
The 2 A.M. Physics of Recovery: Recliner vs. Bed After Shoulder Surgery
Around 2 a.m., the recliner versus bed debate stops sounding like a home setup question and starts feeling like applied physics with bad timing. One surface may calm the shoulder but punish your neck and lower back. The other may feel softer overall yet turn every bathroom trip into a clumsy, one-armed engineering problem.
That is why so many patients get stuck. They are not just trying to sleep. They are trying to protect a repair, manage night pain, follow sling rules, and stand up without twisting, pushing, or nearly falling. After rotator cuff repair, shoulder arthroscopy, labral surgery, or even replacement, the wrong setup can quietly make recovery harder than it needs to be.
Keep guessing, and you risk trading one kind of pain for another, or turning simple overnight movements into setbacks.
This guide helps you choose the safer, more workable option for your actual recovery stage. You will see why elevation matters, how pillow support changes everything, and when a recliner really does beat a bed, or when a properly built bed setup wins.
The method here is practical, not decorative: judge each setup by shoulder support, transfer safety, whole-body comfort, and repeatability over several nights. Because comfort is only half the story. Safe exits matter too. And night pain has patterns. Once you see those patterns, the furniture question gets much easier to answer.
Table of Contents
Safety / Disclaimer
This article is for general education, not personal medical advice. After shoulder surgery, positioning, sling use, icing, and medication timing can vary based on the procedure, your surgeon’s protocol, and your health history. Follow your orthopedic team’s instructions first, especially if they conflict with general recovery advice.
That matters more here than in many recovery topics. “Shoulder surgery” is not one thing. A rotator cuff repair, labral repair, instability procedure, arthroscopy, and shoulder replacement can all create different early restrictions. Some patients are told to sleep elevated for comfort. Some are told to keep the sling on at night. Some can start moving the elbow and hand right away, while others still need stricter protection of the shoulder itself. A broad internet rule can sound confident and still be wrong for your exact repair.
There is also a simple but important distinction between comfort advice and safety advice. Comfort asks, “Which surface hurts less?” Safety asks, “Can you get in, stay positioned, and get out without twisting, reaching, pushing, or nearly falling?” The second question usually deserves more respect than it gets.
- Procedure type changes the answer
- Sling rules matter at night
- Safe entry and exit matter as much as comfort
Apply in 60 seconds: Put your surgeon’s discharge instructions beside your sleeping area before the first night home.
When This Comparison Matters Most: Who This Is For / Not For
This is for you if you are trying to decide where to sleep for the first few weeks after shoulder surgery
The first week is when the question feels loudest. Swelling is fresh. Muscle guarding is dramatic. The nerve block may wear off like a villain exiting on cue. Even people who normally sleep anywhere, on planes, couches, hotel beds with tragic pillows, suddenly become very particular creatures.
This is for you if getting in and out of bed feels harder than the pain itself
That is not laziness. It is mechanics. A flat bed often asks more from your trunk, core, hips, and non-surgical arm. If the exit sequence is awkward, pain can spike before you are even fully awake. Many families discover this the hard way on night one, usually after saying the famous last words: “We’ll just figure it out when we get home.”
This is for you if you are a caregiver setting up a recovery space before surgery day
Caregivers often focus on ice packs, medication, and extra pillows, which is wise. But the hidden variable is choreography. Where will the patient place the good hand? What side will they enter from? Where will the water, phone, sling pillow, and medications sit? Tiny distances become important when one arm is off duty.
This is not for you if your surgeon has already given strict, procedure-specific sleep positioning rules
If your team has given exact instructions, that outranks this article. Full stop. Some patients need less improvisation, not more.
This is not for you if you are looking for emergency medical advice about severe pain, breathing trouble, or surgical complications
Severe uncontrolled pain, chest pain, breathing trouble, fever, drainage, blue or cold fingers, or a hand that feels suddenly different are not “sleep setup” questions. Those belong to your surgeon’s office, urgent care, or emergency care depending on severity.
Eligibility checklist: Is this a furniture question or a surgeon question?
| Question | Yes / No | Next step |
|---|---|---|
| Can you sit, reposition, and stand without using the surgical arm? | If no | Prioritize the setup with easier exits and caregiver help |
| Do you have clear sling-at-night instructions? | If no | Call before improvising |
| Does lying flat sharply worsen pain or nausea? | If yes | Start with a recliner or elevated bed setup |
| Are you having red-flag symptoms? | If yes | Seek medical help, not pillow advice |
Neutral action: Use this checklist before shopping, rearranging furniture, or assuming the bed is fine.
First Question First: Why Recliners Often Win Early
A recliner can reduce the misery of lying flat when swelling and guarding are highest
Early after surgery, many people simply feel better with the upper body elevated. A semi-upright position can make the shoulder feel less dragged on, less vulnerable, less theatrically angry. Official patient instructions from orthopedic sources commonly mention that some patients are more comfortable sleeping in a reclining chair or propped up in bed during the first days or weeks after shoulder surgery. That does not make the recliner magical. It makes it mechanically forgiving.
The semi-upright angle may make it easier to protect the shoulder while standing up
This is the sleeper issue, no pun intended. Going from nearly flat to standing often forces a person to roll, push, brace, twist, or grab. A recliner shortens that journey. Instead of a deep-core maneuver at dawn, you are starting closer to vertical. For many patients, that alone is worth the chair’s imperfections.
Controlled positioning can reduce the chance of rolling onto the surgical side in your sleep
A recliner creates walls without looking like walls. Armrests, a fixed angle, and less room to flop around can be genuinely useful. For back sleepers, that is a gift. For side sleepers, it is an intervention bordering on a hostage negotiation, but still often effective.
Here’s what no one tells you: sometimes the real issue is not sleep quality, but exit strategy at 2 a.m.
Bathroom trips expose weak setups. The best recliner is not merely the softest. It is the one from which you can rise without a dramatic one-person wrestling match. If getting out feels safe and predictable, your pain often feels more manageable because you stop bracing for the next movement.
One very common scene goes like this: the patient says the recliner is not especially comfortable, but still prefers it because the bed feels like a trap. That is useful information. It means the problem may be transitions, not the sleeping surface itself.
Show me the nerdy details
Why recliners often feel better early on comes down to angle, support, and movement control. Elevation may reduce the subjective discomfort of lying flat, and a more upright starting position can lower the amount of trunk rotation and pushing needed to stand. The shoulder also benefits when the forearm and elbow stay supported instead of drifting backward or outward during sleep.
- Elevation often feels better early
- Less rolling means less accidental strain
- Easier standing can lower fear and pain spikes
Apply in 60 seconds: Test whether you can stand from the recliner using only the non-surgical side and your legs.
Bed Setup Reality Check: A Bed Is Not Automatically the Wrong Choice
A standard bed can work when pillows are used to create a stable, elevated position
The bed is not the villain. A badly prepared bed is. Many patients do well with a wedge pillow, stacked firm pillows, or an adjustable base that keeps the torso elevated and the arm supported. The phrase that matters is stable elevation. If the pillow mountain collapses by 1:15 a.m., you do not have a setup. You have optimism with upholstery.
Side sleepers often struggle more unless they can tolerate temporary sleep retraining
People who have spent years curled on one side do not become disciplined back sleepers because a discharge packet asked nicely. This is one reason the bed can feel harder. It offers freedom, and freedom is not always helpful in early recovery. A bed can absolutely work, but it sometimes requires more intentional barriers: a wedge behind the back, support under the forearm, and enough side blocking to keep the body from rotating toward the surgical shoulder.
Adjustable beds change the equation more than most comparison articles admit
An adjustable bed narrows the gap between bed and recliner dramatically. When the head section rises and the knees bend slightly, the body is less likely to slide down and less likely to feel like it is peeling itself off a flat surface. This can turn “bed is impossible” into “bed is decent, which counts as victory.”
If your pain spikes only when getting up, the bed itself may not be the real problem
Sometimes the patient sleeps reasonably well once positioned, then suffers during entry and exit. In that case, the fix may be technique, bed height, or support placement rather than abandoning the bed entirely. A low, soft mattress can be especially unhelpful because it swallows the hips and forces extra effort to stand.
Families often learn this by accident. The expensive pillow wedge gets blamed, but the true culprit is that the patient has to do a small abdominal performance piece just to get upright. The shoulder then joins the protest.
Decision card: When the bed makes more sense than the recliner
| Choose bed first when… | Why it can work |
|---|---|
| You have an adjustable bed | It can mimic reclined support without the chair’s neck and hip problems |
| Your lower back hates recliners | A mattress may distribute pressure better overnight |
| A caregiver can help with setup and rising | Transition pain may be more manageable |
| You can maintain elevation all night | The bed no longer acts like a flat surface |
Neutral action: Test your actual bed with the full pillow setup before concluding that beds never work after shoulder surgery.
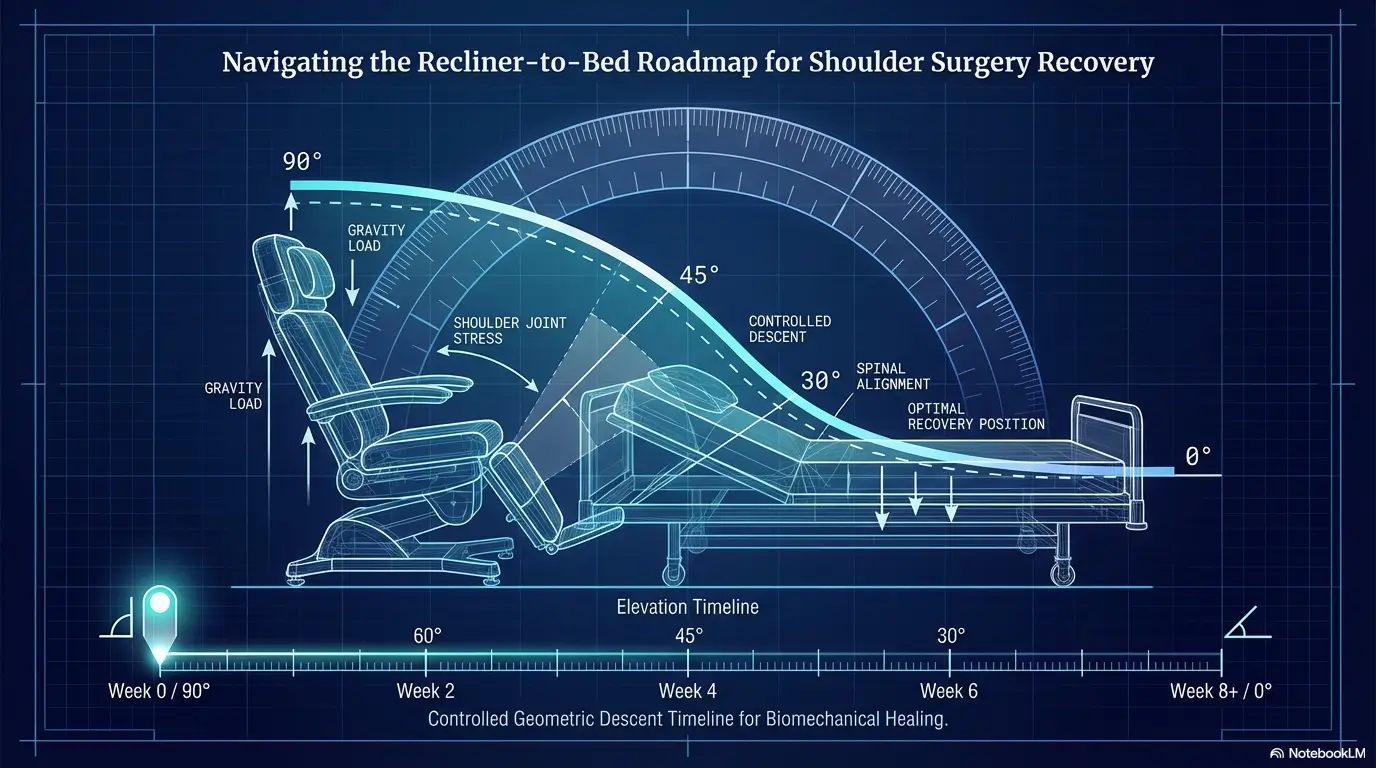
Pain at Night Has Patterns: What Makes One Setup Hurt More Than the Other
Pain often rises when the arm loses support, not simply because you chose the “wrong” surface
Night pain is sneaky. It is not always the mattress or the chair. Often it is the moment the forearm drops, the elbow loses its pillow, or the shoulder drifts into a position your body immediately dislikes. Patients sometimes blame “the bed” when the actual problem is that the arm is hanging in space like a badly parked crane.
Shoulder stiffness, swelling, and muscle guarding can build after the nerve block wears off
This is why night two or three can feel more difficult than expected. The initial haze of anesthesia support is gone, swelling settles in, and the body starts guarding like a suspicious bouncer. If the setup cannot keep the arm protected without constant waking adjustments, pain tends to collect interest overnight.
Poor neck, elbow, and wrist support can make shoulder pain feel worse than it is
The shoulder rarely complains alone. A forward-jutted neck, an over-flexed wrist, or an elbow dangling off a pillow can magnify discomfort. This is one reason a recliner can feel wonderful for the shoulder but dreadful for the neck. The reverse can happen in a bed. A soft mattress may soothe the spine while letting the arm migrate into nonsense. If that neck component starts becoming its own subplot, it helps to think through broader neck and shoulder pain sleeping positions rather than assuming the postoperative shoulder is the only actor on stage.
Let’s be honest: a bad pillow arrangement can turn either option into a small torture chamber
Most failed setups are not dramatic. They are sloppy. The pillow under the elbow is too low. The wedge is too soft. The head is pushed forward. The sling pillow is there but not actually bearing weight. This is why thoughtful support beats sheer quantity. Ten random pillows can still perform worse than three placed well.
Short Story: A family member preparing for surgery once built what can only be described as a pillow cathedral in the bed: majestic, high, and structurally unserious. It looked comforting in daylight. At midnight, the upper layers slid, the elbow lost support, the shoulder tensed, and the patient woke angry at both gravity and interior design.
The fix was almost boring: fewer pillows, firmer ones, one wedge behind the back, one under the forearm, one along the side to block rolling. Suddenly the room stopped feeling like a panic project and started feeling like recovery. That is often the shift. Not more equipment. Better geometry.
- Early elevation
- Less rolling
- Easier standing
- Contained arm position
- Whole-body comfort
- More room to reposition safely
- Better pressure distribution
- Flexible pillow systems
The Hidden Trade-Off: Recliner Comfort Versus Whole-Body Comfort
Recliners may help the shoulder while irritating the lower back, hips, or neck
This is the classic trade. The shoulder says, “Thank you.” The lumbar spine says, “Absolutely not.” A recliner that fixes one problem can create a new parade of discomfort somewhere else. That does not mean the recliner failed. It means your whole body also expects a vote.
Beds may feel softer overall but create more risk of twisting during sleep
A bed is usually kinder to the rest of the body. Hips, knees, and neck may all prefer it. But softness can invite rolling, and rolling can invite protective reflexes, half-awake reaching, or that dreadful sharp reminder that the shoulder is not available for normal life yet.
Patients with reflux, back pain, or mobility limits may respond very differently to each setup
This is why internet polls are not enough. A patient with reflux may appreciate elevation. A patient with spinal stenosis may hate prolonged recliner posture. Someone with weak legs may need the setup that offers the safest path to standing, even if it is not the most comfortable at rest. Recovery is rarely a single-variable equation. In homes where both shoulder recovery and spine irritation are competing for attention, the practical lessons from managing lumbar fusion car ride pain are oddly relevant: support geometry and transfer mechanics often matter more than the surface itself.
The best setup is sometimes the one your whole body can tolerate for five nights in a row
Night one matters, but night four often decides the winner. Can you keep using this setup without your neck seizing, your hips complaining, or your patience evaporating? Shoulder recovery is long enough already. You do not need to add a second feud with your furniture.
One practical truth: some patients do best with a hybrid plan. Recliner for the first several nights, bed with wedge support after swelling eases a bit. Recovery is allowed to evolve. You are not signing a lifelong treaty with either surface.
- Recliners can create whole-body strain
- Beds can create movement risk
- The winner may change over time
Apply in 60 seconds: Rate both setups from 0 to 10 for shoulder comfort, whole-body comfort, and ease of standing.
Don’t Guess on This: Match the Setup to Your Surgery and Mobility
Rotator cuff repair patients may need more protection from sudden movement
When a repair needs quiet protection, the setup that limits surprise motion often wins. This is one reason a recliner or a tightly supported elevated bed can be useful early. The point is not to freeze the body like museum pottery. The point is to reduce accidental positioning that startles the shoulder into protest.
Labrum, instability, or arthroscopy patients may have different comfort and sling needs
Not every arthroscopic case feels the same. A more minor procedure may still hurt quite a bit at night, while a bigger repair may come with stricter movement protection. The word “arthroscopy” can sound smaller than the actual recovery experience. Tiny incisions do not automatically mean tiny sleep problems.
Patients who cannot push off easily with the non-surgical arm may struggle more in bed
If the good arm is also weak, painful, arthritic, or simply not up to heroics, bed exits become harder. That can tip the decision toward a recliner, a higher bed, or added caregiver support. This is especially true for older adults and for patients who are already moving more cautiously before surgery.
Caregiver availability matters more than most recovery checklists mention
A strong bed setup with a helper nearby can outperform a mediocre recliner. Likewise, a recliner may be safer for someone sleeping alone because it reduces the odds of a clumsy, half-asleep maneuver. Recovery plans often fail because they assume the patient will be at their best exactly when they are least graceful.
Quote-prep list: What to gather before you compare setups or equipment
- Your procedure name and surgeon’s sleep-position instructions
- Sling-at-night rules
- Bed height and whether you have an adjustable base or wedge
- Recliner type, seat depth, armrest height, and ease of standing
- Whether a caregiver will help with transfers during the first week
Neutral action: Make this list before buying wedge pillows, renting equipment, or moving furniture around the house.
Show me the nerdy details
Procedure-specific restrictions can change how much active use of the shoulder is allowed, how long the sling stays on, and how cautious the patient must be during transfers. Mobility also matters beyond the shoulder itself: leg strength, bed height, trunk control, and the condition of the non-surgical arm can all change which setup is genuinely safer.
Common Mistakes That Make Post-Op Pain Harder to Control
Choosing the recliner without testing whether you can safely get in and out of it
Some recliners are soft in all the wrong ways. Deep seats, low height, and awkward lever placement can make standing up harder, not easier. If you sink and then have to claw your way out with your legs and one arm, the chair may be sabotaging the plan.
Choosing the bed without building elevation and arm support before the first night home
Do not leave this for post-op improvisation. The patient will be tired, medicated, sore, and deeply uninterested in engineering. Build the bed setup in advance. Then sit in it. Then lie in it. Then get out of it. Dry runs are not overkill here. They are mercy.
Waiting until pain escalates before taking surgeon-approved medication on schedule
Night pain is easier to prevent than to chase. If your surgeon has given a medication schedule, especially for the first days, do not treat bedtime like a test of character. Stoicism is a poor pillow. A setup that seems impossible may suddenly feel workable when pain control is timed properly. For patients dealing with insurance-heavy orthopedic care, it can also help to understand the bigger picture of orthopedic pain management with an HDHP before the invoices start arriving with their own nocturnal personality.
Assuming the sling alone is enough support while sleeping
The sling helps protect the arm, but it does not replace thoughtful pillow support under the elbow, forearm, and sometimes behind the upper arm or trunk. Unsupported weight can still tug in ways that feel miserable. If you are sorting through what gear is genuinely useful versus decorative, a broader look at orthopedic braces and supports that may be HSA eligible can help frame the decision.
Ignoring how bathroom trips, icing, and medication timing affect the overnight plan
A brilliant setup that turns every bathroom trip into a high-risk event is not brilliant. Think through lighting, footwear, path clearance, and where ice or water will sit. Pain management begins before the pain arrives and before the trip becomes urgent.
- Test rising before surgery day
- Build support before the first night home
- Match medication timing to bedtime, if approved
Apply in 60 seconds: Rehearse one full bedtime-to-bathroom-to-back-in-bed sequence while the shoulder is still calm.
Don’t Do This: Sleep Setup Errors That Quietly Backfire
Do not sleep completely flat if your surgeon advised elevation
Some official post-op instructions specifically warn that lying flat can worsen shoulder discomfort and suggest elevation with pillows or a recliner. If your team told you to stay elevated, do not “just try flat for one night” because you are tired of the chair. Fatigue is persuasive, but not always wise.
Do not keep improvising with unstable pillows that slide away overnight
Support that disappears at 1 a.m. is not support. Look for firmness and friction. Slippery satin may be glamorous, but in recovery it can behave like a tiny betrayal.
Do not remove the sling at night unless your orthopedic team told you to
For many procedures, the sling is part of the overnight protection plan. If you are unsure, ask. Nighttime half-sleep is exactly when people drift into positions they would never choose while fully awake.
Do not force yourself into a setup that causes repeated near-falls when standing up
Near-falls count as data. They are not a character-building opportunity. If a surface repeatedly makes transfers unsafe, it is the wrong setup or the wrong setup for now.
Anyone who has cared for a shoulder surgery patient recognizes this strange phase of recovery: the body is tired, the mind is foggy, and ordinary motions become elaborate projects. That is why quiet risks matter. They tend to arrive disguised as “I can probably manage.”
What a Good Recliner Setup Actually Looks Like
The chair should support a stable, semi-upright angle without forcing the head forward
The right recliner angle is usually not bolt upright and not fully lounged out. You want a supported semi-upright posture that lets the shoulder rest without the chin being shoved toward the chest. If your neck feels like it is auditioning for a separate injury, adjust the angle or add neck support.
Pillows should protect the elbow, forearm, neck, and low back, not just the shoulder
Think in zones. One support zone for the head and neck. One for the low back if needed. One under the elbow and forearm so the shoulder is not carrying weight it does not need to carry. Sometimes a small pillow or rolled towel at the side helps prevent awkward drift. This is less glamorous than buying gear and more effective than buying gear.
A small table, medications, water, and ice supplies should be within easy reach
The best recliner setup includes a landing zone. Water, tissues, phone charger, medication log, and ice should be close enough that the patient does not start inventing dangerous reaches with the non-surgical arm while half asleep.
Nighttime lighting and a safe path to the bathroom are part of pain management too
Pain control is not only pills and ice. It is also preventing the jolt of panic that comes from fumbling in the dark. A soft night light, stable footwear, and a cleared path may do more good than one extra decorative pillow pretending to be useful.
Many families over-focus on the chair and under-focus on the ecosystem around it. But the ecosystem is what turns a chair into a recovery station rather than a lonely piece of furniture with delusions of medical importance.
What a Good Bed Setup Actually Looks Like
Use wedge support or layered pillows to create elevation that does not collapse overnight
A good bed setup usually starts with a firm wedge or a thoughtfully layered pillow base that keeps the torso elevated. The point is not dramatic height. It is reliable height. If the patient slides flat after an hour, the setup is not doing its job.
Protect the surgical arm with side support so it does not drift or pull
The arm needs a place to rest. Support under the forearm and elbow is often the difference between “I slept a little” and “I woke up every hour.” Some patients also do well with a pillow on the surgical side to create a gentle barrier against rolling or drifting.
Make the non-surgical side the easier side for entry and exit when possible
This matters more than most people expect. If the patient can enter and exit from the side that favors the good arm and reduces twisting, the whole bedtime routine becomes less dramatic. Small layout decisions have big consequences at 3 a.m.
Practice the get-up sequence before surgery if you can
Roll slightly, engage the legs, use the good arm as instructed, avoid using the surgical arm to push, and stand in a controlled way. It sounds almost too basic to mention until you see how much distress it saves. A bed is easier to trust when the patient already knows the choreography.
Show me the nerdy details
Bed success usually depends on three variables: elevation, arm support, and transfer mechanics. Adjustable beds improve the first two variables immediately. Standard beds can still work, but low mattress height, soft surfaces, and collapsing pillows often increase trunk effort and uncontrolled shoulder movement during exits.
The Decision Test: How to Tell Which Option Is Better for You
Choose the recliner if lying flat sharply increases pain or getting out of bed feels unsafe
This is the clearest early signal. If flat or nearly flat positions make the shoulder throb, or if bed exits require too much twisting, bracing, or one-armed heroism, the recliner often earns its place. Comfort plus safer transfers is a strong combination.
Choose the bed if you can maintain elevation, protect the shoulder, and rise without twisting
If the bed can reproduce a reclined posture and the exit sequence is controlled, it may be the better long-term option. This is especially true for people whose neck, back, or hips get cranky in a recliner.
Consider using both if your first phase and second phase recovery needs are different
You do not need to crown one winner for the entire recovery. Some patients start in the recliner for several nights or weeks, then transition to the bed once swelling and guarding ease. That is not inconsistency. That is adaptation, which recovery generally appreciates.
The right answer may change after the first several nights as swelling and stiffness shift
A setup that feels impossible on night one may become perfectly workable on night six. Likewise, a recliner that saves the day early may become irritating later. Stay practical. Recovery is a moving target, not a personality test.
Mini calculator: Which setup wins tonight?
Give each setup a score from 0 to 5 in three areas:
- Shoulder comfort
- Ease of standing
- Whole-body comfort
Total score = comfort + standing + whole-body tolerance.
If one setup wins by 3 points or more, that is usually your better choice for tonight. If the scores are close, pick the safer transfer option.
Neutral action: Re-score after three nights rather than assuming the answer stays fixed.
- Use comfort and safety together
- Reassess after the first several nights
- Switch setups when recovery phase changes
Apply in 60 seconds: Score your current recliner and bed instead of debating them in the abstract.
When to Seek Help
Pain suddenly becomes severe and does not improve with prescribed or surgeon-approved measures
Some pain is expected. Pain that suddenly surges, feels dramatically different, or does not respond at all to your approved plan deserves a call.
You notice shortness of breath, chest pain, fever, or signs of infection
Those are not sleep setup issues. They need medical attention promptly.
Your hand becomes numb, cold, unusually swollen, or changes color
Circulation and nerve concerns should never be shrugged off as “probably just how I slept.”
You cannot safely get in or out of your sleeping setup without near-falls
If every transfer feels like a gamble, the setup needs to change or the surgeon’s office needs to guide you. Recovery should be hard enough already.
Your pain plan is not getting you through the night even when followed correctly
Tell your orthopedic team. Night pain that is repeatedly unmanageable may need an adjustment in timing, strategy, or expectations for support. If the medical plan is clear but the billing side is what keeps ambushing you, a careful look at joint injection consultation cost, physical therapy copay vs coinsurance, or even orthopedic pain management after an MRI denial appeal can make the wider recovery picture less foggy.

FAQ
Is a recliner better than a bed after shoulder surgery?
Often early on, yes, especially if lying flat increases pain or if getting out of bed feels unsafe. But “better” is temporary and personal. A well-supported bed, especially an adjustable one, can work very well too.
How long do most people sleep in a recliner after shoulder surgery?
There is no universal number. Some people need it for a few nights. Others prefer it for several weeks. The right timeline depends on the procedure, your surgeon’s instructions, swelling, comfort, and how safely you can transition back to bed.
Can I sleep flat in bed after rotator cuff surgery?
Some patients eventually can, but many are more comfortable elevated at first. Follow your surgeon’s instructions. If you were told to stay elevated or to keep the sling on at night, do not abandon that plan because you are frustrated with the setup.
Why does shoulder pain get worse at night after surgery?
Night pain often rises because of swelling, stiffness, muscle guarding, changing medication timing, loss of arm support, and the challenge of holding one position for longer than your shoulder currently enjoys.
How do I keep from rolling onto my surgical shoulder?
Use positioning barriers. A recliner helps because it limits rolling. In bed, use a wedge behind the back, support under the arm, and sometimes a pillow or body pillow to block drift toward the surgical side. Keep the sling on at night if your surgeon instructed it.
Is an adjustable bed as good as a recliner for shoulder surgery recovery?
For many people, it can be. An adjustable bed can create elevation similar to a recliner while offering better whole-body support. It becomes especially useful if recliners irritate your neck, hips, or lower back.
What pillows help most after shoulder surgery?
The helpful ones are the stable ones. A firm wedge or firm back support, a pillow under the forearm and elbow, and side blocking to prevent rolling often matter more than fancy branding. Slippery, collapsing pillows tend to create more work than relief.
When should I worry that nighttime pain is not normal?
Worry less about “normal” and more about patterns. Seek help if pain becomes suddenly severe, is not improving at all with the approved plan, or comes with fever, drainage, breathing trouble, hand color changes, or alarming numbness.
Next Step
Before surgery or before tonight, test both setups for one full rehearsal: sit down, position pillows, support the arm, stand up safely, and note which option better controls pain without making movement riskier.
That rehearsal is where the vague question finally becomes useful. You stop asking, “Which is better, recliner or bed?” and start asking the question that actually protects you: “Which setup lets me sleep supported and stand up without making my shoulder negotiate with gravity at dawn?” In most recoveries, that is the real answer hiding behind the furniture debate.
If you have 15 minutes, do three things now. First, write down your surgeon’s sleep and sling instructions in plain English. Second, score your bed and recliner for shoulder comfort, exit safety, and whole-body comfort. Third, stage the environment: pillows, water, medication plan, charger, night light, and a clean path to the bathroom. It is not glamorous. Neither is shoulder surgery. But this kind of quiet preparation often buys the most relief.
Last reviewed: 2026-03.
