
A single MRI can swing by thousands—not because the image changed, but because the building did.
If chronic back pain costs have started to feel like roulette—MRI here, PT there, an injection consult “just to see”—you’re not bad at budgeting. You’re stuck inside a system that stacks charges by default: facility fees you never saw coming, prior authorization landmines, and open-ended therapy plans that quietly turn into subscriptions.
Keep guessing and you don’t just lose money—you lose time, momentum, and the ability to make calm decisions while you’re already in pain.
This post gives you a safer, faster way to cut real out-of-pocket spend without skipping care: compare site-of-service before you schedule, force all-in quotes, time imaging to decisions (not anxiety), and run PT on milestones—not vibes.
I’m not handing you “hacky” tricks—I’m sharing the boring, repeatable method that stops cost stacking. Here’s where the money hides. Here’s how to surface it before it lands.
Table of Contents
Cost map first: where the $1,000+ typically hides
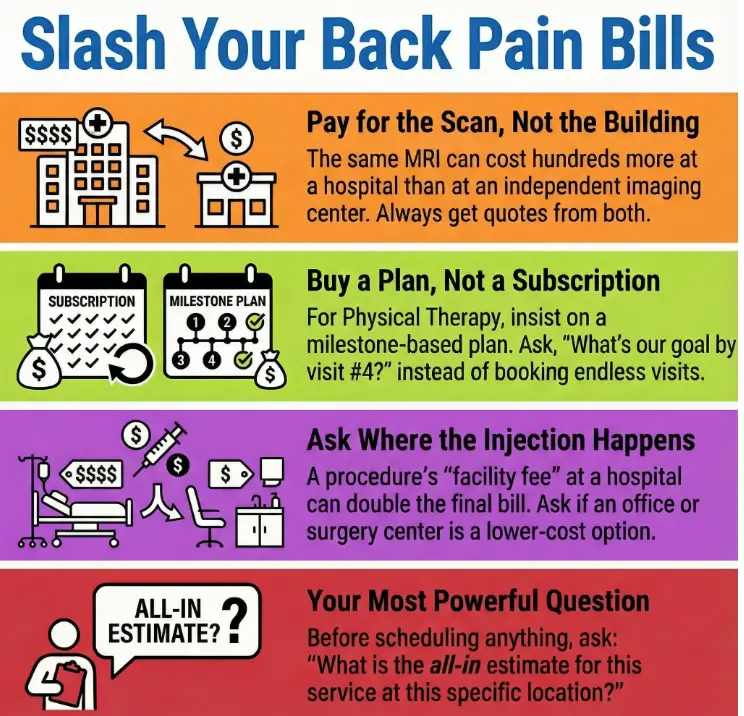
The most expensive part of chronic back pain care isn’t always the “big” thing you fear. It’s the stacking: one test triggers a referral, which triggers a procedure, which triggers a facility fee, which triggers follow-ups you didn’t budget for.
The “three-bucket” bill (MRI, PT, injections)—plus the stealth fourth
- MRI (imaging): price swings wildly by location and billing structure.
- Physical therapy: costs creep when visits don’t have measurable milestones.
- Injections/procedures: the base price is only half the story.
- The stealth fourth: facility fees, “professional vs technical” charges, and repeat visits.
I learned this the annoying way: I once scheduled an imaging appointment because the slot was “available next week.” Then I asked the price. The number was… loud. That’s when I realized the system rewards speed, not clarity.
- Pick the right sequence (exam → plan → pricing → schedule).
- Compare site-of-service (hospital vs independent vs office).
- Get all-in quotes (not “starting at”).
Apply in 60 seconds: Write down the next appointment you’re about to book and ask: “What else could this trigger?”
Open loop: Which single choice most often doubles the final bill?
It’s usually one of these: (1) choosing a high-cost site-of-service (often hospital outpatient), (2) missing prior authorization, or (3) agreeing to “we’ll bill insurance and see” without an all-in estimate. We’ll pin this down section by section so you can spot it before it lands.
- Hospital outpatient: more likely to include facility fees.
- Independent imaging/clinic: often simpler pricing, fewer stacked charges.
- Office-based: may reduce facility fees for certain services.
Apply in 60 seconds: Circle “hospital outpatient” on any upcoming appointment and mark it as “needs a quote.”
Quick cost-comparison table (use this to ask better questions)
| Service | Price driver that varies most | Question to ask |
|---|---|---|
| MRI | Site-of-service + billing split | “What’s the all-in cash price and what’s included?” |
| PT | Visit count + add-on codes | “What’s the plan after 4–6 visits if I’m not improving?” |
| Injection | Facility fees + levels + guidance | “Is this billed as hospital outpatient, ASC, or office?” |
| Follow-ups | Frequency + “routine” imaging | “What’s the next decision point—and what would change it?” |
If you fix Steps 2 and 3 before you schedule, you often prevent the most expensive surprises. If you want a fuller benchmark for what people pay over time, compare this playbook to a typical chronic low back pain cost per year breakdown.
Who this is for / not for (and when saving money is the wrong priority)
This guide is for time-poor, purchase-intent readers—people who want relief and want to stop feeling financially ambushed. But there’s a line: sometimes the safest move is not the cheapest move.
For you if: recurring low back pain bills + unclear next step
- You’ve had pain for weeks/months and the spend keeps growing.
- You feel pushed into “next test, next referral” without a clear plan.
- You want to compare options calmly before you schedule anything new.
Not for you if: red-flag symptoms or rapidly worsening weakness
If you have new or worsening weakness, new bowel/bladder changes, fever, recent significant trauma, a history of cancer with new severe back pain, or numbness in the “saddle” area, treat this as urgent. Saving money is great. Missing something serious is not. If you’re weighing urgency, use this low back pain emergency checklist as a safety-first filter.
Pattern interrupt: Let’s be honest—“cheap” care is expensive if you miss a red flag
I’ve watched smart people bargain with symptoms because they were tired of bills. “It’ll pass.” Then they pay more later, with interest. If you’re unsure, get evaluated promptly—and then use the rest of this guide to avoid unnecessary spending afterward.
Plan before you pay: the one-page “care + cost” brief that stops random ordering
The system moves fast when you’re in pain. Speed can be a gift—until you realize you’ve scheduled three expensive steps without knowing which one actually changes your treatment.
The 7 questions that stop drive-by MRI/PT/injection orders
- What decision will this test/treatment change? (If nothing changes either way, pause.)
- What’s the cheapest step that can answer the same question?
- What must be documented for coverage? (symptoms, exam findings, “failed conservative care”)
- Where is this billed? (hospital outpatient vs independent vs office)
- What’s the all-in cost estimate? (not “we’ll bill insurance”)
- What are the next two steps if it works? and if it doesn’t?
- What’s the stop rule? (when you pause, reassess, or switch plans)
Document it like insurance cares (because they do)
Many insurers approve imaging or procedures based on documented symptoms, exam findings, and prior conservative management. You don’t need to become a coder, but you do want a clean record: what hurts, what makes it worse, what improves it, what you’ve tried, and what function you’ve lost (sleep, walking, work). If conservative care includes meds, it helps to understand NSAID safety for back pain so you’re not “trying things” that quietly create new problems.
Show me the nerdy details
In plain terms: coverage decisions often hinge on “medical necessity.” That’s usually supported by a consistent story (symptoms + duration), objective findings (exam or neuro signs), and a documented attempt at conservative care. If the chart is vague, approvals get harder and bills get messier.
Short Story: The appointment that multiplied
Years ago, I watched a friend schedule an MRI because the pain was relentless and the clinic had an opening. The MRI led to a referral. The referral led to an injection consult. The consult led to a procedure at a hospital outpatient center because “that’s where the doctor operates.” Nobody was malicious—everyone was simply moving the next chess piece. But the bills arrived like confetti. What would’ve changed the whole month? One page of clarity: “What decision does this change? Where will it be billed? What’s the all-in estimate?” It wasn’t about distrust. It was about not sleepwalking into stacked costs.
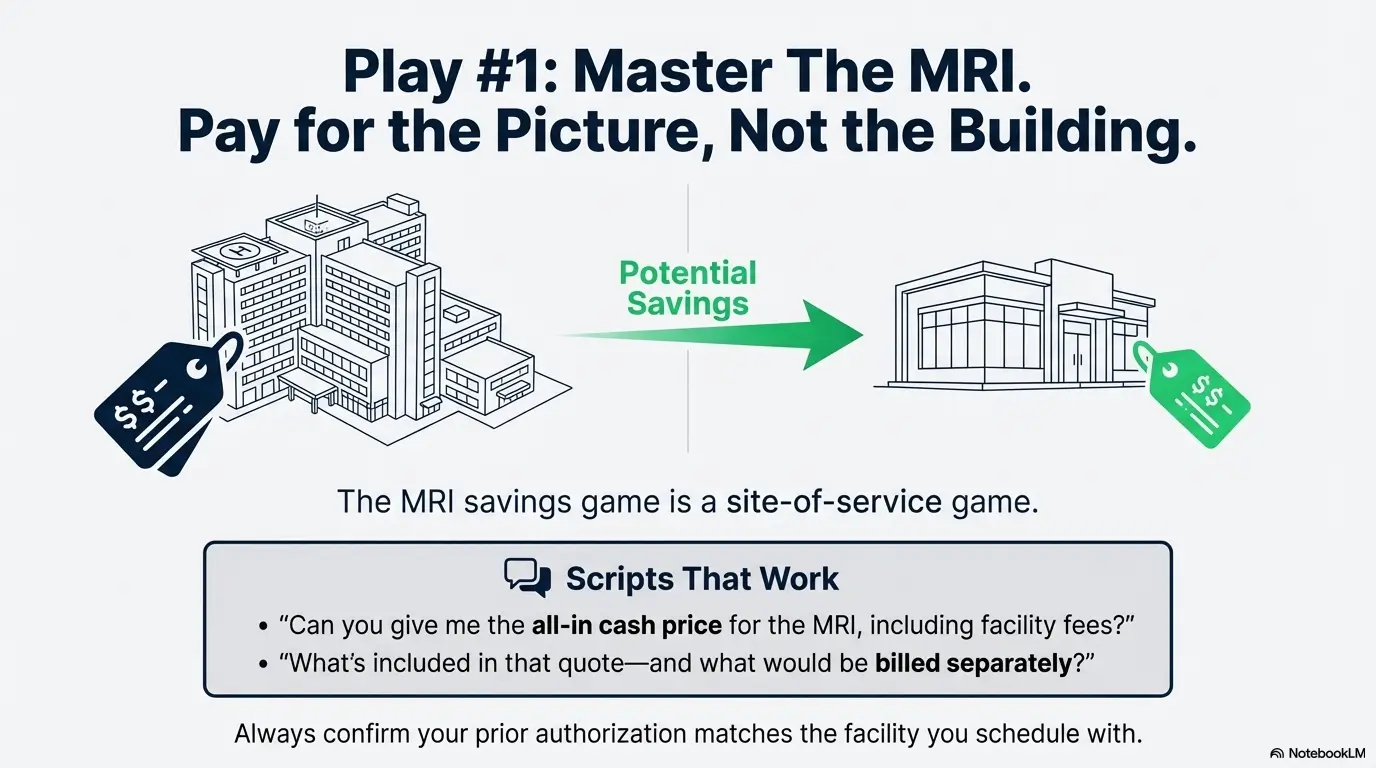
MRI savings: pay for the picture, not the building
MRI pricing is notorious because you’re not only paying for imaging—you’re paying for the billing environment around it. In the US, the same scan can cost dramatically different amounts depending on site-of-service and how charges are split. If you’re on a high-deductible plan, it’s worth reading how lumbar MRI costs work on an HDHP so your “in-network” decision doesn’t turn into an out-of-pocket surprise.
Hospital outpatient vs independent imaging center: what typically changes
- Facility fees: more common in hospital outpatient settings.
- Billing splits: charges may be separated into “technical” and “professional” components.
- Convenience pricing: the building can cost more than the image.
Ask for cash price even if insured (and when it makes sense)
This surprises people: sometimes a cash/self-pay rate can be competitive—especially if you have a high deductible you haven’t met. The goal isn’t to “game” anything; it’s to compare the real out-of-pocket numbers before you commit.
Prior auth basics: how denials become your bill
If your plan requires prior authorization and you skip it, you can end up with a denial that sticks. The safest approach is boring: ask the ordering clinician’s office if they will handle authorization, then confirm with your insurer that it’s approved (and for which facility).
Open loop: The two phrases that unlock the real MRI price on the phone
Try these—calmly, like you’ve done this before:
- “Can you give me the all-in cash price for the MRI CPT and facility fees?”
- “What’s included in that quote—and what would be billed separately?”
You don’t need to win an argument. You need a number you can compare.
- Ask for all-in quotes before you schedule.
- Confirm prior authorization matches the facility.
- Don’t assume “in-network” means “predictable.”
Apply in 60 seconds: Text yourself: “MRI = quote + auth + site-of-service.”
MRI timing: when it helps—and when it quietly triggers more spending
This is where chronic back pain costs get sneaky. An MRI can be genuinely useful—especially with certain symptom patterns—but it can also start a spending chain that doesn’t improve outcomes.
What “conservative care” means in coverage language
Many coverage pathways expect a documented attempt at conservative care (often a combination of time, activity modification, and guided rehab) unless you have red-flag symptoms or significant neurologic issues. That’s not a moral judgment. It’s a bureaucratic reality.
Imaging alternatives: X-ray vs MRI vs reassess
- X-ray: can help screen for certain structural concerns but doesn’t show soft tissues the way MRI does.
- MRI: better for discs, nerves, and soft tissue—but more expensive and more likely to lead to downstream decisions.
- Reassess after a milestone: sometimes the cheapest “test” is a focused plan and a short, timed re-check.
Mistake #1: Booking MRI before clarifying nerve signs vs mechanical pain
If your symptoms are mainly mechanical (worse with certain movements, better with rest/position changes) and there are no red flags, a milestone-based approach can reduce unnecessary imaging. If you have signs of nerve involvement (progressive weakness, significant radiating pain with neurologic findings), your clinician may reasonably escalate sooner. The cost move is not “never MRI.” It’s “MRI at the right time, at the right site, with the right paperwork.”
Show me the nerdy details
Imaging can reveal findings that are common even in people without pain. That can lead to more referrals and more procedures. A good clinician correlates imaging with symptoms and function, not just pictures.
PT savings: build a milestone plan (not an endless visit count)
Physical therapy can be one of the best investments in back pain care—when it’s structured like a plan. When it’s not, it becomes a subscription you forgot you signed up for. If you want a deeper, chronic-specific blueprint, compare this section to a chronic low back pain physical therapy plan so your visits map to outcomes (not calendar weeks).
The “visit math”: why 6 focused visits can beat 18 vague ones
A milestone plan asks: what should change in 2 weeks, 4 weeks, and 6 weeks? Pain scale is one measure, but function is often more useful: walking tolerance, sleep, sitting time, ability to lift, ability to work.
Choose the right PT model: in-network vs cash-based vs hybrid
- In-network: can be cost-effective after deductible, but visit limits and add-ons matter.
- Cash-based: sometimes offers clearer pricing and longer sessions; compare all-in costs.
- Hybrid: a few in-person visits plus a home program can reduce total spend.
How to request a home program that actually replaces visits
Here’s the phrase: “I want a home plan with progression rules—what do I do when this gets easier?” That single question turns PT from “show up forever” into “learn, practice, progress.” If your back pain includes leg symptoms, you may also want a sciatica-focused PT roadmap so your home plan matches nerve-irritation patterns (and doesn’t accidentally flare you).
Pattern interrupt: Here’s what no one tells you—PT costs explode when goals are vague
If the goal is “feel better,” you can always justify another visit. If the goal is “walk 20 minutes without stopping,” you can measure progress and decide rationally.
- Choose A: More visits when you need coaching, red-flag screening, or form correction.
- Choose B: Fewer visits when you can follow a progression plan and track outcomes.
- Set a re-check point at 4–6 visits.
Apply in 60 seconds: Ask your PT: “What’s my milestone by visit 4?”
PT billing traps: the small codes that add up fast
Even when PT is in-network, the out-of-pocket can sting—especially with deductibles, coinsurance, and add-on codes. You don’t need to memorize billing. You do need to recognize patterns.
Eval + re-eval + modalities + add-ons: what to ask before your second visit
- Evaluation: often billed once at the start.
- Re-evaluation: may be billed periodically (ask when and why).
- Modalities: heat, ultrasound, electrical stimulation—can add cost with varying value.
- Therapeutic exercise/manual therapy: core of many plans; clarify time allocation.
Deductible/coinsurance + visit limits: the math most clinics won’t do for you
Clinics can estimate, but insurers define the real out-of-pocket. If you have a high-deductible plan, the first chunk of PT may be mostly on you. That’s not a reason to avoid PT. It’s a reason to demand a plan with milestones. If you’re comparing providers, it can help to read chiropractor vs physical therapy through a cost-and-outcomes lens so “cheaper per visit” doesn’t turn into “more visits forever.”
Mistake #2: Accepting an open-ended plan with no re-check milestone
“Let’s do 2–3x/week for 8 weeks” might be appropriate for some cases—but many people don’t need that cadence for months. A better question is: “What would tell us this plan is working by week 2? What would tell us it’s not?”
Show me the nerdy details
PT billing often reflects time-based units and specific service categories. The practical move is not fighting codes—it’s clarifying what each visit will focus on and whether add-ons are essential or habitual.
Injection costs: what you’re really paying for (and why the same shot can cost 2×)
Spine injections can be valuable for diagnosis and symptom relief, especially when used thoughtfully. But cost variation is massive—often because of where the procedure is performed and how it’s billed.
Epidural vs facet/medial branch blocks vs RFA: don’t mix these up
These procedures are not interchangeable. They target different pain generators and are billed differently. If you’re unclear on which one you’re getting, it’s almost impossible to compare quotes accurately. If your “injection” is really a TFESI, use a self-pay TFESI cost guide to sanity-check quotes and understand what typically gets billed separately.
Office vs ASC vs outpatient hospital: the facility fee trap
The same clinician can perform a similar procedure in different settings. The setting influences whether a facility fee appears and how large it is. This is the “single choice” that can quietly double your final bill.
Coverage rules that change the bill: prior auth, number of levels, diagnosis alignment
- Prior authorization: common for injections.
- Number of levels: more levels can mean more billing complexity.
- Imaging guidance: may affect coding and coverage.
- Diagnosis alignment: the clinical story and documentation matter.
Open loop: The single billing detail that can double your injection price
Ask: “Will this be billed as hospital outpatient, ambulatory surgery center (ASC), or office-based?” Then ask for an all-in estimate for that specific site. If the answer is “we don’t know,” treat that as a sign you need more clarity before you schedule. If you’re comparing ESI approaches, TFESI vs interlaminar ESI can help you ask better “apples to apples” questions before you ever talk price.
Infographic: Where chronic back pain costs stack (and where to intervene)
Step 1: Ordering
Risk: “Schedule first” momentum
Intervene: one-page care + cost brief
Step 2: Site-of-service
Risk: facility fees
Intervene: compare hospital vs independent vs office
Step 3: Authorization
Risk: denial → you pay
Intervene: confirm prior auth + facility match
Step 4: Follow-through
Risk: endless PT / repeat procedures
Intervene: milestones + stop rules
If you fix Steps 2 and 3 before you schedule, you often prevent the most expensive surprises. For facet-driven pathways, it helps to know lumbar facet RFA vs facet steroid injections so you’re not pricing the wrong procedure.
Negotiate like a grown-up: scripts that work (and what to write down)
Negotiation doesn’t have to be aggressive. Think of it as calm procurement. You’re buying a service. You’re allowed to compare.
“Can you quote the total?”—forcing an all-in estimate
Use this exact structure:
- “I’m trying to budget my out-of-pocket cost.”
- “Can you quote the total cost for the service at this location?”
- “What’s included, and what could be billed separately?”
Bundles + prompt-pay discounts + payment plans: what to ask, when
- Bundle ask: “Is there a self-pay package for consult + procedure + follow-up?”
- Prompt-pay ask: “Is there a discount if I pay in full?”
- Plan ask: “What payment options exist if the estimate is higher than expected?”
What to record so the quote doesn’t mysteriously change
Write down: date/time, representative name, facility address, service name, and “all-in quote includes X; excludes Y.” I once forgot this and had to re-run the entire call chain. My spine hurt and my patience hurt too. (If your pathway includes medial branch blocks, you’ll also want clarity on criteria like the percent-relief cutoff for MBB—because “what counts as success” can change what gets authorized next.)
- Ask for “all-in” and “what’s excluded.”
- Confirm site-of-service in the quote.
- Record who told you what.
Apply in 60 seconds: Start a note titled “Back pain quotes” and paste the template below.
Quote-prep list (gather before calling)
- Insurance card (member ID + plan type)
- Ordering clinician name
- Service requested (MRI lumbar spine, PT eval, injection type)
- Preferred location and two alternatives
- Your deductible status (met or not met, if known)
Neutral next step: Pick one item you’re missing and get it before you call.
Mini calculator (no math anxiety)
If you compare two sites-of-service, your savings is often:
Savings ≈ (Higher all-in quote) − (Lower all-in quote)
Now add a “mistake buffer”: if prior auth is missing, assume the risk is the whole amount.
Neutral next step: Get two all-in quotes for the same service and subtract.
Common mistakes that blow up chronic back pain budgets
Most overspending isn’t reckless. It’s tired. It’s pain-brain. It’s “I’ll deal with billing later.” Let’s prevent the predictable losses.
MRI mistakes: wrong site, wrong timing, wrong authorization
- Scheduling at a high-cost site-of-service by default.
- Getting imaging before you know what decision it changes.
- Assuming the clinic handled authorization without confirmation.
PT mistakes: paying for visits instead of outcomes
- No milestones by visit 4–6.
- Add-ons you didn’t agree to or understand.
- Home program without progression rules (so you “need” more visits).
Injection mistakes: wrong facility, missing prior auth, unclear diagnosis coding
- Scheduling in hospital outpatient when an ASC/office option exists.
- Not confirming prior auth and the approved location.
- Not knowing the specific procedure type (so quotes aren’t comparable).
Open loop: Which mistake are you making right now without realizing it?
If you’re feeling stuck, it’s usually one of these two: you’re about to schedule something without an all-in quote, or you’re letting a plan run without a milestone. Fixing either one often creates real savings—fast. If you’re already deep into the “next referral, next procedure” spiral, it can help to recognize the pattern early (and reset expectations) with a failed back surgery syndrome overview—not because surgery is inevitable, but because the cost curve changes when the pathway becomes reactive instead of planned.
When to seek help now (safety)
Cost control is a tool, not a rule. There are symptom patterns where speed matters more than shopping.
Red flags that shouldn’t wait for the cheapest option
- New or worsening weakness in a leg
- New bowel or bladder changes
- Fever with severe back pain
- Recent significant trauma
- History of cancer with new, severe back pain
- Numbness in the groin/saddle area
What to do if you’re unsure: urgent care vs ER vs same-week clinician visit
If any red flag is present, seek urgent evaluation (urgent care or ER depending on severity and access). If you’re unsure but concerned, err toward getting assessed promptly—then return to this guide for the cost-optimized pathway once safety is addressed.
FAQ
How much does an MRI for back pain cost in the US with and without insurance?
It varies widely by location and site-of-service. With insurance, your out-of-pocket depends on deductible and coinsurance. Without insurance (or paying cash), many facilities can provide an all-in estimate—especially if you ask specifically for it before scheduling.
Is it cheaper to get an MRI at an independent imaging center than a hospital?
Often, yes—because hospital outpatient settings are more likely to include facility fees or higher negotiated rates. The only reliable way to know is to request two all-in quotes for the same MRI and compare what’s included.
When will insurance approve an MRI for chronic back pain?
Many plans require documentation that supports medical necessity, sometimes including a period of conservative care (unless red flags are present). The practical move: confirm whether prior authorization is required and ensure the approved facility matches where you plan to go.
How many PT sessions do you really need for chronic low back pain?
It depends on your symptoms and functional goals. A common cost-smart approach is a milestone plan: a few focused visits to assess, teach, and progress a home program—then re-check at a defined point (often 4–6 visits) to decide whether to continue, adjust, or escalate care.
Can I do PT at home to lower costs and still improve?
Often, yes—especially if you have a structured progression plan and clear goals. Many people benefit from a hybrid model: limited in-person sessions for coaching and form correction, plus consistent home work that reduces the need for frequent visits.
What’s the typical cost of an epidural steroid injection (ESI) in the US?
Prices vary significantly by setting (office vs ASC vs hospital outpatient), insurance coverage, and billing details. If you want predictable budgeting, ask for an all-in estimate for the specific site-of-service and confirm prior authorization if required.
Why did my injection bill include a facility fee—and can I avoid it?
Facility fees commonly appear when procedures are billed through hospital outpatient departments and sometimes ASCs. You may be able to reduce this by choosing an alternative setting when clinically appropriate. Ask your clinician’s office whether the procedure can be performed in a lower-cost site-of-service.
Do injections count toward my deductible the same way PT does?
Often they do, but plan rules differ. Some services fall under different benefit categories, and cost-sharing can vary by site-of-service. The clean approach is to ask your insurer how the specific procedure is processed under your plan.
How do I ask for a cash price if I have insurance?
Say: “I’m budgeting my out-of-pocket—can you give me the all-in cash price and what’s included?” Then compare that to your expected insured out-of-pocket based on deductible and coinsurance. You’re not committing; you’re comparing.
What’s the cheapest next step if my back pain keeps coming back?
Usually it’s not “the cheapest test.” It’s the cheapest step that changes your decision. For many people, that’s a focused exam, a milestone-based rehab plan, and two all-in quotes before scheduling anything expensive.
Next step: one concrete action today (20 minutes)
This is where you convert “good intentions” into real savings. You’re going to build a simple, comparison-ready plan—three numbers, one page.
Call one imaging center + one PT clinic + your insurer and build your 3-number plan
- MRI number: all-in estimate at two sites-of-service (same service, same location region).
- PT number: estimated out-of-pocket for the first 6 visits (with a milestone plan).
- Injection number: all-in estimate with site-of-service stated (office vs ASC vs hospital outpatient).
Your mini-template: what to ask and what to write down
3-number worksheet (copy/paste into a note)
- MRI: Location A all-in quote = ____ ; Location B all-in quote = ____ ; prior auth needed? yes/no
- PT: Cost per visit estimate = ____ ; milestone by visit 4 = ____ ; add-ons expected? yes/no
- Injection: Site-of-service = ____ ; all-in quote = ____ ; prior auth approved? yes/no
Neutral next step: Fill in one blank today—any one—and you’ve started saving.
Fastest $1,000+ win: MRI site-of-service check + injection facility fee check
Remember the open loop from the start—the choice that doubles the final bill? For many readers, it’s where the service is billed. Fix site-of-service first, then confirm authorization. That alone can prevent the most expensive surprises.
Safety / Disclaimer
This article is educational and cost-focused, not medical advice. Back pain has many causes, and the safest plan is the one matched to your symptoms and exam. If you have red-flag symptoms (new weakness, bowel/bladder changes, fever, severe trauma, unexplained weight loss, cancer history, saddle numbness), seek urgent evaluation.
Conclusion
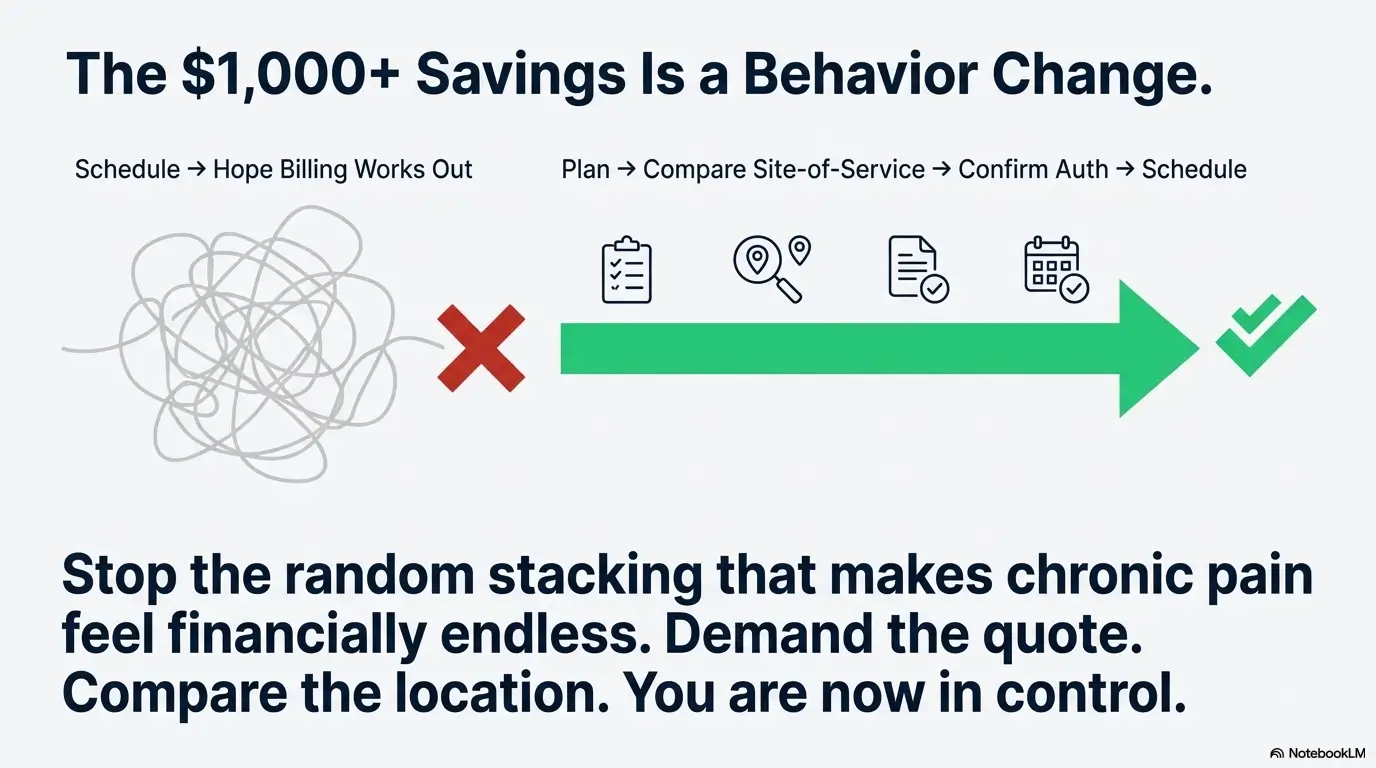
Here’s the punchline you came for—without the drama: the biggest savings in chronic back pain costs usually come from one simple behavior change. Don’t schedule first and hope billing behaves. Build the one-page plan, compare site-of-service, confirm authorization, and demand all-in quotes. That’s how you stop the “random stacking” that makes chronic pain feel financially endless. And if your plan is trending toward a longer procedure pathway, it helps to know what durability can look like—for example, how long lumbar medial branch RFA may last—so you can evaluate “cost per month of relief,” not just the invoice.
If you have 15 minutes, do this: open a note titled “Back pain 3-number plan” and get two quotes for the next service you’re considering. You don’t need perfect information. You just need your first real comparison.
Last reviewed: 2025-12
