
Decoding the Medical Billing Fog: From Estimates to Clarity
A clinic tells you the self-pay cash price is “$150 to $600,” and suddenly the number feels less like an estimate and more like weather with bad manners. That range is frustrating, but it usually is not random. It is the visible edge of a billing system shaped by visit complexity, likely CPT codes, site of service, and the very real possibility of labs, imaging, or a second bill arriving later.
For uninsured patients, high-deductible plan holders, and anyone comparing urgent care, primary care, or hospital outpatient options, the hardest part is not the price itself. It is not knowing which version of the price you are hearing. Visit-only? Self-pay discount? A bundled rate? Something that quietly excludes the radiology read?
“Keep guessing, and you risk the two-bill surprise, the wrong care setting, or a budget decision made in a fog.”
This guide helps you decode why clinics quote ranges, ask for a tighter good-faith estimate, and budget for the realistic worst case without spiraling. It also shows when price-shopping is smart, and when safety should win the argument immediately.
Because in medical billing, clarity is rarely handed to you. You have to ask for it. And a few precise questions can shrink the fog fast.
Table of Contents

Who this is for / not for
Who this is for
- You’re uninsured, between jobs, or your plan has a high deductible.
- You’re out-of-network and comparing cash pay vs using insurance.
- You want to know why “$150–$600” isn’t a con, but a math problem.
Who this is not for
- If you have chest pain, signs of stroke (face droop, arm weakness, speech trouble), trouble breathing, severe bleeding, severe allergic reaction, or suicidal thoughts, do not price-shop. Seek emergency care.
- If you need a guaranteed final price without codes or clinical details, many settings can’t do that honestly. You can still get a much tighter estimate, but “guaranteed” is rare.
A quick personal note: I’ve watched smart, budget-savvy people freeze at the word “range” and then make the worst possible move, which is doing nothing. The goal is not perfect certainty. The goal is bounded uncertainty so you can act.
- Ranges widen when tests, imaging, or procedures might be needed.
- They tighten when you ask what’s included and request likely codes.
- Safety comes first when symptoms are urgent.
Apply in 60 seconds: Write down your top symptom, how long it’s been happening, and whether you’re a new patient. Those three details shrink the range fast.
Range logic, decoded: the 5 switches that flip the price
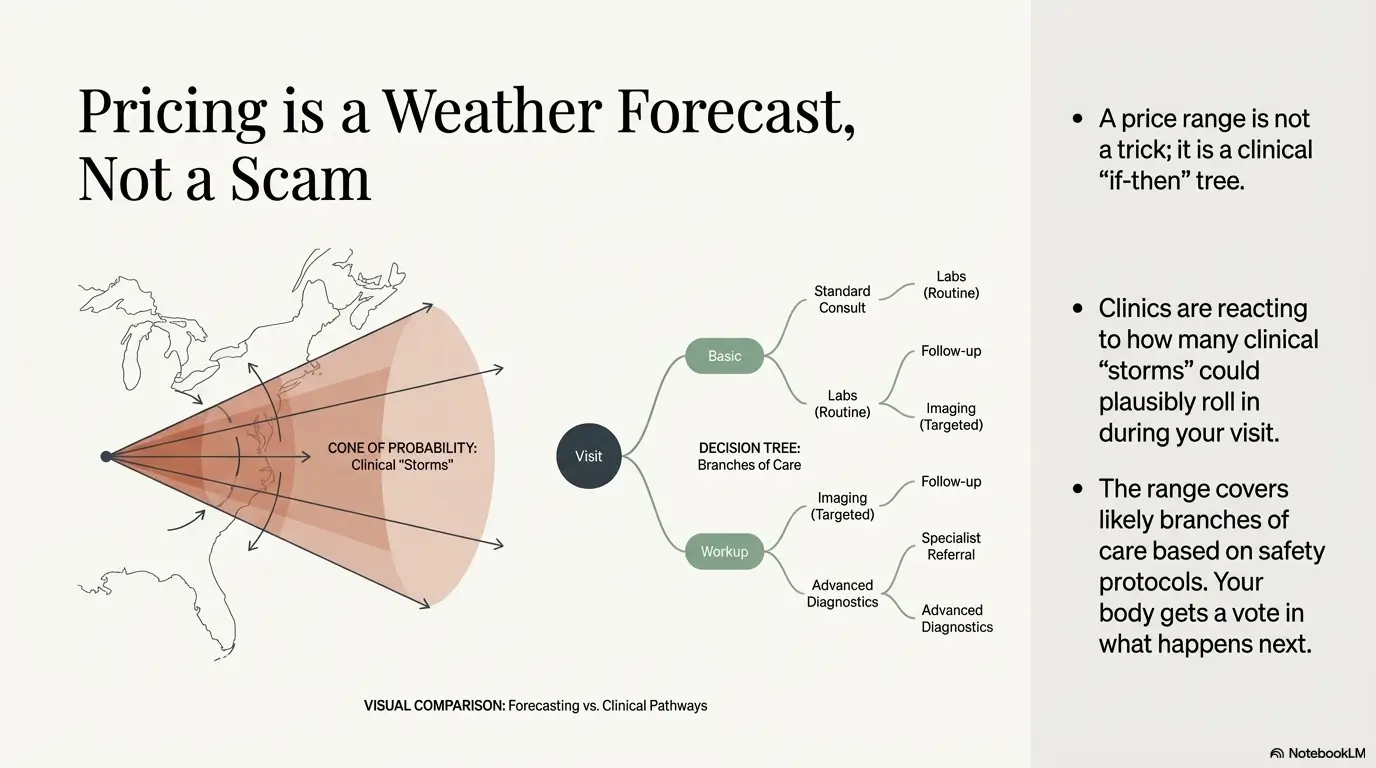
Think of a clinic quote like a weather forecast. They’re not dodging. They’re reacting to how many storms could plausibly roll in. Below are the five most common switches that change your total.
Switch 1: “Visit only” vs “visit + workup”
A basic visit is one thing. A visit that turns into a workup is another. A sore throat that stays a sore throat is usually cheaper than a sore throat with “let’s rule out pneumonia” energy.
- Visit only: evaluation, exam, plan, maybe a prescription.
- Visit + workup: labs, imaging, EKG, breathing treatment, stitches, splinting, injections, rapid tests.
Anecdote: I once went in for what I called “a quick look” at a rash. The clinician did the right thing and asked a few extra questions. Suddenly we were talking about an allergy trigger, a medication change, and a second follow-up. My wallet learned a new vocabulary word: “complexity.”
Switch 2: New patient vs established patient
New patient visits often cost more because the clinician must document a fuller history, reconcile meds, and build a baseline. Established patients sometimes move faster because the chart already knows your story.
Switch 3: Complexity, not vibes
Billing is tied to documented complexity, not how dramatic you feel (or how stoic you pretend to be). Multiple problems, chronic disease management, medication decisions, and higher-risk symptoms often push the level up.
Switch 4: Time is a billable ingredient (sometimes)
Some services can be billed based on time thresholds when documentation supports it. That’s why a “same complaint” visit can cost more if it took longer due to counseling, care coordination, or complicated decision-making.
Switch 5: Who owns the building matters
An independent clinic and a hospital-owned outpatient department can price the same type of visit very differently. Hospital systems may have additional billing structures, and some settings can add facility-related charges. You’re not imagining it when the same visit feels pricier in a hospital-branded clinic, especially if you’ve already seen how a hospital outpatient facility fee can change the final total.
Show me the nerdy details
In many outpatient settings, “visit levels” are influenced by documentation of medical decision-making (problem complexity, data reviewed, and risk) and sometimes by time when allowed. Separate codes can apply for tests, procedures, and supplies. The range exists because a clinic can’t know, before you’re evaluated, which branch you’ll land on.
- If no tests are needed, you stay near the floor.
- If safety requires tests, you climb the ladder.
- Ownership and setting can change the baseline.
Apply in 60 seconds: Ask: “Is that range for the visit only, or visit plus common tests?”
- Tier 1: Visit only (evaluation + plan). Next step: Ask for the self-pay visit code range.
- Tier 2: Visit + 1 quick test (rapid strep, urine dip, pregnancy test). Next step: Ask which rapid tests are likely.
- Tier 3: Visit + labs (bloodwork) or EKG. Next step: Ask if lab billing is separate.
- Tier 4: Visit + imaging (X-ray, ultrasound). Next step: Ask who reads the imaging and if you’ll get two bills.
- Tier 5: Visit + procedure (stitches, splinting, breathing treatment). Next step: Ask for procedure and supply estimates.
Neutral action: Identify which tier best matches your situation, then request an estimate for that tier.
Here’s what no one tells you: “cash price” isn’t one number
“Cash price” sounds like a single sticker on a single item. But in healthcare, it can mean three very different things. If you don’t clarify which one you’re being offered, surprises breed in the dark like mushrooms.
Cash price can mean three different things
- Prompt-pay discount: Pay today, get a lower rate.
- Self-pay rate: A standard rate for people not billing insurance.
- Package/bundled price: One price including specific items (common for certain tests, imaging bundles, or membership-style clinics).
Pattern-interrupt micro H3: Let’s be honest…
Most people ask, “What’s your cash price?” when what they really need is: “What does that price include?” Those are not the same question. One gets you a number. The other gets you a plan.
Anecdote: A friend paid cash at an urgent care and felt victorious. Then the radiology read arrived later from a separate group. The victory balloon made a sad squeak and deflated. Nobody lied. We just asked the wrong question.
Show me the nerdy details
Many services are billed using standardized code sets (CPT codes maintained by the American Medical Association, and HCPCS codes maintained by CMS). “Cash price” is a policy label, not a code. Different policies can attach to the same underlying set of billable items, which is why definitions matter.
The hidden add-ons: labs, imaging, supplies, and “separate bills”
This is where ranges get their wings. The visit itself might be one line item. But the universe loves sequels: labs, imaging, supplies, and interpretation fees can arrive later like plot twists you didn’t consent to.
Lab and imaging are often billed separately
A clinic can order a test, but a separate lab company may perform it and bill you. Same for imaging. The scan can happen in one place, while a radiology group reads it and bills separately. If your visit could lead to imaging, it helps to understand the cost gap in lumbar MRI costs on a high-deductible plan before you assume the clinic quote covers the whole story.
Supplies and procedures are the usual range-expanders
- Wound care and stitches
- Breathing treatments
- Joint injections
- Splints, crutches, braces
Read fees: the “someone has to interpret it” line item
Even if the image is taken on-site, a professional interpretation component can be billed. That’s one reason “X-ray included” can still turn into “X-ray plus interpretation.”
Anecdote: I once asked, “Is the X-ray included?” and felt proud of myself. Later I learned the correct question was, “Is the read included?” My pride became educational material.
- Ask who performs the test (clinic vs outside lab).
- Ask who interprets the test (radiology group, cardiology read, pathology).
- Ask if supplies are included or itemized.
Apply in 60 seconds: Say: “Before I come in, can you tell me which parts might be billed by someone else?”
Site-of-service traps: how the same visit becomes pricier
Same symptom, different front door, different universe of pricing. Site of service is a polite phrase for “where you walk in determines which billing rules wake up.”
Clinic vs ER vs hospital outpatient
- Independent clinic: Often the simplest pricing structure.
- Urgent care: Can be transparent, but add-ons can stack fast.
- ER: Designed for emergencies, staffed and equipped accordingly, usually the highest cost structure.
- Hospital outpatient department: Sometimes includes additional facility-related charges and higher baselines.
Hospital-owned clinic pricing quirks
A hospital-owned clinic can look like a normal clinic and feel like a normal clinic and still bill like a hospital setting. That’s why “same doctor, same complaint” can cost more under a different corporate umbrella. If you want a deeper rabbit hole on this, compare how hospital outpatient vs ASC facility fees can reshape what looks like the same visit on paper.
After-hours and urgent scheduling effects
After-hours care can require different staffing and resources. Even when the visit code is similar, the likelihood of add-ons can change when you come in at 9:30 p.m. versus 9:30 a.m.
Anecdote: I once did the classic “I’ll just go after work.” The clinic was busy, the provider moved fast, and the decision was reasonable: a quick test to rule out something risky. The price didn’t punish me for after-hours. It punished me for needing certainty.
Show me the nerdy details
“Facility fee” conversations often trace back to how a site is categorized for billing purposes. Not all places charge these, and terminology varies. If you want clean budgeting, ask directly whether the estimate includes any facility-related fees and whether bills will come from multiple entities.
- Choose a primary care clinic if symptoms are stable, you can wait 24 to 72 hours, and you want the tightest estimate. Trade-off: slower access.
- Choose urgent care if you need same-day care but are not in danger signs territory. Trade-off: add-ons can widen the range.
- Choose the ER if there are red flags (chest pain, stroke symptoms, severe breathing trouble, fainting, uncontrolled bleeding). Trade-off: highest cost, but the right level of safety.
Neutral action: Pick the safest setting first, then ask for an estimate for that setting.
Common mistakes that inflate your cash price
If you want to keep your cost on the low end of the range, you don’t need secret hacks. You need to avoid the predictable mistakes that turn a reasonable visit into an expensive fog machine.
Mistake 1: Asking for “the price” instead of “the codes”
Without likely CPT/HCPCS codes (and sometimes diagnosis codes), you’re not buying clarity. You’re buying the concept of clarity. Codes aren’t magic, but they anchor estimates to something real. That becomes even more obvious once you see how a spine injection bill breaks down by CPT codes instead of vibes, guesses, and crossed fingers.
Mistake 2: Not clarifying “estimate includes what?”
Visit-only versus all-in. Labs, imaging, supplies, follow-up. If you don’t define the basket, you can’t compare baskets.
Mistake 3: Forgetting the “two-bill problem”
One bill from the clinic, another from the lab/radiology/pathology group. This is the most common “I thought I asked the right question” moment.
Mistake 4: Paying before you ask about discounts
Many places offer prompt-pay discounts, payment plans, or income-based assistance. You don’t need to negotiate like you’re buying a used car. You just need to ask what policies exist.
Anecdote: I once paid quickly because I wanted the problem gone. Later I learned there was a same-day discount. The money wasn’t huge, but the lesson was: don’t let anxiety swipe your card.
- Ask what the estimate includes.
- Ask whether you’ll get separate bills.
- Ask what discounts apply and when.
Apply in 60 seconds: Say: “Can you give me an all-in estimate for a typical visit for my symptoms, including common add-ons?”
Don’t do this: 7 phrases that create expensive confusion
These phrases sound harmless. They are not. They invite misunderstanding, and misunderstanding is how ranges become regrets.
“I just need a quick check”
“Quick” can become complex if your symptoms warrant a workup. It’s better to describe the symptom and ask what a typical evaluation includes.
“No tests, please”
Providers may still recommend essentials for safety. A better approach is to ask, “Which tests are essential versus optional, and what do they cost?”
“Can you quote the whole thing over the phone?”
Sometimes they can, but only if you define assumptions. Ask for a written estimate with line-item assumptions instead of a single phone number.
“I don’t want any separate bills”
I get the impulse. But the system doesn’t always comply. The smarter move is to ask who the separate billers are so you can plan.
“My friend paid $X”
Your friend is not your chart. Their setting, provider, documentation, and add-ons might be different.
“I’ll pay cash, so it’ll be cheaper, right?”
Sometimes yes, sometimes no. Cash can reduce administrative steps, but it doesn’t erase the cost of tests or procedures.
Pattern-interrupt micro H3: Here’s the awkward part…
If your symptoms change mid-visit, the plan changes, and the price follows. The goal isn’t a cheap visit. It’s the right visit at a price you understand.
- Are you a new or established patient?
- Your top symptom and duration (example: “sore throat for 3 days”).
- Any red flags (fever, shortness of breath, injury mechanism).
- What you think you might need (strep test, X-ray, refill, stitches).
- Whether you can do telehealth or need in-person.
Neutral action: Read this list verbatim to the scheduler and ask for an estimate based on it.
The estimate script: how to get a real number (not a shrug)
This is the part you can copy, paste, and use. You’re not asking staff to predict the future. You’re asking them to define assumptions and give you the most honest forecast they can.
Step 1: Ask for the “self-pay good-faith estimate”
If you are uninsured or self-pay, you can request a written good-faith estimate in many situations. Even when a formal estimate isn’t available, asking for an “estimate in writing with assumptions” usually improves clarity fast.
Step 2: Ask for likely CPT codes (and alternatives)
Try this sentence: “If it’s minor versus moderate complexity, what codes are typical?” You’re not demanding a guarantee. You’re asking for common patterns.
Step 3: Confirm separate billing partners
Ask: “Which lab do you use?” “Who reads X-rays?” “Will I get separate bills from radiology, pathology, or a lab company?”
Step 4: Ask about discounts and payment policies
- Prompt-pay discount
- Self-pay discount policy
- Sliding scale or financial assistance (if applicable)
- Payment plan options
- Refunds if you overpay
Step 5: Get it in writing
Email, portal message, or a printed estimate beats memory. Memory is a notorious liar when you’re stressed.
Anecdote: I once walked into a visit armed only with a phone note that said “around $200.” Later, the staff kindly explained that “around” is not a legal unit of currency. Now I ask for a message in the portal. It’s not confrontational. It’s clean.
Input 1: Low-end visit quote (example: $150)
Input 2: High-end visit quote (example: $600)
Input 3: Expected add-ons count (0, 1, or 2)
Rule of thumb output: Budget the high end, then add a cushion for add-ons.
If add-ons count is 0, budget near the high end.
If 1, add a cushion you can tolerate (example: +25% of the high end).
If 2, add a larger cushion (example: +50% of the high end).
Neutral action: Pick a cushion you can actually pay, then ask what would trigger add-on #1 and #2.
Show me the nerdy details
Estimates tighten when the clinic can anchor to likely code families: an evaluation and management (E/M) service plus specific test/procedure codes. Staff may not know exact codes until documentation is complete, but they can often share typical patterns for common complaints.
Why your friend paid less: pricing variability that’s real
Healthcare pricing is not a single clean ladder. It’s more like a staircase where different buildings use different staircases. Here’s what legitimately drives variation between patients and visits.
Patient factors
- New vs established patient
- Medical history complexity
- Medication list and interactions to consider
- Risk level of the symptom (what must be ruled out)
Provider and documentation factors
Two clinicians can take different approaches, order different tests, and document different risk considerations. Sometimes the “more expensive” route is simply the safer route for your situation.
Operational factors
- In-house lab vs send-out lab
- Imaging availability on-site
- Staffing and protocols
Contracting factors (even for cash)
Some clinics set self-pay rates that mirror typical allowed amounts, while others use internal cash schedules. Even “cash” can be policy-driven, not universal.
Anecdote: I once compared two urgent cares five miles apart. The first bundled a rapid test into a package. The second itemized everything like a restaurant receipt where every olive gets its own line. Same city, same symptom, different philosophy. That wider pattern is one reason many families underestimate the real costs of chronic back pain over time, even before major procedures enter the picture.
- Different sites price differently.
- Different clinicians choose different workups.
- Different billing partners can create separate invoices.
Apply in 60 seconds: When comparing clinics, compare the same tier: visit-only vs visit-plus-workup, not apples vs meteorites.
When to seek help now (not shop prices)
Price shopping is smart. But there’s a line where shopping turns into delay, and delay turns into danger. If you’re on that line, step back and choose safety.
Go to urgent/emergency care if you have
- Chest pain, pressure, or new severe chest discomfort
- Severe shortness of breath, blue lips, or trouble speaking full sentences
- Signs of stroke: face droop, arm weakness, speech difficulty
- Fainting or near-fainting with concerning symptoms
- Uncontrolled bleeding, major injury, or severe burns
- Severe allergic reaction (swelling, wheezing, trouble breathing)
- Suicidal thoughts or self-harm risk
Don’t delay safety-critical evaluation for price certainty
A “cheaper” visit that happens too late can become the most expensive kind of care. If you’re unsure, err toward being seen, then deal with billing with a calmer brain. That is especially true when symptoms drift into territory that looks less like routine low-back pain and more like a low back pain emergency.
Anecdote: I’ve seen people try to out-stubborn a symptom because they didn’t want to spend money on “maybe.” The body rarely rewards that strategy. If you’re scared, it’s okay to say, “I’m scared.” Just don’t let fear make the decision silently.
FAQ
Why do clinics give a range instead of one cash price?
Because they can’t know in advance whether you’ll need tests, imaging, procedures, or extra time. The range covers likely branches of care based on common patterns and safety protocols.
What’s the difference between “self-pay” and “cash-pay” pricing?
Clinics use these terms differently, but often “self-pay” means not billing insurance, while “cash-pay” sometimes implies a prompt-pay discount or a specific bundled package. Always ask what’s included.
Can I negotiate a self-pay price at an urgent care?
You can often ask about discounts, prompt-pay policies, payment plans, or financial assistance. Negotiation varies by clinic policy. The most effective approach is requesting a written estimate with assumptions and asking about available self-pay discounts.
Will I get separate bills for labs or X-rays?
Possibly. A lab company or radiology group may bill you even if the clinic orders the test. Ask directly: who performs the test and who interprets it.
What should I ask for to get an accurate estimate?
Ask what the estimate includes, likely CPT/HCPCS codes for common scenarios (minor vs moderate complexity), whether there are separate billing partners, and whether discounts apply for prompt payment.
Does “hospital-owned” clinic mean higher charges?
Sometimes. Hospital-owned outpatient settings can have different billing structures and may include facility-related charges. It’s not guaranteed, but it’s a real possibility worth asking about upfront.
If I pay cash, can I still submit to insurance later?
Sometimes you can request an itemized receipt and submit a claim yourself, but policies and plan rules vary. If you want that option, ask the clinic for the documentation you’ll need before you pay.
Are telehealth self-pay visits usually cheaper?
Often, yes, especially for straightforward issues that do not require an exam, labs, or imaging. But if telehealth leads to an in-person visit anyway, you may end up paying for two steps.
What is a “facility fee” and will I be charged one?
A facility fee is an additional charge that can appear in some hospital outpatient settings. Not every site charges it. If you’re self-pay, ask: “Does your estimate include any facility-related fees, and will I receive more than one bill?”
Can a clinic change the price after the visit?
Yes, if the services provided change. If additional tests, procedures, or complexity occurs, the final bill can be higher than the initial “visit-only” expectation. That’s why written estimates should include assumptions.

Next step
Use the “3-Ask” checklist before you book
- “What does the estimate include?” (visit-only vs all-in)
- “What CPT codes are likely?” (and common add-ons)
- “Will I receive separate bills?” (lab/radiology/pathology)
- Tests might be needed
- Imaging is possible
- Procedures/supplies are likely
- Separate billers are involved
- Site of service is hospital-owned
- You define visit-only vs all-in
- You ask for likely codes
- You confirm separate bills
- You request a written estimate
- You ask about discounts early
- Pick the safest setting
- Use the 3-Ask checklist
- Budget the high end plus cushion
Conclusion
So, why do clinics quote ranges? Because they’re forecasting a visit that hasn’t happened yet, and your body gets a vote in what happens next. The curiosity loop from the beginning closes here: the range is the clinic admitting uncertainty honestly. Your job is to turn that uncertainty into a plan by defining what’s included, anchoring to likely codes, and eliminating the “separate bill” ambush.
If you do one thing in the next 15 minutes, do this: copy the “3-Ask” checklist into your notes app (or on paper), call the clinic, and request an estimate in writing based on your symptom and whether you’re a new patient. You don’t need perfect certainty to move. You just need a boundary you can live inside. And if your future care path includes imaging, injections, or escalating spine treatment, it helps to understand what happens when failed conservative care leads to an MRI request or when a procedure becomes a self-pay question like self-pay TFESI cost.
Last reviewed: 2026-03-06
