
The Reality of Discharge: Navigating Post-Surgical Rehab
Discharge day is when orthopedic pain management stops being a tidy line on a chart and turns into real life. The patient is exhausted, the family is overloaded, and a rehab decision that sounded straightforward in the hospital can become painfully complicated by bedtime.
For families choosing rehab after surgery, the hard part is rarely just pain itself. It is figuring out whether pain control will actually support walking, sleeping, toileting, therapy, and safe recovery in the setting you choose. Home health, skilled nursing, and inpatient rehab can all sound reasonable until medication timing slips, side effects build, or no one is sure who handles a pain spike after hours.
Keep guessing, and the cost is not just stress. It can mean slower recovery, missed therapy, unsafe sedation, preventable setbacks, and one bad night turning into a much bigger problem.
This guide helps you compare rehab options with clearer eyes. You will see how post-surgical pain management really works, which questions expose weak systems fast, and how to choose a setting that protects both comfort and function without drifting into false reassurance.
The approach here is practical on purpose: real family decision points, real rehab trade-offs, real red flags, and the ordinary details that often decide whether recovery steadies or starts to wobble.
Because this is where the choice becomes real. Not in the brochure. Not in the discharge packet. In the middle hours, when pain, mobility, and family capacity finally meet.
Table of Contents
Start Here: What “Orthopedic Pain Management” Really Means After Surgery
It is not just pain relief, but recovery support
Families often hear the word “pain management” and picture pills in a weekly organizer. Real post-op pain management is wider than that. It includes medication timing, icing, elevation, safe movement, bathroom logistics, sleep protection, wound observation, constipation prevention, and the small choreography of daily care. The job is not to erase every ache. The job is to keep pain from hijacking recovery.
The real goal: enough comfort to move, sleep, and heal
After orthopedic surgery, comfort and function need to cooperate. Too little pain control can make the patient guard, refuse movement, skip therapy, breathe shallowly, or stay frozen in bed. Too much sedation can trade one problem for another: dizziness, falls, confusion, missed exercises, and the glassy-eyed feeling families recognize instantly but struggle to describe. The sweet spot is practical, not theatrical. The patient should be comfortable enough to participate, not flattened into stillness.
Why families often underestimate the rehab side of pain control
A surgeon may do excellent work in the operating room, but recovery lives in the hours afterward. I once watched a family compare facilities based on décor and distance from home. The prettier place lost its charm the first night the patient needed help getting to the bathroom and no one explained when pain medication could safely be given again. That is the hidden truth: the rehab setting can amplify or soften pain, not because the surgery changes, but because the surrounding support does.
- Comfort should support walking, transfers, and sleep
- Medication safety matters as much as pain relief
- Rehab quality shows up between therapy sessions
Apply in 60 seconds: Ask yourself whether the current plan helps the patient move, rest, and stay alert enough to participate.
Who This Is For, and Who Should Probably Read Something Else
Best for families choosing between home rehab, skilled nursing, or inpatient rehab
This guide is for the family member who suddenly becomes the organizer, the noticer, the list-maker, and the person everyone turns toward when the room gets quiet. It is especially useful when you are deciding between going home with services, using a skilled nursing facility, or choosing inpatient rehabilitation. That decision is rarely just about convenience. It is about whether the pain plan can survive real life.
Especially relevant after joint replacement, fracture repair, spine surgery, or major orthopedic procedures
The details differ by procedure, but the family questions often rhyme. Total joint replacement patients may need close attention to mobility and swelling. Fracture repair can bring sudden pain spikes with movement. Spine surgery adds a different layer of concern around nerve symptoms, positioning, and walking tolerance. The machinery changes, but the family burden is familiar: who gives what, when, and what do we do if the plan stops working at 8:30 p.m.?
Not for emergencies, uncontrolled pain crises, or situations needing urgent medical review
If pain is severe and suddenly different, or if it comes with chest symptoms, breathing trouble, new confusion, new weakness, calf swelling, fever, or wound drainage, do not use an article as a waiting room. Use the care team or emergency services. A calm internet tab is a poor substitute for a real clinician when the body is throwing flares into the night sky.
- Yes / No: Do you know the patient’s weight-bearing or movement restrictions?
- Yes / No: Do you have the current medication list, including timing?
- Yes / No: Can someone describe what happens if pain spikes after hours?
- Yes / No: Do you know who to call first for a non-emergency pain problem?
- Yes / No: Do you know whether the patient can transfer, toilet, and walk safely today?
Neutral next action: If you answered “no” to two or more items, pause the comparison and get those answers before choosing a setting.
Rehab Choice First: Why the Setting Can Change the Pain Story
Home health rehab: more familiar, but more responsibility falls on family
Home can be emotionally soothing. The chair is known, the hallway is known, the dog may greet the patient like a minor celebrity. But home also turns families into unofficial shift workers. Someone has to manage medication timing, note side effects, assist with transfers, monitor swelling, handle meals, navigate stairs, and call for help when something feels off. When home works, it can feel wonderfully humane. When it does not, it can feel like a small private hospital with none of the staffing.
Skilled nursing facility: more support, but not always the same therapy intensity
A skilled nursing facility can provide nursing oversight, medication administration, and help with daily care. That can be a relief for families who are already wrung out. But the key question is not simply, “Is there staff?” It is, “How does pain management interact with therapy and response time?” A building can have professional staff and still feel sluggish if medication review, night coverage, or therapy coordination is inconsistent.
Inpatient rehab: when mobility goals and medical oversight both matter
Inpatient rehabilitation is usually considered when the patient has meaningful functional goals and also needs closer oversight or a more structured therapy environment. Families often like the idea because it sounds purposeful. Purpose helps, but only if the patient can tolerate the pace and the setting is actually appropriate for the medical picture. Not every patient needs that level. Not every patient can do without it.
The hidden question: who is managing pain between therapy sessions?
Here is the awkwardly important question many families do not think to ask: what happens in the unspectacular middle hours? Not during rounds. Not during therapy. Between them. That is when pain often blooms. That is when a patient decides whether to move, avoid the bathroom, skip a snack, or refuse the next session. The best rehab choice is often the one that handles these ordinary hours well.
Show me the nerdy details
Post-op pain control is rarely a single-ingredient recipe. Orthopedic teams often combine medication and non-medication strategies because pain, swelling, muscle guarding, sleep disruption, and therapy tolerance affect one another. Families do not need to master pharmacology, but they do need to understand timing, expected side effects, and how the setting changes response speed.
Pain Plan Basics: What Families Should Understand Before Discharge
Scheduled medicine vs as-needed medicine
One of the most common family confusions is timing. Some medications are scheduled. Others are given as needed. Those two phrases sound deceptively tidy on paper. In real life, they shape whether pain is prevented or chased. A patient who waits until pain becomes dramatic may need longer to settle. A patient who takes medicine too early or too often can end up sleepy, nauseated, or unsteady. The family does not need to improvise. The family needs clarity.
Ice, elevation, positioning, and timing therapy around pain peaks
Medication is only one instrument in the orchestra. Swelling can increase pressure and stiffness. Poor positioning can turn a manageable evening into a cranky one. Ice and elevation, when approved in the discharge plan, are not decorative wellness gestures. They can make the difference between “I think I can do therapy” and “absolutely not.” Timing matters too. A well-planned therapy session often rides on what happened 30 to 60 minutes earlier.
Why “pain-free” is often the wrong benchmark after surgery
Many families quietly hope they can keep the patient comfortable enough to feel almost normal. That hope is tender and understandable. It is also often unrealistic in the early phase. A better benchmark is this: is the patient safe, able to rest, able to move some, able to eat and drink, and able to participate in the plan? Pain that is present but purposeful is different from pain that is escalating, chaotic, or out of proportion.
Let’s be honest… many families are sent home with instructions that sound clearer on paper than they feel in real life
The discharge packet often has the confidence of a cookbook written by someone who has never seen your kitchen. Families go home and discover the missing parts immediately. Which med is first? What if the patient sleeps through a dose? What if nausea starts after dinner? What if the pain is worse only during standing? This is why written questions matter. It is also why the rehab setting matters. Good systems reduce ambiguity before it becomes panic.
| Situation | Leaning | Trade-off to notice |
|---|---|---|
| Patient is medically stable and family help is reliable | Home rehab may fit | More caregiving falls on family |
| Patient needs more hands-on daily support | Skilled nursing may fit | Response speed and therapy coordination vary |
| Patient has high mobility goals and needs structured oversight | Inpatient rehab may fit | Tolerance for therapy intensity matters |
Neutral next action: Match the setting to the caregiving reality, not the nicest-sounding brochure language.
Don’t Choose Blind: Questions to Ask Every Rehab Option About Pain Control
Who reviews pain meds, and how often?
This question sounds clinical because it is clinical. It is also deeply practical. Families should ask who actually reviews pain medications, how often that review happens, and what triggers a change. If the answer is vague, that vagueness will not become clearer at 2 a.m. Good answers sound specific. They name roles, timing, and process.
How quickly can staff respond if pain suddenly worsens?
Response time matters because pain does not politely worsen during business hours. Ask how urgent pain complaints are handled overnight, on weekends, and during shift changes. You are not being difficult. You are measuring whether the system has bones. A beautifully worded brochure is no match for a slow response to a patient who cannot transfer without severe pain.
What happens when pain blocks physical therapy participation?
Therapy refusal is often interpreted too quickly. Families may hear “noncompliant” when the real story is “timing, swelling, fear, dizziness, nausea, or inadequate pain control.” Ask what the rehab team does when pain interferes with participation. Do they reassess timing? Adjust positioning? Coordinate with prescribers? Or does everyone just stare at the patient’s reluctance like it is a personality trait?
How are nights, weekends, and medication side effects handled?
The glamorous parts of rehab are easy to advertise. The dull parts are where trust lives. Ask how constipation, nausea, dizziness, brain fog, missed sleep, and excessive drowsiness are handled. Pain plans fail quietly when side effects are treated like unrelated inconveniences. They are not. They can derail walking, appetite, therapy, and morale in under 24 hours.
- Ask for process, not reassurance
- Probe nights and weekends
- Watch how clearly the staff answer
Apply in 60 seconds: Write down four questions about meds, response time, therapy barriers, and side effects before the next discharge conversation.
Therapy and Pain: The Line Between Productive Discomfort and a Bad Plan
Soreness after activity vs warning-sign pain
Not all post-therapy pain means harm. Some soreness, fatigue, and stiffness can be part of rebuilding function. But pain that is suddenly sharper, stranger, spreading, or paired with swelling, redness, new numbness, or loss of function deserves a different level of attention. Families do not need a perfect diagnostic vocabulary. They need to notice changes in pattern, quality, and consequence. In some cases, it helps to understand the difference between nerve pain and muscle soreness after physical therapy, because those sensations can lead families toward very different questions.
Why under-treated pain can stall recovery just as much as over-sedation
Families sometimes lean toward toughness because they worry about medication risks. That concern is legitimate. Yet under-treated pain has its own costs. The patient may stop walking, hold their breath during movement, sleep poorly, eat less, or start fearing therapy before it begins. Recovery can shrink around that fear. On the other hand, too much sedation can make therapy feel like a wobbly moonwalk. Neither extreme helps.
How timing medication before therapy can change outcomes
When the care plan allows it, timing can be a quiet hero. A patient who receives appropriate pain relief before therapy may walk farther, transfer more safely, and participate with less panic. This does not mean the answer is always “more medication.” It means timing, route, and coordination matter. A good rehab team knows this. A good family asks about it.
Here’s what no one tells you… the best rehab programs are not the ones that promise comfort only, but the ones that protect function while pain is still real
The honest goal is not to build a cocoon. It is to help the patient function through a temporary difficult season without drifting into unnecessary risk. I have seen families feel guilty when a loved one had pain during therapy, as if any discomfort meant failure. Often the real failure was not the existence of pain, but the absence of a smart plan around it.
Short Story: A daughter I once spoke with kept saying, “He’s stubborn.” Her father had undergone a major orthopedic procedure and was refusing therapy on day three. Everyone in the room was telling a different story. One person said he needed motivation. Another said he was fearful. The daughter looked exhausted and angry with herself for not fixing it. Then someone asked one simple question: when, exactly, had he last received pain medication, and what happened afterward?
The answer changed the room. He was trying to stand at the worst point of his pain cycle, after a poor night’s sleep and with nausea building. The plan shifted. Timing improved. The therapist adjusted the sequence. He still had pain, but he could participate. Nothing magical happened. Something better did. The story stopped being about character and started being about care.
Common Mistakes Families Make When Choosing Rehab After Orthopedic Surgery
Picking the nearest option without asking how pain is actually managed
Nearness matters. Families are tired, traffic is real, parking lots are their own little epic poems of annoyance. But distance is not the whole equation. A closer option that handles pain poorly can cost more time, more stress, and more setbacks than a slightly farther one with better coordination. Convenience is useful. It is not a care model.
Assuming stronger medication automatically means better care
This is one of the biggest traps. Stronger medication can be appropriate in some cases, but it is not a trophy. The right plan is the one that fits the patient’s surgery, age, health history, and response. Families should be especially cautious with the seductive logic that a heavily medicated patient must be a well-cared-for patient. Sometimes the opposite is unfolding quietly in the chair. A broader look at orthopedic pain management can help families step back from the reflex that more medicine must always mean better recovery.
Ignoring how sleep disruption and constipation can worsen the whole recovery picture
Sleep loss can make pain feel louder. Constipation can make everything feel grim, heavy, and harder to tolerate. Nausea can reduce eating and drinking. Dizziness can shrink confidence. These are not side quests. They are part of the main story. MedlinePlus and other patient education sources regularly emphasize that pain medicines can bring side effects families need to notice early, not shrug off three days later when everyone is miserable. For some patients, nighttime positioning issues can compound the problem, which is why it can be useful to think through related sleep setups such as whether a recliner or bed works better after shoulder surgery.
Treating therapy refusal as laziness instead of a pain-management signal
Some patients are indeed frustrated, frightened, or fatigued. But refusal often carries information. Maybe the timing is wrong. Maybe the pain has changed character. Maybe the patient is dizzy, confused, or simply not understanding the goal. Families do better when they translate refusal into questions rather than judgments.
Add these three numbers:
- Minutes needed for medication, icing, and basic monitoring per day
- Minutes needed for transfers, walking help, meals, and bathroom support
- Minutes needed for phone calls, follow-up, and unexpected slowdowns
If the total routinely exceeds the family’s realistic coverage window, home rehab may be harder than it sounds.
Neutral next action: Estimate one ordinary day, not your most heroic day.
Do Not Miss These Red Flags After Transfer to Rehab
Pain that is suddenly worse, different, or out of proportion
Routine post-op pain is one thing. Pain that abruptly changes tone is another. Families should pay attention when the patient says a familiar pain has become sharper, deeper, more constant, more swollen, or “not the same.” The patient does not need elegant wording. “Different” is a useful clinical clue.
Confusion, heavy sedation, or unsafe drowsiness after medication
If the patient seems unusually hard to wake, unsteady, newly confused, or is slurring speech after medication, that deserves timely review. Older adults can be especially vulnerable to medication-related confusion or falls. This is one reason families should not judge a pain plan by comfort alone. Alertness and safety matter too. That balance becomes even more important in orthopedic pain management for older adults, where a narrow safety margin can change the whole recovery rhythm.
Swelling, fever, drainage, calf pain, chest symptoms, or new numbness
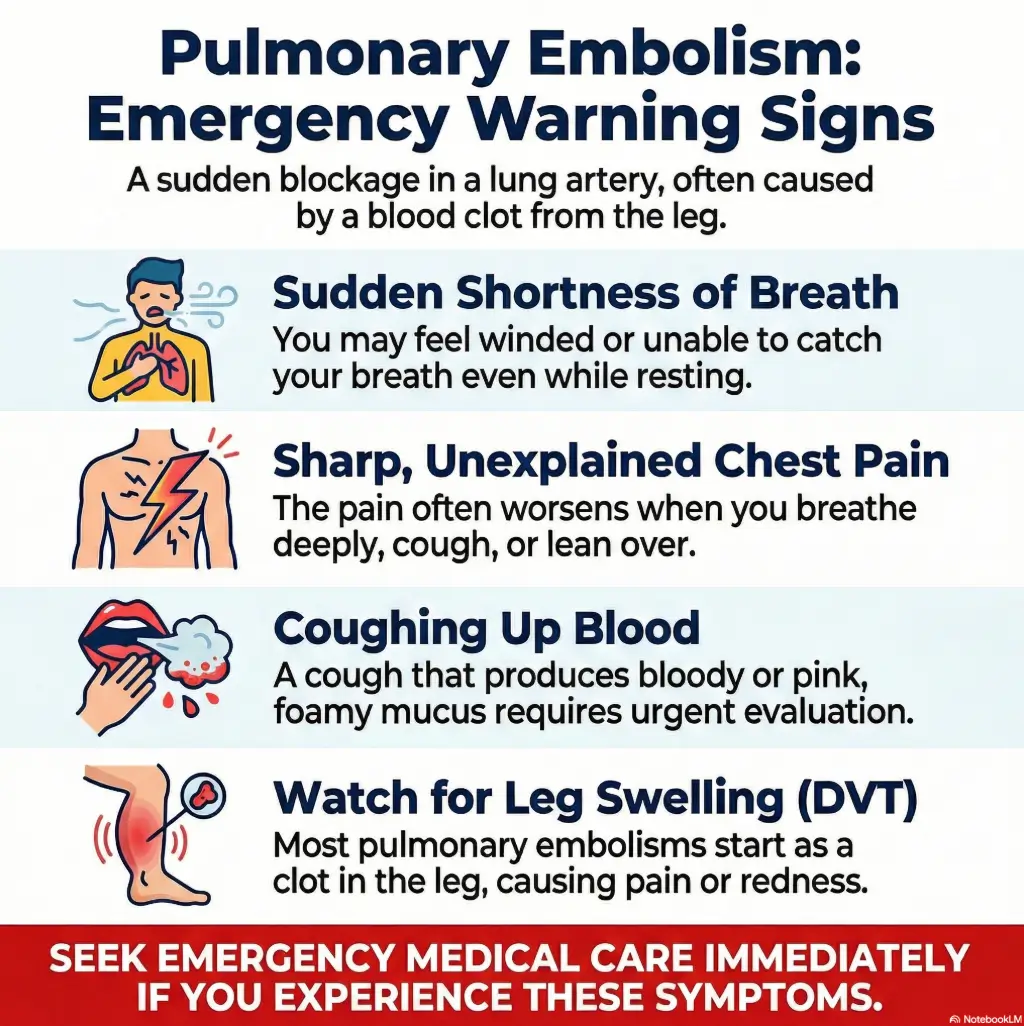
The American Academy of Orthopaedic Surgeons highlights warning signs such as increasing wound redness or drainage, fever, and increasing pain. NIH and MedlinePlus patient resources also describe symptoms of blood clots and pulmonary embolism such as new calf pain or swelling, shortness of breath, and chest pain, especially with breathing. You do not need to memorize every possibility. You do need to treat these symptoms seriously.
When the rehab setting may no longer fit the patient’s needs
Sometimes the issue is not the surgery. It is the mismatch. The patient may need more oversight, a different therapy structure, or a reassessment of the medication plan. Families often hesitate to question the setting once a transfer has happened, as if moving the patient has locked fate into place. It has not.
- Watch for new confusion or unsafe sedation
- Take fever, drainage, calf symptoms, and chest symptoms seriously
- Reassess the rehab setting if the patient keeps outgrowing it
Apply in 60 seconds: Make a tiny red-flag list on your phone so you do not rely on memory when everyone is tired.
Medication Trade-Offs: What Families Need to Watch Without Panicking
Opioids, non-opioids, and why the balance matters
Many orthopedic pain plans use a mix of approaches rather than one medication doing all the work. That balance exists for a reason. Opioids may have a role in acute post-surgical pain, but official guidance from bodies such as the CDC and FDA has also stressed careful use and attention to risk. Non-opioid options and non-medication supports may reduce the total burden when they are appropriate for the specific patient and procedure. Families who are weighing the next step after conservative measures sometimes also benefit from reading about pain management before cortisone injection, because it sharpens the habit of asking what problem each treatment is actually solving.
Side effects that quietly derail recovery: constipation, nausea, dizziness, and brain fog
These side effects are common enough to be boring and important enough to wreck a week. Constipation can make appetite vanish and pain feel worse. Dizziness can make transfers unsafe. Nausea can sabotage hydration. Brain fog can make the patient less able to follow instructions or describe how the pain is changing. Families are not being dramatic when they bring these up. They are doing their job.
Why older adults may need a more cautious pain strategy
Older adults often have narrower margins for medication burden. The body may clear drugs differently. Sedation may last longer. Falls can be more dangerous. Confusion can appear faster than families expect. A cautious strategy is not a lesser strategy. It is often a smarter one. That is especially true for families navigating pain management for seniors waiting on joint surgery and then carrying those same caution habits into the post-op phase.
The family job is not to prescribe, but to notice patterns early
This may be the most useful mindset shift in the whole article. Families do not need to become amateur pharmacists. They need to become excellent observers. What changed after the last dose? What happens before therapy? Is the patient waking up clearly? Are bowel issues building? Is pain more manageable at rest but impossible with transfers? Pattern recognition beats guesswork.
Show me the nerdy details
FDA and CDC materials continue to emphasize that opioid risks include oversedation, breathing problems, and longer-term harms with ongoing use. For families in the immediate post-op phase, the practical lesson is simpler: use the discharge plan exactly, ask before making changes, and report side effects early rather than waiting for a “better” time.
Home Reality Check: Can Your Family Actually Support Rehab Safely?
Who will help with transfers, walking, meals, and medication tracking?
Home recovery sounds gentle because home has emotional furniture. But family support is often the real infrastructure. If one person is doing nearly everything, that matters. If the patient needs help getting up, reaching the bathroom, managing stairs, or tracking meds while another adult is at work, that matters even more. Love is not the same thing as coverage.
What happens at night, on stairs, or during bathroom trips?
These moments are the true exam. Plenty of homes look manageable at noon and impossible at 2 a.m. The distance to the bathroom, the height of the bed, the presence of stairs, the timing of pain medication, and the patient’s steadiness all shape whether home is safe. Families tend to picture the daytime version of recovery and forget the darker, sleepier, more treacherous version. For patients recovering from hip procedures, even ordinary routines like showering after hip surgery can reveal whether the home setup is genuinely workable.
When “recovering at home” sounds comforting but functions like a full-time job
There is no shame in admitting that home is too much. In fact, that honesty can be a form of care. A spouse with back pain, an adult child juggling work, or a household with limited physical help may not be able to safely provide what the patient needs in the first week. That is not failure. That is math wearing sensible shoes.
A useful test: if pain spikes tonight, who responds first?
If the answer is “we are not sure,” or “probably me, alone,” pay attention. A rehab choice should not rely on noble improvisation every evening. It should have an actual plan.
- Current medication list with dosing schedule
- Weight-bearing and movement restrictions
- Baseline mobility: transfers, walker use, stairs, toileting
- Home layout notes: bathroom distance, bed setup, stairs
- Who is available day, evening, and overnight
- Key medical concerns: confusion history, fall risk, bowel issues, nausea
Neutral next action: Put these items on one page so every conversation starts from the same facts.
Mistakes That Cost Progress: When Good Intentions Backfire
Waiting too long to report worsening pain
Families often wait because they do not want to overreact. This instinct is understandable and occasionally expensive. When pain is escalating despite the plan, early contact is usually better than heroic silence. Problems are easier to steer when they are still small and legible.
Stopping movement completely out of fear
After a difficult surgery, fear can become the house manager. Families may start protecting the patient from all movement, hoping to keep pain low. But complete stillness can bring its own trouble: stiffness, deconditioning, slower progress, and sometimes more pain with each attempt to resume. The aim is safe movement within the plan, not a museum exhibit of the recovering body.
Pushing too hard because “therapy must hurt to work”
This old slogan has injured a lot of common sense. Some effort and discomfort can be part of rehabilitation. But pain should not be treated as proof of virtue. The best therapy is not punishment with clipboards. It is structured progress with feedback. When families understand that, they stop equating grimaces with success.
Changing medication timing without checking the discharge plan
Well-meaning relatives sometimes adjust timing on their own, often because they are trying to help. That is risky. The safer move is to call, clarify, and document. Improvisation feels efficient until it collides with dizziness, excess sedation, or under-treated pain.
Compare Smarter: How Families Can Evaluate Rehab Options Without Guesswork
Compare staffing, therapy schedule, pain-response process, and follow-up access
When families compare facilities, they often get flooded with broad promises. Narrow the lens. Who can assess pain changes? How often? What is the therapy schedule? Can therapy timing be coordinated with the pain plan? How does the team handle side effects? Who communicates with the surgeon’s office if the plan is failing? These are decision-grade questions.
Look for care coordination, not just a polished brochure
Some facilities are excellent at sounding excellent. Coordination is harder to fake. Listen for whether nursing, therapy, and prescribing teams seem connected. Disconnected teams create a familiar family nightmare: one person blames another while the patient sits in pain waiting for the chart to catch up.
The best choice is often the place where pain management and mobility planning actually talk to each other
This is the heart of it. The winning setting is not always the fanciest or the closest. It is often the one where movement goals and pain control are treated as one conversation. Families can sense this quickly when staff answer questions with specifics rather than fog. If budget pressure is part of the decision, it may also help to think through the broader cost logic in orthopedic pain management with an HDHP and even practical rehab billing questions like physical therapy copay vs coinsurance.
Use one-page notes so decisions do not get blurred by fatigue and stress
Decision fatigue is real. By the third call, many families can no longer remember which facility said what. Use one page. Same questions. Same columns. Same scoring method. It is not glamorous, but neither is having to reconstruct yesterday’s phone call from memory while balancing a paper cup of hospital coffee.
| Tier | Support picture | Pain-management implication |
|---|---|---|
| 1 | Home, limited help | High family burden, slower response risk |
| 2 | Home with some support | Needs strong planning and clear escalation path |
| 3 | Home health plus reliable caregiver | Can work well if transfers and nights are manageable |
| 4 | Skilled nursing | More oversight, but ask about speed and coordination |
| 5 | Inpatient rehab | Structured therapy and closer monitoring when appropriate |
Neutral next action: Place your patient where their real support tier fits, not where you wish it fit.
Who gives meds, how quickly pain is reassessed, and what happens after hours.
Transfers, walking, stairs, bathroom help, and whether therapy timing supports success.
Watch for constipation, nausea, dizziness, confusion, oversedation, and falls.
Know who to call, when to call, and which symptoms mean urgent help.
When to Seek Help Instead of Waiting It Out
Call the care team for pain that is escalating despite the plan
If the patient is following the plan and pain is still climbing, that is worth a call. So is pain that keeps blocking therapy or basic function. Families do not get extra points for stoicism. They get better outcomes when they report changes clearly and early.
Seek urgent help for breathing trouble, chest pain, severe confusion, or signs of clot/infection
Shortness of breath, chest pain, severe confusion, high fever, wound drainage, or new calf swelling are not “let’s see how tomorrow goes” symptoms. They require prompt medical attention. It is better to feel briefly embarrassed about a false alarm than quietly correct about a dangerous delay.
Contact the surgeon if pain changes alongside wound issues or loss of function
If the wound looks worse, the patient suddenly cannot do something they could do yesterday, or the pain changes in a way that feels wrong, contact the surgical team. Surgeons and their staff would rather hear a precise concern than receive a delayed crisis with a sad little backstory about how no one wanted to bother them.
When family instinct says “something is off,” treat that as data, not drama
Family instinct is not mystical. It is pattern recognition built from attention. If you sense that the patient’s alertness, pain, mobility, breathing, or wound has changed in a concerning way, document what you are seeing and act on it.
FAQ
Is rehab at home better than a facility after orthopedic surgery?
Not automatically. Home may be a strong option when the patient is medically stable, the home layout is manageable, and reliable help exists for medications, transfers, walking, toileting, and follow-up. A facility may fit better when the family cannot safely cover those needs or when the patient needs closer monitoring.
How much pain is normal during post-surgical physical therapy?
Some soreness and discomfort can be expected, especially with movement after orthopedic surgery. What matters is pattern and function. Pain that settles, stays understandable, and still allows progress is different from pain that is escalating, sharply different, or paired with swelling, redness, numbness, severe dizziness, or loss of function.
Can a rehab facility adjust pain medication after surgery?
That depends on the facility’s process and the patient’s care plan. Families should ask who reviews medications, how changes are authorized, how quickly concerns are escalated, and how the rehab team communicates with the surgeon or prescribing clinician.
What if pain keeps the patient from participating in therapy?
That should trigger reassessment, not blame. Ask whether medication timing, swelling control, positioning, nausea, dizziness, or excessive sedation is interfering. A better sequence, rather than simply “more willpower,” may be the real answer.
How do families know whether a rehab center is a good fit?
Look for specifics: therapy schedule, overnight support, medication review process, side-effect management, response time to worsening pain, and communication with the surgical team. A good fit sounds organized, not merely reassuring.
Are stronger pain medicines always better after orthopedic surgery?
No. Stronger medication can be appropriate in some situations, but more intensity is not the same as better care. The right plan balances relief with safety, alertness, mobility, bowel function, sleep, and the patient’s overall risk profile.
When should families worry that post-op pain is not normal?
Worry is reasonable when pain is suddenly worse, feels different, keeps rising despite the plan, or appears with fever, wound drainage, new swelling, calf pain, chest pain, shortness of breath, confusion, or new numbness.
What questions should we ask before choosing inpatient rehab or skilled nursing?
Ask who manages pain after hours, how medications are reviewed, how therapy is timed around pain control, how side effects are handled, how quickly staff respond to pain changes, and how concerns are escalated to the surgeon’s office.
Next Step: Do This Before You Say Yes to Any Rehab Option
Make a side-by-side checklist of pain coverage, therapy timing, staffing response, and after-hours support
Before you decide, make one page with four columns: pain coverage, therapy coordination, side-effect handling, and after-hours response. Under each rehab option, write down what you actually know, not what you hope. Empty boxes are information too. They usually mean the decision is being made in fog.
Ask the surgeon’s office which rehab setting best matches the patient’s procedure and mobility limits
Families sometimes avoid this question because they assume the answer will be generic. Sometimes it is. Sometimes it is the single most clarifying conversation in the week. If the office knows the procedure, restrictions, and expected mobility burden, they can often tell you whether home, skilled nursing, or inpatient rehab sounds more realistic.
Bring one written question list to discharge planning so nothing important gets lost in the shuffle
This closes the loop from the beginning of the article. Discharge day feels chaotic because it is chaotic. The family’s best defense is not perfect memory. It is paper. Or a notes app. Or the back of a visitor pass if that is what civilization has left you. Write the questions down. Ask them in order. Get names. Confirm timing. Clarify who to call. In the first 15 minutes, this is the highest-leverage thing most families can do.
- Match the setting to real caregiving capacity
- Compare pain response, not just location and reputation
- Use written questions to protect decisions from discharge-day fog
Apply in 60 seconds: Start a four-column comparison note before the next conversation with the hospital or rehab team.
Families do not need to become fearless, only clearer. Pain after orthopedic surgery is real, but so is the difference a good rehab fit can make. The right setting will not promise a fairy tale. It will offer something better: a workable plan for comfort, movement, safety, and response when the recovery day gets rough around the edges. If you want a broader companion read, this related guide on orthopedic pain management can help reinforce the bigger picture around function, safety, and day-to-day decision-making.
Last reviewed: 2026-03.
