
Bridging the Gap: Safe Orthopedic Recovery at Home
The first week after an orthopedic discharge is where good intentions often meet the friction of reality. Pain management for older adults isn’t just about the medication. It’s a delicate balance of mobility, safety, and routine within the “quiet chaos” of the home environment.
“Home recovery is not just ‘hospital lite.’ It is a different sport altogether.”
We move beyond the guesswork that leads to falls and medication confusion. Our approach organizes pain relief, fall prevention, and red-flag monitoring into a visible, actionable plan designed to handle the pressures of daily life.
Fast Answer: Orthopedic pain management for elderly adults after hospital discharge works best when pain control, mobility, medication safety, bowel care, and follow-up planning move together. The real goal is not chasing a lower number on a pain scale. It is helping an older adult rest, walk safely, avoid medication mix-ups, notice warning signs early, and recover at home without avoidable detours.
Safety / Disclaimer: This content is educational and not a substitute for medical advice, diagnosis, or treatment. Older adults can face higher risks after discharge, including falls, medication side effects, infection, blood clots, constipation, confusion, and dehydration. If pain becomes suddenly severe, clearly worse, or comes with red-flag symptoms, contact the discharging team or seek urgent care promptly.
Table of Contents
After Discharge First: why pain control gets harder at home
Hospital structure disappears, but the pain often does not
In the hospital, recovery moves on rails. Nurses bring medications on schedule. Someone checks the wound. Someone else asks whether the patient walked. At home, the rails vanish. Pain medicine becomes a memory test. Ice packs migrate to odd corners of the freezer. The walker somehow ends up three rooms away, as if it has personal goals.
That is why the first 72 hours at home can feel harder than discharge day itself. Not because the surgery failed. Not because the family is careless. Because pain management at home is a systems problem. It depends on timing, environment, hydration, sleep, bowel function, safe transfers, and whether the person can get to the bathroom without turning a routine step into a suspense film.
The real challenge is not pain alone, but pain plus fatigue, stairs, and scheduling
Older adults rarely experience pain in isolation. Pain arrives holding hands with stiffness, weakness, dizziness, poor appetite, anxiety, and interrupted sleep. Add a few stairs, a low toilet seat, a cluttered hallway, or a medication list that reads like a small novella, and recovery can stall for reasons that have nothing to do with toughness.
Aging agencies and orthopedic guidance alike keep circling the same truth: recovery at home improves when mobility and safety planning are addressed alongside pain, not after it. The CDC notes that falls are a major threat to adults 65 and older and that medications and home hazards both raise risk. The National Institute on Aging also notes that some medications can increase fall risk by causing dizziness or confusion.
Why “doing okay in the hospital” does not always predict a smooth first week at home
A patient may look surprisingly steady during discharge teaching and then struggle once the adrenaline fades. I have seen families interpret that change as backsliding, when often it is simply reality arriving without fluorescent lighting and call buttons. The home environment asks different questions: Can they sit, stand, pivot, walk, swallow pills safely, remember what was taken, and sleep without waking in a small panic at 2:10 a.m.?
That is the shift to understand from the start. Home recovery is not a lighter version of hospital recovery. It is a different sport.
- Pain control fails when timing falls apart
- Mobility fails when the room is working against the patient
- Confusion grows when no one owns the plan
Apply in 60 seconds: Decide who tracks doses, who watches walking, and where the care plan will physically live.
Who this is for, and who it is not for
Best for older adults recovering from orthopedic surgery, fractures, joint procedures, or severe musculoskeletal pain after discharge
This guide is built for families dealing with the messy middle after discharge. That includes recovery from hip or knee replacement, fracture repair, spine procedures, severe arthritis flares, or significant orthopedic pain being managed at home. It is also useful when the older adult has several overlapping risks, such as multiple medications, prior falls, memory issues, or a home layout that makes movement harder than it should be. Families navigating similar questions earlier in the care journey may also find it helpful to compare this phase with broader guidance on orthopedic pain management for older adults.
Especially useful for family caregivers managing medications, mobility, and follow-up appointments
Caregivers often end up doing triage without being told they are doing triage. They are interpreting sleepiness, encouraging walking, checking whether the patient has eaten, and trying to decode instructions delivered at hospital speed. If that sounds familiar, this article is very much for you. You do not need a medical degree. You need a framework sturdy enough to survive real life.
Not for chest pain, sudden shortness of breath, new one-sided weakness, uncontrolled bleeding, or other emergency symptoms
This is where plain language matters. Some symptoms are not “watch and see” symptoms. Trouble breathing, sudden chest pain, stroke-like symptoms, uncontrolled bleeding, collapse, or profound new confusion belong in urgent or emergency evaluation. Orthopedic sources warn that signs of a blood clot or pulmonary embolism after joint surgery can include calf pain or swelling, shortness of breath, and chest pain.
Eligibility checklist
- Yes: Recently discharged after an orthopedic hospitalization and now managing pain at home
- Yes: Needs help coordinating medications, walking, wound checks, or follow-up
- Yes: Family wants a safer daily structure, not vague reassurance
- No: Severe breathing problems, chest pain, stroke-like symptoms, uncontrolled bleeding, or sudden collapse
Neutral next step: Use this guide for home recovery planning, but switch to urgent medical help when symptoms cross into emergency territory.
Pain plan first: do not build recovery around pills alone
Why the best home pain plan combines medication, movement, positioning, and routine
Medication matters, of course. But medication alone is a flimsy bridge. Good pain management after discharge is layered. It usually includes prescribed medicines, scheduled rest, ice or elevation when appropriate, short walks, careful positioning, and a realistic daily pattern. Think orchestra, not soloist. The tablet may be loudest, but it should not be playing alone.
In many homes, pain gets treated as a surprise even when it arrives at predictable hours. That is how the day turns jagged. A smoother plan asks: When is pain usually worse? Before walking? Before bed? During the first transfer out of a chair? Once you know the pattern, you can support function rather than merely reacting to distress.
Pain relief should support walking, sleeping, and basic function, not just lower a number
Families often ask whether a pain score of 6 is acceptable, as if the number itself holds the key. A more useful question is whether the current plan allows the person to do the jobs that matter most: get up safely, take a few walks, sleep enough to think clearly, and participate in basic self-care. Pain management that supports function is usually more valuable than pain management that briefly lowers a number but leaves the patient woozy and unsteady.
Here’s what no one tells you… pain control that is too heavy can slow recovery too
This part is unintuitive. Under-treated pain can block walking and sleep. Over-treated pain can create sedation, dizziness, constipation, and mental fog. MedlinePlus and FDA opioid guidance both warn about drowsiness, dizziness, confusion, constipation, and breathing problems with opioid pain medicines. In older adults, that can quietly increase fall risk and delay movement.
I once watched a family celebrate that their parent was “finally sleeping,” only to realize by evening that the patient had barely eaten, barely walked, and could not clearly answer what medications had been taken. Comfort matters. So does clarity. A safer goal is calm enough, mobile enough, and awake enough. For a broader look at this balancing act, see how orthopedic pain management can support function without tipping into overmedication.
Show me the nerdy details
Multimodal pain control means using more than one method so that no single treatment has to do all the work. In practice, that can mean combining prescribed medications with icing, elevation, timed walking, positioning, and sleep support. The benefit is often not dramatic pain elimination. It is reducing the extremes: the pain spikes that stop movement and the sedation that stops safe function.
- Use medication to support walking and sleep
- Layer in ice, positioning, and short movement
- Avoid the trap of chasing zero pain at any cost
Apply in 60 seconds: Write the next three “must-function” tasks for today and judge the pain plan by whether it supports them.
Medication map next: where older adults get into trouble fast
Opioids, acetaminophen, NSAIDs, and nerve pain medicines do different jobs
One reason discharge feels chaotic is that different pain medicines are solving different problems. Opioids are usually reserved for stronger pain, especially when pain limits critical function. Acetaminophen may be used as a base layer. NSAIDs, when the surgical team allows them, may help reduce inflammation and lower the need for opioids. Some patients also receive nerve-pain medicines or muscle relaxants, though those can add sedation. AAOS explains that NSAIDs may reduce the need for opioids and therefore reduce common opioid side effects such as constipation and drowsiness.
The trick is not memorizing pharmacology. It is avoiding accidental overlap and misunderstanding the role of each medication. “Take as directed” sounds simple until 8 p.m. arrives and three people are trying to remember whether the noon dose happened.
Why older adults face higher risks from sedation, constipation, dizziness, and confusion
Older adults are less forgiving of medication side effects. A dose that seems “fine” on paper can become a real problem when it meets dehydration, poor appetite, low blood pressure, poor sleep, or a midnight bathroom trip. NIA fall-prevention guidance and CDC fall-prevention materials both underscore that medications can raise fall risk, particularly when they cause dizziness or confusion.
NSAIDs deserve their own caution sign. MedlinePlus notes that common NSAIDs such as ibuprofen and naproxen can cause ulcers, bleeding, or holes in the stomach or intestine, and that risk is higher in older adults. That does not mean they are never used. It means they should be used exactly as the treating team intended, not as freelanced problem-solvers pulled from a kitchen drawer. If families are trying to sort out where conservative pain strategies end and specialty input begins, the difference between a pain clinic and an orthopedist can help clarify the lane.
The hidden danger of duplicate ingredients from “extra” over-the-counter products
This is one of the quietest and most common hazards at home. A patient may be prescribed a combination pain medication that already contains acetaminophen, then also take a “regular” over-the-counter acetaminophen product, then later reach for a cold medicine with the same ingredient. The FDA warns not to take more than one acetaminophen-containing product at a time, and MedlinePlus advises checking labels because acetaminophen may appear under abbreviations like APAP.
That is why every discharge plan needs a medication map, not just a medication pile.
Medication role map
| Medicine type | What it may help | What families often miss |
|---|---|---|
| Opioid | Stronger pain that blocks walking or rest | Drowsiness, constipation, slowed breathing, confusion |
| Acetaminophen | Baseline pain control | Can be duplicated across products |
| NSAID | Pain plus inflammation | Bleeding and stomach risks may matter more in older adults |
| Nerve pain or muscle medicine | Specific pain patterns or muscle spasm | Can add dizziness or fogginess |
Neutral next step: Make a one-page medication sheet listing exact names, strength, timing, and “contains acetaminophen: yes/no.”
Mobility matters more: the quiet link between pain and decline
Under-treated pain can reduce walking, appetite, confidence, and sleep
When pain is not managed well enough, older adults often start protecting themselves by moving less. That instinct makes sense in the moment. It also has a cost. Less movement can mean more stiffness, more fear, less appetite, worse sleep, and a faster slide into deconditioning. NIA materials on aging and mobility emphasize that loss of mobility is tied to lower independence and worse outcomes.
Walking is not only exercise after orthopedic discharge. It is part of the treatment plan. It helps circulation, bowel function, confidence, and the daily proof that recovery is still moving forward even when pain has not received the memo.
Over-treated pain can raise fall risk and delay safe movement
The opposite problem looks quieter but can be just as disruptive. A heavily medicated patient may say pain is better while transfers become slower, balance less reliable, and alertness shakier. Older adults do not need heroic doses. They need just enough relief to move with less distress and less danger.
Let’s be honest… many setbacks begin when pain control and movement stop working together
I have seen recovery improve dramatically when a family stopped asking only “How bad is the pain?” and started asking “Could you walk to the bathroom safely?” and “Could you do one short hall walk before lunch?” Those are more boring questions. They are also better questions.
Short Story: On the third day after a hip procedure, one daughter told me her father’s pain seemed “all over the place.” Morning was grim. Afternoon was sleepy. Night was restless. When she described the day in order, the pattern finally appeared: medicine was delayed until pain was already loud, then he felt too groggy to walk, then he got stiff, then bedtime became a small disaster. They changed almost nothing dramatic.
They timed the first dose before the morning routine, set out water and the walker in the same place, and aimed for three tiny walks instead of one noble march. By the next evening, his pain score had not become magical, but his day had become legible. That was the real win. Recovery likes legibility. Families facing longer gaps before specialist follow-up may also want to read about how to manage orthopedic referral wait times without losing momentum.
- Too little relief can block walking
- Too much relief can increase fall risk
- Function is the scoreboard that matters most
Apply in 60 seconds: Set one small mobility target for the next 4 hours, such as one safe walk to the bathroom and back.
Do not wait on red flags: the symptoms that change the plan
Pain that suddenly spikes instead of gradually improving
Not every rough day is an emergency. Recovery has texture. Some soreness increases after physical therapy or a more active day. But pain that suddenly spikes, becomes distinctly different, or stops responding in the usual way deserves attention. The question is not whether pain exists. The question is whether the pattern still makes sense.
Fever, wound changes, calf swelling, chest symptoms, or new confusion
AAOS patient guidance after joint replacement highlights warning signs such as persistent fever, increasing redness or drainage from the wound, increasing pain, calf pain or swelling, shortness of breath, and chest pain. Those are not decorative details on discharge paperwork. They are the lines that change the plan. New confusion in an older adult after discharge also deserves prompt medical attention, especially if it appears alongside medication changes, dehydration, infection concerns, or reduced intake.
When severe constipation, vomiting, or medication side effects deserve a call the same day
Constipation is often treated like a side quest. It is not. Opioids commonly cause constipation, drowsiness, nausea, and mental fog, and unresolved bowel problems can worsen pain, appetite, sleep, and willingness to move. When vomiting, severe constipation, profound sleepiness, or medication confusion enter the picture, same-day contact with the clinical team is often the smarter move. If symptoms start crossing from “rough recovery” into “something may be wrong,” the decision framework in urgent care vs. orthopedic clinic for orthopedic pain can help families think more clearly about where to go.
Decision card: watch, call, or go now?
Watch: Expected soreness that still fits the recovery pattern and improves with the usual plan.
Call same day: New confusion, medication side effects, wound concerns, repeated vomiting, severe constipation, or pain that no longer behaves normally.
Urgent help now: Chest pain, trouble breathing, sudden major leg swelling, stroke-like symptoms, collapse, or uncontrolled bleeding.
Neutral next step: Keep the surgeon’s office, primary care, and urgent contact numbers in one visible place before evening arrives.
Common mistakes: what makes home recovery harder than it needed to be
Taking medicine only after pain becomes overwhelming
Waiting until pain is already shouting often makes it harder to regain control. For many patients, especially in the early post-discharge window, the better strategy is to follow the prescribed timing closely enough that the day does not repeatedly fall into a hole.
Skipping walking because rest feels safer in the moment
Rest is useful. Immobility is expensive. When families become understandably protective, they can accidentally help create more stiffness, more fear, and more dependence. Small, safe movement usually beats prolonged stillness.
Missing the bowel plan while focusing only on pain relief
Few household dramas are less glamorous than post-op constipation, yet it is one of the most predictable ways recovery gets derailed. Outpatient orthopedic guidance often includes medications to help prevent constipation because the problem is that common.
Treating sleepiness, dizziness, and poor appetite as “normal” without checking the cause
Some symptoms are common. That does not mean they are harmless. Sleepiness might reflect medication load. Dizziness might reflect blood pressure changes, dehydration, or medication effects. Poor appetite may point to nausea, constipation, pain, or a brewing complication. Families do best when they stay curious instead of assuming every unpleasant thing is “just part of recovery.”
Show me the nerdy details
Many post-discharge setbacks are not caused by one catastrophic mistake. They come from stack-ups: missed doses, delayed walking, dehydration, constipation, poor sleep, and a mildly unsafe room all nudging recovery in the wrong direction at once. The fix is often less dramatic than the problem. It is about friction reduction.
Do not do this: five discharge habits that quietly create setbacks
Mixing old prescriptions with new discharge medications
This is the classic cabinet trap. Someone still has a prior pain medicine from a dental procedure, an old muscle relaxant, or a leftover prescription from months ago. It feels wasteful not to use it. It can also scramble the safety picture fast. Older adults often take multiple medications already, and NIA warns that taking medicines the wrong way or mixing certain drugs and supplements can be dangerous.
Waiting too long to schedule orthopedic or primary care follow-up
Follow-up is not administrative garnish. It is part of the treatment. Questions that seem minor on day 2 can become much harder to sort out on day 7. If the discharge papers say call, call. Calendar optimism is a lovely human trait. It is not a care plan.
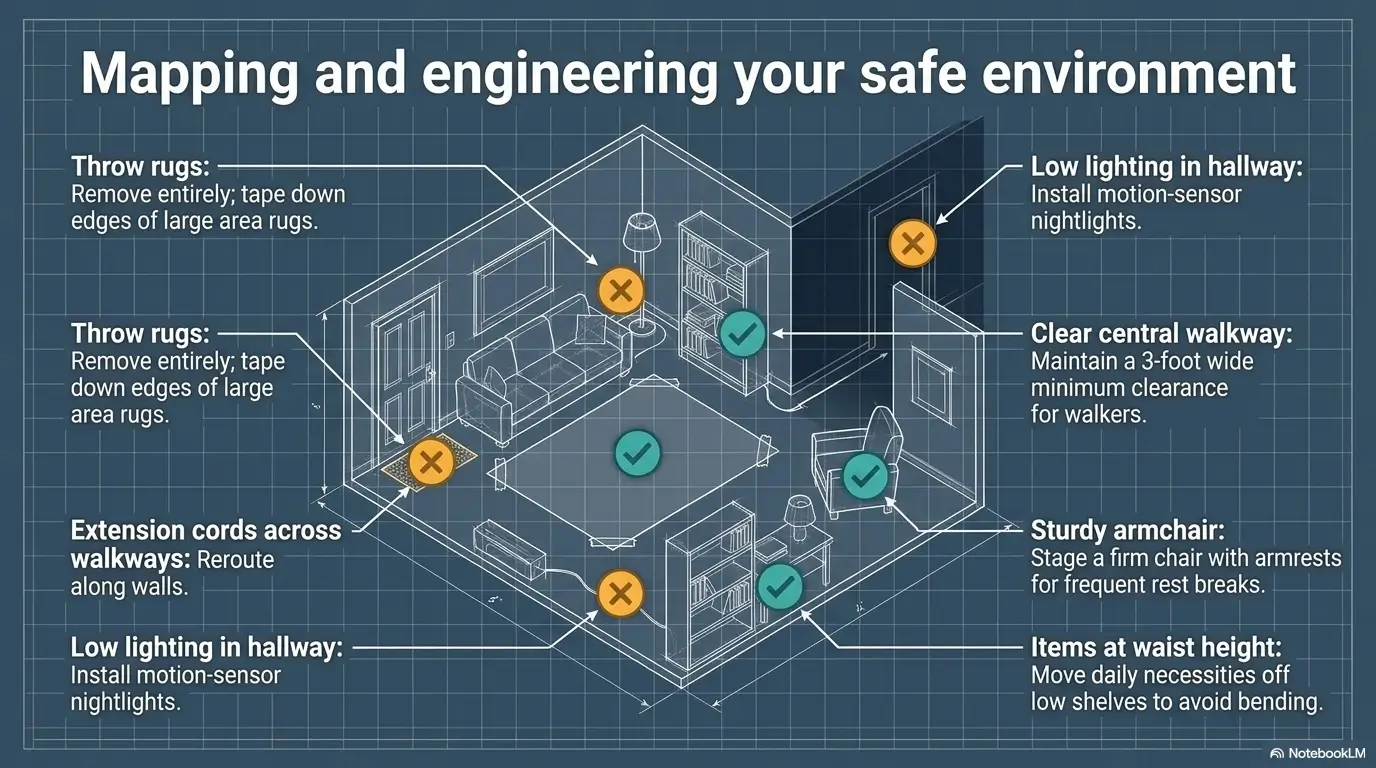
Letting the home setup stay risky with loose rugs, poor lighting, or hard-to-reach essentials
The CDC and NIA both identify home hazards as a real contributor to falls in older adults. Loose rugs, dim hallways, low chairs, cluttered paths, and a phone that requires a hiking expedition to reach all add avoidable risk.
Assuming “more pain” always means “more medication”
Sometimes pain increases because the person is constipated, dehydrated, overdue for repositioning, sleeping badly, or trying to move from a chair that is too low. The answer might be medication. It might also be timing, ice, elevation, hydration, a bowel intervention already authorized by the team, or a same-day call for guidance. When home measures stop matching the pain pattern, some families end up wondering whether they are looking at normal imaging with pain that still continues or a problem that needs a deeper workup.
What to gather before you call the office
- Current medication names, doses, and last time taken
- Today’s pain pattern, not just one pain number
- Walking ability compared with yesterday
- Bowel movement timing, appetite, hydration, and urine output
- Any wound changes, fever, swelling, or confusion
Neutral next step: Put this list near the phone so the call starts with facts rather than memory gymnastics.
Home setup counts: small environment fixes that protect recovery
Chair height, bathroom access, ice placement, and walking paths matter more than people expect
Families often imagine recovery success depends mainly on medication choice. In practice, the room itself votes. A chair that is too low turns every stand into a negotiation. A bathroom with no easy route becomes a nightly hazard. An ice pack stored behind frozen peas and a morally confusing bag of dumplings will not help anyone at 11 p.m.
A safer setup does not need to look like a showroom. It needs to be boring in the best way. Clear walking path. Good lighting. Water within reach. Phone within reach. Walker where it will actually be used, not where it photographs well.
Why a bedside routine can reduce nighttime pain panic and falls
Night is when otherwise sensible plans become folklore. People are sleepy, disoriented, and less steady. A bedtime setup can reduce both pain panic and fall risk: water, tissues, prescribed medications organized for the next timing window, glasses, a lamp that turns on easily, and a clear path to the bathroom. If the recovery involves a hip procedure, practical home details such as safer showering after hip surgery can fit naturally into this same “remove friction before nightfall” mindset.
The goal is not a perfect home, but a safer one by tonight
That phrase matters because perfection delays action. You do not need a full home makeover. You need to remove the biggest friction points before the next transfer, the next walk, and the next nighttime wake-up.
Infographic: The first-night home recovery setup
Clear path, walker parked where it is used, no loose rugs, no cords.
Lamp, phone, water, glasses, and call numbers within reach.
One visible schedule, no old prescriptions mixed in, dose times recorded.
Ice or elevation supplies ready, not buried. Comfort should not require archaeology.
Caregiver role clarified: support without taking over everything
What caregivers should track each day: pain, walking, sleep, bowel movements, appetite, and alertness
Caregiving goes better when it stops pretending memory will save the day. A simple daily log beats heroic recall. Track six things: pain pattern, walking, sleep, bowel movements, appetite, and alertness. Those six usually tell a clearer story than a single pain score ever will.
How to help with medication timing without creating confusion or conflict
Use one list. One pen. One location. Record what was taken when it was taken. Do not leave the plan floating across text messages, a fridge note, and the vague confidence of the cousin who says, “I’m pretty sure we already gave that.” The older the adult and the more medications involved, the more valuable visible simplicity becomes.
When the caregiver’s observation becomes the missing clinical clue
Clinicians often rely on caregiver observations because those observations reveal pattern change. “He is just not quite right today” is not a diagnosis, but it can be an important clinical clue, especially after discharge. If you notice less alertness, less walking, worse intake, or a new kind of confusion, say so plainly and early.
- Track patterns, not perfection
- Use one medication record
- Report “not quite right” changes early
Apply in 60 seconds: Start a one-page daily log with six lines: pain, walking, sleep, bowel, appetite, alertness.
The follow-up window: questions to bring before problems snowball
Ask what level of pain is expected, and what change is not expected
Families do better when they know the expected range, not just the emergency range. Ask what kind of pain trajectory is normal for this procedure and this patient. “Some pain is expected” is true and not especially helpful. “Pain should be gradually improving, even if unevenly” is more useful.
Clarify how much walking, exercise, and weight-bearing is actually allowed
This is another place where vague reassurance causes trouble. “Move as tolerated” can mean many things to many frightened people. Ask the team to translate instructions into plain actions: how often to walk, whether weight-bearing is limited, whether stairs are permitted, and how to handle swelling after activity. If physical therapy access is part of the concern, families may also want to review how Medicare Part B physical therapy coverage works when follow-up rehabilitation is being planned.
Confirm when to taper medication, when to call, and who owns the next step
One of the most common discharge failures is ownership confusion. Does the orthopedic office handle medication questions? Does primary care manage sleepiness or constipation? When should pain medicine be tapered? Which number should be used after hours? A recovery plan becomes much safer once those questions stop floating. For families who are weighing convenience against hands-on evaluation, telehealth vs. in-person orthopedics can also shape that next step.
Show me the nerdy details
Good follow-up questions reduce uncertainty in three domains: expected recovery pattern, medication responsibility, and escalation route. That sounds dry, but it is exactly what prevents 8 p.m. guesswork from turning into unnecessary suffering or an avoidable emergency visit.
When to seek help: know the line between discomfort and danger
Seek urgent help for trouble breathing, chest pain, sudden leg swelling, severe weakness, or signs of stroke
These symptoms are not waiting-room philosophy questions. They are urgent. Orthopedic and medication safety guidance consistently flags trouble breathing, sudden chest pain, major leg swelling, and overdose-like breathing suppression as reasons for emergency action.
Contact the care team for worsening wound redness, drainage, fever, uncontrolled pain, repeated vomiting, or new confusion
Same-day contact is often appropriate when the problem is serious but not necessarily ambulance-serious. Worsening redness, drainage, fever, pain that is not being controlled as expected, repeated vomiting, or new confusion should move the family from observation to communication.
Call sooner, not later, when an older adult seems “not quite right” after discharge
That phrase can sound vague, but families know what it means. The person is off. More withdrawn. More foggy. Not eating. Not moving. Not themselves. In older adults, small changes can be early clues. Better one sensible call than one silent night that grows teeth. When the problem is severe pain without obvious answers, the path from symptom to imaging can also become relevant, especially in situations where a clinician may consider an MRI referral for orthopedic pain.
FAQ
How much pain is normal after orthopedic discharge in an older adult?
Some ongoing pain is expected, especially during movement, transfers, and the first days at home. The key is whether the pain pattern still makes sense and whether the patient can do essential activities more safely over time. Gradual improvement matters more than a perfect number.
When should pain start improving instead of staying the same?
Many patients improve unevenly rather than in a straight line. A rough morning or a harder day after therapy can still be normal. But pain that is sharply worsening, changing character, or no longer responding as expected deserves a call.
Is it better to stay ahead of pain or wait until pain gets bad?
For many early post-discharge patients, following the prescribed plan before pain becomes overwhelming works better than chasing pain once it is already loud. The goal is not overmedication. It is preventing repeated pain spikes that disrupt walking, eating, and sleep.
What should I do if pain medicine causes constipation or sleepiness?
Do not shrug and assume that is simply the price of recovery. Review the medication plan, hydration, movement, and bowel routine, and contact the clinical team if symptoms are significant or worsening. Opioids commonly cause constipation and drowsiness.
When is swelling normal, and when is it a warning sign?
Some swelling near the surgical area can be expected, especially after activity. But swelling that is sudden, severe, one-sided in a concerning way, or paired with calf pain, redness, or shortness of breath deserves prompt medical attention.
How can an elderly adult sleep better without making falls more likely?
Start with the basics before adding complexity: better pain timing, easier bed setup, clear path to the bathroom, water nearby, fewer nighttime obstacles, and avoiding unnecessary sedating extras. Sleep should be supported without turning the patient into a midnight fall risk. For procedure-specific comfort planning, articles such as whether a recliner or bed works better after shoulder surgery can be useful when positioning becomes part of the problem.
What if my parent refuses to walk because it hurts?
Acknowledge the fear first. Then shrink the task. One short walk is often more realistic than “exercise.” Frame walking as part of pain management, circulation, and recovery, not punishment for being sore. If refusal persists or pain seems out of proportion, contact the care team.
Should we call the orthopedic office or the primary care doctor first?
For surgery-specific pain, wound concerns, mobility restrictions, or procedure-related questions, the orthopedic office is usually the first call. For broader medication reconciliation or chronic medical issues, primary care may also matter. The best answer is to clarify this before the first problem appears.
Mini calculator: is the current plan working?
Count these three items for today:
- Number of safe walks completed
- Number of meals or meaningful snacks taken
- Number of concerning side effects noticed
Read the result: If walking is near zero, intake is poor, or side effects are increasing, the pain plan may not be supporting recovery well enough.
Neutral next step: Use the result to structure a same-day call rather than relying on a vague “it’s just been hard.”
Next step: make one page before the next dose is due
Write down the medication schedule, warning signs, follow-up numbers, and today’s mobility goal
This is the practical hinge of the whole article. Before the next dose is due, make one visible page. Include the exact medication names, timing, last dose given, warning signs that mean call, warning signs that mean urgent help, and one mobility goal for today. One page. Not five. Recovery does not need a bureaucracy.
Put that page where both the patient and caregiver can see it
The refrigerator, a side table, or the main medication area all work. Visibility reduces duplication, conflict, and the sort of half-panicked uncertainty that makes everyone sound less kind than they usually are.
One clear sheet can prevent the kind of confusion that turns a hard week into a return visit
That is the curiosity loop from the beginning. Home does not become safer because it feels familiar. It becomes safer because the plan becomes visible. In the first week after discharge, clarity is a form of pain control. It lowers delay, lowers conflict, lowers guesswork, and helps the right action happen a little sooner. When the discharge destination itself is uncertain, families may also benefit from thinking through how to choose rehab after surgery before small problems become larger ones.
- List medicines and last dose times
- List call-now and urgent-now symptoms
- List today’s walking goal and follow-up numbers
Apply in 60 seconds: Start the page before the next medication window, not after the next confusing moment.
Last reviewed: 2026-04-14.
