
Mastering the Night: Your Post-Hip Replacement Recovery System
By day, a new hip can seem almost reasonable. By night, it can turn into a loud little parliament of swelling, stiffness, muscle guarding, and awkward angles.
Nighttime exposes every weakness in the recovery setup. While pain medication helps, it cannot fix poor pillow support or the swelling built up since dinner. This is not a sign that recovery is failing. It is a challenge of timing, angle, and system.
What you will find in this guide:
- Safer sleep positioning and pillow support
- Better evening pacing to manage late-day swelling
- Clear symptom patterns and “when to call the surgeon” indicators
- Evidence-based logic from sources like AAOS and MedlinePlus
Stop guessing and start sleeping. Systems can be improved.
Table of Contents

Fast Answer
Orthopedic pain management after hip replacement sleeping discomfort is usually less about “just needing more pain medicine” and more about position, timing, swelling, muscle guarding, and how the evening routine is set up. The most useful approach often combines safer sleep positioning, medication timing as prescribed, pillow support, gentle movement, and attention to red-flag symptoms that should not be brushed off as normal recovery.
Safety / Disclaimer
This content is educational and not a substitute for medical advice, diagnosis, or treatment. Pain and sleep disruption after hip replacement can be common, but severe pain, new swelling, calf pain, chest pain, fever, drainage, shortness of breath, sudden weakness, or a sharp change in mobility should be reviewed promptly by the surgical team or appropriate urgent care. Recovery instructions can vary by surgeon, implant approach, and personal medical history.
- Keep your surgeon’s written precautions nearby at night
- Use the exact medication plan you were given
- Treat red-flag symptoms as a call prompt, not a wait-and-see game
Apply in 60 seconds: Put your after-visit summary, surgeon phone number, and medication list within arm’s reach of the bed.
Sleeping discomfort after hip replacement is not “just pain”
Why nighttime pain often feels worse even when daytime activity seemed manageable
At night, there are fewer distractions, fewer posture changes, and more time for the body to report every little complaint with theatrical confidence. A hip that tolerated walking, sitting, and bathroom trips during the day may protest once you hold still. Swelling can pool. Muscles that spent hours stabilizing the joint can tighten. Stiffness becomes easier to notice when the room is quiet and your attention has nowhere else to go.
I have seen this pattern described by recovering patients in almost identical language: “I was okay until bed.” That does not automatically mean something is wrong. It often means the day’s load finally presented the bill. In some cases, people dealing with hip pain at night notice the same basic rhythm long before or long after surgery, even though the causes and precautions may differ.
The real culprits may be swelling, stiffness, muscle guarding, and position fatigue
After hip replacement, discomfort at night often comes from a mix of inputs rather than one villain. Swelling can create pressure and heaviness. Muscle guarding can make turning feel sharp or clumsy. A single position can become irritating after 20 or 40 minutes, even if it felt comfortable at first. That is why one person says the hip “aches,” another says it “burns,” and a third says it feels “tight and full.” They may be describing different shades of the same recovery orchestra.
Why the bed can become the place where recovery finally gets loud
The bed removes momentum. During the day, tiny shifts happen without much thought. At night, every turn becomes a committee meeting. Your operated leg has opinions. Your back has opinions. The pillow seems to have none. This is why sleep discomfort is not a character flaw and not proof that recovery is failing. It is often a systems problem.
What helps most is treating the night like a setup challenge, not a pain contest.
Who this is for, and who it is not for
Who this helps: patients dealing with soreness, stiffness, pressure, or restless nights after hip replacement
This guide is for adults in home recovery who are dealing with ordinary-seeming but disruptive nighttime discomfort: soreness, tightness, restlessness, pressure, swelling, difficulty turning, or fear of lying the “wrong” way. It is also for caregivers trying to make the setup less chaotic at 11:30 p.m. when nobody is at their best.
Who may need a different plan: people with severe symptoms, possible complications, or pain that feels suddenly different
If pain is suddenly worse, paired with drainage, fever, redness spreading at the incision, calf pain, chest symptoms, new weakness, or a major drop in function, this article is not the solution. That is surgeon-office or urgent-care territory. MedlinePlus notes that sleeping position after hip surgery should follow the instructions you were given, and those instructions can vary for a reason. If you are unsure which care setting fits the moment, it may help to understand the difference between urgent care vs orthopedic clinic decisions for musculoskeletal problems.
This is for home recovery questions, not emergency decision-making
The aim here is practical nighttime problem-solving. Think of it as a recovery field manual, not a permission slip to ignore warning signs.
Eligibility checklist
- Yes: Your discomfort is familiar, not dramatically new
- Yes: You are following a surgeon-provided medication and movement plan
- Yes: You are mainly struggling with night positioning, swelling, or sleep disruption
- No: You have chest pain, shortness of breath, new calf pain, fever, or concerning drainage
Neutral next step: If you checked any “No,” contact your care team before trying to optimize the bedtime routine on your own.
Position first, panic later
How sleep position can reduce strain before you reach for another solution
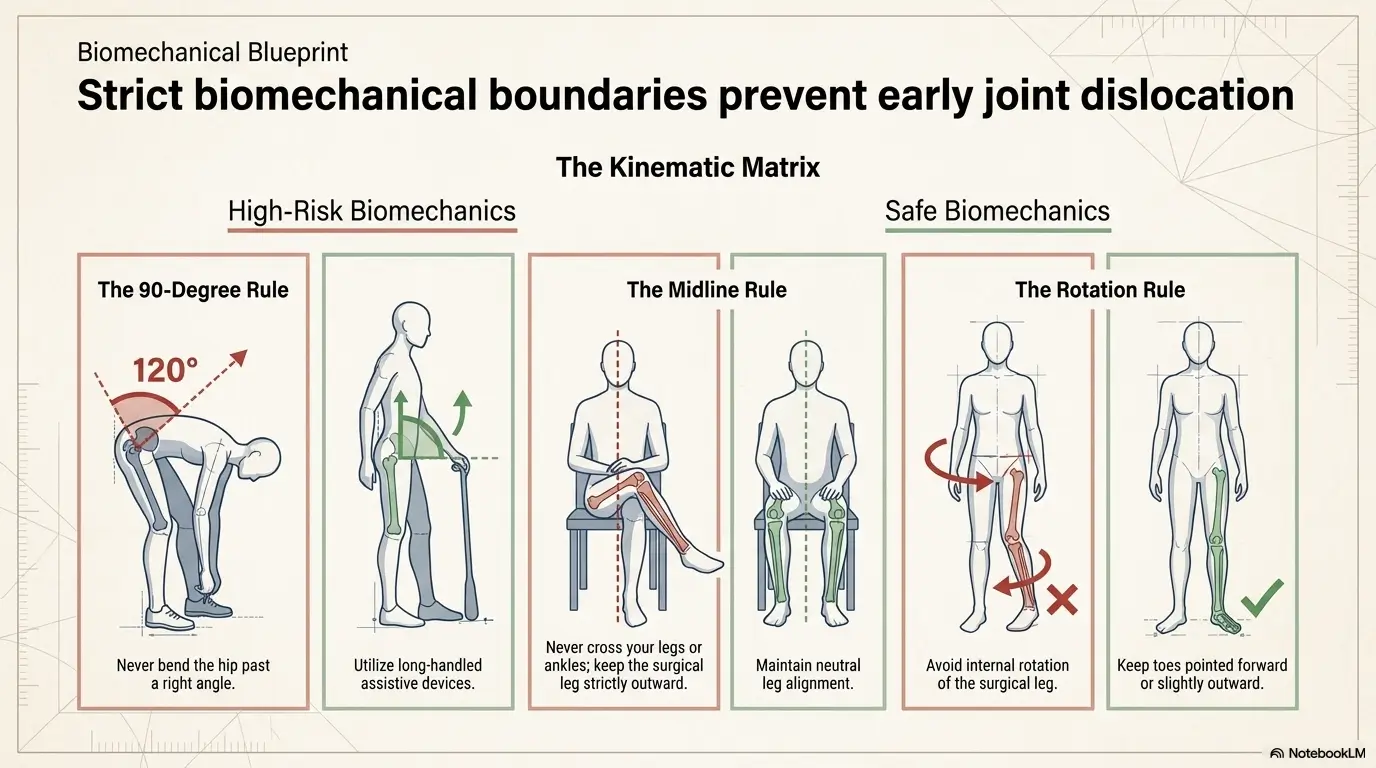
Position is not glamorous, but it is often the fastest lever. Official patient guidance from MedlinePlus notes that many patients are told not to sleep on the side of the new hip early on, and that if sleeping on the other side is allowed, a pillow between the thighs may help keep alignment. AAOS also emphasizes following any hip precautions given by your surgical team, especially in the early healing window.
That means your first question is not “What else can I buy?” It is “What position was I told is safe, and how long can I maintain it comfortably?”
Back sleeping, side sleeping, and pillow placement: what changes the pressure map
Back sleeping is often the simplest early option because it reduces twisting and makes pillow placement predictable. A pillow or wedge between the legs, or under the knees if your surgeon allows it, can change the pressure map enough to calm things down. If side sleeping on the non-operative side is allowed, a pillow between the thighs usually matters more than people expect. Without it, the top leg can pull the hip into a position your tissues dislike immediately.
A caregiver once described this perfectly: “We kept changing blankets, but the problem was really the angle.” Exactly. The angle wins more arguments than the blanket.
Let’s be honest… sleep becomes much harder when every turn feels like a negotiation
Turning in bed after hip replacement is often awkward because it is a combined task. You are moving the hip, protecting the incision, stabilizing your trunk, and trying not to violate precautions. That can make a person tense before the movement even begins, which then makes the movement feel worse. The body is rarely subtle at 2 a.m.
- Use the position your surgeon cleared
- Place pillows to prevent drifting into a bad angle
- Expect turning to feel clumsy before it feels normal
Apply in 60 seconds: Before bed, rehearse one supported turn with your pillows already in place.
The evening setup that quietly decides the whole night
Why late-day overactivity often shows up at midnight instead of right away
Recovery has a sneaky accounting system. You may feel almost normal in the afternoon, get ambitious, do “just a few more things,” and then discover at midnight that your hip kept the receipts. Overactivity does not always announce itself immediately. Sometimes it waits until tissues swell, the body cools down, and you stop moving.
This is why a decent night often starts at 5 p.m., not 10 p.m. Evening pain is frequently built earlier in the day.
How to think about timing pain medication, icing, hydration, and bathroom trips
Your bedtime routine works best when it is sequenced. Use medication exactly as prescribed and think in terms of timing, not rescue drama. If your plan includes icing, do it in the window your care team recommended so you are not trying to cool down a fully irritated hip after it has already flared. Hydrate enough to avoid feeling wrung out, but not so much that the night turns into a parade of bathroom trips and awkward bed exits.
MedlinePlus home-care guidance also notes practical environmental details that matter more than they look on paper: a bed that is the right height, a firm mattress, and an easy path to the bathroom. Tiny frictions become giant at night. Similar logic shows up when people compare how to choose rehab after surgery, because the environment often shapes recovery more than families expect.
Small pre-bed adjustments that can make the first two hours less miserable
The first 90 to 120 minutes often tell you whether the setup is working. Helpful adjustments include laying out pillows before you are exhausted, wearing clothing that does not bunch under the hip, making sure your path to the bathroom is clear, and avoiding a final burst of unnecessary chores. Nobody wins a medal for “I reorganized the kitchen at 8:45 p.m. after joint replacement.”
Decision card: When A vs B
A: You feel okay in the evening. Choose pacing anyway, because good hours can become bad nights.
B: You already feel tight and irritable by dinner. Choose a quieter evening, earlier setup, and fewer transfers in and out of bed.
Time/cost trade-off: A calmer evening may feel restrictive, but it often buys a better first sleep block without changing medication.
Neutral next step: Test one quieter evening and compare how the first two hours of sleep feel.
Swelling control matters more than many patients expect
Why swelling can feel like pain, tightness, heaviness, or pressure in bed
People often say “pain” when they mean a mix of pressure, fullness, tightness, and irritated tissue. Swelling is a shape-shifter. In bed, it can feel heavier because the body is still, the mind is alert to it, and the joint no longer benefits from gentle daytime movement. If the hip feels thick, full, or stubborn when you lie down, swelling may be part of the story.
What makes nighttime swelling feel sharper and more intrusive
Long sitting stretches, a busy day, late errands, and multiple up-and-down transfers can all increase evening irritation. So can poor limb support in bed. When the body is trying to settle, inflamed tissue resists. That resistance can feel sharper simply because you are no longer distracted by life’s usual noise.
When “aching” may really be inflammation asking for better routine management
This is why a person can sincerely say, “The meds are not working,” when the better answer may be, “The routine is not supporting the meds.” Medication can help with pain perception, but it does not by itself fix poor positioning, too much late-day activity, or a sloppy bedtime setup. Broadly speaking, this is the same principle behind orthopedic pain management: relief usually works best when medication, pacing, and mechanics are all pulling in the same direction.
Sometimes the hip is not demanding more intensity. It is asking for less chaos.
Show me the nerdy details
Night discomfort after joint surgery is often multi-factorial. Tissue irritation, edema, muscle guarding, reduced movement variability, and attention bias can all amplify symptoms once a patient lies still. That is why the same pain score can feel very different at 2 p.m. versus 2 a.m. A stable setup reduces the mechanical triggers that keep reactivating those symptoms.
Do not chase sleep by guessing
Why random pillow stacking can backfire on the hip, back, or knees
Improvisation has charm in cooking. It has mixed results in postoperative sleep. Stack too many pillows and you may torque the lower back, strain the knees, or tilt the pelvis into a position your hip hates. Use too little support and the leg drifts. The right pillow setup is not the tallest one. It is the one that maintains safe alignment and stays put.
Why taking more than prescribed is not a sleep strategy
This deserves plain language. Taking more medication than prescribed is not a valid workaround for a bad setup. It can be dangerous, and it may still fail because the core problem is mechanical or inflammatory rather than purely pain intensity. If the prescribed plan is not enough, that is a prescriber conversation, not a midnight experiment.
Here’s what no one tells you… a bad sleep setup can imitate worsening pain
A crooked night can convince you the hip is deteriorating when what really happened is simpler: poor angle, too much turning, too much evening activity, or pillow drift. That does not mean you should dismiss every bad night. It means you should not assume the most dramatic explanation first. Sometimes pain anxiety grows when people start mentally leaping from one rough evening to worst-case scenarios, which is exactly the spiral described in discussions of cyberchondria and chronic pain.
Mini calculator: how much night stress did you stack?
Count these three inputs from today:
- Late-day walking or chores longer than planned
- More than 3 extra bed/chair transfers after dinner
- No structured pre-bed positioning or icing routine
Output: If you checked 2 or 3, your night may be worse from load and setup, not just pain severity.
Neutral next step: Reduce one input tomorrow and compare the first sleep block.
Common mistakes that make nights harder
Doing too much on a “good day” and paying for it after dark
The classic recovery trap is mistaking a decent afternoon for a fully healed hip. Good hours are not fake, but they are not blank checks. Many painful nights are built on the back of optimistic daytime decisions.
Waiting until pain peaks before using the pain plan provided by the care team
When a plan says to use medication on schedule or within a certain safe pattern, waiting until pain is raging can make the whole night harder to regain. This is especially true when discomfort has a swelling or muscle-tension component layered on top.
Treating every painful night as failure instead of feedback
This one is emotional. A rough night can make people feel defeated, fragile, or behind. But recovery is rarely a neat staircase. One of the most useful mental shifts is to treat the night as data. What position lasted longest? What activity happened too late? Was the pain sharp, tight, heavy, or restless? The answers guide tomorrow.
I once heard a patient say, half laughing, half furious, “Apparently my hip keeps notes.” That is a smart way to look at it. Your job is to read the notes.
- Track what happened in the 6 hours before bed
- Notice whether the discomfort felt mechanical or inflammatory
- Compare patterns over 3 nights, not one
Apply in 60 seconds: Put a small note on your nightstand that says: “What changed today?”
Pain medicine is only one piece of the nighttime puzzle
Why medication alone may not fix discomfort caused by position or muscle tension
Medication can lower pain, but it cannot single-handedly solve poor alignment, trapped swelling, or a leg that keeps drifting into an irritating position. That is why some patients feel betrayed by pills that “should have worked.” They were not wrong to expect relief. They were just solving only one layer of the problem.
How to think about pain control without turning the whole night into a dosage experiment
A calm approach looks like this: use the prescribed plan, support the joint well, reduce unnecessary nighttime transfers, manage swelling as instructed, and give each variable a fair trial before changing five things at once. Recovery improves faster when you can tell what actually helped.
What patients often mean by “the meds are not working”
Sometimes they mean the pain returns before the next allowed dose. Sometimes they mean turning in bed still hurts. Sometimes they mean they can fall asleep but wake up in 90 minutes when the hip stiffens. Those are different problems. They deserve different fixes and, when needed, a clearer call to the surgeon’s office. For people trying to think through escalating care more broadly, the distinction between a pain clinic vs orthopedist can also be useful once recovery stops following the usual script.
AAOS patient education also highlights the importance of ice for reducing pain and swelling. That matters because it reminds us that pain relief after joint replacement is typically multimodal by design.
Don’t ignore the pattern of the pain
Soreness, stiffness, burning, pressure, and sharp pain do not all tell the same story
Words matter. “Sore after activity” points in a different direction than “sharp when turning.” “Heavy and tight at night” suggests something different than “burning near the incision.” You do not need a medical degree to notice pattern. You just need honest description.
What it may mean when pain appears mainly during turning, lying down, or getting settled
Pain with turning can suggest a mechanical trigger: movement, muscle guarding, or the effort of repositioning. Pain that builds after lying still can point more toward stiffness or swelling. Pain that is dramatically worse with each passing day, or newly paired with other concerning symptoms, deserves medical review rather than bedtime creativity.
The pattern matters more than the drama of one bad night
One ugly night can happen after a busier day, poor sleep posture, constipation, dehydration, or simple overfatigue. Patterns across several nights are more useful. This is where a short log becomes powerful. If the pattern starts sounding less like ordinary recovery and more like pain that keeps outlasting expected findings, readers sometimes find it helpful to think about the broader problem of normal imaging but pain that continues.
Quote-prep list: what to gather before calling the surgeon’s office
- When the pain starts and how long it lasts
- What it feels like: sore, tight, sharp, burning, heavy, or throbbing
- What position worsens it
- Any swelling, redness, drainage, fever, or calf symptoms
- What you already tried from the prescribed plan
Neutral next step: Keep these notes by the bed so you can describe the pattern clearly the next morning.
Movement before bed can help, but only if it is the right kind
Why gentle movement may calm the hip better than collapsing straight into bed
Some people do better when they do a brief, surgeon-approved bit of movement before bed rather than dropping into stillness like a toppled bookshelf. A short walk to loosen up, a few approved exercises, or gentle ankle pumps can help the body settle. Movement can reduce that first-wave stiffness that arrives when you lie down too abruptly.
What “too much” evening activity looks like during recovery
Too much is not just exercise. It can be repeated stair trips, prolonged standing while cooking, enthusiastic tidying, long car transfers, or multiple “I’ll just grab one more thing” moments. Recovery has a cruel sense of humor. The hip rarely complains while you are doing the extra task. It sends the invoice later.
The goal is to quiet the joint, not test it
Evening movement should feel like a downshift, not a challenge. This is not the time to prove that you are tougher than your joint. The best bedtime movement looks boring on paper. Boring is often beautiful in recovery. The same practical restraint matters with other after-surgery routines too, including seemingly simple tasks like showering after hip surgery.
Infographic: A calmer bedtime flow after hip replacement
1. Slow the evening
Avoid the late “good day” sprint.
2. Use the plan
Medication and icing only as prescribed.
3. Build the bed
Pillows first, then get in.
4. Log the pattern
Note what position lasted longest.
When sleep loss starts affecting recovery itself
How repeated poor sleep can change pain tolerance, mood, and mobility confidence
Sleep loss does not stay politely in the bedroom. After several bad nights, pain tolerance drops, patience thins, movement confidence shrinks, and ordinary decisions feel heavier. That does not mean you are coping badly. It means sleep deprivation is doing what it does.
Why fear of bedtime can become its own recovery problem
This is an under-discussed issue. Once someone expects the night to be miserable, the body can tense before bed even begins. That anticipatory stress can make turning, settling, and falling asleep harder. In other words, bedtime itself can become a trigger. For some readers, it may also be worth exploring structured sleep strategies such as CBT-I for insomnia with chronic pain if the sleep disruption stops behaving like a minor side issue.
When the sleep issue is no longer minor, even if the incision looks fine
If you are consistently getting very little sleep, feeling afraid of the bed, or losing confidence in recovery because nights are so rough, it is reasonable to contact the surgical team. “Everything looks fine” on the outside is not the whole story if your function and rest are falling apart.
Recovery is not only about what the incision looks like. It is also about whether life is becoming workable again.
Short Story: the night that stopped being a referendum on recovery
One caregiver described the first two weeks after a family member’s hip replacement as “a nightly courtroom drama.” Every difficult turn in bed felt like evidence that something had gone wrong. They kept changing blankets, adding cushions, and debating whether the medication was failing. What finally helped was smaller than they expected. They stopped treating the whole night as one giant event and started focusing on the first 90 minutes.
They moved the phone charger, cleared the path to the bathroom, set up pillows before the patient was tired, reduced the late-evening “one more little task” habit, and wrote down what the discomfort actually felt like. The next night was not perfect, but it was less chaotic. By the third night, they realized something quiet and useful: the problem was not simply pain. It was pain plus timing plus angle plus exhaustion. That changed the mood of the whole recovery. The night stopped feeling like a verdict and started feeling like a puzzle they could actually solve.
- Track how many nights in a row have felt unmanageable
- Notice if fear of bedtime is building
- Tell the surgeon’s office how sleep loss is affecting mobility and recovery
Apply in 60 seconds: Rate tonight’s concern from 0 to 10 before bed and again in the morning to see whether anxiety is amplifying the problem.
When to seek help instead of waiting for one more night
Pain that is suddenly worse, unusual, or paired with swelling, fever, or drainage
This is where caution matters. A familiar sore-and-stiff night is one thing. A sudden change is another. Concerning signs include fever, significant new swelling, drainage, spreading redness, a sudden jump in pain, or inability to do what you could do yesterday.
Calf pain, shortness of breath, chest pain, or other symptoms that should not be normalized
These are not bedtime inconveniences. They need urgent attention. Do not explain them away as “probably from the mattress” or “maybe just because I moved funny.” Recovery is no time for brave denial.
How to describe the problem clearly when calling the surgeon’s office
Be concrete. Say when it started, how it changed, what it feels like, what other symptoms are present, and whether it is preventing sleep, walking, or bed mobility. Clear description helps the team decide faster whether this is expected recovery discomfort or something that needs prompt review. If getting specialist advice becomes part of the next step, knowing the realities of orthopedic referral wait times can help families plan more calmly.
| Tier | What it looks like | Practical response |
|---|---|---|
| Tier 1 | Usual soreness, stiffness, manageable turning discomfort | Adjust setup, pacing, and symptom logging |
| Tier 2 | Several bad nights, poor sleep, routine not helping | Contact surgeon’s office during business hours |
| Tier 3 | Sudden worsening, fever, drainage, new swelling, sharp functional decline | Seek prompt medical guidance |
| Tier 4 | Calf pain, chest pain, shortness of breath | Urgent evaluation |
Neutral next step: Save your surgeon’s number in your favorites before the next rough night arrives.
FAQ
Why is hip replacement pain worse at night?
Nighttime discomfort often feels worse because swelling, stiffness, muscle guarding, and position fatigue become more noticeable when you lie still. The body also has fewer distractions at night, so ordinary soreness can feel louder.
What is the best sleeping position after hip replacement?
The best position is the one your surgical team said is safe for your specific recovery phase and surgical approach. Many patients are initially guided toward back sleeping, and some are allowed to sleep on the non-operative side with a pillow between the thighs. Follow your own precautions first.
How long does sleeping discomfort usually last after hip replacement?
There is no one timeline that fits everyone. Recovery can vary by surgical approach, activity level, swelling, general health, and how well the evening routine supports the joint. If nighttime discomfort is not gradually improving, or if it is worsening, contact your care team.
Is it normal to have trouble turning in bed after hip replacement?
Yes, many people find turning difficult early on because it combines movement, balance, coordination, and concern about precautions. Trouble turning can be common, but sudden inability to move the leg, major new weakness, or dramatic worsening should be reviewed.
Should I sleep on my back or my non-operative side?
That depends on the instructions you were given. MedlinePlus notes that many patients are told not to sleep on the side of the new hip early on, and if sleeping on the other side is allowed, a pillow between the thighs may be recommended. Your surgeon’s guidance takes priority.
Why does my hip feel tight or heavy when I lie down?
Tightness or heaviness can come from swelling, tissue irritation, stiffness after activity, or muscle guarding. Many people describe this as “pain,” even when pressure and inflammation are major parts of the sensation.
Can swelling make nighttime pain feel worse after hip replacement?
Yes. Swelling can create pressure, fullness, heaviness, and aching that become more noticeable in bed. That is one reason pacing, positioning, and prescribed icing can matter so much.
When should I call my surgeon about nighttime pain after hip replacement?
Call if the pain is suddenly worse, feels unusual compared with prior nights, is not improving over time, or is paired with fever, drainage, redness, major swelling, calf pain, chest pain, shortness of breath, or a clear drop in function.
Next step: build a one-night recovery test, not a perfect system
Choose one variable tonight: position, pillow support, timing, or activity pacing
The smartest next step is not a total bedtime reinvention. It is one small test. Change one variable tonight: use the approved position more carefully, fix pillow placement, calm the evening schedule, or tighten the timing of your prescribed routine. One change is measurable. Five changes create fog.
Write down what the pain feels like, when it spikes, and what changed
This matters because vague memory is a terrible night nurse. A 30-second log can reveal whether the first sleep block is the problem, whether turning is the trigger, whether swelling dominates after busy days, or whether the issue is actually bathroom trips and repeated bed exits. Patterns are easier to fix than panic.
Use one calmer night as data, not as proof the problem is solved
And this closes the loop from the opening: the night feels loud because many things speak at once. The answer is rarely brute force. It is better listening. If tonight goes better, wonderful. Treat that as useful evidence, not graduation. If tonight goes poorly, that is still information. Recovery often improves by quieter choices, better alignment, and faster recognition of what deserves a phone call. When those experiments stop helping enough, it can also be reasonable to think about telehealth vs in-person orthopedics for the next conversation with your care team, depending on the symptoms and urgency.
- Change one variable
- Log the pattern
- Escalate promptly if the pain becomes suddenly different or concerning
Apply in 60 seconds: Decide now what tonight’s single test will be and write it down before fatigue makes every idea feel equally bad.
Last reviewed: 2026-04.
