
Smarter Dosing: Mastering Sciatica & Knee Arthritis
The biggest mistake isn’t picking the wrong move. It is picking one that feels fine now but charges interest tomorrow. When back and knee symptoms alternate, treating them as separate problems is why most routines fail.
“Track what happens tomorrow morning, then adjust today’s plan. That single habit turns random flare cycles into measurable progress.”
- ✔ Nerve-Calming Mobility
- ✔ Neutral-Spine Core Work
- ✔ Hip & Glute Strength
- ✔ Knee-Friendly Cardio
Shift from “Harder Workouts” to Smarter Dosing.
With both sciatica symptoms and knee osteoarthritis, the winning strategy is low-impact, symptom-guided training: neutral-spine core work, hip/glute strengthening, gentle nerve-friendly mobility, and knee-friendly cardio like cycling, pool walking, or flat walks. Avoid deep knee flexion, high-impact drills, and aggressive “stretch through tingling” moves. Use a 24-hour rule: if pain spikes later or next day, reduce range, load, or duration.
Table of Contents

Why “Back vs Knee” Thinking Fails Fast
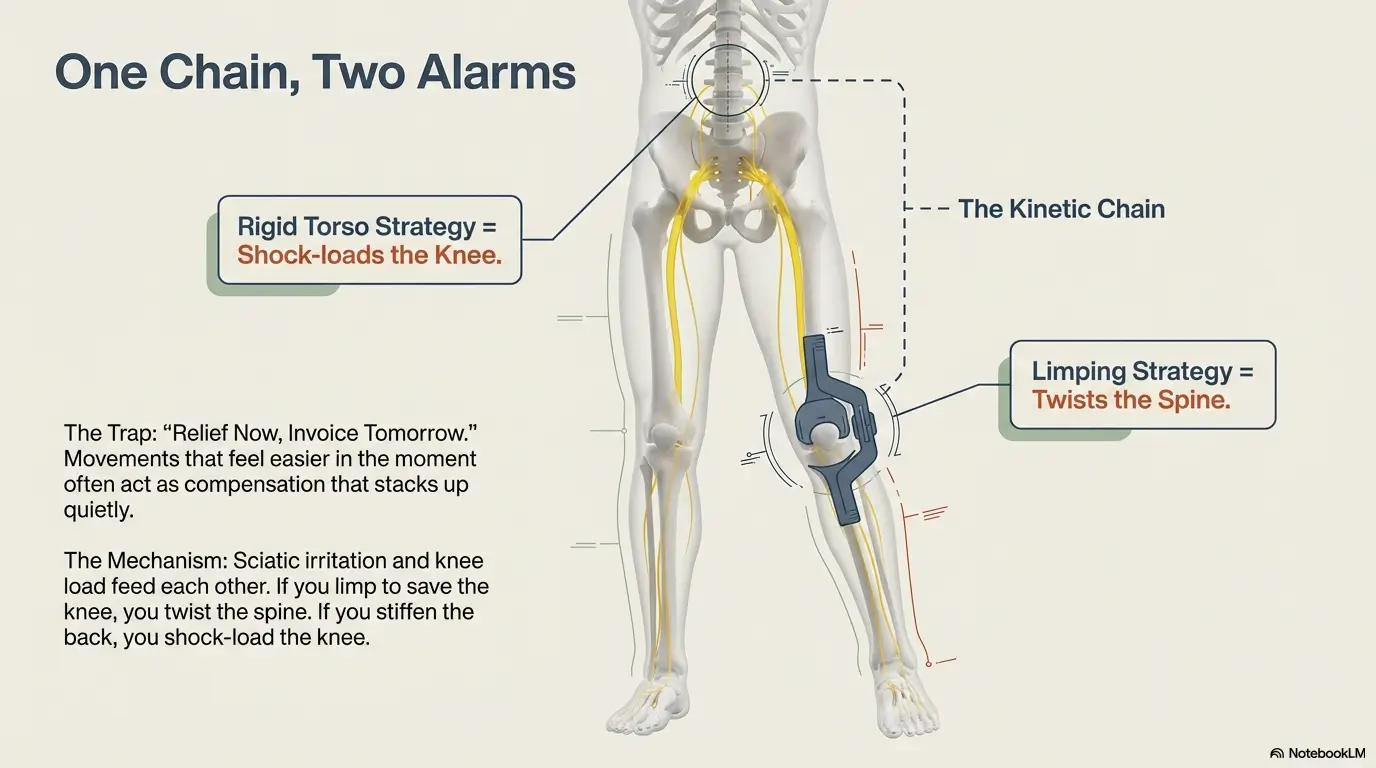
One chain, two alarms: sciatic irritation and knee load feed each other
Your body is not a set of isolated parts with separate customer service lines. If your knee hurts, you may shorten your stride, rotate your pelvis differently, and stiffen your trunk. That change can increase stress through the low back and nerve-sensitive tissues. If your back flares, you may unload one leg and shift knee loading. Different symptom, same movement chain.
I learned this the hard way on a week I tried to “protect my knee” by babying it. By Friday, my low back felt like a locked suitcase and my calf buzzed on stairs. The problem was not weakness alone. It was compensation stacking up quietly in the background.
Pain map triage: where symptoms start vs where compensation shows up
Track two things, not one:
- Primary signal: where symptoms first appear during activity.
- Compensation signal: where discomfort appears later or next morning.
If discomfort appears in a new area 6 to 24 hours later, your current dose is probably too high or your mechanics need adjustment. This one shift in tracking catches problems earlier than “How do I feel right now?” ever will.
Open loop: the movement that feels easier now but costs you tomorrow
Some movements give instant relief by avoiding the painful range, but they secretly increase stiffness elsewhere. The classic example is moving with a rigid torso to spare the back, then overloading knees during sit-to-stand and stairs. Relief now, invoice tomorrow.
- Track primary pain during exercise and compensation pain next day.
- Adjust dose before adding new exercises.
- Prioritize consistent, tolerable movement over dramatic sessions.
Apply in 60 seconds: Start a note titled “Today vs Tomorrow” and log one line after each workout.
Safety First Filter: Who This Is For / Not For
This is for: stable symptoms, walking tolerance, no progressive neurologic signs
This guide fits people with recurring but stable symptoms, mild to moderate activity tolerance, and the ability to modify movement without severe symptom escalation. If you can walk short distances, perform gentle home exercises, and recover to baseline within a day, you are likely in the right place to use this plan.
Not for: acute trauma, rapidly worsening weakness, bowel/bladder red flags
If symptoms include progressive leg weakness, sudden foot drop, numbness in saddle area, or changes in bowel/bladder control, skip self-experimentation and seek urgent medical evaluation. If you had recent trauma, fever, unexplained weight loss, or night pain that doesn’t settle, get assessed before loading any routine.
Pattern interrupt: “If your leg feels numb, do not push through this”
“No pain, no gain” belongs in old gym posters, not nerve-sensitive rehab. With sciatica patterns, sharp, electric, spreading, or numbing symptoms are not a badge of effort. They are a feedback alert. Reduce range, reduce load, or stop and reassess.
- Can you walk 5 to 10 minutes on flat ground without major symptom escalation? Yes/No
- Do symptoms return near baseline within 24 hours after light activity? Yes/No
- No progressive weakness, no bowel/bladder changes, no saddle numbness? Yes/No
Neutral next action: If any answer is “No,” prioritize clinician review before progressing load.
Pick Your Starting Lane in 2 Minutes
Lane A (flare week): pain-calming mobility + isometrics
Use this when morning stiffness is high, symptoms spike quickly, or walking tolerance is low. Goal: calm tissue irritability while keeping movement rhythm alive. Think short sessions, small range, slower tempo. Your mission this week is to preserve function, not “catch up.”
Lane B (rebuild week): controlled strength + short cardio blocks
Use this when symptoms are present but manageable. You can do daily tasks with some modifications, and you recover by next day. Add controlled strengthening and low-impact cardio intervals. Progress comes from repeatability, not heroics.
Lane C (maintenance): progression with symptom caps
Use this when symptoms are mild, stable, and predictable. You can progress one variable at a time: range, then reps, then load, then speed. Keep a ceiling rule: no symptom jump that persists beyond next morning.
Open loop: why your best lane can change by evening
Sleep quality, stress, and cumulative sitting can shift your lane within a single day. Morning Lane B, evening Lane A is normal. Flexible programming beats rigid plans every time.
When A: Pain-reactive day, low tolerance, protect consistency.
When B: Stable enough for controlled loading, rebuild capacity.
When C: Mostly stable week, progress one dial at a time.
Time/cost trade-off: A feels “small” but prevents lost days; C grows fitness but only if recovery stays predictable.
Neutral next action: Choose today’s lane before exercise, not during panic halfway through.
Nerve-Calm Moves That Don’t Provoke the Knee
Supine sciatic nerve glides (small range, no ballistic tension)
Lie on your back with one hip flexed comfortably, hands behind thigh. Slowly extend and bend the knee through a gentle range while flexing and pointing the ankle lightly. Keep the movement smooth, 6 to 10 reps, 1 to 2 sets each side. You are aiming for glide, not stretch heroics. If you want a dose-specific troubleshooting guide, see morning sciatica nerve glides and what to modify first.
If tingling increases and lingers, reduce range or stop. Nerve glides should feel like a gentle conversation, not an argument. If nerve flossing consistently makes symptoms worse later, review why sciatic nerve flossing can backfire before increasing reps.
Supported pelvic tilts and breathing for lumbar decompression
On your back with knees bent, inhale into ribs, exhale and gently flatten lower back, then release to neutral. 6 to 8 breaths per set, 2 to 3 sets. This pairs spinal control with breath-driven downregulation, which helps when pain has turned your nervous system volume too high. On highly reactive nights, a brief 90-90 position for sciatica can make this sequence easier to tolerate.
Seated slump-modified glides for desk days
Sit tall at chair edge. Extend one knee lightly while lifting chest and keeping neck neutral. Return and switch. Keep it tiny. On long desk days, this can reset stiffness every 60 to 90 minutes without stressing arthritic knees. Pair this with a practical sit-stand schedule for desk job sciatica to reduce symptom accumulation.
Don’t do this: aggressive hamstring stretching into tingling
If a stretch causes electric, shooting, or spreading symptoms, you are likely irritating nerve-sensitive tissue. Stretching harder rarely fixes that. Scale down and shift to glides, breathing, and gradual loading. For a clear distinction between muscle tightness and neural irritation, read hamstring stretch vs nerve pain.
Show me the nerdy details
Nerve “mobility” work is often better tolerated as oscillating glide than long end-range holds. The dose variable is not just reps, but symptom latency. If irritation appears 6 to 12 hours later, your effective dose was too high even if it felt fine in-session.
Core Stability Without Knee Compression
Dead bug regressions with heel taps
Start with both knees bent, feet on floor. Brace gently on exhale, lift one foot a few centimeters, tap heel down, repeat. Keep ribs quiet and spine neutral. 5 to 8 reps each side, 2 sets. If back symptoms rise, make range smaller before quitting. For progressions and regressions that match symptom-sensitive days, use this dead bug exercise for sciatica guide.
Side-lying anti-rotation holds (short sets, crisp form)
Lie on side, knees slightly bent, top hand pressing lightly into floor in front as you resist trunk rolling. Hold 10 to 20 seconds, 3 to 5 reps each side. It looks simple. It works because it targets control without knee compression.
Bird-dog at countertop height for low-knee demand
Hands on countertop, step back slightly, neutral spine. Extend one leg behind lightly, opposite arm forward if tolerated. Hold 3 to 5 seconds, 6 reps each side. This variation avoids kneeling stress and keeps alignment clearer for beginners.
Pattern interrupt: “No, crunches are not your shortcut”
Crunches often train trunk flexion endurance, not the anti-rotation and anti-extension control that protects daily movement with less flare risk. Your spine prefers good control over dramatic repetitions.
- Choose anti-rotation and neutral-spine drills first.
- Stop chasing fatigue as proof of quality.
- Clean reps beat longer sets when symptoms are reactive.
Apply in 60 seconds: Replace one ab exercise this week with countertop bird-dog.
Hip & Glute Strength: Your Shock Absorber System
Glute bridge (short lever) with symptom-based tempo
Lie on your back with feet closer to hips than usual to reduce hamstring dominance. Lift hips to comfortable height, pause 1 second, lower slowly for 2 to 3 seconds. 6 to 10 reps, 2 to 3 sets. If knees complain, narrow range and focus on smooth control. For setup details that reduce nerve irritation, check glute bridge for sciatica pain.
Clamshell and sidestep band walks for lateral hip control
Clamshell: 8 to 12 controlled reps per side. Band sidestep: 6 to 10 steps each direction, torso quiet, knees soft. These improve frontal-plane control, often reducing knee irritation during stairs and uneven walking.
Sit-to-stand from elevated surface (depth-controlled)
Use a higher chair or cushions. Lean slightly forward from hips, stand with both feet grounded, sit back slowly. 5 to 8 reps. Depth is adjustable. A controlled partial range today can build capacity faster than deep painful reps that sabotage tomorrow.
Open loop: the glute weakness pattern most people miss
Many people can “squeeze glutes” lying down but lose pelvic control during transitions like standing, turning, and stairs. Train transfer movements, not just isolated squeezes.
Quick story: I once watched a friend crush clamshells with perfect form, then twist hard every time she got up from a chair. The fix was not a new band color. It was practicing sit-to-stand with calm trunk control for two weeks. Pain didn’t vanish, but flare days dropped noticeably.
Cardio Swaps That Protect Both Nerve and Joint
Recumbent bike vs upright bike: when each wins
Recumbent bike often feels friendlier during reactive knee weeks and when upright posture aggravates back symptoms. Upright bike can be fine if seat height is set to avoid deep knee flexion and cadence stays smooth. Start with 8 to 12 minutes, easy effort, then reassess 24-hour response. For fitting and posture tweaks, use recumbent bike setup for sciatica, and for decision criteria compare recumbent vs upright bike for sciatica.
Pool walking / water aerobics on high-pain days
Water reduces joint loading while preserving movement volume. For mixed sciatica-knee symptom weeks, pool sessions can protect consistency and mood when land sessions feel too costly. If you are deciding session structure, this guide on swimming with sciatica helps map intensity without post-session payback.
Flat-walk intervals with cadence control
Try 2 minutes walk + 1 minute easy pace, repeated 5 to 8 rounds on flat surfaces. Slightly quicker cadence with shorter stride can reduce joint stress compared with long-stride marching. If walking itself triggers symptoms, review sciatica pain when walking for terrain and pacing modifications.
Elliptical reality check: helpful for some, provocative for others
Ellipticals are low impact, but not universally tolerated. If symptoms spread down leg during or after, reduce resistance/incline first, then duration. If still provocative, swap to bike or pool temporarily. A side-by-side comparison in sciatica treadmill vs elliptical can speed up this choice.
Don’t do this: incline spikes and long downhill walks during flares
Steep incline can overload calves/hips and alter trunk posture. Long downhill walks often increase knee compressive demand. During flare weeks, flatter is smarter. The same caution applies to stair-heavy machines and routines. If stairs are unavoidable, see stair climber sciatica and sciatica going down stairs for safer substitutions.
Inputs: session minutes, discomfort rise (0 to 10), next-day recovery (hours).
If discomfort rise is ≤2 and recovery is within 24 hours, keep or progress by 5 to 10%. If discomfort rise is ≥3 or recovery exceeds 24 hours, cut next session volume by 20 to 30%.
Neutral next action: Write your three numbers after each cardio session for one week.
Common Mistakes That Prolong Flare Cycles
Mistake 1: Chasing intensity instead of consistency
One hard workout followed by two bad days is not progress. Four modest sessions with stable recovery usually win over time. Capacity is built by repeatable stress, not dramatic spikes.
Mistake 2: Deep knee bends while sciatic symptoms are active
During active nerve irritability, deep flexion patterns can amplify compensation. Use range you can own cleanly. Increase depth later when baseline is stable.
Mistake 3: Copying “back pain” routines that ignore OA mechanics
Some back-focused routines assume knees tolerate kneeling, deep squat patterns, or long holds in bent positions. If your knees object, modify the setup, not your self-respect. And if you are tempted to jump into barbell work too early, read deadlifting with sciatica before loading patterns that require higher tolerance.
Mistake 4: Ignoring 24-hour symptom feedback
Session pain is only half the story. Next-day stiffness and walking confidence matter more for real-world function.
Short Story: The Tuesday Trap (120–180 words)
On a Tuesday morning, I did what many of us do when pain finally dips: I celebrated too early. Extra incline, extra reps, extra confidence. During the workout, I felt unstoppable. That evening, my knee started whispering. By dawn, it was giving speeches. My sciatic symptoms joined like backup singers I never invited. I spent Wednesday negotiating stairs and pretending everything was fine.
The weird part was not the pain. It was the confusion. “But it felt good yesterday.” That sentence kept replaying. What changed my trajectory was one boring decision: I started grading workouts by next-day function, not same-day pride. If I could walk, sit, and stand with less drama the next morning, it was a good session. If not, I adjusted dose. Within three weeks, flare frequency dropped. Nothing magical happened. I just stopped rewarding workouts that sent me a bill later.
Progression Rules That Keep You Out of the Boom-Bust Loop
The 24-hour response rule (progress only if baseline returns)
Progress after stability, not after motivation. If symptoms settle by next day and function is equal or better, you can increase one variable. If not, keep or reduce dose.
Micro-progression menu: range, reps, load, then speed
Use this order:
- Range
- Reps
- Load
- Speed
Why this order? It usually minimizes unnecessary irritation and preserves form quality. Jumping straight to speed often turns clean movement into joint negotiation.
Flare protocol: what to reduce first and what to keep
During flare days, reduce volume and range first. Keep frequency if possible with short sessions. Stopping everything can increase stiffness and fear, while tiny consistent movement often stabilizes symptoms sooner.
Open loop: when “less” training produces more weekly volume
Counterintuitive truth: smaller sessions can increase total weekly work by preventing derailment. Think like an investor choosing steady compounding over risky spikes.
Show me the nerdy details
Load management works like tolerance budgeting. The tissue system has a moving threshold influenced by sleep, stress, and recent cumulative demand. Micro-progression narrows variance and improves decision quality under uncertainty.
- Increase one variable per week, not three at once.
- Use next-day function as your green light.
- Keep some movement even during flare days.
Apply in 60 seconds: Circle one variable to progress this week and freeze the rest.
Build Your 20-Minute, 3-Day Starter Plan
Day 1 template: nerve + core + easy cardio
- 3 minutes: breathing + pelvic tilts
- 5 minutes: gentle nerve glides
- 6 minutes: dead bug regression + countertop bird-dog
- 6 minutes: easy bike or flat walk
Day 2 template: hip strength + mobility + short walk
- 4 minutes: warm-up mobility
- 8 minutes: bridge + clamshell + sit-to-stand (elevated)
- 8 minutes: flat-walk intervals
Day 3 template: mixed circuit + recovery downshift
- 10 minutes: 4-move circuit (small range, crisp form)
- 5 minutes: low-intensity cardio
- 5 minutes: downshift breathing + gentle mobility
Weekly review checkpoint: pain, stiffness, walking confidence
Score each from 0 to 10 every Sunday. If two out of three improve or stay stable, continue. If two worsen, reduce total volume 20% for 1 week and rebuild.
- Your 7-day symptom log with 24-hour responses.
- Top 3 movements that provoke symptoms.
- Top 3 movements that help symptoms.
- Current activity capacity: walking minutes, sit-to-stand count, stairs tolerance.
Neutral next action: Bring this list to your next appointment for faster, more specific exercise modifications. If you need a broader conservative-care roadmap, this page on physical therapy for sciatica can help shape questions for your visit.
When to Seek Help Instead of Self-Adjusting
Same-day clinician call signs
Call your clinician the same day if symptoms are clearly escalating over several days despite reducing load, if night pain is increasing, or if walking tolerance suddenly drops.
Urgent red flags: progressive weakness, saddle symptoms, bowel/bladder changes
These need urgent evaluation. Do not wait to “see if it settles.” Prompt care matters. If you are unsure what crosses the emergency threshold, review low back pain emergency signs.
How to ask for PT modifications for both sciatica and knee OA
Use this script: “I need a program that respects both nerve irritability and knee load. Can we set one flare version and one rebuild version, with progression rules based on next-day symptoms?” You will get better care faster when your request is specific.
In real clinics, the best plans are often boring on paper and brilliant in outcomes. Clear constraints create better exercise choices.

FAQ
Can I do squats if I have sciatica and knee arthritis?
Yes, often in modified form. Start with elevated sit-to-stand or partial-range squats and control tempo. If symptoms spread or next-day pain spikes, reduce depth and total reps first.
Is walking better than cycling for this combo?
Neither is universally “best.” Walking helps function carryover, but cycling may be better during reactive knee days. Use the 24-hour response rule to choose your current winner. Footwear also matters more than most people expect, so sciatica-friendly walking shoes can be a meaningful upgrade.
Are nerve glides supposed to hurt?
They should not create sharp, electric, or lingering symptoms. Gentle tension can occur, but increasing or spreading symptoms means the dose is too high or the range is too large.
Should I rest completely during a flare-up?
Usually no. Relative rest with reduced range, load, and duration works better than full shutdown for many people. Short, calm sessions can reduce stiffness and fear.
Is heat or ice better before exercise?
Use whichever helps you move more comfortably and safely. Heat often helps stiffness; ice may calm irritability post-session. Your functional response matters more than ideology. For overnight heat safety questions, see sleep with a heating pad for sciatica.
How do I know if an exercise is helping or harming?
Track same-day tolerance plus next-day function. Helpful exercise usually keeps symptoms stable or improves walking confidence within 24 hours.
Can I use resistance bands safely with knee OA?
Yes, especially for hip-focused work like clamshells and sidesteps. Begin with light tension, controlled speed, and smaller volume than you think you need.
Do I need imaging before starting exercises?
Not always. Many people begin with symptom-guided conservative exercise first. Imaging is usually guided by red flags, persistent progression, or unclear diagnosis.
Can weight loss reduce knee pain enough to improve sciatica exercise tolerance?
For many people, reducing excess load can improve knee symptoms and movement confidence, which may indirectly improve tolerance for back-friendly training. Progress can be gradual and still meaningful.
How long until I notice meaningful improvement?
Some notice changes in 2 to 4 weeks with consistent low-impact work. Bigger changes in confidence and capacity often appear over 8 to 12 weeks, depending on baseline and consistency.
Next Step
Here is your 15-minute mission: run the 2-minute lane check, pick three exercises (one nerve-calm, one core, one hip strength), and do one short cardio block. Then log your 24-hour response tomorrow morning. That closes the loop from the hook: you stop guessing and start deciding with evidence from your own body.
You do not need perfect days. You need repeatable days. A calm, consistent program is less dramatic, but it quietly gives your week back.
- Pick today’s lane before training.
- Scale by next-day function, not same-day emotion.
- Build capacity with low-impact consistency.
Apply in 60 seconds: Put tomorrow’s 24-hour check-in on your calendar now.
Last reviewed: 2026-02.
