
Buying a bike with sciatica is weirdly personal: five “comfortable” minutes can turn into a calf buzz and a limp the next morning.
The problem isn’t the brand—it’s the seat position that quietly decides whether your sciatic nerve pain stays calm or starts sending signals down your leg.
If you’re weighing recumbent bike vs upright bike for sciatica, the goal is simple: choose the setup that prevents symptom travel (sensations creeping farther down the thigh, calf, or foot) during a short, easy ride. Keep guessing, and you risk buyer’s remorse plus a flare that steals your walks, your sleep, and your patience—especially if you’re already dealing with how to sleep with sciatica nights.
This post gives you a fast, low-risk way to decide: a 2-minute test ride protocol, the cockpit and saddle tweaks that reduce hip flexion and hunching, and two “looks comfy” setups that backfire later (hello, low saddle + long reach). I’m pulling from the hard-earned version of experience—the one where a tiny adjustment stopped the foot tingling.
Small changes. Clear signals. No heroics.
Slow breaths first. One adjustment at a time. Watch the direction—then choose.
Table of Contents
Seat position first: where bikes “poke the nerve” (before brands)
If you read ten articles, you’ll get ten opinions. But your nerve doesn’t care about opinions. It cares about positions. Specifically: how much your hips fold, how your pelvis tips, and whether the pedal stroke turns into a stealth stretch.
I learned this the hard way years ago on a “totally gentle” stationary bike—five minutes in, I felt fine; fifteen minutes in, my leg started whispering threats. It wasn’t the bike. It was my posture plus a seat set too close. The good news: these are fixable.
Posture load — neutral spine vs the quiet C-shape slump
When your low back rounds (think “C-shape”), you change how the spine handles pressure and tension. Many sciatica flares are sensitive to that rounding. On a bike, rounding usually comes from: reaching for low handlebars, sliding your pelvis under you, or sitting too far back without support.
Hip flexion load — why deeper bend can feel like a “wire tug”
Hip flexion is simply how folded your hip is. Seats set too low (upright) or too close (either bike) create a deep bend. For some people, that deep bend feels like a tugging line from the low back to the hamstring—because the nervous system and the tissues around it don’t love being compressed and stretched at the same time.
Hamstring tension — when the pedal stroke becomes a nerve stretch
Overreaching the pedals (especially on recumbents) can lock your knee near the bottom of the stroke and pull hard on the hamstrings. If your symptoms respond to tension, that can be the difference between “mild workout” and “why is my calf buzzing?”
- Rounding = higher risk for many people
- Deep hip bend = common trigger
- Overreaching pedals = sneaky tension problem
Apply in 60 seconds: Sit on the bike and see if you can keep a tall chest without bracing.
- Yes — Symptoms are stable, no new weakness, and you can walk around the house without escalating pain.
- No — You have rapidly worsening weakness, new numbness in the groin/saddle area, or bowel/bladder changes.
- Maybe — Pain is hot today, but not spreading downward; keep the test ride to 2 minutes and stop early.
Neutral action: If you’re in the “maybe,” do the 2-minute test ride and write down exactly what you felt (where it started, where it traveled).
Recumbent seat reality: when recline helps (and when it backfires)
Recumbent bikes get recommended because they feel supportive. And often they are. But “supportive” can also mean “quietly encouraging you to slump.” The recumbent advantage is real—as long as the recline and pedal distance don’t turn you into a curled shrimp.
When I test recumbents, I do one thing first: I check whether my pelvis wants to roll backward the moment I relax. If it does, I adjust before I pedal. Most people pedal first. That’s how we earn our problems.
Seat distance dial — the hidden lever for hamstring + nerve tension
Too close: your knees bend deeply, hips fold, and the front of the hip gets cranky. Too far: you reach, your knee locks out, and the back of the leg tugs. The sweet spot is where you can keep a slight knee bend at the bottom of the stroke and you don’t feel like you’re “pointing your toes” just to reach.
Recline angle — back support that still rounds your pelvis
Many recumbents let you recline more than you think. Past a point, recline can push your pelvis into a tucked position, flattening the low back. If your symptoms dislike flexion, that tucked posture can be the matchstick.
Open loop: The adjustment most people skip… then blame the bike
It’s the seat pan angle / lumbar contact issue: if the backrest hits you high but doesn’t support the low back, your spine rounds while your upper back feels “held.” It’s comfort theater. Fix it by adjusting the recline to a more upright notch, adding a small towel roll at the low back (temporary test), or choosing a model with better lumbar contour.
- Don’t overreach the pedals
- Don’t recline into a pelvic tuck
- Check lumbar contact before you pedal
Apply in 60 seconds: Do 10 slow pedal strokes—if symptoms creep downward, adjust distance first.
Upright bike without the hunch: the sciatica-friendlier cockpit
Upright bikes have a reputation for being “harder on the back.” Sometimes they are. But that’s often because the default setup encourages reaching and rounding. An upright bike can be surprisingly nerve-friendly if you build a cockpit that lets you sit tall.
I’ve used upright setups (including spin-style bikes like Peloton or similar designs from Schwinn and NordicTrack) where my back felt great—because the handlebars were up, the saddle was not jammed forward, and I stopped pretending I was training for the Tour de Pain.
Saddle height — why “too low” is often worse than “a bit high”
Too low increases hip flexion and makes the pedal stroke feel like a deep squat—great for quads, not always great for irritated nerves. A slightly higher saddle reduces the bend. The goal is not a locked knee; it’s a smoother stroke without deep folding.
Handlebar height + reach — the anti-hunch combination
For sciatica-sensitive riders, “low and far” is usually the wrong vibe. Raise the bars and shorten the reach so your shoulders don’t roll forward. If you feel your low back rounding just to hold the bars, you’re not “working core”—you’re negotiating with your symptoms.
Saddle tilt + fore/aft — small degrees, big nerve mood swings
If the saddle tips you backward, you tuck the pelvis. If it tips too far forward, you slide and grip. Aim for neutral (or a tiny nose-down if needed) and set fore/aft so you aren’t drifting into a slump. Tiny adjustments—think 5–10 mm—can change everything.
- You can’t tolerate forward-leaning
- You want back support to stay relaxed
- You can adjust distance to avoid overreaching
Trade-off: Recline can encourage slumping if lumbar contact is poor.
- You can set bars high and reach short
- You do better with a more neutral pelvis
- You prefer a compact footprint
Trade-off: Low bars + low saddle can flare symptoms fast.
Neutral action: Choose the bike you can set up to keep your chest tall and symptoms from traveling downward in 2 minutes.
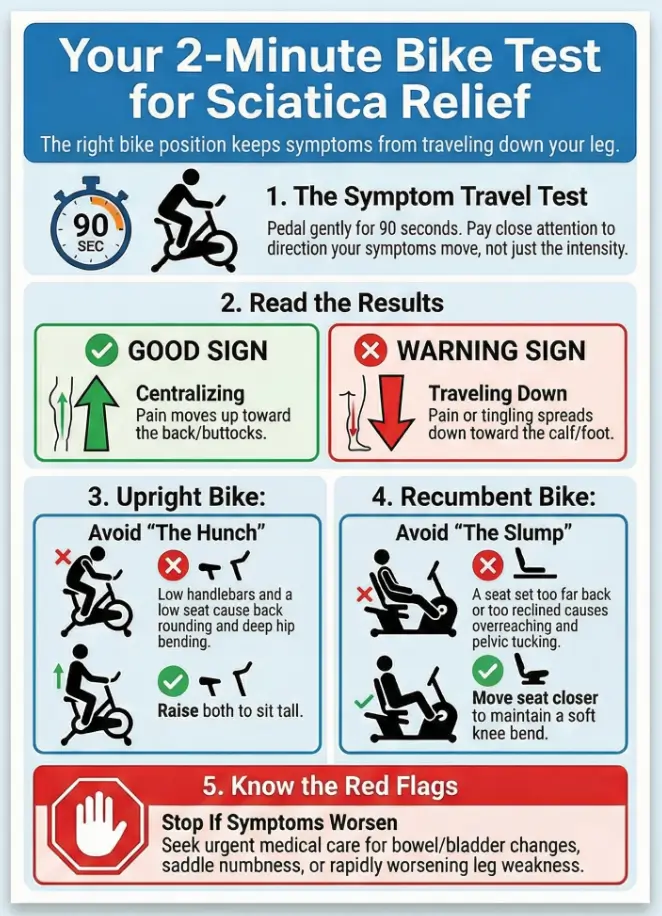
The 2-minute test ride: choose the seat that stops symptom travel
If you only remember one thing, make it this: the best bike is the one that keeps symptoms from traveling down your leg. That “travel” matters more than intensity, calories, or any sales description that uses the word “ergonomic” like a magic spell.
Here’s the test I wish someone had handed me the first time I tried to “exercise through it.” It takes 2 minutes. It saves weeks.
Test A — breathing + bracing check (can you relax your ribs?)
Sit, place a hand on your ribs, and take three slow breaths. If you can’t breathe without bracing—if your torso feels like it’s holding itself up with panic—your setup is asking for trouble. Adjust bars (upright) or recline/lumbar contact (recumbent). If you’re building a safe baseline, pairing this with a simple core routine like McGill Big 3 in 10 minutes can help you learn “stiff but not tense” bracing off the bike, too.
Test B — heel-on-pedal check (distance without overreaching)
Place your heel on the pedal and rotate to the bottom position. Your leg should be close to straight, not hyperextended. Then put your foot normally and pedal slowly. If you feel like you’re reaching, bring the seat closer (recumbent) or move the saddle forward slightly (upright) while keeping height reasonable.
Test C — symptom drift check (centralize vs creep downward)
Pedal gently for 60–90 seconds. Pay attention to where sensations go. If symptoms centralize (move upward toward the butt/back) or settle, that’s typically a better sign than if they creep downward toward the calf/foot.
Let’s be honest… tingling in the foot isn’t “good soreness.”
Pattern interrupt time. If you feel tingling, buzzing, or numbness spreading into the foot, that’s not “working it out.” That’s your nervous system raising a hand. Stop, adjust, and retest. If it repeatedly travels downward, biking may not be today’s tool—especially if you’re trying to rule out look-alike causes like diabetic neuropathy vs sciatica.
- Relaxed breathing = better setup
- No overreaching = less tension
- Down-the-leg travel = stop and adjust
Apply in 60 seconds: Do Test C with very easy resistance and watch symptom direction.
At minute 18, the tingling slid into my foot like a cold coin. I told myself, “It’ll warm up.” It didn’t. The next day, I walked like I was trying not to wake a sleeping tiger. Later, a physical therapist watched me ride for 30 seconds and said, “Your seat is too low and you’re reaching.” We raised the saddle, moved the bars, and suddenly my leg stopped complaining—exactly the kind of practical guidance you get in physical therapy for sciatica. The bike didn’t change. The position did.
Your sciatica pattern matters: who tolerates recline vs upright better
One reason online advice feels contradictory is that “sciatica” is a label, not a single experience. Two people can both have sciatic pain and respond opposite ways to the same seat. This section isn’t diagnosis; it’s a practical sorting hat for bike choice.
Disc-like behavior — when flexion is the villain
Many people feel worse with prolonged sitting, slumping, and deep bending. If that’s you, a recumbent that encourages pelvic tuck can be a trap. You may do better upright with higher bars (less slump) or with a more upright recumbent setting and good lumbar support—especially if your pattern lines up with sciatica vs herniated disc behavior (flexion-sensitive, sitting-sensitive).
Stenosis-like behavior — when flexion can feel oddly relieving
Some people feel better leaning forward and worse standing tall for long periods. If your symptoms calm slightly in a gentle forward position, an upright bike (with a comfortable reach) may feel soothing. A recumbent can still work, but test which position reduces symptom travel. And if walking is part of your plan, people with stenosis-like patterns often end up researching practical supports like a rollator for lumbar spinal stenosis for longer outings.
Sitting intolerance — what to do when both seats annoy you
If sitting itself is your trigger, don’t force a seated tool. Consider shorter bouts (2–5 minutes), more frequent breaks, or alternatives like walking, pool walking, or PT-guided graded activity. It’s not quitting. It’s choosing the least provocative path—especially if your day-to-day pattern resembles desk job sciatica flare-ups where sitting stacks the deck against you.
Open loop: The surprising case where upright feels better than reclined
It happens when upright lets you keep a more neutral pelvis and avoids hamstring overreach—especially if recumbent recline pushes you into a tucked position. Your test ride will reveal this quickly. If upright calms the leg and recumbent sends symptoms downward, believe your body over the internet.
Common mistakes: the 5 setups that reliably flare sciatica
If sciatica had a favorite hobby, it would be exploiting “almost fine” setups. The worst flares aren’t always from dramatic mistakes—they’re from tiny misfits repeated for 20 minutes.
Mistake #1 — seat too close (deep bend → more hip flexion load)
You’ll feel cramped. Knees rise high. Hips fold deep. Some people get hip pinching; others get a tug down the back of the leg. Fix: move the seat back (upright) or farther (recumbent) until the stroke feels smoother and less compressed.
Mistake #2 — long reach to bars (rounded back + nerve irritability)
Reaching turns your spine into a hinge. If you catch yourself shrugging or rounding to grab low bars, bring bars up and closer, or choose a model designed for upright comfort rather than racing posture.
Mistake #3 — big gears, slow grind (torque spikes)
High resistance with slow cadence creates “torque spikes”—big force demands per stroke. That’s often when symptoms wake up. Start easy. Build time first. Then adjust load.
Mistake #4 — recumbent pedals too far (hamstring tug-of-war)
Too far means you reach with the toes and lock the knee near the bottom. The hamstring becomes a rope in a tug-of-war you didn’t agree to. Fix: bring the seat closer until the bottom of the stroke keeps a soft knee bend.
Mistake #5 — ignoring delayed flares (the 20-minute trap)
Open loop, answered: the delayed flare often shows up when a position is “tolerable” but still provocative. Your system stays quiet until cumulative stress crosses a threshold—then symptoms drift downward later, sometimes after you’ve gotten off the bike. That’s why short test rides matter.
Don’t do this: two copy/paste “bad fits” to avoid at home
This is the loss-prevention section. If you copy nothing else from this article, copy these “don’t do this” templates and save yourself the flare.
Don’t do this: low saddle + low bars + long reach = flexion overload
What it looks like: knees high, back rounded, neck craned forward, hands locked on low bars.
Why it backfires: deep hip flexion plus spinal rounding can irritate symptoms in people sensitive to flexion.
Fix: raise saddle slightly, raise bars, shorten reach, and keep resistance easy for the first rides.
Don’t do this: reclined seat + locked knees = nerve stretch + hamstring strain
What it looks like: you’re “lounging,” legs almost straight at the bottom, toes pointing to reach.
Why it backfires: you’re pulling on the back of the chain (hamstrings) while the nervous system is already irritated.
Fix: bring the seat closer, choose a less reclined notch, and aim for a soft knee bend at the bottom.

Ride programming that’s gentler on nerves: cadence, load, time
Once the setup is good, the next trap is programming. People think they need a “real workout” to make it count. With sciatica, a better question is: what dose builds tolerance without provoking symptoms?
I’ve had the best results (personally and anecdotally) treating bike work like a confidence ladder: short, easy, repeatable. The win is finishing a ride and feeling normal an hour later.
The calm default — low resistance + higher cadence
Lower resistance reduces force demands. A slightly higher cadence spreads the effort out. Your goal is a smooth circle, not a stomp. If you can talk in full sentences, you’re in the right neighborhood.
The flare-up rule — shorten time before you increase load
If symptoms are volatile, change only one variable at a time. Add 2–3 minutes to duration before you add resistance. If the nerve starts traveling downward, that’s your stop sign.
Here’s what no one tells you… “harder” often means “more hip pinch,” not “more progress.”
When resistance goes up, people brace, grip, and move differently. That’s how “just a bike ride” becomes a full-body tension event. Keep it boring. Boring is safe. Safe is consistent. Consistent is how you actually get better.
Show me the nerdy details
Think of each pedal stroke as a “force event.” High resistance + low cadence makes each event bigger. Low resistance + higher cadence makes each event smaller but more frequent. For irritated nerves and sensitive tissues, smaller events often create fewer spikes in symptoms. This isn’t a promise—just a practical way to control load when you’re experimenting.
Pick your current symptom level and time available. Then use the output as your first test dose.
- Symptom level: Low / Medium / High
- Time available: 5 / 8 / 12 minutes
Output rule: If symptoms are High, choose 5 minutes, easy resistance, smooth cadence. If Medium, choose 8 minutes. If Low, choose 12 minutes. Stop early if symptoms travel downward.
Neutral action: Record the result 30 minutes after the ride (better / same / worse).
Who this is for / not for (and safer alternatives)
This guide is for time-poor, purchase-intent readers who want a bike that doesn’t turn a workout into a flare. It’s not for people who need urgent evaluation or who are trying to “push through” neurological changes.
Good fit — stable symptoms, walking tolerated, pain not rapidly worsening
If your symptoms are annoying but stable, you can usually test bikes safely with the 2-minute protocol. The goal is to find a setup that feels neutral and repeatable.
Not a fit — progressive weakness, major numbness, escalating radiating pain
If you’re noticing new weakness (like your foot “slaps” when walking), significant numbness, or rapidly worsening symptoms, it’s time to pause experiments and get medical guidance.
If cycling isn’t today’s move — walking, pool walking, or PT-guided options
Walking is often a gentle first-line option for many people, especially in small doses. Pool walking reduces load and can feel surprisingly good. And if you’re working with a physical therapist, ask for a graded plan that matches your symptom behavior—plus practical details like sciatica-friendly walking shoes if even short walks tend to “talk back.”
- Stable symptoms = test rides are reasonable
- Progressive weakness/numbness = pause and get help
- Alternatives exist when sitting is provocative
Apply in 60 seconds: Decide if today is a test day or a “walk and reassess” day.
When to seek help: red flags + the exact symptom notes to bring
Let’s keep this straightforward. Most sciatica isn’t an emergency—but some patterns are. MedlinePlus and orthopedic guidance commonly highlight red flags like bowel/bladder changes and significant weakness as reasons to seek urgent care. If you’re unsure, err on the safe side—especially if your symptoms match the kind of situations covered in low back pain emergency guidance.
Red flags — bowel/bladder changes, saddle numbness, worsening weakness
If you have trouble controlling urine or stool, numbness in the groin/saddle area, or rapidly worsening leg weakness, seek urgent evaluation. Conditions like cauda equina syndrome are treated as emergencies because delays can lead to lasting problems.
What to track — “where it starts,” “where it travels,” “what stops it”
Clinicians take you more seriously when you give a clean pattern. Write down:
- Start point: low back / butt / thigh
- Travel: does it move below the knee? into the foot?
- Time: how many minutes until symptoms change?
- Relief: what position calms it?
What to ask — PT bike-fit cues + graded return plan
Ask for help dialing in: seat height/distance, handlebar reach, and a progression that increases time before intensity. Organizations like the American Physical Therapy Association encourage individualized rehab approaches—because your pattern matters more than generic rules.
FAQ
Is a recumbent bike better than an upright bike for sciatica?
Often, yes—because many people can stay more relaxed with trunk support. But it only “wins” if the recumbent setup avoids low-back rounding and pedal overreach. Use the 2-minute test ride and watch symptom direction.
Can a stationary bike make sciatica worse even if it’s low impact?
Yes. “Low impact” doesn’t automatically mean “low irritation.” A low seat, long reach, or high-torque pedaling can aggravate symptoms even without impact.
What seat position on a recumbent bike is best for sciatica?
A position that keeps a soft knee bend at the bottom of the stroke, avoids a tucked/slumped pelvis, and does not cause symptoms to travel downward during easy pedaling.
How high should my upright bike seat be if I have sciatica?
High enough to avoid deep hip folding, but not so high that your hips rock side to side. Start slightly higher than “comfort low,” then fine-tune in small increments.
What resistance setting is safest during a sciatica flare-up?
Start with very low resistance. Your goal is smooth movement without bracing. If you need to grit your teeth to turn the pedals, it’s too high for a flare day.
Why do my foot or toes tingle after biking?
That can be a sign that symptoms are traveling downward, which usually means the position or load is provocative. Stop, adjust, and retest. If tingling persists, consider pausing biking and seeking medical guidance.
Should I stop biking if pain goes below the knee?
If pain or tingling is moving farther down the leg during the ride, that’s a strong signal to stop and adjust. If it repeatedly travels downward despite adjustments, biking may not be the right tool right now.
Is cycling okay with a herniated disc?
It depends on symptom behavior and posture tolerance. Some people tolerate upright cycling well; others flare with sitting and flexion. Keep the test ride short and track symptom direction. If you’re trying to sort the “what is this, actually?” question, it can help to review herniated disc sciatica treatment options alongside your symptom pattern.
Is a recumbent bike good for spinal stenosis-type sciatica?
Some people with stenosis-like patterns feel better in slightly flexed positions, which can make biking tolerable. But the correct answer is still the same: test the position and watch for downward symptom travel.
How long should I ride if I’m trying not to aggravate sciatica?
Start with 5–12 minutes depending on symptom stability. Increase time first (by 2–3 minutes), then consider resistance. Your goal is a ride that doesn’t haunt you later—because the “after” matters as much as the ride, especially if your nights are already fragile and you’re experimenting with mattress firmness for sciatica to keep symptoms from blooming at bedtime.
Close the loop: pick your seat, protect your nerve, ride today
We opened with a question: recumbent or upright—which seat irritates the nerve less? Here’s the honest closure: whichever seat lets you breathe, pedal smoothly, and keeps symptoms from traveling down the leg. That’s the win condition. Everything else is marketing.
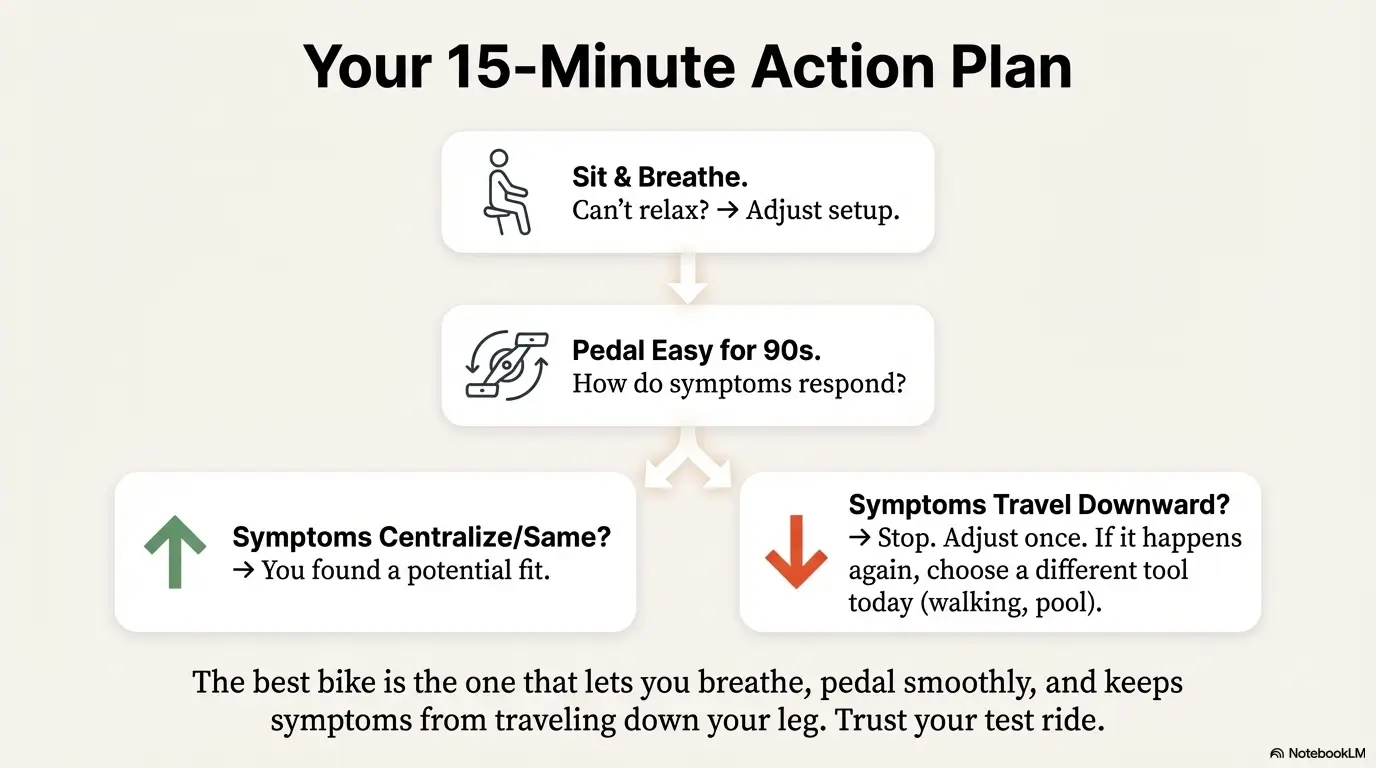
If you want a simple plan for the next 15 minutes:
- Choose one bike to test (recumbent or upright).
- Do the 2-minute test ride with easy resistance.
- If symptoms drift downward, adjust distance/reach, then retest once.
- If it still travels downward, stop and choose an alternative today (walk/pool/PT guidance).
Sit → breathe 3 slow breaths.
Can’t relax? Adjust bars/recline/lumbar contact.
Pedal easy for 60–90 seconds.
Symptoms centralize/same? Continue to Step 3.
Symptoms travel downward? Stop.
Adjust distance/reach → retest once.
Still travels downward?
Choose walking/pool/PT today. Reassess later.
- Recumbent: seat distance range, backrest contour, recline settings
- Upright: handlebar height range, reach adjustability, saddle fore/aft
- Both: return policy, warranty length, step-through ease, noise level
- Real-life fit: can you set it up without reaching or locking knees?
Neutral action: Save this list and compare two models side-by-side before you check out.
Last reviewed: 2025-12.
