
Protecting Your Mobility: A Warehouse Worker’s Guide to Knee Health
By the time most warehouse workers start searching for orthopedic pain management, the knee has already been sending invoices for weeks.
First, it complains after a shift. Then stairs get rude. Finally, one low pick from a bottom shelf feels like the joint has hired legal counsel. The real problem isn’t just the ache, it’s the reality of a job that demands squatting, pivoting, and concrete-floor endurance while your body is quietly negotiating its limits.
Without a clear strategy, bad self-diagnosis is dangerously easy. Overuse, patellofemoral pain, and meniscus irritation blur together, risking a manageable problem turning into a costly, long-term interruption.
What actually helps is a smarter map: understanding which pain patterns signal overload, identifying signs that require medical attention, and adopting work-aware tools or job modifications.
Stop treating every knee problem like the same old ache. Not all sore knees are telling the same story, and the difference matters before your next shift turns a warning into a setback.
Table of Contents
Safety / Disclaimer: This article is for general education, not personal medical advice. Knee pain in warehouse work can come from overuse, strain, arthritis, meniscus problems, tendon irritation, bursitis, or injury. Pain relief strategies, work restrictions, imaging needs, and return-to-work decisions should be guided by a licensed clinician who can evaluate your specific symptoms, job demands, and medical history.
Start Here First: Who This Is For / Not For
This is for you if long shifts, lifting, squatting, stairs, or concrete floors make your knee pain worse
If your pain seems to follow the rhythm of work, that matters. Warehouse knee pain often has a load pattern. The knee may feel tolerable during the first hour, grumpy by lunch, and openly hostile by the final two hours. That pattern does not automatically mean the damage is severe, but it does mean your knee is reacting to demand. The reaction can come from irritated soft tissue, poor recovery, a movement problem, arthritis, or a structure that has finally decided it has had enough.
This is for you if you are trying to stay functional at work while figuring out what is actually causing the pain
Plenty of people are not asking, “How do I become a knee scholar?” They are asking, “How do I survive Thursday?” Fair. But the tricky thing is that surviving the week and solving the problem are related, not identical. A good orthopedic-style plan protects function while also narrowing down the likely cause. That is where better decisions begin.
This is for you if you want practical, orthopedic-style options beyond “just rest and hope”
Rest can help. It can also become a vague, unhelpful shrine people kneel before while nothing improves. Warehouse workers often cannot fully rest anyway. Rent remains theatrically unconcerned about tendon irritation. What helps more is targeted load reduction, smarter symptom tracking, supportive equipment when appropriate, and clinician input when the pattern suggests something more than temporary overload.
This is not for you if the knee looks deformed, gives out suddenly, locks, or you cannot bear weight
Those symptoms move the problem out of the “let’s observe and adjust” bucket and into “get evaluated” territory. Sudden inability to bear weight, severe instability, or a locked joint can point to injury patterns that need faster assessment.
This is not for you if you have fever, major swelling after trauma, calf swelling, or pain that feels urgent
Urgent symptoms deserve urgent care. MedlinePlus notes that knee pain can come from injury, infection, arthritis, and other causes, and symptoms such as significant swelling, redness, or inability to use the joint should not be shrugged off.
- Track what motions trigger pain
- Notice swelling, locking, or instability
- Treat urgent symptoms as urgent
Apply in 60 seconds: Write one sentence: “My knee hurts most when I ________.” That sentence is the seed of a better plan.
Before You Treat It: What Kind of Knee Pain Are You Actually Dealing With?
Front-of-knee pain that flares with stairs, kneeling, or repeated bending
Pain at the front of the knee often gets lumped into the vague swamp of “bad knees,” but the pattern matters. Front-of-knee pain that worsens with stairs, crouching, or getting up after sitting can show up when the tissues around the kneecap are irritated. AAOS describes patellofemoral pain as pain sensed around the kneecap and nearby soft tissues, which is one reason repeated bending and loaded knee flexion can feel so annoying.
I once knew a worker who described this pain as “the forklift isn’t what squeaks, I am.” Not elegant, but useful. It captured something true: the pain showed up not in one dramatic incident but in repetitive, everyday motions that kept poking the same region.
Inner or outer knee pain that appears with twisting, pivoting, or getting up from a crouch
This pattern raises different questions. Twisting, pivoting, or standing up from a deep crouch can irritate structures on either side of the joint. Sometimes it is a strain. Sometimes it is a meniscus issue. Sometimes it is the mechanical result of doing the same awkward movement 150 times a shift. Location alone will not solve the mystery, but location plus trigger plus timing gets you much closer.
Pain with swelling, stiffness, and the “rusty hinge” feeling after sitting
This often makes people think, “I’m too young for arthritis,” which is a sentence knees never asked for. Arthritis is not the only explanation, but gradual pain, swelling, and stiffness can point toward degenerative or inflammatory patterns rather than a simple irritated tendon. AAOS notes that knee arthritis commonly develops gradually and may involve pain, inflammation, and stiffness. In some cases, readers also benefit from understanding how knee arthritis exercise choices can affect symptom tolerance when lower-body pain patterns start to overlap.
Sharp pain under load versus dull pain that builds across the shift
Sharp pain when you load the knee usually gets your attention fast. Dull pain that builds slowly is easier to dismiss, which is exactly why people dismiss it for too long. A sharp jab during one movement may suggest a more specific mechanical trigger. A dull ache that climbs with cumulative work may fit overload, poor shock absorption, or an irritated structure that is being asked to repeat the same complaint all day.
Here’s the catch: the same warehouse task can irritate very different structures
Two workers can both hate stairs for completely different reasons. One may have front-of-knee pain from repetitive loaded bending. Another may have joint-line pain and swelling after twisting. A third may have arthritis that resents every hard surface in the building. This is why copying a coworker’s brace or YouTube routine is a little like borrowing someone else’s glasses and insisting the blur is character-building.
Show me the nerdy details
Orthopedic evaluation often starts with pain location, aggravating motion, onset pattern, swelling, instability, range of motion, and mechanical symptoms such as catching or locking. None of those alone makes a diagnosis. Together, they help separate tendon overload, patellofemoral irritation, arthritis, bursitis, ligament issues, and possible meniscal injury.
Shift Pain or Structural Problem? The Clues That Change the Plan
Pain that eases on days off versus pain that lingers no matter what
If your knee feels noticeably better after one or two days off, that leans toward a load-sensitive problem. It does not prove the issue is minor, but it suggests the knee is reacting to demand. If pain stays the same regardless of workload, or continues to worsen despite rest and adjustment, the plan changes. That is when a more formal evaluation becomes more useful.
Swelling after work, morning stiffness, and the difference between overload and injury
A little soreness after a rough shift is common. Recurrent swelling is not something to normalize forever. Swelling means the joint or nearby tissues are reacting. Morning stiffness can show up with arthritis, inflammation, or a knee that is being overworked and under-recovered. Significant swelling after a twist, pop, or misstep deserves more caution than the everyday ache that slowly simmers after repetitive squats.
Clicking is common, but locking is a different story
Many knees click. Some knees sound like a snack bag being folded in a quiet room. Clicking without pain can be harmless. But true locking, where the knee cannot move normally or feels mechanically stuck, is different. That symptom belongs in the “get assessed” pile, not the “I’ll buy better socks and see” pile.
Let’s be honest… many workers normalize red-flag symptoms for too long
This is not because they are careless. It is because workplaces can train people into symptom minimalism. If you work around speed metrics, staffing shortages, and a culture that celebrates powering through pain, you can slowly lose your sense of what deserves medical attention. By the time someone says, “I guess this isn’t normal,” the knee has often been dropping hints for months.
- Days-off improvement is a clue
- Swelling changes the seriousness
- Locking and giving way deserve faster attention
Apply in 60 seconds: Think back over your last two days off. Did your knee clearly calm down, barely change, or get worse?
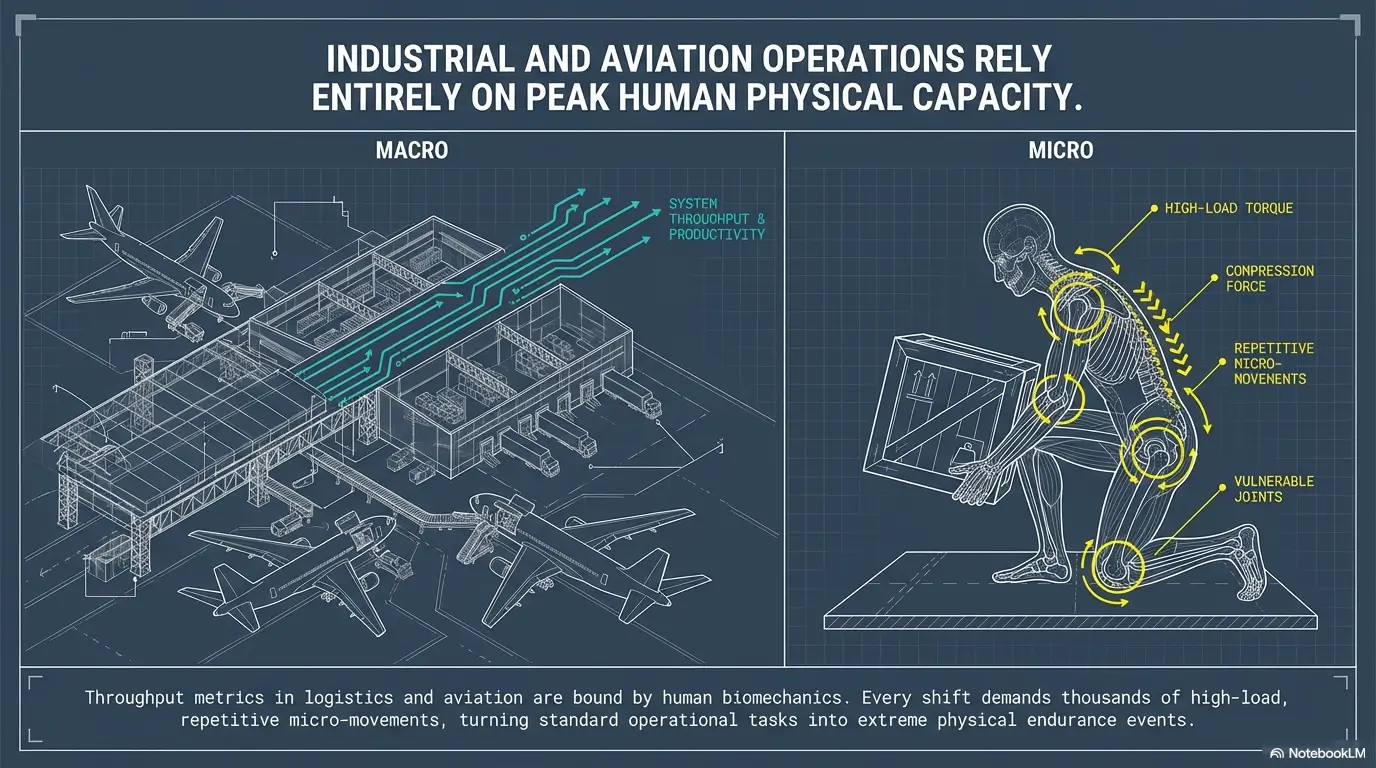
Workday Triggers First: Why Your Knee May Hurt More at the Warehouse Than Anywhere Else
Repeated squatting, pallet work, low picking, and awkward turns
Warehouses create perfect little obstacle courses for knees. Low picking means repeated flexion. Pallet work means forward reach plus partial squat plus rotation. A rushed turn with a planted foot can irritate the joint in ways ordinary walking never does. The task itself matters just as much as the diagnosis. A plan that ignores the task will feel thoughtful and fail anyway.
Concrete floors, poor shock absorption, and cumulative irritation
Hard floors turn small mechanics problems into loud ones. Poor shock absorption from worn footwear or thin insoles can increase how much force your body has to manage across a long shift. It is not magic. It is accumulation. One step is nothing. Ten thousand is an editorial.
Long standing versus stop-start walking versus heavy carries
Not all warehouse pain comes from the same type of demand. Long standing can increase stiffness and dull ache. Stop-start walking can flare irritation around the kneecap. Heavy carries can magnify compressive load, especially if form gets sloppy when fatigue arrives. When someone says, “My knee hurts at work,” the next useful question is, “During what exact kind of work?”
Speed pressure, understaffing, and why “pushing through” often backfires
NIOSH materials on workplace musculoskeletal risk repeatedly emphasize ergonomics, risk-factor identification, worker involvement, and recovery rather than simple grit narratives. In plain English: the body does not care about a supervisor’s optimistic timing spreadsheet. Repetition, awkward posture, force, and limited recovery matter.
One of the most revealing things you can do is name the specific point in the shift where mechanics deteriorate. For many workers, the first three hours are fine, the next three are compromised, and the last two are where compensations arrive wearing a fake mustache and pretending to be productivity. Similar work-design thinking also shows up in guides on musculoskeletal pain at warehouse jobs, where repeated load, hard floors, and rushed movement patterns create cumulative trouble faster than people expect.
Infographic: The Warehouse Knee Pain Cycle
Squats, pivots, hard floors, stairs, heavy carries
Front-knee pain, joint-line pain, swelling, stiffness
Limping, altered lifting, avoiding depth, slower recovery
Diagnosis, workload changes, rehab, support, follow-up
Best use: Find the earliest box where you can realistically interrupt the cycle before symptoms snowball.
Decision card: When is it probably a workload problem versus something that needs quicker evaluation?
| Pattern | Leans toward | Neutral action |
|---|---|---|
| Pain worsens during shift, eases with time off | Load-sensitive irritation | Track triggers and reduce repeated aggravating tasks |
| Swelling after twist, pop, or pivot | Possible injury pattern | Arrange clinical evaluation |
| Giving way, locking, or inability to bear weight | Red-flag mechanical issue | Seek urgent assessment |
Next step: circle the row that fits your last bad shift best.
Pain Relief Is Not the Whole Game: What Orthopedic Management Usually Includes
Short-term symptom relief versus fixing the load pattern causing the pain
Orthopedic pain management is not just about “What reduces pain today?” It is also about “What keeps this from becoming a larger problem next month?” Symptom relief matters. Nobody becomes wiser by hobbling theatrically through a 10-hour shift. But pain reduction without diagnosis or workload change can let a worker move more comfortably into worse mechanics. For readers navigating insurance friction as part of that process, this broader guide to orthopedic pain management with an HDHP can help frame the practical side of getting care.
When bracing, taping, sleeves, or compression may help function
Supportive tools can help some workers feel more stable or more aware of the knee. A sleeve may provide warmth, light compression, and a sense of support. A more structured brace may be used for specific diagnoses. The error is assuming all support is good support. The right device depends on the problem. Random brace shopping at 11:40 p.m. after a brutal shift can feel productive, but it is often just retail therapy with Velcro. If cost or account eligibility is part of the decision, it can also help to review how orthopedic braces and supports fit HSA eligibility rules.
When physical therapy matters more than another week of guessing
Physical therapy is often where the useful boring stuff happens: strengthening, movement retraining, mobility work, load progression, and figuring out which tasks provoke symptoms. AAOS notes that a well-structured knee conditioning program can help reduce stress on the joint by strengthening supporting muscles and improving function.
I have seen people spend four weeks comparing insoles online when what they really needed was guidance on quad strength, hip control, and how to stop dropping into the same painful squat pattern 200 times a day. Gear matters. Rehab often matters more. If budget questions are slowing you down, understanding physical therapy copay versus coinsurance can make the next step feel less foggy.
When imaging may be discussed after exam findings and symptom pattern
Imaging is not a prize for suffering. It is a tool. Clinicians usually decide whether imaging is useful based on the history, exam, swelling, trauma, instability, mechanical symptoms, and how the problem has behaved over time. Some knee pain improves with targeted conservative care and never needs imaging. Some patterns clearly deserve it sooner. When that conversation stalls, this explainer on what “failed conservative care” means for MRI approval can help readers understand the paperwork logic behind the delay.
Here’s what no one tells you… pain control without workload changes can hide a worsening problem
This is one of the most important ideas in the whole article. If a worker uses pain relief only to keep performing the same aggravating mechanics, the knee may feel temporarily better while the workload problem stays intact. The goal is not moral purity. It is accurate feedback. Your body needs at least some chance to tell the truth.
- Pain control helps, but it is not the whole answer
- Braces should match the problem
- Physical therapy often turns vague frustration into a plan
Apply in 60 seconds: Ask yourself whether your current strategy changes the cause, or only mutes the signal.
The Job-Safe Toolkit: Work-Aware Options That May Reduce Knee Stress
Footwear support, insoles, and shock management for hard floors
Hard floors are famous for making small lower-body issues louder. Footwear with better cushioning, stable support, and a less worn-out midsole may help some workers tolerate long shifts better. Insoles can also help, especially when the current shoe has gone soft, flattened, or uneven. This is not glamorous advice. Neither is changing your windshield wiper blade, yet both can prevent absurd amounts of avoidable suffering.
Knee sleeves, braces, and when support helps versus irritates
A sleeve can be useful if it improves comfort and confidence without causing bunching, skin irritation, or false security. A hinged or more structured brace should usually follow a clearer diagnosis or clinician recommendation. If the brace makes you move differently in a way that feels worse after a shift, it may not be helping as much as you hoped.
Cart use, lift strategy, and reducing deep knee bend frequency
Even small task modifications matter. A cart used more often. A load staged higher. A turn done with the feet rather than a planted twist. Fewer deep knee bends when a hip hinge or alternate setup works. None of this sounds heroic. That is exactly why it works. Good joint protection often looks embarrassingly ordinary.
Rotation, micro-breaks, and task sequencing that buys your knee some breathing room
Task variety can reduce how much one movement pattern hammers the same tissues all shift long. Even short micro-breaks, especially if they interrupt repetitive loaded bending or prolonged standing, may reduce cumulative irritation. The best sequence is often not “do the hardest knee-demanding task until your body files a protest” but “spread demand before fatigue wrecks mechanics.”
Ice, elevation, and recovery habits after a punishing shift
Recovery is not glamorous either, but it counts. If swelling is part of the pattern, cooling the area, elevating the leg when appropriate, and giving the knee a chance to settle can help symptom control. MedlinePlus notes that for non-arthritic joint pain, both rest and exercise can matter, and common home-care approaches may include stretching and appropriate medication guidance.
Quote-prep list: If you are comparing braces, insoles, or therapy options, gather these first.
- Your pain location: front, inner, outer, or behind the knee
- The three tasks that trigger symptoms fastest
- Whether swelling, stiffness, or instability shows up
- Your shoe type and how old your current work shoes are
- Whether symptoms ease with 1 to 2 days off
Next step: bring this list to a clinician, PT, or product comparison so the advice fits your actual workday.
Medication Mistakes at Work: Don’t Trade Today’s Shift for Tomorrow’s Worse Pain
Using pain relief only to push through unsafe mechanics
This is the classic trap. Relief becomes permission. The worker feels 30 percent better and immediately spends that improvement on the same workload pattern that caused the problem. Medication can absolutely have a role, but when it simply enables worse mechanics for longer, it is doing an incomplete job.
Doubling up on over-the-counter medications without checking ingredients
Over-the-counter does not mean consequence-free. Workers sometimes stack products without realizing they contain overlapping ingredients. Others take more than directed because the shift is long and the body is louder than the label. That is a good way to trade one problem for another.
Ignoring drowsiness, dehydration, stomach issues, or blood pressure concerns
Some medications can raise risks that matter on the job. If a product increases drowsiness, stomach irritation, dehydration risk, or blood pressure concerns, that matters more when the work involves heat, long hours, driving equipment, or limited break opportunities. MedlinePlus advises discussing NSAID use and other medication choices with a clinician when relevant, rather than assuming more is safer.
Assuming “if it helps, more is better”
The body is not a customer service line where volume guarantees satisfaction. With medication, more can mean more risk rather than better function. If you regularly need medication just to perform a normal shift, that is not only a symptom problem. It is information.
Eligibility checklist: Are you relying on medication in a way that deserves a plan upgrade?
- Yes / No: I need pain relief before most shifts
- Yes / No: I use it mainly to keep doing the same painful tasks
- Yes / No: I have not reviewed the ingredients or warnings recently
- Yes / No: I have swelling, locking, or instability in addition to pain
Next step: if you answered “Yes” to 2 or more, move from self-management to a clinician-guided strategy.
Don’t Do This: Common Mistakes Warehouse Workers Make With Knee Pain
Waiting until the knee swells every day before taking it seriously
People often wait for repeat swelling before they admit the issue is real. By then the pattern is more established, compensation habits are more ingrained, and frustration is higher. Earlier attention usually creates better options.
Wearing any brace without knowing what problem it is supposed to solve
The knee-brace aisle can make anybody feel like recovery is one strap away. But a brace should solve a problem, not create a costume. If you do not know whether you need compression, stability, unloading, or simply a reminder not to move recklessly, you may end up with discomfort and false confidence.
Resting hard for two days, then returning at full intensity
This is a favorite pattern because it feels productive. Total rest, then total ambition. The knee often disagrees. A more useful return is usually gradual, with attention to volume, depth of bend, lifting pattern, and shift length when possible.
Blaming age when the real issue may be task design or movement pattern
Age can matter. So can conditioning, prior injury, and joint wear. But do not let “I’m getting old” become a fog machine that hides obvious triggers like deep repetitive squatting, bad shoes, hard floors, awkward turns, and poor recovery. Sometimes the problem is not age. Sometimes it is that the body has become an accountant and is finally itemizing the bill.
Using someone else’s diagnosis as your template
Your coworker’s “meniscus thing” is not automatically your meniscus thing. Shared job duties do not guarantee shared pathology. Similar pain words can come from different structures. That is why symptom pattern and exam still matter.
- Do not normalize swelling or giving way
- Do not buy support without a reason
- Do not confuse temporary relief with readiness
Apply in 60 seconds: Pick one habit from this section that you are currently doing and write its replacement.
When the Floor Fights Back: How to Talk to a Clinician in a Way That Gets Better Care
Describe the exact tasks that trigger pain, not just the pain score
“It hurts a lot” is honest but incomplete. “It spikes when I squat below parallel to pull cases from the bottom rack, especially after hour six” is far more useful. Orthopedic and rehab decisions improve when the job description becomes concrete.
Mention squatting depth, lifting frequency, stairs, pivoting, kneeling, and walking distance
Task detail matters because different movements load the knee differently. If you climb stairs 20 times a shift, say that. If the pain shows up after repeated kneeling or carrying loads over a certain distance, say that. Clinicians cannot infer your warehouse choreography from the word “physical job.”
Track swelling, instability, stiffness, and how long symptoms last after work
This is where many visits become dramatically better. Tell them whether the knee swells only after work or also at rest. Tell them if it feels unstable or catches. Tell them if stiffness is worst in the morning, after sitting, or at the end of the day. Those details help sort overload from arthritis from injury patterns.
Bring a workday timeline so the visit reflects real job demands
One of the smartest things you can bring is a mini timeline: when pain starts, what task triggers it, whether swelling appears, and what recovery looks like by the next morning. It takes maybe five minutes to record and can make the visit far more specific.
Mini calculator: Estimate your knee-demand stack for one shift.
Input 1: Number of deep bends or squats you do in a shift
Input 2: Hours spent on concrete
Input 3: Number of times pain hits 5/10 or higher
Output guide: If all three numbers are high, self-management alone is less likely to be enough. If one number is high, task redesign may buy quick relief.
Next step: bring these three numbers to your next appointment.
Short Story: A worker I once interviewed for a similar topic kept telling his clinician, “It hurts when I work.” That produced generic advice. On the next visit, he brought a note: pain started around hour four, spiked during low picking, worsened after carrying uneven loads, and calmed somewhat if he could rotate to a higher station for 30 minutes. Same knee. Same job.
Entirely different conversation. Instead of another vague “take it easy,” he left with a clearer rehab plan, better recommendations for work modification, and a more realistic return-to-duty path. The lesson was not that notebooks are magical. It was that detail creates traction. Pain described as fog gets foggy answers. Pain described as a pattern gets a plan.
When to Seek Help: Red Flags You Should Not Tough Out
You cannot bear weight or the knee gives out unexpectedly
A knee that suddenly refuses weight or collapses is not asking for inspirational quotes. It is asking for assessment. Sudden instability can accompany injuries that need prompt attention.
The joint locks, catches severely, or loses range of motion
Severe catching or true locking deserves evaluation because mechanical symptoms can point to problems beyond ordinary soreness. This is especially true if the knee physically will not move the way it normally does.
Swelling becomes significant, recurrent, or follows a twist or pop
Swelling is one of the most under-respected clues. Recurrent swelling after work is worth noting. Swelling after a twist, pop, or pivot deserves more urgency. MedlinePlus and AAOS both describe swelling as a meaningful symptom across many knee conditions, not a quirky personality trait of the joint.
Pain wakes you at night or keeps getting worse despite reduced load
If pain ignores your attempts to reduce workload and continues climbing, that weakens the argument that this is a simple temporary irritation. Night pain is not a diagnosis by itself, but it is one more reason not to keep improvising forever.
You notice calf swelling, fever, redness, or other urgent symptoms
Those symptoms belong outside the self-management lane. Infection, vascular issues, or other urgent conditions are not warehouse badges of honor. They are reasons to get help.
Show me the nerdy details
Red flags matter because knee pain is not one disease. When clinicians hear inability to bear weight, rapid swelling after trauma, locking, calf swelling, fever, or progressive loss of motion, the risk calculation changes. That affects how quickly imaging, referral, or urgent assessment may be considered.
The Return-to-Work Trap: Feeling Better Is Not the Same as Being Ready
Less pain at rest does not always mean load tolerance is back
This is one of the nastiest little tricks in recovery. The knee feels better on the couch. Confidence returns. Then the worker meets eight hours of concrete, turning, lifting, and low-level fatigue, and the truth comes back wearing steel toes. Pain at rest and tolerance under load are related, but they are not twins.
Why first shift back is often the real test
The first shift back often reveals what normal life hides. You may tolerate light walking just fine and still flare during repeated deep bends or long standing. That does not mean recovery failed. It means the test got more specific. Progress needs exposure that is smart, not heroic.
Modified duty, gradual ramp-up, and protecting progress
Modified duty is not weakness. It is strategy. A gradual ramp-up, fewer deep bends, less twisting, better task rotation, or temporary changes in carrying demands can protect progress while the knee rebuilds tolerance. This is often where good communication between worker, clinician, and employer matters most. When workplace paperwork becomes part of the problem, some readers find it useful to review broader guidance on how accommodation letters are framed for musculoskeletal pain before discussing modified duty.
Let’s be honest… re-injury often happens on the “I think I’m fine now” week
Because pain has dropped, people assume capacity has returned equally. Sometimes it has. Sometimes the knee has merely become quieter. That is why structured rehab, progressive demand, and honest symptom tracking beat optimistic improvisation.
Coverage tier map: What changes from Tier 1 to Tier 5 recovery readiness?
- Tier 1: Pain at rest, swelling, poor tolerance for normal walking
- Tier 2: Basic walking okay, shifts still flare symptoms quickly
- Tier 3: Light duty tolerated, deep bends and long standing still limited
- Tier 4: Most work tolerated with careful pacing and support
- Tier 5: Full shift tolerated without swelling, giving way, or late-day breakdown
Next step: mark your current tier honestly before increasing workload.
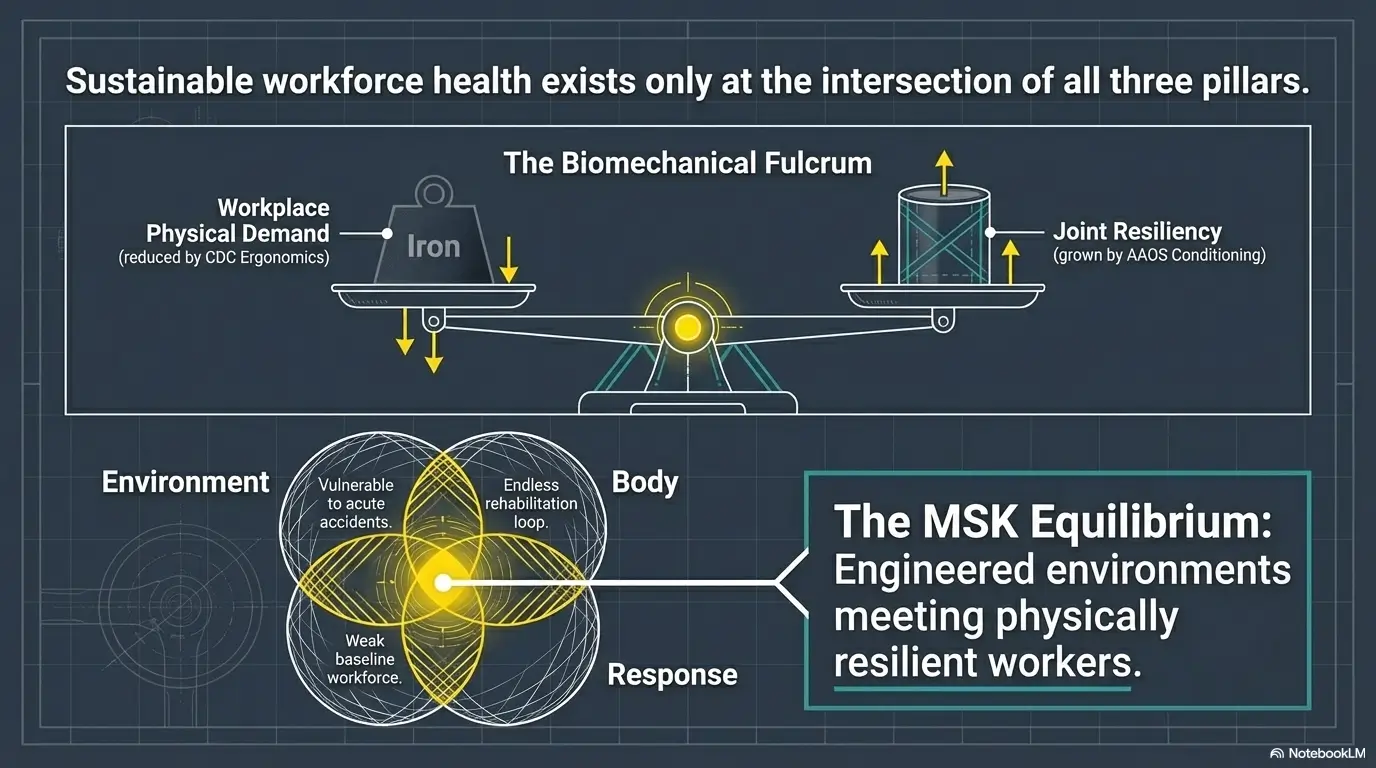
FAQ
Can I keep working a warehouse job with knee pain?
Sometimes yes, but that depends on the cause, your symptoms, and whether work modifications are possible. If pain is mild, load-sensitive, and improving with smarter pacing or support, some workers can continue while they get evaluated and start rehab. If you have swelling, instability, locking, or worsening pain, continuing unchanged is harder to defend.
When is knee pain serious enough to see an orthopedic specialist?
It is reasonable to seek orthopedic or sports-medicine evaluation when pain persists despite conservative steps, keeps interfering with shifts, involves recurrent swelling, or includes instability, locking, major stiffness, or loss of function. Urgent symptoms such as inability to bear weight or fever require faster care.
Is a knee brace actually useful for warehouse work?
It can be, but only when the type of support matches the problem. A sleeve may improve comfort for some workers. A more structured brace may help in specific cases. The wrong brace can irritate the skin, alter mechanics, or give false confidence without solving the underlying issue.
Should I walk more or rest more when my knee hurts after a shift?
The answer is often “both, but intelligently.” Too much total rest can make some knees stiffer and weaker. Too much activity can keep symptoms stirred up. Many people do better with relative rest from the aggravating motions, while keeping tolerable movement and rehab exercises in the plan.
What is the difference between overuse knee pain and a meniscus problem?
Overuse pain often follows repetitive demand and may improve with time off, pacing, and rehab. Meniscal or other structural issues may be more likely when twisting, pivoting, swelling, catching, or locking are part of the pattern. But symptom overlap is real, so diagnosis should not rely on internet archeology alone.
Can concrete floors really make knee pain worse?
Yes, they can worsen tolerance for some workers by increasing cumulative stress across long shifts, especially when footwear support is poor or the job involves prolonged standing and heavy repetition. Hard surfaces are not the only factor, but they are often a meaningful one.
Is swelling after work normal or a warning sign?
Some temporary irritation can happen after heavy demand, but repeated swelling is a sign worth respecting. Significant swelling, swelling after a twist or pop, or swelling with instability should raise the urgency of evaluation.
What should I tell a doctor if my knee only hurts during certain tasks?
Be specific: name the task, the motion, the point in the shift when pain starts, whether swelling follows, and what makes it better or worse. “Low picking after hour five” is much more useful than “It hurts sometimes.”
Next Step: Do This Before Your Next Shift
Write down three specific triggers: the task, the motion, and when the pain starts
Not “work hurts.” Better than that. Try: “Pain starts during low picking after about 90 minutes,” or “Stairs with a load trigger sharp pain at the front of the knee.” Specificity creates leverage.
Note whether swelling, stiffness, locking, or instability appears during or after work
This is where patterns become visible. Symptoms that show up only during the shift tell one story. Symptoms that linger into the next morning tell another. Mechanical symptoms tell a louder one.
Bring that record to a clinician or physical therapist so the plan matches your actual job
The curiosity loop from the beginning closes here. The smarter workday survival guide is not one miracle product, one magical stretch, or one heroic act of willpower. It is a better map. When you understand the pattern, you stop treating your knee like a random betrayal and start treating it like a system under load.
In the next 15 minutes, do one small thing: make a three-line note in your phone with your top trigger, whether swelling happens, and what one work modification seems most realistic. That tiny record can turn a vague problem into a useful appointment, a better brace choice, or a smarter first week of rehab. And that is often how the bigger fix begins, quietly, before the next shift even starts.
Last reviewed: 2026-03.
