
The “$650 TFESI” is often real—until the second envelope shows up.
If you’re shopping self-pay TFESI cost, you’re not comparing one number. You’re navigating a modular system where the injection, fluoroscopy guidance, facility fee (office vs ambulatory surgery center vs hospital outpatient), and optional sedation/anesthesia can live on separate quotes—and arrive on separate timelines.
Keep guessing and you don’t just overpay. You schedule on false certainty, then lose leverage when the “missing layer” appears after the procedure.
TFESI (transforaminal epidural steroid injection) is an imaging-guided epidural placed near a specific nerve root. That precision is clinical—and financial—because it’s exactly where billing stacks and scope changes tend to hide.
This post helps you turn TFESI pricing into something you can actually plan: a written, itemized, all-in estimate tied to your exact side, level(s), and setting—plus the one sentence that forces clarity without starting a fight. (If you’re also comparing approaches, start with TFESI vs interlaminar ESI for sciatica so you’re not pricing two different procedures by accident.)
Table of Contents
TFESI price first: what you’re actually buying
Reader payoff: You’ll know which line items belong in a real TFESI total, so you don’t accept a “half-quote.”
TFESI (transforaminal epidural steroid injection) is a specific kind of epidural injection, typically done with imaging guidance to place medication near a targeted nerve root. That specificity matters—because the billing often becomes a four-part stack:
- Procedure (the injection itself)
- Imaging guidance (fluoroscopy or CT guidance may be baked in or separately billed, depending on how the facility structures charges)
- Facility layer (office vs ambulatory surgery center vs hospital outpatient)
- “Other professionals” (sometimes separate bills if additional clinicians/entities are involved)
A common scene: a clinic coordinator says, “It’s $X cash.” You feel relief. Two weeks later, you open mail and discover that “$X” was only the professional component—while the facility layer lived in a different universe. The goal of this article is to make that universe visible before you schedule. (If your workup includes imaging first, bookmark lumbar MRI cost on an HDHP—it’s the same “layered billing” story in a different outfit.)
- Ask for an itemized estimate tied to your exact side/level(s).
- Confirm the setting (office vs ASC vs hospital outpatient).
- Get “no separate bills” confirmed in writing.
Apply in 60 seconds: Text or email the scheduler: “Please confirm whether this quote includes facility and imaging, and whether I’ll receive any separate bills.”

Procedure vs guidance vs facility: the 4-part bill stack
Even when you’re self-pay, billing often behaves like a modular system. That’s not “bad” by itself—it’s just how healthcare accounting is built. The problem is when a quote covers only one module, and you assume it covers all four.
Why “epidural” quotes mislead TFESI shoppers
Online ranges for “epidural steroid injection cost” can blur multiple approaches (transforaminal, interlaminar, caudal) and multiple settings. TFESI is its own beast. If your quote doesn’t explicitly say transforaminal and specify the level(s), you’re comparing mismatched items. (If you want the clean terminology breakdown, see transforaminal vs interlaminar epidural.)
Here’s what no one tells you… the cheapest quote can be the most expensive
The “cheapest” quote is often the one that quietly excludes the facility layer or leaves the imaging line item undefined. Your job isn’t to find the lowest number. It’s to find the lowest all-in number for the same clinical plan.
Real cash anchors: CPT-level clues you can request
Reader payoff: You’ll learn what to ask for so your quote can’t “mutate” later.
You don’t need to become a coder or a billing specialist. You only need a handful of anchors that keep your estimate from drifting.
Lumbar TFESI + additional levels: why “one level” is the money word
TFESI estimates change when the plan changes from one level to two levels, or from unilateral (one side) to bilateral (both sides). Those aren’t small details. They’re often the difference between “this fits my budget” and “why did the total jump?” (If your doc is talking about very specific targets, you may also see adjacent terms like L5–S1 selective nerve root block—make sure you’re pricing what’s actually planned.)
Imaging guidance line item: why it often appears separately (and how to ask)
Some quotes treat imaging guidance as part of the TFESI bundle; others list it as a separate technical charge. The practical move is simple: ask for the estimate to state plainly whether imaging guidance is included and whether any technical imaging fees apply in your setting.
Show me the nerdy details
Billing often separates “professional” work (physician/clinician services) from “technical” components (facility, equipment, staffing). Even when a code descriptor mentions imaging guidance, facilities may still show technical charges in their internal estimate formats. Your protection is clarity: “Is imaging guidance included in the all-in estimate for this setting?”
The minimum you need in writing: side, level(s), setting, codes, total
If you only remember one checklist from this article, make it this one:
- Side (right/left/bilateral)
- Level(s) (example: L4–L5; “one level” vs “two levels”)
- Setting (office vs ASC vs hospital outpatient)
- What’s included (imaging guidance, facility, supplies, sedation if any)
- Total self-pay amount (the final number you’ll pay if nothing changes)
- “One level” and “bilateral” can change totals dramatically.
- Office vs ASC vs hospital outpatient is often the biggest lever.
- Included/excluded imaging guidance decides whether the quote is honest.
Apply in 60 seconds: Reply to the scheduler with: “To confirm: this is for TFESI at ___ (level), ___ side, in ___ (setting), and includes facility + imaging?”
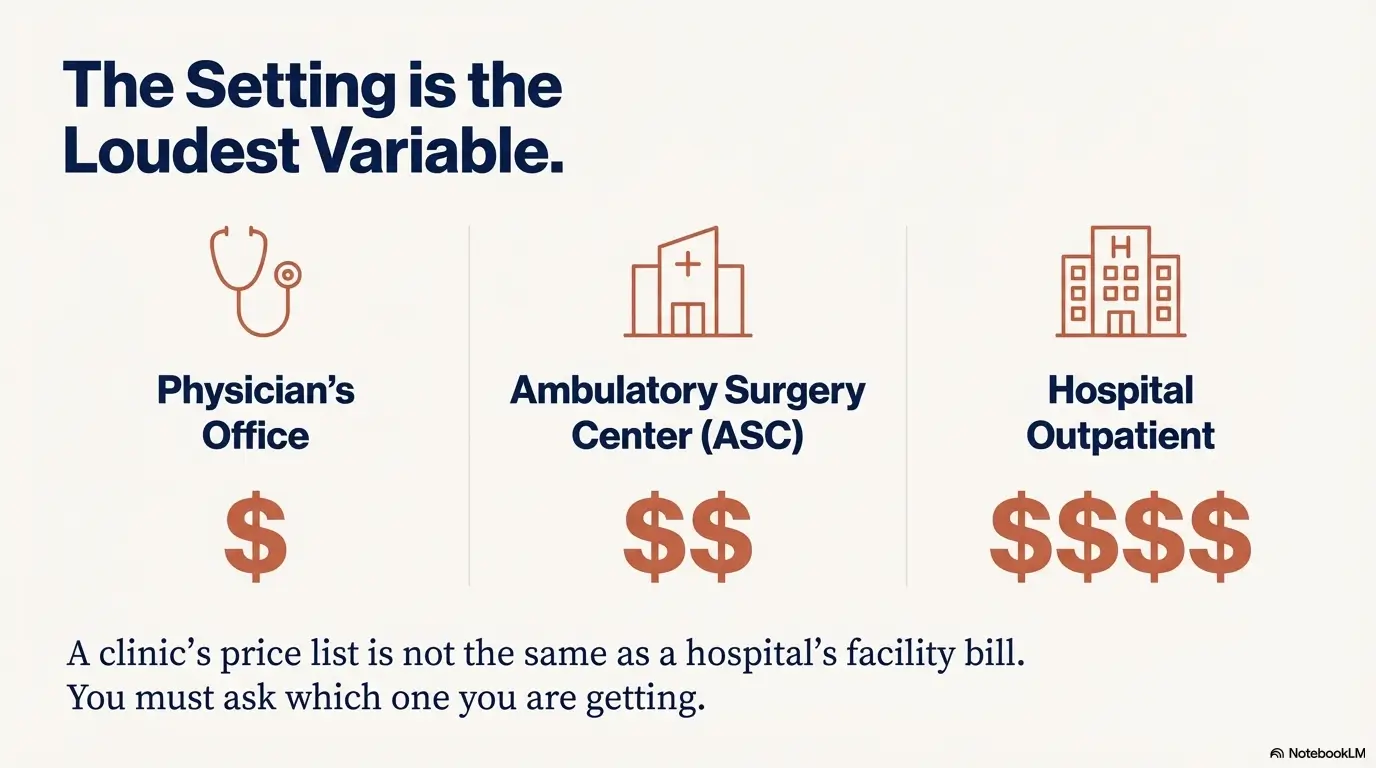
Office vs ASC vs hospital: where the total jumps
Reader payoff: You’ll know why two “TFESI quotes” can differ wildly—without anyone lying.
If you’re trying to control cost, setting is often the loudest variable. Not always, but often.
Clinic fee schedules vs facility pricing: why they’re not interchangeable
Some practices publish self-pay rates that look refreshingly transparent. Here’s the catch: a clinic schedule may reflect the professional component (and maybe some bundled supplies), but it may not represent a full ASC or hospital outpatient facility bill stack. If your procedure is scheduled in an ASC or hospital outpatient department, you need a facility estimate too.
When “facility included” is real—and when it’s marketing language
“All-inclusive” can mean different things in different buildings. One facility uses it to mean “facility + supplies + imaging,” another uses it to mean “procedure only, but we’re discounting it.” You don’t have to argue. You just have to ask the defining question: Which entities are billing me?
Curiosity gap: why your friend’s price can’t be copied (even same city)
Same city isn’t the same setting, and “same injection” isn’t the same level count. A one-level unilateral office TFESI and a two-level ASC TFESI are not price cousins—they’re different products wearing similar names.
Hidden fee menu: the charges that arrive later
Reader payoff: You’ll spot omissions before scheduling, not after paying a deposit.
If TFESI billing were a restaurant menu, the surprise charges wouldn’t be the entree. They’d be the “small print” line items that show up when you thought you were done ordering.
Separate professional bills: who can bill besides the injector?
Depending on setting and staffing, you may see separate bills from different entities. This is the part patients rarely anticipate because it’s not intuitive: you experience one appointment, but the system can treat it as multiple services performed by multiple parties. (This “multiple-entities, one-visit” pattern also shows up when people escalate care—see failed back surgery syndrome for why clarity early matters.)
Sedation/anesthesia: optional clinically, expensive financially
Some TFESIs are done with local anesthetic and reassurance; others involve sedation. If sedation is on the table, ask two questions: (1) is it clinically necessary for you, and (2) is it included in the self-pay estimate? A “yes” to sedation without an all-in number is where surprise bills love to breed. (If you want a broader lens on how anesthesia can change the bill stack, compare how it’s handled in endoscopic discectomy anesthesia discussions.)
Add-ons that change the total: bilateral, contrast, extra level(s)
Most cost blow-ups are not scams—they’re scope changes. “Add one level.” “Do both sides.” “We used contrast.” Each of these may be reasonable clinically. Your job is to make sure each scope change has a cost conversation attached to it.
Show me the nerdy details
Scope changes often trigger additional supplies, time, imaging confirmation, or documentation requirements. Even when the clinical experience feels identical (“still one appointment”), billing systems may map those changes to different charge structures. That’s why a “levels/sides confirmed” estimate is your best protection.
- Ask who else can bill: facility, anesthesia, radiology/technical components.
- Confirm sedation policy and whether it’s included.
- Lock level(s) and side(s) in writing.
Apply in 60 seconds: Ask: “If the plan changes to two levels or bilateral, what is the updated self-pay total?”
Quote script: force an all-in number (politely)
Reader payoff: You’ll get a comparable estimate that doesn’t collapse into “it depends.”
This is the part most people skip, because it feels awkward. The irony is that a clean script makes it less awkward. You’re not accusing anyone of hidden fees—you’re asking for a complete estimate so you can plan.
The “all-in bundle” sentence that stops the missing-piece game
Use this: “I’m self-pay. Could you provide an itemized, all-in estimate for TFESI that includes facility, imaging guidance, supplies, and sedation/anesthesia if used?”
The “no separate bills” question (and what a safe answer sounds like)
Ask this: “Can you confirm whether I will receive any separate bills from other entities?”
Safe answers sound like: “No, it’s bundled,” or “Yes—facility and anesthesia bill separately, and here are the estimates.” Unsafe answers sound like: “Probably not,” “Usually,” or “We’ll see after.”
Let’s be honest… if they won’t itemize, you’re not shopping—you’re guessing
If a provider can’t or won’t provide an itemized estimate, you can still proceed—but understand what you’re choosing: uncertainty. For a time-poor, budget-bounded decision, that’s often a bad trade.
- Your planned level(s) and side(s)
- Your preferred setting (office/ASC/hospital outpatient)
- Whether sedation is expected or optional
Apply in 60 seconds: Write one sentence: “TFESI at ___, ___ side, ___ level(s), in ___ setting.” Use it in every quote request.
Common mistakes: the two-minute errors that cost four figures
Reader payoff: You’ll avoid the quote traps that create the most financial regret.
Mistake #1: “procedure-only” pricing (no facility, no guidance)
If the quote only names the injection and a cash price, it may be incomplete. The fix: ask explicitly what’s included and whether any facility charges apply.
Mistake #2: skipping level/side in the request (your quote won’t match your care)
This is the silent killer. Without level(s) and side(s), you’re not pricing TFESI—you’re pricing a vague concept. And vague concepts are always cheaper than real procedures.
Mistake #3: paying deposits without cancellation/refund terms in writing
Deposits aren’t evil. But they should be transparent: what triggers forfeiture, what happens if the clinician changes the plan, and how rescheduling works.
Micro-scene: You schedule on Monday, pay a deposit Tuesday, and by Friday you realize the setting is different than you assumed. That’s a painful week. A single email—“confirm setting and included fees”—would have prevented it.
Negotiation that works: discounts, timing, and what to ask for
Reader payoff: You’ll negotiate ethically without turning the call into a defensive conversation.
Negotiation works best when it’s not a fight. It’s a clarity request plus a financial preference.
Ask for global self-pay total (not just “discounted procedure”)
Some places happily discount the injection fee but leave the facility layer untouched. When you negotiate, negotiate the total or at least ask which parts are discountable.
Best timing: after codes are confirmed, before the slot is locked
Once the schedule is booked and staff are assigned, flexibility shrinks. Your best leverage is early: “I’m comparing two itemized estimates for the same TFESI plan.”
When a “package price” is good—and when it’s a trap
Good package: states what’s included (facility, imaging, supplies, sedation policy). Trap package: uses “all-inclusive” without itemizing or confirming no separate bills.
Show me the nerdy details
Healthcare discounts often live in policy buckets: “self-pay discount,” “prompt-pay discount,” or “bundled procedure program.” Facilities may be more rigid than clinics. If you ask for “the global self-pay total in writing,” you’re asking for a policy application, not a favor.
- Choose Office when transparency and minimal facility layers matter most.
- Choose ASC when you have a clear bundle and predictable staffing.
- Choose Hospital outpatient when clinical complexity requires it—then demand a written estimate.
Apply in 60 seconds: Ask: “Which setting gives me the most predictable all-in self-pay total for this plan?”
Who this is for / not for: quick fit check
Reader payoff: You’ll know whether cost-shopping is appropriate right now—or whether safety should override shopping.
Good fit: cash-pay, HDHP, out-of-network, planned non-urgent TFESI
This guide fits if you’re stable enough to compare quotes, you’re trying to control cost, and you can wait long enough to get a written estimate before you commit. (If you’re still sorting out whether your pain pattern is truly sciatica, use sciatica vs herniated disc as a quick clarity check so you’re shopping the right next step.)
Not a fit: red flags, rapidly worsening symptoms, urgent evaluation needed
If symptoms suggest urgent neurological issues, you don’t “shop harder.” You seek medical evaluation first. Cost clarity matters—but not more than safety. (If you’re unsure whether you’re in “urgent” territory, read low back pain emergency signs before you keep calling for quotes.)
- My symptoms are not rapidly worsening today.
- I can provide level(s)/side(s) or ask my clinician for them.
- I have time to get an itemized estimate in writing.
Apply in 60 seconds: If any answer is “no,” pause shopping and ask for clinical guidance first.
Safety / Disclaimer: pricing info ≠ medical advice
Reader payoff: Clear boundaries so you don’t delay needed care while chasing a better quote.
This article is about cost predictability, not diagnosis. TFESI is an invasive procedure with risks. The right clinical plan comes from a qualified clinician who understands your symptoms, exam, and imaging (when appropriate). Pricing varies by state, facility, and billing structure. Treat every estimate as conditional on the plan staying the same.
A gentle truth: the best time to worry about hidden fees is before the injection—because after the injection, your leverage is mostly gone.
When to seek help: don’t bargain-hunt these symptoms
Reader payoff: You’ll know when to stop comparing quotes and get evaluated.
Urgent red flags (get urgent evaluation)
- New bowel or bladder changes
- Saddle numbness (numbness in the groin/inner thighs area)
- Rapidly worsening weakness in the leg or foot
- Severe, escalating neurological symptoms
Same-week evaluation triggers
- Fever with severe back pain
- Major trauma
- New severe pain with concerning medical history (discuss promptly with a clinician)
On a Wednesday morning, a person calls three places for a TFESI quote. The first says “$650 cash,” the second says “$1,900,” and the third won’t quote at all. By lunch, confusion wins and the cheapest option feels like the only sane choice. But then a friend asks one simple question: “Where is it being done—office, ASC, or hospital?” Suddenly the story changes.
The $650 quote was office-based, no sedation, one level. The $1,900 quote included a facility layer and a written no-surprise estimate. The third place could have been either—nobody knew. The person chooses the option that can name every component in writing. It’s not the lowest number. It is, however, the first number that feels like the truth.

FAQ
1) What is a reasonable self-pay TFESI cost in the US?
There isn’t one universal number because setting and scope matter. A “reasonable” price is the one that is itemized, matches your exact plan (side/level count), and clearly states whether facility and imaging are included. If two quotes can’t be compared on the same plan, the cheaper one may not be cheaper.
2) Does a TFESI cash quote usually include fluoroscopy guidance?
Sometimes yes, sometimes no—depending on how the facility structures the estimate. Don’t assume. Ask directly whether imaging guidance is included and whether any technical imaging charges apply in your setting.
3) Why do ASC and hospital outpatient TFESI totals differ so much?
ASCs and hospital outpatient departments often have different facility fee structures, staffing models, and internal charge frameworks. The injection might be the same; the facility layer often isn’t.
4) How do one-level vs two-level TFESI injections change price?
More levels typically means more time, supplies, and documentation, and it may shift how the procedure is billed. If you want an accurate quote, your estimate must specify level count (and which levels). (If your broader plan includes other procedure options down the road, keep your comparisons clean—don’t mix this with pricing for lumbar facet RFA vs facet steroid injections.)
5) Can I get separate bills even if I’m “self-pay”?
Yes, it can happen—especially in facility settings where multiple entities participate. The protection move is asking, in writing, whether any separate bills will be issued and by whom.
6) Is sedation required for TFESI—and what does it add?
Sedation is not always required. If it is planned, it can add meaningful cost because it may involve additional staff and billing entities. Ask whether sedation is optional for you and whether it’s included in the estimate.
7) What details should I provide to get an accurate quote?
Provide: (1) TFESI (transforaminal), (2) side (right/left/bilateral), (3) level(s), and (4) setting (office/ASC/hospital outpatient). Then ask for a written all-in estimate that states what’s included and whether separate bills apply.
8) When does self-pay ever beat insurance with an HDHP?
Sometimes self-pay can be simpler and occasionally cheaper than paying full contracted rates until the deductible is met—but it depends on your plan, the setting, and whether negotiated discounts apply. If you’re comparing, compare all-in totals and ask how insurance billing would change the final amount.
9) What should I do if the clinic refuses to give CPT-based estimates?
Some places won’t provide codes or itemized details. If they won’t give an all-in estimate in writing, treat that as a risk signal. Consider requesting a different setting, a different facility, or using a hospital price estimator tool where available.
10) TFESI vs interlaminar ESI: are prices comparable?
Not reliably. They can differ in approach, scope, and how a facility bundles charges. If you’re shopping, make sure every quote is for the same approach (TFESI), with the same level count and setting. (If you want the simplest “apples-to-apples” framing, revisit TFESI vs interlaminar ESI for sciatica before you request your next estimate.)
Next step: get a written all-in estimate in 10 minutes
Reader payoff: A concrete action you can do today that reduces surprise-billing risk immediately.
Here’s the simplest next step: send one message that forces clarity. Copy/paste and fill the blanks.
Message to send:
“Hi—I’m self-pay. Please provide a written, itemized all-in estimate for a TFESI (transforaminal) at [LEVEL(S)] on the [RIGHT/LEFT/BILATERAL] side, performed in [OFFICE/ASC/HOSPITAL OUTPATIENT]. Please confirm whether the total includes facility, imaging guidance, supplies, and sedation/anesthesia (if used), and whether I will receive any separate bills from other entities. Thank you.”
- Layer 1: procedure quote
- Layer 2: facility estimate (if ASC/hospital outpatient)
- Layer 3: sedation/anesthesia (if used)
Apply in 60 seconds: Add your three numbers. If any layer is “unknown,” treat the total as “unknown,” too.
Conclusion
Remember the hook: you’re not buying “a shot.” You’re buying a stack of line items—and the surprise happens when one layer stays invisible until later. The fix isn’t complicated or confrontational. It’s one written request that forces clarity: TFESI, side, level(s), setting, what’s included, and whether separate bills apply. (And if your bigger picture is sciatica decision-making, you may want herniated disc sciatica treatment options as a next read so “price” doesn’t become the only decision lever.)
If you only have 15 minutes, do this: send the copy/paste estimate message, then compare two itemized totals side-by-side. Choose the option with the fewest unknowns, not the cutest headline number.
Last reviewed: 2025-12-23
