
The Reality of Day 1: Navigating the Post-Injection Flare
Day 1 can feel like a betrayal: you did the sensible, expensive, needle-in-your-spine thing… and your pain gets louder anyway. That’s why an epidural steroid injection relief timeline matters more than optimism or panic.
In the first 72 hours, soreness and a flare can mimic failure, especially with sciatica/radiculopathy where symptoms already travel like bad gossip from back to butt to leg. If you’re still unsure which nerve pattern you’re dealing with, a quick anatomy-based decoder like L4 vs L5 vs S1 sciatica patterns can help you describe your symptoms with less guesswork. Keep guessing and you risk two classic losses: either you overdo it on a “good” day and trigger a rebound, or you miss a true red flag because it looks like “normal pain.”
Here, you’ll learn what’s normal from Day 1 to Day 14 using a simple function-first log.
- ✔ Spot the “noise” window vs. the steroid ramp
- ✔ Track walking, sitting, and sleep like a clinician would
- ✔ Know exactly when to call, and what to say
No vibes. No doom-scrolling. Just a day-by-day map.
Table of Contents

Fast Answer (snippet-ready)
Safety / Disclaimer (read this once)
This guide is educational, not medical advice. Your exact timeline depends on your diagnosis (sciatica/radiculopathy vs spinal stenosis vs something else), injection level (cervical/thoracic/lumbar), technique (interlaminar, transforaminal, caudal), and medication mix (local anesthetic + steroid type/dose). If you’re not even sure whether the pain is coming from the hip joint or the spine, start with hip vs spine pain (how to tell) so you’re not tracking the wrong “story.”
If you have new leg weakness, numbness in the groin/saddle area, loss of bowel/bladder control, fever/chills, a severe positional headache (worse standing, better lying down), chest pain, trouble breathing, or rapidly worsening symptoms, seek urgent care or call your clinician’s on-call line. If you want a focused checklist specifically for the most time-sensitive “don’t wait” scenario, read cauda equina syndrome red flags.
- Expect soreness and sometimes a short flare.
- Judge the steroid by function around Days 7–14.
- If you’re suddenly weaker, febrile, or numb in the saddle area, don’t wait.
Apply in 60 seconds: Write down your injection date/time and your clinic’s after-hours number now, before you need it.
Quick eligibility checklist: “Can I watch-and-wait… or should I call now?”
Check “Yes” or “No.” If you hit any “Yes” in the red section, treat that as a call-now moment.
- Injection-site soreness/bruised feeling (Yes/No)
- Temporary pain flare without new weakness (Yes/No)
- Mild flushing/jitters/insomnia the first few days (Yes/No)
- New or worsening leg weakness (Yes/No)
- Fever/chills, spreading redness, drainage (Yes/No)
- Severe headache that is worse standing, better lying flat (Yes/No)
- New saddle/groin numbness or bowel/bladder changes (Yes/No)
- Chest tightness, trouble breathing, facial swelling (Yes/No)
Neutral next step: If you’re unsure, send a short portal message with your symptom timeline and ask, “Is this expected post-ESI?”
Day 1 reality check: “Why do I feel worse?”
Day 1 is the most unfair day. You did the brave, sensible thing, then your body responds by acting like it didn’t get the memo. I still remember sitting in my car after a procedure once, gripping a water bottle like it was a stability device, thinking, “Was that supposed to help… or audition for a horror movie?” That emotional whiplash is common.
Normal-ish sensations (that still feel alarming)
- Injection-site soreness: bruised feeling, tenderness, a “hot spot” where the needle went in.
- Heaviness or achiness along the usual pain path (back-to-butt-to-leg is a classic “greatest hits” route).
- Mild flush/jittery feeling or a slightly revved-up mood if steroid effects hit quickly.
- Temporary numbness if local anesthetic was used (it can feel like relief, or like your leg is “not fully yours”).
Post-injection flare: the pain spike nobody warns you about
A flare is basically your tissues saying, “Excuse me, what was that?” You had a needle in a crowded neighborhood of nerves, ligaments, and irritated structures. Even when everything goes smoothly, there can be temporary inflammation from mechanical irritation, plus the local anesthetic wearing off like a curtain dropping.
- What a flare is (plain English): short-term irritation that makes pain feel louder before it quiets.
- Typical duration: often 24–72 hours. Some people feel it fade faster; some feel “wobbly” for a few days.
- “Worse first” vs true deterioration: a flare hurts, but it usually doesn’t add new neurologic loss (like new weakness) or systemic illness signs (fever/chills). If you’re unsure whether you’re dealing with “nerve pain” vs plain muscular soreness, use nerve pain vs muscle soreness (what it feels like) as a reality check.
Micro-check: Rate it, don’t narrate it
Your brain wants a novel. Give it a spreadsheet. Rate pain 0–10 and track can you walk / sleep / sit. That’s the signal. The rest is plot. (And if you catch yourself spiraling into symptom-googling at 2 AM, cyberchondria with chronic pain is the gentle slap you’ll thank later.)
- Pain now (0–10): ____
- Walking minutes total today: ____
- Best position (sitting/standing/lying): ____
- One task I could/couldn’t do: ____
Show me the nerdy details
Many clinicians describe a “local anesthetic phase” (hours) followed by an “irritation phase” (1–3 days) before steroid anti-inflammatory effects ramp. That’s why early pain can be a poor predictor of the Day 7–14 outcome.
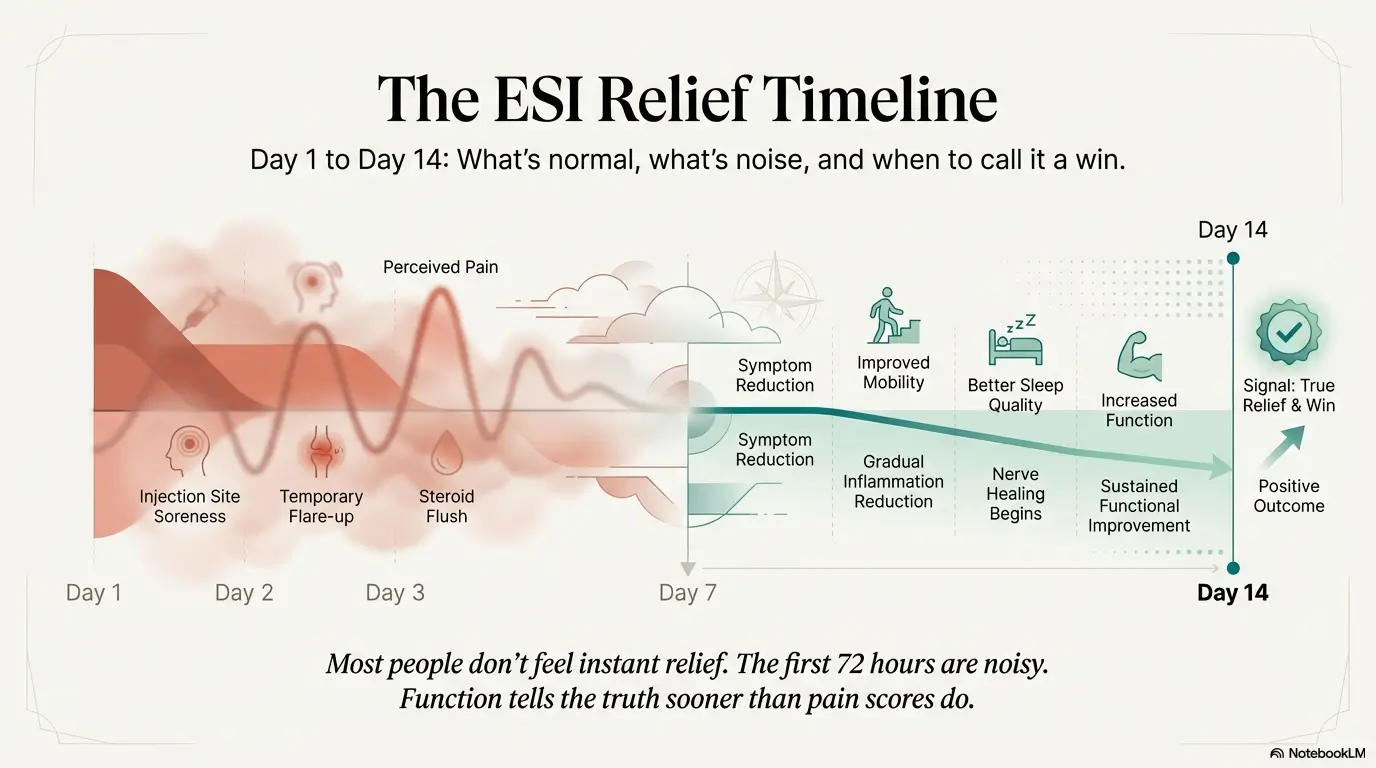
Day 2–3: the inflammation hangover window
If Day 1 is the jump-scare, Day 2–3 is the hangover: you’re functional-ish, but everything feels tender and your sleep might be weird. I’ve watched more than one friend text, “I was amazing yesterday and now I’m worse,” like their body is violating a contract. That pattern can be normal.
What’s normal in this pocket of time
- Residual numbness or heaviness (especially if local anesthetic lingered or you guarded your movement).
- Stiffness and tenderness in the low back or buttock.
- Sleep disruption: steroid + stress + “I keep checking if it hurts” is a rude combination. If nights are your worst enemy, it may help to compare side sleeping with sciatica at night strategies, then fold them into a broader plan like how to sleep with sciatica.
- Appetite changes or feeling a little wired (some people get the opposite: a mini-crash).
Here’s what no one tells you: relief can be uneven
Bodies don’t “improve” in a neat line. It can feel lopsided and confusing, like your pain is negotiating separate treaties.
- Leg pain improves, back pain lags (or vice versa).
- One side calms down first, especially if one nerve root was more irritated.
- Function changes before pain scores: you walk longer, but the pain number hasn’t gotten the memo yet.
The red-flag split: discomfort vs danger
This is where people get stuck: “It hurts” feels scary, and it is unpleasant, but danger is usually signaled by new weakness, fever, severe positional headache, or bowel/bladder changes. Pain alone can be loud without being emergent. If you want a broader “when is back pain an emergency?” map (beyond injections), bookmark low back pain emergency: when to go in.
Decision card: When to watch vs when to call (Days 1–3)
- Soreness at the injection site
- Flare pain that slowly settles
- Sleep jitters/flush without fever
Time/cost trade-off: You save an urgent visit, but you commit to tracking function daily.
- New weakness (foot drop, knee buckling, can’t toe-raise)
- Fever/chills, spreading redness, drainage
- Severe positional headache
- Saddle/groin numbness or bowel/bladder changes
Time/cost trade-off: More hassle now, but you reduce risk if something rare is brewing.
Neutral next step: If it’s “watch,” schedule a check-in time each evening to log, then stop symptom-hunting.
Day 4–7: “Is it starting to work… or am I imagining it?”
This window is where hope tiptoes in wearing socks, trying not to wake the anxiety. Many clinicians describe steroid benefit beginning around 3–7 days for some patients, but it can be subtle. Not fireworks. More like someone turned the volume down a notch.
The steroid ramp: what “kicking in” often looks like
- Shorter morning pain window (you stand up and it’s not instantly a crime scene). If mornings are uniquely sharp, compare with morning sciatica nerve glides so you’re not doing the wrong “stretch” at the wrong time.
- Less burning/shooting intensity, even if ache remains.
- Longer sitting/walking tolerance before symptoms shout. If walking is your main trigger, this can help you interpret patterns: sciatica pain when walking.
- Fewer “electric” surprises when you change positions.
Curiosity gap: Why your pain map may change
Nerves calm in layers. As inflammation reduces, you might notice your pain “moves” or becomes more localized. That can be a normal part of a nerve settling down. What matters is whether the changes come with new neurologic deficits (weakness, saddle numbness) or systemic symptoms (fever). If your imaging “sounds scary” but your symptoms don’t line up, the mismatch is common enough to deserve its own explanation: when MRI findings don’t match pain.
- Centralization (often reassuring): pain retreats from the foot/calf toward the buttock/back while function improves.
- New symptoms (more concerning): new weakness, new saddle numbness, or worsening numbness that changes what you can do.
Let’s be honest: you want a date on the calendar
Clinicians often say “give it a week” because it’s a practical checkpoint, not because your body is a punctual employee. Some people improve by Day 4. Some need the full 10–14 days to show a clear difference. If you’re at Day 6 and unsure, you’re not failing. You’re simply in the foggy part of the map.
- Measure walking/sitting time, not just intensity.
- Expect uneven improvement.
- New weakness or fever isn’t part of “ramp-up.”
Apply in 60 seconds: Pick one daily benchmark (e.g., “walk to the mailbox”) and time it.
Day 7–10: the first honest verdict window
This is the window many people secretly crave: the moment you can stop interpreting tea leaves and start reading outcomes. I once marked Day 8 on my phone as “truth day” after a different procedure, and the funny thing is it helped, not because it changed biology, but because it gave my brain a railing to hold onto.
The “function-first” scorecard (more reliable than pain alone)
Pain ratings are real, but they’re mood-sensitive. Function is harder to fake. Try this scorecard for Days 7–10:
- Walking time: ____ minutes before symptoms force a stop
- Sleep quality: ____ hours, and how many wake-ups
- Sitting tolerance: ____ minutes before you have to change position (desk workers often benefit from a sit-stand schedule for sciatica instead of “powering through”).
- Rescue meds: fewer / same / more (note what changed)
- Work/ADLs: one thing you can do again (or still can’t)
Curiosity gap: If it worked, how long will it last?
Durability ranges widely because the injection targets inflammation, not the entire cause (disc herniation size, stenosis mechanics, degenerative changes, posture/strength patterns). Many major medical institutions describe ESI as a tool for reducing pain to help people participate in rehab and daily life, and for some it’s short-term, for others it buys meaningful time. The only honest promise is this: your response teaches your care team something useful. If the next step is rehab, a grounded overview like physical therapy for sciatica (what actually helps) makes it easier to spend your “lower-pain window” wisely.
The trap: over-testing your back “to see if it’s fixed”
When the pain quiets, your brain goes full celebratory raccoon: it wants to raid the whole pantry of activities in one night. That’s where people get the “one big day” hangover.
- Why it backfires: irritated nerves dislike sudden spikes in load and bending/twisting.
- How to test safely: increase one variable at a time (longer walk OR longer sit, not both).
- Rule of thumb: if tomorrow is worse by 2+ points and function drops, scale back. If you’re tempted to “prove” recovery with stretching, make sure you can tell hamstring stretch sensations vs nerve pain so you’re not poking an angry nerve and calling it flexibility.
Mini calculator: “Is my function actually improving?”
Enter three numbers. This doesn’t diagnose anything. It simply turns fuzzy days into a clearer signal.
Neutral next step: If walking improves but pain doesn’t, tell your clinician: “Function is better even if pain is still present.”
Day 10–14: when to call it a win, a maybe, or a miss
By the end of two weeks, you usually have enough data to talk like an operator instead of a panicked detective. And yes, it’s emotionally annoying that the “verdict” takes this long. But if you can hold the timeline, it gives you clarity and leverage at follow-up.
Three outcomes that are all real
- Clear improvement: pain lower and function better in a way you can repeat most days.
- Partial improvement: fewer flares, longer walking tolerance, better sleep, but not fully “back.”
- Minimal change: pain/function look similar to baseline, beyond early flare noise.
Curiosity gap: What if relief is partial?
Partial doesn’t mean pointless. It can mean the inflammation component was real, but mechanics still need help. In US practice, clinicians may discuss a second injection depending on diagnosis, response, and safety factors. They may also pivot to PT (with better tolerance now), medication strategy, imaging review, or reassessment of whether the pain generator is truly the suspected nerve root. If you’re stuck at “Do I need more imaging?” the decision often starts with MRI vs X-ray for sciatica (what each shows).
When you describe partial relief, avoid vague words like “kinda.” Give specifics: “Walking improved from 5 minutes to 15. I sleep 6 hours instead of 3. The burning down the calf is less frequent, but sitting still triggers pain.”
The “don’t wait forever” line
If there’s no meaningful functional gain by about two weeks, that’s not a moral failure. It’s actionable information. Ask what the next hypothesis is: different level? different pain source? different plan? If your clinician brings up nerve testing, it helps to know when EMG is actually useful for sciatica. I’ve seen people lose months because they kept waiting for a magic day that never arrived.
- Clear win: better days become your new normal.
- Maybe: partial relief guides the next step.
- Miss: helps your clinician pivot faster.
Apply in 60 seconds: Write one sentence that begins, “Compared to before the injection, I can now…”
What’s normal vs not normal (symptom decoder)
Think of this as the translation key. Not everything uncomfortable is dangerous, but some rare complications deserve a fast response. Your job isn’t to diagnose. Your job is to recognize the difference between “annoying” and “urgent.” If you want a simple at-home provocation clue (not a diagnosis), you can learn the straight leg raise test at home so you can describe what you feel more precisely.
Normal-ish (common, usually self-limited)
- Local soreness, bruised feeling at the injection site
- Temporary pain flare for 1–3 days
- Mild flushing, jitteriness, insomnia, appetite changes
- A temporary “different” sensation as local anesthetic wears off
Not normal: urgent call-now signals
- New or worsening leg weakness (tripping, foot slapping, knee buckling)
- New numbness in saddle/groin area
- Fever/chills, drainage, redness spreading away from injection site
- Severe positional headache (worse standing, better lying down)
- Chest pain, trouble breathing, facial swelling (possible allergic reaction)
On Day 3, a caregiver I know did what most of us do: she turned her home into a diagnostic lab. She watched how her dad stood up from the couch, how he turned the corner into the hallway, how long he lasted before his face tightened. The pain number changed hourly, which made her panic hourly. Then she started timing one thing instead: the hallway lap.
Day 3 was two slow laps, one stop, a wince. Day 7 was four laps, one stop, less guarding. The pain rating still floated around the same number, like a stubborn balloon. But the hallway didn’t lie. When they messaged the clinic, they didn’t say “it’s weird.” They said: “Function improved from 2 to 4 laps, sleep went from 3 to 6 hours, no new weakness.” The reply came fast, calm, and useful. Data makes help easier to give.
Who this is for / not for
This is for
- Adults in the US who had an ESI for sciatica/radiculopathy/spinal stenosis
- Caregivers tracking symptoms and function
- People trying to decide when to message their clinician
This is not for
- Anyone with red-flag symptoms (skip to When to seek help)
- Post-op spine surgery patients unless your surgeon said this applies
- People seeking dosing advice or medication changes (clinician-only)
Common mistakes: the two-week timeline sabotage kit
Most “failed injections” don’t fail because the medicine is useless. They fail because expectations and behavior throw a wrench in the data. I say that with affection; I’ve been the person who tried to “prove I’m fine” too early, then spent the evening bargaining with a heating pad.
Mistake #1: judging success in the first 24 hours
Local anesthetic can create a false win on Day 1. When it wears off, pain returns and people think they’re worse. The steroid timeline is different. Give it the full window.
Mistake #2: doing a heroic workout on Day 3
“I felt better so I lifted” is a common spiral. Even if nerves are calming, tissues are still sensitive. Test gradually. If you’re returning to training, be extra careful with movements that spike load and hinge depth; this guide on deadlifting with sciatica shows how “one set to check” becomes a multi-day flare.
Mistake #3: stopping or doubling meds without a plan
Changing meds abruptly can create rebound symptoms, withdrawal, or unsafe combinations. If something feels off, call your clinician or pharmacist, especially if you’re mixing pain meds, muscle relaxants, and sleep aids.
Mistake #4: tracking pain but not function
Function is the north star. Pain is weather. Track both, but let function make the decision.
Mistake #5: waiting too long to report red flags
“Toughing it out” becomes risky when it involves weakness, fever, severe positional headache, or bowel/bladder changes.
Don’t do this: recovery behaviors that quietly prolong pain
These are the quiet saboteurs. They don’t feel dramatic in the moment, but they keep your nervous system on high alert.
Don’t: immobilize for days
Gentle movement can help circulation and reduce guarding. You’re not training for a marathon. You’re teaching your system: “We are safe to move.” A short walk every few hours is often more helpful than one long effort.
Don’t: “stretch into nerve pain”
Sharp, electric, radiating pain is not the stretch you “push through.” If your clinician or PT gave you nerve-friendly mobility, follow that plan. If not, keep movement gentle and avoid aggressive hamstring pulls that light up your leg. Also, if nerve flossing made things worse, that’s a known pattern; see when sciatic nerve flossing backfires so you can course-correct instead of doubling down.
Don’t: chase every twinge with Google
Set a 2-minute symptom log rule. Log it, then stop scrolling. Your nervous system doesn’t need more horror stories. It needs predictable input.
- Time: ____
- Pain (0–10): ____
- Function impact (walk/sit/sleep): ____
- Any red-flag signs (weakness/fever/headache/bowel-bladder): Yes/No
- Next action (move, rest, message clinic): ____
When to seek help (and where US patients usually go)
US systems differ by clinic and insurer (Medicare, Medicaid, commercial plans like Blue Cross Blue Shield, UnitedHealthcare, Aetna, Cigna), but the “where do I go?” logic is usually the same: call your clinic/on-call for urgent guidance, and use urgent care/ER for true red flags.
Call your clinician’s office/on-call line ASAP for
- New weakness
- Escalating numbness
- Severe positional headache
- Fever/chills, spreading redness, drainage
Go to urgent care or ER for
- Bowel/bladder changes or inability to urinate
- Saddle anesthesia (groin/inner thighs numbness)
- Severe allergic symptoms (trouble breathing, facial swelling)
- Uncontrolled pain with neurologic changes
What to say on the phone (script)
Script: “I had an epidural steroid injection on (date). Since then I’ve noticed: (symptom). My function changed like this: (walking/sleep/sitting). I have (fever/temp, weakness, positional headache, bowel/bladder changes) yes/no. What should I do next?”
Tip: If you have a temperature, give the number. If you have weakness, describe the function (e.g., “can’t toe raise” or “foot keeps catching”).
Care setting “tier map” (what changes from Tier 1 → 5)
This isn’t a rulebook. It’s a practical map of where US patients usually land.
- Tier 1: Home + symptom log (expected soreness/flare, stable strength)
- Tier 2: Patient portal message (questions, uneven relief, med side effects)
- Tier 3: Clinic call/on-call line (new weakness, fever, severe positional headache)
- Tier 4: Urgent care (needs hands-on exam but not clear ER-level red flags)
- Tier 5: ER (bowel/bladder changes, saddle anesthesia, severe allergic symptoms)
Neutral next step: Decide your tier, then act once. Re-checking every 10 minutes feeds panic, not clarity.
Next step: one concrete action
Do this today. It takes 3 minutes, and it turns your follow-up into a high-signal conversation.
Create a Day 1–Day 14 mini-log (four lines)
- Pain (0–10)
- Walking minutes
- Sleep hours
- One “can/can’t” task (e.g., “sat through dinner,” “drove 15 minutes,” “showered without bracing”)
Neutral next step: Bring this to follow-up or send a screenshot via your patient portal.
Quote-prep list: what to gather before comparing next options
If your follow-up includes PT, imaging, a second injection discussion, or a specialist referral, these details help you get a clean plan faster:
- Injection date, level (if known), and technique (if you were told). If technique comes up, you may see terms like transforaminal vs interlaminar in your notes; your symptom pattern often matters more than the jargon.
- Your Day 1–14 mini-log (pain + function)
- Current meds list (including OTC NSAIDs, supplements, sleep aids)
- Any prior imaging results (MRI report words matter)
- What worsens symptoms (sitting, walking, bending) and what helps
Neutral next step: Put this in one note on your phone titled “ESI follow-up.”

FAQ
1) How long does it take for an epidural steroid injection to start working?
Many people notice early changes between Days 3–7, but the clearest judging window is often Days 7–14. Early Day 1 relief can be from local anesthetic and may fade before steroid benefit ramps.
2) Is it normal for pain to get worse after an epidural steroid injection?
Yes, a temporary flare can happen in the first 24–72 hours. It’s usually soreness or irritation without dangerous red flags. Worsening pain paired with new weakness, fever, severe positional headache, or bowel/bladder changes is not normal.
3) What is a steroid flare and how long does it last?
A steroid flare is a short-term pain increase after the injection, often from local irritation or inflammatory response around already-angry tissues. Many people feel it settle within a few days. Track function and watch for red flags.
4) How do I know if my injection “worked” by Day 14?
Look for repeatable improvements in walking time, sitting tolerance, sleep quality, and reduced need for rescue meds. A single good day is encouraging, but the “worked” verdict is about consistency across several days.
5) Can an epidural steroid injection cause new numbness or weakness?
Temporary numbness can happen if local anesthetic was used. New or worsening weakness (or new saddle/groin numbness) should be treated as urgent and discussed with your clinician immediately.
6) What activities should I avoid the first week after an ESI?
Avoid “hero moves” that spike load: heavy lifting, deep bending/twisting, or testing maximal workouts. Gentle walking and light daily movement are often fine, but follow your clinic’s instructions. The goal is steady function, not a victory lap.
7) Why do I feel great the first day and worse on Day 2?
Day 1 can be a local anesthetic effect (temporary) plus adrenaline relief. When it wears off, soreness and irritation can rise. This doesn’t automatically mean the steroid won’t help. Judge over Days 7–14.
8) How long can relief last from an epidural steroid injection?
It varies widely. Some people get brief relief that helps them start PT; others get longer benefit. Diagnosis, severity, and rehab all matter. Your response helps your clinician decide what to try next.
Conclusion
Here’s the loop we opened at the start: “Is this normal… and when do I know if it worked?” The honest answer is: Days 1–3 are noisy, Days 3–7 are the ramp, and Days 7–14 are the verdict window. Your best compass isn’t a single pain score. It’s whether your life gets a little more livable in measurable ways.
If you do one thing in the next 15 minutes, do the mini-log and pick a single benchmark (walking minutes, sitting time, or sleep). Then send your clinic a tight message if you’re worried. You deserve reassurance that’s earned by data, not held together by vibes.
Last reviewed: 2026-02.
epidural steroid injection relief timeline day by day · day 1 after epidural steroid injection normal symptoms · day 2 pain worse after epidural injection flare · how long does steroid injection take to work sciatica · epidural injection soreness vs complication · day 7 after epidural steroid injection still pain · day 14 no relief after epidural steroid injection what next · epidural injection red flags fever weakness numbness · epidural steroid injection headache worse standing · when to call doctor after epidural steroid injection
