
Navigating the Divide: Pain Management vs. Orthopedics
Choosing between a pain clinic and an orthopedist sounds like a small scheduling decision, but it can quietly cost people weeks. When orthopedic pain management goes sideways, the trouble is often not the pain alone. It is the wrong first stop, the wrong workup, and the wrong kind of waiting.
That is why this choice feels heavier than it should. Back pain, sciatica, joint pain, nerve symptoms, and arthritis can blur together fast, especially when every clinic page seems to promise help in the same polished language. Meanwhile, your real life keeps shrinking around the pain: sleep gets thinner, work gets harder, stairs become negotiations.
Keep guessing too long, and you can lose time, momentum, and in some cases the chance to catch something that needs faster evaluation. This guide helps you sort the decision more cleanly. You will be able to tell when the smarter first move is an orthopedist, when pain management makes more sense, and when neither is the right answer because red-flag symptoms change the urgency.
Fast Answer: If your pain may come from a structural problem like a fracture, torn tendon, unstable joint, or worsening nerve compression, an orthopedist is often the better first stop. If the diagnosis is already known, surgery is not clearly needed, and the main goal is pain control and function, a pain clinic may fit better. The smartest choice depends on whether you need a cause identified first or symptoms managed first.
Safety / Disclaimer: This content is informational and not medical advice. Severe pain, rapidly worsening weakness, numbness in the groin area, fever with back or joint pain, loss of bladder or bowel control, major trauma, chest pain, or a visibly deformed limb need urgent medical evaluation. AAOS and MedlinePlus both flag weakness, bladder or bowel changes, fever with back pain, and major trauma as reasons to seek prompt care.
Table of Contents

Start Here First: What You Are Really Choosing Between
Orthopedist usually means “What is structurally wrong?”
An orthopedist is trained to evaluate bones, joints, ligaments, tendons, cartilage, and many spine-related structural issues. In plain English, this is the lane for questions like: Is something torn? Is the joint unstable? Is there degeneration, a fracture, or a compressive problem that changes treatment? AAOS patient guidance consistently frames orthopedic evaluation around anatomy, diagnosis, imaging when appropriate, and whether surgical or nonoperative orthopedic treatment is indicated.
Pain clinic usually means “How do we reduce pain and improve function?”
Pain management is usually broader and more symptom-focused. A pain clinic may use medications, targeted procedures, exercise strategies, rehabilitation coordination, and behavior-based tools to reduce pain and improve function. Cleveland Clinic describes pain management as using medications, procedures, exercises, and therapy, often in combination rather than as a one-trick spectacle.
The real fork in the road is diagnosis-first vs relief-first
This is the sentence most people need, and almost no booking page says clearly: if the first unanswered question is what is causing this, orthopedics often makes more sense. If the diagnosis is already fairly clear and the first unanswered question is how do I live better now, pain management may be the better first move. The American Academy of Pain Medicine describes pain medicine as involving identification, diagnosis, and treatment of complex chronic pain, but in real-world care its center of gravity is often function, symptom reduction, and stepwise management rather than “find the torn thing and fix it.”
- Choose orthopedics when structural damage is the main concern
- Choose pain management when the diagnosis is known but daily life is still getting crushed
- Choose urgent care or the ER when red flags appear
Apply in 60 seconds: Write one sentence that starts with “My biggest question is…” and use it to decide where to book.
Who This Is For and Not For
This is for people deciding where to book first for joint, back, neck, shoulder, hip, knee, or nerve-related pain
If your pain lives in that messy intersection where muscle, bone, disc, tendon, and nerve all take turns acting suspicious, this article is for you. It is especially useful when the body part is obvious but the best doorway into care is not.
This is for caregivers trying to avoid specialist ping-pong
Caregivers often become unpaid logistics directors. One office says get imaging first. Another says no, come in first. A third says you need a different specialist. By the third phone call, even the hold music starts to sound judgmental. This guide is meant to reduce that drift.
This is not for emergencies, major injury, or red-flag symptoms
AAOS, MedlinePlus, and NIH-linked resources all treat symptoms like loss of bladder or bowel control, new major weakness, worsening numbness in the groin area, fever with back pain, major trauma, or visible deformity as signs that urgent medical assessment may be needed. This is not the moment for polite optimization. It is the moment for speed.
This is not for people who already have a clear surgical plan in motion
If you have already been evaluated, the anatomy is clear, and a surgeon has outlined a specific plan, your next question is not “pain clinic or orthopedist first?” It is more likely “How do I prepare, confirm, or get a second opinion?” That is a different crossroads.
Eligibility checklist: Is this guide the right tool right now?
- Yes: You are unsure where to start for musculoskeletal pain
- Yes: You want to avoid wasted referrals and repeat visits
- No: You have bowel or bladder changes, severe trauma, visible deformity, or rapidly worsening weakness
- No: You already have a confirmed surgical pathway and are choosing between surgeons or procedures
Neutral next step: If you checked a “No,” seek urgent or direct specialist evaluation rather than using a booking heuristic.
Pain Pattern Clues: When an Orthopedist Often Makes More Sense
Pain after injury, fall, twist, sports trauma, or overuse flare
Orthopedics tends to make more sense when pain begins after a specific mechanical event. A fall. A twist. A pop. A weekend of pretending your rotator cuff is 19 again. Acute injuries raise the odds that the question is structural: fracture, tendon tear, ligament injury, dislocation, or a joint problem that needs hands-on examination and possibly imaging. AAOS knee injury guidance specifically points to popping, giving way, inability to move the knee, limping, and swelling as reasons to get the knee assessed.
Locking, catching, instability, swelling, deformity, or loss of range of motion
These clues matter because they suggest mechanics, not just pain. “It hurts” is one kind of problem. “It buckles when I step off a curb” is another. “It locks halfway down the stairs” is another, especially for readers also weighing support tools like a hinged knee brace for stairs. “My shoulder suddenly will not lift past this angle” is another, and the recovery questions can look different from something like shoulder surgery sleeping setup decisions. These patterns often justify an orthopedic exam because treatment may depend on which structure is failing, not just how intense the pain feels.
Suspected fracture, tendon tear, ligament damage, or joint degeneration
Structural damage does not always mean surgery, but it does usually mean diagnosis matters early. A tendon tear left vague for too long can change recovery options. A fracture you “walk off” can have the social grace of a raccoon in a pantry. Degenerative joint disease may still be managed conservatively, yet orthopedics often helps clarify how much of the pain is wear-and-tear, how much is inflammation, and whether biomechanics are driving the problem. That distinction becomes especially important in older adults, where orthopedic pain management for older adults often requires different pacing and risk trade-offs.
Here’s what no one tells you: “severe pain” is less useful than “what changed suddenly”
People understandably focus on pain level. Clinicians often focus on pattern change. AAOS and MedlinePlus red-flag guidance repeatedly emphasizes weakness, inability to bear weight, major trauma, and bladder or bowel changes rather than using pain intensity alone as the key triage tool. The sharp clinical question is not only “How much does it hurt?” but also “What new loss of function came with it?”
Show me the nerdy details
Structural clues have higher triage value because they change the pretest probability of fracture, tendon rupture, instability, nerve compression, or urgent surgical disease. Pain severity is real and important, but it is noisy. Sudden weakness, deformity, or inability to bear weight is often more decision-shaping than a pain score of 9 out of 10.
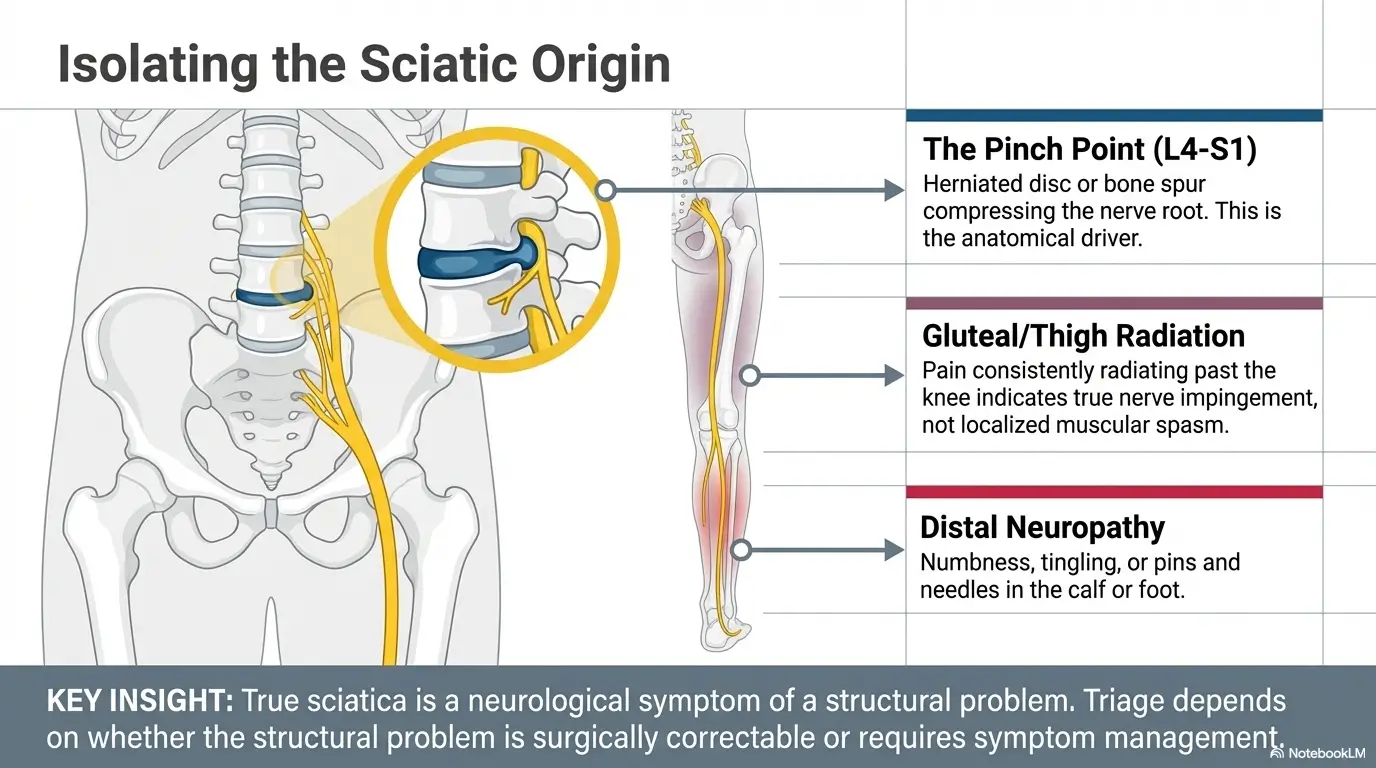
Function First: When a Pain Clinic May Be the Better Entry Point
Long-lasting pain with a known diagnosis and no clear surgical target
If you already know the diagnosis, or at least know the broad neighborhood of the diagnosis, pain management may be the cleaner first stop. Think chronic back pain, sciatica with prior workup, arthritis-related pain, spinal stenosis already identified, or post-surgical pain that did not politely leave when the stitches did. A pain clinic is often most valuable when the puzzle is not “What is this?” but “How do we make life possible while we manage it?” Cleveland Clinic describes pain management as combining therapies rather than relying on one lane alone.
Back, neck, or nerve pain that needs stepwise non-surgical management
Back and neck pain are classic places where patients get lost. Not every episode needs an orthopedic surgeon first. Not every case needs an MRI in the opening scene. Not every injection is a shortcut to paradise. AAOS notes that low back pain often improves with conservative care, while advanced imaging and specialist escalation depend on pattern, persistence, and red flags. Pain clinics are often strong when the plan needs to be stepwise, non-surgical, and function-focused. For office workers, this may overlap with practical ergonomic fixes like keyboard and mouse placement for desk-job sciatica or broader orthopedic pain management strategies for remote workers.
Medication review, injections, rehabilitation coordination, and symptom control
Pain specialists may help with targeted injections, medication strategy, rehab coordination, and goal-setting around sleep, walking, work tolerance, and flare control. This matters because many patients do not need a miracle. They need the week to stop falling apart. The month to become livable again. The ability to sit through a meeting without negotiating with their own spine like it is a hostile foreign state.
When the goal is not cure today, but getting life back this month
That is not a lesser goal. It is often the most honest one. The American Academy of Pain Medicine notes that chronic pain self-management and support matter because cure is rare and complete pain relief is even rarer. That sounds sobering, but it can also be freeing. You do not need a cinematic ending by Friday. You need traction.
- Known diagnosis usually favors relief-first care
- Back and neck pain often need stepwise non-surgical management
- Good pain care is about function, not just pain scores
Apply in 60 seconds: List your top two goals: pain reduction, sleep, walking, work, or avoiding surgery. That goal list points toward pain management.
The Diagnosis Trap: Why Starting in the Wrong Place Can Waste Weeks
Pain control without a clear workup can delay the real answer
Sometimes relief-first care is exactly right. Sometimes it becomes a velvet curtain in front of an unanswered diagnosis. Sciatica, for example, is not really a diagnosis so much as a pain pattern. AAOS explains that sciatica is a broad term for nerve pain and that the real diagnosis is the cause of nerve compression, such as a herniated disc or spinal stenosis. If the cause is still foggy, symptom treatment alone can leave the patient improved but directionless. That is one reason many patients end up comparing sciatica MRI vs X-ray questions too early or too vaguely.
Structural workups without a function plan can leave people hurting longer
The reverse is also true. Patients can get imaging, labels, and highly detailed anatomical vocabulary, then go home still unable to sleep, work, or sit comfortably. An MRI can tell a precise story while daily life continues to collapse around breakfast. A strong plan needs both: diagnostic clarity and function strategy. When scan findings and symptoms do not line up neatly, the problem can start to resemble the frustrating terrain of MRI pain mismatch.
Referral loops, repeat imaging, and “come back later” fatigue
One quiet cost of starting in the wrong lane is not just time. It is morale. You repeat your story. You carry discs and reports like a traveling exhibit. You hear “let’s wait and see” from people who are not the ones missing shifts or waking at 3 a.m. This is one reason a clean first question matters. It shortens the loop.
Let’s be honest… most patients are not confused about pain, they are confused about the system
I have watched otherwise decisive adults freeze at this step. Not because they are weak. Because modern specialty care speaks in doors, not maps. And when every door has a scheduling link, all of them start looking equally official. The system rewards knowing the language in advance. This article is trying to hand you the phrasebook.
Decision card: When A vs B
| If your real question is… | Usually start here | Trade-off |
|---|---|---|
| What is torn, broken, unstable, or compressed? | Orthopedist | May solve diagnosis first, function plan second |
| How do I reduce pain and function now? | Pain clinic | May improve symptoms before root-cause clarity is complete |
| Am I having urgent neurologic or trauma red flags? | Urgent or emergency evaluation | Speed matters more than perfect specialist matching |
Neutral next step: Choose the lane that answers your first unanswered question, not the one that merely sounds familiar.
Don’t Do This: Common Mistakes That Make Orthopedic Pain Harder to Untangle
Waiting too long because you hope it will “settle down”
Some pain absolutely does settle down. Some does not. AAOS notes that low back pain often improves with time and conservative treatment, but persistent symptoms, weakness, or bladder or bowel changes change the urgency. The mistake is not optimism. It is optimism with no decision point attached.
Choosing only by who can see you fastest
Speed matters, but only up to a point. The fastest appointment in the wrong lane can still lengthen the whole journey. A same-week visit that cannot answer your main question sometimes only adds one more note to the chart and one more place to park badly.
Assuming injections and surgery are the only two options
This false binary wastes a lot of emotional energy. Many patients sit between those poles: physical therapy, medication adjustment, activity modification, rehab strategies, sleep improvement, weight-bearing advice, ergonomic changes, and time-limited interventional procedures. Medicine is often less like a duel and more like a toolkit drawer. For some people, cost questions also muddy the picture early, whether they are estimating a joint injection consultation cost or comparing physical therapy copay vs coinsurance.
Using pain intensity alone to choose the specialist
A dramatic pain number can come from a non-surgical flare. A tolerable pain number can hide a more urgent neurologic issue. MedlinePlus and AAOS both emphasize associated findings like weakness, trauma, fever, inability to bear weight, and bowel or bladder symptoms, not just intensity. Severity matters. Pattern matters more.
Imaging, Injections, and Procedures: What Patients Often Get Backward
An orthopedist may focus on diagnosis, biomechanics, and surgical decision points
This is why orthopedics can be especially useful when your symptoms suggest a structural driver. The exam is not only about pain. It is about stability, range of motion, strength, mechanical symptoms, and how the anatomy behaves under load. For spine complaints, that may include sorting nonspecific back pain from disc, stenosis, spondylolisthesis, or myelopathy patterns. AAOS materials on herniated disc, stenosis, and cervical myelopathy all emphasize pattern-based diagnosis and escalation based on neurologic signs and structural findings.
A pain clinic may focus on nonoperative pain strategies and interventional relief
That can include injections, medication changes, rehab planning, and realistic goal-setting around function. Cleveland Clinic’s pain management pages describe an assessment-first approach followed by treatment planning that may combine several methods. The key idea is not “pain clinic equals shots.” It is “pain clinic equals structured symptom and function management.” Patients trying to compare procedures often benefit from more specific distinctions such as nerve root block vs ESI or SI joint injection vs lumbar ESI before assuming every injection does the same job.
Not every MRI changes treatment
This is one of the most emotionally difficult truths in musculoskeletal care. People often feel, quite reasonably, that a scan means certainty. Sometimes it does. Sometimes it mostly gives the pain a high-resolution biography. AAOS notes that MRI helps visualize soft tissues and may be used when a disc problem, infection, or other specific concern is suspected. That is different from “everyone with back pain should start with MRI.” Insurance friction can also distort timing, especially when patients are navigating orthopedic pain management after an MRI denial appeal or trying to document failed conservative care for MRI approval.
Not every injection solves the underlying problem
Injections can be valuable. They can calm inflammation, reduce pain enough to restore motion, and sometimes help confirm the pain generator. But they are not magical erasers. If the core issue is instability, severe compression, or a major tear, symptom relief may be real without being the end of the story. Even when injections work, the lived question often becomes what to expect from the epidural steroid injection relief timeline or from a temporary steroid flare after injection.
Show me the nerdy details
Imaging is most useful when it changes management. In orthopedics and spine care, that usually means suspected structural pathology, red flags, or symptoms that persist despite conservative treatment. Injections can be therapeutic, diagnostic, or both, but their value depends on matching the procedure to the likely pain generator and the broader care plan.
- MRI is a tool, not a trophy
- Injections can help without fixing the root cause
- Good care links diagnosis, treatment, and function
Apply in 60 seconds: Before any procedure or imaging request, ask, “How will this result change my treatment?”
Body Region Matters: The Best First Stop Often Depends on Where It Hurts
Shoulder, knee, hip, hand, foot, and sports injury pain
These regions often lean orthopedic first, especially after injury or when there is swelling, catching, instability, weakness, or loss of motion. Knees that buckle, shoulders that suddenly stop lifting, ankles that cannot bear weight, or hands that lose function after trauma usually deserve structural assessment. HSS and AAOS guidance both point patients with acute injury signs toward orthopedic evaluation. In practice, some of these cases later branch into narrower questions like whether a TENS unit helps knee pain, what hip pain at night may signal, or even how pickleball hip pain behaves differently from ordinary soreness.
Back and neck pain with or without radiating nerve symptoms
This is the most mixed territory. Back pain without red flags often begins with conservative care. Back or neck pain with nerve symptoms may still be non-surgical, but progressive weakness, gait problems, worsening numbness, or bladder or bowel changes raise the urgency. AAOS, NIAMS, and MedlinePlus all flag weakness and elimination changes as more serious signs in spinal conditions. When the picture is muddy, it can help to think through comparisons like hip vs spine pain, sciatica vs herniated disc, or region-specific patterns such as L4 vs L5 vs S1 sciatica.
Arthritis pain vs acute injury pain vs unexplained pain
Arthritis pain often straddles the line. If you already know you have arthritis and the problem is day-to-day symptom control, pain management may help. If the joint is suddenly much worse, swollen, unstable, or hard to move, orthopedics may be the wiser first step. Unexplained pain, especially with neurologic or systemic symptoms, should not be forced into a neat category just because scheduling websites demand confidence you do not have.
One body part, three very different care paths
A knee can hurt because of arthritis, a meniscus tear, referred hip mechanics, inflammatory disease, nerve irritation, or a fresh ligament injury. The body part is the same. The route is not. That is why region matters, but pattern matters more.
Coverage tier map: What often changes from Tier 1 to Tier 5 concern
- Tier 1: Mild flare, no red flags, function mostly intact
- Tier 2: Persistent pain, known diagnosis, sleep or activity affected
- Tier 3: Mechanical symptoms, repeated flares, work or walking limited
- Tier 4: Inability to bear weight, marked weakness, major motion loss, or deformity
- Tier 5: Bladder or bowel changes, saddle numbness, fever with spine or joint pain, major trauma
Neutral next step: Tiers 1 to 2 often allow thoughtful booking. Tiers 4 to 5 deserve urgent escalation.
Surgery Question: Are You Trying to Avoid Surgery or Find Out If You Need It?
Orthopedist is often stronger when the question is “Is something torn, broken, unstable, or surgical?”
This is the home turf of orthopedics. It does not mean every orthopedic visit ends with surgery. In fact, many do not. It means the clinician is well-positioned to decide whether surgery is unnecessary, premature, reasonable, or urgent. That distinction matters more than the internet’s favorite drama: “Will they push surgery?” The best orthopedic visit often rules surgery out just as usefully as it rules it in.
Pain clinic is often stronger when the question is “How can I function better without surgery?”
That question is not timid. It is strategic. Many people are not anti-surgery. They are trying to understand whether they can walk, sleep, work, parent, drive, and exercise better without crossing that bridge yet. Pain management can be the right answer when nonoperative quality-of-life improvement is the actual mission.
The best visit starts when you know which question you are actually asking
I have seen patients say they want to avoid surgery when what they really want is to avoid an unnecessary surgery. Those are not the same sentence. Others say they want pain relief when what they really want is certainty. Again, not the same sentence. Clarity here saves weeks.
Short Story: A friend once spent nearly two months chasing lower back and leg pain. First urgent care, then general follow-up, then a well-meaning detour into medication tweaks that helped but did not explain much. At every step, the story got flatter: pain score, duration, refill, next appointment.
What finally changed things was one small sentence: “I need to know whether this is just pain or actual nerve compression.” That sentence shifted the visit. The exam became sharper. The questions changed. The referral changed. Nothing magical happened overnight, but the path stopped wobbling. That is the point. Sometimes the body does not need a louder complaint. It needs a clearer question.
Red Flags First: When to Seek Help Urgently
New weakness, foot drop, or rapidly worsening numbness
New or worsening neurologic deficits should not be shrugged off as “probably inflammation.” AAOS, MedlinePlus, and NIH-linked resources all flag weakness, progressive sensory change, gait trouble, or loss of movement as warning signs that may require prompt assessment. Foot drop, for example, is not a decorative symptom. It means the mechanics of walking are already being changed by a neurologic problem.
Fever, chills, or unexplained illness with back or joint pain
Back or joint pain paired with fever, chills, redness, swelling, or systemic illness deserves more caution than ordinary strain. AAOS and MedlinePlus both identify fever with back pain as a reason to seek medical attention because infection and other serious causes need to be considered.
Loss of bladder or bowel control, saddle numbness, or severe neurological changes
This is the classic do-not-wait group. Cauda equina syndrome is rare, but AAOS explicitly calls it a surgical emergency, and NIH-linked resources describe bladder or bowel dysfunction and saddle anesthesia as key warning symptoms. If these appear, do not turn this into a leisurely specialist-shopping exercise. For a more focused breakdown, see cauda equina syndrome red flags.
Trauma, visible deformity, or inability to bear weight
Serious falls, twisting injuries with immediate swelling, a limb that looks deformed, or a joint that cannot bear weight push the situation out of routine booking territory. HSS, MedlinePlus, and AAOS all treat inability to bear weight, major injury, or deformity as reasons for faster evaluation. Similar urgency logic also shows up in broader guides to when low back pain is an emergency.
Infographic: The 3-door triage map
Door 1: Urgent evaluation
Go here first for bladder or bowel changes, saddle numbness, new major weakness, major trauma, visible deformity, or fever with significant back or joint pain.
Door 2: Orthopedics
Go here first when the question is structural: fracture, tear, instability, locking, catching, sudden motion loss, or possible surgical disease.
Door 3: Pain management
Go here first when the diagnosis is known or partly known, surgery is not clearly needed, and the main goal is better function, sleep, work tolerance, and symptom control.
- New weakness changes urgency
- Bladder or bowel symptoms are emergency-level clues
- Fever with spine or joint pain deserves prompt medical attention
Apply in 60 seconds: If any red flag is present today, stop comparing clinics and seek urgent evaluation.
Visit Smarter: What to Bring So the First Appointment Is Not a Dead End
Exact pain location, trigger pattern, and what movement makes it worse
Do not bring only the pain score. Bring the map. Is it in the groin, buttock, joint line, shin, low back, shoulder blade, or hand? Does it hurt when rising from a chair, climbing stairs, looking up, reaching overhead, standing still, or walking downhill? Specifics help more than adjectives. “Burning down the leg below the knee” tells a different story than “my back is killing me.” MedlinePlus specifically notes pain traveling below the knee as a pattern worth mentioning in back pain evaluation.
Prior imaging, procedure history, medication list, and therapy attempts
Bring what has already happened. X-rays, MRI reports, procedure notes, medication list, prior injections, physical therapy attempts, and what helped or failed. This reduces duplication and helps the first visit build rather than restart. For patients paying out of pocket or carrying a high-deductible plan, it can also help to know the landscape around a self-pay cash price range or an HDHP imaging cost estimate before agreeing to repeated testing.
What you want most: diagnosis, relief, function, sleep, work ability, or surgery opinion
This may be the most underrated preparation step. Say the priority out loud. If your job involves lifting, say that. If your biggest fear is surgery, say that. If your biggest fear is missing one more month of work, say that. Clinicians are not mind readers, and your chart will not always volunteer your actual life.
Here’s what no one tells you: the clearest patient history often beats the longest pain story
I say this gently because pain makes people narrate in spirals. Understandably. But a compact timeline usually wins. What changed. When. What movement triggers it. What symptoms came with it. What function is now limited. That is gold.
Quote-prep list: What to gather before comparing specialists
- Date and trigger of onset
- One-sentence goal for the visit
- Key function loss: walking, sleep, work, stairs, lifting, dressing
- Prior imaging and reports
- Medication list, therapy history, and any prior injections or surgeries
Neutral next step: Put these in your phone notes before you book. It makes almost every visit better.
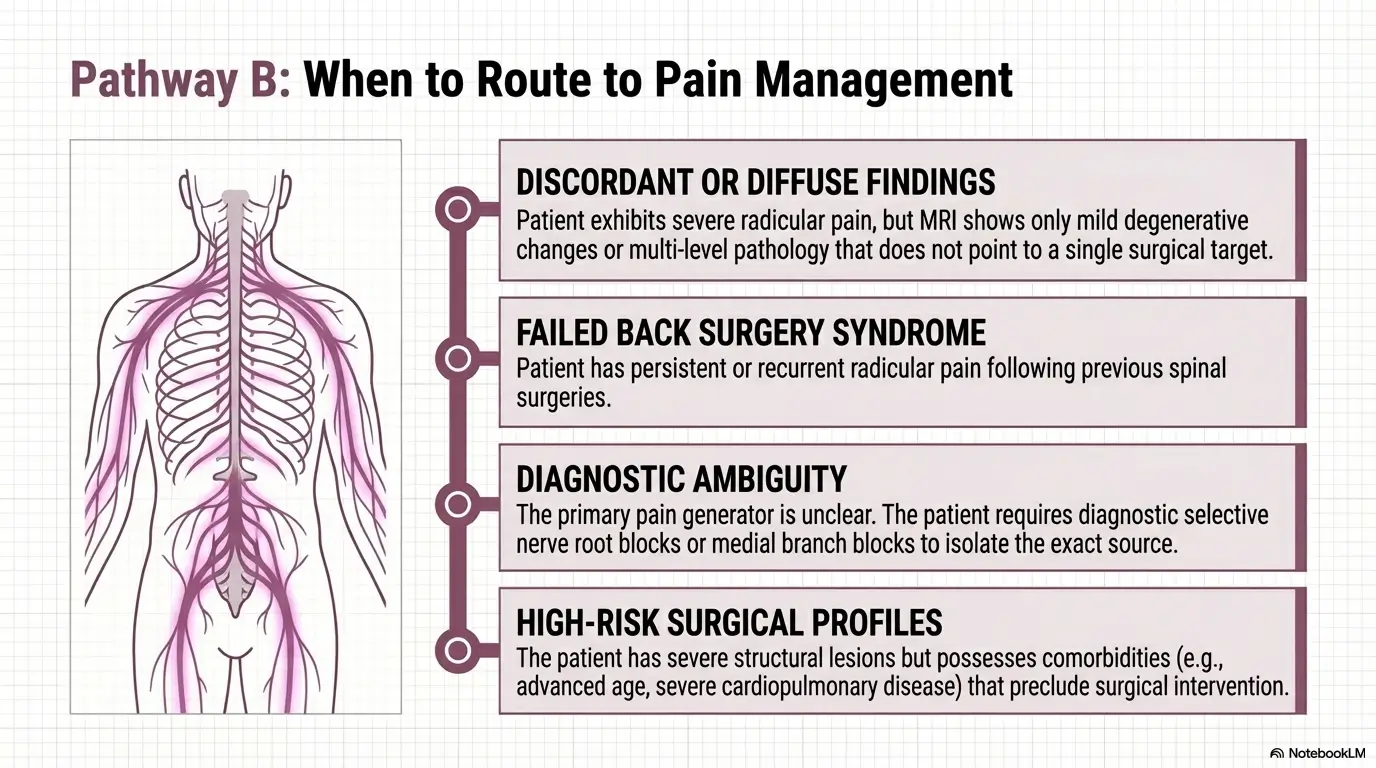
FAQ
Should I see a pain clinic or orthopedist for back pain?
It depends on the pattern. If your back pain is new after trauma, involves major weakness, loss of bladder or bowel control, gait changes, fever, or a concern for structural compression, orthopedics or urgent evaluation is often more appropriate. If the diagnosis is already partly known and the main need is non-surgical pain and function management, a pain clinic may fit better. AAOS and MedlinePlus both emphasize red flags like weakness and bladder or bowel changes in back pain triage.
Can a pain clinic diagnose the cause of my pain?
Sometimes, yes. Pain medicine is not diagnosis-free territory. AAPM describes pain medicine as involving identification, diagnosis, and treatment of chronic pain conditions. But if your core question is whether there is a fracture, tear, instability, or a surgical spine issue, orthopedics is often a more direct starting lane.
Do I need an MRI before seeing either specialist?
Usually not by default. MRI can be very helpful when symptoms suggest a disc problem, infection, nerve compression, or another specific structural issue, but not every case needs immediate advanced imaging. AAOS explains MRI as a tool that is useful in the right context rather than a universal first step.
Is an orthopedist only for surgery?
No. Many orthopedic visits are diagnostic or nonoperative. Orthopedists often guide bracing, activity modification, rehab, imaging decisions, injections in some settings, and whether surgery is unnecessary. One of the quiet benefits of orthopedics is getting a clean answer that surgery is not the right move.
Can I go to a pain clinic first for sciatica?
Yes, in some cases, especially if the diagnosis is already known and there are no red flags. But AAOS notes that sciatica is a symptom pattern rather than a final diagnosis, so unexplained or worsening nerve symptoms may still require structural evaluation. Progressive weakness, bladder or bowel changes, or rapidly worsening neurologic symptoms should push urgency much higher. Readers who are still sorting the symptom picture sometimes need narrower comparisons such as sciatica vs piriformis syndrome or even diabetic neuropathy vs sciatica.
Who treats arthritis pain better?
There is no universal winner. If the issue is known arthritis and the main need is symptom control and daily function, pain management may help. If the issue is whether the joint is mechanically failing, suddenly worsening, unstable, or at the point where orthopedic options need review, orthopedics may be the better first stop. Sometimes both are useful at different stages.
When should nerve symptoms change where I go first?
Nerve symptoms become much more urgent when they include progressive weakness, foot drop, balance problems, saddle numbness, or bladder or bowel changes. NIH-linked and AAOS resources treat these as warning signs that may require prompt specialist or emergency assessment rather than routine scheduling.
What if I have chronic pain and a new injury at the same time?
In that case, the new injury often deserves priority because it may represent a new structural problem layered on top of an old pain condition. Chronic pain history can make people underreact to fresh danger signals. If the new event caused instability, swelling, deformity, major motion loss, inability to bear weight, or new neurologic changes, start by ruling out the new structural issue.
Next Step: Use This One-Question Filter Before You Book
If your first question is “What is damaged?” start with orthopedics
Use this when the pain followed injury, the joint feels unstable, something locks or catches, you suspect a tear or fracture, or nerve compression seems to be escalating. Orthopedics is usually the cleaner first lane when anatomy itself is the question.
If your first question is “How do I reduce pain and function now?” start with pain management
Use this when the diagnosis is already known or partly known, the issue is chronic or recurrent, surgery is not clearly needed, and your real goal is better sleep, walking, work tolerance, and less daily disruption. Relief-first care is not giving up. It is choosing the problem you most need solved first.
If red flags are present, skip both and seek urgent care immediately
When bladder or bowel changes, saddle numbness, fever with back or joint pain, visible deformity, inability to bear weight, or rapidly worsening weakness enter the story, the choice is no longer “pain clinic or orthopedist?” It is “How fast can this be medically assessed?” AAOS, MedlinePlus, and NIH-linked resources are aligned on that basic point.
Mini calculator: Which lane fits better?
Count 1 point for each “yes”:
- There was a clear injury or sudden mechanical change
- You have locking, buckling, deformity, or inability to bear weight
- You mainly want to know what is structurally wrong
2 to 3 points: Orthopedics is often the better first stop.
Now count 1 point for each “yes”:
- The diagnosis is already known or partly known
- Surgery is not clearly needed right now
- Your main goal is function, sleep, work, or flare control
2 to 3 points: Pain management may be the better first stop.
Neutral next step: If red flags are present, ignore the score and seek urgent medical evaluation.
The hook at the start of this article was the feeling that choosing the appointment can hurt almost as much as the condition. Here is the honest closing thought: the system becomes far less confusing when you stop asking, “Which specialist treats pain?” and start asking, “What problem do I most need solved first?” That one shift untangles a lot.
In the next 15 minutes, write down three things: what changed, what function you lost, and the single question you want answered first. Then book based on that. It is a small act, but in musculoskeletal care, small acts often open the right door.
Last reviewed: 2026-03.
