
Stop Paying Twice for the Wrong Orthopedic Appointment
The wrong orthopedic appointment can cost you twice: once in money, and again in momentum.
A quick virtual visit that ends with “you should come in anyway” may look efficient on paper, but for knee pain, shoulder weakness, joint swelling, or a fresh sports injury, it can turn one problem into a slow two-step.
Choosing between telehealth and in-person orthopedics is not really a convenience decision. It is a decision about what kind of evidence your body needs to give, and whether a screen can capture it. For some musculoskeletal problems, virtual care is a smart first move. For others, the missing piece is a hands-on exam, a stability check, or a closer look at whether imaging should happen next for orthopedic pain.
Keep guessing, and the price is not just a copay. It is delayed diagnosis, extra appointments, more missed work, and another week of living around pain instead of dealing with it.
This guide helps you choose the visit type that gets you to a useful answer faster, with less drift, less wasted cost, and less calendar theater. It is built around real decision points: function change, diagnosis clarity, red flags, and whether the exam itself is part of the treatment path.
Because in orthopedic pain management, the cheapest visit is not always the least expensive choice. Here is where the decision gets clearer—and where it often goes wrong. Let’s sort that out before you book.
Table of Contents
Fast Answer: Orthopedic pain management choosing telehealth or in-person orthopedics comes down to one question: do you need hands-on examination, imaging coordination, or urgent evaluation, or do you mainly need guidance, follow-up, medication discussion, and a care plan? Telehealth often works well for triage, chronic pain check-ins, and treatment adjustments. In-person care usually matters more when function is changing, pain is severe, swelling is visible, or the diagnosis is still unclear.

Start Here: What This Choice Really Decides
This is not just about convenience. It is about what kind of problem you need solved.
Most people compare telehealth and office care as if they were two delivery apps with different fees. They are not. They are two different ways of gathering information, making judgments, and moving a treatment plan forward. A video visit can be excellent at history-taking, follow-up, medication review, and pattern recognition. An in-person visit can do something a screen cannot fully imitate: hands-on examination, resistance testing, stability checks, gait observation, precise swelling assessment, and the small physical clues that often separate “annoying” from “important.”
A familiar scene: someone wakes up with a knee that has gone from grumpy to theatrical. It hurts going downstairs, looks a little fuller than usual, and suddenly every step feels negotiated. In that moment, the question is not simply “Which appointment is faster?” It is “What kind of information is missing, and which visit can get it?”
The wrong visit type can delay answers, not just waste time
This is the sneaky part. A visit can feel efficient because it happens sooner, costs less, or spares you the drive. But if it cannot answer the question that actually matters, it becomes a very polished delay. Plenty of musculoskeletal problems are partly visual and partly physical. A clinician may be able to watch you lift an arm on video, but that is not the same as checking strength, instability, tenderness, warmth, or joint mechanics in person.
That is why some “cheap first steps” quietly become expensive second steps. You save one afternoon and lose two weeks. The calendar smiles while your shoulder does not.
Why “cheaper and faster” is not always the better first move
Time-poor readers often do a quick mental equation: lower copay + no commute + faster slot = obvious winner. Sometimes that math is right. Sometimes it is wearing a very convincing disguise. The better metric is cost per useful answer. If a telehealth visit gives you a clear plan, confirms that you do not need urgent evaluation, reviews prior imaging, or adjusts treatment without another appointment, wonderful. If it only tells you to come in anyway, the bargain was decorative.
- Use telehealth when guidance, triage, or follow-up is the main need.
- Use in-person care when the exam itself may change the diagnosis or next step.
- Think in answers gained, not minutes saved.
Apply in 60 seconds: Write one sentence: “What do I need this visit to decide?” Let that sentence choose the format.
Who This Is For and Not For
Best for adults weighing joint, back, shoulder, knee, hip, hand, or sports-injury care
This guide is for adults trying to choose the most useful entry point into orthopedic care. Maybe it is knee pain after a weekend project that became an accidental CrossFit audition. Maybe it is shoulder pain that has slowly turned reaching overhead into a negotiation. Maybe it is back pain with stiffness, hand pain that interferes with grip, a follow-up question after imaging, or a sports injury that seems improved until it suddenly is not.
It is especially relevant when you are not deciding whether to seek care at all. You have already crossed that bridge. You are deciding which visit type gives you the cleanest next step.
Especially useful for people juggling work, caregiving, travel time, or high-deductible costs
For many readers, the real problem is not just pain. It is pain braided together with work schedules, caregiving, school pickup, parking, and the small domestic chaos that makes a “simple appointment” feel like a military exercise. Telehealth can reduce a great deal of that friction. It can also help if you live far from specialty care or need a first-pass conversation before committing to travel, imaging, or procedural planning.
There is also the high-deductible reality. When every visit feels like it should come with a receipt wrapped in mild emotional damage, choosing the right first appointment matters even more. Readers trying to balance that math may also want a deeper look at orthopedic pain management with a high-deductible plan.
Not ideal for symptoms that look urgent, rapidly worsening, or physically obvious in ways a screen cannot capture
This guide is not for trying to rationalize away symptoms that deserve hands-on care now. If you have a new inability to bear weight, a visibly deformed limb, rapidly worsening numbness or weakness, major swelling after trauma, fever with a hot swollen joint, or a back-pain picture that includes bowel or bladder changes, the conversation has left the “which format is convenient?” stage.
In those cases, the body is waving a larger flag than the booking interface. Respect the flag.
Eligibility Checklist: Is Telehealth a Reasonable First Step?
- Yes: You already have a diagnosis or prior imaging to review.
- Yes: You need medication, home-care, or therapy-plan adjustments.
- Yes: Your symptoms are stable enough to describe clearly.
- No: You cannot bear weight, your joint looks obviously abnormal, or weakness is worsening.
- No: You suspect a fresh injury that needs a hands-on exam.
Next step: If you hit mostly “yes,” telehealth may be a sensible opener. If you hit one strong “no,” book in-person or urgent evaluation.
Telehealth First: When Virtual Orthopedic Care Actually Makes Sense
Chronic pain follow-ups, medication review, and care-plan adjustments often fit well
Telehealth is often strongest when the diagnosis is partly known and the task is refinement rather than discovery. Think chronic knee osteoarthritis check-ins, tendon pain that is already being managed, medication side-effect review, progress updates after physical therapy, activity modification discussions, or questions about whether your current plan is actually earning its rent.
This is where virtual care often shines. The clinician can review how symptoms changed over 2 to 6 weeks, what made things better or worse, whether sleep or daily function improved, and what the next non-surgical or diagnostic step should be. No one has to pretend video can replace every physical test. It simply does not need to. The goal here is judgment and planning.
Telehealth can work when you already have imaging, prior notes, or a known diagnosis
If you already have X-rays, an MRI report, a prior orthopedic assessment, or an established condition, telehealth becomes much more powerful. Suddenly the visit is not wandering through the forest with a flashlight. It is reviewing a map. A clinician can connect symptoms to known findings, explain what matters and what often looks scarier on paper than it feels in real life, and help you decide whether the next step is therapy, watchful progression, another imaging study, bracing, injection discussion, or surgical referral.
One of the most practical uses of telehealth is simple but underrated: sorting the pile. Which symptom deserves attention first? Which home treatments are worth keeping? Which activity is fine, and which one is quietly setting the whole problem on fire?
It is often strongest as a sorting visit, not a miracle shortcut
Telehealth works best when you let it be what it is. It is not a wizard’s cloak for every musculoskeletal mystery. It is often a triage tool, a follow-up tool, and a plan-adjustment tool. That is not a weakness. That is a proper job description.
A common real-life win looks like this: your pain is not clearly dangerous, but it is persistent enough to deserve a professional decision. You book telehealth, review the pattern, get told what red flags would change urgency, and leave with a specific plan rather than spending another week “monitoring” something you are already thinking about every ten minutes.
Show me the nerdy details
Virtual orthopedic visits are most effective when the clinical question is narrow: review prior imaging, assess symptom trend, clarify whether conservative care is working, or decide whether a procedure or in-person exam is necessary. History often carries a large share of the diagnostic value in musculoskeletal medicine, but the missing piece is frequently the physical exam. The more known information you already have, the more efficient telehealth becomes.
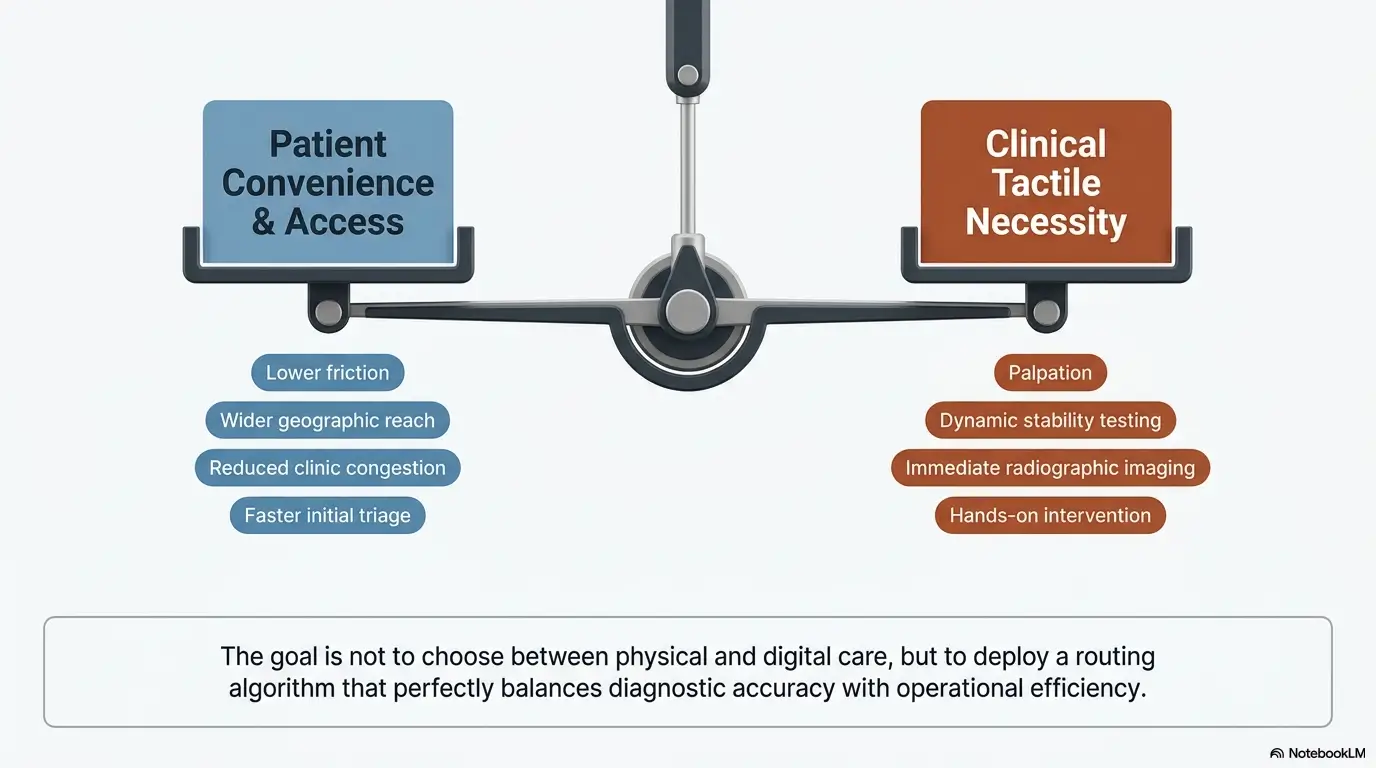
In-Person First: When Hands-On Orthopedics Matters More Than Speed
New injuries, visible swelling, weakness, instability, or range-of-motion loss often need a physical exam
In-person care matters more when the body is telling a physical story that needs to be touched, tested, compared, and watched in motion. New injuries after a fall or twist. A shoulder that suddenly feels weak. A knee that buckles. A hand that cannot grip normally. A hip that turns walking into careful bargaining. Visible swelling, bruising, warmth, instability, and meaningful loss of range of motion are all signs that the exam itself may be diagnostic, not ornamental.
MedlinePlus descriptions of joint pain and swelling make this plain in gentle clinical language: swelling, warmth, pain with motion, and abnormal movement are part of what gets evaluated in person. That is not dramatic medicine. It is practical medicine.
Why “I can describe it well” still may not replace touch, testing, and movement assessment
Some readers are excellent symptom narrators. They know when it started, what movement triggers it, and which side feels different. That helps. It does not erase the value of hands-on care. A clinician may need to test resistance, compare sides, feel for tenderness, assess laxity, identify mechanical catching, or determine whether pain is actually coming from a nearby structure rather than the joint you blame with absolute confidence.
The body is a gifted ventriloquist. Hip problems can masquerade as knee pain. Neck issues can cosplay as shoulder trouble. Tendons, bursae, joints, nerves, and referred pain all enjoy wearing each other’s coats.
When injection discussions, bracing decisions, or procedural planning tip the scale toward office care
If you are specifically seeking an injection conversation, bracing decision, post-injury stability assessment, procedural planning, or surgical examination, in-person care often gets you farther, faster. Not always, but often. Even when a telehealth visit is allowed as the formal first step, the plan may still hinge on findings that only make sense after examination.
A useful rule of thumb is this: if the next likely step involves a procedure, fitting, direct testing, or immediate imaging decisions based on exam findings, office care has an advantage that convenience cannot cancel out. That is especially true when you are already comparing whether a pain clinic or an orthopedist is the better fit for the question in front of you.
Decision Card: When Telehealth vs In-Person Usually Wins
| Situation | Usually Better | Why |
|---|---|---|
| Known diagnosis, follow-up pain plan | Telehealth | History and treatment review do most of the work |
| Fresh injury with swelling or weakness | In-person | Exam findings may change urgency and imaging needs |
| Questions after MRI or X-ray | Telehealth or in-person | Depends on whether exam changes next steps |
| Injection, bracing, instability, procedure planning | In-person | Hands-on findings often matter |
Neutral action: Match the visit to the likely next decision, not the shortest wait.
Cost Trap Ahead: The Cheapest Visit Can Become the Most Expensive Path
A low-cost telehealth visit can still add cost if it only leads to a second appointment and delayed imaging
Healthcare math is rarely as charming as we would like. A lower-cost virtual visit can be excellent value when it resolves the problem, clarifies the plan, or safely narrows the next step. But if it mainly confirms that the clinician needs to examine you in person anyway, the cheaper first visit can become a fee for staying in line longer.
That does not make telehealth bad. It just means the first question should not be, “What is the lowest-priced slot?” It should be, “What is most likely to answer the main question in one move?”
A common example: someone with new shoulder pain chooses telehealth because the copay is lower and the opening is tomorrow. The virtual clinician takes a careful history, watches a few movements, and concludes that an in-person exam is needed to assess strength and impingement signs. Nothing improper happened. But the reader who thought they were buying certainty really bought sequence.
In-person may cost more upfront but answer the real question faster
In-person visits can cost more at the front end, especially under high-deductible plans. Yet they can save money indirectly by reducing repeated intake, shortening delays, and letting the clinician decide faster whether you need imaging, therapy, a brace, a procedure, or simple conservative care. The value is not always on the bill. Sometimes it hides in the path.
Time has a cost too. Missed work, repeated scheduling, extra childcare, fuel, parking, and the emotional tax of staying uncertain all count. Patients are not spreadsheets, but we do live inside calendars.
How to think in “cost per useful answer,” not just copay math
Try a slightly better frame: cost per useful answer. Ask yourself what the visit needs to accomplish. Do you need reassurance and a treatment adjustment? Telehealth may be high value. Do you need someone to determine whether the joint is unstable, inflamed, weak, or mechanically restricted? Office care may be the cheaper truth even if it is the pricier appointment. If finances are shaping the choice, it also helps to understand self-pay cash price ranges for orthopedic care before you book blindly.
Mini Calculator: Your Real Appointment Cost
Use three inputs:
- Visit fee
- Travel/work disruption cost
- Chance you will still need a second visit
Quick estimate: If telehealth saves $80 today but has a high chance of leading to a $250 office visit anyway, it may not be your cheaper path. If telehealth resolves the issue or safely narrows the next step, it may be the best bargain on the board.
Neutral action: Before booking, write down both the visit price and the price of staying unsure for another week.
- A lower copay can still produce a longer and more expensive path.
- In-person visits often cost more upfront but may answer more in one step.
- The best metric is what the appointment actually resolves.
Apply in 60 seconds: Ask: “If this visit cannot settle the main question, what happens next?”
Diagnosis Clarity: The Hidden Factor Most Patients Miss
Telehealth works better when the diagnosis is already partly known
Diagnosis clarity is the quiet hinge of this whole decision. When the likely diagnosis is already narrowed, telehealth becomes much more useful. The clinician is not trying to identify a shape in the fog. They are comparing symptoms against known information, adjusting treatment, and deciding whether progress is normal, stalled, or headed off-script.
This is why a telehealth follow-up after prior imaging can feel satisfyingly crisp. The visit has context. It has something to push against. The conversation gets better because the uncertainty is smaller.
In-person usually wins when pain is vague, referred, mechanical, or hard to reproduce on camera
When pain is vague, referred, mechanical, intermittent, or difficult to demonstrate, in-person care usually gains ground. Mechanical symptoms in particular can be slippery over video. Catching, locking, giving way, weakness that appears only under resistance, pain that shows up at certain angles, or tenderness in a structure the patient cannot identify well all benefit from examination.
A small but memorable truth: some pain is not where it lives. A knee can complain because a hip is misbehaving. A shoulder can protest because a neck is involved. What feels obvious from inside the body can look entirely different once someone tests movement and mechanics from outside it. When that overlap is muddy, articles on hip versus spine pain or even neck and shoulder pain from laptop work can help readers see why a body part is not always a reliable narrator.
Here’s what no one tells you: uncertainty is often the real reason visits multiply
Patients often think repeat visits happen because doctors are being cautious or systems are slow. Sometimes that is true. But a large share of repeated visits comes from something simpler: the first encounter did not reduce uncertainty enough. The problem stayed fuzzy. The next step stayed conditional. The plan stayed provisional.
That is why choosing the correct format up front matters. Not because one is modern and one is old-fashioned, but because certainty has a cost curve. Every unresolved variable can breed another appointment like a damp basement breeds opinions about dehumidifiers.
Short Story: A reader once described a shoulder problem that sounded, at first pass, perfectly telehealth-friendly. The pain had built slowly. There was no fall, no dramatic bruise, and no emergency mood to the whole thing. On video, they could raise the arm halfway, point to the sore spot, and describe three weeks of careful stretching. It seemed straightforward. But the phrase that changed the whole picture was simple:
“It is not just pain. It feels weak when I reach out with any weight.” That one detail shifted the visit logic. Weakness is not merely discomfort with better branding. It can change what the clinician needs to test, what injury pattern becomes more plausible, and whether the next step should be imaging, an office exam, or immediate protection of the joint. In the end, the most useful decision was not the faster screen. It was the hands-on visit that turned a floating symptom story into a concrete plan.
Don’t Start Here: Common Mistakes That Make Orthopedic Care Slower
Choosing telehealth just because the schedule is open sooner
The next-day slot has a seductive glow. It whispers competence. It smells like momentum. But speed only helps when the format is capable of solving the right problem. Booking telehealth purely because it appears first on the screen is like choosing luggage by wheel shine. You may still arrive. You may also regret your relationship with stairs.
If the issue likely needs hands-on examination, sooner is not always better. Sooner can mean sooner to discover you needed a different appointment all along.
Booking in-person automatically when a virtual triage visit could have clarified next steps
The reverse mistake happens too. Some readers assume orthopedic pain automatically deserves an office visit because musculoskeletal care seems inherently physical. Yet if the diagnosis is already known, the symptoms are stable, and the real need is plan review, medication discussion, or interpreting prior studies, a telehealth visit may do the job beautifully. Not every ache deserves a drive, a parking ticket disguised as a validation process, and 47 minutes in a waiting room chair designed by a committee that feared comfort.
Treating “pain level” as the only decision factor instead of function, swelling, weakness, and timeline
Pain score matters, but it is not the whole story. A moderate pain level with sudden weakness or new instability may be more urgent than a very painful but familiar flare. Functional change often tells you more than raw intensity. Can you bear weight? Can you grip? Can you raise the arm? Is the joint visibly swollen? Did symptoms start after a twist, fall, or pop? Are they getting worse quickly? These details do more decision work than a lone number from 1 to 10.
Quote-Prep List: What to Gather Before Comparing Visit Options
- Date symptoms started and whether there was an injury
- What function changed: walking, reaching, gripping, sleeping, stairs
- Any visible swelling, redness, bruising, deformity, or warmth
- Prior imaging, therapy, injections, braces, or orthopedic notes
- Your real-life constraint: work, travel, deductible, caregiving
Neutral action: Gather this list before booking so the first visit is shaped by facts, not guesswork.
Let’s Be Honest: Many People Are Not Choosing Care, They Are Choosing Friction
Commute time, childcare, missed work, and clinic fatigue shape decisions more than people admit
This is the part people whisper to themselves but rarely say out loud: sometimes the choice is not between telehealth and in-person care. It is between possible and unlikely. The office may be clinically ideal, but if getting there requires missed wages, a borrowed car, school pickup improvisation, and a two-hour block of life that simply does not exist, patients start choosing the least destructive option, not the best theoretical one.
That does not make them careless. It makes them human. Orthopedic pain often unfolds in ordinary lives, not in textbook margins.
Telehealth can reduce life-friction even when it is not the final stop
This is where telehealth earns real respect. It can lower the entry barrier enough for people to get professional guidance earlier. That matters. Sometimes the most important thing a virtual visit does is not solve the entire problem. It gets the patient unstuck. It tells them what is urgent, what can wait, what warning signs matter, and what kind of in-person visit is worth the effort.
A mother with hand pain and no spare afternoon. A warehouse worker with knee stiffness who cannot lose another half day. A rural patient facing a long drive just to ask whether the next step is imaging or therapy. For these readers, telehealth is not laziness. It is a bridge. Some of those day-to-day pressures look a lot like the patterns described in warehouse worker knee pain or orthopedic pain management for remote workers.
The best choice is often the visit type that gets you to the right next action with the least drift
The perfect appointment is less important than the useful one. Sometimes that means booking in-person immediately. Sometimes it means using telehealth to avoid another week of indecision and then moving quickly to office care only if needed. The key word here is drift. You want the least drift between symptom, decision, and action.
- Telehealth can be the most realistic first step for busy or remote patients.
- Reducing friction often means earlier guidance and less avoidant delay.
- Use the format that keeps care moving, not drifting.
Apply in 60 seconds: Ask yourself which option you can actually complete this week without derailing the rest of your life.
Before You Book: Questions That Separate a Useful Visit From a Placeholder
Do I need hands-on testing to move the diagnosis forward?
This is the single best booking question in the whole article. If the answer is yes or even probably yes, in-person care deserves the edge. Hands-on testing matters when weakness, instability, tenderness, swelling, gait change, or limited range of motion are part of the story. If the answer is no, or if the diagnosis is already reasonably established, telehealth becomes more attractive.
Do I already have imaging or prior orthopedic records to review?
Records are rocket fuel for a virtual visit. They give the conversation shape. A clinician can interpret progression, compare findings, and explain what the images do and do not mean. Patients often fear imaging reports because the wording sounds like a Victorian ghost story. Degeneration, tears, lesions, impingement, narrowing. It is a vocabulary that could use better public relations. A telehealth review can help translate the findings into practical decisions. That conversation becomes even more useful when patients understand why MRI findings and pain do not always match neatly.
Am I seeking reassurance, a treatment adjustment, or an answer only an exam can provide?
If what you need is reassurance, treatment adjustment, explanation, or triage, telehealth may be plenty. If what you need is a clinician to determine whether the body is mechanically unstable, acutely injured, infected, or neurologically changing, the exam itself is part of the answer.
Quick Visual: Which Visit Fits Which Problem?
Telehealth tends to fit:
- Known diagnosis
- Follow-up questions
- Medication or plan changes
- Review of MRI or X-ray reports
- Need for triage before travel
In-person tends to fit:
- New injury after twist or fall
- Visible swelling or deformity
- Weakness or instability
- Meaningful motion loss
- Injection, bracing, or procedure planning
Use this rule: If the exam may change the next step, do not outsource the visit to convenience.
Red Flags First: When This Should Not Stay a Telehealth-Only Decision
Sudden inability to bear weight, major weakness, deformity, or worsening numbness needs more than convenience logic
Some situations simply outgrow telehealth-only thinking. If you suddenly cannot bear weight, a limb looks deformed, weakness is significant or worsening, or numbness is spreading, the question is no longer which format feels efficient. The question is how quickly you need hands-on assessment.
That is particularly true after trauma, major twists, falls, or sudden functional collapse. A camera can witness a lot. It cannot palpate, stabilize, or rule out structural damage by polite observation alone.
Fever, trauma, severe swelling, or rapidly escalating pain changes the equation
Fever with a hot swollen joint, severe swelling after injury, rapidly escalating pain, or symptoms suggesting infection or major structural injury deserve prompt direct evaluation. Official health references repeatedly point patients toward more urgent care when joint swelling, inability to use a limb normally, or major injury features are present. In plain English: some symptoms are too physical, too fast, or too potentially serious to keep at arm’s length. When the question is no longer routine orthopedics but where to go right now, comparing urgent care versus an orthopedic clinic may be more useful than debating telehealth.
When “watch and wait” starts sounding less like patience and more like avoidance
There is a noble version of watchful waiting and a shabby one. The noble version is clinically reasonable, time-limited, and paired with clear warning signs. The shabby one is what happens when a person is avoiding inconvenience, cost, or bad news so skillfully that they start calling it prudence.
If your symptoms are worsening, interfering with sleep, or sharply limiting function, do not let “I’ll give it a few more days” become a hobby.
- Inability to bear weight changes the urgency.
- Fever, hot swelling, major weakness, or deformity deserve prompt evaluation.
- Rapid worsening is its own clue, even before a diagnosis is named.
Apply in 60 seconds: If function has dropped sharply or the joint looks dramatically different, stop comparing convenience and seek direct care.
Common Mistakes
Waiting too long because the pain is “probably just inflammation”
Inflammation is one of those words people use when they want their body to be less mysterious than it currently is. Sometimes that guess is fine. Sometimes it delays useful care. Pain that is stable and mild can often be managed conservatively. Pain that is worsening, disrupting sleep, limiting function, or paired with weakness, swelling, or injury history deserves more respect.
Assuming imaging is the first step instead of one tool inside a larger exam-and-history process
Many readers imagine the pathway as pain, then MRI, then truth. Real orthopedic care is usually more textured than that. Imaging is important, but it lives inside a larger process that includes history, examination, function, symptom timing, and response to prior care. Some findings on scans are meaningful. Some are common background noise. This is one reason a good visit matters more than a reflex demand for imaging. For patients stuck at the imaging step, it can help to read about what “failed conservative care” means before an MRI or even how to handle orthopedic pain after an MRI denial appeal.
Using a virtual visit without preparing symptom history, movement limits, and prior treatment details
A telehealth visit gets much better when the patient shows up prepared. Know when symptoms started, what movement is limited, what you have already tried, and whether anything is getting weaker, more swollen, or more unstable. Virtual care is not inherently flimsy. Unprepared virtual care can be.
Show me the nerdy details
For musculoskeletal complaints, the most decision-rich patient details are often onset, mechanism, symptom progression, functional loss, focal weakness, visible swelling, neurologic changes, prior treatment response, and whether the pain is reproduced by specific movements. In telehealth, these details carry even more weight because the exam is narrower.
FAQ
Is telehealth good for orthopedic pain management?
It can be very good when the goal is triage, follow-up, medication review, plan adjustment, or discussion of prior imaging and known diagnoses. It is less reliable as a first stop for fresh injuries, major swelling, instability, or problems where the physical exam is likely to change the diagnosis.
When should I choose in-person orthopedics instead of telehealth?
Choose in-person care when you have a new injury, visible swelling, inability to bear weight, weakness, instability, major motion loss, deformity, worsening numbness, or a problem that may need a hands-on exam, brace fitting, injection discussion, or urgent evaluation.
Can an orthopedic doctor diagnose knee or shoulder pain over video?
Sometimes, especially when the likely diagnosis is already narrowed and the visit is focused on history, symptom pattern, and next steps. But many knee and shoulder complaints still benefit from direct examination because strength, stability, tenderness, and mechanics matter.
Will I still need an in-person visit after telehealth?
Possibly. That is common when the telehealth visit uncovers a need for direct examination, imaging coordination, procedures, or hands-on testing. The best telehealth visits reduce uncertainty. If they cannot reduce it enough, an office visit may still be the right second step.
Is telehealth cheaper than seeing an orthopedic specialist in person?
It is often cheaper at the visit level, but not always cheaper at the pathway level. If telehealth resolves the issue, it may save real money. If it mostly leads to a second visit and delayed decisions, it can become the more expensive path overall.
Can telehealth help with MRI or X-ray decisions?
Yes. It can be useful for reviewing whether symptoms, timing, and prior treatment make imaging reasonable. It can also help interpret results you already have. But when the imaging decision depends heavily on exam findings, in-person care may be more efficient.
What symptoms make virtual orthopedic care a poor fit?
Fresh trauma, inability to bear weight, major weakness, rapidly worsening numbness, visible deformity, fever with a swollen joint, severe swelling, or rapidly escalating pain are all signs that telehealth alone may be a poor fit.
Is telehealth useful for follow-up after an orthopedic diagnosis?
Very often, yes. Follow-up care is one of the strongest uses of telehealth because the diagnosis, prior treatment, and progression can all be reviewed without recreating the entire clinical story from scratch.
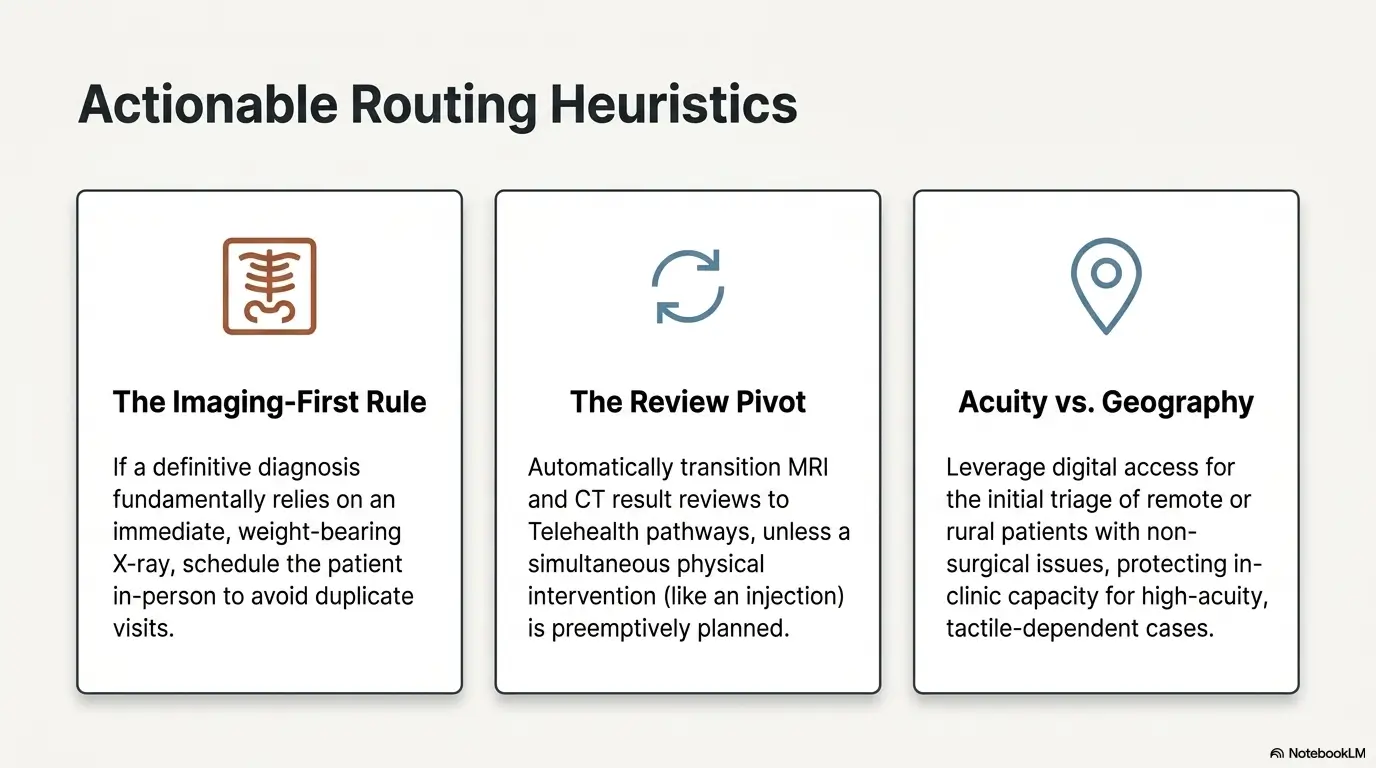
Next Step: Make the Decision With One Filter, Not Ten
Write down your main symptom, how function changed, what you already tried, and whether you likely need a hands-on exam
If you do one useful thing today, make it this. Write four short notes before you book:
- Your main symptom
- What function changed
- What you already tried
- Whether the exam itself likely matters
That tiny list closes the curiosity loop from the beginning of this article. The question was never just telehealth or in-person. The question was what kind of information your problem requires. Once you see that clearly, the visit choice gets quieter and smarter.
Book telehealth if you need triage, follow-up, or treatment review
Telehealth is a strong first move when your symptoms are stable enough to describe, you already have records or a likely diagnosis, and you mainly need guidance, interpretation, or next-step planning. In that role, virtual care is not second-best. It is precisely right-sized.
Book in-person if the diagnosis is unclear, function is dropping, or the body is telling a more physical story than a camera can catch
If function is falling, weakness is new, swelling is visible, the diagnosis is muddy, or the next step may involve direct testing, bracing, injection, or urgent judgment, office care usually earns the trip. Think of it this way: when the body is speaking in mechanics, examination is part of the language. And if support devices become part of that path, it may help to compare HSA-eligible braces and supports before you spend reactively.
- Conversation-heavy problems often fit telehealth.
- Exam-heavy problems usually fit in-person care.
- Function change is often more informative than pain alone.
Apply in 60 seconds: Set a 15-minute timer and make your four-note booking list before the day gets noisy again.
Safety / Disclaimer
This content is educational and decision-supportive, not medical diagnosis or personal treatment advice. Orthopedic pain can range from overuse irritation to something that needs urgent evaluation. When symptoms are severe, rapidly worsening, associated with trauma, major swelling, fever, numbness, weakness, or inability to use the limb normally, prompt medical assessment matters.
When to Seek Help
Seek urgent or prompt care for severe injury, deformity, inability to bear weight, new major weakness, or worsening numbness
These are not subtle signs. If the limb looks wrong, works much less than before, or the neurologic picture is worsening, timely direct evaluation matters.
Seek medical evaluation sooner when pain is escalating despite rest, interfering with sleep, or sharply limiting function
Escalation is information. Pain that keeps climbing, interrupts sleep, or reduces daily function deserves a clearer plan rather than endless home speculation.
Get evaluated if you are unsure whether this is routine pain management or something that needs hands-on care now
Uncertainty itself is a reason to seek care, especially if you are stuck between minimizing symptoms and catastrophizing them. A good first visit should reduce that uncertainty, not decorate it.
Final Word
There is no medal for enduring uncertainty longer than necessary. There is also no prize for booking the slickest-looking appointment type if it cannot answer the question your body is asking. The useful path is often simpler than it first appears: telehealth when the visit is mostly about judgment, review, and triage; in-person when the exam is part of the answer. Make the decision with that one filter, and much of the noise falls away.
Last reviewed: 2026-04.
