
Is It a Steroid Flare or Something More?
By tonight, the numbing medicine can clock out, and the injection site can clock in loud, hot, and strangely persuasive. A steroid flare after injection can feel like your body filed a complaint in ALL CAPS, right when you’re trying to sleep.
What makes it scary is the uncertainty: is this normal post-injection soreness, or the start of something you shouldn’t sit on? If you keep guessing, you risk the two worst outcomes: delaying care you actually need, or panic-cycling yourself into a sleepless, symptom-Googled spiral.
A steroid flare is a short-term spike in pain, warmth, and soreness near the injection site, often starting within hours and usually settling over 1–3 days. It’s commonly irritation from steroid crystals, not infection.
Our approach focuses on: Temperature + Skin Check + Trend.
- ✔ Read this next if you want calm, not chaos.
- ✔ If you want clear thresholds, not vibes.
- ✔ If you want words for the clinic, not a freestyle performance.
Inside: A simple timeline, flare vs. infection vs. allergy grid, and a 60-second call script that gets you an answer fast.
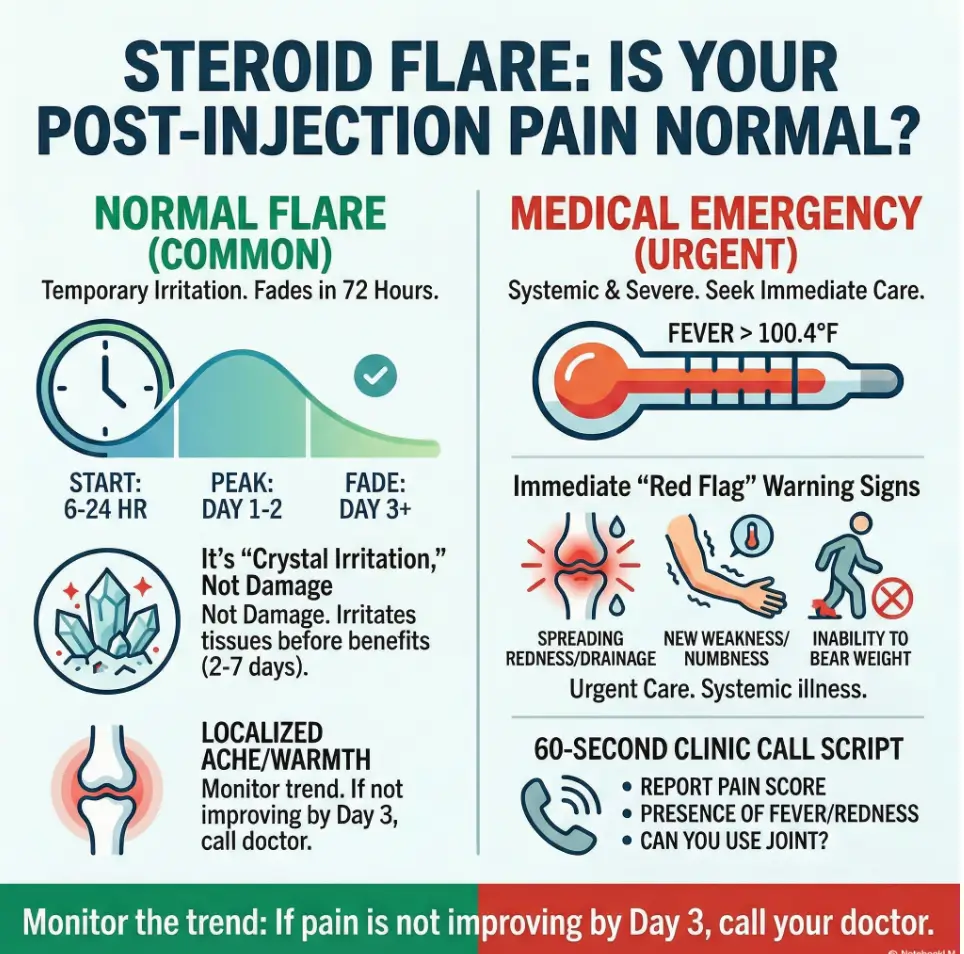
A steroid flare after injection is a short-lived spike in pain, warmth, and soreness near the injection site that can start within hours and last 1–3 days (sometimes a bit longer). It’s usually caused by irritation from steroid crystals, not infection. Use your clinician’s aftercare plan, protect the joint, and track symptoms. Call your doctor if pain is worsening after 48–72 hours, you develop fever, spreading redness, drainage, or can’t bear weight.
Table of Contents
Safety / Disclaimer (Read This First)
This is educational, not medical advice. Injection reactions vary by body area (knee, shoulder, spine, hip, hand), medication, technique, and your medical history. If you’re unsure, the safest move is simple: call your clinic. If you have severe symptoms (high fever, rapidly spreading redness, shortness of breath, new weakness/numbness, loss of bladder/bowel control, or signs of anaphylaxis like facial swelling or throat tightness), seek urgent/emergency care.
- Timeline matters: flare usually peaks day 1–2 and starts fading by 48–72 hours.
- Systemic illness is a warning: fever/chills plus worsening pain is not “just soreness.”
- Neuro symptoms after spine procedures deserve urgent attention (see cauda equina syndrome red flags).
Apply in 60 seconds: Take your temperature, look at the skin, and write down “trend: better/same/worse.”
Who this is for / not for
Who this is for
- People who had a cortisone/steroid injection (joint, bursa, tendon sheath, epidural, facet) and now have more pain than expected
- Anyone trying to tell “normal flare” vs “something’s wrong” without spiraling (if doom-scrolling is the problem, read cyberchondria and chronic pain)
- Patients with diabetes watching for blood sugar changes
Who this is not for
- Anyone with severe allergic symptoms (hives, facial swelling, wheezing, throat tightness)
- Anyone with red-flag neuro symptoms after spine injections (new weakness, numbness in groin/saddle area, bowel/bladder changes)
- Anyone with rapidly spreading redness, high fever, drainage, or feeling very ill
Quick personal note: I’ve watched smart, tough people get knocked flat by a post-procedure pain spike, then feel embarrassed for being worried. Don’t do that part. Concern is a feature, not a glitch.

Steroid flare: the “signature feeling” to expect
What it typically feels like (the common script)
- Local ache or deep soreness
- A warmth/pressure sensation around the injection area
- Pain that feels “sharper” when you move the joint or load it
One reason flares spook people: the pain can feel strangely “pure.” Like the injection turned the volume knob up and snapped it off. I once had a minor procedure where the discomfort waited politely until evening, then arrived like a late-night drummer practicing rudiments in my knee. Loud. Annoying. Not dangerous. But wow, persuasive.
Timeline tells a story (and it matters)
- Onset: often within 6–24 hours (many people notice it as numbing medicine wears off)
- Peak: usually day 1–2
- Fade: commonly by 48–72 hours (for a bigger picture, compare to the epidural steroid injection relief timeline)
Major medical organizations describe a short-term pain flare after cortisone shots that typically settles within a couple of days. That’s the “normal loud.” Your job is noticing whether you’re trending quieter over time.
Where it shows up differs by injection site
- Knee/shoulder/hip: movement and weight-bearing amplify soreness
- Hand/wrist/finger: tight “throbbing” in a small space (it can feel extra dramatic)
- Spine/epidural/facet: soreness at injection site, sometimes temporary symptom change (if the pain source is unclear, see hip vs spine pain)
Show me the nerdy details
Many injectable steroids are suspensions, meaning tiny crystals sit in fluid rather than fully dissolving. In some tissues, those particles can temporarily irritate local structures before the anti-inflammatory effect dominates. Add in “mechanical poke + already-inflamed area,” and you get a pain spike that feels personal, even when it’s not.
Why it happens (and why it’s usually not “damage”)
The crystal irritation explanation (plain English)
Some steroids are made as tiny particles (crystals) suspended in liquid. For a short window, those particles can irritate local tissues. Think: brief chemical sand-in-the-shoe feeling, not “the joint is being destroyed.” It’s rude, not ruinous.
Inflammation math: the short spike before the drop
Your body can respond to the needle, the fluid volume, and the irritated tissue with a temporary inflammatory response. Meanwhile, the steroid’s anti-inflammatory effect often takes a few days to show up, especially for spine-related injections. That gap is where anxiety grows legs and starts pacing.
Here’s what no one tells you…
A flare can feel dramatic even when it’s benign because the area was already sensitized and then mechanically poked. Pain systems are protective and sometimes… theatrical. They’d rather be wrong and loud than right and quiet.
- The steroid’s benefit can lag by 2–7 days depending on the site and condition.
- Early pain can reflect local irritation, not treatment failure.
- Trend beats intensity: better over time is reassuring (and if imaging is freaking you out, read MRI pain mismatch).
Apply in 60 seconds: Ask yourself: “Am I 5% better than yesterday?” If yes, you’re likely on the right track.
Flare vs infection vs allergy: the quick triage grid
This is the part people want: the mental flowchart. It won’t replace clinical judgment, but it can stop the doom-scrolling loop.
Next step: Follow aftercare + log symptoms for 24 hours.
Next step: Call with specifics using the script below.
Next step: Contact clinic today for instructions.
Next step: Seek urgent evaluation.
Next step: Emergency care now.
Neutral action: Choose the highest tier that matches your symptoms and follow the next step.
Flare is more likely when…
- Pain is localized near the injection area
- It starts within hours and peaks day 1–2
- You have no fever and you don’t feel systemically ill
- Redness (if any) is small and not expanding
Infection is more likely when…
- Fever or chills
- Spreading redness or warmth that expands beyond the injection area
- Drainage, pus, or a rapidly enlarging swelling
- Pain is rapidly worsening, especially after the first day
Allergy is more likely when…
- Hives, widespread itching
- Lip/face swelling, wheezing, throat tightness
- Dizziness, fainting, or feeling like you can’t get air
Let’s be honest…
If you’re sitting there thinking, “This feels wrong,” your safest move is not more Googling. It’s a quick call with specifics. Clinics are used to this question. You’re not the first person to call about a joint that suddenly decided to become a drama critic.
A friend once texted me at 11:43 p.m.: “I think my knee hates me.” She’d had a steroid injection that afternoon and felt fine until the numbing wore off. Then the ache showed up with a megaphone. She did what all of us do when we’re tired and scared: she started comparing symptoms to strangers on the internet. The next morning, she had a small warm patch near the injection site, pain with stairs, no fever, and she could still walk. We made a pact: two things first, always, before the spiral.
Temperature check and trend check. By late afternoon she was a little better. By day three, she was annoyed but functional. The story’s boring ending was the point: loud doesn’t always mean dangerous. But the temperature + trend ritual kept her from guessing in the dark.
When to call your doctor (and when to go now)
Call same day or within 24 hours if:
- Pain is severe and not improving with the agreed plan
- You can’t use the limb/joint or pain is escalating fast
- You have diabetes and see unexpected high glucose that’s hard to control
Call urgently (or go to urgent care/ER) if:
- Fever (especially with joint pain), chills, feeling very unwell
- Spreading redness or warmth expanding beyond the injection area
- Drainage, pus, or a rapidly enlarging swelling
- New weakness/numbness after spine procedures, severe headache after epidural (especially positional), or bowel/bladder changes (if you’re unsure what counts, read low back pain emergency)
- Any anaphylaxis warning signs
A reputable orthopedic source will tell you the risk of infection from a steroid injection is small but real, and that a joint infection can be serious. That’s why we treat fever + worsening joint pain like a fire alarm, not a “wait and see.”
This does not diagnose anything. It’s a structured way to decide whether you should call the clinic now versus monitor with a symptom log.
Enter your details, then click “Run check.”
Neutral action: Use the output to decide whether to call, then read your symptom log verbatim.
What to do in the first 24–72 hours (without making it worse)
Protect the area (the “quiet joint” approach)
Reduce load and avoid provocative movements for 24–48 hours (or per clinic instructions). This is the moment to be boring on purpose. I know the temptation: “It feels okay, I’ll just test it.” That’s how flares become extended editions.
Cold vs heat: choose the right tool
- Ice can help early soreness and reduce that “hot pressure” feeling.
- Heat may help later stiffness for some people, but follow clinician guidance, especially if there’s swelling (and if “heat at night” is your question, compare sleep with a heating pad for sciatica for safety-style thinking).
Medication do’s and don’ts (follow your discharge sheet)
Use only what your clinician approved, especially if you’re on blood thinners or you have kidney/GI risks. If you’re tempted to stack NSAIDs like you’re building a pain-fighting sandwich, pause. More isn’t always safer. It’s just… more.
Show me the nerdy details
Pain perception is amplified by uncertainty. A structured plan reduces threat prediction, which can lower perceived pain intensity even before medication changes. That’s why “quiet joint + log + check-in thresholds” often works better than improvising new remedies hourly.
Common mistakes that turn a flare into a longer story
Mistake #1: “Testing it” every hour
Repeated stress can keep tissues irritated and delay improvement. If you keep doing the exact motion that makes you wince, your body doesn’t get the memo that it’s safe to calm down.
Mistake #2: Ignoring infection clues because “flare is normal”
A true flare tends to plateau, then improve. Infection tends to worsen, often with expanding warmth/redness and systemic symptoms. The difference is not perfect, but the trend is meaningful.
Mistake #3: Doubling meds without a plan
Mixing meds improperly can cause harm. If you need stronger pain control than expected, that’s information your clinician should hear, not a puzzle you solve alone at midnight.
- Pick one safe plan and run it for a full day.
- Track trend, not moment-to-moment spikes.
- Escalate appropriately if you hit red flags (and if you’re stuck trying to label pain, see nerve pain vs muscle soreness after physical therapy).
Apply in 60 seconds: Set a 6-hour check-in alarm instead of re-evaluating every 20 minutes.
Don’t do this: two high-cost moves to avoid
Don’t soak/steam/immerse too soon if told not to
Hot tubs and pools can increase risk depending on wound care instructions. If you were told to keep the site clean/dry for a period, treat that like a seatbelt: mildly annoying, highly worth it.
Don’t treat new neuro symptoms like “just soreness” (spine injections)
New weakness, numbness, groin/saddle numbness, or bowel/bladder changes need urgent evaluation. Don’t negotiate with those symptoms. They don’t bargain.
- Starts within hours
- Localized soreness/warmth
- No fever, not ill
- Plateaus then improves by 48–72h
Time/cost trade-off: Rest now, faster recovery later.
- Fever/chills or very unwell
- Redness/warmth spreading
- Drainage/pus
- Rapid worsening pain
Time/cost trade-off: Earlier evaluation can prevent serious complications.
Neutral action: If you’re straddling the line, call the clinic and let them decide the next step.
Special populations: the flare can look different here
Diabetes: the blood sugar bump watch
Steroids can raise blood glucose for days. Some people see changes quickly; others notice it the next day. If you use insulin or have had trouble with control before, have a monitoring plan and a “when to call” threshold. The annoying truth: your joint may feel better while your glucose runs a temporary sprint.
- Yes/No: I use insulin or have a history of large glucose swings.
- Yes/No: My A1C has been above my target recently (or I’m unsure).
- Yes/No: I’ve had steroid-related glucose spikes before.
- Yes/No: I don’t have a clear plan for medication adjustments.
Neutral action: If you answered “Yes” to any item, consider messaging/calling your diabetes care team for a temporary plan.
Immunosuppressed or high infection risk
If you’re immunosuppressed or have higher infection risk, keep a lower threshold for calling about fever, spreading redness, or “I feel off.” This is not the moment for heroic waiting. It’s the moment for professional reassurance or prompt care.
Anticoagulants/blood thinners
Know the hematoma warning signs your clinician mentioned: expanding bruising, increasing swelling, worsening pain, or new neurologic symptoms after spine injections. If you were told to watch for something specific, treat that instruction like a personal map.
Show me the nerdy details
Steroids can influence glucose via increased insulin resistance and hepatic glucose production. The magnitude and duration vary with dose, type, and route. That’s why some people see a 24–48 hour bump while others notice a longer ripple, especially if baseline control is already tight-rope walking.
The 60-second call script (so you get a clear answer fast)
What to say to triage
- “I had a steroid injection in my ___ on (date/time).”
- “Pain started at ___ hours after. It’s now ___ /10.”
- “Redness is (none/localized/spreading). Fever: (yes/no, temp).”
- “I can/can’t bear weight / use the arm.”
- “Any drainage? Any numbness/weakness? Any rash or swelling elsewhere?”
What to ask
- “Does this fit a typical steroid flare timeline for this injection?”
- “What home care do you want me to follow and for how long?”
- “What would make you want to see me today?”
Tiny insider trick: lead with the “big three” first. Fever? Spreading redness? Function? (Can you bear weight/use the limb?) Those three answers often decide the next step faster than any adjective like “awful” or “weird.”

FAQ
1) How long does a steroid flare last after an injection?
Many flares peak in the first 24–48 hours and improve by 48–72 hours. Some people run longer, especially if they keep “testing” the joint, the area is small/tight (hand), or the underlying inflammation was already severe. If you’re worsening at 72 hours, call your clinic.
2) Can a steroid flare start the next day?
Yes. A very common pattern is: numbing medicine helps initially, you feel okay, then soreness ramps up later that day or the next morning. That “delayed punch” is one reason flares feel so alarming.
3) How do I know if it’s infection or just a flare?
No single sign is perfect, but the combination matters. Fever/chills, feeling very unwell, spreading redness/warmth, drainage, and rapidly worsening pain push concern higher. A flare is more often localized and improves over time. When in doubt, call with the script.
4) Is it normal for pain to be worse after a cortisone shot?
It can be. A temporary flare is a known short-term side effect described by major medical institutions. “Normal” here means time-limited and trending better. If it’s getting worse after 48–72 hours, you’re not obligated to tough it out.
5) What should I do at home for steroid flare pain?
Follow your discharge instructions first. Common basics include resting the area, using ice in the first day or two, and using only clinician-approved pain medication. Most importantly: stop “proving” you can do stairs. Let the area quiet down.
6) When should I call my doctor after a steroid injection?
Call the same day if pain is escalating fast, you can’t bear weight/use the limb, you have diabetes with hard-to-control glucose, or you’re simply unsure and anxious. Seek urgent care for fever, spreading redness, drainage, severe illness, or red-flag neurologic symptoms after spine procedures.
7) Can a cortisone shot cause fever?
Some people feel flushed or “off,” but a true fever plus worsening pain should be taken seriously because infection is the main concern. If you have a measured fever (especially 100.4°F / 38°C or higher) with increasing pain, call urgently.
8) Does a steroid injection raise blood sugar, and for how long?
It can. Many people with diabetes notice higher readings for a few days, sometimes longer. The duration varies by steroid type, dose, and your baseline control. If you’re seeing unexpectedly high numbers that don’t respond to your usual plan, call your diabetes clinician for a temporary adjustment strategy.
9) Can I exercise after a cortisone injection if it feels okay?
“Feels okay” is not always “is ready.” Many clinicians recommend a short rest window (often 24–48 hours) before returning to higher-load activity, depending on the injection site. If you exercise too early, you can keep the flare alive. If you’re unsure, ask for a clear return-to-activity plan.
10) Why didn’t my steroid injection help yet?
Steroids often take days to show meaningful benefit. Early pain can be flare, not failure. If you’re past a week with no improvement, or you’re worse with new concerning signs, check back with your clinician to reassess the diagnosis and next step options (if diagnostic confusion is part of your story, compare sciatica MRI vs X-ray and MRI pain mismatch thinking).
Next step (one concrete action)
Do this now
Open your phone notes and start a 3-line symptom log:
- Injection date/time + location
- Current pain score + trend (better/same/worse)
- Fever/redness/drainage: yes/no
If pain is worsening after 48–72 hours or you have any red flags, call your clinic and read the log verbatim. This is how you turn anxiety into usable information.
Conclusion
Remember the curiosity loop from the beginning: “Is this normal loud soreness, or is something wrong?” Now you have the answer pattern. A flare usually has a recognizable timeline and a “localized, trending-better” shape. Infection and allergic reactions announce themselves with different, higher-stakes signals. Your job isn’t to be perfect. Your job is to notice fever, spreading redness, drainage, loss of function, or new neurologic symptoms, and then call promptly.
Numbing wears off. Soreness may ramp up. Log symptoms and protect the area.
Flare often feels loudest here. Look for trend by the end of day 2.
Many flares start improving. If worsening or function is declining, call the clinic.
Fever/chills, spreading redness/warmth, drainage/pus, severe illness, anaphylaxis signs, or new weakness/numbness (especially after spine injection) → urgent evaluation.
If you have 15 minutes: do the symptom log, run the mini check tool, and make the call if you hit a red flag or you’re worsening at 72 hours. You’ll feel better the moment a clinician says, “Yes, that fits a flare” or “No, we want to see you today.” Either way, you’re back in the driver’s seat.
Last reviewed: 2026-02
