
The 15-Minute Trap: A Post-Microdiscectomy Guide to Sitting and Driving
At first, 15 minutes feels like nothing. After a lumbar microdiscectomy, it can be the difference between a calm evening and a midnight flare that rewrites tomorrow.
The problem isn’t permission. It’s the sneaky combo of car-seat flexion, vibration, and nerves that complain on a delay. You “do fine” during the ride and pay for it 2–12 hours later. Keep guessing, and you risk turning a simple pharmacy run into a 3-day setback.
- Time-based & symptom-based timelines
- Driving readiness checklist
- Passenger-ride trap avoidance
- Practical car setup tweaks
Deliberately unglamorous: timers, resets, and next-morning feedback. Because nerves don’t care about optimism.
Read this like a dose plan. Not a dare.
Let’s keep your progress cheap.
Table of Contents
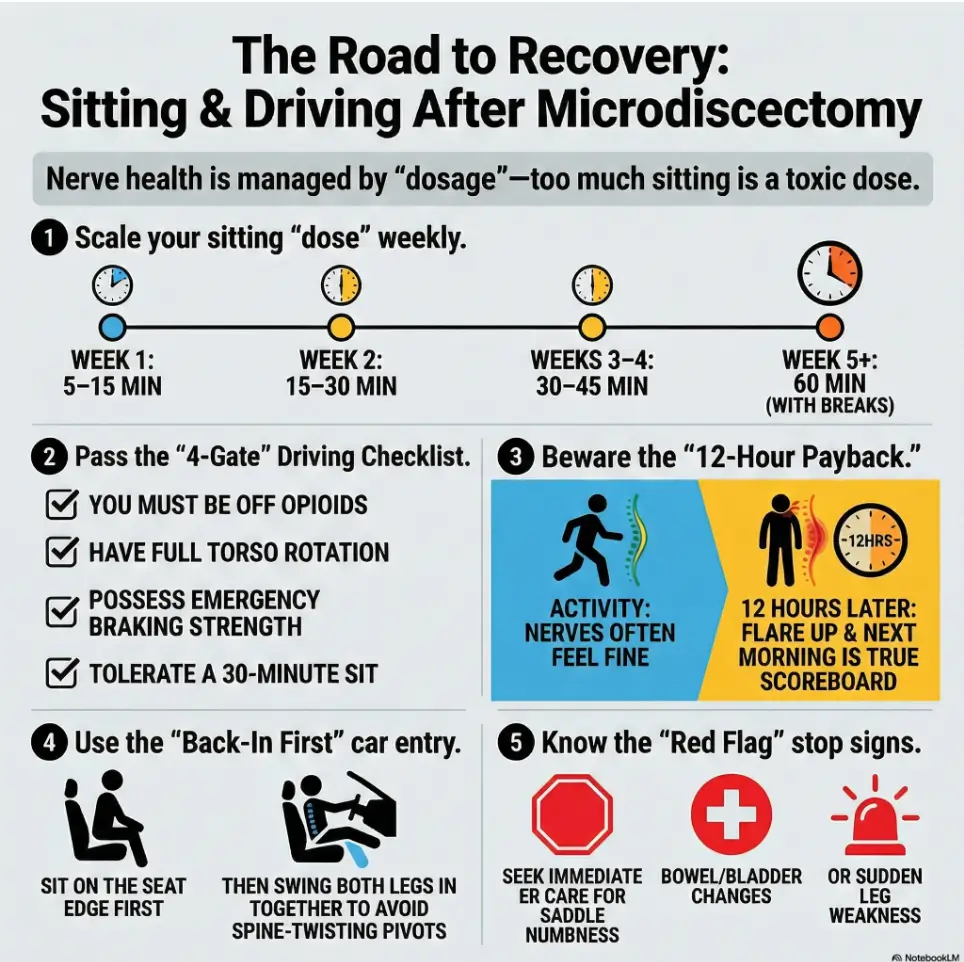
Fast Answer (Snippet-ready, 40–80 words)
Most people can sit in short blocks within the first 1–2 weeks after microdiscectomy, but the safest approach is time-based + symptom-based: start with 5–15 minutes, stand/walk to reset, then gradually increase. Driving is usually delayed until you’re off opioid pain meds, can brake safely, and can sit without a symptom spike often 1–3 weeks for short drives, longer for commutes. Your surgeon’s restrictions and your nerve symptoms decide the pace.
Safety and Disclaimer (read this once)
This article is general education, not medical advice. Your surgeon’s protocol wins if it differs. Do not drive while taking opioids, sedating muscle relaxers, or anything that impairs reaction time. (US driving safety guidance consistently treats “operating heavy machinery” warnings as including driving, and it’s not just about feeling sleepy, it’s about reaction time and judgment.)
- Use a timer for sitting. Guessing is how you overshoot.
- Driving requires braking confidence, not bravery.
- Your leg symptoms are the vote that counts.
Apply in 60 seconds: Put a 10–15 minute “reset alarm” on your phone before any sit or car ride today.
Red flag reminder: New bowel/bladder changes, saddle numbness, rapidly worsening weakness, fever with wound issues, or severe unrelenting pain needs urgent evaluation. If you want a clean checklist you can keep bookmarked, see cauda equina syndrome red flags.
Show me the nerdy details
After microdiscectomy, symptoms are influenced by tissue healing, inflammation, and nerve irritability. Nerves can “complain late,” meaning you might feel fine during the activity and worse hours later. That’s why delayed symptoms are weighted heavily in this guide.
Who this is for / not for
For you if…
- You had a lumbar microdiscectomy (often L4-L5 or L5-S1) and want an activity-specific sitting and driving plan. (If you’re still unsure which nerve level matches your symptoms, L4 vs L5 vs S1 sciatica patterns can help you describe it clearly to your team.)
- You’re rebuilding confidence for commutes, school runs, desk work, or travel.
- You want rules you can follow: minutes, breaks, and stop-sign symptoms.
Not for you if…
- You had fusion, multi-level revision, significant complications, or new neurologic deficits.
- You’re being treated for infection, CSF leak, progressive weakness, or severe uncontrolled pain.
One honest moment: I’ve seen people treat “minimally invasive” like “minor.” Then they try a 45-minute sit on day four and wonder why their leg turns into a live wire at midnight. This guide is built for the reality that small incisions can still mean big nerve feelings.

Timeline logic first: “the clock” + “the nerve”
The two dials that control sitting/driving
- Tissue healing dial: incision healing, deep tissue irritation, inflammation curve.
- Nerve recovery dial: leg pain, tingling, numbness, weakness, symptom “aftershocks.”
The rule that prevents setbacks
Increase one variable at a time: time or intensity or frequency. Not all three. The classic trap is “I sat longer, more often, and in a worse chair,” then blaming the surgery. (The chair always looks innocent. The chair is not innocent.)
Here’s what no one tells you…
Your back often tolerates an activity during it, then complains 2–12 hours later. That delayed flare is your real feedback. If you’re trying to sort “normal soreness” from “nerve irritation,” this is where nerve pain vs muscle soreness after PT becomes a useful mental filter.
Eligibility checklist: Are you ready to “level up” sitting this week?
- Yes/No: Incision pain is stable or improving over the last 48 hours.
- Yes/No: Leg symptoms are not progressively worsening day to day.
- Yes/No: You can walk a few minutes without a spike.
- Yes/No: You can do a 10–15 minute supported sit without “payback” later.
Neutral next step: If you answered “No” to any, keep the same sitting dose for 2–3 more days and focus on resets, not increases.
Show me the nerdy details
Many post-op protocols emphasize early walking and caution with prolonged sitting because sitting increases lumbar flexion tendencies and static load. Even with good posture, “stillness” can irritate a sensitized nerve root.
Sitting timeline by week: how long is “too long”?
Before the timeline, a quick calibration: “too long” isn’t a moral failing. It’s a dose mismatch. Think of sitting like a medication: right dose helps, too much gives side effects.
Rule: If symptoms flare later (evening/next morning), your “true” limit is lower than the clock suggested. Adjust the dose.
Week 0–1: “micro-sits” with resets
- Target: 5–15 minutes sitting, then stand/walk 2–5 minutes.
- Best uses: meals, bathroom breaks, short car rides as a passenger.
I remember the first “real” sit after a friend’s surgery: it felt fine for 8 minutes. Minute 12 arrived like a plot twist. The lesson: quit while you’re winning. That’s not laziness, that’s strategy. (Same logic applies to bed mobility too, which is why the log roll technique exists: boring moves, fewer surprise zaps.)
Week 2: stack short blocks without the “payback”
- Target: 15–30 minutes per sitting block.
- Add: lumbar support, neutral hips, feet supported, no slouch-marathons.
Week 2 is when people start negotiating with themselves: “I’m basically fine.” Your nerve may disagree. The compromise is structure: short, planned sits, and you stand up before symptoms ramp.
Weeks 3–4: build toward real-life sitting
- Target: 30–45 minutes per block, with scheduled breaks.
- Start testing: short desk sessions, short meetings, short dining out.
Here’s a weird truth: restaurants are harder than desks. Soft booths, forward head posture, twisting to talk, then the check arrives and you realize you’ve been sitting for 52 minutes like it’s your job. (It is not your job.)
Weeks 5–8: transition to “normal” with guardrails
- Target: 45–60+ minutes if symptoms stay stable.
- Still smart: break every 30–45 minutes for nerve-sensitive recoveries.
- Use the next morning as your scoreboard.
- Increase by 10–20%, not by vibes.
- If your leg symptoms rise, reduce time first, not posture-only.
Apply in 60 seconds: Write your current safe sit time on a sticky note and treat it like a speed limit for 72 hours.
Mini calculator: Your daily “sitting budget” (2 inputs)
Pick a safe sit block (minutes) and how many blocks you need today.
- Input 1: Safe sit block = ____ minutes (start with 10–15 if early post-op).
- Input 2: Number of blocks today = ____ (meals, appointments, etc.).
Output: Total sitting minutes today = block × blocks. If you feel worse tonight or tomorrow, reduce either the block size or the number of blocks by 1.
Neutral next step: Choose tomorrow’s budget before you wake up and improvise your way into a flare.
Driving timeline: when “allowed” becomes “safe”
Driving is not just sitting. It’s sitting plus vibration, reaction time, braking force, and the tiny panic of “what if I need to swerve.” That’s why a checklist beats a calendar date. (And yes, special cases exist, like driving a manual transmission with sciatica, where the clutch leg can complicate “I feel fine” math.)
The 4-gate driving checklist (pass all four)
- Medication gate: off opioids and sedating meds.
- Movement gate: can turn torso/neck comfortably to check mirrors.
- Brake gate: can brake hard without pain spike or leg giving way.
- Sitting gate: can sit 20–30 minutes without nerve flare afterward.
US safety messaging from traffic authorities is blunt for a reason: prescription drugs like opioids, sedatives, and muscle relaxants can increase crash risk and impair coordination and judgment. If the label says “don’t operate heavy machinery,” read that as “don’t drive.”
Typical US time ranges (what many patients experience)
- Short local drives: often 1–3 weeks (if gates are met).
- Commute-length drives (30–60 min): often 3–6 weeks.
- Long drives/road trips: often 6–12+ weeks, symptom-dependent.
Some hospital instruction sheets and clinical education materials mention driving commonly around 2 weeks when you are off narcotic pain meds, while research reviews on driving after spine surgery often land in the 2–3 week neighborhood for certain lumbar procedures when opioid use is not involved. The point is not the number. The point is the gates.
Let’s be honest…
The first “I drove and felt fine” is not the test. The test is: How do you feel tonight? How do you feel tomorrow morning?
Decision card: Drive vs. Ride (early weeks)
Choose A (Drive) if: all four gates pass, you can do a 20–30 minute sit without later flare, and you can make stops easily.
Choose B (Ride as passenger) if: you’re unsure about braking strength, you’re stiff turning, or you’re still on any sedating meds.
Time/cost trade-off: Driving saves time but raises risk if a flare costs you 2–4 days of progress.
Neutral next step: Pick the lower-risk option for your first two outings, then reassess with your symptom log.
Show me the nerdy details
Driving readiness is often discussed in terms of driver reaction time, medication effects, and ability to perform an emergency stop. Even if your back feels fine, delayed nerve irritation can change how safely you can respond the next day.
Short Story: The “quick errand” that wasn’t (120–180 words) …
A week after surgery, a friend swore they felt “good enough” to ride to the pharmacy. It was five minutes away. The plan was perfect in their head: in and out, no big deal, tiny victory lap. The first bump in the parking lot reminded them that the car has opinions.
They got through it fine, even laughed a little, because the body can be polite in public. That night, the leg tingling climbed like a bad ringtone you can’t silence. By morning, they’d rewritten the narrative: “Maybe I overdid it.” Not catastrophic. Just… expensive in recovery currency.
The fix wasn’t dramatic. Next ride: a lumbar towel roll, a timer, and a stop at minute 15 to stand and breathe. Same destination. Different ending.
Passenger rides: the hidden trap before driving
Why riding can be harder than driving
- More slump, less active bracing, surprise bumps.
- You twist to grab a bag, look at directions, or “just reach” for a water bottle.
- You feel passive, which makes you ignore early warning signals.
The passenger plan (especially weeks 0–2)
- Sit back, hips level, small lumbar support, avoid twisting to grab bags.
- Stops: every 20–30 minutes early on, even if you feel okay.
- When you stand up: give yourself 30–60 seconds to “unfold” before walking fast.
“Bump strategy” that saves nerves
Slow over driveway lips and potholes; brace gently before impact. I’ve watched people tense hard on bumps and then wonder why their back feels like a clenched fist for hours. Gentle brace, exhale, survive the speed bump like a professional.
Quote-prep list: What to ask your surgeon/PA about sitting & driving
- Do you have a no-driving window regardless of symptoms?
- Are there special rules for right-leg symptoms (braking foot) or weakness?
- What’s your definition of “off narcotics” (24 hours? 48 hours?)
- Any restrictions on commutes, rideshares, or travel in the first month?
- What symptoms mean stop and call vs. “normal nerve noise”?
Neutral next step: Paste these into your patient portal message so you’re not improvising during a 7-minute callback.
Car setup that reduces flare-ups (cheap fixes, big payoff)
Seat geometry: what you’re aiming for
- Hips slightly higher than knees (small wedge or towel if needed).
- Lumbar support to prevent slouch-flexion.
- Feet supported, not dangling like a sad chandelier.
In/out technique (protect the spine)
- “Back in first”: sit, then swing both legs together (avoid twisting).
- Use door frame or seat edge for controlled lowering/standing.
- Move like you’re holding a bowl of soup. No sudden pivots.
If you drive a low sedan or anything that makes you “fold yourself in,” it helps to practice a consistent entry/exit pattern. (This overlaps with getting in and out of a low car with sciatica, because the mechanics and the risks are basically cousins.)
Gear hacks for US commutes
- Supportive cushion, small towel roll.
- Ice/heat pack for after (follow your team’s guidance on incision care).
- Grabber tool for items, because bending for a dropped phone is how tragedies begin.
Does a lumbar cushion help or is it placebo? Sometimes “placebo” is just your body finally getting out of the slouch shape that irritates it. Also: if it works, who cares what we call it.
Show me the nerdy details
Car seats tend to encourage posterior pelvic tilt and lumbar flexion. A small lumbar support can restore neutral alignment and reduce sustained flexion, which some patients find provocative early in recovery.
Work and commute planning: returning without the crash
Desk job timeline: the “stair-step” schedule
- Start with 2–4 short blocks/day, not one long sit.
- Add 10–15 minutes per block every few days if stable.
- Schedule resets like meetings. Treat them as non-negotiable.
If you want a plug-and-play template for breaks, your best friend is a structured sit-stand schedule for a desk job with sciatica (same logic, different diagnosis label).
Commute + desk is a double-load
Treat drive time + desk time as one combined “sitting budget.” If you drive 30 minutes each way and sit 4 hours straight, your spine hears: “We’re doing an endurance event.” Your spine did not sign up for an endurance event.
If your job won’t flex, do this first
- Ask for temporary remote days.
- Put breaks on the calendar.
- Use a standing option (even if it’s a high counter and a laptop stand).
- Shorter meetings, camera-off if you need to shift positions.
If you’re stuck arguing “chair vs standing,” you’ll like the practical framing in ergonomic chair vs standing desk: the winner is usually “variety,” not purity.
- Drive + desk counts as one total load.
- Breaks work best when scheduled, not reactive.
- Your first “full day” should be a test day, not a performance.
Apply in 60 seconds: Add two 5-minute “reset” events to your work calendar for tomorrow.
Common mistakes that delay recovery (and how to dodge them)
Mistake 1: “I feel better, so I catch up”
Fix: cap increases at 10–20% per week for sitting/driving load. Catching up is for missed TV shows, not nerve healing.
Mistake 2: Testing driving before testing sitting
Fix: prove you can sit 20–30 minutes without next-day flare, then drive. If sitting alone is shaky, driving adds vibration and braking force and multiplies the odds of payback.
Mistake 3: Slump sitting (flexion) plus long rides
Fix: lumbar support + time blocks + resets, especially early weeks. “I’ll just lean back” often becomes “I slid into a C-shape.”
Mistake 4: Ignoring the leg symptoms because the back feels fine
Fix: treat new/worsening leg pain as your stop sign, not a challenge. I’ve seen people brag through tingling like it’s a marathon medal. It is not a medal. If you’re second-guessing whether a sensation is “nerve” or “muscle,” bookmark hamstring stretch vs nerve pain as a reality check.
Coverage tier map: Your “care escalation” tiers (1→5)
- Tier 1: Mild soreness, improves with resets. Continue gradual plan.
- Tier 2: Delayed nerve flare after sitting/driving. Reduce time 20–30% and add more breaks.
- Tier 3: Symptoms trending worse over 2–3 days. Contact clinic for guidance.
- Tier 4: New or worsening weakness, significant leg pain spike, wound concerns. Call urgently.
- Tier 5: Bowel/bladder changes, saddle numbness, rapidly worsening deficits, fever with wound issues. Go to urgent care/ER.
Neutral next step: Decide your current tier today and write it in your notes app so you respond faster if things change.
“Don’t do this” list: the setback recipes
Don’t do this: the “one big drive” gamble
A single long drive can trigger a flare that costs you a full week. I’ve watched the math happen: 1 brave hour in the car, then 5 cautious days undoing it. Bad trade.
Don’t do this: drive while sedated “just a little”
Reaction time + braking force are non-negotiable for safety and liability. If you feel “a bit foggy,” treat that as “not today.” (If anxiety is making you doubt every sensation, it can help to name the pattern: cyberchondria and chronic pain is a surprisingly practical read.)
Don’t do this: white-knuckle through tingling
If tingling ramps during sitting/driving, switch to resets and reduce time until stable. White-knuckling is how you turn a warning light into a repair bill.
When to seek help (red flags and “call today” symptoms)
Go to urgent care/ER now if you have
- New bowel/bladder control problems.
- Saddle anesthesia (numbness in groin/perineal area).
- Rapidly worsening weakness, foot drop, severe unrelenting pain, fever with wound issues.
Call your surgeon/clinic promptly if
- Increasing leg pain that doesn’t settle with rest/reset.
- Wound drainage, redness, swelling, or escalating incision pain.
- Symptoms steadily worsening over several days instead of trending down.
One more lived-experience note: it’s emotionally hard to call because it feels like failing. It’s not failing. It’s data-sharing. Your surgical team can’t help with symptoms they never hear about.

FAQ
1) How long after microdiscectomy can I sit normally?
“Normal” usually returns in stages. Many people build from 5–15 minute sits in week 1, to 15–30 minutes around week 2, to 30–45 minutes by weeks 3–4, and 45–60+ minutes by weeks 5–8 if symptoms stay stable. If your leg symptoms flare later, your personal normal is smaller for now and that’s okay.
2) When can I drive after microdiscectomy if I’m off pain meds?
Being off opioids is necessary, but not sufficient. Use the 4-gate checklist: off sedating meds, can turn comfortably, can brake hard safely, and can sit 20–30 minutes without a later flare. Many patients land in the 1–3 week range for short local driving when these gates are met, but your surgeon’s plan wins.
3) Is riding as a passenger safer than driving after surgery?
It can be safer because you remove the braking and emergency-response demands, but it can also be harder on your body if you slump or twist. Use lumbar support, keep hips level, and stop every 20–30 minutes early on. Think “supported and boring,” not “tough it out.”
4) How long can I sit in a car at 2 weeks post-op?
Many people tolerate 15–30 minutes at two weeks if symptoms are stable, but it’s highly individual. Plan stops, use lumbar support, and treat “feels fine right now” as only half the result. If you flare later that day or the next morning, shorten the ride time and increase breaks.
5) What if sitting makes my leg pain come back?
First, don’t panic. Nerves can be reactive while healing. Use resets (stand/walk 2–5 minutes), reduce the sitting block by 20–30%, and avoid slouching or twisting. If leg pain is steadily worsening over several days, or you develop weakness or red flags, contact your clinic promptly.
6) Can I drive if I’m taking a muscle relaxer at night only?
Some muscle relaxers are sedating and can cause next-day grogginess in certain people. The safest approach: don’t drive until you know how you respond, and avoid driving if you feel foggy or slowed. If the medication warning includes operating machinery, treat that as a no-driving warning until you’re confident you’re unimpaired.
7) When can I return to a 45-minute commute after microdiscectomy?
Often this lands around 3–6 weeks for many patients if driving gates are met and sitting tolerance supports it, but it can be longer if nerve symptoms are sensitive. Practice with shorter drives, stop every 30–45 minutes (or sooner early on), and remember commute + desk time is a combined sitting load.
8) Does a lumbar cushion actually help, or is it placebo?
It can help by reducing slump and keeping your lumbar spine closer to neutral. Even if some of the benefit is “comfort,” comfort changes posture and tension patterns. Choose a simple support (small towel roll works) and judge it by one metric: fewer symptom spikes later.
9) What’s the best way to get in and out of the car after microdiscectomy?
Use the “back in first” method: sit first, then swing both legs together, avoiding twisting. Use the door frame or seat edge for controlled movement. Move slowly and deliberately. The goal is not speed, it’s zero sudden rotation.
10) When is it safe to take a road trip after microdiscectomy?
Road trips are usually safer later, often 6–12+ weeks depending on symptoms and your surgeon’s plan. Build up by practicing 30–60 minute drives with planned stops, and ensure you can sit without a delayed flare. If you must travel earlier, plan frequent breaks and consider being a passenger instead of driving.
Conclusion
Remember that car seat you were side-eyeing at the top? Here’s the curiosity loop closure: the seat isn’t your enemy. The enemy is unmeasured time. The fix is wonderfully unglamorous: a timer, a reset plan, and the humility to treat “feels fine” as a draft, not a final verdict.
In the US, big institutions often frame early recovery around gradual return to routine activities and driving only when you’re able and not on narcotic pain meds, and traffic-safety authorities are clear that certain prescriptions can impair driving. Use that mindset, but make it personal with your symptom log.
Next step (one concrete action)
Pick one baseline test today: set a timer and do a 10-minute supported sit, then log symptoms at 2 hours and next morning. If stable, repeat tomorrow. If not, reduce time and add more reset breaks. This becomes your personal “sitting prescription” for driving readiness.
Last reviewed: 2026-02.
