
Navigating Stairs with Confidence: A Hinged Brace Strategy
One stair trip can turn a decent knee day into a swelling-and-regret evening.
Orthopedic pain management with a hinged knee brace for stairs is about reducing the number of bad steps your knee has to survive. Beyond the pain, challenges like brace slippage, carrying laundry, slick socks, and poor lighting create a “perfect storm” for instability.
“I’ll just do it quickly” is the most dangerous thought you can have on a landing.
The Safety Method
- Brace fit & support check
- The strong-leg stair rhythm
- Home setup & fall prevention
The Protocol
- Check the brace
- Assess the stairs
- Listen to the “bargaining”
Table of Contents

Fast Answer
Orthopedic pain management with a hinged knee brace for stairs is about more than wearing the brace tightly. The safer approach is to confirm brace fit with a clinician, reduce stair trips, use railings, move slowly, lead with the stronger leg going up, protect the painful leg going down, and stop if pain, swelling, buckling, or instability increases.
A hinged knee brace may support the joint, but it does not replace balance, footwear, lighting, strength, or common sense. The brace is a tool. The staircase is still a staircase. It remains undefeated in the category of “places where tiny mistakes become large problems.”
- Brace position matters before every stair trip.
- Handrails and clear hands matter as much as the brace.
- Pain, swelling, or buckling should change the plan.
Apply in 60 seconds: Before the next stair trip, check brace position, shoes, rail access, and whether your hands are free.
Safety / Disclaimer
This article is for general education, not diagnosis or personal medical advice. A hinged knee brace may be used for knee instability, ligament injuries, arthritis, post-surgical protection, or recovery support, but the correct brace type, hinge setting, fit, and activity limits should come from a healthcare provider, surgeon, orthopedist, athletic trainer, or physical therapist.
Do not change hinge settings, brace tightness, medication timing, exercise limits, walking aid use, or stair routines based only on an article. Bodies are inconveniently specific. Knees are even more specific. The knee that behaves at 9 a.m. may stage a small rebellion at 7 p.m.
Seek urgent medical help after a major injury or sudden change, especially if the knee looks deformed, you heard or felt a pop, you cannot bear weight, pain is intense, or swelling appears suddenly. Also get prompt medical advice for fever, redness, warmth, new calf swelling, repeated buckling, or a brace that will not stay in place.
Start Here: The Brace Is Support, Not Permission
Why a Hinged Knee Brace Changes the Stair Problem
A hinged knee brace may help limit certain motions and provide side-to-side support, especially when the knee feels unstable. That can be useful for some ligament injuries, arthritis patterns, post-injury recovery plans, and clinician-directed mobility support.
But stairs ask for more than knee support. They ask for balance, hip strength, ankle control, timing, vision, hand placement, and the quiet courage to go slowly even when you are late for the laundry buzzer.
I once watched someone do everything “right” with a brace, then almost lose balance because they carried a mug, a phone, and one sock with a mysterious emotional attachment. The brace was doing its job. The hands were not.
The Real Goal: Fewer Bad Steps, Not Braver Steps
The point is not to prove that you can still handle stairs. The point is to reduce the number of risky moments your knee has to survive in one day.
That means asking better questions:
- Can this trip wait until pain is lower?
- Can I move the item to one level instead?
- Can I use the railing without carrying anything?
- Is the brace still where it started?
- Am I rushing because I am actually safe, or because I am annoyed?
Let’s be honest: Stairs Expose Every Weak Link
Stairs are not impressed by optimism. They expose swelling, weak hips, poor lighting, slick socks, loose rugs, medication side effects, morning stiffness, and the strange human habit of thinking “I’ll just do it quickly” right before doing the least quick thing imaginable.
The practical shift: treat stairs as a planned task, not background scenery. A planned stair trip is slower, emptier-handed, better lit, and less dramatic.
Who This Is For, and Who Should Pause First
For Knee Pain With Instability, Arthritis, or Recovery Limits
This guide is for adults using a hinged knee brace because stairs feel unstable, painful, or unpredictable. That may include people managing arthritis, ligament recovery, mild buckling, a prior knee injury, or a clinician-directed brace plan.
It is also for the person who says, “I’m fine,” while gripping the rail like it owes them money. Fine is not a measurement. Function is.
Not For Sudden Injury, Severe Swelling, or a Deformed Knee
Some knee problems should not be handled with stair tips. If pain is sudden, severe, or linked to a fall or twist, pause the home strategy and get medical guidance.
Mayo Clinic’s knee pain guidance tells people to seek urgent care after a major injury when the knee is deformed, a popping sound happened at the time of injury, the knee cannot bear weight, pain is intense, or swelling is sudden.
Caregiver Note: Watch the Stairs, Not Just the Pain Score
If you are helping a spouse, parent, or older adult, do not rely only on “How bad is the pain from 1 to 10?” Pain scores have their place, but stair behavior often tells the truth first. For a broader look at aging, home safety, and pain patterns, see this guide to senior orthopedic pain management.
Watch for hesitation, sideways stepping, gripping both rails, avoiding stairs, pausing halfway, or saying “I’ll do it later” three days in a row. That little phrase can be a smoke alarm with manners.
- Yes if the brace was prescribed or recommended and stairs feel manageable with caution.
- Yes if pain is familiar, not suddenly severe, and you can bear weight as instructed.
- No if there is sudden swelling, deformity, intense pain, fever, redness, warmth, or inability to bear weight.
- No if the knee repeatedly buckles or the brace will not stay positioned.
Neutral next step: If any “No” applies, ask a clinician or physical therapist before using stairs as usual.
Brace Fit First: The Small Slippage That Becomes a Big Risk
Check the Hinge Line Before the First Step
Before you climb, check whether the brace sits where your provider told you it should sit. For many hinged knee braces, the hinge should line up around the knee joint area according to the specific brace instructions. But brace designs vary, and surgical protocols can be very specific.
Cleveland Clinic explains that a healthcare provider or physical therapist should show patients how to wear and adjust a knee brace so it supports the knee joint properly.
That matters because a brace that has drifted down the leg may feel present without actually supporting the knee the way it was intended. It becomes a security blanket with straps. Cozy, perhaps. Not ideal.
Tight Is Not the Same as Safe
Many people respond to slipping by tightening every strap until the brace feels like medieval upholstery. That can backfire.
A brace should generally feel secure, but over-tightening can cause problems such as discomfort, skin irritation, numbness, tingling, or swelling below the brace. If that happens, stop and follow the adjustment guidance you were given. People comparing brace costs, eligibility, and reimbursement questions may also want to understand HSA eligible braces and supports before buying extra gear.
- Check skin after longer wear periods.
- Notice numbness, tingling, color change, or swelling.
- Do not use pain as proof the brace is “working.”
- Ask for a fit check if the brace repeatedly slides.
Here’s what no one tells you: The Brace Can Drift Midday
A brace can fit well in the morning and shift by lunch. Sweat, swelling changes, pant fabric, repeated sitting, and walking can all change how the brace behaves.
I learned this watching a relative adjust a brace perfectly before breakfast, then stand up after two hours of sitting and find the hinge had migrated south like it had vacation plans.
The fix is not panic. It is habit. Check the brace before stairs, after long sitting, after sweating, and after any moment when the knee feels different.
Stair Method: The Safer Rhythm Most People Forget
Stronger Leg Up, More Protected Leg Down
A common stair strategy is often taught this way: lead with the stronger or less painful leg when going up, and protect the painful or braced leg when going down. Many people remember it with the old rehab phrase: “up with the good, down with the bad.”
That phrase is not poetry. It is more like refrigerator-magnet wisdom from the physical therapy kingdom. But it sticks because it helps you avoid asking the painful knee to do the hardest job at the worst moment.
Follow your clinician’s instructions if they differ. Post-surgical restrictions, brace settings, weight-bearing limits, and injury type can change the safest method. If the knee issue is connected to joint replacement recovery, the stair plan should fit the larger knee replacement pain management strategy rather than becoming a separate little staircase experiment.
One Rail Is Good; Two Points of Contact Are Better
The brace supports the knee. The rail supports your balance. These are different jobs.
When possible, keep one hand on a sturdy handrail. If you were prescribed a cane or crutch, use it exactly as instructed. Do not carry laundry, coffee, pets, trash bags, or toddlers on stairs while you are testing a sore knee. The toddler may object. The knee will object louder.
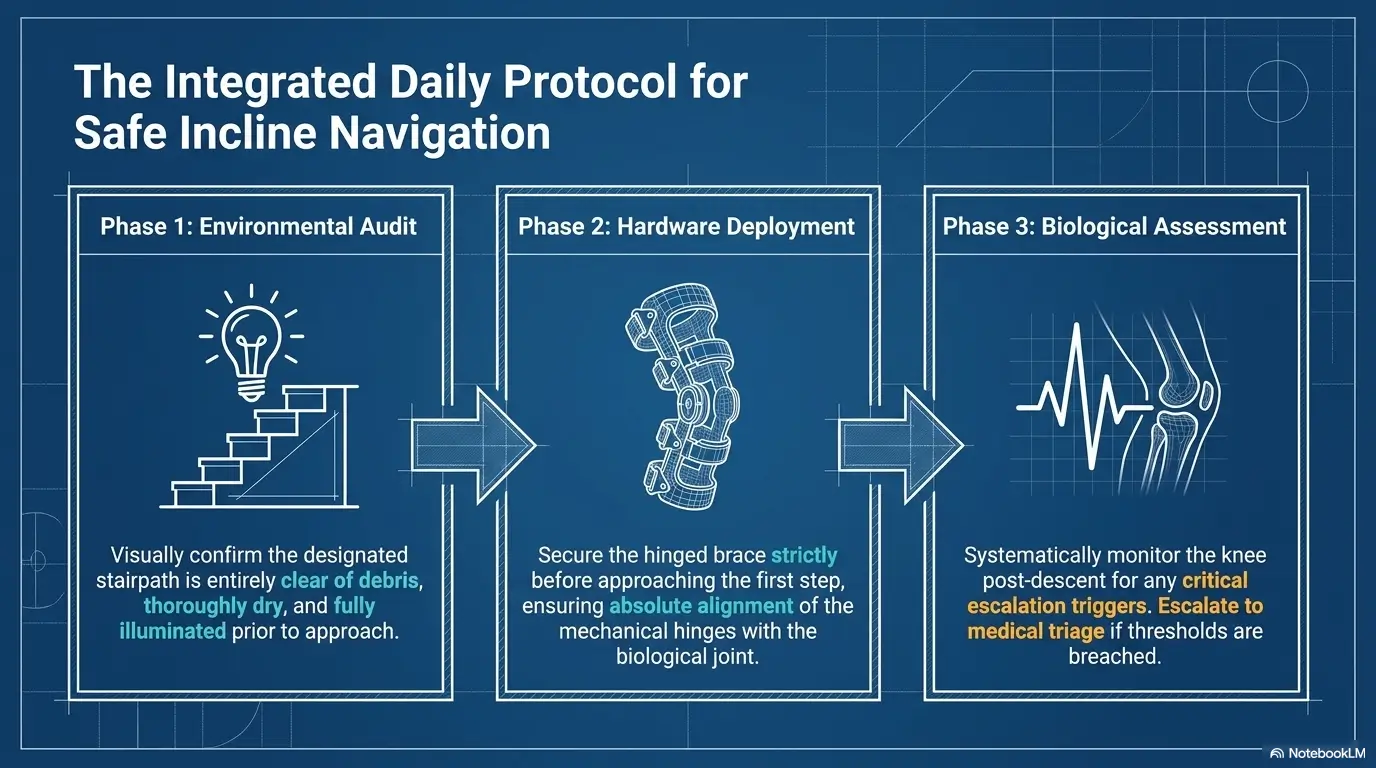
Stair Safety Rhythm: Brace + Rail + Pause
1️⃣
Check
Brace position, straps, shoes, lighting.
2️⃣
Hold
Use the rail. Keep at least one hand free.
3️⃣
Step
Stronger leg up, protected leg down, unless told otherwise.
4️⃣
Pause
At landings, check pain, wobble, breath, and brace drift.
Stop at the Landing Before the Knee Negotiates Without You
Landings are not wasted space. They are negotiation tables. Use them.
Pause for 5 to 10 seconds. Notice whether the knee wobbled, whether pain increased, whether your breathing changed, and whether the brace still sits correctly. If something feels off, that is not weakness. That is useful data arriving before the invoice.
- Use the rail every time.
- Keep your hands free.
- Pause at landings before continuing.
Apply in 60 seconds: Practice one slow stair trip with empty hands before you need to carry out a real task.
Pain Timing: When Stairs Hurt Before the Knee Complains
Morning Stiffness Needs a Different Plan Than Evening Swelling
Knee pain is not always the same pain all day. Morning stiffness may make the first stair trip feel wooden and uncertain. Evening swelling may make the knee feel heavy, hot, or less trustworthy. Same stairs. Different knee weather.
For some people, a short warm-up on level ground, clinician-approved movement, or waiting until stiffness settles may help. For others, late-day stair trips need to be reduced because fatigue and swelling make mechanics sloppy.
The practical move is to schedule necessary stair trips during your best window. This is not indulgent. It is logistics.
Pain Spikes Are Data, Not Drama
A pain spike is not a moral failure. It is information. The trick is to write it down before memory turns it into fog.
Track just 4 things:
- Did pain worsen going up or going down?
- How many steps triggered it?
- Did the knee buckle, lock, or feel unstable?
- Did pain settle after rest, or keep building?
Those details help a clinician or physical therapist adjust the plan. “Stairs hurt” is true but vague. “Going down hurts after step 4, and the brace slips after sitting” is a map. If you keep hearing that imaging looks fine while function still feels wrong, this explainer on a normal X-ray but pain that continues may help you organize the next conversation.
Don’t Use the Brace to Bargain With Pain
A brace can make you feel more supported. That does not mean you get unlimited stair credits.
It is tempting to think, “The brace is on, so I can push through.” That sentence has caused many knees to file formal complaints. If pain, swelling, buckling, or instability increases, the plan should shrink, not expand.
Show me the nerdy details
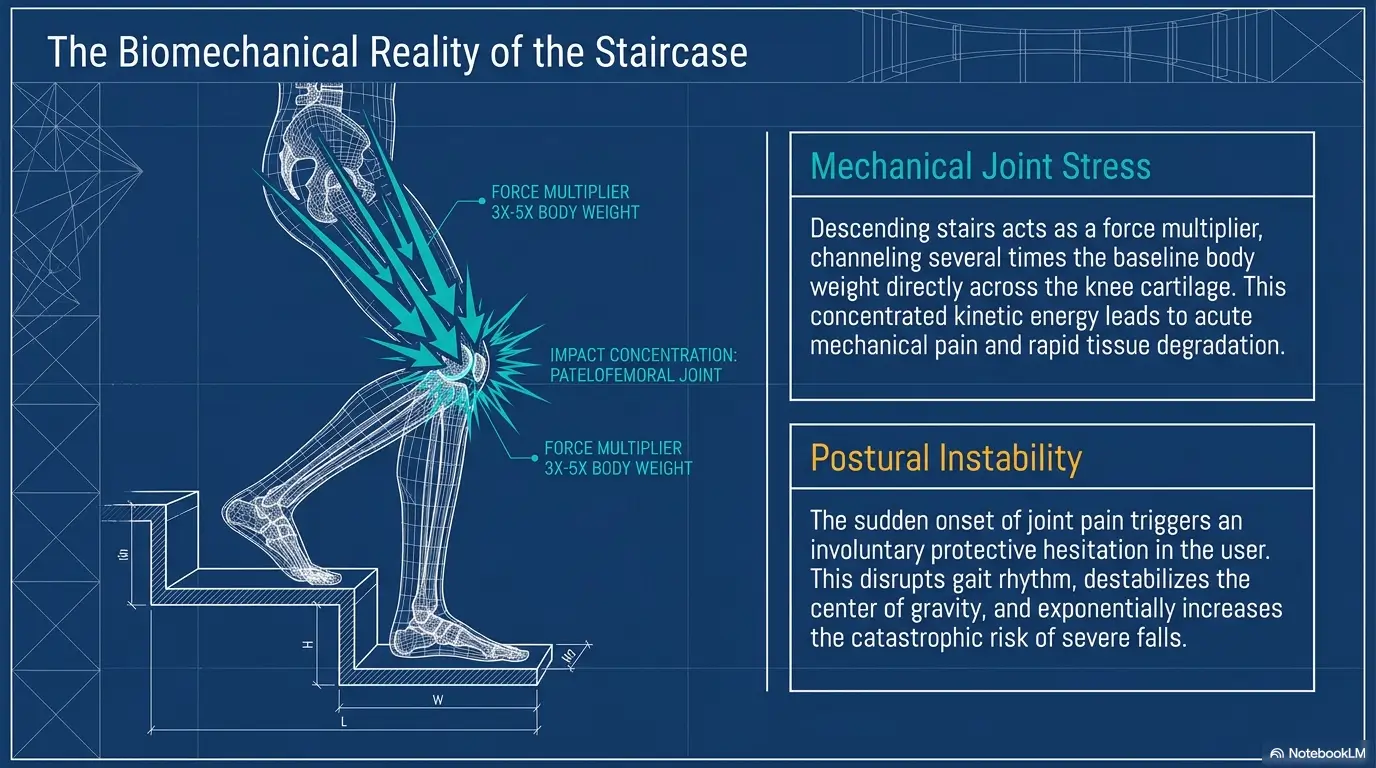
Stairs increase demand because the knee must control body weight while flexing and extending. Descending stairs can feel especially difficult because the body lowers under control, asking the quadriceps, hips, ankle, and balance systems to coordinate. A hinged brace may influence knee motion and stability, but it does not replace muscle control, proprioception, visual input, or safe environmental setup.
Common Mistakes: Don’t Let the Brace Become a Blindfold
Mistake 1: Wearing the Brace but Skipping the Handrail
This is the classic trap. The brace feels supportive, so the rail starts to seem optional. It is not.
The handrail gives your upper body a way to help with balance. It also buys time if the knee hesitates. A brace may support the joint, but it cannot grab the wall for you. It has many talents. Fingers are not among them.
Mistake 2: Taking Stairs While Carrying Too Much
Laundry baskets are sneaky. They block your view, steal both hands, and turn a normal stair trip into an obstacle course with fabric softener.
During a flare-up or recovery period, use smaller loads. Make two trips on level ground if needed, but reduce stair carrying. Better yet, stage items near the stairs and move them when someone else can help.
Mistake 3: Trusting the Brace After It Slips
If the brace slips, stop safely. Hold the rail. Move to a stable landing if possible. Readjust only according to your instructions.
Do not keep going because “it’s only a few more steps.” Many household injuries have begun with that exact phrase, wearing slippers and carrying a basket.
Mistake 4: Ignoring Shoes, Socks, and Stair Edges
Footwear matters. Slick socks, loose slippers, worn soles, curled stair mats, poor lighting, and low-contrast stair edges can all make a braced knee less safe.
The CDC emphasizes that falls are not inevitable with age and that proven strategies can reduce fall risk. For stairs, that often means plain, unglamorous fixes: clearer walkways, better lighting, sturdy rails, safer shoes, and fewer rushed trips. These same principles matter in broader elderly orthopedic pain management, where the home environment can quietly decide whether a good plan survives real life.
- Go now if pain is familiar, brace fit is stable, lighting is good, hands are free, and the rail is available.
- Delay if pain is rising, the knee feels wobbly, the brace slipped, or you are carrying something awkward.
- Ask for help if stairs require both hands, the descent feels unsafe, or the knee buckled recently.
Neutral action: Choose the lowest-risk option for this trip, not the option that proves the most.
Home Setup: Make the Stairs Less Demanding Before You Climb
Move Daily Items to One Level Temporarily
A stair diet is simple: reduce unnecessary stair trips while the knee is painful, unstable, swollen, or healing.
That may mean keeping duplicate basics upstairs and downstairs: phone charger, water bottle, medications if safely stored, reading glasses, tissues, comfortable shoes, and a small trash bag. No one wins a medal for climbing stairs to retrieve lip balm. If such a medal exists, it should be discontinued.
I have seen one small basket at the top and bottom of the stairs change an entire recovery week. Not fancy. Not expensive. Just fewer “I forgot something” climbs.
Light the Landing Like It Matters
Lighting is not decoration when you are managing knee pain. It is safety equipment.
Use bright, even lighting on stairways and landings. Reduce glare where possible. Make stair edges easier to see, especially if vision is low, depth perception is poor, or nighttime bathroom trips are part of the routine.
Remove the Almost-Invisible Hazards
The most dangerous hazards are often boring: a curled mat, a charging cord, a pet toy, a slippery transition, a shoe left near the bottom step, or a dark landing that everyone “knows” is there.
- Clear clutter from the top and bottom of stairs.
- Secure or remove loose mats near stairways.
- Keep pets away during stair trips if they weave underfoot.
- Use night lights for late bathroom trips.
- Make sure railings are sturdy, not decorative noodles.
Short Story: The Laundry Basket That Lost Its Throne
Short Story: A woman I know had a hinged brace after a knee injury and insisted the stairs were “fine.” The real problem was laundry. Twice a day, she carried a full basket downstairs, leaning backward to see over it, then used her elbow against the wall because both hands were occupied.
Nothing dramatic happened at first, which made the habit seem safe. Then one afternoon her brace slipped after sitting, the basket blocked her view, and she froze halfway down. Her spouse did not ban stairs. They changed the system. Smaller laundry bags replaced the basket. A rail-side hand stayed free. Clean clothes waited downstairs until evening. The knee did not magically heal overnight, but the staircase stopped feeling like a daily exam she could fail.
Pain Relief Stack: What Supports the Brace Without Overpromising
Use Clinician-Approved Ice, Heat, Rest, or Medication Timing
Pain relief should support safer movement, not disguise a problem so you can overdo it.
Ask your clinician or pharmacist about medication timing, especially if you are older, take blood thinners, have kidney disease, have stomach ulcer history, use multiple medicines, or are recovering from surgery. Over-the-counter does not mean consequence-free. It means “available near the toothpaste,” which is not the same thing.
Ice, heat, rest, elevation, compression, or gentle movement may be useful for some people, but the right choice depends on the cause of pain, swelling, injury stage, and medical history. Some people also ask about device-based options, and this guide to a TENS unit for knee pain can help frame that conversation without treating gadgets like magic.
Match Activity to the Knee’s Best Window
Many people have a best movement window. Maybe it is after morning stiffness eases. Maybe it is before late-day swelling arrives. Maybe it is 20 minutes after a clinician-approved routine.
Use that window for necessary stairs. Save optional stair trips for better days, or skip them altogether when the knee is sending storm clouds.
Build Strength Around the Knee, Not Just Protection Over It
A brace protects from the outside. Physical therapy often works on the system around the knee: hips, quadriceps, glutes, calves, balance, gait mechanics, and confidence.
That matters because stairs are a team sport. If the hip is weak, the knee may take the blame. If balance is poor, the brace may become a psychological life raft. If the ankle is stiff, the knee may get extra stress. The knee is not always the villain. Sometimes it is just the employee who keeps getting assigned too much work.
Use this simple self-check before a flare-up day. No data is stored.
Enter your numbers, then calculate.
Neutral action: Use the result to reduce stair trips, not to override medical restrictions.
When to Seek Help: The Stair Problem That Should Not Wait
Get Urgent Care After a Major Injury or Sudden Change
Some knee symptoms deserve prompt medical care, not a better stair strategy. Get urgent help after major injury or sudden change if there is deformity, sudden swelling, intense pain, inability to bear weight, or a pop at the time of injury. When the question is where to go, not how to cope at home, comparing urgent care vs. an orthopedic clinic can make the next step less foggy.
Also take fever, redness, warmth, or new calf swelling seriously. These can point to problems that should not be treated as ordinary soreness.
Call the Clinician if the Knee Keeps Buckling
Repeated buckling, giving way, locking, worsening instability, or increasing reliance on the brace can mean the plan needs adjustment.
That does not mean you did something wrong. Recovery plans are not carved into stone tablets. They are more like recipes written by a careful cook who still expects you to report when the oven is smoking.
Ask for PT if Stairs Become the Daily Barrier
If stairs are the main reason you avoid normal life, ask whether physical therapy could help. PT can address stair mechanics, brace use, strength, balance, gait, swelling management, and confidence. If you have already tried sessions and feel stuck, it may help to read what to consider when physical therapy is not helping orthopedic pain.
For many people, the useful question is not “Do I need more willpower?” It is “What part of the movement system is failing first?” That question is much kinder. It is also more fixable.
Caregiver Lens: Safer Help Without Turning Into the Stair Police
Ask Better Than “Does It Hurt?”
Caregivers often ask, “Does it hurt?” That is loving, but it can be too broad. Better questions make the invisible visible.
- Did the knee buckle today?
- Was going up or going down worse?
- Did you avoid stairs because of pain?
- Did the brace slide or pinch?
- Did you carry anything on the stairs?
These questions help without turning every conversation into a medical deposition over dinner.
Watch the Descent
Going downstairs often feels riskier because the knee must control body weight while bending. Descent can reveal weakness, fear, brace slippage, or pain that climbing did not expose.
If you are nearby, do not hover dramatically. Hovering can make people feel studied, which is not the same as supported. Stay close enough to help, keep the path clear, and let the person move at a sane pace.
Keep Dignity in the Room
The goal is independence with fewer risks, not control dressed up as concern.
Try language that preserves agency: “Let’s make this easier,” not “You can’t do that.” “Want me to carry the basket?” not “You’re going to fall.” The second version may be true in your anxious imagination, but it lands like a cymbal crash in a small kitchen.
- Bring the brace to the appointment.
- Write down when stairs hurt most.
- Note whether the brace slips, pinches, or feels unstable.
Apply in 60 seconds: Write one sentence today: “My knee feels worst on stairs when ______.”
💡 Read official fall prevention guidance
FAQ
Can I go up and down stairs with a hinged knee brace?
Some people can use stairs with a hinged knee brace, but it depends on the injury, diagnosis, brace type, hinge setting, pain level, strength, balance, and clinician instructions. A brace does not make stairs automatically safe. Use the handrail, move slowly, keep your hands free, and stop if pain, swelling, buckling, or instability increases.
Should my hinged knee brace be locked or unlocked on stairs?
That depends on the prescribed brace settings and the reason you are wearing it. Do not change hinge settings without guidance from your clinician, surgeon, or physical therapist. A locked brace may be required in some recovery plans and inappropriate in others. This is exactly the kind of detail that should come from the person managing your care.
Why does my knee hurt more going downstairs?
Going downstairs often asks the knee to control body weight while bending. That can stress painful joints, healing tissue, irritated cartilage, weak muscles, or unstable ligaments. Descent also requires balance and confidence. If downstairs pain is new, worsening, or linked to buckling, ask a clinician or physical therapist for guidance.
What should I do if the brace slips while I am on the stairs?
Stop safely, hold the rail, and move to a stable landing if possible. Readjust only according to the instructions you were given. Do not keep walking on stairs with a shifted brace. If the brace repeatedly slips, pinches, causes numbness, or will not stay positioned, schedule a fit check.
Is a hinged knee brace better than a sleeve for stairs?
A hinged knee brace may provide more structural support than a simple compression sleeve, especially when instability is part of the problem. But “better” depends on the diagnosis, activity, fit, comfort, and treatment plan. A sleeve may be enough for some mild symptoms, while a hinged brace may be used for specific instability or recovery needs. Ask a qualified clinician which brace matches your knee and your stairs.
Can a hinged knee brace prevent falls?
A hinged knee brace may help some people feel more supported, but it cannot prevent falls by itself. Fall risk also depends on footwear, lighting, railings, balance, strength, medications, vision, home hazards, fatigue, and whether the knee buckles. Treat the brace as one layer of protection, not the whole safety plan.
When should I stop using stairs temporarily?
Consider avoiding stairs until you get medical advice if pain spikes sharply, swelling increases, the knee buckles, the brace will not stay in place, you feel unsafe, or you cannot bear weight as instructed. Also pause after a fall, twist, sudden pop, or sudden swelling.
Should older adults use extra caution with knee braces on stairs?
Yes. Older adults should be especially cautious because falls can threaten independence and recovery. Medication side effects, vision changes, balance issues, weaker muscles, nighttime bathroom trips, and home hazards can all raise risk. A brace may help the knee, but the stair environment still needs attention.
Next Step: Do One Stair-Safety Rehearsal Today
The 60-Second Brace-and-Stair Check
The curiosity loop from the first step is simple: the question is not “Can I conquer the stairs?” The better question is “Can I remove enough risk that this stair trip becomes boring?” Boring is the goal. Boring gets you upstairs with fewer negotiations from the knee.
Before the next stair trip, check 4 things:
- Brace position: Is it where your provider said it should be?
- Shoe grip: Are you wearing secure footwear instead of slick socks?
- Rail access: Can one hand stay on the rail?
- Carrying load: Are your hands free?
Write Down the One Step That Feels Worst
Do not try to document your entire life. Just write down the worst stair moment.
For example: “Going down hurts more than going up.” “The knee feels unstable at the landing.” “The brace slips after sitting.” “Pain spikes after the third step.” That small note can save 10 minutes of vague explanation at an appointment. If the appointment is partly about whether more testing is needed, you may also want to organize your symptoms before asking for an MRI for orthopedic pain.
Bring That Note to the Clinician or PT
A clinician or physical therapist can do more with a specific pattern than a general complaint. “Stairs hurt” is a fog bank. “The knee buckles going down after the brace slides” is a lighthouse.
Within the next 15 minutes, do one calm stair-safety rehearsal when you are not rushed. Empty hands. Good shoes. Rail available. Brace checked. One slow trip. Then write down what happened. That is not overthinking. That is orthopedic pain management with a hinged knee brace for stairs in its most practical form: less guesswork, fewer pain spikes, and a knee that does not have to improvise on the landing.
Last reviewed: 2026-04.
