
The Hidden Cast of Spine Procedure Billing
A spine procedure can be fully “covered” on paper and still produce an anesthesiology bill or pathology charge that feels like it came from a different universe. That is the quiet trap behind surprise bills: patients verify the surgeon and the facility, yet still get blindsided by billing entities they never knowingly chose.
The pain isn’t just the number, it’s the confusion. Was this a true out-of-network surprise, ordinary coinsurance, or a balance-billing issue protected by the No Surprises Act? By the time these questions arise, most are too exhausted to navigate the paperwork fog.
“Keep guessing, and you risk overpaying, missing appeal windows, or letting a negotiable bill harden into a permanent problem.”
This guide helps you spot where anesthesia, pathology, and neuromonitoring slip into your case. Learn to separate the billers, match the claims, and ask the narrow questions that yield real answers. Because in U.S. medical billing, the visible procedure is rarely the whole cast.
Table of Contents
- The surgeon and facility are not the whole cast
- Anesthesia and pathology can bill separately
- Documentation before surgery matters more than memory after surgery
Apply in 60 seconds: Start a one-page call log now with columns for provider name, tax ID if available, network status, and who told you.

Who This Is For / Not For
This is for you if you are
Scheduling a spine injection, decompression, fusion, discectomy, or related outpatient or inpatient procedure in the United States. It is also for the exhausted grown child helping a parent compare surgery centers, the spouse staring at a pre-op packet with a calculator nearby, and the self-pay patient trying to figure out whether the quote is a number or just a polite shrug.
I have seen this pattern with families who did everything “right.” They called ahead. They used the in-network hospital. They brought a notebook. Then the real confusion arrived in installments, which is a very American form of suspense.
This is not for you if you are
Looking for medical advice about whether to have spine surgery, researching surgical outcomes, or comparing recovery timelines. This piece stays on the billing side of the river. We are talking about the paper, the claims, the network status, and the parts that tend to go foggy when a procedure involves more people than the patient ever sees.
Eligibility checklist:
Answer yes or no.
- Do you have a scheduled or recently completed spine procedure?
- Did anyone use the words “covered,” “authorized,” or “in-network” without naming every participant?
- Do you expect separate bills from more than one entity?
- Are you uninsured, self-pay, or on a commercial plan where network status matters?
Next step: If you answered yes to even two of these, use the checklist later in this article before you sign anything else.
Hidden Players First, Why the Bill Multiplies After the Procedure
The “one surgery” illusion breaks fast
Patients understandably imagine a spine procedure as one event with one bill. Real billing behaves more like a string quartet where every musician sends a separate invoice. The surgeon may submit one claim. The hospital or ambulatory surgery center may submit another. Anesthesia may bill separately. Pathology may bill if tissue or material is reviewed. Imaging, radiology interpretation, neuromonitoring, assistants, implants, and device-adjacent services may pile on behind the curtain.
Why anesthesiology and pathology feel especially surprising
They feel surprising because patients usually do not shop for them the way they shop for surgeons. You choose the visible person. You rarely choose the backstage infrastructure. In normal life, that division is merely annoying. In billing, it becomes expensive.
One family once described this to me as “buying concert tickets, then being invoiced later by the oboist.” That image has never left me because it captures the emotional texture perfectly. The patient thinks they bought admission to the whole performance. The system thinks they purchased access to a venue with optional musicians.
Let’s be honest…
Most people do not know the name of the anesthesia group until the envelope arrives. That is not a character flaw. It is the design of the experience.
Show me the nerdy details
In U.S. billing, a single episode of care can generate separate professional and facility claims, often under different tax IDs and contracts. That is why network status for one participant does not automatically tell you the status of the others.
In-Network Mirage, Why “Covered Hospital” Does Not Always Mean Covered Team
Facility network status is not the whole story
A hospital or ambulatory surgery center can be in-network while some clinicians practicing inside it are not. That is the mirage. The building may belong to your network. The professionals inside the building may not all belong to your network. Those are different facts, and billing loves the difference.
Separate billing entities create the gap
Anesthesiologists, pathologists, radiologists, assistant surgeons, and neuromonitoring vendors often bill under separate legal and contracting structures. When patients hear “the procedure is covered,” they may be hearing a sentence that applies to the facility, the surgeon, or the broad category of service, but not to every biller attached to the date of service.
The phrase that causes trouble
“Your procedure is covered” is one of those sentences that sounds warm and complete, yet frequently arrives wearing missing buttons. It may not answer the sharper question: Which specific billing entities are in-network for this exact procedure, in this exact setting, on this exact plan?
Federal No Surprises Act protections apply to many non-emergency services from out-of-network providers furnished at certain in-network facilities, and CMS guidance specifically identifies anesthesiology, pathology, radiology, and certain other ancillary services as categories where balance-billing protections are especially important.
- Verify the facility separately
- Verify the surgeon separately
- Verify every supporting biller separately
Apply in 60 seconds: Replace “Is this covered?” with “Who will bill me separately?” on your next call.
Anesthesiology Trapdoors, How Patients Get Billed by a Group They Never Chose
Assignment is often automatic
Many facilities assign whichever anesthesia group is scheduled that day. Patients often have little or no practical ability to choose a different anesthesiologist or CRNA, especially for a hospital-based or surgery-center procedure. That is why the surprise feels so personal. The patient never made the selection that later becomes the billing problem.
Medical direction, supervision, and CRNA mix-ups
Anesthesia billing can involve more than one professional arrangement. You may see references to an anesthesiologist, a CRNA, medical direction, medical supervision, or a group entity that employs everyone involved. Patients hear a name in pre-op for 90 seconds, then months later discover the bill is tied less to the face they met than to the contract structure behind that face.
Emergency changes on procedure day
Schedules shift. Staffing gets swapped. A clinician calls out sick. A case runs long. A different anesthesia team steps in. Hospitals do not treat that shuffle as dramatic. Patients often do, once it appears on paper. I once saw a family compare it to airline seat changes, except with less legroom and worse consequences.
Here’s what no one tells you…
The person you meet briefly before sedation may not be the only line item that matters. The group contract is often the real weather system. The cloud is not the individual clinician. It is the entity submitting the claim.
Decision card: When to worry more about anesthesia billing
| Situation | Risk signal | Best move |
|---|---|---|
| Hospital says “we use a rotating group” | You cannot verify the biller early | Ask for the group name and tax ID in writing |
| ASC gives only a facility quote | Professional claim may be missing | Request every separate biller list |
| Procedure may need sedation changes | Day-of staffing can shift | Confirm who bills if assigned team changes |
Neutral action: Keep this table beside your pre-op paperwork when you call.
Official No Surprises Act guidance from CMS
Pathology Surprise Logic, Why a Tissue Sample Can Trigger a Second Financial Shock
Not every spine procedure involves pathology, but some do
If tissue, bone, cyst material, disc material, or another specimen is removed and sent for review, pathology may generate a separate claim. That part feels strange to many patients because the procedure itself already feels like one large event. The idea that a small cup, a lab route, and a professional interpretation can become a new financial chapter is rarely explained in plain English.
The lab may be outside your network even when the surgeon is not
Specimens may be routed to an independent pathology group or laboratory with its own contracts. This is where the phrase “routine specimen review” can become quietly expensive. The surgeon may be in-network. The facility may be in-network. The lab path can still take a scenic route through a different contracting landscape.
“Routine specimen review” still bills
Patients sometimes assume that examination of removed material is bundled into the surgery. Sometimes it is not. That does not always mean anyone acted improperly. It does mean the estimate you were handed may have described only the visible mountain and not the smaller hills behind it.
CMS materials on the No Surprises Act identify pathology as an ancillary service category, which matters because patients generally do not choose pathologists directly and federal surprise-billing protections limit certain out-of-network balance-billing scenarios in these settings.
Not Just Anesthesia, The Other Quiet Add-Ons That Travel With Spine Cases
Neuromonitoring can be the stealth invoice
Intraoperative neuromonitoring may be billed by a separate company. Patients often do not hear the vendor’s name until after the surgery because it sounds technical, distant, and tucked inside the operating room workflow. Then it appears later, crisp and impersonal, like a stranger arriving with a receipt.
Assistant surgeons and physician assistants
A first assist, assistant surgeon, or surgical assistant may generate an additional professional claim. In some cases, these charges are expected and contractually handled. In other cases, the patient never realized another biller had entered the scene at all.
Imaging and radiology interpretations
Fluoroscopy guidance, CT guidance, MRI interpretation, or follow-up imaging reads can show up as distinct line items. Imaging is the wallpaper of modern procedure care. Because it is always there, patients may stop noticing it as a separate cost driver. If you are already wrestling with lumbar MRI costs on an HDHP or comparing a broader high-deductible imaging cost estimate, this is exactly where the numbers can start stacking in ways that do not feel obvious on the front end.
Implant, biologics, and device-adjacent charges
These do not always qualify as “surprise bills” in the classic legal sense, but they can absolutely widen the cost gap between what you expected and what the case ultimately generated. This is where the distinction between hidden and surprising matters. Some charges are disclosed badly rather than disclosed never. Either way, the bank account still notices.
Coverage tier map: what changes as billing visibility improves
- Tier 1: You know only the surgeon and facility
- Tier 2: You know the anesthesia group
- Tier 3: You know lab, radiology, and assistants
- Tier 4: You have CPT codes and call-reference numbers
- Tier 5: You have written confirmation of network status for each biller
Neutral action: Do not confuse a Tier 2 case with a Tier 5 case. They feel similar until the bills arrive.
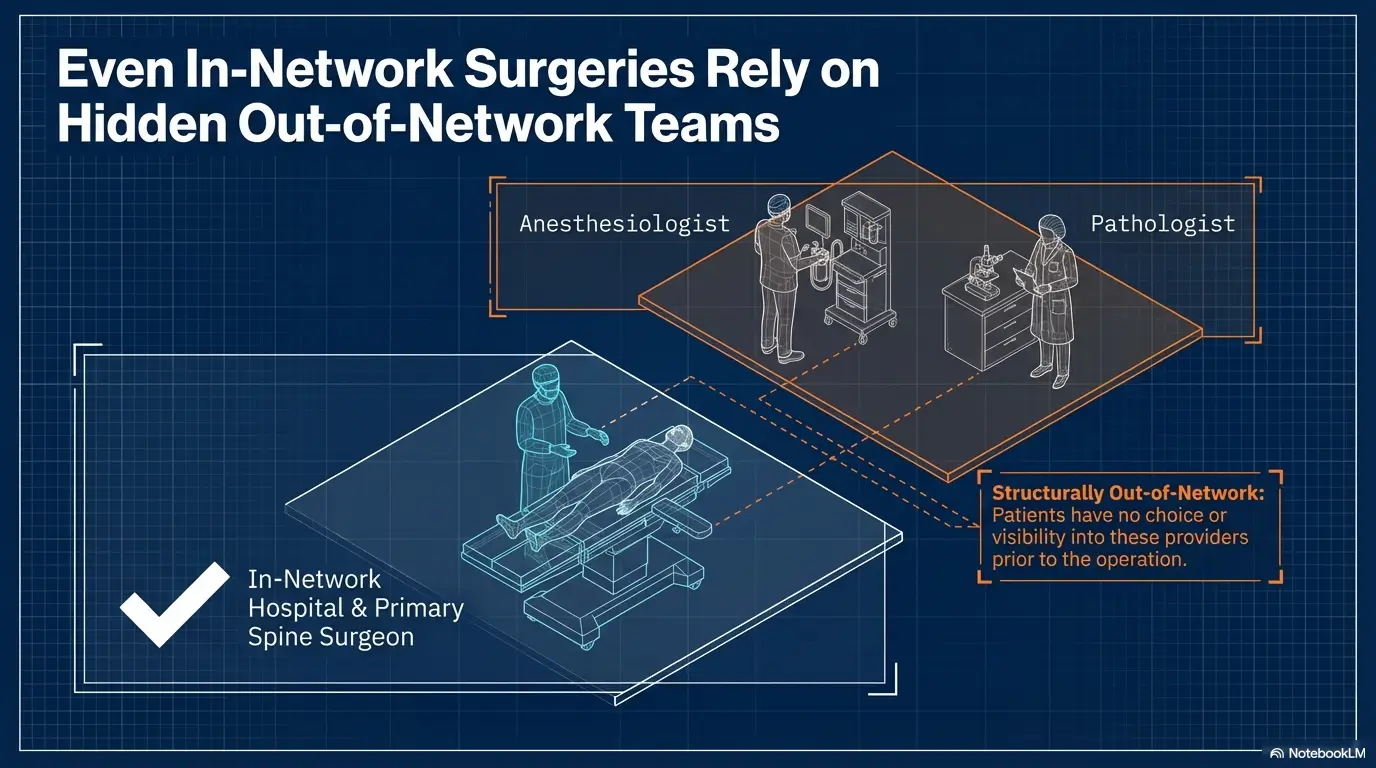
Before You Schedule, Questions That Expose Billing Risk While There Is Still Time
Ask the facility for every billing entity, not just one estimate
Request a written list of all professional and facility billers that may be involved. Not “What does the surgery cost?” Ask instead, “Please list every entity that may bill separately for this date of service.” That wording is less elegant and much more useful.
Ask your insurer the narrow question
Do not ask, “Is the surgery covered?” Ask, “Are the surgeon, facility, anesthesia group, pathology lab, neuromonitoring provider, radiologist, and assistant all in-network for these likely CPT codes?” Yes, it sounds like a mouthful. Mouthfuls are cheaper than mysteries.
Get the lab path straight
Ask where specimens would be sent if pathology is needed and whether that lab is in-network. Even if the answer is “pathology may not be necessary,” that is still useful. Conditional services are exactly where billing surprises like to live.
Curiosity gap worth chasing
If nobody can name the anesthesia group or pathology lab in writing, treat that uncertainty itself as a warning sign. Fog is information. It is telling you where visibility is poor and where follow-up matters most.
Quote-prep list: gather these before comparing facilities
- Insurance member ID and group number
- Name of surgeon and practice tax ID if available
- Name of facility and NPI or tax ID if available
- Likely CPT codes or at least procedure description
- Whether sedation, pathology, implants, or neuromonitoring are likely
- Your notes with dates, names, and reference numbers
Neutral action: Gather the list first, then make the insurer call once instead of five scattered calls.
For uninsured or self-pay patients, CMS says providers and facilities must provide a good faith estimate after scheduling or upon request, and federal patient-provider dispute rights may apply if the final bill is substantially higher than the estimate under the applicable rules. If that is your situation, it also helps to compare the general self-pay cash price range before you assume the first number placed in front of you is the only number the story can hold.
Don’t Do This, Pre-Op Assumptions That Create the Worst Billing Hangovers
Do not stop at the surgeon’s office estimate
Surgeon estimates are often sincere and still incomplete. They may exclude anesthesia, pathology, assistants, imaging interpretation, and outside vendors. The estimate is not always wrong. It is sometimes simply lonely.
Do not treat prior authorization as a price guarantee
Prior authorization is not the same as network confirmation, final payment amount, or your actual liability. Patients understandably cling to authorization because it feels official. In practice, it often confirms a medical-necessity review or plan processing step, not a full financial promise. That same paperwork tangle shows up earlier in the journey too, especially when people are trying to prove failed conservative care for an MRI and mistake approval steps for actual financial certainty.
Do not assume outpatient means simple billing
Ambulatory surgery centers can still produce multiple claims and multiple professional entities. The room may be smaller and the parking lot friendlier. The billing architecture can remain gloriously complicated. Anyone comparing a hospital bill against an ASC quote should also keep an eye on the difference between a hospital outpatient vs ASC facility fee, because that split alone can change the financial weather before anesthesia or pathology even enters the frame.
- Authorization is not a price lock
- Outpatient does not mean single-bill
- Incomplete estimates are common
Apply in 60 seconds: Highlight every place in your paperwork where a cost is described broadly instead of by billing entity.
Common Mistakes
Mistake 1: Asking only “Am I covered?”
That question is too broad to catch hidden professional claims. Coverage is a roof. Billing disputes happen in the corners.
Mistake 2: Forgetting that pathology may be conditional
Patients may not ask about pathology because they are unsure whether a specimen will even be taken. That uncertainty is exactly why it needs to be asked. “If tissue is sent, who bills?” is not overkill. It is adulthood in paperwork form.
Mistake 3: Ignoring the difference between estimate and contract status
A low estimate does not prove every participant is in-network. A high estimate does not prove the bill is final. Estimates are planning tools, not sacred texts.
Mistake 4: Failing to save names, dates, and reference numbers
When disputes begin, documentation becomes your flashlight. I once watched a patient win a reprocessing review because she had three things most people do not keep: the date, the first name, and the call reference number. Tiny details, giant leverage.
Mistake 5: Waiting too long to challenge a bill
Appeal windows, negotiation leverage, and dispute paths can narrow quickly. Paper is slow until suddenly it is not.
No, Really, Why This Still Happens Even After Surprise Billing Protections
Federal protections changed the landscape, not the entire maze
The No Surprises Act changed a great deal. It did not turn U.S. medical billing into a clear mountain stream. It turned it into a river with guardrails in important places. Those guardrails matter. They just do not answer every billing question a real patient encounters.
Ground ambulance, uncovered services, and classification disputes
Patients can still run into gray zones involving service type, plan design, notice-and-consent questions, claim classification, denied claims, or ordinary cost-sharing that feels like a surprise even when it is not legally a prohibited balance bill. Emotional surprise and legal surprise are cousins, not twins.
Self-funded plan details and state-federal overlap
The rules can shift depending on whether the health plan is fully insured or self-funded, whether state protections add something, and how the claim is categorized. That is why two families with almost identical procedures can have very different outcomes on paper.
Here’s the quiet catch…
Even when a bill should be challenged, it may still arrive first and clarity may arrive later. The mailbox does not wait for justice to warm up.
CMS guidance also explains that the notice-and-consent exception does not apply to several ancillary categories, including anesthesiology, pathology, radiology, assistant surgeons, and certain diagnostic services, which is one reason these categories matter so much in patient education.
Infographic: How one spine procedure becomes many bills
Surgeon + facility
Anesthesia team, assistants, vendors
Pathology, imaging, neuromonitoring, implants
Professional + facility claims, sometimes from separate contracts
Bottom line: The visible procedure is only the front stage. The billing exposure often lives backstage.
If the Bill Already Arrived, How to Untangle It Without Panicking
Step 1: Separate the claims by who billed
Sort the paperwork into piles: surgeon, facility, anesthesia, pathology, imaging, neuromonitoring, assistants, and any outside vendors. The goal is not elegance. It is containment. Panic thrives in piles. Progress begins in categories.
Step 2: Compare EOBs against invoices
An alarming invoice without the matching explanation of benefits can distort what is actually owed. Sometimes the bill arrived before insurer processing finished. Sometimes the provider statement reflects a gross charge before plan adjustments. Sometimes the problem is real. Sometimes it is simply early.
Step 3: Ask whether the charge is a balance bill, denied claim, or cost-share issue
These are different problems. A prohibited balance-billing issue is not the same as coinsurance. A denial for lack of prior authorization is not the same as an out-of-network ancillary provider dispute. Patients get stuck when they try to fight three separate problems with one generic sentence.
Step 4: Escalate in writing
Request an itemized bill, network-status confirmation, claim reprocessing if appropriate, and any applicable review pathway. If you speak with your insurer, ask them to note the account. If you speak with the provider, ask for the department name and call reference if available. The goal is to leave footprints every time you touch the case.
Mini calculator: estimate your immediate exposure bucket
Use three inputs: billed amount, insurer allowed amount if shown, and any payment already made.
Quick math: If the bill is $2,000, the allowed amount on the EOB is $700, and insurance already paid $500, your likely live issue may be the remaining patient cost-share on the allowed amount, not the full $2,000 headline number.
Neutral action: Do this math before paying from fear.
Healthcare.gov explains that internal appeals and external review rights can matter when a claim has been denied or processed in a way you believe is wrong, and consumer assistance or state insurance help may also be available depending on the plan and situation.
When to Seek Help
Seek help quickly if the bill is large relative to your income
Large anesthesia, pathology, or neuromonitoring invoices can move from stress to collections pressure with impressive speed. The larger the number, the less useful denial becomes as a coping strategy. I say that with affection. Denial is free, but it is not billable to the problem.
Seek help if there is a surgery date mismatch or unknown provider name
These are red flags for billing errors, misapplied claims, or opaque vendor involvement. If you do not recognize the entity name, slow the process down. Ask for itemization and verification before paying.
Seek help if you are being asked to pay before insurer processing finishes
Premature pressure can push patients into paying amounts that should have been reduced, reprocessed, or challenged. A bill can be urgent without being final.
Useful help paths
Your insurer’s escalation unit. Hospital or surgery-center patient financial services. A state consumer assistance or insurance complaint channel. Your employer benefits team if the coverage is job-based. In more severe disputes, a medical billing advocate or healthcare attorney may be worth the cost. Think of this as assembling a small chamber ensemble of adults who are willing to read the fine print with you.
Short Story: The envelope with the second surprise
A daughter once helped her father schedule a lumbar procedure at an in-network facility. She did the responsible things people are always told to do. She called the surgeon’s office. She confirmed the hospital. She wrote down the pre-op time on a sticky note that lived on the refrigerator like a small yellow flag of competence. Three weeks later, a pathology bill arrived from a name she had never heard.
At first she assumed it was a scam. Then she assumed it was bundled. Then she assumed, most dangerously, that if she ignored it long enough it might vanish back into the administrative woods. Instead, she called the facility, learned a specimen had been sent to an outside group, matched the bill against the EOB, and got the claim reviewed with the plan. The lesson was not that the system was fair. It was that clarity came only after she separated the actors and asked sharper questions than the first round of paperwork ever invited.
Next Step
Build a one-page “spine billing checklist” before you book
Write down the surgeon, facility, anesthesia group, pathology lab, neuromonitoring vendor, assistant provider, insurer reference number, and estimated CPT codes if available. One page, one call log, one folder. That single sheet can save you from a paper storm later.
Here is the version worth using in real life:
- Procedure: exact name or plain-language description
- Surgeon: name, practice, and phone number
- Facility: hospital or ASC name and billing office
- Anesthesia group: entity name, phone, network status
- Pathology lab: entity name if specimen might be sent
- Other billers: radiology, neuromonitoring, assistant, implants if disclosed
- Insurer call log: date, name, reference number, summary
- Estimate notes: what is included and what is specifically excluded
The magic here is not organizational beauty. It is friction reduction. In the middle of pain, pre-op nerves, and life still happening around you, the brain gets slippery. A single page gives the future version of you a handle.
- Write down every entity
- Track every call reference
- Keep estimates and EOBs together
Apply in 60 seconds: Open a notes app or grab paper and create the eight fields above before the day gets away from you.

FAQ
Can I get a surprise anesthesiology bill if my spine surgeon is in-network?
Yes. The anesthesia group may bill separately and may have different network status than the surgeon or facility. Even with federal protections in place for many situations, patients still need to understand whether the issue is prohibited balance billing, ordinary cost-sharing, or a claim-processing problem. This confusion can show up even in smaller outpatient pain cases, including questions around spine injection bill CPT codes or whether sedation for an epidural steroid injection creates an extra billing lane.
Why would pathology bill me after back surgery?
If tissue or other material was sent for examination, pathology may generate a separate professional claim. Patients often do not realize this because the specimen review happens behind the scenes and may involve a separate lab or pathology entity.
Is prior authorization proof that every provider is in-network?
No. Prior authorization is not a guarantee that all clinicians, vendors, or labs participating in the case are in-network, and it is not a final statement of your financial liability.
Are spine injections also at risk for surprise bills?
Yes. Depending on the setting and how the case is staffed, separate anesthesia, radiology, facility, or interpretation-related claims may appear. Patients comparing procedure types often run into this when choosing between a nerve root block vs epidural steroid injection, a SI joint injection vs lumbar ESI, or a TFESI vs interlaminar ESI for sciatica, because the clinical decision and the billing architecture do not always travel in a tidy pair.
Can an ambulatory surgery center still create surprise bills?
Yes. Outpatient settings can still involve multiple separate billers and contracting entities. Smaller building, same paperwork weather.
What should I ask before scheduling a spine procedure?
Ask for every expected billing entity, each provider’s network status, likely CPT codes if available, and where pathology specimens would be sent if taken. Also ask which charges are not included in the quote you were given.
What if I never signed anything mentioning out-of-network anesthesia?
That does not automatically erase liability, but it can matter depending on the circumstances, the category of service, and the applicable protection or review pathway. Save the paperwork and get the claim type clarified before paying from panic.
Can I negotiate a pathology or anesthesia bill after the fact?
Sometimes yes. Negotiation can be possible when network status was unclear, insurer processing is incomplete, the bill exceeds a good faith estimate for an uninsured or self-pay patient under applicable rules, or the provider offers prompt-pay or hardship adjustments. The same money logic tends to matter when patients are already comparing procedural price ranges such as self-pay TFESI cost, Medicare facet joint RFA cost, or broader lumbar spinal stenosis surgery costs.
What is the difference between a balance bill and coinsurance?
Balance billing generally refers to billing beyond the allowed amount in situations where that is not permitted or where the provider seeks the gap between charges and plan allowance. Coinsurance is your contractual share of covered costs under the plan. They feel similar in the wallet and are very different in the rulebook.
Final Thought
Back at the beginning, we named the trap: the patient thinks the surgery is the product, while the billing system treats the episode as a stack of participants. That is the curiosity loop, and now we can close it cleanly. Surprise bills around spine procedures often happen not because the patient failed to care, but because the visible decision and the invisible billing ecosystem are not the same thing.
The practical win is modest and powerful. In the next 15 minutes, create the one-page checklist, call the facility, and ask for every separate billing entity by name. Then call the insurer with that list instead of a vague question. That is how you turn a foggy “Am I covered?” into a precise map. It will not make the system beautiful. It will make you harder to surprise.
This article is for general U.S. medical billing education only and is not legal, insurance, or medical advice. Billing protections, appeal rights, and network rules can vary by health plan, employer funding structure, state overlap, and procedure setting. For a live bill, confirm details directly with your insurer and the billing entities involved.
Last reviewed: 2026-03.
