
Turning Noise into Signal: Navigating Post-Op Sciatica Rebound
A “normal” week after back surgery can unravel in one afternoon: two errands, one long sit, one extra grocery bag, and suddenly your leg pain is back, sharp and insulting. Post-op sciatica rebound is often the result of nerve irritation and inflammation as your activity levels shift. While less common, persistent symptoms can sometimes point toward scar tissue or recurrent issues. If sitting is the main spark, it helps to understand the usual microdiscectomy sitting and driving pitfalls that flare nerves during the “I feel fine, so I did normal life” phase.
The hardest part isn’t the pain—it’s the guessing. Misreading these signals leads to risky overexertion or unnecessary panic. This guide helps you decode the pattern using timing, pain mapping, and a clinical-grade 48-hour Signal Log.
Read this before you “test it.” Save your future self a week of recovery.
Table of Contents

Fast Answer (Snippet-Ready)
Post-op sciatica “rebound” is often inflammation/irritation (early, fluctuating, activity-sensitive, may respond to rest/anti-inflammatories) or less commonly scar tissue (epidural fibrosis) (later, more persistent, less position-dependent, may feel “stuck” despite rehab). Timing, symptom pattern, and red flags matter more than any single clue. Track a 48-hour “signal log,” protect the nerve, and contact your surgeon urgently for new weakness, bladder/bowel changes, fever, or escalating pain.
- Early + fluctuating often leans inflammation/irritation
- Late + persistent can lean scar tissue or recurrent compression
- New weakness, bladder/bowel changes, fever, saddle numbness = urgent
Apply in 60 seconds: Write down “when it started, what triggers it, what resets it” in one sentence.
Who this is for / not for
Who this is for
- You had back surgery (microdiscectomy, laminectomy, decompression, fusion) and leg pain returned or shifted
- You’re trying to separate “normal healing noise” from “something changed”
- You want clinic-ready language and a short tracking method
Who this is not for
- Anyone with new foot drop, worsening weakness, saddle numbness, bladder/bowel changes
- Anyone with fever, wound drainage, severe unrelenting pain, or rapidly worsening symptoms
- Anyone who needs personalized medical advice (this is pattern recognition, not diagnosis)
A quick, human note: I’ve watched caregivers do the “quiet panic” thing, trying to stay calm while Googling at 2:17 a.m. If that’s you, you’re not dramatic. You’re trying to keep someone safe. (Also: if you feel your brain looping into doom tabs, you’re not alone, and cyberchondria in chronic pain is a real thing with real downstream stress costs.) Let’s put structure under that fear.
Define the “rebound” in one sentence (before you spiral)
Before you chase explanations, define the event. Your brain wants a story; your clinician needs a timeline. One sentence turns chaos into signal.
The three common rebound stories
- Same pain, same path: symptoms resemble pre-op sciatica
- New map: pain shifts to a different dermatome or side
- Volume change: baseline improves but flares spike sharply
Let’s be honest…
“It came back” feels like failure. Often it’s signal, not verdict: nerves hate being touched, even when helped. Surgery can decompress a nerve and still leave it irritated, like taking a tight shoe off a bruised toe. Relief and sensitivity can coexist.
Show me the nerdy details
“Rebound” is not a formal diagnosis. It’s a useful patient shorthand for recurrent radicular symptoms after an intervention. Clinicians usually sort it into categories: inflammatory neuritis/irritation, recurrent compression (like a recurrent disc herniation), adhesions/scar-related tethering, or less commonly infection/hematoma/CSF-related complications. The sorting relies heavily on timing, neurologic exam, and trend.
- Yes: Pain fluctuates; no new weakness; no bladder/bowel change; no fever
- No: New weakness, saddle numbness, bladder/bowel change, fever/drainage
- Maybe: Worsening trend over 48–72 hours despite your post-op plan
Apply in 60 seconds: Circle “Yes/No/Maybe,” then decide: track, call, or urgent evaluation.
Timing tells tales: the post-op clock that changes the odds
Timing doesn’t prove the cause, but it shifts the odds. Think of it as a weather forecast, not a courtroom verdict. The same symptom at Day 5 and Month 5 can mean very different things.
Week 0–2: irritation and swelling are loud
- Surgical manipulation + local inflammation can make nerves reactive
- Hematoma (blood collection) is uncommon but time-sensitive, and usually comes with escalating symptoms
- Pain can wax/wane and change with movement as tissues settle
I’ve heard patients describe this phase as “my nerve is a smoke alarm that goes off when I make toast.” That metaphor is annoyingly accurate: it’s sensitive, not necessarily dangerous, but you still respect it.
Weeks 2–12: inflammation vs mechanical triggers
- Rehab load changes faster than nerve tolerance
- Sitting tolerance is often the last thing to come back (and a smart sit-stand schedule for desk-job flare control can keep you from accidentally stacking long sits)
- “Good days, bad days” is common, but trend matters
Months 3+: scar tissue becomes a more plausible driver
- Epidural fibrosis (scar tissue around the nerve area) develops over time
- Symptoms can feel persistent and less “resettable” by rest
Why did it wait… then hit?
Because your body can mute symptoms when you’re resting, then amplify them when activity returns. Many rebounds show up right after a “confidence day,” when you finally felt normal and did two normal-person things in one afternoon.
Show me the nerdy details
Post-op radicular pain can reflect inflammatory sensitization (chemical irritation, edema) even when mechanical compression is reduced. Later-onset symptoms may relate to recurrent disc herniation, foraminal stenosis progression, adhesions, or adjacent segment stress (especially after fusion). Clinicians often use contrast-enhanced MRI selectively because enhancement patterns can help separate scar from recurrent disc, but the decision depends on symptoms and exam. If you’re trying to understand why imaging choices vary, this breakdown of sciatica MRI vs X-ray decision logic can help you ask better questions.
Scar tissue vs inflammation: clue grid (without pretending it’s perfect)
Here’s the honest truth: at-home clues are probabilistic, not definitive. But they can still steer you toward the right next step and the right questions. Think “more likely,” not “certain.”
Clue grid (quick read)
Leans inflammation/irritation
- Earlier onset (days to weeks)
- Fluctuates with activity, posture, sleep, swelling
- Partial “reset” with rest, pacing, ice/heat, meds as directed
- Often a “burning” or “electric” sensitivity that comes and goes
Leans scar tissue (epidural fibrosis) or tethering
- Later onset (often months), creeping persistence
- Pain feels anchored, fewer “reset” moments
- Less position-responsive
- Rehab plateaus despite good adherence
The “stuck nerve” feeling
Some people describe a tethered, pulling sensation. That can point toward adhesions, but it can also be plain nerve sensitization. Translation: it’s a clue, not a diagnosis. If you’re thinking, “It feels like it catches when I move,” write that down, along with the exact movement.
Decision card: When A vs B
A) Track + protect the nerve (next 48 hours) if: symptoms fluctuate, you can find a position that eases them, and there is no new weakness or bladder/bowel change.
B) Call your surgeon (same/next business day) if: the trend is worsening over 48–72 hours, new numbness area appears, or sleep is being hijacked nightly.
C) Urgent evaluation now if: new weakness (buckling/foot drop), saddle numbness, bladder/bowel changes, fever, wound drainage, or rapidly escalating pain.
Neutral next step: Pick A, B, or C, then document your “why” in one sentence.
The map matters: where the pain travels (and what it whispers)
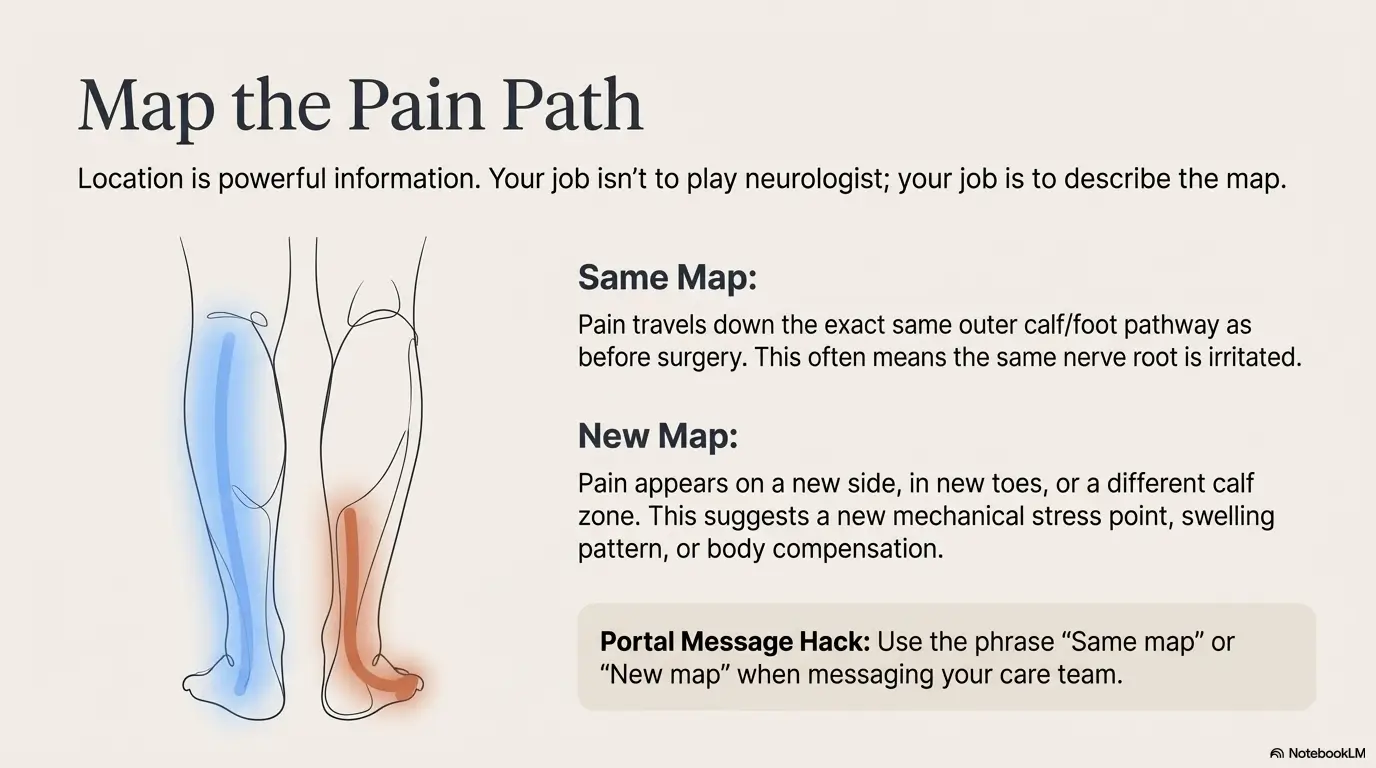
Location is information. Not perfect information, but useful information. Your job isn’t to play neurologist; your job is to describe the map clearly enough that your clinician can.
Dermatomes and “same root” return
If pain returns down the same outer calf/foot pathway you had pre-op, that can fit a similar nerve root being irritated again. If it’s a new pathway (new side, new toes, different calf zone), that can suggest a different driver: compensation, swelling pattern, or a new mechanical stress point. Either way, “same map vs new map” is a powerful sentence in your portal message. If you want a clean reference for how clinicians talk about distribution, this guide to L4 vs L5 vs S1 sciatica patterns can help you label your “map” without overreaching into diagnosis.
Centralization vs peripheralization (your most useful home test)
Here’s a simple pattern that many PTs pay attention to:
- Centralization: symptoms move upward toward the back/buttock and away from the foot. Often a better sign.
- Peripheralization: symptoms march downward toward the calf/foot and stay there. Often a “respect the nerve” sign.
If your clinician uses provocative testing language, you’ll sometimes hear about the straight-leg raise. If you’re considering any at-home checks, keep it gentle and data-focused, and see a step-by-step description of the straight leg raise test at home so you record what you feel without turning it into a “prove it” moment.
Here’s what no one tells you…
“More imaging” isn’t always the next best move. Better pattern data often earns better care. If you show up with a clear timeline, triggers, and a simple strength screen, you’re not being “extra.” You’re making the visit efficient. And if you’ve ever felt dismissed because a scan didn’t “match” the pain, you’re not imagining that disconnect: MRI pain mismatch is common enough that it deserves its own vocabulary.
Show me the nerdy details
Dermatomes are not perfect road maps; people vary, and pain can refer. That said, consistent distribution plus consistent triggers can increase clinical confidence. Clinicians integrate dermatomal symptoms with motor testing (e.g., dorsiflexion weakness), reflex changes, and provocative maneuvers. Your home job is to record, not to diagnose.
The 48-hour Signal Log: a tiny tool that makes doctors listen
This is the part that changes appointments. A one-page pattern log often does more than a long emotional explanation, even when the emotion is completely justified.
What to track (fast, concrete, un-ignorable)
- Pain 0–10 (leg vs back separately)
- Numbness/tingling areas (draw a quick map, even a messy one)
- Weakness checks (only if safe): heel walk, toe walk, single-leg sit-to-stand
- Triggers: sitting minutes, walking minutes, bending/twisting, coughing/sneezing
- Relief: positions, ice/heat, pacing, meds (as prescribed)
How to summarize for a visit
Use clinic language that’s short and testable:
- “Started on Day X after Y activity; worsens with sitting >15 minutes; improves lying flat.”
- “Numbness patch stable; no bladder issues; strength feels the same.”
- “Trend: worse for 2 days vs improving overall with spikes.”
💡 Read the official sciatica symptoms and causes guidance
Mini calculator: “Call timing” (pattern-based, not diagnostic)
Enter three observations from your last 48 hours:
- Trend: improving / flat / worsening
- Reset: do you have a position that reliably eases symptoms within 30–60 minutes? yes / no
- Neurologic change: new weakness or new bladder/bowel symptoms? yes / no
Output:
- If neurologic change = yes → urgent evaluation now.
- If trend = worsening AND reset = no → call surgeon same/next business day.
- If trend = improving/flat AND reset = yes → track + protect the nerve for 48 hours, then reassess.
Neutral next step: Screenshot your “inputs” and bring them to PT or message your surgeon’s portal. If you need a reliable “reset” option to test (without drama), many people start with the 90-90 position for sciatica and simply record whether symptoms settle within an hour.
Small lived-experience moment: I once watched someone do a perfect, detailed explanation in a clinic room, and the clinician still missed the key trigger. The next visit, they brought a two-day log. The clinician’s posture changed. Not because pain became “more real,” but because the pattern became easier to act on.
Common mistakes that turn a flare into a setback
A flare is not automatically a setback. But certain reactions can turn it into one. These are common, understandable, and fixable.
Mistake 1: Treating pain like a scoreboard
Chasing 0/10 can lead to two bad extremes: over-rest (stiffness, fear, deconditioning) or over-training (irritation, inflammation spiral). Better goal: trend + function. Can you walk a little more comfortably this week? Can you sit 2 minutes longer without paying for it?
Mistake 2: Upgrading activity too fast because you felt “finally normal”
Your muscles and motivation can recover faster than your nerve’s tolerance. It’s common to feel great at Week 3, then flare at Week 4 after stacking errands, stairs, and “just one more thing.” (The human body hates “just one more thing.”) If PT is part of the story, it also helps to separate “good training sore” from “angry nerve signal,” and this guide to nerve pain vs muscle soreness after physical therapy can give you language for that difference.
Mistake 3: Ignoring new neurologic changes because the incision “looks fine”
Nerves don’t care about neat stitches. If you notice new weakness, buckling, or a new numbness zone that’s spreading, that’s not a “tough it out” moment.
- Don’t stack stressors (long sit + long walk + chores)
- Respect delayed payback (symptoms can spike 6–24 hours later)
- Trend beats intensity: one bad hour matters less than three worsening days
Apply in 60 seconds: Pick one activity to scale back by 20% for 48 hours.
Don’t do this: two high-cost moves people regret
Don’t do this #1: “Test it” with bending, twisting, or heavy lifting
You don’t prove healing by stressing the exact tissues that are irritated. “Testing” often creates a new data point that’s expensive: more inflammation, more fear, more guarding. If you need reassurance, use controlled, surgeon-approved progressions, not a dramatic one-rep max of laundry baskets. For day-to-day movement safety, many people do better when they use a consistent “out of bed” strategy like the log roll technique for sciatica instead of improvising through pain.
Don’t do this #2: Self-adjusting meds or mixing NSAIDs without a plan
Drug interactions and kidney/GI risks climb quietly. Many post-op plans already include specific limits (especially after fusion, depending on your surgeon’s preferences). If you’re tempted to improvise, that’s a sign you need a call to the care team, not a medication “freestyle.”
Short Story: I remember a caregiver telling me about “The Grocery Bag Moment.” Week 5 after surgery, things were finally calm. They felt brave. They carried two light bags in one trip because it felt ridiculous to make two. That night, the leg pain returned, sharp and insulting. The next morning, panic arrived with coffee. They wanted an MRI immediately. Instead, they did something smarter: they wrote a 48-hour log and noticed the pattern.
Sitting was the villain, not walking. Lying down reset symptoms within 40 minutes. No weakness, no bladder changes. They messaged the surgeon with three lines of data, not a novel. The reply came fast: reduce load, adjust pacing, watch strength, call if the trend worsened. Within a week, the flare faded. It wasn’t “nothing.” It was inflammation talking.
(If “two light bags” is your personal Achilles’ heel, it helps to decide a simple grocery bag weight limit for sciatica before the next “I’ll just do it in one trip” moment.)
What your surgeon/PT may do next (so you can walk in prepared)
When you walk in prepared, you tend to get a clearer plan. In the U.S., care pathways often involve your surgeon’s office, your PT, and sometimes a pain specialist (especially if injections are considered). Different roles, different tools.
Conservative resets (often first)
- Activity modification and pacing adjustments
- Targeted PT (often hip mobility, core control, graded exposure)
- Nerve glides when appropriate (timing matters, technique matters)
- Medication adjustments (only via your clinician; if oral steroids come up, here’s a practical overview of an oral steroid taper for sciatica so you understand what it is and what it isn’t)
Imaging and procedures (when pattern suggests it)
- MRI (sometimes with contrast) when symptoms or exam suggest recurrent compression vs scar tissue
- Consideration of injections when inflammation is suspected and symptoms persist (patients often ask how options differ; this comparison of nerve root block vs epidural steroid injection can help you follow the conversation)
The clinic questions that change the conversation
- “Does this pattern fit recurrent compression, inflammation, or adhesions?”
- “What findings would change the plan in the next 2–4 weeks?”
- “What is my no-regret activity ceiling until symptoms stabilize?”
Quote-prep list: what to gather before comparing opinions
- Your surgery type and level(s) (from discharge paperwork)
- Day-by-day symptom timeline (even 7 lines helps)
- 48-hour Signal Log (map + triggers + reset positions)
- Any new neurologic changes (strength, numbness zones)
- Your current post-op restrictions and meds list
Neutral next step: Put these in one note on your phone before your next visit.
Commercial entity signals (neutral, practical): depending on where you are, your workflow might run through a health system portal like MyChart, a surgeon group tied to a major hospital, and guidance aligned with groups such as the American Academy of Orthopaedic Surgeons (AAOS) or the North American Spine Society (NASS). The point isn’t the logo. It’s getting the right person to interpret your pattern.
If an epidural steroid injection is part of the plan, patients often ask what “normal” feels like afterward; this epidural steroid injection relief timeline can help you separate expected pacing from true worsening. And if you get a temporary spike and wonder whether you “made it worse,” the concept of a steroid flare after injection is worth knowing (without assuming that’s what’s happening).
When to seek help (urgent vs soon)
This is the “don’t be polite to danger” section. If you’re a caregiver, this is also the section you bookmark so you can stop re-litigating the decision every hour.
Go now / urgent evaluation
- New or worsening weakness (foot drop, buckling, can’t heel/toe walk like before)
- New bladder/bowel dysfunction or saddle numbness (if you want the clearest label for what “counts,” see cauda equina syndrome red flags)
- Fever, wound drainage, severe unrelenting pain
- Severe headache after spinal anesthesia (especially if positional) or rapidly escalating symptoms
Call your surgeon soon (same/next business day)
- New numbness area, pain trending worse over 48–72 hours
- Night pain escalating, or pain not responding to your post-op plan
- New symptoms after a specific event (fall, heavy lift)
Coverage tier map: 5 urgency tiers (simple, memorable)
- Tier 1 (Track): fluctuating pain, no neuro changes, has reset positions
- Tier 2 (Message): worsening trend, new numbness patch, sleep disruption
- Tier 3 (Call): escalating pain + no reset + function dropping
- Tier 4 (Urgent): new weakness/buckling, severe uncontrolled pain
- Tier 5 (Emergency): bladder/bowel change, saddle numbness, fever with wound concerns
Neutral next step: Write your tier in your log so you don’t have to renegotiate reality later.
Safety / Disclaimer (High-risk topic)
This content is for education and symptom-pattern tracking, not diagnosis or treatment. Post-op neurologic symptoms can become urgent quickly. If you have new weakness, bladder/bowel changes, saddle numbness, fever, wound drainage, or rapidly worsening pain, seek urgent medical evaluation.
Infographic: Post-op sciatica “rebound” triage (print-friendly)
1) Any red flag?
Weakness, bladder/bowel change, saddle numbness, fever/drainage
→ Yes: urgent evaluation
2) Trend over 48–72 hours?
Improving / flat / worsening
→ Worsening: call surgeon
3) Can you “reset” it?
Position helps within 30–60 minutes
→ Yes: track + protect nerve
Accessibility note: This infographic is a text-based triage flow designed for screen readers and printing.

FAQ
Is post-op sciatica “rebound” normal after microdiscectomy?
It can happen. Many people have a period where nerve irritation flares as swelling shifts and activity increases. What matters is the trend and whether there are any new neurologic deficits. “Normal” should still be monitored and documented, not dismissed.
How long can nerve inflammation last after back surgery?
Nerve irritation can linger for weeks and sometimes longer, especially if the nerve was compressed for a while before surgery. The useful question isn’t “how long in general,” but “am I trending better week to week?” Your 48-hour Signal Log helps show whether you’re improving, plateauing, or worsening.
What does scar tissue pain feel like compared to inflammation?
People often describe scar-related symptoms as more persistent, less position-responsive, and harder to “reset” with rest. Inflammation/irritation more often fluctuates with activity, sitting time, and daily load. But these are tendencies, not guarantees.
Can scar tissue cause sciatica months after surgery?
Scar tissue (epidural fibrosis) can be associated with persistent or recurrent symptoms later on. It’s also not the only late cause. Recurrent disc herniation, foraminal narrowing, adjacent segment stress, and general nerve sensitization can also contribute. A clinician’s exam plus selective imaging can help sort the most likely driver.
Does an MRI show scar tissue vs recurrent disc herniation?
Sometimes. Clinicians may choose MRI with contrast because enhancement patterns can help distinguish post-surgical scar from recurrent disc material in certain cases. Whether you need imaging depends on your symptoms, exam findings, and response to conservative care.
Why does sitting make post-op sciatica worse?
Sitting can increase pressure and tension through the lumbar spine and can irritate a sensitive nerve root, especially early in recovery. Many people tolerate walking better than sitting in the first 2–12 weeks. If sitting is your main trigger, track “minutes to flare” and “minutes to reset.”
What are red flags after lumbar surgery that mean ER now?
New or worsening weakness (including foot drop), new bladder/bowel dysfunction, saddle numbness, fever with wound concerns, wound drainage, or rapidly escalating pain. If you’re not sure, it’s safer to call the surgeon’s on-call line or seek urgent evaluation.
Can physical therapy make sciatica worse after surgery?
PT can temporarily flare symptoms if progression outpaces nerve tolerance or if movements irritate sensitive tissues. That doesn’t mean PT is “bad,” but it does mean the program needs calibration. Bring your Signal Log and ask for a no-regret activity ceiling and a clear plan for flare management.
Are epidural steroid injections used after surgery for rebound pain?
They can be considered in some cases, especially when inflammation is suspected and symptoms persist despite conservative measures. Timing and appropriateness depend on your surgery type, healing stage, and clinical findings, so this is a surgeon-led decision.
What questions should I ask my surgeon if my leg pain returns?
Ask: “Does this pattern fit inflammation, recurrent compression, or adhesions?” “What would make you change the plan in the next 2–4 weeks?” “What activities are safe to keep, and what should I pause for now?” Those three questions often turn vague reassurance into a clear plan.
Conclusion
Let’s close the loop from the top: a post-op sciatica “rebound” feels like betrayal because it arrives dressed like the old pain. But often, it’s not the old story. It’s a sensitive nerve reacting to swelling, load, and recovery timing. Sometimes it’s scar-related tethering. Sometimes it’s mechanical again. Your job isn’t to guess perfectly. Your job is to capture the pattern and escalate quickly when red flags appear.
Do the next right thing in the next 15 minutes: open a note on your phone and start the 48-hour Signal Log with three lines: start date, top trigger, best reset position. If you’re worried about neurologic change, do not negotiate with doubt. Call the surgeon’s office or seek urgent evaluation. 💡 Read the official sciatica warning signs and neurologic red flags guidance 💡 Read the official sciatica symptoms, triggers, and when to seek care guidance
Last reviewed: 2026-03
