
The Hidden Cost of the “Gap”
An out-of-network spine surgeon can look like the answer, right up until the paperwork starts speaking in half-promises. A gap exception request often arrives dressed as reassurance, but the real story lives in the fine print.
That is where families get stuck. Not at the point of diagnosis, but in the quieter, stranger moment when a scheduler sounds confident, the insurer sounds conditional, and no one is answering the one question that matters most: What financial risk is still alive here?
A gap exception is usually a request for your insurer to treat an out-of-network provider as if they were in-network because no suitable in-network option is reasonably available.
This guide helps you read a gap exception request the way billing departments eventually will: line by line, scope by scope. We focus on the actual weak points that break first—surgeon, facility, anesthesia, and follow-up care—because they do not always move together.
Start here. Because the dangerous part is rarely the first page. It is the blank space after it.
Table of Contents
Fast Answer
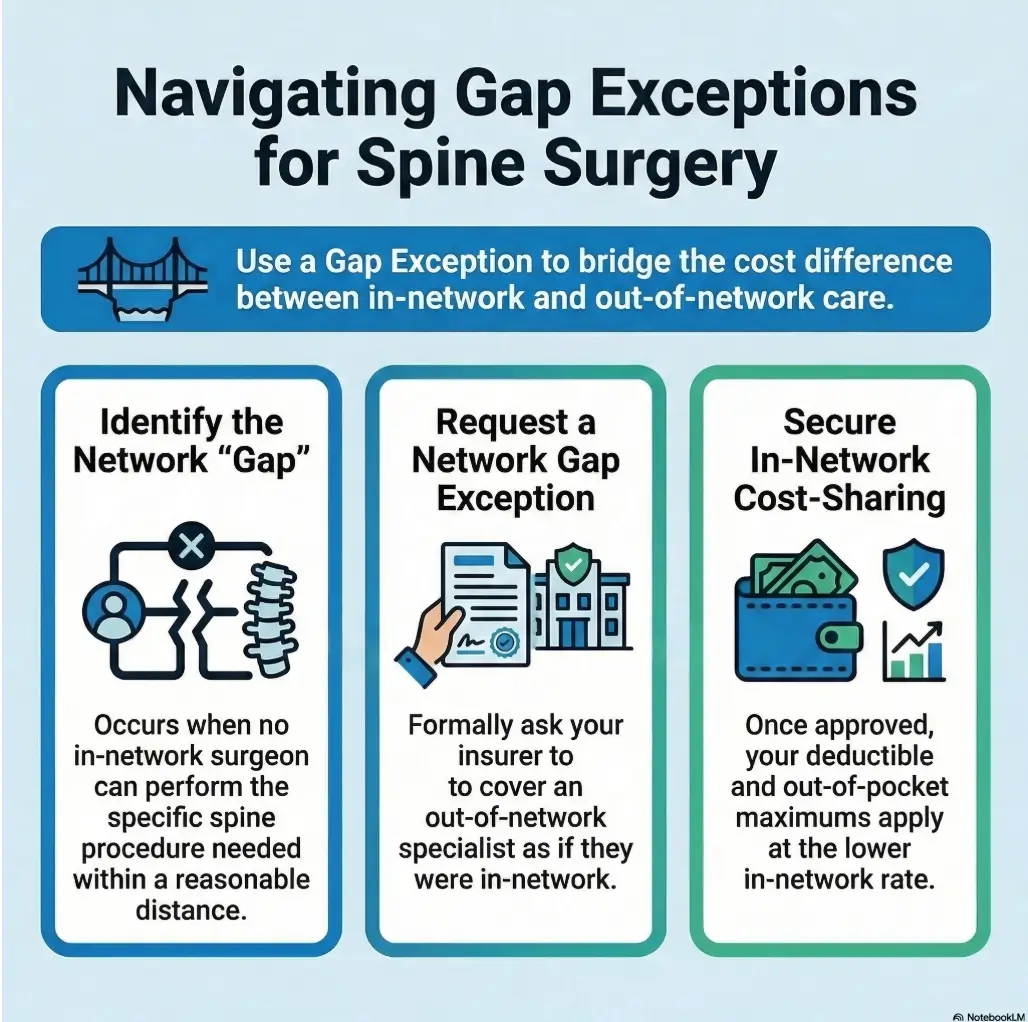
A gap exception request is usually a health plan document asking the insurer to treat an out-of-network spine surgeon as if they were in network because no suitable in-network option is reasonably available. The safest way to read it is to look for five things first: medical reason, network insufficiency, distance or wait-time problem, service requested, and whether the exception applies to both the surgeon and facility.
- Look for who is covered, not just whether “the case” is covered
- Separate authorization from cost-sharing level
- Treat vague wording as unfinished business, not reassurance
Apply in 60 seconds: Circle every noun tied to coverage: surgeon, facility, anesthesia, assistant, imaging, and follow-up.
Safety / Disclaimer
This guide is informational only and not legal, medical, or insurance advice. Coverage decisions, appeal rights, and surprise-billing protections depend on your plan type, state rules, employer arrangement, and the exact wording in your documents. Before surgery or a major deposit, confirm everything in writing with your insurer and provider.
One important guardrail matters here. Healthcare.gov explains that preauthorization is not a promise that your health plan will pay, which is exactly why families can feel “approved” and still get financially blindsided later. CMS also explains that federal surprise-billing protections exist in certain situations, but those protections do not magically convert every out-of-network spine surgery arrangement into a simple in-network transaction. For a more focused breakdown of how these charges can unfold around procedures, see surprise bills for spine procedures.
Who this is for / not for
This is for
Patients who were told their spine surgeon is out of network, but the needed expertise may not exist nearby in network. It is also for caregivers trying to decode preauthorization, single-case agreement, or gap exception language while the calendar starts breathing down their neck.
It is especially useful for families comparing whether to appeal, escalate, or slow down scheduling until paperwork becomes concrete. In my experience, the most dangerous moment is not outright denial. It is the soft-focus maybe. That polite haze where everyone sounds helpful and nobody is quite saying who pays for what.
This is not for
This is not medical advice about whether surgery is the right treatment. It is not a substitute for a surgeon’s clinical judgment, and it will not tell you whether a particular spinal procedure is appropriate.
It is also not mainly for cases where the surgeon is already confirmed in network and the only question is whether your deductible is painfully high. Painful deductibles are real, but that is a different beast. This guide is about document reading when network status, approval scope, and financial liability are still wobbling around the room like folding chairs after a rushed banquet.
Start with the real question: what is a gap exception actually trying to prove?
It is not just “I prefer this surgeon”
A gap exception usually argues that the plan’s network cannot provide the needed service within reasonable standards of access, timing, specialty, or clinical suitability. Read that sentence slowly, because it changes the whole posture of the document. This is not a love letter to your preferred doctor. It is a failure report about the network.
That matters because families often approach the request as a permission slip. The insurer often reads it as a challenge: prove that our network is insufficient in a way that matters. Those are two different songs, played in different keys.
It is really a network-failure document
The quiet engine inside the request is often this: the insurer says in-network care exists, while the patient or provider is trying to show that, in practical terms, it does not. The proof might be lack of a subspecialist, lack of timely appointments, lack of revision experience, or a facility-access problem that turns “available” into something merely theoretical.
I once saw a family cling to the phrase “in-network options identified” as if it settled the issue. Then they read the details. The listed specialists were hours away, booked far out, and not obviously a match for the requested surgery type. On paper, the network looked sturdy. In life, it looked like cardboard in rain.
Let’s be honest…
Many people read the form as if it were a yes-or-no gate. It is closer to an argument packet. Every sentence is trying to prove necessity, not convenience. And every missing detail gives someone, somewhere, room to reinterpret the whole thing after the surgery has already happened.
Show me the nerdy details
In practical insurance workflow terms, a gap exception request often sits adjacent to prior authorization, network adequacy, provider contracting, and claims adjudication. Those systems do not always talk to each other cleanly. A medically approved case can still produce out-of-network claim handling if the exception scope is narrow or poorly loaded into the plan’s systems.
- Preference is weak evidence
- Access failure is stronger evidence
- Clinical mismatch can matter as much as distance
Apply in 60 seconds: Write one sentence that starts with “In-network care is not reasonably available because…” and test whether your paperwork truly supports it.

Read these five lines first: the phrases that decide everything
Medical necessity language
Look for wording that explains why the service, procedure, or surgeon specialty is clinically needed, not merely desired. The best language is specific enough to be meaningful and restrained enough to sound credible. “Complex revision deformity case requiring procedure-specific expertise” lands very differently than “patient wants a highly regarded surgeon.”
Network inadequacy language
Watch for phrases such as no available specialist, no qualified provider, excessive travel distance, unreasonable appointment delay, or lack of procedure-specific expertise. These are the bones of the request. If they are missing, the letter may be dressed like a gap exception while functioning more like a hope note.
Scope-of-exception language
Check whether the request applies only to the surgeon, or also to the assistant surgeon, anesthesia, facility, imaging, and follow-up care. Families miss this constantly. Understandably. The surgeon is the star of the poster, so everyone forgets the supporting cast until the invoices arrive in separate envelopes with excellent posture.
Dates and episode-of-care limits
Some approvals cover only a narrow window, one surgery date, or a single treatment episode. That tiny date line can become a very expensive trap. If surgery moves because of lab work, illness, OR scheduling, or the surgeon’s calendar, expired approval language can turn a nearly solved problem back into a live grenade.
Reimbursement wording
The most important hidden distinction is whether the request says the care will be covered at in-network benefit level, or merely reviewed as an exception without clearly promising in-network cost sharing. Healthcare.gov states that preauthorization is not a promise your plan will cover the cost, which makes this wording far more than legal wallpaper. It is the hinge between hopeful planning and actual exposure.
Verbal reassurance only
Highest confusion risk
Prior authorization noted
Still not payment certainty
Gap exception approved for surgeon
Facility and ancillary risk remains
Written in-network benefit language
Much stronger, still verify scope
Written scope for surgeon + facility + ancillary services
Safest practical position
The hidden hinge: surgeon approval is not always facility approval
One approval can mask another denial
A gap exception for the spine surgeon does not automatically mean the hospital, ambulatory surgery center, neuro-monitoring team, or assistant providers are covered the same way. In real life, families often hear one glowing sentence from the surgeon’s office and assume the rest of the ecosystem came along for the ride. It often did not.
This is where a lot of bills learn to multiply. Not because someone lied in a cartoon-villain way, but because different participants bill separately, contract separately, and are processed separately. Insurance is full of nouns that look married and act single.
Facility status matters more than people expect
Even when the surgeon is the headline problem, facility network status can drive a large part of the final patient bill. That is one reason federal surprise-billing protections matter so much in some settings, especially for certain out-of-network bills tied to in-network facilities or emergency scenarios. CMS explains those protections, but whether and how they apply depends on the setting, the service, the notice-and-consent context, and the plan arrangement. Families comparing site-of-service exposure may also want to review how a hospital outpatient vs. ASC facility fee can change the financial picture.
Here’s what no one tells you…
Some families celebrate too early after hearing “the exception was approved,” only to discover later that the approval was narrower than the operation itself. Surgeon approved. Facility not clearly approved. Anesthesia unclear. Assistant surgeon not named. Imaging silent. Follow-up visits ambiguous. It is like being told the wedding venue is booked, then learning nobody actually reserved the chairs.
Mini decision card: If the document names only the surgeon, you likely need more written clarification before surgery. If it names the surgeon and facility but says nothing about anesthesia or assistant services, you still have real loose ends. If it clearly states in-network benefit handling for the relevant providers and dates, your footing is better. Neutral next step: make a written gap list of every participant in the surgery day.
Network proof matters: what evidence usually strengthens the request
Distance and travel burden
The document is stronger when it shows how far the nearest in-network option is, how hard the trip is, or why repeated travel is unrealistic. Distance alone is not always enough, but distance plus follow-up needs, mobility limits, caregiver logistics, or missed work starts to sound like the life people actually live.
I have watched families spend more time arguing about miles than about feasibility. The better question is not “Is the provider technically on a map?” It is “Can this course of care be carried out safely and reasonably from where the patient actually lives?”
Wait time and scheduling delay
A long delay for consultation or surgery can matter, especially when symptoms are worsening or the requested timing is clinically relevant. The strongest letters do not merely say “delay is bad.” They tie delay to symptoms, functional decline, or treatment planning reality.
Missing expertise, not just missing availability
The argument gets sharper when it explains why the needed subspecialty, revision experience, deformity background, or pediatric/adult-specific expertise is not reasonably available in network. This is a subtle but powerful move. “There is an orthopedic spine surgeon in network” is not the same sentence as “there is an in-network surgeon reasonably available for this exact case.” In some cases, that exact-case question also overlaps with procedure choice, such as whether a patient is being steered toward fusion when decompression without fusion may still be part of the conversation.
Failed in-network search
Requests often become more persuasive when they document actual calls, referrals, or denials from in-network providers rather than relying on general statements. In other words, show the dead ends. Paperwork loves receipts.
- Document calls, names, and dates
- Show clinical mismatch, not just inconvenience
- Connect delay to real care impact
Apply in 60 seconds: Build a 4-row log with provider name, date called, outcome, and why it was not a workable in-network option.
Show me the nerdy details
“Network adequacy” can mean different things across plan types and regulatory settings. For article purposes, the practical question is whether the record shows a real access failure for this patient and this service. Exact legal standards vary, but operationally the same evidence tends to help: unavailable specialists, excessive delay, travel burden, and lack of relevant expertise.
Words that sound safe but are slippery
“May be covered”
This usually signals uncertainty, not approval. It sounds comforting because the sentence wears a cardigan, but it is still uncertainty. If money is at stake, “may” should trigger more questions, not relief.
“Subject to medical review”
This means the insurer is still reserving room to deny, narrow, or reinterpret the request. Sometimes that is routine. Sometimes it means the file is still a weather system and you are standing in it without an umbrella.
“At plan allowance”
This can mean the insurer will pay something while leaving the patient exposed to a large balance. Families often read it as “great, covered.” It can instead mean “partially processed in a way that still hurts.”
“Single-case agreement”
This is related but not identical. A single-case agreement is often a negotiated payment arrangement with the out-of-network provider, while a gap exception is often an access-based coverage exception. Sometimes they overlap. Sometimes they pass each other in the hallway and do not make eye contact.
Eligibility checklist:
- Do you have written language saying the surgeon is handled at in-network benefit level? If no, keep digging.
- Does the document name the facility? If no, you still have a material gap.
- Are surgery dates or episode dates printed clearly? If no, timing risk remains.
- Are anesthesia or assistant services addressed anywhere? If no, flag them now.
Neutral next step: convert every soft phrase into a yes-or-no question for the insurer.
Don’t sign too fast: where patients accidentally accept the wrong financial terms
Out-of-network consent forms
Provider paperwork may contain broad financial responsibility language that survives even if you thought the insurer would process the case at in-network levels. CMS provides standard notice-and-consent materials tied to certain No Surprises situations, and the point is worth stating plainly: signing papers without understanding the billing consequences can change your protections in important ways.
That does not mean every consent form is a trap. It means every financial paragraph deserves slow eyes. The sentence that costs the most is rarely the loudest one.
Deposit requests before approval
Large advance payments can signal that coverage details are still foggy. That fog has a habit of turning into invoices. Sometimes deposits are standard workflow. Sometimes they are a bright little lighthouse telling you that the reimbursement structure is not yet settled. If the office is already discussing direct-pay numbers, it can help to compare that moment with a broader self-pay cash price range before assuming the deposit is routine.
Verbal reassurance without written confirmation
Phone calls are helpful, but the paper trail is the real floor beneath your feet. I once watched a family keep a spiral notebook full of call names, reference numbers, and dates. At the time it looked slightly intense. Later it looked like genius with handwriting.
Quote-prep list:
- Exact surgeon name and tax ID if available
- Facility name and network status
- Procedure description and CPT list if the office will provide it
- Expected surgery date and follow-up window
- Whether anesthesia, assistant surgeon, monitoring, imaging, pathology, and DME are separately billed
Neutral next step: ask for one written estimate or status note covering each of those items.
Common mistakes
Mistake 1: Reading only the first page
Important restrictions often live in later pages, attachment notes, or authorization remarks. Insurance documents have an almost literary love of burying the plot twist after the intermission.
Mistake 2: Assuming the surgeon’s office and insurer mean the same thing
Provider staff may use “approved” conversationally, while the insurer means “submitted,” “pending,” or “partially authorized.” Nobody is necessarily acting in bad faith. They are just using the same word for different stages of reality, which is how families end up emotionally checking out while the paperwork is still very much awake.
Mistake 3: Ignoring CPT codes or procedure descriptions
If the exception is tied to a narrow service description, related services may still fall outside the approval. Narrow wording can turn a broad hope into a skinny result. That is especially true when readers do not yet understand how separate procedural billing can work, which is one reason a primer on spine injection bill CPT codes is useful even outside the injection setting.
Mistake 4: Forgetting the anesthesia and assistant bill
The surgical spotlight is bright. Secondary professional bills arrive from the shadows. They are not side characters to your bank account.
Mistake 5: Missing the expiration date
An approval that expires before surgery can collapse at the exact moment you thought the path was clear. Healthcare.gov notes that plans must notify patients about internal appeal timelines in certain circumstances, including 15 days for prior authorization decisions for treatment requests and 72 hours for urgent care cases. Those process timelines are not the same as your scheduling timeline, but they do remind us that paperwork clocks matter.
- “Approved” may not mean what you think
- Narrow service wording can shrink coverage
- Dates matter as much as dollars
Apply in 60 seconds: Find the expiration date, covered service description, and named providers before you read anything else.
Don’t do this: expensive assumptions that break families later
Do not confuse access hardship with automatic approval
A hard travel burden helps, but it does not guarantee the plan will treat the surgeon as in network. Strong facts improve the case. They do not cast a spell.
Do not treat “authorized” as “fully paid”
Authorization addresses permission. Payment level, balance billing, and cost sharing are separate creatures. Healthcare.gov’s glossary says exactly what families need to remember in plain language: preauthorization is not a promise your plan will cover the cost. That sentence should practically be stitched onto a throw pillow for every medical billing office in the country.
Do not skip employer-plan escalation
For employer-sponsored coverage, HR or benefits teams can sometimes help surface plan details or escalation routes that front-line calls never reveal. They are not magicians, but sometimes they know which door is real when the hallway seems full of decorative ones. When work limitations are part of the case, some readers may also need cleaner documentation language, such as ADA accommodations for sciatica doctor note wording.
Mini calculator: If the office asks for a $5,000 deposit and the approval does not clearly state in-network benefit handling for surgeon and facility, your unresolved exposure is not “maybe small.” It is at least large enough to pause. If two major participants are still unclear, assume you have two separate billing risks until proven otherwise. Neutral next step: ask for written clarification before money moves.
Build a reader’s checklist: how to scan the document in under ten minutes
First pass: circle the scope
Identify who is covered, what service is covered, where it is covered, and for what dates. Think of this as building the cast list and the stage. If you cannot tell who is in the show, you do not yet know what the approval means.
Second pass: mark the condition
Find the sentence that explains why in-network care is inadequate. That is the engine of the request. If the letter never really says why the network failed, the document may be weaker than everyone is pretending.
Third pass: flag the money language
Highlight benefit level, allowed amount, coinsurance, deductible, and any note about balance billing. CMS says the No Surprises Act creates federal protections against certain surprise medical bills, but those protections are situation-specific. So you still need to know whether this exact arrangement is being processed as in-network cost sharing, out-of-network reimbursement, or something fuzzier. If your plan is a high-deductible plan and imaging or pre-op testing is part of the case, comparing an HDHP imaging cost estimate can add useful realism to the numbers.
Fourth pass: isolate open risks
Write down anything not clearly covered, especially facility, anesthesia, imaging, pathology, durable equipment, and post-op follow-up. A useful rule is simple: if it does not have a written status, it is not “probably fine.” It is unresolved.
Fee/rate table:
| Item | What to verify | Risk if missing |
|---|---|---|
| Surgeon | In-network benefit wording, dates, procedure scope | Out-of-network claim handling or narrower coverage |
| Facility | Named facility and network status | Large facility bill remains exposed |
| Anesthesia / assistant | Separate billing and coverage status | Unexpected professional bills |
| Follow-up care | Episode-of-care language or visit count | Post-op claims processed differently |
Neutral next step: turn this table into your own one-page summary before scheduling.
Short Story: The approval that sounded complete but wasn’t
A caregiver I once spoke with had a folder that looked reassuring from a distance. Surgeon letter, authorization note, printed portal screen, names of three phone reps, all clipped together with the optimism of office supplies. The scheduler said they were “good to go.” That phrase can do an astonishing amount of emotional damage.
When they slowed down and read the papers line by line, the surgeon had been addressed, but the surgery center was not clearly named, and anesthesia was nowhere on the page. A deposit request had also arrived, which they had nearly paid out of sheer fatigue. Instead, they made a four-column sheet: provider, facility, service, written status. Three blanks appeared immediately. Those blanks were not dramatic.
They were just honest. Within two days, the office confirmed one gap, the insurer clarified another, and the family delayed payment until the record caught up. It was not glamorous. It was adult life in fluorescent light. But it likely saved them from a very expensive misunderstanding. And when care does move forward, families often discover the paperwork story continues into recovery, which is why it helps to understand issues like post-op sciatica rebound before every strange symptom gets folded into billing panic.
When to seek help
Seek help quickly if surgery is close
If the procedure date is near and approval language is vague, get written clarification immediately from both insurer and provider billing. Time compresses judgment. That is true in airports, kitchen fires, and insurance paperwork.
Seek help if the plan language conflicts
When the provider says “covered” but the insurer’s wording is conditional or narrow, escalate before the procedure. Healthcare.gov explains internal appeals and external review rights for many health plans, including timing rules for denials. Those rights matter most when you act before the case becomes a pile of after-the-fact explanations.
Seek help if you are being asked for a large upfront payment
A large deposit can be a clue that the reimbursement structure is unsettled. It may not always signal danger, but it certainly signals homework.
Seek help if the case involves complex spine care
Revision surgery, deformity care, multi-level procedures, or rare expertise gaps often deserve extra review because the billing ecosystem is more layered. More layers mean more places for scope drift, network mismatch, and paperwork optimism. Some readers also benefit from grounding the clinical side of the decision in adjacent explainers, such as failed conservative care for MRI, when the insurer is still questioning why the pathway escalated at all.
Show me the nerdy details
Appeal and review pathways depend heavily on plan type. Marketplace, many employer plans, Medicare Advantage, Medicaid managed care, and state-regulated commercial products may follow different processes. For readers, the practical move is not to master every rule. It is to identify the governing plan, get the denial or conditional language in writing, and preserve your deadlines.

FAQ
What is a gap exception in health insurance for an out-of-network spine surgeon?
It is a request for the insurer to make an exception because no appropriate in-network option is reasonably available. The core argument is usually network insufficiency, not simple preference.
Is a gap exception the same as a single-case agreement?
Not always. A gap exception is usually about access failure in the network. A single-case agreement is often a payment arrangement with the out-of-network provider. In some cases they overlap, but you should not assume one automatically creates the other.
Does approval for the surgeon also cover the hospital or surgery center?
Not necessarily. Facility coverage may require separate confirmation. The same is true for anesthesia, assistant surgeons, monitoring, and other ancillary services.
Can I still get balance billed after a gap exception?
Sometimes, yes. The answer depends on plan terms, provider agreement, care setting, and whether in-network cost sharing or surprise-billing protections clearly apply to your specific situation. CMS explains that federal surprise-billing protections apply in certain circumstances, but not every out-of-network situation works the same way.
What should I look for first in the request letter?
Look for medical reason, network inadequacy reason, covered providers, covered facility, dates, and benefit-level wording. Those are the lines that decide whether the document is sturdy or theatrical.
What if the insurer says there is an in-network specialist available?
The dispute often becomes whether that specialist is realistically available, timely available, or clinically appropriate for the case. A provider being listed in a directory is not the same as a workable treatment path.
Does preauthorization mean the bill will be paid as in network?
No. Healthcare.gov states that preauthorization is not a promise your plan will cover the cost. Even where a service is approved, cost-sharing level and billing exposure still need separate confirmation. Downstream costs can also continue after approval, including rehab, so readers sometimes need a separate explanation of physical therapy copay vs. coinsurance.
What if the surgeon’s office says everything is approved but I still feel unsure?
Ask for the exact written approval, the scope of services, and confirmation of how claims will process for surgeon, facility, anesthesia, and follow-up care. Your unease may be doing useful work.
Next step
Before scheduling or paying anything large, make a one-page coverage summary for this case with four columns: provider, facility, service, and written coverage status. If any row is blank, the gap exception story is not finished yet.
That is the curiosity loop we opened at the beginning, and here is the answer plain and unsentimental: the most important thing about a gap exception request is not whether it sounds promising. It is whether the document is complete enough to survive contact with billing. In other words, the safest reader is not the most hopeful one. It is the one with a pencil, a short checklist, and a healthy disrespect for vague reassurance.
Within the next 15 minutes, pull out the letter, portal screenshot, or authorization note and do one pass only for scope: surgeon, facility, anesthesia, assistant, dates, and benefit language. You do not need to solve the entire case tonight. You just need to stop calling blank spaces “probably fine.” That single move is often where the money starts to come back under your control.
Last reviewed: 2026-03.
