When pain is no longer “expected soreness”
Some soreness after activity can be expected in recovery. But sharp worsening pain, new inability to bear weight if that is a change, sudden mechanical pain, or pain that feels dramatically different from your recent pattern deserves attention. Do not let the sentence “I probably just overdid it” become a blanket over everything.
Signs of wound trouble, dizziness, instability, or swelling you should not normalize
Worsening redness, unusual warmth, drainage, foul odor, fever, or an incision that looks increasingly angry rather than gradually calmer should move you out of DIY mode and into call-the-team mode. So should faintness, near-falls, or sudden swelling. If the shower routine starts to feel less safe instead of more routine, that is data.
When to stop the shower routine and call the surgical team
Stop if you are unsure whether the wound can get wet, if pain suddenly spikes, if you feel unstable, or if you cannot complete transfers safely. Recovery plans are allowed to change. A paused shower is not failure. It is sometimes exactly what competence looks like.
When to Seek Help
Call your surgeon or care team if
- You are unclear whether showering is allowed yet
- Your pain is worsening instead of gradually easing
- The incision shows drainage, spreading redness, or unusual warmth
- You feel newly unsteady, faint, or unable to manage transfers safely
Seek urgent care right away for
- Chest pain or trouble breathing
- Sudden severe calf swelling or pain
- A fall with possible injury
- Fever with concerning wound changes
- Sudden severe hip pain, deformity, or inability to bear weight if that is a new change
This part is intentionally plain. No lyrical flourish is worth muddying an emergency threshold. If you think, “This feels wrong in a way that scares me,” that is a legitimate piece of clinical information. Respect it.
MedlinePlus also suggests asking your doctor specific aftercare questions, including when you can shower and what wound problems to watch for. That small act of asking may prevent a surprisingly large amount of uncertainty. Many people do not need more courage at this stage. They need fewer unanswered questions.
Build a Repeatable Bathroom Routine, Not a Daily Gamble
Why recovery gets easier when the sequence stays boring
Boring is beautiful in recovery. The same towel spot, the same bench position, the same order of movements, the same timing window, the same supplies within reach. Repetition lowers stress because the brain does not need to invent a plan in a wet room while the hip is muttering complaints.
A simple shower checklist that lowers stress before it lowers pain
- Confirm showering is allowed today
- Take medication only as directed, with enough lead time if prescribed
- Set out towel, clothes, walker, toiletries, and dressing supplies
- Check floor traction and seat stability
- Keep the shower short and the sequence familiar
- Sit for part or all of the shower if that improves safety
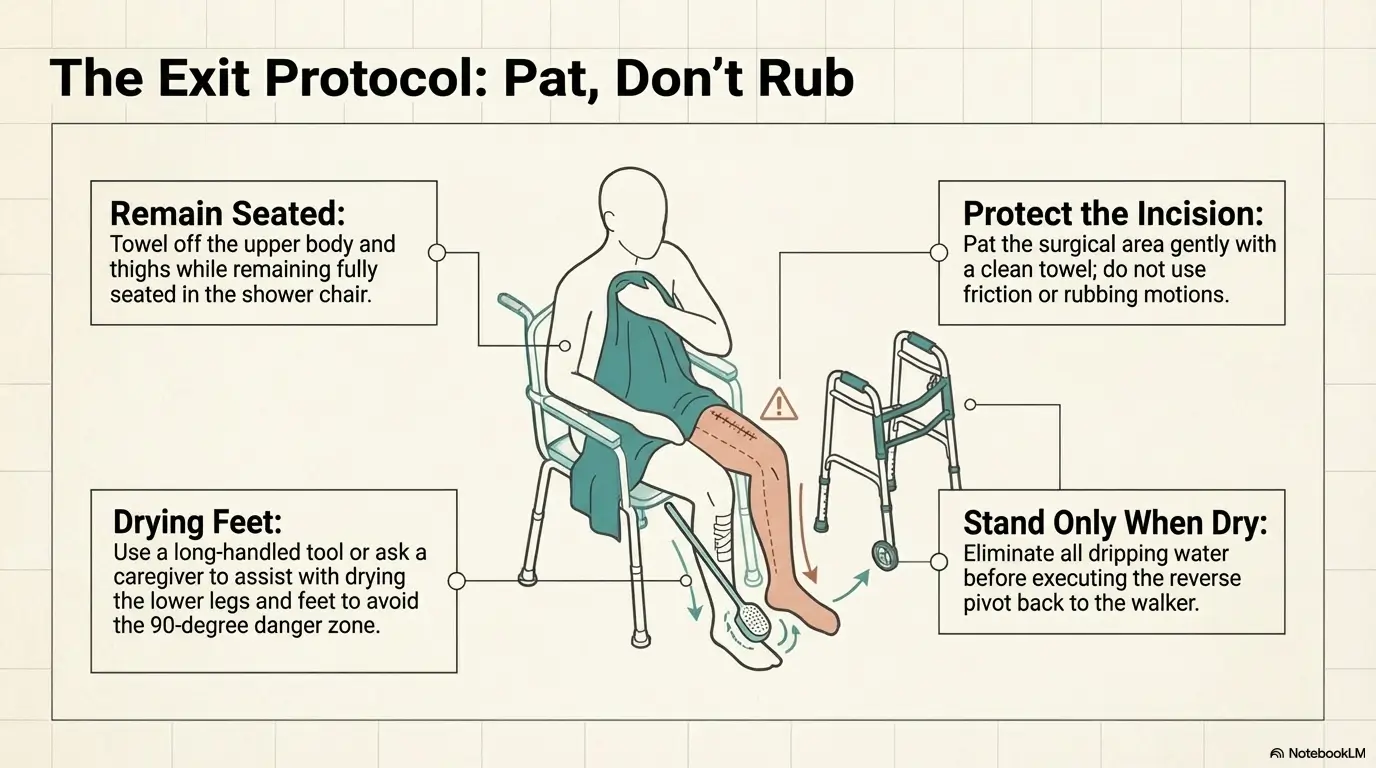
- Pat the incision dry exactly as instructed by your care team
The goal is not confidence theater. It is predictable safety.
Confidence matters, but dependable sequence matters more. The hook from the start of this article was simple: the bathroom can feel like a small unwanted exam. The way out is not to ace it with flair. It is to redesign the exam until it becomes a routine. The real victory is not a dramatic “I did it alone.” It is a string of uneventful, safe showers that let healing continue without interruption.
- Repeat the same setup
- Reduce reaching and last-minute decisions
- Let safety, not pride, choose the method
Apply in 60 seconds: Make a three-line shower script on paper: “Set up. Sit early. Exit slowly.” Tape it where you will see it.
FAQ
When can you shower after hip surgery?
That depends on your surgeon’s protocol, dressing type, and wound instructions. MedlinePlus notes that some patients are told not to shower until 3 to 4 days after surgery or until their surgeon says it is okay. Follow your discharge instructions, not a generic timeline from the internet.
How do you shower after hip replacement without bending too much?
Use a shower chair or bench if recommended, keep soap and towels within easy reach, consider a handheld showerhead, and avoid reaching to the floor or twisting suddenly. Long-handled tools can also help reduce bending if your care team has cleared them.
Should you use a shower chair after hip surgery?
Many people benefit from one, especially early in recovery or if standing tolerance is limited. A shower chair helps inside a walk-in shower, while a tub transfer bench is often better for getting over a tub wall. The right choice depends on your bathroom layout and transfer ability.
Is it normal to have more pain after showering?
Mild soreness or fatigue can happen because showering combines standing, stepping, and balance work. But worsening pain, sharp new pain, or pain paired with instability, swelling, or wound concerns should not be brushed off as “normal.”
Can warm water help hip pain after surgery?
Warm water may make muscles feel less guarded and can be more comfortable than cold water. But comfort does not override wound rules, and very hot water may increase fatigue or dizziness for some people. Keep the shower comfortable, not extreme.
What should you do if you feel dizzy in the shower after hip surgery?
Stop immediately, sit if it is safe to do so, and get help. Do not try to “finish quickly.” Dizziness can raise fall risk fast. If it is new, significant, or recurrent, contact your care team promptly.
Do you need grab bars after hip surgery, or is a walker enough?
A walker helps you get to the bathroom, but it is not a substitute for secure support inside a wet shower area. Properly installed grab bars can make transfers safer. The two tools solve different problems.
How long should a shower be after hip surgery?
As short as practical while still getting clean and following wound instructions. Early on, a shorter shower is often wiser than a long one because it reduces time spent standing, balancing, and getting fatigued.
Next Step
Do one bathroom safety rehearsal today
Before the next real shower, do a dry run with no water: place supplies within reach, test entry and exit, confirm seating height, check floor traction, and time pain medication only as directed by your care team. Recovery often improves when the bathroom stops being a place of improvisation and becomes a place of sequence.
Inside the next 15 minutes, you can make this meaningfully safer. Move the towel. Place the chair. Clear the floor. Decide whether someone should be nearby. Write down the incision rule you must not break. That small rehearsal may do more for your next shower than a hundred pep talks. And if the bigger picture right now is simply getting through recovery with less depletion, the same function-first mindset appears in this guide on managing the wait for joint replacement without arriving at surgery more worn down.
Last reviewed: 2026-03.
