
Fast Answer (snippet-ready, 40–80 words)
The 90/90 position aims to reduce irritation by placing your hips and knees at roughly 90° while your calves rest on support. For most adults, the “right” pillow height is the height that keeps thighs level and shins supported without your low back arching or hips pinching—often 8–14 inches on a bed and 10–16 inches on the floor (because the surface is firmer). Use a quick check: relaxed belly, neutral low back, no tingling increase.
Mastering the 90/90 Setup: No More 2 A.M. “Pillow Jenga”
At 2 a.m., a “simple” 90/90 setup can turn into a nightmare—one wrong inch and your leg starts buzzing like a flickering fluorescent light. It’s time to stop the guessing game and start calming your nervous system.
The 90/90 position is a symptom-calming posture where your hips and knees rest at roughly 90° with your calves fully supported. The goal? Let your low back and hamstrings finally stop bracing.
The catch: Height matters less than the contact point and whether your pelvis stays neutral.
The 3-Check Method
- Thigh Level
- Low-back Neutrality
- 60-second Symptom Check
The Fix
Exact, testable setups for bed vs. floor. Fast fixes when sensations change—without turning relief into a flare.
No anatomy lectures. No hero holds. Just calmer nights, one variable at a time.
Table of Contents
Safety / Disclaimer (read first)
This is general education, not medical advice. Stop if pain, numbness, tingling, or weakness worsens. Avoid if you have a recent fall/trauma, fever, cancer history with new back pain, loss of bladder/bowel control, or rapidly progressing weakness—seek urgent care. If you’re unsure whether your symptoms cross that line, use this as a reality check: how to recognize a low back pain emergency.
For example, Mayo Clinic notes urgent evaluation for symptoms like sudden leg weakness/numbness and trouble controlling bowels or bladder, and UK NHS guidance flags numbness around genitals/anus or new bladder/bowel control problems as emergency “go now” signs. Use those as your safety ceiling: if you’re anywhere near that line, don’t “position-hack” it at home.
- Stop if symptoms intensify or spread.
- Urgent red flags beat “try one more tweak.”
- When in doubt, get checked—especially with weakness or bladder/bowel changes.
Apply in 60 seconds: Do a quick “strength check” (can you do a strong heel-walk/toe-walk?) and a bladder/bowel sanity check before you settle in.
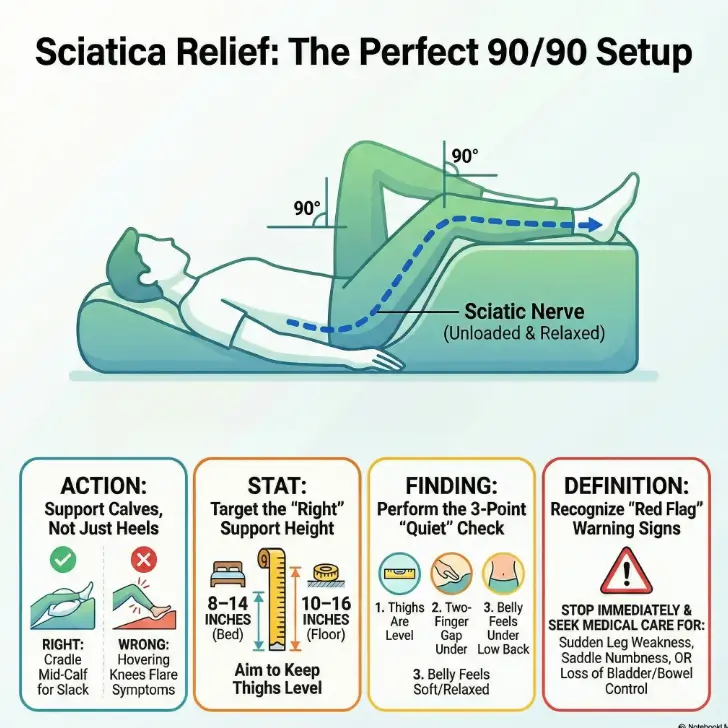
1) 90/90 mechanics: what you’re actually trying to “unload”
Pressure off the nerve: the simple model (no anatomy lecture)
Think of sciatica-like symptoms as a volume knob your nervous system turns up when it feels threatened—irritated tissue, cramped spaces, tense muscles, or a sensitive nerve root. The 90/90 position is a way to say, “Hey body, you’re safe enough to stop shouting.” It often does that by nudging your low back and pelvis toward a less provocative alignment and reducing constant tension through the back of the legs.
Personal note: the first time I tried a “knees-up” position, I did it wrong—ankles on a pillow, knees floating—and my hamstrings felt like guitar strings at full tension. Not relaxing. Not quiet.
The real goal: neutral pelvis + quiet hamstrings (not “perfect angles”)
The magic isn’t the number 90. The magic is neutral pelvis (not arched, not tucked aggressively) plus supported legs so your hamstrings can stop guarding. When your hamstrings chill out, your pelvis often stops being pulled into a position that feeds irritation.
Curiosity gap: why 90/90 helps some people… and irritates others
If your symptoms feel better with gentle bending-forward positions, 90/90 may feel like a small miracle. But if hip flexion (bringing knees toward chest) spikes symptoms—common for some patterns—90/90 can backfire. That’s why we’re going to build this as a testable setup, not a belief system. If you’re not sure what you’re actually dealing with, it can help to compare patterns like sciatica vs. herniated disc symptoms and sciatica vs. piriformis syndrome before you commit to one “magic position.”
Show me the nerdy details
In practice, 90/90 is a “position of relative flexion” that can reduce extension load for some backs and reduce neural tension for some legs—if the calves are supported and the pelvis isn’t forced into an exaggerated tilt. Small changes in knee height, calf contact point, and pelvic position can change symptoms quickly because they change load distribution and perceived threat.
2) Who this is for / not for: the “green light / yellow light / red light” screen
Good fit: leg pain that eases with bending/relaxing positions
Green-light patterns often include: leg pain that eases when you lie down, symptoms that calm with knees supported, and a sense that the leg “settles” when the low back relaxes. If you’ve ever found yourself naturally curling slightly on a couch and thinking, “Oh… that’s quieter,” 90/90 may be worth a careful try.
Not a fit: symptoms that spike with hip flexion or sitting
Yellow light: if sitting, driving, or knees-up positions reliably spike tingling, deep buttock pain, or a sharp “electric” feeling, don’t force 90/90. You might need a different position (more neutral, less hip flexion) or a shorter test dose with more conservative height.
Red flags: when positioning advice is not enough
Red flags are not “internet drama.” They’re patterns clinicians take seriously: worsening weakness, numbness in saddle area, new bladder/bowel control problems, severe trauma, fever with back pain, or rapidly escalating symptoms. If that’s you, your next step is not a pillow stack.
Quick Eligibility Checklist (Yes/No)
- Yes if your symptoms feel calmer lying down with knees supported.
- Yes if you can change the “volume” with small position tweaks.
- No if you have new bladder/bowel issues, saddle numbness, or rapidly worsening weakness.
- No if knee-up positions reliably spike symptoms within 60 seconds.
Neutral next step: If you’re a “maybe,” try a 3-minute test with conservative height, then reassess.
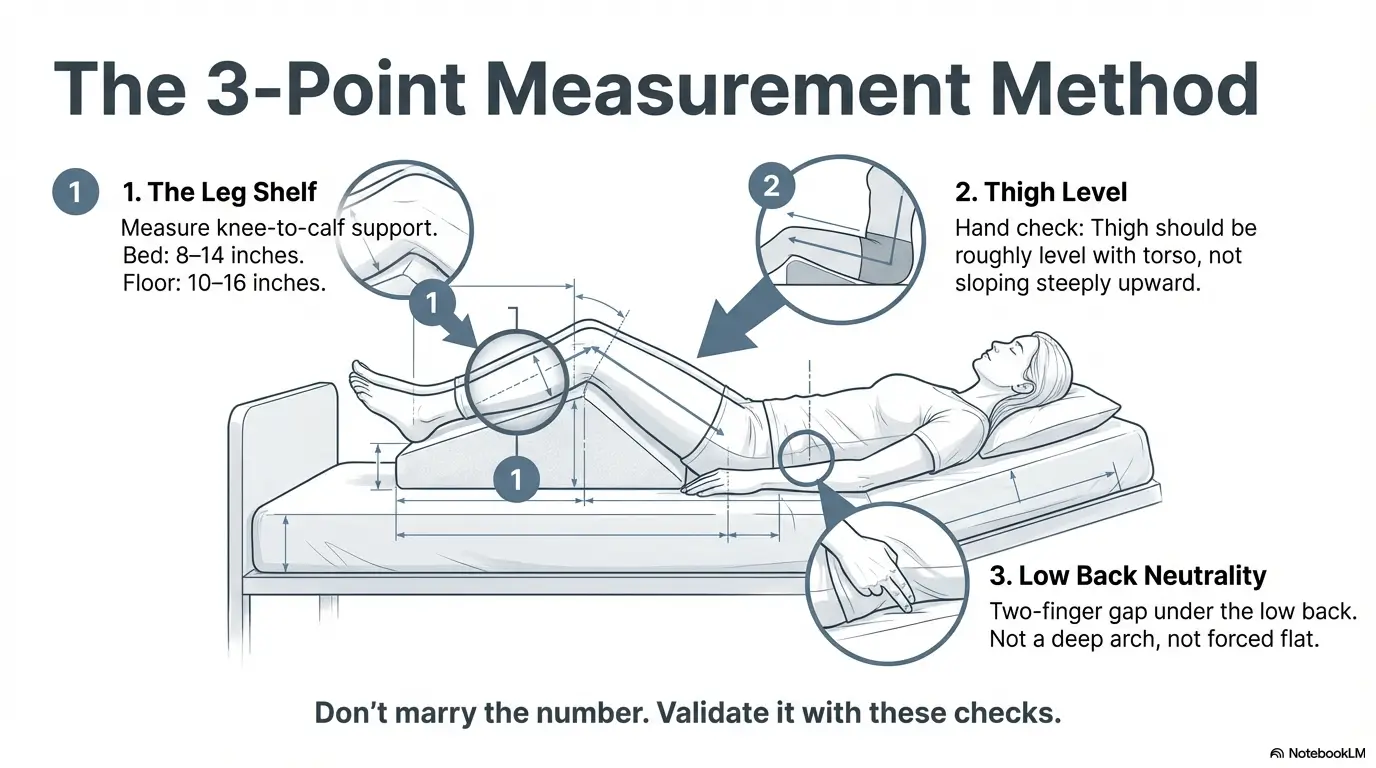
3) Exact pillow height: the 3-point measurement method (no guessing)
Step 1: measure “knee-to-calf shelf” (the number that matters)
Here’s the shift: you’re not chasing “pillow height.” You’re building a leg shelf that supports calves so the knees can rest near 90° without stretching hamstrings.
A practical starting estimate:
- On a bed: start around 8–14 inches of support height under the calves.
- On the floor: start around 10–16 inches (firmer surface often needs more height to create the same joint angles).
If you’re smaller, start lower; taller, start higher. But don’t marry the number. We’ll validate it with checks.
Step 2: match thigh level (use your hand as a level)
Place your hand flat on the front of your thigh. Your goal is “quiet level,” not rigid perfection: thighs roughly level relative to your torso, not sloping steeply upward toward your hips. If your knees are way higher than your hips, you’re likely over-flexing.
Step 3: confirm low-back neutrality (two-finger check)
Slide two fingers under your low back. You want a small, natural gap—not a deep arch that could load your back, and not a forced flattening that feels like you’re doing an ab workout. Your belly should feel soft. If you’re bracing, you’re negotiating with pain, not calming it.
Here’s what no one tells you… “height” is secondary to where the support touches
If the support touches only your heels/ankles, your hamstrings can stay under tension and your pelvis may tip. If the support touches the mid-calf (or lower calf), your hamstrings often relax faster. This is why two setups with the same “height” can feel totally different.
Mini Calculator: Starting Support Height (Not a Rule—A Launch Pad)
Enter your height and where you’re doing 90/90. You’ll get a conservative starting range to test with the 3 checks.
Output will appear here.
Neutral next step: Use the range to pick one setup, set a timer for 3–5 minutes, and adjust only one variable.
4) Bed setup: pillow stack, ottoman, or wedge—what actually stays put
Bed rule #1: support the calves, not the heels
If your heels are the only contact point, your knees hover and your hamstrings keep working. Slide support up so it cradles the lower to mid-calf. Your ankles can hang slightly off the edge—comfortably—like your legs are finally allowed to be heavy.
Tiny lived-experience moment: I once “solved” the height with a beautiful pillow tower… that supported only my ankles. My hamstrings disagreed loudly at minute two.
Bed rule #2: prevent hamstring stretch (the silent flare trigger)
Your hamstrings connect into the pelvis. If they’re stretched, the pelvis can tip and the low back can react. In a bed setup, the goal is zero tug behind the thigh. If you feel a stretch, either lower the knee height slightly or move the contact point higher on the calves.
Best options: wedge vs pillows vs sofa cushion (stability vs adjustability)
You’re choosing between stability and micro-adjustability:
- Wedge: stable, consistent angle, less midnight sliding. Downside: less fine-tuning if it’s slightly too high/low.
- Pillow stack: endlessly adjustable. Downside: it can shift, compress, and turn into a saggy ramp at 2 a.m.
- Sofa cushion / firm ottoman: often the best “cheap stability,” especially if it’s firm and wide enough for calves.
Decision Card: Wedge vs Pillows (Bed)
Choose a wedge if…
- You wake up because the stack slid.
- You want repeatability night to night.
- You do better when you “set and forget.”
Choose pillows/ottoman if…
- You need tiny tweaks (1–2 inches matters).
- Your hips pinch easily with fixed angles.
- You’re still finding your “quiet” range.
Neutral next step: Pick one option and test it for 3 nights before changing equipment.
Pattern interrupt: Let’s be honest… pillows slide at 2 a.m.—fix it like this
The fix is not willpower. It’s friction and containment:
- Put a towel over the pillow stack (less slippery).
- Use a pillowcase on the whole stack like a “bundle.”
- Brace the stack with a firm cushion behind it.
- If your mattress is very soft, place a thin board or firm foam pad under the stack to reduce sink-and-slide. If you’re debating whether a topper will help or hurt, see 2 vs. 3 inch mattress toppers for back pain setups so you’re not guessing with your wallet.
5) Floor setup: firmer surface, different math (and fewer surprises)
Why floor often needs more height (counterintuitive but common)
On the floor, your pelvis doesn’t sink. That means you sometimes need more calf height to reach the same hip/knee angles you get on a mattress. The floor is unforgiving—but in a good way: when you find the right build, it usually stays put. If your bed setup keeps “drifting,” it can also help to revisit mattress firmness for sciatica so your surface stops changing the math mid-session.
Two safe builds: chair/ottoman method vs stacked cushions method
- Chair/ottoman method: Lie on your back and place calves on a stable chair seat. Add a folded towel under calves if you need a small lift.
- Stacked cushions method: Use firm couch cushions or dense foam blocks. Avoid “puffy” pillows that collapse.
Lived experience: when my back was cranky, the chair method was the first one that felt “engineered” instead of improvised. It’s hard for a chair to betray you at 2 a.m.
The “hip pinch” test: when your support is too high
Hip pinch often means you’re too flexed or your knees are too close together. First response: lower by 1–2 inches or widen knee spacing slightly. If pinch persists, move support lower on the calves and re-check low-back neutrality.
Curiosity gap: why the floor version can feel better in 60 seconds
Because there’s less “mattress math.” On a soft bed, your pelvis sinks, your calves sink, the stack compresses, and your angles drift. On the floor, what you set is what you get—so your nervous system can relax faster.
6) Micro-adjustments that change everything: tilt, spacing, and toe position
Knee spacing: “hip-width” vs “together” (which calms the leg?)
Start at hip-width. If you feel inner-hip strain or hip pinch, go a touch wider. If you feel unstable through the pelvis, bring knees slightly closer. The right spacing often feels boring—in a good way.
Toe angle: neutral feet to reduce calf tension
Let feet rest neutral—no hard pointing, no hard flexing. If you notice your calves “working,” you’re accidentally bracing. Wiggle toes, then let them go slack.
Pelvic tilt: the 1-inch tuck that can stop the flare
If your low back arches, try a tiny posterior tilt: imagine zipping up tight jeans—just a one-inch tuck. Not a crunch. If that makes symptoms worse, undo it. We’re looking for “quiet,” not discipline.
Open loop: the tiny adjustment most people miss—until day 3
The contact point. Many people keep changing height and never change where the support touches. Move the shelf from ankles to mid-calf and re-test before you add another pillow. This is the sneaky lever.
7) Common mistakes: 7 ways people accidentally make sciatica angrier
Mistake #1: pushing the knees too high (over-flexion)
Knees way above hips can increase hip flexion and irritate certain patterns. Fix: lower support 1–2 inches and re-check tingling.
Mistake #2: supporting only ankles (creates hamstring tension)
Fix: slide support up to the calves. Your hamstrings should feel like they’ve been fired from their job.
Mistake #3: arching the low back to “find comfort”
A deep arch can load sensitive structures. Fix: adjust calf height first, then add or remove a tiny towel roll (more on that in troubleshooting).
Mistake #4: holding the position too long, too soon
If the nervous system is sensitive, long holds can provoke. Start small. Earn your minutes.
Mistake #5: chasing numbness relief while ignoring weakness
Numbness changes can be confusing. But if you notice true weakness (foot drop, can’t lift toes well), don’t treat it like a comfort puzzle. Get evaluated.
Mistake #6: using a soft mattress without stabilizing the stack
Soft surfaces change the angles over time. Fix: firmer support under the calves (ottoman, wedge, or a firm base under pillows). (If you’re trying to decide whether to change the surface itself, start with a sciatica-focused mattress firmness guide so you’re not troubleshooting on quicksand.)
Mistake #7: treating 90/90 as a cure, not a tool
90/90 is a symptom-calming position. It can buy you sleep and reduce irritability—so you can walk, move, and rehab more comfortably. That’s a win. It’s not a forever home.
8) Don’t do this: time, frequency, and the “relief trap”
The relief trap: why longer isn’t always better
When something finally helps, the brain says, “Do it forever.” But sensitive systems can rebound. If you stay too long, you may stiffen up, shift pelvic load, or wake up sore in a new place. Relief is the point—but stable relief is the pointier point.
A safer ramp-up: 3–5 minutes → 8–12 minutes → stop rule
Try this progression:
- First test: 3–5 minutes, then stand up and walk 60 seconds. If getting up is the flare moment, use a gentle log roll technique for sciatica so you don’t “win the position” and lose the transition.
- If quieter: 8–12 minutes next time.
- Stop rule: if symptoms increase or shift “down the leg” more intensely, end the session and switch to walking or a neutral position.
Anecdote: the nights I tried to “sleep in it,” I woke up with hips crankier than my original problem. Shorter sessions were oddly more powerful.
What to do if symptoms shift sides or move down the leg
Treat it as data. Stop, reset, and try a smaller change next time. If symptoms consistently worsen or migrate, 90/90 may not be your move right now.
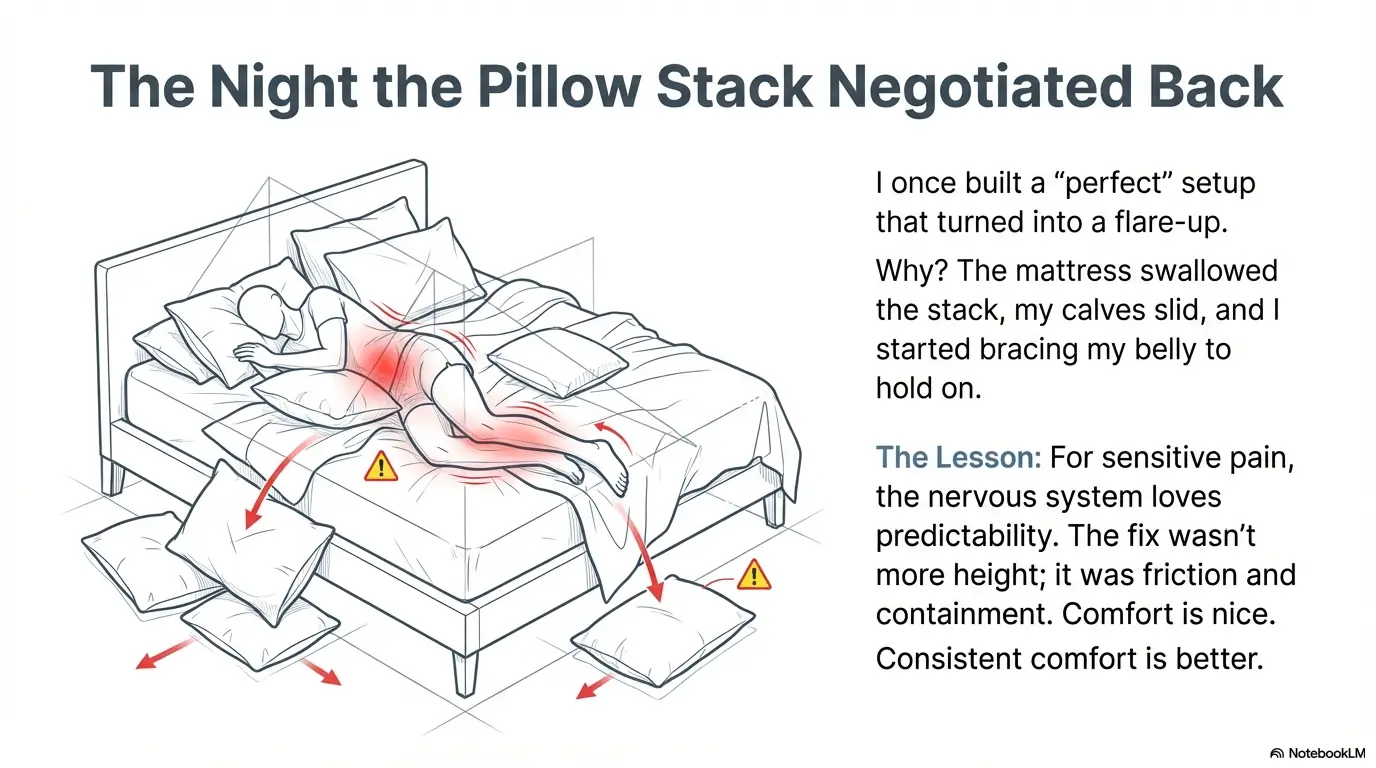
Short Story: The Night the Pillow Stack Negotiated Back
I once built a perfect-looking 90/90 setup on my bed—two pillows, a folded blanket, a sense of triumph. For ten minutes, it felt like a small miracle. Then, slowly, the mattress swallowed the stack. My calves slid. My knees drifted higher. Without noticing, I started bracing my belly to “hold position.” That’s when the tingling got louder—like someone turned on a fluorescent light in my leg. The fix wasn’t more height. The fix was contact point (support under calves, not heels), then a firmer base so the stack couldn’t melt into the bed. I learned the boring truth: for sensitive pain, the nervous system loves predictability. Comfort is nice. Consistent comfort is better.
9) Troubleshooting by symptom: fast fixes in under 60 seconds
If pain increases: lower the knees by 1–2 inches first
Don’t overhaul the setup. Lower support slightly and re-check symptoms for 30–60 seconds. Over-flexion is a common trigger.
If tingling increases: change calf contact point (not just height)
Slide support from ankles to mid-calf, or from mid-calf to lower calf, and re-test. Your hamstrings may relax with a better contact point even at the same height.
If low back aches: add a small lumbar towel roll (or remove it)
A tiny roll (think: hand-towel thickness, not a foam log) can fill an excessive gap if your back is arching. But if you feel “jammed,” remove it. Your low back should feel neutral—not pinned.
If hips pinch: widen knees + reduce hip flexion
Widen knee spacing slightly, then lower support 1–2 inches. Hip pinch often responds to “less flexion, more space.”
If nothing changes: when 90/90 isn’t your move (yet)
No change after 3 careful attempts can mean: the pattern needs a more neutral position, you’re too inflamed for this angle, or you need a different strategy (short walk breaks, side-lying pillow setup, clinician guidance). A simple “next morning” experiment that pairs well with sleep positioning is morning sciatica nerve glides—short, conservative, and easy to track.
- Height first (1–2 inches).
- Then contact point (ankle vs calf).
- Then spacing (knees hip-width vs wider).
Apply in 60 seconds: Pick one change, set a 60-second timer, and decide: better, worse, or same.
10) When to seek help: the “don’t wait” checklist
Same-day care: new bladder/bowel issues, saddle numbness, major weakness
If you notice new bladder/bowel control problems, numbness around the genitals/anus (“saddle” area), or significant/worsening weakness, seek urgent medical evaluation. This is the category where major medical resources like Mayo Clinic and NHS guidance consistently say “don’t wait.”
Within 24–72 hours: worsening numbness/tingling or pain that won’t settle
If symptoms are escalating despite reasonable self-care, or you’re losing sleep night after night, get help sooner rather than “proving toughness.” Sleep debt makes pain louder.
PT/clinician fit: recurring flares, sleep disruption, walking limitation
If your walking is limited, flares keep returning, or you’re building your life around avoiding symptoms, a physical therapist or clinician can help identify the pattern and guide safer progressions. If you want a grounded overview of what that process can look like, start with physical therapy for sciatica.
Quote-Prep List (If You’re Comparing Wedges, Pillows, or a PT Visit)
- Your best-feeling support height range (after testing).
- Bed firmness (soft/medium/firm) and whether the stack compresses.
- What worsens symptoms: sitting, bending, standing, walking, sleeping.
- Whether symptoms are one-sided or both sides.
- Any weakness (toe lift, heel walk) or new numbness zones.
Neutral next step: Write these in your phone notes before you shop or book—your future self will thank you.
11) FAQ: 90/90 position for sciatica (US PAA-style)
How long should I stay in 90/90 for sciatica?
Start with 3–5 minutes. If symptoms are calmer (or at least not worse), build to 8–12 minutes. If you’re using it for sleep, consider it a “reset” before bed rather than an all-night posture.
What pillow height is best for 90/90 on a bed?
Many adults land around 8–14 inches of calf support on a bed, but the best height is validated by your checks: thighs roughly level, low back neutral, and no tingling increase. Height matters less than calf contact point and stack stability.
Is a wedge better than pillows for 90/90?
A wedge is often better for stability and repeatability. Pillows are better for micro-adjustments. If your pillows slide or compress overnight, a wedge or firm ottoman usually wins.
Should my thighs be perfectly parallel to the bed/floor?
No. Aim for “quiet comfort,” not geometry perfection. If you chase exact parallel and force the knees too high, you can irritate symptoms. Let the checks decide.
Why does 90/90 make my tingling worse?
Common reasons: knees too high (too much hip flexion), ankles supported instead of calves (hamstring tension), or low back arching. First tweak: lower support 1–2 inches. Second tweak: change calf contact point. If it still worsens, stop and choose a more neutral position.
Can I sleep in 90/90 all night?
It’s usually better as a short reset than an all-night setup—unless your clinician has specifically recommended it for your pattern and you can maintain a stable, neutral position without bracing. If you wake up stiffer or more symptomatic, shorten your time. If sleep has become the main battleground, you’ll probably get more mileage from a broader approach like how to sleep with sciatica rather than betting everything on one posture.
Is 90/90 better on the floor or on the bed?
The floor often provides more predictable angles because it doesn’t compress, but it can also feel harder on sensitive backs. Bed is gentler, but the setup can drift as the mattress and pillows compress. Pick the surface that stays stable and keeps symptoms quieter.
What if my pain is on one side—do I adjust knee spacing?
Start hip-width. If you feel hip pinch, widen slightly. If you feel pelvic wobble, bring knees a touch closer. Keep adjustments small and test for 60 seconds.
Does 90/90 help piriformis syndrome too?
Sometimes—especially if the setup reduces guarding and lets the hip muscles relax. But piriformis-like symptoms can respond differently to hip flexion. If it spikes buttock pain or tingling, stop and try a different position.
What’s the best alternative if 90/90 doesn’t help?
Often: side-lying on the non-painful side with a pillow between knees, or a gentle “neutral” back-lying setup with a smaller knee pillow (less hip flexion). If you’re unsure which prop is actually helping, compare knee pillow vs. body pillow for sciatica. If symptoms persist, a PT can help identify which direction of movement calms your pattern.
12) Next step: the 2-minute setup you can do tonight
Do this now: build support, run the 3 checks, set a timer, log the result
- Build your shelf: support under calves (not just heels).
- Run the 3 checks: thigh level (roughly), low-back neutral (two-finger gap), no symptom increase (60 seconds).
- Set a timer: start with 3–5 minutes.
- Log one sentence: “Better / worse / same, and where.”
Anecdote: the nights I wrote one sentence, I stopped “reinventing the setup” every evening. My body likes boring patterns.
Keep it simple: one variable change per night (height or contact point)
If you change height, contact point, spacing, and pelvic tilt all at once, you’ll never know what helped. Make one tweak, test, and move on with your night.
- Support calves first.
- Adjust in 1–2 inch steps.
- Stop if symptoms worsen.
Apply in 60 seconds: Set a 60-second “symptom check” timer after every tweak before you decide anything.
Conclusion
Here’s the loop we opened at the start: “What’s the exact pillow height?” The honest answer is: it’s the height that passes the checks—thighs roughly level, calves supported, low back neutral, and symptoms not louder. The most powerful move is not adding a third pillow; it’s moving the support from ankles to calves and stabilizing the build so your body can trust it.
Check 1 — Thighs
Roughly level. Not knees way above hips.
Check 2 — Calf contact
Support under calves (not just heels/ankles).
Check 3 — Low back
Small natural gap. No deep arch, no forced flattening.
Stop rule
If tingling/pain worsens: end, walk 60 seconds, reassess.
If you have 15 minutes right now, do this: build one shelf, run the 3 checks, do a 5-minute timer, then write one sentence about what happened. That single note is how you stop guessing—and start sleeping. (And if side-sleeping is still your “real life default,” you’ll probably also want side sleeper sciatica at night tips so your whole night isn’t decided by one posture.)
Last reviewed: 2026-01-24.
FAQ
Is it normal to feel “weird” in the first 30 seconds?
Sometimes. A new position can feel unfamiliar. What matters is the trend: within 60–120 seconds, you should feel quieter or at least not worse.
Should I add heat before 90/90?
If heat helps you relax and you use it safely, it can make the position more comfortable. If heat increases inflammation-feel or makes you sleepy in a risky way, skip it and keep the session short. If you want a safety-first rundown before you try it, see sleeping with a heating pad for sciatica.
What if my mattress is extremely soft?
Expect more drift. Use a firmer base under the calves (ottoman, wedge, firm cushion), or test the floor version for predictability. If you’re deciding whether to change the bed feel itself, start with mattress firmness for sciatica.
What if my knees can’t comfortably bend to 90°?
You don’t need perfect angles. Lower the support until your hips and knees feel easy and your symptoms are calmer.
When should I stop experimenting and get help?
If symptoms worsen over a few days, sleep keeps breaking, or you notice weakness, numbness expansion, or any red flags—get evaluated.
